Abstract
The human bile acid-sensitive ion channel (hBASIC) is a cation channel of the degenerin/epithelial Na+ channel gene family that is expressed in the intestinal tract and can be activated by bile acids. Here, we show that in addition to its sensitivity for bile acids, hBASIC shares further key features with its rat ortholog: it is blocked by extracellular divalent cations, is inhibited by micromolar concentrations of the diarylamidine diminazene, and activated by millimolar concentrations of flufenamic acid. Furthermore, we demonstrate that two major bile acids present in human bile, chenodeoxycholic acid and deoxycholic acid, activate hBASIC in a synergistic manner. In addition, we determined the single-channel properties of hBASIC in outside-out patch clamp recordings, revealing a single-channel conductance of about 11 pS and a high Na+ selectivity. Deoxycholic acid activates hBASIC in patch clamp recordings mainly by reducing the single-channel closed time. In summary, we provide a thorough functional characterization of hBASIC.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
A trimeric structure with each subunit containing two transmembrane domains, a large extracellular domain and cytosolic N- and C-termini characterizes the members of the degenerin/epithelial Na+ channel (DEG/ENaC) family of cation channels [7]. However, their physiological functions and their modes of activation vary strongly. Constitutive activity, ligand activation by protons or peptides, and mechanosensitivity evolved in this family. The physiological function of DEG/ENaC channels ranges from epithelial Na+ absorption, over synaptic transmission to the sensation of touch [8].
In humans, the DEG/ENaC family comprises nine different genes. Four genes encode acid-sensing ion channels (ASICs), proton-gated channels expressed in the peripheral and the central nervous system [17]. Four genes encode subunits of the epithelial Na+ channel (ENaC), a constitutively active, amiloride-sensitive channel in various epithelia [8]. The ninth gene encodes the bile acid-sensitive ion channel (BASIC), which is closely related to ASICs but insensitive to protons.
BASIC was cloned more than a decade ago and initially named intestine Na+ channel (INaC) in humans [14] and brain liver intestine Na+ channel (BLINaC) in mouse and rat [13]. The names INaC and BLINaC referred to the main sites of expression of their mRNA. In humans, the mRNA is predominantly expressed in the intestine. In mouse and rat, the mRNA is additionally expressed in brain and liver [13, 14].
Rat BASIC (rBASIC) is inactive at rest and the resting state is stabilized by physiological concentrations of extracellular divalent cations. Consequently, removal of divalent cations activates the channel and changes ion selectivity from the non-selective resting state to a Na+-selective active state [18]. Strikingly, BASIC from mouse (mBASIC) has a drastically decreased affinity for divalent cations, rendering the channel constitutively active and Na+-selective under physiological concentrations of extracellular divalent cations [18], such that mBASIC functionally resembles ENaC. This difference between rat and mouse BASIC could be attributed to one single amino acid residue (A/S387) in the extracellular domains of the channels [18]. Similar to rBASIC, human BASIC (hBASIC) is in a low-activity state at rest when expressed in heterologous cells [14, 20] and can be activated by the removal of divalent cations [20].
A common feature of mBASIC and rBASIC is the inhibition by diarylamidines [19], blockers of ASICs [1]. A feature specific to rBASIC is its activation by millimolar concentrations of fenamates, in particular flufenamic acid (FFA) [19]. The identification of this artificial activator of rBASIC nourished the initial hypothesis that BASIC might be a ligand-gated channel like ASICs. Together, diarylamidines and FFA are pharmacological tools to study the physiological role of BASIC in native tissue.
Recently, the location of BASIC in the liver was narrowed to cholangiocytes, the epithelial cells of the bile ducts. Furthermore, bile acids were identified as putative physiological ligands of BASIC, which led to the renaming of the channel to Bile Acid-Sensitive Ion Channel - BASIC [20, 21]. Bile acids present in rat bile were shown to activate rBASIC and bile acids present in human bile were shown to activate hBASIC [20].
In the present study, we focused on a detailed electrophysiological characterization of hBASIC and a comparison with mBASIC and rBASIC. hBASIC shares the major characteristics like inhibition by divalent cations and diminazene and activation by flufenamic acid with rBASIC. Moreover, we show that bile acids characteristic for human bile—deoxycholic and chenodeoxycholic acid—robustly activate hBASIC. Finally, we report, for the first time, single-channel properties of hBASIC and demonstrate its activation by deoxycholic acid at the single-channel level. Taken together, our data provide novel insights into the function of the human DEG/ENaC channel BASIC.
Materials and methods
Molecular biology
The cDNA for hBASIC was cloned into pRSSP as described previously [20]. Capped cRNA was synthesized by SP6 RNA polymerase from linearized cDNA using the mMessage mMachine kit (Ambion, Austin, TX, USA).
Two-electrode voltage clamp measurements
Preparation of Xenopus laevis oocytes is described elsewhere [15]. After injection of hBASIC cRNA into stage V or VI oocytes, oocytes were incubated in low Na+ OR-2 medium (in mM: 5 NaCl, 77.5 N-methyl-d-glucamine (NMDG), 2.5 KCl, 1 Na2HPO4, 5 HEPES, 1 MgCl2, 1 CaCl2, and 0.5 g/l polyvinylpyrrolidone, pH 7.3) at 19 °C. Forty eigth to seventy two h post injection, whole-cell currents were recorded as described previously [20]. Standard bath solution for two-electrode voltage clamp measurements contained (in mM) 140 NaCl, 1.8 CaCl2, 1.0 MgCl2, and 10 HEPES, pH 7.4. Bath solution with low concentrations of divalent cations contained (in mM) 140 NaCl, 10 HEPES, 2 EDTA or HEDTA, and the appropriate amount of CaCl2 or MgCl2 calculated using the software CaBuf [11]; it was supplemented with 100 μM flufenamic acid to block the conductance induced in Xenopus oocytes by divalent-free extracellular solutions.
Single-channel recordings in outside-out patches
Oocytes injected with hBASIC cRNA were stored in ND96 solution (in mM: 96 NaCl, 2 KCl, 1.8 CaCl2, 1 MgCl2, 5 HEPES, pH 7.4 with Tris) supplemented with 100 units/ml penicillin and 100 μg/ml streptomycin. Single-channel recordings in outside-out membrane patches of hBASIC expressing oocytes were performed two days after cRNA injection essentially as described previously [2, 3, 6, 10, 12] using conventional patch clamp technique. Patch pipettes were pulled from borosilicate glass capillaries and had a tip diameter of about 1–1.5 μm after fire polishing. Pipettes were filled with K-gluconate pipette solution (in mM: 90 K-gluconate, 5 NaCl, 2 Mg-ATP, 2 EGTA, and 10 HEPES, pH 7.28 with Tris). Seals were routinely formed in a low sodium NMDG-Cl bath solution (in mM: 95 NMDG-Cl, 1 NaCl, 4 KCl, 1 MgCl2, 1 CaCl2, 10 HEPES, 7.4 pH with Tris). In this bath solution, the pipette resistance averaged about 7 MΩ. After seal formation, the NMDG-Cl solution was switched to a NaCl bath solution in which NMDG-Cl (95 mM) was replaced by NaCl (95 mM). For continuous current recordings, membrane patches routinely were voltage-clamped at −70 mV, close to the calculated equilibrium potential of Cl− (\( {E}_{{\mathrm{CI}}^{-}} \) = −77.4 mV) and K+ (\( {E}_{K^{+}} \) = −79.4 mV) under our experimental conditions. Experiments were performed at room temperature (∼23 °C). Single-channel current data were initially filtered at 2.5 kHz and sampled at 10 kHz. The current traces were re-filtered at 650 Hz to resolve the single-channel current amplitude (i) and channel activity. The latter was derived from binned amplitude histograms as the product NPo, where N is the number of channels and Po is open probability [2, 3, 9, 10, 16]. The current level at which all channels are closed was determined in the presence of 10 μM diminazene. Single-channel data were analyzed using the program “Patch for Windows” written by Dr. Bernd Letz (HEKA Elektronik, Lambrecht/Pfalz, Germany) and a program written by Dr. V. Nesterov (Institut für Zelluläre und Molekulare Physiologie, Friedrich-Alexander-Universität Erlangen-Nürnberg, Erlangen, Germany). Using a 3 M KCl flowing boundary electrode, the liquid junction (LJ) potential occurring at the pipette/NaCl bath junction was measured to be ∼12 mV (bath positive) and was not significantly affected by the removal of divalent cations. To correct for this, the I/V plot shown in Fig. 6 was shifted to the left by 12 mV. The V hold values indicated for single-channel current traces are not LJ potential corrected.
Results
Human BASIC is inhibited by physiological concentrations of extracellular divalent cations
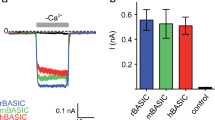
The heterologous expression of human BASIC in Xenopus laevis oocytes revealed a weak, constitutive current with an average amplitude of 0.5 ± 0.1 μA (n = 10), which was partly blocked by amiloride (4 mM; Fig. 1a). This is in line with previous studies for hBASIC and rBASIC [14, 20]. Similarly to rBASIC [18], complete removal of extracellular Ca2+ and Mg2+ drastically increased the current amplitude to 3.4 ± 0.6 μA (n = 10; Fig. 1a). This was not the case in non-injected control oocytes (Fig. 1b). The apparent IC50 was 18 ± 2.6 μM for Ca2+ and 51.4 ± 10.2 μM for Mg2+ (Fig. 1c and d), similar to rBASIC (IC50 Ca2+ = 13.2 ± 2 μM and IC50 Mg2+ = 79 ± 10 μM) [21]. At physiological concentrations of extracellular divalent cations, hBASIC is almost completely inhibited, suggesting that extracellular divalent cations stabilize its inactive resting state.
hBASIC is inhibited by physiological concentrations of extracellular divalent cations. a Representative current trace of an oocyte expressing hBASIC. The amiloride (4 mM) sensitive inward current component was determined under normal standard bath conditions (1.8 mM Ca2+ and 1.0 mM Mg2+) or in the absence of divalent cations. b Representative current trace of a non-injected oocyte in the presence and absence of extracellular divalent cations (−Ca2+). c Upper panel representative hBASIC current trace obtained in response to decreasing extracellular Ca2+ concentrations in the absence of Mg2+. Lower panel representative hBASIC current trace obtained in response to decreasing extracellular Mg2+ concentrations in the absence of Ca2+. d Concentration-dependent inhibition of hBASIC by extracellular Ca2+ (closed circles) and Mg2+ (open circles). Currents were normalized to the currents in the absence of Ca2+ or Mg2+, which had amplitudes of 2.9 ± 0.5 μA (n = 10) and 3.6 ± 0.4 μA (n = 14), respectively. Curves represent fits to the Hill equation. Error bars SEM
Pharmacological properties of human BASIC
rBASIC and mBASIC are both inhibited by micromolar concentrations of the diarylamidine diminazene [19]. When we applied increasing concentrations of diminazene in the presence of physiological concentrations of divalent cations to oocytes expressing hBASIC, we observed a concentration-dependent decrease in the amplitude of the weak constitutive current (Fig. 2a); the apparent IC50 was 3.4 ± 1 μM (n = 11; Fig. 2b) and thus in a similar range as for rBASIC and mBASIC (3.5 ± 0.6 and 2.1 ± 0.3 μM, respectively) [19]. Similar to rBASIC [19], application of millimolar concentrations of FFA rapidly induced robust, concentration-dependent currents in oocytes expressing hBASIC (Fig. 3a). In non-injected control oocytes, millimolar concentrations of FFA did not elicit any currents (data not shown). Due to the limited solubility of FFA in standard bath solution, FFA-induced hBASIC currents reached no plateau and the apparent EC50 of FFA for hBASIC could only be estimated (≈10 mM; Fig. 3b). Taken together, the pharmacological profile of hBASIC closely resembled that of rBASIC.
hBASIC is inhibited by diminazene. a Representative current trace of hBASIC recorded in the presence of increasing concentrations of diminazene (DIMI). b Concentration-dependent inhibition of hBASIC by DIMI. Currents were normalized to the total current carried by Na+, which had an amplitude of 0.3 ± 0.04 μA (n = 11), as revealed by replacing Na+ by NMDG+. Curve represents fit to the Hill equation. Error bars SEM
hBASIC is activated by flufenamic acid. a Representative current trace of hBASIC showing its activation by repetitive application of increasing concentrations of FFA. b Concentration-dependent activation of hBASIC by FFA. Peak currents were normalized to the peak current at 1 mM FFA, which had an amplitude of 4.5 ± 0.5 μA (n = 7). Dotted line represents fit to the Hill equation. Error bars SEM
Ion selectivity of human BASIC
While mBASIC is a Na+-selective channel, the ion selectivity of rBASIC varies between the resting state, which is unselective for monovalent cations, and the active state induced by the removal of divalent cations, which is Na+-selective [18]. We therefore tested whether hBASIC also changes its selectivity upon removal of extracellular divalent cations. The reversal potential of hBASIC-expressing oocytes was −12.8 ± 1.6 mV (n = 9) in normal concentrations of Ca2+ and Mg2+ (1.8 mM Ca2+, 1 mM Mg2+) and significantly shifted by approximately 24 mV to 11.3 ± 1.6 mV (n = 18, p < 0.005) upon removal of the extracellular divalents (Fig. 4). Since background conductances of the oocyte contributed to these reversal potentials, we cannot exclude that the shift was merely due to an increased contribution of hBASIC to the total current. Still, the reversal potential observed after removal of divalent cations was less positive than expected for a typical Na+ equilibrium potential in a normal oocyte with a low intracellular Na+ concentration. This may be explained by Na+ loading of the oocytes mediated by the small constitutive activity of hBASIC. Activation of hBASIC by FFA, however, did not shift the reversal potential (E rev,FFA − 11.3 ± 1.6 mV, n = 20, p = 0.5; Fig. 4), arguing that selectivity of hBASIC for Na+ indeed increased upon removal of extracellular divalent cations but not upon activation by FFA, which is at variance with rBASIC, for which the reversal potential shifts to more positive values in the presence of FFA [19]. Thus, although we gained some evidence that in whole oocytes hBASIC is a relatively unselective cation channel, which increases its ion selectivity upon removal of Ca2+, ion selectivity of hBASIC could not be precisely determined in whole oocytes.
Selectivity of hBASIC depends on extracellular divalent cations. Mean current–voltage relationship of hBASIC in standard bath (SB, open squares), in standard bath containing 1 mM FFA (FFA, triangles), and in bath solution containing 10 nM Ca2+ and 0 Mg2+ (−Ca2+, circles). The holding potential was increased stepwise from −100 to +60 mV in 20 to 30 mV steps; currents were normalized to the current at −100 mV, which had amplitudes of 1.8 ± 0.1 μA (SB, n = 9), 2 ± 0.3 μA (FFA, n = 20), and 7.7 ± 1.8 μA (−Ca2+, n = 18). Error bars SEM
Bile acid activation of human BASIC
rBASIC is potently and reversibly activated by chenodeoxycholic acid (CDCA) and hyodeoxycholic acid (HDCA), two bile acids present in rat bile [20]. When applied together, CDCA and HDCA synergistically activate rBASIC. In a previous study, we demonstrated that CDCA also activates hBASIC [20], while HDCA, which is absent from human bile, elicited only small currents compared to rBASIC, and the CDCA activation was not potentiated by HDCA. Here, we revisited activation of hBASIC by the three main bile acids present in human bile: CDCA, cholic acid (CA), and deoxycholic acid (DCA). Individual application of 1 mM of CDCA, CA, or DCA rapidly induced non-desensitizing currents ranging from 0.1 to 1.7 μA (n = 17–25), with CDCA and DCA more potently activating hBASIC than CA (CDCA, 1.7 ± 0.4 μA; CA, 0.1 ± 0.02 μA; DCA, 1.0 ± 0.2 μA; Fig. 5a and b). Combined application of CA and DCA (0.5 mM each) did not potentiate hBASIC currents (0.3 ± 0.05 μA, n = 25), but rather decreased them compared to 1 mM DCA alone, suggesting that CA and DCA do not act synergistically. The reduction in activity by co-application of CA and DCA is most likely due to the partial substitution of the potent hBASIC activator DCA by the less potent activator CA. In contrast, co-application of CDCA and DCA, each at 0.5 mM, more strongly activated hBASIC (3.8 ± 1 μA, n = 25; p < 0.05) than individual application of either 1 mM CDCA or 1 mM DCA, suggesting a synergistic activation by these two bile acids, similar to the synergistic activation of rBASIC by CDCA and HDCA.
Activation of hBASIC by bile acids. a Left representative current trace from an hBASIC expressing oocyte. hBASIC was activated by removal of extracellular divalent cations (-Ca2+) and by subsequent application of 1 mM DCA, CA, CDCA, and the combination of either DCA and CA or DCA and CDCA at 0.5 mM each. Right scatter dot plot illustrating the quantification of hBASIC activation induced by DCA, CA, DCA/CA, CDCA, and DCA/CDCA (n = 24–30). b As in a, but bile acids were applied in the absence of divalent cations (n = 12). Current amplitudes were determined by subtracting the current before bile acid activation from the peak current. Currents were normalized to the current in the absence of divalent cations (0 Mg2+, 10 nM Ca2+). Bars mean and SEM, respectively. c Activation of hBASIC by CDCA and recovery after washout for 30 s. d The residual current after washout of CDCA is blocked by 100 μM DIMI. e Activation of hBASIC by CDCA is blocked by 100 μM DIMI. f Non-injected oocytes did not respond to 1 mM CDCA. Current traces are representative for 10 experiments
Furthermore, we tested whether the application of bile acids in the absence of divalent cations potentiates the hBASIC response, as previously reported for rBASIC [21]. This was indeed the case. Application of 1 mM of the individual bile acids (CA, CDCA, and DCA) in the absence of divalent cations strongly increased the current amplitude compared to the application of the bile acids in the presence of divalent cations (Fig. 5b). The co-application of CDCA and DCA also showed a synergistic effect compared to their individual application. No synergistic effect was observed when CA and CDCA were co-applied (Fig. 5b).
CDCA induced a current in hBASIC-expressing oocytes that did not fully recover within seconds upon the removal of bile acids in the presence of divalent cations (Fig. 5a and c). To unequivocally confirm that the current induced by CDCA is due to activation of hBASIC rather than to a non-specific permeabilization of the oocyte plasma membrane, we applied 100 μM diminazene after washout of 1 mM CDCA when the current had not fully returned to baseline. The remaining current was completely blocked by 100 μM diminazene (Fig. 5d) indicating that hBASIC slowly recovers from CDCA-activation. This is in contrast to activation by DCA and CA, from which hBASIC quickly recovered after washout of the bile acids. In addition, we applied 1 mM CDCA in the presence of 100 μM diminazene to hBASIC-expressing oocytes. Under these conditions, the CDCA-induced current was almost completely blocked suggesting that CDCA specifically activated hBASIC (Fig. 5e). CDCA did not induce currents in non-injected oocytes (Fig. 5f).
Taken together, these data support previous findings that hBASIC is activated by bile acids. In addition, they demonstrate that CDCA and DCA, which constitute ∼60 % of bile acids in human bile, synergistically activate hBASIC.
Single-channel conductance and ion selectivity of hBASIC
Single-channel properties of hBASIC have not yet been elucidated. To resolve hBASIC single-channel currents, we performed patch clamp experiments in the outside-out configuration using oocytes expressing low levels of hBASIC as confirmed by two-electrode voltage clamp experiments. A typical current recording from an outside-out patch obtained from an oocyte expressing hBASIC is shown in Fig. 6. At a holding potential of −70 mV, washout of diminazene resulted in the appearance of readily detectable single-channel current transitions as shown on an expanded time scale in the inset below the continuous current trace. The single-channel current amplitude (i) increased by hyperpolarizing the patch to −100 mV and decreased with more positive holding potentials. The I/V plot shown in Fig. 6b summarizes data from similar experiments as shown in Fig. 6a. A Goldman–Hodgkin–Katz fit of these data is consistent with a sodium selective ion channel with a single-channel conductance for Na+ of about 11 pS. This latter value is in the range of the unitary conductance reported for rBASIC activated by a mutation of the degenerin site (9–10 pS) [13]. To further investigate the ion selectivity of hBASIC, we performed additional ion substitution experiments. Replacing Na+ by Li+ in the bath solution (Fig. 7a) did not change the single-channel current amplitude of hBASIC, which at a holding potential of −70 mV averaged −0.99 ± 0.02 pA (n = 15) and −1.04 ± 0.02 pA (n = 4) in the presence of Na+ and Li+, respectively. This indicates that hBASIC has a similar single-channel conductance for Na+ and Li+. In contrast, when extracellular Na+ was replaced by K+ (Fig. 7b) single-channel current events were no longer observed which suggests that hBASIC has no detectable single-channel conductance for K+. Thus, our outside-out patch clamp experiments indicate that hBASIC is a small conductance sodium-selective channel with an ion selectivity sequence of Li+ = Na+ > > K+.
Single-channel conductance of hBASIC. a Representative single-channel current trace at different holding potentials (V hold) from an outside-out patch of an oocyte expressing hBASIC. Diminazene (DIMI, 10 μM) was present in the bath solution as indicated above the trace by the black bar. The insets show the indicated segments of the current trace on expanded scales. b Average single-channel I/V plot calculated from recordings (nine patches from three batches of oocytes) similar to those shown in a. Binned current amplitude histograms (not shown for clarity) were used to determine the single-channel current amplitude (i) at each holding potential. The dashed line represents a Goldman–Hodgkin–Katz fit of the data for a Na+-selective channel with a predicted Na+ equilibrium potential (ENa+) of 75.4 mV. Single-channel conductance (g*) was calculated from the fit of the average I/V plot. Error bars SEM
Ion selectivity of hBASIC. a and b, representative single-channel current recordings obtained at V hold = −70 mV from an outside-out patch of an oocyte expressing hBASIC. The bars above the traces indicate the bath solution exchanges from NaCl to LiCl or from NaCl to KCl. The delay of the effect of the solution exchange on the single-channel currents reflects the time needed for a complete bath solution exchange. The insets show the indicated segments of the current traces on an expanded time scale. The current level at which all channels are closed was determined in the presence of DIMI (10 μM). No detectable single-channel events were observed in the trace in the presence of KCl in the bath
Removal of extracellular divalent cations increases single-channel activity and single-channel current amplitude of hBASIC
To investigate the effect of extracellular divalent cation removal on hBASIC at the single-channel level, we performed outside-out patch clamp recordings from oocytes expressing hBASIC (V hold = −70 mV) as shown in Fig. 8. As described above, removal of diminazene resulted in the appearance of single-channel current transitions (Fig. 8a) confirming the functional expression of hBASIC not detectable in non-injected control oocytes (Fig. 8d). Removal of divalent cations caused a shift in the baseline current level, which was also observed in non-injected control oocytes (Fig. 8d). Therefore, this shift cannot be attributed to an effect on hBASIC activity but is probably an effect mediated by a reduction of the seal resistance known to be affected by divalent cations. Importantly, after removal of extracellular divalent cations the activity (NPo) of hBASIC increased significantly as summarized in Fig. 8c. The insets in Fig. 8a demonstrate an increased frequency of channel transitions with longer channel openings in the absence of extracellular divalent cations (inset 2.) compared to control conditions (inset 1.). In addition, at a holding potential of −70 mV the single-channel current amplitude of hBASIC increased on average from −0.94 ± 0.05 pA (n = 11) in presence of Ca2+ and Mg2+ to −1.28 ± 0.03 pA (n = 11, p < 0.001) in the absence of Ca2+ and Mg2+ in the bath solution (Fig. 8b). Diminazene added in the absence of extracellular divalent cations decreased channel activity confirming that the channel activity elicited by removal of divalent cations can be attributed to hBASIC (Fig. 8a, inset 3.). In summary, these data demonstrate that removal of extracellular divalent cations activates hBASIC by a dual mechanism: The major effect is an increase in channel open probability with an increased frequency of channel gating and an increase in the duration of channel openings. In addition, an increased single-channel conductance contributes to the effect.
Effect of extracellular divalent cation removal on hBASIC at the single-channel level. a Representative single-channel current recording obtained at V hold = −70 mV from an outside-out patch of an oocyte expressing hBASIC. Diminazene (DIMI, 10 μM) was present and divalent cations were absent (−Ca2+) in the bath solution as indicated by the bars above the traces. The insets (1., 2., and 3.) show the indicated segments of the continuous current trace on expanded scales. b, c Average single-channel current amplitude and NPO of hBASIC before (wash DIMI) and after removal of extracellular divalent cations (−Ca2+) from similar experiments as shown in a. Numbers inside the columns indicate the number of individual patches measured. Six different batches of oocytes were used. Error bars SEM. d Representative current recording obtained at V hold = −70 mV from an outside-out patch from a non-injected control oocyte
DCA activates hBASIC mainly by reducing the single-channel closed time
We investigated the activation of hBASIC by DCA at the single-channel level (Fig. 9). Outside-out patch clamp recordings from oocytes expressing hBASIC were performed at a continuous holding potential of −70 mV and experiments were started in the presence of diminazene (10 μM) in the bath solution. Washout of diminazene revealed hBASIC channel activity which further increased after exposure of the patch to DCA (0.5 mM). Re-addition of diminazene demonstrated that stimulated channel activity was sensitive to this blocker confirming that the increased channel activity can be attributed to hBASIC (Fig. 9a). Using amplitude histograms (Fig. 9b) we demonstrated that DCA increased NPo but did not alter the single-channel current amplitude (i) of hBASIC (Fig. 9c). Importantly, diminazene removal and DCA application essentially had no effect in control experiments performed in non-injected oocytes (Fig. 9d). A quantitative analysis of single-channel current traces from 15 experiments demonstrated that the observed increase in NPo by diminazene washout is caused by a significant increase in the apparent mean open time and a reduction of the apparent mean closed time of the channel (Fig. 10). After washout of diminazene, the subsequent application of DCA caused an additional increase in NPo. This was accompanied by a non-significant trend for a further increase in apparent mean open time (Fig. 10b) and a significant reduction of the apparent mean closed time (Fig. 10c). Thus, stimulation of human BASIC by DCA can be attributed mainly to a decrease of the single-channel closed time.
Activation of hBASIC by deoxycholic acid (DCA) resolved at the single-channel level. a Representative single-channel current recording obtained at V hold = −70 mV from an outside-out patch from an oocyte expressing hBASIC. Diminazene (10 μM) and the taurine conjugate of deoxycholic acid (0.5 mM) were present in the bath solution as indicated by the bars. The insets (1. and 2.) show the indicated segments of the continuous current trace on an expanded time scale. b Single-channel binned current amplitude histograms were obtained from the current trace shown in a after washout of diminazene (wash DIMI) or in the presence of DCA (DCA). These histograms were used to evaluate single-channel current amplitudes (i) and channel activity (NPo). c Average single-channel current amplitude of hBASIC before (wash DIMI) and after stimulation with DCA from similar experiments as shown in a. Numbers inside the columns indicate the number of individual patches measured. Five different batches of oocytes were used. d Representative single-channel current recording obtained at V hold = −70 mV from an outside-out patch from a non-injected control oocyte. Error bars SEM
Deoxycholic acid activates hBASIC mainly by reducing the single-channel closed time. Single-channel traces from experiments as shown in Fig. 9a were further analyzed to determine NPo a, apparent mean channel open time b and apparent mean channel closed time c in the presence of diminazene (DIMI), after removal of diminazene (wash DIMI), in the presence of DCA (DCA), and in the presence of DCA together with diminazene (DCA + DIMI) in the bath solution. In patches used for this analysis more than one channel may have been active. For example, in the representative experiment shown in Fig. 8a a second channel level occasionally was observed after channel activation by DCA. Thus, the values reported do not strictly reflect the mean open and mean closed time of a single channel and therefore were termed apparent mean open and apparent mean closed time. Fifteen individual patches were analyzed from five different batches of oocytes. Error bars SEM. *p < 0.05, **p < 0.01, ***p < 0.001, paired t test
Discussion
The amino acid sequence of the human DEG/ENaC BASIC is 79 % identical to that of its orthologs from mouse and rat. In terms of their electrophysiological and pharmacological features, however, they vary substantially. While mBASIC is a constitutively active channel, rBASIC is almost completely inactive at rest. Diarylamidines inhibit both rat and mouse BASIC while fenamates, in particular FFA, activate rBASIC but not mBASIC [19]. In this study, we focussed on the electrophysiological and pharmacological characteristics of hBASIC in comparison with mouse and rat BASIC. Furthermore, we characterized the single-channel properties of hBASIC.
Electrophysiological and pharmacological profile of hBASIC
In line with previous findings, our data suggest that hBASIC is almost inactive at rest. Strong reduction of the concentration of extracellular divalent cations rapidly increased the current amplitude. The affinity for extracellular Ca2+ and Mg2+ was in a similar range as for rBASIC and slightly higher for Ca2+ than for Mg2+. Furthermore, human BASIC was inhibited by diminazene and activated by FFA. Taken together, this pharmacological profile closely resembles that of rBASIC. Another similarity of human and rat BASIC is their sensitivity for bile acids. We have shown previously that hBASIC is activated by CDCA, besides CA one of the major bile acids in humans [20]. In this study, we revisited the activation of hBASIC by bile acids and included DCA in our analysis, which contributes approximately 10–15 % to the total bile acid pool [4]. Interestingly, DCA also strongly activated hBASIC. This is different from rBASIC, which is only weakly activated by DCA (Wiemuth D. and Gründer S., unpublished observation). The response of hBASIC to bile acids is also dependent on the presence of extracellular divalents as the removal of divalent cations strongly increased the response of hBASIC to bile acids, representing another common feature of human and rat BASIC. Co-application of DCA and CDCA to hBASIC had a similar synergistic effect as the co-application of CDCA and HDCA to rBASIC. These findings suggest a species-specific effect of bile acids and that bile acids and BASICs co-evolved.
Oocytes expressing rBASIC and hBASIC had a slightly negative reversal potential (−10 mV; Fig. 4) [18], suggesting that the channel is a non-selective cation channel. Upon removal of divalent cations, the reversal potential of the oocytes shifted to positive values suggesting that the Na+-selectivity of BASIC increased. We note, however, that it is not straightforward to derive the selectivity of an ion channel from whole oocyte reversal potentials. Several channels contribute to the reversal potential of oocytes and we estimate that at rest BASIC contributed approximately 50 % to the whole oocyte conductance. This contribution will increase upon activation of BASIC, for example by bile acids or removal of divalent cations. In addition, oocytes expressing rBASIC and hBASIC likely accumulate Na+, due to the weak activity of the channels at rest, which would shift the Na+ equilibrium potential to less positive values than usual. The resting potential of oocytes expressing hBASIC and rBASIC was indeed usually slightly shifted towards less negative values compared to non-injected oocytes, supporting the intracellular accumulation of Na+. For these reasons, the ion selectivity of BASIC is better investigated in excised membrane patches.
Single-channel properties of hBASIC
We report here for the first time the single-channel properties of hBASIC. The patch clamp recordings revealed a single-channel conductance of 11 pS, which fits well with the single-channel conductance of rBASIC containing an activating mutation at the degenerin site (9–10 pS) as previously reported by Sakai et al. [13]. Furthermore, the I–V relation of hBASIC determined by patch clamp recordings is consistent with a theoretical reversal potential as expected for a Na+ selective channel. Ion substitution experiments support this finding and show that the channel is equally permeable for Na+ and Li+ but virtually impermeable for K+. These results contrast with the observations in whole oocytes but might be explained by the fact that the experimental conditions are better controlled in outside-out patch clamp recordings compared to whole-cell recordings. It is possible, however, that in the outside-out configuration intracellular protein components of a putative channel complex that could theoretically affect the selectivity of the channel might have been removed and that the selectivity of the channel in whole cells is indeed different from its selectivity in excised patches. Since such intracellular protein partners are currently hypothetical, we provisionally conclude that hBASIC is a Na+-selective channel.
The selectivity of hBASIC for Na+ over K+ is thus very similar to αβγENaC. In contrast, αβγENaC is more permeable for Li+ than for Na+ compared to hBASIC, which is equally permeable for Na+ and Li+. Interestingly, δβγENaC is less permeable for Li+ compared to αβγENaC and thus more similar to hBASIC [5]. The selectivity filter motif GAS in the second transmembrane domain is identical between hBASIC and δENaC (GAS) and slightly different between hBASIC and αENaC (GSS). It is tempting to speculate that this difference in the selectivity filter is responsible for the observed differences in Li+ and Na+ permeability.
Inhibition of the channel by diminazene and activation by DCA were also observed on the single-channel level. Analysis of the data revealed that the stimulatory effect of DCA was mainly mediated by a reduction of the apparent closed time of hBASIC but not by an increase in single-channel amplitude. The trend for an increase of channel open time by DCA was not statistically significant. On this basis, we speculate that DCA and probably other bile acids activate the channel mainly by destabilizing the closed state. Stabilization of the open state likely plays a secondary role in the activation of the channel. Interestingly, we previously concluded that removal of divalent cations opens BASIC also by destabilizing the closed state [18]. Additive stimulation by simultaneous removal of divalents and application of bile acids indicate that neither manoeuver alone completely destabilizes the closed state and transfers all channels into the open state.
The expression of BASIC in the intestinal tract is shared by human, mouse, and rat BASIC. This information together with the fact that bile acids can reach effective millimolar concentrations in the intestine implies a physiological role for BASIC in vectorial Na+ transport in the intestinal epithelium. It remains to be shown, however, whether BASIC is a bona fide ligand-gated channel with bile acids as its natural ligand or whether the effect of bile acids is indirect and mediated via modulation of the membrane. These are important questions to be addressed in future studies.
Abbreviations
- AMIL:
-
Amiloride
- ASIC:
-
Acid-sensing ion channel
- BASIC:
-
Bile acid-sensitive ion channel
- BLINaC:
-
Brain liver intestine Na+ Channel
- CA:
-
Cholic acid
- CDCA:
-
Chenodeoxycholic acid
- DCA:
-
Deoxycholic acid
- DIMI:
-
Diminazene
- ENaC:
-
Epithelial Na+ channel
- FFA:
-
Flufenamic acid
- HDCA:
-
Hyodeoxycholic acid
- HyNaC:
-
Hydra Na+ channel
- INaC:
-
Intestine Na+ channel
References
Chen X, Qiu L, Li M, Durrnagel S, Orser BA, Xiong ZG, MacDonald JF (2010) Diarylamidines: high potency inhibitors of acid-sensing ion channels. Neuropharmacology 58:1045–1053
Diakov A, Korbmacher C (2004) A novel pathway of epithelial sodium channel activation involves a serum- and glucocorticoid-inducible kinase consensus motif in the C terminus of the channel’s alpha-subunit. J Biol Chem 279:38134–38142
Diakov A, Bera K, Mokrushina M, Krueger B, Korbmacher C (2008) Cleavage in the {gamma}-subunit of the epithelial sodium channel (ENaC) plays an important role in the proteolytic activation of near-silent channels. J Physiol 586:4587–4608
Fisher MM, Yousef IM (1973) Sex differences in the bile acid composition of human bile: studies in patients with and without gallstones. Can Med Assoc J 109:190–193
Haerteis S, Krueger B, Korbmacher C, Rauh R (2009) The delta-subunit of the epithelial sodium channel (ENaC) enhances channel activity and alters proteolytic ENaC activation. J Biol Chem 284:29024–29040
Haerteis S, Krappitz M, Diakov A, Krappitz A, Rauh R, Korbmacher C (2012) Plasmin and chymotrypsin have distinct preferences for channel activating cleavage sites in the gamma subunit of the human epithelial sodium channel. J Gen Physiol 140:375–389
Jasti J, Furukawa H, Gonzales EB, Gouaux E (2007) Structure of acid-sensing ion channel 1 at 1.9 A resolution and low pH. Nature 449:316–323
Kellenberger S, Schild L (2002) Epithelial sodium channel/degenerin family of ion channels: a variety of functions for a shared structure. Physiol Rev 82:735–767
Korbmacher C, Volk T, Segal AS, Boulpaep EL, Fromter E (1995) A calcium-activated and nucleotide-sensitive nonselective cation channel in M-1 mouse cortical collecting duct cells. J Membr Biol 146:29–45
Krueger B, Haerteis S, Yang L, Hartner A, Rauh R, Korbmacher C, Diakov A (2009) Cholesterol depletion of the plasma membrane prevents activation of the epithelial sodium channel (ENaC) by SGK1. Cell Physiol Biochem 24:605–618
Nilius B, Prenen J, Droogmans G, Voets T, Vennekens R, Freichel M, Wissenbach U, Flockerzi V (2003) Voltage dependence of the Ca2+-activated cation channel TRPM4. J Biol Chem 278:30813–30820
Rauh R, Diakov A, Tzschoppe A, Korbmacher J, Azad AK, Cuppens H, Cassiman JJ, Dotsch J, Sticht H, Korbmacher C (2010) A mutation of the epithelial sodium channel associated with atypical cystic fibrosis increases channel open probability and reduces Na+ self-inhibition. J Physiol 588:1211–1225
Sakai H, Lingueglia E, Champigny G, Mattei MG, Lazdunski M (1999) Cloning and functional expression of a novel degenerin-like Na+ channel gene in mammals. J Physiol 519(Pt 2):323–333
Schaefer L, Sakai H, Mattei M, Lazdunski M, Lingueglia E (2000) Molecular cloning, functional expression and chromosomal localization of an amiloride-sensitive Na(+) channel from human small intestine. FEBS Lett 471:205–210
Springauf A, Gründer S (2010) An acid-sensing ion channel from shark (Squalus acanthias) mediates transient and sustained responses to protons. J Physiol 588:809–820
Stewart AP, Haerteis S, Diakov A, Korbmacher C, Edwardson JM (2011) Atomic force microscopy reveals the architecture of the epithelial sodium channel (ENaC). J Biol Chem 286:31944–31952
Waldmann R, Champigny G, Bassilana F, Heurteaux C, Lazdunski M (1997) A proton-gated cation channel involved in acid-sensing. Nature 386:173–177
Wiemuth D, Gründer S (2010) A single amino acid tunes Ca2+ inhibition of brain liver intestine Na+ channel (BLINaC). J Biol Chem 285:30404–30410
Wiemuth D, Gründer S (2011) The pharmacological profile of brain liver intestine Na+ channel: inhibition by diarylamidines and activation by fenamates. Mol Pharmacol 80:911–919
Wiemuth D, Sahin H, Falkenburger BH, Lefevre CM, Wasmuth HE, Gründer S (2012) BASIC – a bile acid-sensitive ion channel highly expressed in bile ducts. FASEB J 26:4122–4130
Wiemuth D, Sahin H, Lefevre CM, Wasmuth HE, Gründer S (2012) Strong activation of bile acid-sensitive ion channel (BASIC) by ursodeoxycholic acid. Channels (Austin) 7:38–42
Acknowledgments
We thank A. Oslender-Bujotzek, L. Pieper and R. Rinke for expert technical assistance. This project was supported by the START-program of the Faculty of Medicine of RWTH Aachen University (grant AZ 36/11 to DW) and a grant from the ‘Johannes und Frieda Marohn-Stiftung’ (grant BASIC to CK).
Author information
Authors and Affiliations
Corresponding author
Additional information
Cathérine M.T. Lefèvre and Alexei Diakov contributed equally to this work
Rights and permissions
About this article
Cite this article
Lefèvre, C.M.T., Diakov, A., Haerteis, S. et al. Pharmacological and electrophysiological characterization of the human bile acid-sensitive ion channel (hBASIC). Pflugers Arch - Eur J Physiol 466, 253–263 (2014). https://doi.org/10.1007/s00424-013-1310-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00424-013-1310-4