Abstract
Ca2+ plays a key role in intracellular signaling and controls various cellular processes such as proliferation, differentiation, cell growth, death, and apoptosis. Aberrant changes in intracellular Ca2+ levels can promote undesired cell proliferation and migration and are therefore associated with certain tumor types. Many research groups have suggested a potential role for voltage-gated Ca2+ channels in the regulation of tumor growth and progression, particularly T-type channels due to their unique biophysical properties. T-type channels are expressed in normal tissues throughout the body and in different types of tumors such as breast carcinoma, retinoblastoma, neuroblastoma, and glioma. It has been demonstrated that increased functional expression of the α1 subunit of T-type channels plays a role in the abnormal proliferation of glioblastoma cells. As such, siRNA-mediated knockdown of the expression of the α1 subunit of T-type channels decreases the proliferation of these cells. Moreover, pharmacological blockade of T-type channels significantly decreases tumor growth. In this review, we focus on the use of T-type channel blockers for the potential treatment of cancers, particularly highly proliferative tumors such as glioblastoma. We conclude that T-type channel blockers such as endostatin can serve as a potential therapeutic tool for tumors whose proliferation depends on increased T-type channel expression.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Control of intracellular Ca2+ [Ca2+]i levels is crucial for orderly cell cycle progression, and this control plays a vital role in the regulation of cell proliferation and growth [13, 37]. Voltage-gated Ca2+ channels (VGCCs) are found in the plasma membrane of many excitable and non-excitable cells [6]. When VGCCs are open, they permit the influx of Ca2+ into the cytoplasm, and these Ca2+ ions act as a secondary messenger and initiates diverse physiological cellular processes [68]. Ten unique α1-subunit genes are categorized into three families (Cav1, CaV2, and CaV3), and they encode low-voltage-activated (LVA) T-type and high-voltage-activated L-, N-, P/Q-, and R-type Ca2+ channels, with distinct biophysical and pharmacological properties [7, 63]. Among these channels, T-type Ca2+ channels (T-type channels) open after small depolarization of the membrane. They are found in neurons where they generate low-threshold Ca2+ spikes and influence action potential firing patterns [4] in endocrine cells where they regulate hormone secretion [5], in heart cells where they influence impulse conduction and pacemaking [15, 69], in smooth muscle cells where they regulate proliferation and myogenic tone [14], and in cancerous cells whereas their functional role is under investigation [18].
There is increasing evidence suggesting that T-type channels play a direct role in regulating [Ca2+]i, especially in non-excitable tissues, including some cancerous cells [34, 50]. Thus, far, three different T-type channel subunits have been identified, including CACNA1G, CACNA1H, and CACAN1I, which encode α1G (Cav3.1), α1H (Cav3.2), and α1I (Cav3.3) isoforms [42, 45, 53], respectively. The α1 subunit refers to the channel’s primary ion-conducting protein, which consists of four domains (I–IV) each containing six transmembrane helices (S1 through S6). The S4 segment in each domain contains positively charged amino acid residues at every third or fourth position and forms part of the voltage sensor driving the channel to open and close in response to membrane potential changes (Fig. 1a). The four major domains are linked by cytoplasmic regions of different sizes and the N- and C-termini are localized on the cytoplasmic side [52] (Fig. 1b). Although there are other auxiliary channel subunits, the T-type channel α1 subunits can function as a standalone transmembrane protein. Each T-type channel isoform exhibits distinct cellular and subcellular distributions [52]. The Cav3.1 and Cav3.2 currents reflect the prototypical LVA T-type channel currents recorded in native cells, whereas Cav3.3 currents show markedly slower inactivation kinetics [29, 44, 45]. In addition, alternative splicing of Cav3 notably enhances the potential diversity of T-type channel isoforms [47], and there is growing evidence of significant differences in the tissue expression [28] and biophysical properties of the various splice variants [8, 54, 80]. The unique low-voltage-dependent activation/inactivation and slow deactivation of T-type channels indicate that these channels may play a physiological role in regulating [Ca2+]i at low voltages. At appropriate membrane potentials, T-type channels produce the “window current” that results in a sustained inward Ca2+ current through the portion of channels that are not completely inactivated. The window current allows T-type channels to regulate Ca2+ homeostasis under resting membrane conditions [53]. This modulation of Ca2+ homeostasis allows T-type channels to control cell proliferation and differentiation; the loss of control of the T-type channel may lead to aberrant cell growth and tumor progression [34, 50]. It has been hypothesized that a link exists between abnormal T-type channel expression and cancer progression [34]. For example, silencing of Cav3.1 channels by methylation of CpG islands (GC-rich regions of DNA) was observed in primary tumors [34], indicating that Cav3.1 may be a putative tumor suppressor gene [66]. In addition, Cav3.2 T-type channels may also be involved in cancer growth, as the neuroendocrine differentiation of cancer epithelial cancer cells was associated with an increase in their functional expression [38]. Furthermore, the impairment of T-type channels displayed an inhibitory effect on cancer development and progression [34]. Our recent data that were consistent with these results suggested that blockade of T-type channels inhibited U87 cell proliferation and migration, whereas inhibition of L-type channels elicited no such effects. Although recent studies identified T-type channel expression in a number of cancerous cells [18], their functional role is under investigation. Therefore, T-type channel blockers may provide novel strategies for treating certain types of cancer. This review focuses on recent advances in our understating of T-type channel expression and their role in tumors, particularly the blockade of T-type channels by endostatin (ES) for the potential treatment of glioblastoma.
T-type channels are broadly expressed in tumor cells
T-type channels are expressed in normal tissue throughout the body, including the brain, kidneys, heart, and smooth muscle [65]. However, they are also expressed in several different types of tumor including human glioma [28], esophageal tumor [35], breast cancer [65], and ovarian cancer tissues [33]. A recent study revealed the presence of T-type channel mRNA in biopsies of human breast tumors [65]. It has been demonstrated that T-type channel α1 subunit genes, either α1H alone or together with α1G and α1I, are overexpressed in human esophageal tumors compared to adjacent normal tissues which display lower α1 expression [35]. Furthermore, expression of these channels in tumor cell lines has been widely reported in prostate tumors [38], breast tumors [19, 65], fibrosarcomas [22], leukemia cells [66, 77], pheochromocytoma [16], retinoblastomas [2], neuroblastomas [29, 50], and gliomas [28], as summarized in Table 1. For example, human breast adenocarcinoma MDA-231 and MCF-7 cell lines exhibit transient expression of α1G and α1H T-type channel mRNA and T-type channel currents [65]. Human prostate cancer epithelial cells have also been observed to express increased T-type channel currents and α1H mRNA [38]. Although these tumors may express different α1 subunit of T-type channels at different amounts, it has been reported that a tumor-specific splice variant of the α1G isoform is expressed in some gliomas such as the U87 MG and U251 tumor cell lines [28]. Development of antibodies that recognize such tumor-specific α1G variants may offer an antibody-mediated tumor cell-specific killing for the potential treatment [28]. As described in our recent studies, human glioblastoma U87 cells endogenously express all three α1 subunits of Cav3 [79]. However, conflicting data are available regarding the expression of α1 subunits of the T-type channels Cav3.1, Cav3.2, and Cav3.3 in U87MG cells. While Lu et al. failed to detect T-type channel mRNA and T-type channel currents by using real-time PCR and electrophysiological methods [36], Panner et al. identified a significant decrease in the expression of the α1G and α1H subunits, which was correlated to dramatically decreased proliferation [49].
Furthermore, changes in expression of T-type channels depend on the status of the tumor. For example, when prostate tumors become aggressive, some epithelial cells differentiate into neuroendocrine cells that express T-type channels [38, 65]. Although these neuroendocrine cells do not proliferate, their LVA T-type channel activity stimulates the release of growth factors that strongly stimulate the aggressive proliferation of neighboring cells [38]. Similarly, in pheochromocytomas, T-type channels mediate the release of growth factors, such as nerve growth factor [50].
The role of T-type channels in tumor cells, particularly in glioma cells
It is well established that the pathology of a tumor mainly consists of proliferation and migration [26, 46]. Proliferation is considered a key factor in tumor development [26]. A number of previous studies suggested a potential role of T-type channels in controlling cell proliferation and migration. T-type channels play a key role in the regulation of [Ca2+]i during tumor development [18, 26, 50], which is supported by the fact that T-type channel blockers inhibit tumor growth [72]. A role of these channels in promoting cell cycle progression has been previously reported in hepatic, breast, prostate, and brain tumors and leukemia, retinoblastoma, and pheochromocytoma cells [34, 50]. For example, cells in the proliferative phase (G2/M) have been reported to express T-type channels, whereas those in the nonproliferative phases (G0/G1) primarily express L-type channels [56]. In line with this, the upregulation of T-type channels in the proliferative phase has also been identified in a variety of cancer cell lines [75]. The increased T-type channel expression stimulates the proliferation of esophageal cancer cells and the blockade of T-type channels diminishes the cell proliferation [35]. The expression of T-type channels has been genetically manipulated to reveal the contribution of T-type channels for proliferation. Human embryonic kidney cells (HEK293) cells were transfected with the α1H subunit of T-type channels resulting in significantly increased cell proliferation [70]. However, following overexpression of both α1G and α1H subunits in HEK293 cells, Chemin et al. observed increased [Ca2+]i levels but found no evidence of an increased proliferation rate [9].
In gliomas, Panner and colleagues varied the expression of the α1G and α1H subunits of T-type channels in U87MG cells to determine the cell proliferation [49, 50]. The responses to overexpression were studied in an N1E-115 neuroblastoma cell line with known expression of T-type channels (positive control) and COS-7 primate renal tumor cells, which did not express endogenous T-type channels (negative control) [50]. The overexpression of the α1H subunit significantly increased the proliferation of all three cell lines. Conversely, α1G subunit antisense oligonucleotides significantly inhibited the proliferation of the human glioma cell line U87MG and the mouse neuroblastoma cell line N1E-115 (positive control), but it had no effect on the COS-7 cell line that did not express T-type channels [49, 50]. In our recent study, we demonstrated that siRNA-mediated knockdown of the expression of the α1G/H subunit in U87 cells significantly inhibited cell proliferation, whereas the proliferation of the control siRNA-transfected cells was not significantly different from that of the untransfected cells [79]. Although these studies demonstrate the involvement of T-type channels in cell cycle regulation including proliferation, further studies are necessary to understand the underlying mechanism by which specific T-type channel subtypes regulate the proliferation of tumor cells.
Pharmacological blockade of T-type channels in tumor cells
The aforementioned observations suggest that T-type channels might be a target for the treatment of a number of tumors. Notably, the available agents that can affect T-type channels have varying degrees of specificity. Mibefradil was the first mixed T/L channel blocker to be marketed for its ability to block T-type channel currents. Mibefradil is approximately tenfold more selective for the blockade of T-type channels than the blockade of L-type channels [2]. In nude mice implanted with MCF-7 breast cancer cells, the injection of mibefradil at tumor sites resulted in marked tumor degeneration and necrosis [65]. In addition, mibefradil has been recognized as an effective inhibitor of proliferation in many other different cell types including smooth muscle cells [60], endothelial cells [48], liver cells [74], and NG1-8-15 cells [10]. Submicromolar concentrations of mibefradil suppressed the proliferation of U87MG and N1E-115 cells with a 50 % effective concentration (EC50) of 710 and 410 nM, respectively, and its specific effects on the α1G subunit were clarified using siRNA [49]. Bertolesi et al. reported that the EC50 [2] of mibefradil required to block proliferation was higher than that reported by Panner et al. in retinoblastoma and C6 glioma cell lines. The authors did not observe any significant changes in cell death with mibefradil at the EC50 concentration used above [49]. Although mibefradil has been recognized as a T/L-type channel blocker, it does interfere with additional cellular functions/ion channels, particularly at supramicromolar concentrations (30 μM) [48]. Nilius et al. noted that mibefradil can inhibit Ca2 + -activated Cl− currents, volume-sensitive Cl− currents, and store-dependent Ca2+ currents in endothelial cells [48]. Among other effects, the resultant cell swelling induced by mibefradil was considered a possible mechanism by which proliferation might be decreased in the cells studied. Similar results were obtained by other groups [57, 74]. In addition, mibefradil can also be metabolized by cytochromes P450 3A4 and 2D6, leading to drug-drug interactions [50].
Novel T-type channel blockers based on a 3, 4-dihydroquinazoline backbone have been recently synthesized [31, 51]. These compounds exhibited blocking potencies for transfected human Cav3.1 and Cav3.2 T-type channels in the micromolar range. However, the biological activity of these compounds in intact cells rather than transfected systems is yet to be reported. Using the structure-activity relationship of known blockers, Gray et al. synthesized two inhibitors of Ca2+ entry, TH-1177 and TH-1211 [20]. These two compounds with similar potencies and identical stereoselectivity blocked voltage-gated and capacitative Ca2+ entry. They had many properties similar to mibefradil such as the ability to decrease the proliferation of breast and prostate cancer cell lines [20]. TH-1177 was observed to extend the lifespan of mice inoculated with human prostate cancer cells. Using a similar approach of studying the molecular structure of L-type channel blockers, McCalmont et al. tested a new series of agents. They observed a direct correlation between the dose-responses for blocking T-type channels and for blocking proliferation in several different cell lines [40]. In addition, Singh et al. recently reported that SKF96365, originally identified as a blocker of receptor-mediated calcium entry, had notable overlapping physiological and pathophysiological associations between TRPC channels and LVA T-type channels. The authors reported that SKF96365 was actually a potent blocker of LVA T-type channels, which suggests caution in interpreting the results of the use of SKF96365 alone as a diagnostic agent for TRPC activity in native tissues [61]. Other chemicals that can inhibit the T-type channel activity and probably the proliferation include dihydropyridines, benzodiazepines, diphenylbutylpiperidine derivatives, succinimide derivatives, and anesthetics [27], as well as several potential physiological moderators of channel activity that include channel protein phosphorylation by cyclic AMP or G-proteins [78], arachidonic acid derivatives including anandamide [11, 12, 64] and nordihydroguaiaretic acid [12, 71]. Although nordihydroguaiaretic acid inhibits cyclooxygenase, the addition of prostaglandins did not reverse its blocking ability.
The antipsychotic drug pimozide has been reported to inhibit the proliferation of glioma cells [30]. The effects of pimozide have been related to its ability to block T-type channels, which is similar to that of mibefradil. In previous studies, Bertolesli et al. compared the effects of mibefradil and pimozide on retinoblastoma cell lines that express mRNA for the α1G and α1H subunits of T-type channels. They noted a significant increase in cell apoptosis following incubation with pimozide [2]. When retinoblastoma cell lines were treated with α1G subunit antisense, the effects of mibefradil were greatly attenuated, whereas those of pimozide remained unchanged. These investigators concluded that the decreased proliferation observed with pimozide involved a mechanism that was independent of T-type channel blockade but could involve the calmodulin-dependent regulation of T-type channels.
ES as a new inhibitor of T-type channels in glioblastoma
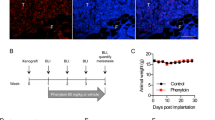
The mechanisms of in vivo antitumor action of ES, the carboxyl-terminal proteolytic fragment of collagen XVIII, are less understood and remain controversial. However, ES was previously considered to interact with several endothelial cell surface receptors that are involved in angiogenesis including caveolin-1, tropomyosin, and vascular endothelial growth factor type 1 receptor [24, 62, 73]. For instance, Peroulis et al. reported that the endogenous expression of ES by C6 glioma cells resulted in a reduced tumor growth rate [55]. Furthermore, Schmidt et al. demonstrated that local intracerebral application of ES improved treatment efficiency and survival in an orthotopic human glioblastoma model [59]. These results suggested that the antiangiogenic effect of ES was essential for the in vivo growth and expansion of tumors including glioblastoma. However, a later study failed to determine any antitumor effects of ES [39]. Growing evidence has recently revealed that ES could play a direct role in inhibiting tumor/cancerous cells [58, 76]. It has been reported recently that peptide 30 derived from ES suppresses the proliferation of HepG2 cells in vitro [32]. In our recent work, we revealed that, in addition to its antiangiogenic effects, ES also directly inhibited in vitro U87 human glioblastoma cell proliferation and migration by targeting T-type channels. We also observed that inhibition of T-type channel currents induced by ES was highly dependent on the inactivation state of the channel [79]. Although it is unclear whether the hyperpolarizing shift of the steady state inactivation curve would produce a significant modification in T-type channel “window currents,” it is conceivable that it could depend on an increased number of channels remaining in the inactivated state after activation. Further studies are required to address how making less T-type Ca2+ channels available for opening mechanistically contributes to the inhibitory effect of ES on glioma cellular responses. In this study, we evaluated the mibefradil data obtained by the siRNA-mediated knockdown approach and by using NNC 55–0396, a mibefradil nonhydrolyzable analog without L-type channel efficacy, to avoid the nonspecific antiproliferative effects of mibefradil [50]. ES or mibefradil inhibits the fibronectin-induced migration of U87 glioma cells. Similarly, mibefradil suppressed T-type-mediated Ca2+ spikes, waves, cell motility, and invasive properties in fibrosarcoma cells [21]. The magnitude of the inhibitory effect of mibefradil on the motility of U87 cells was higher than that induced by ES, further supporting that mibefradil displays broader T/L-type-independent effects as described previously.
ES has been reported to interact with vascular endothelial growth factor type 1 receptor, which associates with a family of receptor protein tyrosine kinases [24]. We identified in a previous study that the effects of ES on the proliferation and migration of U87 human glioma cells is not mediated by tyrosine kinase or G-protein-coupled signaling pathways. T-channel activity can be modulated by neurotransmitters and hormones through protein kinase (PK)-dependent signaling molecules such as PKA, PKC, and PKG; calmodulin-dependent protein kinase II; tyrosine kinases; and protein kinase-independent mechanisms including zinc, redox agents, and lipid derivatives such as arachidonic acid [23, 78]. Therefore, crucial questions about the nature of the signaling pathways involved in the ES-mediated inhibition of T-type channels, and the mechanism by which they regulate Cav3 activity remain unanswered. At present, it is not completely understood whether ES directly phosphorylates/blocks Cav3 channels or represents an indirect consequence of the phosphorylation of associated targeting, anchoring, or signaling proteins. Further studies are necessary to elucidate this issue. In addition, recent reports also suggest a role for extracellular signal-regulated kinase (ERK) pathways in T-type channel activation. For example, ciliary neurotrophic factor increases the expression and currents of T-type channels by triggering the Janus kinase/signal transducers and activators of transcription (JAK/STAT) and ERK signaling pathways [67]. However, this was not the case in this study because the inhibitory effect of ES on Cav3 T-type channel currents is rapid (within 10 min). In conclusion, in addition to the role of ES-induced angiogenesis in tumor progression, our study highlighted the therapeutic potential of ES via targeting T-type channels for the treatment of tumors with the endogenous expression of all three subunits of Cav3, including human glioblastoma multiforme (GBM). We revealed that ES directly inhibited the channel currents of only Cav3.1 and Cav3.2, but not that of Cav3.3 or Cav1.2. Our results highlight the novel mechanism and therapeutic potential of ES via targeting T-type channels for the treatment of human glioblastoma.
Perspectives
Determination of the expression and activity of T-type channels in specific tumors and the development of new, specific T-type channel blockers can potentially offer new approaches for the treatment of some cancers such as GBM that are no longer responsive to conventional treatment strategies. The search for subtype-specific T-type channel blockers has been of considerable interest from the clinical perspective. Although a number of classes of T-type blockers have been described (benzodiazepines, succinimide derivatives, diphenylbutylpiperidine derivatives, dihydropyridines, and anesthetics), their action is not sufficiently selective for T-type channels [17, 41]. T-type channels have isoform-specific properties, and therefore, the need to develop selective drugs for a given T-channel subtype has emerged. The subsequent challenge will be to determine whether specific T-channel isoforms can be selectively targeted for therapeutic intervention. Although a new treatment strategy has been identified with the utilization of genetic approaches recently, such as gene knockout or gene knockdown [3, 25], it does not represent a viable therapeutic approach at this time. Nevertheless, the search for new generations of selective T-type channel blockers is ongoing [1, 43]. In addition, it is also important to understand the regulatory mechanisms of the T-type calcium channel expression, which may lead to the identification of novel strategies of regulating T-type channel activity for therapeutic purposes, especially for controlling tumor growth.
References
Belardetti F, Zamponi GW (2008) Linking calcium-channel isoforms to potential therapies. Curr Opin Investig Drugs 9:707–715
Bertolesi GE, Shi C, Elbaum L, Jollimore C, Rozenberg G, Barnes S, Kelly ME (2002) The Ca(2+) channel antagonists mibefradil and pimozide inhibit cell growth via different cytotoxic mechanisms. Mol Pharmacol 62:210–219
Bourinet E, Alloui A, Monteil A, Barrere C, Couette B, Poirot O, Pages A, McRory J, Snutch TP, Eschalier A, Nargeot J (2005) Silencing of the Cav3.2 T-type calcium channel gene in sensory neurons demonstrates its major role in nociception. EMBO J 24:315–324
Cain SM, Snutch TP (2010) Contributions of T-type calcium channel isoforms to neuronal firing. Channels (Austin) 4:475–482
Carbone E, Giancippoli A, Marcantoni A, Guido D, Carabelli V (2006) A new role for T-type channels in fast “low-threshold” exocytosis. Cell Calcium 40:147–154
Catterall WA (2000) Structure and regulation of voltage-gated Ca2+ channels. Annu Rev Cell Dev Biol 16:521–555
Catterall WA, Perez-Reyes E, Snutch TP, Striessnig J (2005) International Union of Pharmacology. XLVIII. Nomenclature and structure-function relationships of voltage-gated calcium channels. Pharmacol Rev 57:411–425
Chemin J, Monteil A, Bourinet E, Nargeot J, Lory P (2001) Alternatively spliced alpha(1G) (Ca(V)3.1) intracellular loops promote specific T-type Ca(2+) channel gating properties. Biophys J 80:1238–1250
Chemin J, Monteil A, Briquaire C, Richard S, Perez-Reyes E, Nargeot J, Lory P (2000) Overexpression of T-type calcium channels in HEK-293 cells increases intracellular calcium without affecting cellular proliferation. FEBS Lett 478:166–172
Chemin J, Monteil A, Dubel S, Nargeot J, Lory P (2001) The alpha1I T-type calcium channel exhibits faster gating properties when overexpressed in neuroblastoma/glioma NG 108-15 cells. Eur J Neurosci 14:1678–1686
Chemin J, Nargeot J, Lory P (2007) Chemical determinants involved in anandamide-induced inhibition of T-type calcium channels. J Biol Chem 282:2314–2323
Chemin J, Traboulsie A, Lory P (2006) Molecular pathways underlying the modulation of T-type calcium channels by neurotransmitters and hormones. Cell Calcium 40:121–134
Ciapa B, Pesando D, Wilding M, Whitaker M (1994) Cell-cycle calcium transients driven by cyclic changes in inositol trisphosphate levels. Nature 368:875–878
Cribbs LL (2006) T-type Ca2+ channels in vascular smooth muscle: multiple functions. Cell Calcium 40:221–230
Cribbs L (2010) T-type calcium channel expression and function in the diseased heart. Channels (Austin) 4:447–452
Garber SS, Hoshi T, Aldrich RW (1990) Interaction of forskolin with voltage-gated K + channels in PC12 cells. J Neurosci 10:3361–3368
Giordanetto F, Knerr L, Wallberg A (2011) T-type calcium channels inhibitors: a patent review. Expert Opin Ther Patent 21:85–101
Gray LS, Macdonald TL (2006) The pharmacology and regulation of T type calcium channels: new opportunities for unique therapeutics for cancer. Cell Calcium 40:115–120
Gray LS, Perez-Reyes E, Gomora JC, Haverstick DM, Shattock M, McLatchie L, Harper J, Brooks G, Heady T, Macdonald TL (2004) The role of voltage gated T-type Ca2+ channel isoforms in mediating “capacitative” Ca2+ entry in cancer cells. Cell Calcium 36:489–497
Haverstick DM, Heady TN, Macdonald TL, Gray LS (2000) Inhibition of human prostate cancer proliferation in vitro and in a mouse model by a compound synthesized to block Ca2+ entry. Cancer Res 60:1002–1008
Huang L, Keyser BM, Tagmose TM, Hansen JB, Taylor JT, Zhuang H, Zhang M, Ragsdale DS, Li M (2004) NNC 55-0396 [(1S,2S)-2-(2-(N-[(3-benzimidazol-2-yl)propyl]-N-methylamino)ethyl)-6-fluoro-1,2, 3,4-tetrahydro-1-isopropyl-2-naphtyl cyclopropanecarboxylate dihydrochloride]: a new selective inhibitor of T-type calcium channels. J Pharmacol Exp Ther 309:193–199
Huang JB, Kindzelskii AL, Clark AJ, Petty HR (2004) Identification of channels promoting calcium spikes and waves in HT1080 tumor cells: their apparent roles in cell motility and invasion. Cancer Res 64:2482–2489
Iftinca MC, Zamponi GW (2009) Regulation of neuronal T-type calcium channels. Trends Pharmacol Sci 30:32–40
Kim YM, Hwang S, Pyun BJ, Kim TY, Lee ST, Gho YS, Kwon YG (2002) Endostatin blocks vascular endothelial growth factor-mediated signaling via direct interaction with KDR/Flk-1. J Biol Chem 277:27872–27879
Kim D, Song I, Keum S, Lee T, Jeong MJ, Kim SS, McEnery MW, Shin HS (2001) Lack of the burst firing of thalamocortical relay neurons and resistance to absence seizures in mice lacking alpha(1G) T-type Ca(2+) channels. Neuron 31:35–45
Kunzelmann K (2005) Ion channels and cancer. J Membr Biol 205:159–173
Lacinova L (2004) Pharmacology of recombinant low-voltage activated calcium channels. Curr Drug Targets CNS Neurol Disord 3:105–111
Latour I, Louw DF, Beedle AM, Hamid J, Sutherland GR, Zamponi GW (2004) Expression of T-type calcium channel splice variants in human glioma. Glia 48:112–119
Lee JH, Daud AN, Cribbs LL, Lacerda AE, Pereverzev A, Klockner U, Schneider T, Perez-Reyes E (1999) Cloning and expression of a novel member of the low voltage-activated T-type calcium channel family. J Neurosci 19:1912–1921
Lee GL, Hait WN (1985) Inhibition of growth of C6 astrocytoma cells by inhibitors of calmodulin. Life Sci 36:347–354
Lee YS, Lee BH, Park SJ, Kang SB, Rhim H, Park JY, Lee JH, Jeong SW, Lee JY (2004) 3,4-Dihydroquinazoline derivatives as novel selective T-type Ca2+ channel blockers. Bioorg Med Chem Lett 14:3379–3384
Li M, Xiong ZG (2011) Ion channels as targets for cancer therapy. Int J Physiol Pathophysiol Pharmacol 3:156–166
Li W, Zhang SL, Wang N, Zhang BB, Li M (2011) Blockade of T-type Ca(2+) channels inhibits human ovarian cancer cell proliferation. Cancer Invest 29:339–346
Lory P, Bidaud I, Chemin J (2006) T-type calcium channels in differentiation and proliferation. Cell Calcium 40:135–146
Lu F, Chen H, Zhou C, Liu S, Guo M, Chen P, Zhuang H, Xie D, Wu S (2008) T-type Ca2+ channel expression in human esophageal carcinomas: a functional role in proliferation. Cell Calcium 43:49–58
Lu F, Chen H, Zhou C, Wu S (2005) Is there a role for T-type Ca2+ channel in glioma cell proliferation? Cell Calcium 38:593–595, author reply 597
Machaca K (2011) Ca(2+) signaling, genes and the cell cycle. Cell Calcium 49:323–330
Mariot P, Vanoverberghe K, Lalevee N, Rossier MF, Prevarskaya N (2002) Overexpression of an alpha 1H (Cav3.2) T-type calcium channel during neuroendocrine differentiation of human prostate cancer cells. J Biol Chem 277:10824–10833
Marshall E (2002) Cancer therapy. Setbacks for endostatin. Science 295:2198–2199
McCalmont WF, Heady TN, Patterson JR, Lindenmuth MA, Haverstick DM, Gray LS, Macdonald TL (2004) Design, synthesis, and biological evaluation of novel T-Type calcium channel antagonists. Bioorg Med Chem Lett 14:3691–3695
McGivern JG (2006) Pharmacology and drug discovery for T-type calcium channels. CNS Neurol Disord Drug Targets 5:587–603
McRory JE, Santi CM, Hamming KS, Mezeyova J, Sutton KG, Baillie DL, Stea A, Snutch TP (2001) Molecular and functional characterization of a family of rat brain T-type calcium channels. J Biol Chem 276:3999–4011
Minor DL Jr, Findeisen F (2010) Progress in the structural understanding of voltage-gated calcium channel (CaV) function and modulation. Channels (Austin) 4:459–474
Monteil A, Chemin J, Bourinet E, Mennessier G, Lory P, Nargeot J (2000) Molecular and functional properties of the human alpha(1G) subunit that forms T-type calcium channels. J Biol Chem 275:6090–6100
Monteil A, Chemin J, Leuranguer V, Altier C, Mennessier G, Bourinet E, Lory P, Nargeot J (2000) Specific properties of T-type calcium channels generated by the human alpha 1I subunit. J Biol Chem 275:16530–16535
Monteith GR, Davis FM, Roberts-Thomson SJ (2012) Calcium channels and pumps in cancer: changes and consequences. J Biol Chem 287:31666–31673
Murbartian J, Arias JM, Lee JH, Gomora JC, Perez-Reyes E (2002) Alternative splicing of the rat Ca(v)3.3 T-type calcium channel gene produces variants with distinct functional properties(1). FEBS Lett 528:272–278
Nilius B, Prenen J, Kamouchi M, Viana F, Voets T, Droogmans G (1997) Inhibition by mibefradil, a novel calcium channel antagonist, of Ca(2+)- and volume-activated Cl- channels in macrovascular endothelial cells. Br J Pharmacol 121:547–555
Panner A, Cribbs LL, Zainelli GM, Origitano TC, Singh S, Wurster RD (2005) Variation of T-type calcium channel protein expression affects cell division of cultured tumor cells. Cell Calcium 37:105–119
Panner A, Wurster RD (2006) T-type calcium channels and tumor proliferation. Cell Calcium 40:253–259
Park SJ, Lee MJ, Rhim H, Kim Y, Lee JH, Chung BY, Lee JY (2006) Synthesis and SAR studies of a novel series of T-type calcium channel blockers. Bioorg Med Chem 14:3502–3511
Perez-Reyes E (2003) Molecular physiology of low-voltage-activated t-type calcium channels. Physiol Rev 83:117–161
Perez-Reyes E, Cribbs LL, Daud A, Lacerda AE, Barclay J, Williamson MP, Fox M, Rees M, Lee JH (1998) Molecular characterization of a neuronal low-voltage-activated T-type calcium channel. Nature 391:896–900
Perez-Reyes E, Lory P (2006) Molecular biology of T-type calcium channels. CNS Neurol Disord Drug Targets 5:605–609
Peroulis I, Jonas N, Saleh M (2002) Antiangiogenic activity of endostatin inhibits C6 glioma growth. Int J Cancer 97:839–845
Richard S, Neveu D, Carnac G, Bodin P, Travo P, Nargeot J (1992) Differential expression of voltage-gated Ca(2+)-currents in cultivated aortic myocytes. Biochim Biophys Acta 1160:95–104
Rouzaire-Dubois B, Dubois JM (1998) K + channel block-induced mammalian neuroblastoma cell swelling: a possible mechanism to influence proliferation. J Physiol 510(Pt 1):93–102
Santoni G, Santoni M, Nabissi M (2012) Functional role of T-type calcium channels in tumour growth and progression: prospective in cancer therapy. Br J Pharmacol 166:1244–1246
Schmidt NO, Ziu M, Carrabba G, Giussani C, Bello L, Sun Y, Schmidt K, Albert M, Black PM, Carroll RS (2004) Antiangiogenic therapy by local intracerebral microinfusion improves treatment efficiency and survival in an orthotopic human glioblastoma model. Clin Cancer Res 10:1255–1262
Schmitt R, Clozel JP, Iberg N, Buhler FR (1995) Mibefradil prevents neointima formation after vascular injury in rats. Possible role of the blockade of the T-type voltage-operated calcium channel. Arterioscler Thromb Vasc Biol 15:1161–1165
Singh A, Hildebrand ME, Garcia E, Snutch TP (2010) The transient receptor potential channel antagonist SKF96365 is a potent blocker of low-voltage-activated T-type calcium channels. Br J Pharmacol 160:1464–1475
Skovseth DK, Veuger MJ, Sorensen DR, De Angelis PM, Haraldsen G (2005) Endostatin dramatically inhibits endothelial cell migration, vascular morphogenesis, and perivascular cell recruitment in vivo. Blood 105:1044–1051
Talavera K, Nilius B (2006) Biophysics and structure-function relationship of T-type Ca2+ channels. Cell Calcium 40:97–114
Talavera K, Staes M, Janssens A, Droogmans G, Nilius B (2004) Mechanism of arachidonic acid modulation of the T-type Ca2+ channel alpha1G. J Gen Physiol 124:225–238
Taylor JT, Zeng XB, Pottle JE, Lee K, Wang AR, Yi SG, Scruggs JA, Sikka SS, Li M (2008) Calcium signaling and T-type calcium channels in cancer cell cycling. World J Gastroenterol 14:4984–4991
Toyota M, Ho C, Ohe-Toyota M, Baylin SB, Issa JP (1999) Inactivation of CACNA1G, a T-type calcium channel gene, by aberrant methylation of its 5′ CpG island in human tumors. Cancer Res 59:4535–4541
Trimarchi T, Pachuau J, Shepherd A, Dey D, Martin-Caraballo M (2009) CNTF-evoked activation of JAK and ERK mediates the functional expression of T-type Ca2+ channels in chicken nodose neurons. J Neurochem 108:246–259
Turner RW, Anderson D, Zamponi GW (2011) Signaling complexes of voltage-gated calcium channels. Channels (Austin) 5:440–448
Vassort G, Talavera K, Alvarez JL (2006) Role of T-type Ca2+ channels in the heart. Cell Calcium 40:205–220
Wang YQ, Brooks G, Zhu CB, Yuan WZ, Li YQ, Wu XS (2002) Functional analysis of the human T-type calcium channel alpha 1H subunit gene in cellular proliferation. Yi Chuan Xue Bao 29:659–665
Wang Z, Estacion M, Mordan LJ (1993) Ca2+ influx via T-type channels modulates PDGF-induced replication of mouse fibroblasts. Am J Physiol 265:C1239–C1246
Wang G, Lemos JR, Iadecola C (2004) Herbal alkaloid tetrandrine: from an ion channel blocker to inhibitor of tumor proliferation. Trends Pharmacol Sci 25:120–123
Wickstrom SA, Alitalo K, Keski-Oja J (2002) Endostatin associates with integrin alpha5beta1 and caveolin-1, and activates Src via a tyrosyl phosphatase-dependent pathway in human endothelial cells. Cancer Res 62:5580–5589
Wondergem R, Gong W, Monen SH, Dooley SN, Gonce JL, Conner TD, Houser M, Ecay TW, Ferslew KE (2001) Blocking swelling-activated chloride current inhibits mouse liver cell proliferation. J Physiol 532:661–672
Xu XP, Best PM (1990) Increase in T-type calcium current in atrial myocytes from adult rats with growth hormone-secreting tumors. Proc Natl Acad Sci U S A 87:4655–4659
Yang L, Lin Z, Lin J, Weng S, Huang Q, Zhang P, Fu J (2011) Antitumor effect of endostatin overexpressed in C6 glioma cells is associated with the down-regulation of VEGF. Int J Oncol 38:465–471
Yoshida M, Nosaka K, Yasunaga J, Nishikata I, Morishita K, Matsuoka M (2004) Aberrant expression of the MEL1S gene identified in association with hypomethylation in adult T-cell leukemia cells. Blood 103:2753–2760
Zhang Y, Jiang X, Snutch TP, Tao J (2013) Modulation of low-voltage-activated T-type Ca(2)(+) channels. Biochim Biophys Acta 1828:1550–1559
Zhang Y, Zhang J, Jiang D, Zhang D, Qian Z, Liu C, Tao J (2012) Inhibition of T-type Ca(2)(+) channels by endostatin attenuates human glioblastoma cell proliferation and migration. Br J Pharmacol 166:1247–1260
Zhong X, Liu JR, Kyle JW, Hanck DA, Agnew WS (2006) A profile of alternative RNA splicing and transcript variation of CACNA1H, a human T-channel gene candidate for idiopathic generalized epilepsies. Hum Mol Genet 15:1497–1512
Acknowledgments
We thank Dr. Dongsheng Jiang from the University of Ulm for his constructive comment on the manuscript. The work was supported by the National Natural Science Foundation of China (30900437, 81171056, 81200852, 31271258, and 81371229), NSFC-CNRS (81311130114), Natural Science Funding of Jiangsu Province (BK2011293), Natural Science Funding for Colleges and Universities in Jiangsu Province (12KJB320010), Scientific Research Foundation for the Returned Overseas Chinese Scholars of State Education Ministry (to Jin Tao), Suzhou Science and Technology Development Plan (SYS201037 and SYS201102), Young Medical Talents Training Program Grant of Pudong Health Bureau of Shanghai (PWRq2012-08, to Hua Wang), and Dong-Wu Scholar Funding of Soochow University.
Conflict of interest
The authors declare that they have no conflict of interests.
Author information
Authors and Affiliations
Corresponding author
Additional information
Yuan Zhang, Hua Wang, and Zhiyuan Qian contributed to this work equally.
Rights and permissions
About this article
Cite this article
Zhang, Y., Wang, H., Qian, Z. et al. Low-voltage-activated T-type Ca2+ channel inhibitors as new tools in the treatment of glioblastoma: the role of endostatin. Pflugers Arch - Eur J Physiol 466, 811–818 (2014). https://doi.org/10.1007/s00424-013-1427-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00424-013-1427-5