Abstract
Structural deficiencies within the cerebellum have been associated with schizophrenia. Whereas several region-of-interest-based studies have shown deviations in cerebellar volume, meta-analyses on conventional whole-brain voxel-based morphometry (VBM) studies do not implicate abnormalities in the cerebellum. Since this discrepancy could be due to methodological problems of VBM, we used a cerebellum-optimized VBM procedure. We acquired high-resolution MRI scans from 29 schizophrenia patients and 45 healthy controls and used a VBM approach utilizing the Spatially Unbiased Infratentorial toolbox (Diedrichsen in Neuroimage 33:127–138, 2006). Relative to healthy controls, schizophrenia patients showed reductions of grey matter volume in the left cerebellum Crus I/II that were correlated with thought disorder (p < 0.05; one-sided) and performance in the Trail-making test B (p < 0.01). No cerebellar group differences were detected employing conventional whole-brain VBM. The results derived from the cerebellum analysis provide evidence for distinct grey matter deficits in schizophrenia located in Crus I/II. The association of this area with thought disorder and Trail-making performance supports the previously suggested role of the cerebellum in coordination of mental processes including disordered thought in schizophrenia. The failure of conventional VBM to detect such effects suggests that previous studies might have underestimated the importance of cerebellar structural deficits in schizophrenia.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The potential role of the cerebellum in schizophrenia has been highlighted by the “cognitive dysmetria” hypothesis (Andreasen et al. 1996, 1999; Schmahmann 1991) which suggests an impaired coordination of sensorimotor and mental processes. In particular, cognitive dysmetria has been related to thought disorders. Thought disorders, rather than the more obvious signs, such as delusions and hallucinations, have been described as a primary feature of schizophrenia by Bleuler (1911). Previous studies reported volumetric abnormalities of the cerebellum in patients suffering from schizophrenia compared to healthy controls. Most of the studies showed reductions in cerebellar volume in patients (Barak et al. 2002; Heath et al. 1979; Nasrallah et al. 1982; Weinberger et al. 1982) but, in contrast, some others reported cerebellar volume increases (Keller et al. 2003; Levitt et al. 1999). The majority of the early volumetric studies used region-of-interest (ROI) analyses in which total cerebellar volume or substructures of the cerebellum such as the vermis were delineated manually or automatically. More recent studies relied on whole-brain analyses using voxel-based morphometry (VBM), providing a more exhaustive and unbiased assessment of structural differences. Some of these VBM studies have reported cerebellar abnormalities in schizophrenia patients (Chua et al. 2007; Venkatasubramanian 2010). Several quantitative meta-analyses of VBM studies exploring structural changes in brains of schizophrenia patients aimed at identifying regions that were consistently found as being altered. However, these analyses reported no convergence of evidence within the cerebellum, neither in grey (Cheung et al. 2010; Fornito et al. 2009; Glahn et al. 2008) nor in white matter (Di et al. 2009). This overall lack of convergence in quantitative meta-analyses stands in sharp contrast to a more consistent pattern in ROI-based analyses, which could be explained by methodological problems. For VBM methods, the small size of the subdivisions in the cerebellum poses a particular challenge to inter-subject normalization (Diedrichsen et al. 2010). The results rely on accurate normalization of cerebellum which has been shown to be suboptimal in custom analyses (Diedrichsen 2006; Diedrichsen et al. 2009). Recently, a spatially unbiased template has been introduced that addresses these problems. It improves the overlap of the major fissures (e.g., the primary fissure) in the cerebellum between subjects by reducing the spatial variance to one-third (Diedrichsen 2006). Therefore, the purpose of the present study was to employ the Spatially Unbiased Infratentorial (SUIT) toolbox (Diedrichsen 2006) in conjunction with VBM in order to provide an optimized assessment of structural alterations in the cerebellum of schizophrenia patients and their association with the psychopathology of thought disorders and cognitive performance.
Methods
Participants
Twenty-nine schizophrenia patients were compared to 45 healthy control subjects. Demographic and additional data describing patients and control subjects are presented in Table 1.
Patients were recruited among inpatients (n = 13) and outpatients (n = 16) of the Charité Department of Psychiatry and Psychotherapy, Campus Mitte. To confirm the initial previous diagnosis by an independent psychiatrist, a Structured Clinical Interview for Axis I DSM-IV Disorders (First et al. 1996) was performed by an experienced senior consultant psychiatrist. 27 patients had been treated with risperidone at the time of the scan (17 had been treated <1 year, 7 longer than 1 year and 4 longer than 5 years; mean dose 4.1 ± 1.56 mg). Three of the patients received benzodiazepines additionally. The duration of illness was assessed as the time in years between the first episode and the current investigation. Patients with other psychiatric Axis I disorders were excluded.
Control subjects were recruited by means of newspaper advertisements. According to personal interviews (Mini-International Neuropsychiatric Interview, Sheehan et al. 1998) carried out by a psychiatrist, healthy subjects were free of medical, neurological and psychiatric disorders. Control subjects with a family history (first degree) of Axis I disorder were excluded. In addition, exclusion criteria for all subjects were abnormalities in the MRI, general medical disorders, or other clinically relevant abnormalities. The study was approved by the ethics committee of Charité University Clinic Germany. After complete description of the study, the subjects gave a written informed consent.
Symptom measurement and cognitive tests
To assess the severity of schizophrenia symptoms, we used the Brief Psychiatric Rating Scale (BPRS, Overall and Gorham 1962). We administered several cognitive tests including the Trail-making test (TMT A and B, Reitan and Wolfson 1996) providing information on visual search, scanning, speed of processing, mental flexibility and executive control; the Stroop task (Stroop 1935) a test of attentional and executive control; two word fluency test (TWFT): naming animals (Goodglass and Kaplan 1972) and naming words with the letter “S” (Thurstone 1938); the continuous performance test (CPT, Mackworth and Taylor 1963) assessing sustained and selective attention; and a picture memory test (participants saw line drawings of 20 known objects for 30 s and had to name those that they remembered immediately after the 30 s).
Scanning procedure
MR measurements were carried out on a 3-Tesla scanner (MEDSPEC 30/100, Bruker Biospin, Ettlingen, Germany). T1-weighted images were acquired using MDEFT (modified driven equilibrium Fourier transform, with T E = 3.8 ms, T R = 20.53 ms; T I = 550 ms, nominal flip angle 30°; 128 contiguous slices, 1.5 mm thick; 1-mm inplane (x–y) resolution).
Data analysis
First, study-specific templates were built to compensate scanner specific contrast differences and non-uniformities as well as demographic differences between our current sample and the sample from which the standard Montreal Neurological Institute (MNI) templates were created. By means of the isolate function within the SUIT toolbox (http://www.icn.ucl.ac.uk/motorcontrol/imaging/suit.htm, Diedrichsen 2006), we isolated infra-tentorial structures, namely cerebellum and brainstem, from the surrounding tissue. Then a new prior probability distribution defined in the SUIT space was used. Because of the improved anatomical alignment, this prior probability distribution is much more clearly defined than the one used in the first iteration, therefore improving the classification results. The segmented grey matter (GM) images were then normalized to the SUIT template. A modulation of the segmented GM probability map was undertaken to compensate for volume changes during the spatial normalization by multiplying the intensity value in each voxel with the Jacobian determinants. Finally, the resulting GM probability images were smoothed with a 4 mm full-width half maximum (FWHM) kernel in SPM5 to satisfy the Gaussian distribution assumption for statistical analysis of regional differences. The use of the small 4 mm smoothing kernel is in line with previous publications that focussed on cerebellum VBM by means of the SUIT toolbox (D’Agata et al. 2011; Fan et al. 2010). All images were visually inspected to ensure that the pre-processing steps were successful and that the quality of each image was acceptable for subsequent analysis. Because we found significant differences in age, cigarettes per day and the distribution of sex between patients and healthy controls (Table 1), we controlled for brain volume (cerebellum and brainstem) age, sex and cigarettes per day in our analysis. The resulting maps were thresholded with p < 0.001 and cluster size corrected by means of Monte Carlo simulation. Accordingly, significant effects were reported when the volume of the cluster was greater than the minimum cluster size determined by Monte Carlo simulation on the cerebellum GM volume (>120 voxels), above which the probability of type I error was below 0.01 (AlphaSim, Ward 2000). Anatomical localizations (i.e., cerebellar lobules) were determined by the probabilistic MRI atlas of the human cerebellum developed by Diedrichsen et al. (2009).
In order to compare our cerebellum results to those of common whole-brain VBM analyses we computed the same analysis (controlling for age, sex, cigarettes per day and brain volume) on GM maps based on the optimized VBM procedure. This procedure spatially normalizes GM-segmented images to a standard space by matching images to their GM template (Good et al. 2001). We used the same smoothing kernel of 4 mm FWHM as in the previous analysis but a lenient threshold of p < 0.001 (uncorrected), in order to obtain a high sensitivity in detecting GM effects in the cerebellum.
We extracted the GM volume of each participant within the regions of significant difference between schizophrenia patients and healthy controls (in left Crus I/II) by means of MarsBaR (http://marsbar.sourceforge.net). The correlation analysis for cerebellar volume deficit regions and clinical or cognitive parameters was performed using Pearson’s correlation test.
Results
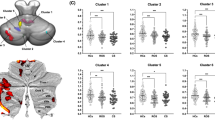
To explore structural differences between schizophrenia patients and healthy control subjects in the cerebellum we contrasted the GM volume maps against one another. We controlled for age, sex, brain volume and cigarette consumption. We found that schizophrenia patients had lower GM volume than healthy controls in left cerebellum Crus I/II (−36, −64, −48, cluster size 505 voxels, cluster corrected at p < 0.01, Fig. 1). There were no regions where GM volume was significantly increased in schizophrenia patients compared to healthy controls.
Significant cluster of cerebellar grey matter volume reduction in left Crus I and II (blue; −36, −64, −48) in schizophrenic patients compared to healthy controls (p values corrected for multiple comparisons, p < 0.01). Top coronal slice, bottom left sagittal slice, bottom right 3D rendering of the cerebellum
In order to relate the cerebellar abnormality to clinical symptoms, we correlated GM volume in Crus I/II with the factor thought disorder of the BPRS. We found a negative correlation between thought disorder and left Crus I/II [r (26) = −0.383, p < 0.05, one-sided, Fig. 2]. There were no significant correlations between left Crus I/II and other factor scores of the BPRS.
Since cerebellar volume has been associated with cognition, we aimed at exploring whether reduced GM volume in Crus I/II is correlated with cognitive performance measures in schizophrenia patients. We found a significant positive correlation between the percent rank in TMT B and GM volume in left Crus I/II [r (26) = 0.55, p < 0.01, Fig. 3], indicating that slower performance was associated with less GM volume but not for TMT A [r (26) = −0.03, p = 0.90]. Both correlation coefficients are significantly different from one another (z = 2.2, p < 0.05; Hinkle et al. 1988).
To compare the results of our cerebellum-optimized VBM procedure to regular whole-brain VBM results in the cerebellum, we analyzed our data with an optimized VBM protocol (Good et al. 2001) but with the same smoothing kernel as in the cerebellum-optimized analysis. In line with several meta-analyses on VBM GM changes in schizophrenia (Cheung et al. 2010; Fornito et al. 2009; Glahn et al. 2008), we found no increases or reductions in GM volume in the cerebellum in this analysis (p < 0.001, uncorrected). No cluster corrected results were found in the whole-brain VBM analysis outside the cerebellum.
Discussion
The present study focussed on structural alteration in cerebellum of schizophrenia patients as compared to healthy controls using a cerebellum-optimized VBM protocol that allows a highly sensitive investigation of cerebellar GM volume. The results show a volume deficit in a particular region of the left Crus I/II in schizophrenia patients predicting the amount of thought disorder in the current psychopathology and performance in the TMT B.
Previous studies that have segmented the entire cerebellum or large substructures of the cerebellum, manually or automatically, frequently reported decreases in cerebellar volume in schizophrenia patients (for an overview: Andreasen and Pierson 2008; Konarski et al. 2005; Picard et al. 2008). A disadvantage of these ROI-based approaches is that the localization within the cerebellum is not very precise; the results are reported mostly for the entire cerebellar hemisphere or vermis.
Recent advances in the analysis of structural brain images introduced whole-brain VBM methods that test for local differences in GM volume on the whole brain level. Although some studies reported VBM findings in the cerebellum of schizophrenia patients (Chua et al. 2007; Venkatasubramanian 2010) the localization of these abnormalities seems to be inconsistent. Quantitative meta-analyses testing for consistent findings across whole-brain VBM studies comparing grey and white matter in schizophrenia patients against healthy controls failed to find overlap in the cerebellum (Cheung et al. 2010; Fornito et al. 2009; Glahn et al. 2008; Di et al. 2009). The VBM results highly depend on accurate normalization. This is problematic for results in the cerebellum, because especially the normalization of the cerebellum and brainstem has been shown to be difficult in custom neuroimaging analysis (Diedrichsen 2006; Diedrichsen et al. 2009).
Our results are in line with these methodological considerations: we found no differences in the cerebellum when processing the structural images according to a common optimized VBM procedures (Good et al. 2001), but we found clear differences when using a cerebellum-optimized VBM procedure (based on the SUIT toolbox, Diedrichsen 2006). The observed reduction of GM volume in left Crus I/II of the cerebellum in schizophrenia patients is in accordance with previous ROI-based studies that reported reductions in the entire cerebellum (Barak et al. 2002; Nasrallah et al. 1982; Weinberger et al. 1982; Keller et al. 2003). A recent study that explored regional cerebellar differences between first-episode schizophrenic patients and controls using cortical pattern matching (Rasser et al. 2010) reports more widespread group differences within the cerebellum including the region of difference, which we observed within Crus I/II.
The absence of whole-brain VBM differences in the cerebrum could be due to our moderate sample size and is at least partly in line with the fact that some studies report GM volume decreases in schizophrenic patients, but others report increases (Glahn et al. 2008; Honea et al. 2005) and the regions in which alterations have been observed are diverse (Honea et al. 2005).
Although the role of the cerebellum has traditionally been seen in the coordination of motor functions, recently non-motor functions such as cognition and emotion have been associated with the cerebellum (Strick et al. 2009). In particular, Crus I and II have been related to cognitive functions. A meta-analysis on functional neuroimaging studies with healthy participants has associated Crus I with verbal working memory and executive functions (Stoodley and Schmahmann 2010). Studies comparing cerebellar activity of schizophrenia patients and healthy controls demonstrated reduced activity during recall of facial pictures (Andreasen and Pierson 2008), working memory (Walter et al. 2007) and recall of practiced wordlists (Crespo-Facorro et al. 1999) in close proximity to the region in which we found GM volume reductions. The “cognitive dysmetria” hypothesis (Andreasen et al. 1996, 1998, 1999) assumes that the cerebellum of schizophrenia patients is less efficient in error detection and in relaying updated information to the cerebral cortex, thus causing symptoms like disordered thought, hallucinations and deficiencies in cognitive task performance.
Based on these functional associations between Crus I/II and cognition and based on the “cognitive dysmetria” hypothesis, we explored correlations between the GM volume within left Crus I/II and symptoms of the BPRS as well as several cognitive tasks within the sample of schizophrenia patients. We found a negative correlation with the symptom-scale thought disorder. The term thought disorders is used to describe patterns of disordered language use that are presumed to reflect disordered thinking. The language is characterized by abnormalities, such as tangentiality, neologisms, flight of ideas, paraphrasias and private use of words (Andreasen 1997). In schizophrenia formal thought disorder has been related to impairments in semantic and executive components as well as self monitoring during language processing (Kerns and Berenbaum 2002). Previous studies have reported associations between thought disorder and cerebellum in schizophrenia patients. Levitt et al. (1999) found a positive correlation between vermis white matter volume and symptoms of thought disorder. Kircher et al. (2001) reported a positive correlation between neural activity of patients while talking about Rorschach inkblots in cerebellar vermis and formal thought disorder. The association between cerebellar abnormalities and formal thought disorder is in accordance with assumptions of the “cognitive dysmetria” hypothesis suggesting that online monitoring of thoughts is impaired or mistimed, leading to a disruption of fluid and coordinated sequences of thought (Andreasen 1999). But the correlation observed does not survive Bonferroni correction when accounting for multiple testing. Future research is needed to explore the relationship between cerebellar volume and thought disorder a priori.
Furthermore, we found that better performance in the Trail-making B test was associated with higher GM volume in left Crus I/II. Being one of the common neuropsychological tests to assess the executive function of mental set shifting, the TMT B is required to search for and connect targets containing digits and letters with a pencil in ascending order, alternating between digits and letters. In order to exclude that the observed results are due to neurological soft signs that have been reported in schizophrenia (Chan and Gottesman 2008; Dazzan et al. 2008; Gupta et al. 1995), we compared the results to the association between Crus I/II and TMT A. TMT A involves the connection of targets but consisting of digits only, so that the task switching component is absent but the motoric component is present as well. Interestingly, we only found a significant association between GM in Crus I/II and the TMT B, not TMT A. Hence, we conclude that the observed association is based on the task switching and therefore cognitive components not on the motoric component of the task. Impaired performance in schizophrenia has been reported at different stages of illness (Bilder et al. 2000; Liddle and Morris 1991; Riley et al. 2000) as well as for healthy relatives of schizophrenia patients (Franke et al. 1993), suggesting the test’s potential as a vulnerability marker. The association of this behavioral vulnerability marker with the GM volume reduction in left Crus I/II indicates its possible role in schizophrenia.
To conclude, the uncovering of effects with the cerebellum-optimized procedure, in contrast to the failure of a common whole-brain VBM analysis to detect such effects, suggests that previous studies exploring structural abnormalities might have underestimated the importance of alterations in the cerebellum of schizophrenia patients. Further research on larger samples of schizophrenia patients is needed to establish connections between thought disorder, cognitive task performance and localized cerebellar GM volume reductions.
References
Andreasen NC (1997) Thought, language, and communication disorders. I. Clinical assessment, definition of terms, and evaluation of their reliability. Arch Gen Psychiatry 36:1315–1321
Andreasen NC (1999) A unitary model of schizophrenia. Bleuler’s “fragmented phrene” as schizencephaly. Arch Gen Psychiatry 56:781–787
Andreasen NC, Pierson R (2008) The role of the cerebellum in schizophrenia. Biol Psychiatry 64:81–88
Andreasen NC, O’Leary DS, Cizadlo T, Arndt S, Rezai K, Ponto LL, Watkins GL, Hichwa RD (1996) Schizophrenia and cognitive dysmetria: a positron-emission tomography study of dysfunctional prefrontal-thalamic-cerebellar circuitry. Proc Natl Acad Sci USA 93:9985–9990
Andreasen NC, Paradiso S, O’Leary DS (1998) “Cognitive dysmetria” as an integrative theory of schizophrenia: a dysfunction in cortical-cerebellar circuitry? Schizophr Bull 24:203–218
Andreasen NC, Nopoulos P, O’Leary DS, Miller DD, Wassink T, Flaum M (1999) Defining the phenotype of schizophrenia: cognitive dysmetria and its neural mechanisms. Biol Psychiatry 46:908–920
Barak Y, Aizenberg D, Mirecki I, Mazeh D, Achiron A (2002) Very late-onset schizophrenia-like psychosis: clinical and imaging characteristics in comparison with elderly patients with schizophrenia. J Nerv Ment Dis 190:733–736
Bilder RM, Goldman RS, Robinson D, Reiter G, Bell L, Bates JA, Pappadppulos E, Willson DF, Alvir JM, Woerner MG, Geisler S, Kane JM, Lieberman JA (2000) Neuropsychology of firstepisode schizophrenia: initial characterization and clinical correlates. Am J Psychiatry 157:549–559
Bleuler E (1911) Dementia praecox oder Gruppe der Schizophrenien. F. Deuticke, Leipzig
Chan RC, Gottesman II (2008) Neurological soft signs as candidate endophenotypes for schizophrenia: a shooting star or a Northern star? Neurosci Biobehav Rev 32:957–971
Cheung C, Yu K, Fung G, Leung M, Wong C, Li Q, Sham P, Chua S, McAlonan G (2010) Autistic disorders and schizophrenia: related or remote? An anatomical likelihood estimation. PLoS One 5:e12233
Chua SE, Cheung C, Cheung V, Tsang JT, Chen EY, Wong JC, Cheung JP, Yip L, Tai KS, Suckling J, McAlonan GM (2007) Cerebral grey, white matter and csf in never-medicated, first-episode schizophrenia. Schizophr Res 89:12–21
Crespo-Facorro B, Paradiso S, Andreasen NC, O’Leary DS, Watkins GL, Boles Ponto LL, Hichwa RD (1999) Recalling word lists reveals “cognitive dysmetria” in schizophrenia: a positron emission tomography study. Am J Psychiatry 156:386–392
D’Agata F, Caroppo P, Boghi A, Coriasco M, Caglio M, Baudino B, Sacco K et al (2011) Linking coordinative and executive dysfunctions to atrophy in spinocerebellar ataxia 2 patients. Brain Struct Funct 216:275–288
Dazzan P, Lloyd T, Morgan KD, Zanelli J, Morgan C, Orr K, Hutchinson G et al (2008) Neurological abnormalities and cognitive ability in first-episode psychosis. Br J Psychiatry 193:197–202
Di X, Chan RCK, Gong Q (2009) White matter reduction in patients with schizophrenia as revealed by voxel-based morphometry: an activation likelihood estimation meta-analysis. Prog Neuropsychopharmacol Biol Psychiatry 33:1390–1394
Diedrichsen J (2006) A spatially unbiased atlas template of the human cerebellum. Neuroimage 33:127–138
Diedrichsen J, Balsters JH, Flavell J, Cussans E, Ramnani N (2009) A probabilistic MR atlas of the human cerebellum. Neuroimage 46:39–46
Diedrichsen J, Verstynen T, Schlerf J, Wiestler T (2010) Advances in functional imaging of the human cerebellum. Curr Opin Neurol 23:382–387
Fan L, Tang Y, Sun B, Gong G, Chen ZJ, Lin X, Yu T et al (2010) Sexual dimorphism and asymmetry in human cerebellum: an MRI-based morphometric study. Brain Res 1353:60–73
First MB, Gibbon M, Spitzer RL, Williams JBW, Benjamin L (1996) User’s guide for the structured clinical interview for DSM-IV axis II personality disorders (SCID-II). Biometrics Research Department, New York State Psychiatric Institute, New York
Fornito A, Yücel M, Patti J, Wood SJ, Pantelis C (2009) Mapping grey matter reductions in schizophrenia: an anatomical likelihood estimation analysis of voxel-based morphometry studies. Schizophr Res 108:104–113
Franke P, Maier W, Hardt J, Hain C (1993) Cognitive functioning and anhedonia in subjects at risk for schizophrenia. Schizophr Res 10:77–84
Glahn DC, Liard AR, Ellison-Wright I, Thelen SM, Robinson JL (2008) Meta-analysis of gray matter anomalies in schizophrenia: application of anatomic likelihood estimation and network analysis. Biol Psychiatry 64:774–781
Good CD, Johnsrude IS, Ashburner J, Henson RN, Friston KJ, Frackowiak RS (2001) A voxel-based morphometric study of ageing in 465 normal adult human brains. Neuroimage 14:21–36
Goodglass H, Kaplan E (1972) The assessment of aphasia and related disorders. Lea & Febiger, Philadelphia
Gupta S, Andreasen NC, Arndt S, Flaum M, Schultz SK, Hubbard WC, Smith M (1995) Neurological soft signs in neuroleptic-naive and neuroleptic-treated schizophrenic patients and in normal comparison subjects. Am J Psychiatry 152:191–196
Heath R, Franklin D, Shraberg D (1979) Gross pathology of the cerebellum in patients diagnosed and treated as functional psychiatric disorders. J Nerv Ment Dis 167:585–592
Hinkle DE, Wiersma W, Jurs SG (1988) Applied statistics for the behavioral sciences, 2nd edn. Houghton Mifflin Company, Boston
Honea R, Crow TJ, Passingham D, Mackay CE (2005) Regional deficits in brain volume in schizophrenia: a meta-analysis of voxel-based morphometry studies. Am J Psychiatry 162:2233–2245
Keller A, Castellanos FX, Vaituzis AC, Jeffries NO, Giedd JN, Rapoport JL (2003) Progressive loss of cerebellar volume in childhood-onset schizophrenia. Am J Psychiatry 160:128–133
Kerns JG, Berenbaum H (2002) Cognitive impairments associated with formal thought disorder in people with schizophrenia. J Abnorm Psychol 111:211–224
Kircher TTJ, Liddle PF, Brammer MJ, Williams SCR, Murray RM, McGuire P (2001) Neural correlates of formal thought disorder in schizophrenia. Arch Gen Psychiatry 58:769–774
Konarski JZ, McIntyre RS, Grupp LA, Kennedy SH (2005) Is the cerebellum relevant in the circuitry of neuropsychiatric disorders? Rev Psychiatr Neurosci 30:178–186
Levitt JJ, McCarley RW, Nestor PG, Petrescu C, Donnino R, Hirayasu Y et al (1999) Quantitative volumetric MRI study of the cerebellum and vermis in schizophrenia: clinical and cognitive correlates. Am J Psychiatry 156:1105–1107
Liddle PF, Morris DL (1991) Schizophrenic syndromes and frontal lobe performance. Br J Psychiatry 158:340–345
Mackworth JF, Taylor MM (1963) The d’ measure of signal detectability during vigilance-like situations. Can J Psychol 17:302–325
Nasrallah HA, McCalley-Whitters M, Jacoby CG (1982) Cortical atrophy in schizophrenia and mania: a comparative CT study. J Clin Psychiatry 43:439–441
Overall JE, Gorham DR (1962) The Brief Psychiatric Rating Scale. Psychol Reports 10:799–812
Picard H, Amado I, Mouchet-Mages S, Olie JP, Krebs MO (2008) The role of the cerebellum in schizophrenia: an update of clinical, cognitive, and functional evidences. Schizophr Bull 34:155–172
Rasser PE, Schall U, Peck G, Cohen M, Johnston P, Khoo K, Carr VJ, Ward PB, Thompson PM (2010) Cerebellar grey matter deficits in first-episode schizophrenia mapped using cortical pattern matching. Neuroimage 53:1175–1180
Reitan RM, Wolfson D (1996) The Halstead–Reitan neuropsychological test battery: theory and clinical interpretation, 2nd edn. Neuropsychology Press, Tucson
Riley EM, McGovern D, Mockler D, Doku VC, O’Ceallaigh S, Fannon DG, Tannakoon L, Santamaria M, Soni W, Morris RG, Sharma T (2000) Neuropsychological functioning in first-episode psychosis—evidence of specific deficits. Schizophr Res 43:47–55
Schmahmann JD (1991) An emerging concept: the cerebellar contribution to higher function. Arch Neurology 48:1178–1187 and 49:1230
Sheehan RV, Lecrubier Y, Sheehan KH, Amorim P, Janavs J, Weiller E, Hergueta T, Baker R, Dunbar GC (1998) The Mini-International Neuropsychiatric Interview (M.I.N.I.): the development and validation of a structured diagnostic interview for DSM-IV and ICD-10. J Clin Psychiatry 59(Suppl 20):22–33
Stoodley CJ, Schmahmann JD (2010) Functional topography in the human cerebellum. A meta-analysis of neuroimaging studies. Neuroimage 44:489–501
Strick PL, Dum RP, Fiez JA (2009) Cerebellum and nonmotor function. Annu Rev Neurosci 32:413–434
Stroop JR (1935) Studies of interference in serial verbal reactions. J Exp Psychol 18:643–662
Thurstone LL (1938) Primary mental abilities. University of Chicago Press, Chicago
Venkatasubramanian G (2010) Neuroanatomical correlates of psychopathology in antipsychotic-naïve schizophrenia. Indian J Psychiatry 52:28–36
Walter H, Vasic N, Hose A, Spitzer M, Wolf RC (2007) Working memory dysfunction in schizophrenia compared to healthy controls and patients with depression: evidence from event-related fMRI. Neuroimage 35:1551–1561
Ward BD (2000) Simultaneous inference for fMRI data. AFNI AlphaSim Documentation, Medical College of Wisconsin
Weinberger DR, DeLisi LE, Perman GP, Targum S, Wyatt RJ (1982) Computed tomography in schizophreniform disorder and other acute psychiatric disorders. Arch Gen Psychiatry 39:778–783
Acknowledgments
SK is a Postdoctoral Fellow of the Research Foundation Flanders (FWO).
Conflict of interest
The authors report no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kühn, S., Romanowski, A., Schubert, F. et al. Reduction of cerebellar grey matter in Crus I and II in schizophrenia. Brain Struct Funct 217, 523–529 (2012). https://doi.org/10.1007/s00429-011-0365-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00429-011-0365-2