Abstract
Hyperammonemia occurs mainly in patients with branched-chain organic acidemias such as propionic, methylmalonic, and isovaleric acidemias. Its pathophysiological process is mainly via the competitive inhibition of N-acetylglutamate synthetase. Oral carglumic acid (N-carbamylglutamate) administration can correct hyperammonemia in neonates with propionic and methylmalonic acidemias, thus avoiding dialysis therapy. Isovaleric acidemia is an autosomal recessive disease of leucine metabolism due to deficiency of isovaleryl-CoA dehydrogenase. For the first time, we report a neonate with isovaleric acidemia, whose plasma ammonia concentration dropped dramatically after one oral load of carglumic acid. This experience suggests that carglumic acid could be considered for acute hyperammonemia resulting from isovaleric acidemia. However, trials with more patients are needed.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Isovaleric acidemia (IVA, OMIM #243500) is an autosomal recessively inherited organic acidemia caused by deficiency of the mitochondrial enzyme isovaleryl-CoA dehydrogenase (IVD, e.c. 1.3.99.10). It is a defect in the catabolism of leucine, resulting in the accumulation of derivatives of isovaleryl-CoA. Early diagnosis and treatment with a protein-restricted diet and supplementation with carnitine and glycine are effective in promoting normal development in severely affected individuals [1]. Two phenotypes have been reported: an acute neonatal and a chronic intermittent presentation. Patients with the acute form become symptomatic within the first 2 weeks after birth (poor feeding, vomiting, decreased consciousness, seizures). The second group presents with nonspecific symptoms such as failure to thrive or developmental delay. Both groups of patients are prone to intermittent acute episodes of decompensation with minor illnesses. Neonates appear initially well then develop nonspecific symptoms which include poor feeding, vomiting, decreased level of consciousness, and seizures [2].
In IVA, hyperammonemia as a symptom of metabolic decompensation is one of the major clinical problems which constitutes a severe insult to the developing infantile brain. Secondary hyperammonemia can occur in IVA and is due to competitive inhibition of N-acetylglutamate synthetase (NAGS, EC 2.3.1.1) by isovaleryl-CoA and/or intracellular depletion of acetyl-CoA, leading to reduced N-acetylglutamate synthesis and impairment of the urea cycle. Hyperammonemia is a neonatal emergency requiring rapid and vigorous treatment. N-Carbamylglutamate (NGG) is a structural analog of N-acetylglutamate, licensed as an orphan drug for the treatment of hyperammonemia due to NAGS deficiency. We report on a full-term neonate with IVA and hyperammonemia responding dramatically to oral NGG, thus avoiding the need for hemodialysis or peritoneal dialysis.
Case report
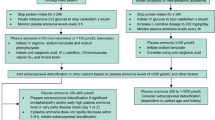
A male infant was born via full-term delivery after an uneventful pregnancy to second-degree consanguineous parents. His birth weight was 3.8 kg; gestational age was 38 weeks; and the Apgar index was 9 at 1 min and 10 at 5 min. A female sibling had died from an unknown cause in the neonatal period, and his other siblings were healthy. On the third day of life, the infant was hospitalized in the neonatal intensive care unit for vomiting, feeding refusal, and drowsiness. The patient was jittery, hypotonic, and dehydrated, and he had sweaty feet odor. His clinical condition and family history suggested an inherited metabolic disease. Laboratory investigations revealed hyperammonemia (568 μg/dl; normal range, 31–123 μg/dl) and ketonuria. Urine gas chromatography revealed an increased excretion of isovalerylglycine (1,277 mmol/mol cr; nv, 0 μmol/l), and blood acylcarnitines demonstrated an elevation of isovalerylcarnitine (9.9 μmol/l; nv, 0–0.6 μmol/l), suggesting that the patient had IVA. Oral feeding was stopped, and the baby was treated with intravenous infusions of glucose, parenteral lipid (after exclusion of fatty acid oxidation defect) and l-carnitine (100 mg/kg per day). In order to enhance metabolic detoxification, a single dose of carglumic acid (150 mg/kg per day) was administered through a nasogastric tube, and it was well tolerated; ammonia was monitored subsequently every 2 h. Over the following 6 h, the plasma ammonia levels dropped dramatically to 72 μg/dl, and blood ammonia remained normal thereafter. The patient began to be bottle-fed and was discharged at 10 days of life. At the age of 2 months, he has been neurologically normal, receiving protein-restricted diet, glycine (150 mg/kg per day) and l-carnitine, with good metabolic control. The IVD activity in the lymphocytes of the patient was severely reduced (<0.12 nmol/min per milligram protein; reference range, 0.89–2.13), confirming IVA.
Discussion
IVD is a mitochondrial enzyme which catalyzes the conversion of isovaleryl-CoA to 3-methylcrotonyl-CoA. Deficiency of this enzyme in patients with IVA results in toxic accumulations of isovaleric acid and other related organic acids. Elevated isovaleric acid itself produces the characteristic “odour of sweaty feet”, which may facilitate early diagnosis. The major metabolite of isovaleric acid which accumulates in this condition is isovalerylglycine. Patients with IVA may show two different forms of clinical presentation, either an acute neonatal or a chronic intermittent presentation. Those with the neonatal onset of the disease usually present with refusal to feed, vomiting, lethargy, severe illness, and death due to overwhelming hyperammonemia. Patients with the chronic intermittent form are asymptomatic at baseline but have episodes of acute metabolic decompensation, usually in the setting of infections, physical exertion, catabolic stress, or increased intake of protein-rich foods. More recently, a third group of individuals with mild biochemical abnormalities who can be asymptomatic have been identified through newborn screening of blood spots by tandem mass spectrometry. IVA is sometimes complicated by episodes of hyperammonemia [7–10].
The use of NGG has been reported in several neonates with hyperammonemia due to organic acidemias such as methylmalonic aciduria (McKusick 251000) and propionic aciduria (McKusick 232000) [5, 6]. NGG is safe, fast, and easy to administer, and it improves the acute therapy of decompensated organic acidemia by increasing ammonia detoxification and avoiding hyperammonemia. Until now, NGG was used only after failure of classical treatment, even though some authors have recommended giving this drug to neonates as soon as they suffer from severe hyperammonemia [3, 4]. To our knowledge, the newborn reported here is the first reported case with IVA to receive NGG for the treatment of hyperammonemia. We used a single dose of NGG, at the loading dose of 150 mg/kg. After one oral load of carbamylglutamate, ammonia decreased with a rate of approximately 100–150 μg/dl per hour. This treatment avoided dialysis, and no adverse effects attributable to carglumic acid were observed in our patient.
In conclusion, this experience suggests that carglumic acid could be considered for acute hyperammonemia in patients with IVA. The patient reported here showed a dramatic fall in the plasma ammonia concentration with a single dose of N-carbamylglutamate (150 mg/kg). Of course, trials with more patients are needed in order to demonstrate its usefulness.
Consent for publication has been obtained from the parents of our patient that was reported.
References
Castorina M, Rigante D, Antuzzi D, Sciascia Cannizzaro G, Ricci R (2008) Different outcome in isovaleric acidemia might be related to unsatisfactory diet compliance. Scand J Gastroenterol 43(6):767–768
Ensenauer R, Vockley J, Willard JM et al (2004) A common mutation is associated with a mild, potentially asymptomatic phenotype in patients with isovaleric acidemia diagnosed by newborn screening. Am J Hum Genet 75(6):1136–1142
Filippi L, Gozzini E, Fiorini P, Malvagia S, la Marca G, Donati MA (2010) N-carbamylglutamate in emergency management of hyperammonemia in neonatal acute onset propionic and methylmalonic aciduria. Neonatology 97(3):286–290
Gebhardt B, Dittrich S, Parbel S, Vlaho S, Matsika O, Bohles H (2005) N-carbamylglutamate protects patients with decompensated propionic aciduria from hyperammonaemia. J Inherit Metab Dis 28(2):241–244
Jones S, Reed CA, Vijay S, Walter JH, Morris AA (2008) N-Carbamylglutamate for neonatal hyperammonaemia in propionic acidaemia. J Inherit Metab Dis (in press)
Schwahn BC, Pieterse L, Bisset WM, Galloway PG, Robinson PH (2010) Biochemical efficacy of N-carbamylglutamate in neonatal severe hyperammonaemia due to propionic acidaemia. Eur J Pediatr 169(1):133–134
Shigematsu Y, Hata I, Tajima G (2010) Useful second-tier tests in expanded newborn screening of isovaleric acidemia and methylmalonic aciduria. J Inherit Metab Dis 33(Suppl 2):S283–288
Shigematsu Y, Hata I, Tanaka Y (2007) Stable-isotope dilution measurement of isovalerylglycine by tandem mass spectrometry in newborn screening for isovaleric acidemia. Clin Chim Acta 386(1–2):82–86
Sogut A, Acun C, Aydin K, Tomac N, Demirel F, Aktuoglu C (2004) Isovaleric acidaemia: cranial CT and MRI findings. Pediatr Radiol 34(2):160–162
Vockley J, Ensenauer R (2006) Isovaleric acidemia: new aspects of genetic and phenotypic heterogeneity. Am J Med Genet C Semin Med Genet 142C(2):95–103
Conflict of interest
The authors have no financial conflict of interest to report.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kasapkara, C.S., Ezgu, F.S., Okur, I. et al. N-carbamylglutamate treatment for acute neonatal hyperammonemia in isovaleric acidemia. Eur J Pediatr 170, 799–801 (2011). https://doi.org/10.1007/s00431-010-1362-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-010-1362-9