Abstract
The stimulation of glucose transport by metabolic stress is an important determinant of myocardial susceptibility to ischemia and reperfusion injury. Stimulation of glucose transport is markedly impaired in cardiomyocytes chronically exposed to excess free fatty acids (FFA), as occurs in vivo in type 2 diabetes. To determine whether chronic low-grade activation of AMP-activated kinase (AMPK) improves substrate metabolism in cardiomyocytes exposed to FFA, isolated cultured cardiomyocytes were exposed for 7 days to FFA ± the AMPK agonist 5-aminoimidazole-4-carboxamide ribonucleoside (AICAR). Glucose transport and glycolysis were then measured during acute metabolic stress provoked by oligomycin. Chronic treatment with AICAR improved basal and oligomycin-stimulated glucose transport in FFA-exposed but not in control cardiomyocytes. Similarly, basal and oligomycin-stimulated glycolysis was reduced in FFA-exposed cardiomyocytes but restored by chronic AICAR treatment. Conversely, fatty acid oxidation was increased in FFA-exposed cardiomyocytes and reduced by chronic AICAR treatment. Chronic AICAR treatment induced in FFA-exposed cardiomyocytes the biogenesis of numerous lipid droplets. Curiously, whereas acute treatment of cardiomyocytes with AICAR increased phosphorylation of the AMPKα subunit on T172, a classical marker of AMPK activation, chronic AICAR treatment almost completely obliterated T172 phosphorylation. However, phosphorylation of the AMPK target protein raptor on S792 was reduced in FFA-exposed cardiomyocytes but restored by AICAR treatment. In conclusion, chronic AICAR treatment induces a metabolic shift in FFA-exposed cardiomyocytes, characterized by improved glucose transport and glycolysis and redirection of fatty acids towards neutral storage. Such metabolic changes in vivo could protect the hearts of patients with type 2 diabetes against ischemia-reperfusion injury.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The heart is remarkably metabolically adaptable, being capable of using of wide variety of metabolic substrates to face the high ATP requirement due to incessant cardiac work. Among these substrates, glucose usually accounts for less than a quarter of the cardiac ATP production. Glucose is however important as a substrate from which energy can be extracted even during ischemia or hypoxia, from substrate-level phosphorylation in glycolysis. Stimulation of glucose uptake is thus a first line of defense for the myocardium undergoing ischemic stress. The importance of stimulation of glucose metabolism to withstand ischemic stress is illustrated by the poor recovery of GLUT4-null hearts [49] or hearts deficient in AMP-activated protein kinase (AMPK) [42], which are incapable of stimulation of glucose transport. Indeed, activation of the AMPK triggers the translocation of GLUT4 [41], stimulates glucose transport, and appears to mediate the effects of ischemia. Most importantly, impairment of AMPK-triggered stimulation of myocardial glucose uptake during ischemia and reperfusion is associated with reduced recuperation of contractile function and increased cardiac injury [42]. Stimulation of glucose transport is deficient in the myocardium of type II diabetes patients [22] as well as in animal models of type II diabetes [37]; this defect presumably contributes to the worse outcome of acute myocardial infarction in diabetic patients [1, 7] and to increased ischemia-reperfusion myocardial injury in animals [24]. Therefore, a pharmaceutical intervention that could improve glucose transport in the diabetic myocardium would open interesting therapeutic perspectives.
A hallmark of type II diabetes is the dyslipidemia, with increased circulating concentrations of free and lipoprotein-bound fatty acids, which is certainly one culprit of the dysregulation of myocardial glucose transport. Chronic exposure of cardiomyocytes to free fatty acids (FFA) [3, 47] or to triglyceride-rich lipoproteins [33] results in marked inhibition of basal, insulin-stimulated, and metabolic stress-stimulated glucose uptake. The mechanisms involved in the reduction of metabolic stress-stimulated glucose transport by FFA exposure involve inactivation of the focal adhesion kinase [51] and chronic activation of protein kinase C δ [52].
5-Aminoimidazole-4-carboxamide ribonucleoside (AICAR) is an adenosine analog that is taken up by cells and phosphorylated into the AMP mimetics 5-aminoimidazole-4-carboxamide ribonucleoside monophosphate (ZMP) [9]; thus, AICAR activates AMPK independently of cellular metabolic stress, unlike biguanides. Therefore, AICAR-derived molecules have potential as treatment of type II diabetes [10, 16]. Bertrand et al. showed that AMPK activation with biguanides could improve glucose transport in cardiomyocytes that had been rendered resistant to insulin but not to metabolic stress [5]. In this study, we determined whether chronic treatment with low doses of AICAR could improve metabolic stress-stimulated glucose transport in cardiomyocytes exposed to FFA, in an effort to model in vitro the in vivo situation of type II diabetes treated with low-grade chronic AMPK activation.
Material and methods
Rat cardiomyocytes culture
Male Sprague Dawley rats (100–200 g) obtained from Janvier Labs (France) were euthanized by an intraperitoneal injection of pentobarbital (150 mg/kg) and hearts harvested under deep coma. Cardiomyocytes were isolated as previously described [2] by retrograde perfusion of the hearts with collagenase (type II; Worthington; 120 IU/ml) and hyaluronidase (1% w/v) [8, 14]. Cardiomyocytes were separated from non-myocyte cardiac cells by preplating the whole cell suspension for 90 min on untreated plastic, to which non-myocyte cells, but not cardiomyocytes, readily adhere. Cardiomyocytes were plated in M199 medium containing 5.5 mM glucose supplemented with 20 mM creatine, 100 μM cytosine-β-d-arabinofuranoside, 100 nM 9-cis retinoic acid, and 20% fetal calf serum (FCS). Dishes were previously coated with 0.1% gelatin for 4 h and incubated overnight with complete culture medium. For confocal microscopy, cardiomyocytes were plated on laminin-coated glass coverslips; for extracellular flux measurements, SeaHorse V7 plates were also coated with laminin. Free fatty acids (FFA) consisted of a 1:1 mix of palmitate (C16:0) and oleate (C18:1 n-9) bound to bovine serum albumin (BSA), at a final total concentration of 0.4 mM. FFA or AICAR were added at the time of plating. The culture medium was renewed every 2–3 days, and subsequent analyses were performed on day 7. At this time point, control cardiomyocytes display a well-differentiated phenotype with stable insulin responsiveness [39].
Metabolic measurements
Glucose transport was estimated by measuring 2-deoxyglucose (2-DG) uptake, as previously described [2, 31]. Briefly, cardiomyocytes were incubated in M199 containing 10 nM [2,6-3H]-2-DG (ANAWA) (1–2 μCi/ml) and 5.5 mM cold glucose at 37 °C for 1 h, in the presence or absence of glucose transport agonists. Glucose transport agonists used were insulin (10−6 M) or oligomycin (10−6 M) to induce metabolic stress. 2-DG uptake was stopped by three washes with ice-cold PBS before lysis in 1 ml 0.1 M NaOH. Two 20-μl aliquots were taken for protein content determination and the remaining NaOH lysate assayed for radioactivity in a TriCARB 1900 TR liquid scintillation analyzer (Packard).
Glycolytic rates were estimated from the detritiation of [5-3H]-glucose [48]. Cardiomyocytes were incubated in M199 containing 10 nM [5-3H]-glucose (ANAWA) (1–2 μCi/ml) and 5.5 mM cold glucose at 37 °C for 1 h, in the presence or absence of glucose transport agonists. At the end of the incubation period, the incubation medium was retrieved, immediately diluted three times with ice-cold water, and 3H2O was separated from [5-3H]-glucose by anion exchange chromatography in Dowex 1 × 4 B4O72−. 3H2O eluted from the Dowex column was counted by liquid scintillation.
Palmitate oxidation was estimated based on the rate of transfer of 3H from [9,10-3H]palmitate to 3H2O [28]. For measurement of palmitate oxidation, cardiomyocytes were incubated for 60 min in medium containing palmitate (0.05 mM), oleate (0.05 mM), and 1 μCi/ml [9,10-3H]palmitate complexed to bovine serum albumin (0.2 mM). At the end of the incubation period, the incubation medium was retrieved, immediately diluted three times with ice-cold water, and 3H2O was separated from [9,10-3H]palmitate by anion exchange chromatography in Dowex 1 × 4 OH−. 3H2O eluted from the Dowex column was counted by liquid scintillation. Cardiomyocytes were washed twice with ice-cold PBS, dissolved in 0.1 M NaOH. Twenty-microliter aliquots were taken for protein content determination and the remaining NaOH lysate assayed for radioactivity by liquid scintillation. Palmitate uptake was estimated from the sum of 3H label transferred to 3H2O and 3H label remaining in the cardiomyocytes.
Oxygen consumption rates were measured in a SeaHorse XFe24 extracellular flux analyzer, following the protocol developed by Readnower et al. [38]. The medium used was unbuffered DMEM (Sigma no. D5030) containing 1 mM pyruvate, 4 mM l-glutamine, and 5 mM glucose.
Preparation of cytosol and membrane fractions
Cytosol and membrane fractions of cultured cardiomyocytes were obtained as previously described [53]. Cardiomyocytes were washed in ice-cold PBS and scraped in buffer A containing 20 mM Tris-HCl pH 7.5, 2.5 mM EGTA, 1 mM EDTA, 100 mM NaF, 2 mM dithiothreitol, and Halt protease and phosphatase inhibitor cocktail. The suspension was sonicated with four 5-s bursts on ice and then centrifuged at 1500×g for 10 min. The supernatant was then ultracentrifuged at 100,000×g for 45 min at 4 °C. The pellet containing the membrane fraction was solubilized in buffer A containing 1% Triton X-100, sonicated, and centrifuged at 15,000×g for 15 min at 4 °C to retain the supernatant.
Immunoblot analysis
Following stimulation with insulin or oligomycin, incubations were terminated by three washes in ice-cold PBS before solubilizing cells in 200 μl lysis buffer containing 150 mM NaCl, 50 mM Tris-HCl (pH 7.5), 1 mM EDTA, 0.5% sodium deoxycholate, 1% Igepal CA 630, Halt protease, and phosphatase inhibitor Cocktail (Pierce, Thermo Scientific). Proteins (30 μg) from each sample were separated on SDS-PAGE gels and transferred onto polyvinylidene difluoride membranes. Primary antibodies used are listed in Table 1. Secondary anti-mouse IgG (115-035-146) and anti-rabbit IgG (111-035-003) HRP-conjugated antibodies were from Jackson ImmunoResearch. Densitometric analysis of chemiluminescent signals captured with a LAS-4000 Luminescent Image Analyzer (Fujifilm) was performed using the ImageJ software (National Institutes of Health, http://rsb.info.nih.gov/ij). For each separate membrane, the data were normalized such that the highest intensity, regardless of treatment, was equal to one.
Confocal microscopy
For confocal fluorescent microscopy, cardiomyocytes cultured on laminin-coated glass coverslips were washed with ice-cold PBS and fixed with 4 mM paraformaldehyde in PBS for 20 min at room temperature. Fixation was quenched with 200 mM glycine in PBS and cardiomyocytes permeabilized with 0.3% Triton X-100 in PBS for 3 min. Non-specific dye or antibody binding was reduced by preincubation with 3% BSA and 0.1% Tween-20 in PBS. Neutral lipids were stained with 2.5 μg/ml Bodipy 493/503 for 30 min [19]; F-actin counterstaining was obtained with AlexaFluor 543-labeled phalloidin (2 U/ml).
For cytoskeleton imaging, fixed and permeabilized cardiomyocytes were incubated overnight at 4 °C with a mouse α-actinin antibody and a rabbit α-tubulin antibody (see Table 1), followed by secondary antibodies AlexaFluor 488-labeled F(ab′)2 goat anti-rabbit IgG (Invitrogen A11070) and AlexaFluor 633-labeled F(ab′)2 goat anti-mouse IgG (Invitrogen A21053); F-actin counterstaining was obtained with AlexaFluor 543-labeled phalloidin (2 U/ml).
Following washes with PBS and H2O, coverslips were mounted on glass slides with ProLong Diamond antifade containing DAPI for DNA staining. Cardiomyocytes were examined with a Leica SP5 (Fig. 5) or a Zeiss LSM800 (Fig. 8) confocal microscope, using a ×63 oil immersion objective. One-micrometer-thick confocal slices were acquired throughout the thickness of the cardiomyocytes and Z-stack projections obtained with the ImageJ software in maximum intensity projection mode. Image luminosity and contrast were digitally enhanced, taking care of applying the same linear adjustments to images from different experimental groups [40].
Statistics
Data are presented as mean ± SD obtained from replicated experiments. Data were compared by one-way or two-way ANOVA (Prism 7, GraphPad Software) followed by post hoc testing for false discovery rates by the method of Benjamini and Yekutieli [4]. ANOVA results are indicated with p values in the text of the “Results” section. Post hoc testing indicated a positive discovery when the false discovery rate q was < 0.05. Throughout the article, the following symbols are used for positive discoveries (q values): * indicates a significant effect of insulin or oligomycin stimulation as compared with unstimulated cardiomyocytes having received the same chronic treatment; # indicates a significant effect of chronic FFA exposure, as compared with cardiomyocytes not exposed to FFA undergoing the same acute stimulation; and § indicates a significant effect of chronic AICAR exposure (but with the same exposure—or absence thereof—to FFA), as compared with cardiomyocytes not exposed to AICAR undergoing the same acute stimulation.
Results
Effects of chronic AICAR treatment in control and FFA-exposed cardiomyocytes on glucose metabolism
In cultured primary cardiomyocytes, both insulin and oligomycin acutely stimulated glucose uptake, 3- and 3.4-fold, respectively (Fig. 1a). As we previously reported [3, 51, 52], chronic (7 days) exposure of primary cardiomyocytes to 0.4 mM FFA markedly reduced basal and stimulated glucose uptake. Remarkably, chronic treatment of control cardiomyocytes with 0.2 mM AICAR abolished insulin-stimulated glucose uptake and reduced oligomycin-stimulated glucose uptake. On the other hand, AICAR treatment significantly improved oligomycin-stimulated glucose uptake in FFA-exposed cardiomyocytes, with non-significant trends towards amelioration of basal and insulin-stimulated glucose uptake; thus, chronic AICAR treatment essentially nullified the effects of FFA on oligomycin-stimulated glucose uptake in cardiomyocytes.
Chronic AICAR treatment improves glucose metabolism in cardiomyocytes exposed to FFA. Cardiomyocytes were cultured for 7 days in the presence (FFA) or absence (BSA) of 0.4 mM free fatty acids concomitantly with 0.2 mM AICAR or its vehicle. Glucose uptake (a) or glycolysis (b) was measured during 1 h in the presence of 10−6 M insulin or 10−6 M oligomycin following chronic treatment with FFA ± AICAR. c Expression of the glucose transporters GLUT1 and GLUT4 relative to that of α-actinin, expressed in arbitrary units. d Representative Western blots of glucose transporters GLUT1 and GLUT4 expression. Results are mean ± SD of the number of separate experiments indicated at the foot of each column. * : q < 0.05 for the effect of insulin or oligomycin. # : q < 0.05 for the effect of FFA. § : q < 0.05 for the effect of AICAR
The variations of glycolytic activity were parallel to those on glucose uptake (Fig. 1b), although with glycolytic rates consistently lower than the rates of glucose uptake. Both insulin and oligomycin stimulated glycolysis in control cardiomyocytes, albeit to a relatively smaller extent than glucose uptake (1.7-fold). FFA reduced basal and stimulated glycolysis, while concomitant treatment with AICAR improved insulin-stimulated and almost completely restored oligomycin-stimulated glycolysis.
Glucose uptake by cardiomyocytes is mediated by two glucose transporters of the GLUT family, GLUT1 and GLUT4. We previously showed using the GLUT4-specific inhibitor indinavir that about 40% of basal glucose uptake and 80% of insulin- or oligomycin-stimulated glucose uptake were GLUT4-mediated in control cultured cardiomyocytes in our model [52]. The expression of neither GLUT1 nor GLUT4 was significantly affected by the culture conditions, with the exception of AICAR significantly restoring expression of GLUT1, which was blunted by exposure to FFA (q = 0.074) (Fig. 1c, d).
Effects of chronic AICAR treatment in control and FFA-exposed cardiomyocytes on AMPK signaling
As both AICAR, chronically in these settings, and oligomycin, acutely, are expected to act through activation of the AMPK complex, we examined AMPK signaling in cardiomyocytes chronically exposed either AICAR, FFA, or both. Phosphorylation of the AMPKα subunit on T172 is classically taken as indicative of AMPK activation [18]; indeed, in control cardiomyocytes, inhibition of mitochondrial ATP synthase with oligomycin resulted in robust phosphorylation of T172-AMPKα (Fig. 2a). A similar effect was observed in FFA-exposed cardiomyocytes, without any difference in T172-AMPKα phosphorylation brought about by FFA exposure. Quite surprisingly though, phosphoT172-AMPKα was much reduced, to the point of being almost undetectable in some experiments, in cardiomyocytes exposed to AICAR, be it in the presence or not of FFA, even after stimulation with oligomycin. This was not caused by downregulation of global AMPK expression, as expression of the AMPKα subunit was slightly but significantly increased by AICAR treatment, both in the presence (q = 0.0152) or absence of FFA (q = 0.0004).
AMPK signaling in cardiomyocytes exposed to FFA and AICAR. a–e Cardiomyocytes were cultured for 7 days in the presence (FFA) or absence (BSA) of 0.4 mM free fatty acids concomitantly with 0.2 mM AICAR or its vehicle. Cardiomyocytes were then stimulated for 10 min with 10−6 M insulin or for 20 min with 10−6 M oligomycin. Left panels: quantitative analysis of the phosphorylation states of AMPKα (on T172, a; on S485, f); acetyl-CoA carboxylase (ACC; on S79, b) and raptor (on S792, c). Results are mean ± SD of the number of separate experiments indicated at the foot of each column. * : q < 0.05 for the effect of insulin or oligomycin. # : q < 0.05 for the effect of FFA. § : q < 0.05 for the effect of AICAR. Right panels: representative Western blots for each phosphorylation site. d, e Correlation between phosphorylation of raptor (phosphoS792) or AMPK (phosphoT172) and glucose uptake. Squares, BSA; triangles, FFA; circles, FFA + AICAR; white symbols, no stimulation; black symbols, oligomycin stimulation. Insulin data points were omitted from this analysis. g AMPK activation in freshly isolated cardiomyocytes stimulated with 0.2 mM AICAR or 10−6 M oligomycin for 5–60 min; Western blots representative of four separate experiments
To further evaluate the activity of the AMPK complex, we assessed the phosphorylation of two of its known substrates, acetyl-CoA carboxylase [34] (ACC; Fig. 2b) and raptor [17] (Fig. 2c). There was a trend across all four culture conditions for phosphoS79-ACC to be higher in oligomycin-stimulated than in insulin-stimulated cardiomyocytes (p = 0.0064 by two-way ANOVA). Chronic AICAR treatment, either in control (p = 0.008) or in FFA-exposed cardiomyocytes (p = 0.0069), increased phosphorylation of S79-ACC, consistent with a possible activation of AMPK by AICAR. FFA had no effect on phosphorylation of S79-ACC. Neither AICAR nor FFA influenced global expression of ACC. These results are consistent with oligomycin- or AICAR-activated AMPK phosphorylating ACC [34] and insulin promoting dephosphorylation of ACC [55]; the sensitivity of S79-ACC phosphorylation as a readout of AMPK activity in cultured cardiomyocytes appeared however to be rather low.
Acute stimulation with oligomycin induced the phosphorylation of raptor on S792 in control cardiomyocytes (q = 0.019); curiously, this effect was lost in cardiomyocytes exposed to AICAR only. In cardiomyocytes exposed to FFA, phosphoS792-raptor was reduced overall (p = 0.0001), but a trend towards an increase with oligomycin remained. In cardiomyocytes exposed to both FFA and AICAR, the control pattern of S792 phosphorylation was restored (p = 0.0007 vs. FFA only). Neither AICAR nor FFA influenced global expression of raptor.
Thus, phosphoS792-raptor taken as a readout of AMPK activity correlated better with glucose uptake in the various culture and stimulation conditions (r2 = 0.797; p = 0.0028; Fig. 2d) than phosphoT172-AMPKα did (r2 = 0.072; p = 0.52; Fig. 2e); data with insulin stimulation were omitted from this analysis as they are not pertaining to AMPK-mediated stimulation of glucose uptake.
Because of the apparent dissociation between T172-AMPKα phosphorylation and glucose uptake in conditions of metabolic stress after exposure to FFA ± AICAR, we considered whether phosphorylation of an inhibitory site on AMPKα [21] could explain some of these discrepancies (Fig. 2f). As previously described, insulin induced the phosphorylation of S485-AMPKα and so did oligomycin-induced metabolic stress. Notably however, these effects were not observed in cardiomyocytes exposed to AICAR alone. The addition of AICAR significantly increased phosphorylation of S485-AMPKα, both in the presence (p = 0.0097) or absence (p < 0.001) of FFA. Culture of cardiomyocytes in the presence of FFA tended to increase phosphorylation of S485-AMPKα (p = 0.051). Therefore, S485-AMPKα phosphorylation does not correlate with glucose uptake either.
In cultured cardiomyocytes, we observed that 1 h of incubation with 0.2 mM AICAR resulted in a slight increase in T172-AMPKα phosphorylation (207 ± 153% of basal; mean ± SD, n = 4, q = 0.24) of AMPK, much lesser than that achieved by oligomycin exposure (732 ± 305% of basal; mean ± SD, n = 4, q = 0.0015; Fig. 2g); phosphorylation of raptor on S792 was not increased (data not shown).
To determine whether stimulation of glucose uptake by oligomycin under chronic FFA + AICAR was actually AMPK-mediated, we measured glucose uptake and raptor phosphorylation in the presence of the AMPK inhibitor compound C (CC) [56]. CC present acutely during incubation with oligomycin prevented the stimulation of glucose uptake both in control cardiomyocytes, as expected, and in cardiomyocytes exposed to chronic FFA + AICAR (Fig. 3a). Similarly, the phosphorylation of raptor on S792 was markedly diminished in the presence of CC (Fig. 3b).
AMPK-dependence of glucose uptake. Cardiomyocytes were cultured for 7 days in medium containing BSA or 0.4 mM free fatty acids ± 0.2 mM AICAR. Glucose uptake (a) or phosphorylation of raptor on S792 (b) was measured during 1 h in the presence or absence of 10−6 M oligomycin and 10−5 M compound C (CC) following chronic treatment with BSA or FFA + AICAR. DMSO is the vehicle of CC. Results are mean ± SD of the number of separate experiments indicated at the foot of each column. * : q < 0.05 for the effect of oligomycin. # : q < 0.05 for the effect of CC. c Representative Western blots of phosphorylated and total raptor
Differential localization of activated AMPK, thereby targeting different substrates, could also potentially explain the discrepancies between phosphoT172-AMPKα, phosphorylation of AMPK substrates, and glucose uptake. To address this question, we first performed immunofluorescence studies of phosphoT172-AMPKα in ex vivo cardiomyocytes to validate the antibody used for immunolabeling. As shown in Fig. 4a, stimulation of ex vivo cardiomyocytes with 1 μM oligomycin for 30′ resulted in increased immunolabeling of phosphoT172-AMPKα, with a distinct striated and nuclear distribution, thus matching findings by other authors who studied the subcellular distribution of AMPKγ in cardiomyocytes [36]. In cultured control cardiomyocytes stimulated with oligomycin, this striated and nuclear pattern of phosphoT172-AMPKα subcellular distribution was maintained, notwithstanding the extensive cytoskeletal remodeling taking place during the 7-day culture period (Fig. 4b). In contrast in both FFA- and FFA + AICAR-exposed cardiomyocytes, the cytoplasmic distribution of phosphoT172-AMPKα appeared to be more diffuse and less intense, perhaps in relation with the disorganization of the cytoskeleton taking place in these culture conditions (see Fig. 8); nuclear distribution of phosphoT172-AMPKα remained prominent.
Active AMPK localization in cardiomyocytes exposed to FFA and AICAR. a Freshly isolated cardiomyocytes were left quiescent or challenged for 30 min with 10−6 M oligomycin, fixed, permeabilized, and stained with an AlexaFluor555-conjugated phosphoT172 AMPKα antibody (red); counterstaining for F-actin (green) was obtained with phalloidin and for DNA (blue) with DAPI. The phosphoT172 AMPKα antibody was omitted for the negative control. b Cardiomyocytes were cultured for 7 days in medium containing BSA or 0.4 mM free fatty acids (FFA) ± 0.2 mM AICAR. Cardiomyocytes were then stimulated for 30 min with 10−6 M oligomycin and stained as above. Scale bar 20 μM
Effects of chronic AICAR treatment in FFA-exposed cardiomyocytes on lipid metabolism
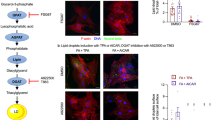
In previous works, we obtained indirect evidence that some by-product(s) of fatty acid oxidation (FAO) could play a role in the reduction of oligomycin-stimulated glucose uptake [3], whereas funneling of fatty acids to triglycerides was associated with preservation of oligomycin-stimulated glucose uptake [52]. We therefore examined fatty acid metabolism in cardiomyocytes exposed to FFA ± AICAR (Fig. 5). Palmitate uptake and oxidation were both increased in cardiomyocytes exposed to FFA, as was to be expected, as fatty acids stimulate expression of proteins of their own import and oxidation [50]. Addition of AICAR to FFA during the 7-day culture period did not alter palmitate uptake but reduced palmitate oxidation down to control levels. Thus, fractional palmitate oxidation, i.e., the fraction of palmitate taken up that is oxidized, was significantly increased in cardiomyocytes exposed to FFA only and reduced in cardiomyocytes exposed to both FFA and AICAR, suggesting a different intracellular fate of fatty acids taken up under AICAR. One possibility was that fatty acids were redirected towards storage in neutral lipids, as occurs in a similar situation of restoration of glucose transport by chronic exposure to a phorbol ester [52]. Indeed, we observed that exposure of cardiomyocytes to FFA + AICAR induced a marked biogenesis of lipid droplets (Fig. 5d). Both the area occupied by lipid droplets (Fig. 5e) and the number of lipid droplets by square millimeter of cell area (Fig. 5f) were significantly increased in cardiomyocytes exposed to FFA + AICAR as compared to FFA only, where very few lipid droplets were visible altogether.
Effect of chronic AICAR on fatty acid metabolism. Cardiomyocytes were cultured for 7 days in medium containing BSA or 0.4 mM free fatty acids (FFA) ± 0.2 mM AICAR. a Palmitate uptake was estimated from the sum of palmitate oxidation and 3H label remaining in the cardiomyocytes. b Palmitate oxidation was estimated from the rate of transfer of 3H from [9,10-3H]palmitate to 3H2O. c Palmitate oxidation expressed as a percentage of palmitate uptake. d Fluorescent imaging of lipid droplets. Green, neutral lipids; red, F-actin; blue, DNA. Scale bar 20 μm. In the negative control, the neutral lipid label (Bodipy 493/503) has been omitted while staining cardiomyocytes with numerous lipid droplets. Images are from a representative experiment. e Percentage of cell surface area labeled as neutral lipids. Results are mean ± SD. f Number of lipid droplets per square millimeter of cell surface area. For both e and f, 12 microscopic frames per condition over 3 separate experiments were analyzed. # : q < 0.05 for the effect of FFA. § : q < 0.05 for the effect of AICAR
Chronic AICAR exposure could reduce mitochondrial activity, which would then explain the observed decrease in fatty acid oxidation. If this were the case, the increase in glucose uptake could be simply due to the inhibition of both glucose and fatty acid oxidation, anaerobic glycolysis remaining the sole way to produce energy. To evaluate this possibility, we assessed basal and maximal mitochondrial activity by monitoring O2 consumption rates (OCR) in the presence of 1 mM pyruvate and 5 mM glucose. Mitochondrial OCR were obtained by subtracting OCR measured in the presence of 10−5 M antimycin A [38]. Both the basal and the maximal OCR, induced by the mitochondrial uncoupling agent carbonyl cyanide-p-trifluoromethoxyphenylhydrazone (FCCP), were reduced in cardiomyocytes chronically exposed to FFA (Fig. 6); AICAR slightly but not significantly improved basal and maximal mitochondrial OCR. Thus, the increased glucose uptake and glycolysis in cardiomyocytes exposed to FFA + AICAR cannot be explained by a further impairment of mitochondrial activity.
AICAR does not alter mitochondrial activity in cardiomyocytes exposed to FFA. Cardiomyocytes were cultured for 7 days in medium containing BSA or 0.4 mM free fatty acids (FFA) ± 0.2 mM AICAR. Oxygen consumption rates (OCR) were measured in an extracellular flux analyzer after sequential addition of 10−6 M oligomycin, 2 × 10−6 M FCCP, and 10−5 M antimycin A to unbuffered DMEM medium containing 1 mM pyruvate and 5 mM glucose. a Time-course of one representative experiment; 70 indicates the total duration of the experiment, in minutes. Results are mean ± SD of six to seven wells. b Basal and FCCP-induced mitochondrial OCR. Results are mean ± SD of four separate experiments. # : q < 0.05 for the effect of FFA
Effects of chronic AICAR treatment in FFA-exposed cardiomyocytes on PKC expression and signaling
Up to this point, there are strong similarities between the effects of AICAR and tetradecanoyl phorbol acetate (TPA) [52] to improve glucose metabolism and redirect fatty acids to neutral storage in cardiomyocytes exposed to FFA. This prompted us to investigate whether such similarities would extend to protein kinase C signaling, which we showed was markedly altered by chronic TPA treatment. Similar to chronic TPA treatment but to a lesser extent, chronic AICAR treatment, either in absence (p = 0.0069 by two-way ANOVA) or in presence of FFA (p = 0.0004), resulted in a reduction of phosphorylation of PKC isoforms on residues homologous to T410 in PKCζ (Fig. 7a). This result indicated a global decrease in the availability of mature PKC across multiple isoforms (α, β, γ, δ, ε, η, θ, ι). In our previous study, we observed that PKCα, δ, and ε were strongly downregulated upon TPA treatment and that PKCδ was recruited to membrane compartments by chronic FFA exposure, indicating a role for PKCδ activation in the impairment of glucose uptake [52]. In contrast, we found no alterations of PKCα, δ, or ε expression in response to AICAR (Fig. 7b), and PKCδ translocation to the membrane fraction was not prevented by AICAR (Fig. 7c).
AICAR reduces activation of some PKC but not translocation of PKCα, δ, or ε. Cardiomyocytes were cultured for 7 days in medium containing BSA or 0.4 mM free fatty acids (FFA) ± 0.2 mM AICAR. a Cardiomyocytes were then stimulated for 10 min with 10−6 M insulin or for 20 min with 10−6 M oligomycin and phosphorylation of PKCs on the site analogous to T410 on PKCζ (indicative of activation or preactivation) assessed by Western blot. α-Actinin served as a loading control. b Expression of PKCα, PKCδ, and PKCε in whole cell extracts was assessed by Western blot, with α-actinin serving as a loading control. c Cardiomyocytes were separated into a cytosol and a membrane fractions and the density of PKC isoforms in the membranes fractions evaluated, with connexin 43 (Cx43) as a loading control for membrane fraction proteins. Results are mean ± SD of the number of separate experiments indicated at the foot of each column. : q < 0.05 for the effect of FFA. § : q < 0.05 for the effect of AICAR. Right panels: representative Western blots
Effects of chronic AICAR treatment in FFA-exposed cardiomyocytes on the cytoskeleton
Both microtubules [31] and actin filaments [46] have been shown to be important for glucose transport; we previously observed that cytoskeletal organization was disrupted in cardiomyocytes exposed to FFA [3, 52] but restored in response to the TPA treatment resulting in restoration of glucose uptake [52]. We therefore investigated whether concomitant treatment with AICAR could also improve the cytoskeletal organization in cardiomyocytes exposed to FFA (Fig. 8). As previously described [3], exposure to FFA for 7 days resulted in disorganization of the microtubular and sarcomeric systems, evidenced by immunofluorescent labeling of α-tubulin and α-actinin and F-actin, respectively. Concomitant AICAR treatment did not significantly ameliorate either component of cytoskeletal organization. In fact, treatment with AICAR alone resulted in disorganization of the cytoskeleton.
AICAR does not improve cytoskeleton disorganization. Cardiomyocytes were cultured for 7 days in medium containing BSA or 0.4 mM free fatty acids (FFA) ± 0.2 mM AICAR. Cardiomyocytes were then fixed, permeabilized, and stained with antibodies against sarcomeric α-actinin (magenta) and α-tubulin (green). F-actin was labeled with phalloidin (red). DNA counterstaining (blue) was obtained with DAPI. Scale bar 20 μm. Images are representative of ten microscopic frames over two experiments for each condition
Discussion
Regulation of glucose metabolism
The first salient finding of this study is the protection to a large extent of insulin- and oligomycin-stimulated glucose transport and glycolysis in cardiomyocytes treated with AICAR in addition to exposure to FFA, as compared to the marked reduction in basal and stimulated glucose transport in cardiomyocytes exposed to FFA alone [3]. We used a supraphysiological concentration of insulin (10−6 M) in these experiments to focus our investigations on maximal insulin responsiveness, not insulin sensitiveness, as we previously observed that FFA exposure reduced the former, not the latter, parameter [3].
Inhibition of glucose uptake by an AMPK agonist, as observed in cardiomyocytes under treatment with AICAR alone, may seem paradoxical; it has however been previously reported, albeit not in a chronic exposure setting. Ségalen et al. reported that stimulation of cardiac myocytes with 2 mM AICAR for 40 min reduced basal and insulin-stimulated glucose uptake [44]; this effect was found to be AMPK-independent and explained by intracellular acidification. Also, the chronic effects of AICAR to reduce insulin-stimulated glucose transport in control cardiomyocytes but improve oligomycin-stimulated glucose transport in FFA-exposed cardiomyocytes are akin to the chronic effects of PPARδ stimulation on glucose transport in cardiomyocytes [3], which would concur with the finding that AICAR could stimulate PPARδ-dependent transcription [32]. However, inhibition of PPARδ with GSK3787 did not alter glucose uptake in cardiomyocytes exposed to FFA + AICAR (data not shown). Finally, the cytoskeletal disorganization brought about by chronic treatment with AICAR alone (Fig. 8) may have contributed to the reduction of glucose uptake.
One important point made by Fig. 1a is that improvement of glucose transport by AICAR in the presence of FFA is not related to a general stimulation of glucose transport regardless of the presence or absence of FFA. It is therefore pertaining to mechanisms existing only in the presence of FFA.
The slightly improved expression of the glucose transporters GLUT1 and GLUT4 could certainly contribute to the amelioration of glucose uptake and glycolysis in cardiomyocytes exposed to FFA + AICAR. One should however not overestimate the importance of GLUT expression in determining glucose uptake, as Kaczmarczyk et al. have shown that above a quite low threshold of expression, glucose uptake in murine myocardium was independent of GLUT4 expression [23].
AMPK signaling
Examining AMPK signaling in relationship with glucose transport in cardiomyocytes exposed to AICAR, FFA, or both together, we made the puzzling observations that phosphorylation of AMPKα on T172, a classical marker of AMPK activation, was very low, to the point of being almost undetectable in some experiments. This unexpected effect was observed with two distinct antibodies (listed in Table 1), thus is unlikely to be an artifact. The antibodies used to detect phosphoT172-AMPKα and total AMPKα were capable of detecting both α1 and α2 isoforms; therefore, the disappearance of phosphoT172-AMPKα was unlikely to be due to a switch in isoform expression. It remains possible that the expression of β or γ subunits of AMPK was massively reduced under AICAR treatment, thereby preventing the assembly of functional AMPK complexes. This appears to be unlikely, as expression of all three subunits is required for the stability of the AMPK complex; therefore, massively reduced expression of β or γ subunits would induce degradation of the normally expressed α subunit [11]. If this were nevertheless the case, it would mean that the stimulation of glucose uptake by oligomycin observed in cardiomyocytes exposed to FFA + AICAR was not due to AMPK activation but to some other mechanism. Luiken et al. reported that oligomycin activated protein kinase D (PKD, also known as PKCμ) in an AMPK-independent manner and that activated PKD participated in the stimulation of glucose uptake by oligomycin in cardiomyocytes [27]. It is thus possible that the remaining stimulation of glucose uptake by oligomycin in condition with chronic AICAR exposure and apparent deactivation of AMPK was entirely due to PKD activation. On the other hand, chronic AICAR treatment might obscure or prevent AMPKα phosphorylation while maintaining AMPK activity by allosteric activation induced by accumulation of the AICAR metabolite ZMP. However, a recent study of AMPK activation concluded that T172 phosphorylation was required for AMPK activity in a cellular context, even though it could be dispensable for allosteric activation in cell-free extracts [54].
In order to differently assess the activity of AMPK, we determined the phosphorylation status of two of its known substrates, acetyl-CoA carboxylase (ACC) [34] and raptor [17]. Phosphorylation of ACC on S79 proved to be a rather insensitive readout of AMPK activation in this model; however, the statistically significant increased overall phosphorylation of S79-ACC in response to AICAR, either in the presence or absence of FFA, suggested that AMPK was being activated by chronic AICAR exposure despite the disappearance of T172-AMPKα phosphorylation.
On the other hand, phosphorylation of raptor on S792 displayed a pattern that was consistent with a reduction of AMPK activity in cardiomyocytes exposed to FFA and an improvement of AMPK activity in cardiomyocytes exposed to FFA and AICAR together. These data again argue for AMPK being activated by chronic AICAR exposure despite the disappearance of T172-AMPKα phosphorylation. Furthermore, phosphoS792-raptor data suggest that AMPK activity is low in cardiomyocytes exposed to FFA alone, despite levels of T172-AMPKα phosphorylation similar to those in control cardiomyocytes. Inhibition of AMPK activity has indeed been observed in neonatal rat cardiac myocytes [20] or mouse myotubes [43] following long (16–20 h) incubation with the fatty acid palmitate but, unlike in our study, was associated with reduced T172-AMPKα phosphorylation and prevented by coincubation with oleate.
The pattern of S792-raptor phosphorylation across the different cardiomyocyte treatments matched that of glucose uptake much better than that of T172-AMPKα did. These data should however not be interpreted as indicating that inhibition of mTORC1 via raptor phosphorylation stimulates glucose uptake; indeed, Ginion et al. have shown that mTORC1 inhibition had no effect on glucose transport in adult cardiomyocytes [15]. If anything, inhibition of mTORC1 activity has rather been associated with a reduction of glucose transport in myoblasts [25] or in adipocytes [35].
Whether AICAR actually induces the phosphorylation of T172-AMPKα and activates AMPK in the myocardium is controversial. While Marsin et al. found no activation of AMPK in the rat heart perfused with 1 mM AICAR [29], Russell et al. observed increased AMPK activity and glucose uptake in rat ventricular papillary muscles incubated with 1 mM AICAR [41]. The reason for these discrepancies is not clear. We observed only a slight increase in T172-AMPKα phosphorylation and no increase in phosphoS792-raptor after stimulation with AICAR for 1 h. Thus, it appears that, at least during short exposure to 0.2 mM AICAR, isolated cardiomyocytes do not take up enough of the compound to sufficiently increase intracellular ZMP concentrations for significant AMPK activation. It remains however possible that longer, chronic administration of AICAR leads to sufficient ZMP accumulation for significant AMPK activation to occur.
To determine whether stimulation of glucose uptake by oligomycin under chronic FFA + AICAR was actually AMPK-mediated, we measured glucose uptake and raptor phosphorylation in the presence of the AMPK inhibitor compound C. Though the specificity of CC is not perfect, these findings strongly suggest that AMPK is actually activated by oligomycin treatment in the FFA + AICAR condition, despite phosphoT172-AMPKα being barely detectable.
Lipid metabolism
These results on lipid metabolism in cardiomyocytes exposed to FFA + AICAR are at odds with the expected effects of AMPK activation, which were that fatty acid oxidation would be increased rather than decreased [6]. On the other hand, these authors exposed cardiomyocytes to AICAR for only 2 h, whereas other investigators observed that a longer exposure of hepatocytes to AICAR (24 h) resulted in a decrease in PPARα transcriptional activity that could explain the reduced fatty acid oxidation [45]. Further to above speculative discussion that some of the effects of chronic AICAR could be due to PPARδ activation, we previously observed that selective PPARδ activation also induced lipid droplets biogenesis to a large extent (unpublished observations).
PKC signaling
We previously observed that chronic exposure to the phorbol ester TPA together with FFA improved FFA-impaired glucose uptake and glycolysis in cardiomyocytes [52], similar to our current findings with AICAR. The similarities between the effects of TPA and AICAR extend to lipid metabolism, with reduced fractional oxidation of fatty acids and increased biogenesis of lipid droplets. Also, both TPA and AICAR reduced the general expression of active or activatable PKC. However, whereas TPA reduced expression of PKCα, δ, and ε and prevented activation of PKCδ, AICAR exerted none of these specific effects. There are three possibilities for the interpretation of these results: (1) the reduction in phosphoT410-PKCζ expression is relevant for restoration of glucose uptake in response to both AICAR and TPA, whereas the translocation of PKCδ is an epiphenomenon. In this case, the identity of the culprit PKC isoform would remain unknown. However, amelioration of glucose uptake with a PKCδ inhibitor [52] speaks against this interpretation. (2) The reduction in phosphoT410-PKCζ is an epiphenomenon in both situations, linked to the changes in the metabolic pattern of fatty acids, and TPA and AICAR act via different mechanisms. Indeed, funneling of fatty acids into neutral storage could reduce the intracellular concentration of diacylglycerols, physiological PKC activators. However, inhibition of lipid droplets biogenesis with diacylglycerol acyl transferase 1 inhibitors did not prevent the reduction in phosphoT410-PKCζ (preliminary data, not shown). (3) Both the reduction in phosphoT410-PKCζ expression and the translocation of PKCδ are relevant for the restoration of glucose uptake; the fact that only the first one occurs in response to AICAR then potentially explains why the restoration of glucose uptake is only partial with AICAR while it is complete with TPA. Speculatively, this would reinforce the idea put forward earlier that the effects of chronic low-dose AICAR might not be solely related to the activity of AMPK.
Cytoskeletal architecture
Integrity and plasticity of the cytoskeleton play a crucial role for the stimulation of glucose transport in cardiomyocytes [31, 46]. In this study, we confirmed the cytoskeletal disarray previously observed in cardiomyocytes exposed to FFA; AICAR co-treatment did not improve the cytoskeletal architecture. This perhaps also partly explains why amelioration of glucose uptake with AICAR in FFA-exposed cardiomyocytes is only partial. It also suggests that the improvement in cytoskeletal organization observed in response to TPA is independent of the effects shared by TPA and AICAR treatments, i.e., fatty acid metabolism and phosphoT410-PKCζ reduction. Dyntar et al. observed myofibrillar disarray in cardiomyocytes exposed to palmitate and linked it to the biosynthesis of ceramides [12]. Promotion of triglyceride synthesis, as occurs under treatment with FFA + AICAR, reduces ceramide biosynthesis [26] and should therefore lead to the preservation of cytoskeletal organization. However, this may have been prevented by the cytoskeletal disorganization effect of AICAR by itself.
About the experimental model
Adult rat cardiomyocytes in long-term primary culture under high FCS conditions, the model used in this study, undergo dedifferentiation and redifferentiation, resulting after 7–8 days in a phenotype with high myofibrillar organization, contractility [13], and a glucose transport response to insulin and metabolic stress almost identical to that observed in freshly isolated cardiomyocytes [31, 39], despite extensive cytoskeletal reorganization leading to the loss of the rod-like shape. In addition, inclusion of 9-cis retinoic acid to the culture medium markedly reduces the extent of transient dedifferentiation and of subsequent hypertrophy [30, 31]. We therefore believe this experimental model to be valid for investigations on the chronic impact of alterations of the extracellular environment on glucose metabolism in cardiomyocytes.
Limitations
Obviously, the main limitation of the present study is that it remains difficult to conclude whether amelioration of glucose metabolism by chronic AICAR co-treatment with FFA exposure is or is not AMPK-mediated. Chronic pharmaceutical inhibition of AMPK activity or AMPK knock-down during AICAR exposure could have resolved this issue, but unfortunately, neither approach proved feasible in our model.
Conclusions
In conclusion (Fig. 9), chronic AICAR treatment of cardiomyocytes restores a normal pattern of substrate metabolism in a context of excessive lipid supply, by redirecting fatty acids to neutral storage. A similar maneuver in vivo in type II diabetes could improve the impaired metabolic stress stimulation of myocardial glucose transport and thus render the diabetic heart less susceptible to ischemic injury.
Summary of main findings and interpretation. In control cardiomyocytes, metabolic stress, as induced by oligomycin and resulting in AMP accumulation, activates AMPK, which stimulates glucose metabolism and phosphorylates raptor. Chronic exposure to free fatty acids (FFA) markedly reduces both AMPK-mediated effects. Chronic AICAR treatment in addition to FFA channels FFA to lipid droplets (LD), reduces FFA oxidation, and restores AMPK-mediated effects
References
Alegria JR, Miller TD, Gibbons RJ, Yi Q-L, Yusuf S (2007) Infarct size, ejection fraction, and mortality in diabetic patients with acute myocardial infarction treated with thrombolytic therapy. Am Heart J 154:743–750. https://doi.org/10.1016/j.ahj.2007.06.020
Asrih M, Pellieux C, Papageorgiou I, Lerch R, Montessuit C (2011) Role of ERK1/2 activation in microtubule stabilization and glucose transport in cardiomyocytes. Am J Physiol Endocrinol Metab 301:E836–E843. https://doi.org/10.1152/ajpendo.00160.2011
Asrih M, Lerch R, Papageorgiou I, Pellieux C, Montessuit C (2012) Differential regulation of stimulated glucose transport by free fatty acids and PPARα or -δ agonists in cardiac myocytes. Am J Physiol Endocrinol Metab 302:E872–E884. https://doi.org/10.1152/ajpendo.00427.2011
Benjamini Y, Yekutieli D (2005) False discovery rate-adjusted multiple confidence intervals for selected parameters. JASA 100:71–81. https://doi.org/10.1198/016214504000001907
Bertrand L, Ginion A, Beauloye C, Hebert AD, Guigas B, Hue L, Vanoverschelde J-L (2006) AMPK activation restores the stimulation of glucose uptake in an in vitro model of insulin-resistant cardiomyocytes via the activation of protein kinase B. Am J Physiol Heart Circ Physiol 291:H239–H250
Chabowski A, Momken I, Coort SL, Calles-Escandon J, Tandon NN, Glatz JF, Luiken JJ, Bonen A (2006) Prolonged AMPK activation increases the expression of fatty acid transporters in cardiac myocytes and perfused hearts. Mol Cell Biochem 288:201–212. https://doi.org/10.1007/s11010-006-9140-8
Clavijo LC, Pinto TL, Kuchulakanti PK, Torguson R, Chu WW, Satler LF, Kent KM, Suddath WO, Pichard AD, Waksman R (2006) Metabolic syndrome in patients with acute myocardial infarction is associated with increased infarct size and in-hospital complications. Cardiovas Revasc Med 7:7–11. https://doi.org/10.1016/j.carrev.2005.10.007
Claycomb WC, Palazzo MC (1980) Culture of the terminally differentiated adult cardiac muscle cell: a light and scanning electron microscope study. Dev Biol 80:466–482. https://doi.org/10.1016/0012-1606(80)90419-4
Corton JM, Gillespie JG, Hawley SA, Hardie DG (1995) 5-Aminoimidazole-4-carboxamide ribonucleoside. A specific method for activating AMP-activated protein kinase in intact cells? Eur J Biochem 229:558–565. https://doi.org/10.1111/j.1432-1033.1995.0558k.x
Coughlan KA, Valentine RJ, Ruderman NB, Saha AK (2014) AMPK activation: a therapeutic target for type 2 diabetes? Diabetes Metab Syndr Obes 7:241–253. https://doi.org/10.2147/DMSO.S43731
Crute BE, Seefeld K, Gamble J, Kemp BE, Witters LA (1998) Functional domains of the α1 catalytic subunit of the AMP-activated protein kinase. J Biol Chem 273:35347–35354. https://doi.org/10.1074/jbc.273.52.35347
Dyntar D, Eppenberger-Eberhardt M, Maedler K, Pruschy M, Eppenberger HM, Spinas GA, Donath MY (2001) Glucose and palmitic acid induce degeneration of myofibrils and modulate apoptosis in rat adult cardiomyocytes. Diabetes 50:2105–2113
Eppenberger HM, Hertig C, Eppenberger-Eberhardt M (1994) Adult rat cardiomyocytes in culture. A model system to study the plasticity of the differentiated cardiac phenotype at the molecular and cellular levels. Trends Cardiovas Med 4:187–193
Eppenberger-Eberhardt M, Flamme I, Kurer V, Eppenberger HM (1990) Reexpression of α-smooth muscle actin isoform in cultured adult rat cardiomyocytes. Dev Biol 139:269–278. https://doi.org/10.1016/0012-1606(90)90296-U
Ginion A, Auquier J, Benton CR, Mouton C, Vanoverschelde J-L, Hue L, Horman S, Beauloye C, Bertrand L (2011) Inhibition of the mTOR/p70S6K pathway is not involved in the insulin-sensitizing effect of AMPK on cardiac glucose uptake. Am J Physiol Heart Circ Physiol 301:H469–H477. https://doi.org/10.1152/ajpheart.00986.2010
Goodman M, Liu Z, Zhu P, Li J (2014) AMPK activators as a drug for diabetes, cancer and cardiovascular disease. Pharm Regul Aff 3:118. https://doi.org/10.4172/2167-7689.1000118
Gwinn DM, Shackelford DB, Egan DF, Mihaylova MM, Mery A, Vasquez DS, Turk BE, Shaw RJ (2008) AMPK phosphorylation of raptor mediates a metabolic checkpoint. Mol Cell 30:214–226. https://doi.org/10.1016/j.molcel.2008.03.003
Hardie DG, Ross FA, Hawley SA (2012) AMPK: a nutrient and energy sensor that maintains energy homeostasis. Nat Rev Mol Cell Biol 13:251–262
Harris L-ALS, Skinner JR, Wolins NE (2013) Imaging of neutral lipids and neutral lipid associated proteins. Methods Cell Biol 116:213–226. https://doi.org/10.1016/b978-0-12-408051-5.00011-5
Hickson-Bick DLM, Buja ML, McMillin JB (2000) Palmitate-mediated alterations in the fatty acid metabolism of rat neonatal cardiac myocytes. J Mol Cell Cardiol 32:511–519
Horman S, Vertommen D, Heath R, Neumann D, Mouton V, Woods A, Schlattner U, Wallimann T, Carling D, Hue L, Rider MH (2006) Insulin antagonizes ischemia-induced Thr172 phosphorylation of AMP-activated protein kinase a-subunits in heart via hierarchical phosphorylation of Ser485/491. J Biol Chem 281:5335–5340
Iozzo P, Chareonthaitawee P, Dutka D, Betteridge DJ, Ferrannini E, Camici PG (2002) Independent association of type 2 diabetes and coronary artery disease with myocardial insulin resistance. Diabetes 51:3020–3024. https://doi.org/10.2337/diabetes.51.10.3020
Kaczmarczyk SJ, Andrikopoulos S, Favaloro J, Domenighetti AA, Dunn A, Ernst M, Grail D, Fodero-Tavoletti M, Huggins CE, Delbridge LMD, Zajac JD, Proietto J (2003) Threshold effects of glucose transporter-4 (GLUT4) deficiency on cardiac glucose uptake and development of hypertrophy. J Mol Endocrinol 31:449–459
Lejay A, Fang F, John R, Van JAD, Barr M, Thaveau F, Chakfe N, Geny B, Scholey JW (2016) Ischemia reperfusion injury, ischemic conditioning and diabetes mellitus. J Mol Cell Cardiol 91:11–22. https://doi.org/10.1016/j.yjmcc.2015.12.020
Liemburg-Apers DC, Wagenaars JAL, Smeitink JAM, Willems PHGM, Koopman WJH (2016) Acute stimulation of glucose influx upon mitoenergetic dysfunction requires LKB1, AMPK, Sirt2 and mTOR–RAPTOR. J Cell Sci 129:4411–4423. https://doi.org/10.1242/jcs.194480
Listenberger LL, Han X, Lewis SE, Cases S, Farese RVJ, Ory DS, Schaffer JE (2003) Triglyceride accumulation protects against fatty acid-induced lipotoxicity. Proc Natl Acad Sci U S A 100:3077–3082
Luiken JJFP, Vertommen D, Coort SLM, Habets DDJ, El Hasnaoui M, Pelsers MML, Viollet B, Bonen A, Hue L, Rider MH, Glatz JFC (2008) Identification of protein kinase D as a novel contraction-activated kinase linked to GLUT4-mediated glucose uptake, independent of AMPK. Cell Signal 20:543–556
Manning NJ, Olpin SE, Pollitt RJ, Webley J (1990) A comparison of [9,10-3H]palmitic and [9,10-3H]myristic acids for the detection of defects of fatty acid oxidation in intact cultured fibroblasts. J Inherit Metab Dis 13:58–68
Marsin A-S, Bertrand L, Rider MH, Deprez J, Beauloye C, Vincent MF, Van den Berghe G, Carling D, Hue L (2000) Phosphorylation and activation of heart PFK-2 by AMPK has a role in the stimulation of glycolysis during ischaemia. Curr Biol 10:1247–1255
Montessuit C, Papageorgiou I, Campos L, Lerch R (2006) Retinoic acids increase expression of GLUT4 in dedifferentiated and hypertrophied cardiac myocytes. Basic Res Cardiol 101:27–35
Montessuit C, Papageorgiou I, Lerch R (2008) Nuclear receptors agonists improve insulin responsiveness in cultured cardiomyocytes through enhanced signaling and preserved cytoskeletal architecture. Endocrinology 149:1064–1074. https://doi.org/10.1210/en.2007-0656
Narkar VA, Downes M, Yu RT, Embler E, Wang Y-X, Banayo E, Mihaylova MM, Nelson MC, Zou Y, Juguilon H, Kang H, Shaw RJ, Evans RM (2008) AMPK and PPARδ agonists are exercise mimetics. Cell 134:405–415. https://doi.org/10.1016/j.cell.2008.06.051
Papageorgiou I, Viglino C, Brulhart-Meynet M-C, James RW, Lerch R, Montessuit C (2016) Impaired stimulation of glucose transport in cardiac myocytes exposed to very low-density lipoproteins. Nutr Metab Cardiovasc Dis 26:614–622. https://doi.org/10.1016/j.numecd.2016.01.010
Park SH, Gammon SR, Knippers JD, Paulsen SR, Rubink DS, Winder WW (2002) Phosphorylation-activity relationships of AMPK and acetyl-CoA carboxylase in muscle. J Appl Physiol 92:2475–2482. https://doi.org/10.1152/japplphysiol.00071.2002
Pereira MJ, Palming J, Rizell M, Aureliano M, Carvalho E, Svensson MK, Eriksson JW (2012) mTOR inhibition with rapamycin causes impaired insulin signalling and glucose uptake in human subcutaneous and omental adipocytes. Mol Cell Endocrinol 355:96–105. https://doi.org/10.1016/j.mce.2012.01.024
Pinter K, Grignani RT, Watkins H, Redwood C (2013) Localisation of AMPK γ subunits in cardiac and skeletal muscles. J Muscle Res Cell Motil 34:369–378. https://doi.org/10.1007/s10974-013-9359-4
Povlsen JA, Løfgren B, Dalgas C, Birkler RID, Johannsen M, Støttrup NB, Bøtker HE (2013) Protection against myocardial ischemia-reperfusion injury at onset of type 2 diabetes in Zucker diabetic fatty rats is associated with altered glucose oxidation. PLoS One 8:e64093. https://doi.org/10.1371/journal.pone.0064093
Readnower RD, Brainard RE, Hill BG, Jones SP (2012) Standardized bioenergetic profiling of adult mouse cardiomyocytes. Physiol Genomics 44:1208–1213. https://doi.org/10.1152/physiolgenomics.00129.2012
Rosenblatt-Velin N, Lerch R, Papageorgiou I, Montessuit C (2004) Insulin resistance in adult cardiomyocytes undergoing dedifferentiation: role of GLUT4 expression and translocation. FASEB J 18:872–874. https://doi.org/10.1096/fj.03-1095fje
Rossner M, Yamada KM (2004) What's in a picture? The temptation of image manipulation. J Cell Biol 166:11–15
Russell RR, Bergeron R, Shulman GI, Young LH (1999) Translocation of myocardial GLUT-4 and increased glucose uptake through activation of AMPK by AICAR. Am J Physiol Heart Circ Physiol 277:H643–H649
Russell RR, Li J, Coven DL, Pypaert M, Zechner C, Palmeri M, Giordano FJ, Mu J, Birnbaum MJ, Young LH (2004) AMP-activated protein kinase mediates ischemic glucose uptake and prevents postischemic cardiac dysfunction, apoptosis, and injury. J Clin Invest 114:495–503. https://doi.org/10.1172/JCI200419297
Salvadó L, Coll T, Gómez-Foix AM, Salmerón E, Barroso E, Palomer X, Vázquez-Carrera M (2013) Oleate prevents saturated-fatty-acid-induced ER stress, inflammation and insulin resistance in skeletal muscle cells through an AMPK-dependent mechanism. Diabetologia 56:1372–1382. https://doi.org/10.1007/s00125-013-2867-3
Ségalen C, Longnus SL, Baetz D, Counillon L, Obberghen EV (2008) 5-Aminoimidazole-4-carboxamide-1-β-d-ribofuranoside reduces glucose uptake via the inhibition of Na+/H+ exchanger 1 in isolated rat ventricular cardiomyocytes. Endocrinology 149:1490–1498. https://doi.org/10.1210/en.2007-1326
Sozio MS, Lu C, Zeng Y, Liangpunsakul S, Crabb DW (2011) Activated AMPK inhibits PPAR-α and PPAR-γ transcriptional activity in hepatoma cells. Am J Physiol Gastrointest Liver Physiol 301:G739–G747. https://doi.org/10.1152/ajpgi.00432.2010
Steinbusch LKM, Wijnen W, Schwenk RW, Coumans WA, Hoebers NTH, Ouwens DM, Diamant M, Bonen A, Glatz JFC, Luiken JJFP (2010) Differential regulation of cardiac glucose and fatty acid uptake by endosomal pH and actin filaments. Am J Physiol Cell Physiol 298:C1549–C1559. https://doi.org/10.1152/ajpcell.00334.2009
Steinbusch LKM, Dirkx E, Hoebers NTH, Roelants V, Foretz M, Viollet B, Diamant M, van Eys G, Ouwens DM, Bertrand L, Glatz JFC, Luiken JJFP (2012) Overexpression of AMP-activated protein kinase or protein kinase D prevents lipid-induced insulin resistance in cardiomyocytes. J Mol Cell Cardiol 55:165–173. https://doi.org/10.1016/j.yjmcc.2012.11.005
TeSlaa T, Teitell MA (2014) Techniques to monitor glycolysis. In: Galluzzi L, Kroemer G (eds) Methods in enzymology, vol 542. Academic Press, Cambridge, pp 91–114. https://doi.org/10.1016/B978-0-12-416618-9.00005-4
Tian R, Abel ED (2001) Responses of GLUT4-deficient hearts to ischemia underscore the importance of glycolysis. Circulation 103:2961–2966. https://doi.org/10.1161/01.CIR.103.24.2961
van der Lee KAJM, Vork MM, De Vries JE, Willemsen PHM, Glatz JFC, Reneman RS, Van der Vusse GJ, Van Bilsen M (2000) Long-chain fatty acid-induced changes in gene expression in neonatal cardiac myocytes. J Lipid Res 41:41–47
Viglino C, Montessuit C (2017) A role for focal adhesion kinase in the stimulation of glucose transport in cardiomyocytes. J Cell Biochem 118:670–677. https://doi.org/10.1002/jcb.25655
Viglino C, Khoramdin B, Praplan G, Montessuit C (2017) Pleiotropic effects of chronic phorbol ester treatment to improve glucose transport in insulin-resistant cardiomyocytes. J Cell Biochem 118:4716–4727. https://doi.org/10.1002/jcb.26139
Wang L, Rolfe M, Proud CG (2003) Ca2+-independent protein kinase C activity is required for α1-adrenergic-receptor-mediated regulation of ribosomal protein S6 kinases in adult cardiomyocytes. Biochem J 373:603–611. https://doi.org/10.1042/bj20030454
Willows R, Sanders MJ, Xiao B, Patel BR, Martin SR, Read J, Wilson JR, Hubbard J, Gamblin SJ, Carling D (2017) Phosphorylation of AMPK by upstream kinases is required for activity in mammalian cells. Biochem J 474:3059–3073. https://doi.org/10.1042/BCJ20170458
Witters LA, Kemp BE (1992) Insulin activation of acetyl-CoA carboxylase accompanied by inhibition of the 5'-AMP-activated protein kinase. J Biol Chem 267:2864–2867
Zhou G, Myers R, Li Y, Chen Y, Shen X, Fenyk-Melody J, Wu M, Ventre J, Doebber T, Fujii N, Musi N, Hirshman MF, Goodyear LJ, Moller DE (2001) Role of AMP-activated protein kinase in mechanism of metformin action. J Clin Invest 108:1167–1174
Funding
This work was made possible by grants from the Swiss National Science Foundation (no. 310030_146537 to CM), the “Fondation Carlos et Elsie de Reuter” (no. 594 to CM), and the “Fondation pour la Recherche sur le Diabète” (to CM).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics statement
All applicable international, national, and/or institutional guidelines for the care and use of animals were followed.
The ethical committee of the Geneva University School of Medicine and the Geneva State Veterinary Office approved the study protocol (authorization no. GE/51/16 and no. GE/217/17), which conforms to the Guide for the Care and Use of Laboratory Animals published by the National Institutes of Health (NIH Publication No. 85-23, revised 1996).
This article does not contain any studies with human participants performed by any of the authors.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Viglino, C., Foglia, B. & Montessuit, C. Chronic AICAR treatment prevents metabolic changes in cardiomyocytes exposed to free fatty acids. Pflugers Arch - Eur J Physiol 471, 1219–1234 (2019). https://doi.org/10.1007/s00424-019-02285-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00424-019-02285-0