Abstract
The sulfonylurea receptors (SURs) ABCC8/SUR1 and ABCC9/SUR2 are members of the C-branch of the transport adenosine triphosphatase superfamily. Unlike their brethren, the SURs have no identified transport function; instead, evolution has matched these molecules with K+ selective pores, either KIR6.1/KCNJ8 or KIR6.2/KCNJ11, to assemble adenosine triphosphate (ATP)-sensitive K+ channels found in endocrine cells, neurons, and both smooth and striated muscle. Adenine nucleotides, the major regulators of ATP-sensitive K+ (KATP) channel activity, exert a dual action. Nucleotide binding to the pore reduces the activity or channel open probability, whereas Mg-nucleotide binding and/or hydrolysis in the nucleotide-binding domains of SUR antagonize this inhibitory action to stimulate channel openings. Mutations in either subunit can alter this balance and, in the case of the SUR1/KIR6.2 channels found in neurons and insulin-secreting pancreatic β cells, are the cause of monogenic forms of hyperinsulinemic hypoglycemia and neonatal diabetes. Additionally, the subtle dysregulation of KATP channel activity by a KIR6.2 polymorphism has been suggested as a predisposing factor in type 2 diabetes mellitus. Studies on KATP channel null mice are clarifying the roles of these metabolically sensitive channels in a variety of tissues.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The adenosine triphosphate (ATP)-sensitive K+ (KATP) channel area has been widely, some would say over, reviewed during the past dozen years. Our intention here is to comment on recent studies with an emphasis on ABCC8 and not reiterate material covered in recent extensive reviews on the muscle-type KATP channels [74, 92, 99, 101, 134, 144].
Background
Adenosine-triphosphate-sensitive K+ channels are responsive to changes in ATP/adenosine diphosphate (ADP) and provide a means to couple movement of potassium ions and, thus, membrane potential to cellular energy status. Metabolic control of membrane potential is a key factor in the regulation of the Ca2+ triggering signals that underlie glucose homeostasis both in the endocrine pancreas and in the central nervous system (CNS). Genetic mutations that disrupt this control lead to a spectrum of changes, mild to severe, in blood glucose levels and energy balance, underscoring the importance of this dominant network.
Adenosine-triphosphate-sensitive K+ channels are assembled from two different subunits: A KIR6.x subunit that forms the ion-conducting pore and a sulfonylurea receptor (SUR), a member of the ABCC subfamily, with affinity for hypoglycemic sulfonylureas (e.g., the channel antagonists tolbutamide and glibenclamide) and hyperglycemic channel agonists (e.g., diazoxide, pinacidil, and cromakalim). KATP channels are obligate hetero-octamers (SUR/KIR6.x)4, whose subunit activities are highly integrated (34, 70, 138; see 2, 27 for review). Ordinarily, neither subunit will reach the cell surface in the absence of its partner. Trafficking from the endoplasmic reticulum to the cell surface is regulated by arginine-rich RKR motifs on both subunits [157] in combination with a C-terminal signal on SUR [136]. These motifs insure the correct assembly of full-length subunits necessary for channel surface expression. The quality control mechanism is not fully understood, but interaction(s) with 14-3-3 proteins are reported to play a role (156; see 96, 107 for review).
The SUR and KIR6.x subunits are the products of two pairs of genes: ABCC8 [SUR1; Online Mendelian Inheritance in Man (OMIM) 600509] is paired with KCNJ11 (KIR6.2; OMIM 600937), which is approximately 5 kb downstream (3′ of ABCC8) on the short arm of human chromosome 11 (11p15.1). ABCC9 (SUR2; OMIM 601439), on the short arm of chromosome 12 (12p12.1), is separated from KCNJ8 (KIR6.1; OMIM 600935) by approximately 26.2 kb. These ABCC genes specify three major SUR isoforms (see 1 for review). SUR1, the receptor with the highest affinity for sulfonylureas, is commonly assembled with KIR6.2, and (SUR1/KIR6.2)4 channels are broadly distributed in the neuroendocrine system. Inhibition of pancreatic β-cell KATP channels by sulfonylurea and nonsulfonylurea hypoglycemic agents, which results in insulin secretion secondary to β-cell depolarization and increased intracellular Ca2+ levels, is the primary mechanism of action of these compounds. Differential splicing of the terminal exon of the ABCC9 gene produces two SUR2 isoforms: SUR2A, paired with KIR6.2 to assemble the KATP channels found in cardiac and skeletal muscle cells, and SUR2B, which assembles with KIR6.1 to make KATP channels in smooth muscle, particularly in parts of the vasculature where they participate in maintenance of vascular tone (see 69 for brief review).
KIR6.x subunits are members of the inward rectifier superfamily
The KIR6.x pores are K+ selective and conduct K+ better into cells than out and are termed “inward rectifiers.” Like other members of the KIR superfamily, KIR6.2 subunits assemble tetramers in which four M2 helices line the permeation pathway and converge to form a gate at the cytoplasmic face of the pore [42]. In crystallographic structures, the outward-facing M1 helices appear accessible for interaction. A submembrane helix termed “the slide helix” immediately precedes and forms approximately a right angle with the M1 helix (illustrated in Fig. 1). By analogy with a proposed mechanical mechanism for regulation of Kv channels [89], motions of this submembrane helix would reposition M1 and M2 to effect gating (see 5 for review).
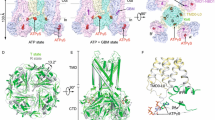
Topology and homology model of KATP channels. (a) The KIR6.x and SUR topologies are illustrated schematically. The amino (N) and carboxyl (C) termini are marked. A and B symbolize the Walker A and B consensus motifs in the two NBDs, respectively. The triangles show the approximate positions of glycosylation sites required for correct trafficking. (b) A homology model for KATP channels. The KIR6.2 model is based on the structures of KirBac1.1 [82] and the carboxy terminus of the KIR3.1 subunit [110]; the model of the SUR core is based on the VC-MsbA-dimer [32]. A detailed description is given in Refs. [7, 26]. The GFG sequence (green) and ball identify the pore selectivity filter and a K+ ion, respectively. TMS sequences in the KIR outer helix, important for association with SUR [132], are shown in red or pink to distinguish neighboring subunits. The bundle of five red cylinders symbolizes TMD0 for which no structural template is available. L0 is illustrated by horizontal red cylinders and connected blue loops, and is positioned to interact with the distal residues of the KIR amino termini in blue. Interactions between domains colored red or pink activate the pore, whereas interactions involving blue domains attenuate the POmax. Gold and yellow residues in the KIR cytoplasmic domains identify ATP-binding sites in neighboring subunits. For the purpose of size comparison, iodo-azidoglibenclamide in an extended conformation is shown on the right. The cyan residue in the lower left is S1237, important for sulfonylurea binding [4]. Two side chains on TM 17 (T1286 and M1290), important for interactions of the channel with openers [103], are in brown. Panel (b) is modified from Ref. [26]
Multiple studies have shown that engineered KIR6.x subunits can assemble functional pores in the absence of a SUR, and that their activity is sensitive to ATP [8, 43, 150]. Biochemical studies have demonstrated ATP binding to the large C-terminal domain [147, 148, 151]. Recent studies have used the coordinates of bacterial K+ channels [42, 82, 110] to make homology models the KIR6.x pore and provide novel information on the adenine-selective, nucleotide-diphosphate-binding pocket, which is composed of residues from both the N- and C-termini (7, 29; reviewed in 5). Based on modeling and earlier analysis of a KIR6.2 mutant channel with substitutions in both the KIR N- and C-termini [9], we proposed a specific model where the amino and carboxy termini that comprise the nucleotide binding site are from adjacent KIR subunits [7]. This model implies that inter-KIR subunit coupling contributes to the concerted transitions characteristic of KATP channels.
Sulfonylurea receptors are typical ABC proteins
The SURs are multidomain proteins with a topology similar to other ABC proteins, including the classic ABC “core” consisting of two bundles of six transmembrane helices (TMD1 and 2) with nucleotide-binding domains (NBD1 and 2) C-terminal to each TMD (Fig. 1). The SURs, and several other ABCC proteins (i.e., ABCC1, 2, 3, 6, and 10), have an additional amino terminal module that consists of a bundle of five transmembrane helices (TMD0) connected to the core via an intracellular linker termed “L0.” In ABCC8 and 9, TMD0-L0 is the principal domain interacting with the KIR subunit as discussed below. The SUR NBDs contain the canonical phosphate-binding Walker A and B motifs, the Q-loop, the signature sequence, and the H-loop, hallmarks of the ABC family. The SURs were among the first ABC proteins recognized to have degenerate, nonsymmetric NBDs with a noncanonical signature sequence, FSQGQ vs LSGGQ, in NBD2 and an aspartate (D) in place of the usual glutamate (E) adjacent to the highly conserved D in the Walker B motif. Early studies on SUR1, without a KIR, indicated tight binding of 8-azido ATP and affinity labeling of NBD1, irrespective of the presence of Mg2+, with no indication of hydrolysis. Mg2+ potentiated nucleotide binding in NBD2 where hydrolysis is thought to occur (93, 94, 97; reviewed in 92). Although not yet explicitly demonstrated, by analogy with other ABC proteins reviewed in this issue of Pflügers Archives, ATP binding and hydrolysis are expected to drive dimerization of the SUR NBDs and produce concomitant rearrangements of TMD1 and TMD2 [154]. In other ABC proteins, these rearrangements are associated with substrate transport, whereas in KATP channels, the challenge is to understand how they are coupled to the gating mechanism of the KIR6.x pore (see 104, 158 for discussion of specific models).
Drug binding sites
SURs are the targets for various compounds that bind and either stimulate or inhibit KATP channel activity. We [26] and others [72, 104, 118, 120] have reviewed this area recently. Therapeutic agents, like tolbutamide, glibenclamide, glipizide, glimeperide, nateglinide, repaglinide, etc., which antagonize the activity of the SUR1/KIR6.2 β-cell channels, are perhaps best known because of their wide use as hypoglycemic agents that restore first phase of insulin secretion in patients with type 2 diabetes. Extensive effort has gone into understanding their pharmacophore structure and the mechanism of action of these compounds along with the location of the binding site. Current evidence suggests the binding site is an extended pocket on the cytoplasmic side of the receptor, which involves residues from TMD2 and L0 and the amino terminus of KIR6.2. The binding of sulfonylureas to SUR1/KIR6.2 channels has a dual effect, partially inhibiting channel activity in the absence of nucleotides and abolishing the stimulatory action of SUR1 on the pore in the presence of Mg nucleotides. Potassium channel openers (KCOs), like diazoxide, have been used to hyperpolarize β cells and reduce insulin release, whereas openers specific for SUR2 have long been sought in an effort to control the excitability of cardiac and vascular smooth muscle (see 120 for review). Amino acid residues in TMD2, in what appears to be a cavity in the homology models of the SUR ABC core, markedly affect KCO binding (Fig. 1b; 38, 102, 103; see 104 for review). Although the properties of these binding sites, and the effects of nucleotide binding and hydrolysis, are not as well studied as the classical ABC drug transporters, the structural parallels are clear.
Modulators
Various compounds have been shown to modulate KATP channel activity, particularly phosphoinositides (20, 52, 121, 130, 140; see 19 for review), long-chain acyl coenzyme As (CoAs) derived from fatty acids [23–25, 121], G proteins (127; but see 13), and phosphorylation (see 88 for review). The functions of these modulators are potentially important, but in most cases, their physiologic role(s) are only beginning to be firmly established. Lower pH has been reported to activate KATP channels by reducing their sensitivity to inhibitory ATP and may play a role in the regulation of vascular tone during hypercapnic acidosis [153]. Several recent studies [18, 22, 119] have shown that Zn2+, cosecreted with insulin and present in high concentrations in areas of the CNS, can activate ATP-inhibited SUR1/KIR6.2 KATP channels via binding to two histidines on the extracellular face of SUR1 [17]. In pancreatic islets, Zn2+ is coreleased with insulin, where it may play an autocrine role or serve to attenuate glucagon release from α cells [56, 71].
Assembly
The pathway(s) of KATP channel assembly are poorly understood. In studying the turnover of individual subunits expressed in COSm6 cells, we observed that SUR1 expressed alone appeared to be long-lived, whereas KIR6.2 subunit turnover was biphasic [36]. We inferred that the slow phase represented assembly of stable KIR6.2 tetramers, whereas the rapid phase was due to degradation. Coexpression with SUR1 eliminated the rapid phase, and SUR1/KIR6.2 complexes were detectable at the earliest time points in pulse-chase experiments. The results are consistent with the hypothesis that during or shortly after their biogenesis, SUR1 and KIR6.2 rapidly dimerize, protecting KIR6.2 from degradation. The SUR1/KIR6.2 dimers then assemble the octameric complex [36]. The results are summarized in Fig. 2.
Summary of KATP channel assembly. Based on turnover studies, KIR monomers are hypothesized to assemble slowly into tetrameric pores. In the absence of SUR, the KIR monomers are degraded rapidly, whereas tetramers are long-lived. When the subunits are coexpressed, the immature core glycosylated form of SUR1 assembles rapidly with KIR6.2. Maturation to a functional channel has a half-time of approximatey 2.2 h and involves multiple steps, including completion of channel assembly, transit through the Golgi complex, and the addition of sialic acid residues. The estimated half-life for the complete, fully glycosylated channel is approximately 7.3 h. The figure is based on Ref. [36]
The TMD0-L0 domain links the SUR ABC core with the pore
Recent studies have emphasized the role of the TMD0-L0 module in both the assembly and regulation of KATP channels. In some ABCC proteins TMD0 is required for correct trafficking [53, 91], whereas in MRP1, L0, but not TMD0, is required for transport activity [15] and is part of the glutathione binding site [75]. Coexpression of SUR1 TMD0 with poorly active (KIR6.2)4 pores demonstrated partial restoration of function, including an increase in their maximum channel open probability (POmax) and the restoration of bursting activity; immunoprecipitation experiments confirmed TMD0 forms complexes with KIR6.2 [7, 31]. TMD0 consists primarily of transmembrane helices, and the idea that one or more TMD0 helices interact with the KIR M1 helix is supported by experiments with chimeric KIR subunits [132] and the observation that KIR6.2 N-terminal fragments containing M1, but not M2 and the C-terminal domain, interact with SUR1 [27]. Because of their smaller size, we termed the TMD0/KIR6.2 complexes “mini-KATP” channels and referred to the TMD0-L0 module as a “gatekeeper.” These mini channels lack many of the defining characteristics of full channels and are not sensitive to sulfonylureas, are not stimulated by Mg nucleotides, and retain the reduced sensitivity to inhibitory ATP characteristic of (KIR6.2)4 pores. Additionally, TMD0 does not support the trafficking of KIR6.2 with an intact ER retention motif to the cell surface, implying that these properties of the full channel require interactions between the TMD0-KIR pore complex and the ABC core [7].
L0 and the KIR amino terminus are critical elements of the transduction mechanism
Early studies with chimeric receptors showed that L0 played a critical role in specifying gating differences between SUR1-based neuroendocrine vs SUR2-based muscle-type KATP channels [11]. Analysis of the mini-KATP channels underscored the importance of L0 in the control of gating. The progressive inclusion of L0 sequence into mini-KATP channels identified a proximal stimulatory segment that stabilized the pore in a continuous bursting mode [7]. This proximal segment contains a conserved, predicted amphipathic helix [5]; a similar sequence in MRP1 is important for transport [14]. The inclusion of more distal segments of L0 attenuated the strong stimulatory effect. The results implied that the TMD0-L0 pore complex had all of the structural elements necessary to affect bidirectional control of gating and dovetailed nicely with studies showing that the initial N-terminus of KIR6.2 plays a critical role in limiting the length of time a KATP channel remains in an open bursting configuration. For example, the deletion of the KIR6.2 amino terminus [9, 79] or the application of a synthetic N-terminal peptide [6] produced channels that burst continuously, suggesting that interaction(s) between the N terminus and a putative binding site on SUR limited burst length. We developed a model in which stimulatory interactions between the proximal helical segment of L0 and the KIR6.2 slide helix are balanced by inhibitory interactions between the more distal half of L0 and the initial N terminus of KIR6.2 (6, 7, 10; reviewed in 5, 27). In this quasimechanical model, the dimerization or reconfiguration of the ABC core as a consequence of ATP binding and hydrolysis is presumed to exert a force that repositions L0 to affect channel gating by moving the slide helix and, thus, M1 and M2. The movements are analogous to those proposed to affect gating in voltage-gated Kv1.2 channels, where changes in membrane potential produce a conformational change in the voltage sensor that moves the S4-S5 linker and repositions S5 and S6 to open or close the gate [89].
Dual regulation of KATP channel activity by adenine nucleotides
In most ABC proteins, hydrolysis of ATP is assumed to power substrate transport across the cell membrane. In KATP channels, adenine nucleotides can bind to both the KIR and SUR subunits and exert inhibitory and stimulatory actions, respectively. The binding of ATP or ADP to KIR6.x subunits reduces channel activity. This binding and inhibitory action are Mg2+-independent and do not require hydrolysis. The stimulatory action of SURs, on the other hand, is Mg-nucleotide-dependent, and nucleotide binding and hydrolysis increases the activity of the ATP-inhibited pore.
In pancreatic β cells, the glycolytic pathway is critically involved in signaling increases in glucose metabolism to KATP channels [46, 90, 95]. The nicotinamide adenine dinucleotide (reduced form; NADH) equivalents derived from glycolysis are transferred into mitochondria via the glycerol-phosphate, dihydroxyacetone-phosphate, and malate-aspartate shuttles. Blockage of either shuttle alone has little effect on glucose-stimulated insulin secretion, whereas blockage of both pathways in mitochondrial glycerol-phosphate dehydrogenase null mice [50, 51] strongly inhibits first-phase insulin release and abolishes second-phase secretion in response to elevated glucose. How the NADH equivalents from glycolysis, via generation of ATP, inhibit KATP channels has not been established, but the results suggest that β-cell KATP channels are not sensing “bulk” cytosolic [ATP]i. One idea is that specific respiratory chains couple the malate-aspartate and glycerol-phosphate NADH shuttles to a mitochondrial creatine kinase which transfers phosphate from matrix ATP to creatine to produce creatine phosphate [80]. The creatine phosphate is then converted to ATP at or near KATP channels. This hypothesis is supported by reports that SUR2A, the regulatory subunit of KIR6.2/SUR2A KATP channels found in striated muscle, is physically associated with creatine kinase [37].
KATP channel pathologies
Multiple genetic disorders of glucose homeostasis and cardiovascular tone have been associated with mutations in KATP channel subunits. KCNJ8 has been suggested as a candidate gene for Prinzmetal angina based on the phenotype of the KIR6.1KO mouse [100], but human mutations have yet to be identified [49]. ABCC9 has not been linked to single-gene disorders at this time, but it has been associated with dilated cardiomyopathy [21].
Hyperinsulinemic hypoglycemia
Mutations in SUR1 and KIR6.2 are an established cause of hyperinsulinemic hypoglycemia of infancy (HI), characterized by excess insulin release for the degree of hypoglycemia (see 1 for review). More than 40 mutations in KCNJ11 and more than 100 ABCC8 mutations have been identified in patients with HI that lead to loss of channel function by affecting subunit assembly and channel trafficking [30, 36, 136, 149] or, in the case of some ABCC8 missense mutations, by impairing the Mg-nucleotide-dependent stimulation of the pore by SUR1 (109, 139; reviewed in 55). The neuroendocrine SUR1/KIR6.2-type KATP channels are a key regulator of membrane potential; thus, their loss in HI individuals abolishes the ability of pancreatic β cells to hyperpolarize when glucose is reduced and, thus, suppress insulin release. This uncoupling results in excess insulin release that produces hypoglycemia. There is no known therapeutic strategy to enhance folding, assembly, or trafficking of mutant subunits, and these cases often require surgical intervention. Many individuals with missense mutations are responsive to diazoxide, a K+ channel opener, or to octreotide, a somatostatin analog, and can be treated pharmacologically.
Neonatal diabetes
Recent studies on the genetic basis of neonatal diabetes (ND) have confirmed the observation in transgenic mice [78] that expression of “overactive” KATP channels results in neonatal hyperglycemia secondary to reduced insulin secretion. Although ND is a rare genetic disorder (estimated at ∼1/400,000 births) [117], these findings are important because they confirm the general ionic mechanism and how that increased KATP channel activity and, thus, more hyperpolarized β cells result in a decrease in insulin release. Multiple mutations in KIR6.2 have been found to produce ND (59, 152; reviewed in 66, 143). Although various structural alterations can be anticipated that would result in more active channels, several of the reported KIR6.2 mutations reduce the apparent affinity for inhibitory ATP, thus leading to more active channels at a given nucleotide level [59, 152]. Although these mutations are dominant, simulating heterozygosity by expression of 1:1 mixtures of mutant, for example, the R201H mutation, and wild-type KIRs with SUR1 yielded a population whose inhibition by ATP was essentially indistinguishable from wild-type channels. The results suggest that the small percentage of homozygous mutant channels, expected to arise from random assortment during assembly of the pore, is sufficient to hyperpolarize β cells. Many of the ND-KIR6.2 mutant channels retain their sensitivity to sulfonylureas, allowing patients to be switched from insulin to sulfonylurea therapy [126].
The dual action of nucleotides on KATP channels outlined above anticipated SUR “gain-of-function” mutations having an enhanced stimulatory action on the pore. Sequencing of the ABCC8 gene in a small population of patients diagnosed with ND, from the French Network for the Study of Neonatal Diabetes Mellitus for Genetic Diagnosis, identified seven mutations that segregated with the disorder [12]. Analysis of two SUR1 mutant channels, I1424V or H1023Y, demonstrated they were more active than wild-type channels both in on-cell recordings from intact mammalian cells and in isolated patches exposed to a quasiphysiologic concentration of MgATP (1 mM). In the absence of Mg2+, when the stimulatory action of SUR1 on the pore was abolished, there was no significant difference in the ATP inhibitory curves of mutant and wild-type channels, indicating the I1424V or H1023Y receptors exert an enhanced stimulatory action on the pore. The simulation of heterozygosity by expression of 1:1 mixtures of ND-SUR1 H1023Y and wild-type SUR1 with KIR6.2 produced average mean channel activities intermediate between the “homozygous” mutant and wild-type channels. The mutant ND-SUR1 channels are inhibited by sulfonylureas, allowing patients to substitute oral hypoglycemic agents for insulin therapy.
Type 2 diabetes
Hyperinsulinemic hypoglycemia and ND are clear examples of rare monogenic disorders of glucose homeostasis that provide insight into the regulation of insulin secretion. Genetic studies indicate KATP channels also may have a role in type 2 diabetes mellitus. Several studies (for example, 54, 60, 63; reviewed in 124) indicate a polymorphism, E32K, in the amino terminus of KIR6.2 is a risk factor for type 2 diabetes. This KIR6.2 polymorphism has a subtle activating effect on KATP channel activity and is reported to reduce sensitivity to inhibitory ATP [131] and increase the stimulatory action of long-chain acyl CoAs [122], particularly long-chain, saturated acyl CoAs [123].
Transgenic mouse models
All of the subunits of KATP channels, including SUR1, SUR2, KIR6.1, and KIR6.2, have been deleted in mice and their phenotypes studied. This area, particularly with respect to KATP channels in muscle, has been reviewed recently [99], and in the interest of space, we focus on the results with Sur1KO animals. Two independent SUR1 null mouse lines have been generated. Seghers et al. [133] replaced exon 2 with puromycin-N-acetyl-transferase, whereas Shiota et al. [137] used a cre recombinase strategy to delete exon 1, leaving a neomycin resistance cassette. Neither strain produces SUR1, and as expected, both strains lack SUR1/KIR6.2-type KATP channels, with no studies showing upregulation of SUR2 subunits and compensatory ionic currents.
We initially developed Sur1KO mice as a potential animal model for the study of HI but unexpectedly found that the mice exhibited normal plasma glucose and insulin levels unless stressed [133], whereas in HI neonates, the loss of KATP channel activity can produce severe hypoglycemia secondary to excess insulin release. The early electrophysiological studies done on isolated β cells from HI neonates using the patch clamp technique demonstrated a loss of KATP channel activity and persistent Ca2+-dependent action potentials consistent with their excessive insulin release [47, 73]. Similar analyses on isolated Sur1KO β cells identified a similar electrophysiological phenotype with loss of KATP channels, persistent Ca2+-dependent action potentials, and elevated and slowly oscillating [Ca2+]c, although in contrast to HI neonates, the knockout animals have normal blood sugar and insulin levels [44, 133, 137]. Later membrane potential measurements on Sur1KO β cells with intracellular microelectrodes revealed an oscillatory pattern (Fig. 3; 44, 65). These papers introduce a cautionary note: membrane potential estimates derived from patch clamp measurements in isolated β cells can differ substantively from those made on β-cell clusters and islets. The results suggest that β cells in Sur1KO mice are probably not persistently depolarized but are rather oscillating, similar to the behavior of wild-type β cells.
Recording of plasma membrane potential using intracellular microelectrodes on intact islets. (a) Wild-type (WT) islets from C57Bl/6 mice in the presence of 3, 15, and 25 mmol/l glucose. (b–d) Continuous oscillations in Sur1KO islets perifused with 0.5, 15, 25, and 40 mmol/l glucose. Record (d) is the direct continuation of (c). The recordings are representative of five (a), nine (b), eight (c), and four (d) experiments. The figure is from Düfer et al. [44]
Newborn Sur1KO mice were found to exhibit significant hypoglycemia secondary to hyperinsulinemia, but this resolved within several days [133], and the KO animals then remain normoglycemic [65, 108, 133]. Intraperitoneal glucose tolerance tests on adult mice showed that knockout animals fail to release insulin in response to a glucose challenge [133, 137], whereas fasted knockout animals are able to secrete insulin in response to feeding [137] consistent with stimulation via the CNS.
Secretion studies on isolated islets have produced divergent results, with some reports consistent with enhanced insulin release, whereas others were consistent with a defect in insulin secretion. Seghers et al. [133] showed a loss of first phase and an attenuated second phase of insulin secretion in response to a glucose challenge. Using animals from the same colony, Nenquin et al. [108] showed increased insulin release from isolated Sur1KO vs WT islets in low glucose (1 mM) consistent with the elevated Ca2+ triggering signal. This study confirmed the lack of first-phase response and showed further that increasing glucose metabolism stimulated insulin release, demonstrating the augmentation pathway (see 67, 68 for review) is intact in the Sur1KO animals. Similar glucose-stimulated insulin secretion was reported by Haspel et al. [65], and Muñoz et al. [105] showed increased insulin release from Sur1KO islets in low glucose plus amino acids. Studies on the Sur1KO animals generated by Shiota et al. [137] have usually failed to show insulin secretion under hypoglycemic conditions or a significant increase in secretion when glucose is elevated, thus leading to the conclusion that loss of SUR1 impairs insulin release [41, 87], although Eliasson et al. [48] reported glucose-stimulated insulin release using this strain. These divergent results with isolated islets, excessive insulin release in low glucose and increased secretion upon increasing glucose vs generally impaired insulin secretion, have suggested opposite compensatory mechanisms must operate to account for the normal insulin and blood sugar levels seen in the knockout animals. Nenquin et al. [108] suggested the need for a mechanism to suppress the excessive insulin release seen in low glucose, whereas Doliba et al. [41] argue for an enhanced stimulation via a neural mechanism.
Role of KATP channels in the generation of Ca2+ and electrical oscillations
A signature feature of islets in elevated glucose is a tight coupling between oscillations of β-cell membrane potential and [Ca2+]c that trigger pulsatile insulin release [58, 129]. Several mechanisms proposed to account for the generation of these oscillations involve the response of KATP channels to changes in ATP/ADP (see, for example, 40, 81). Using intracellular microelectrode recording techniques, Düfer et al. [44] showed that Sur1KO islets exhibit Vm and [Ca2+]c oscillations in 15 mM glucose, which, in contrast to wild-type islets, persist in 0.5 mM glucose, implying KATP channels are not essential for oscillation. The microelectrode experiments showed that the electrical activity of Sur1KO β cells in islets was modulated by glucose as illustrated in Fig. 3. In contrast to wild-type β cells, the application of sodium azide did not result in hyperpolarization of Sur1KO β cells but did reduce the amplitude of Ca2+-dependent action potentials by directly inhibiting Ca2+ channels [44, 45]. Neither tolbutamide nor diazoxide had any effect on Vm oscillations in KATP null islets. The activation of a low-conductance, Ca2+-dependent K+ current, termed “IKslow,” has been implicated in the oscillatory activity of wild-type β cells [61, 62]. Haspel et al. [65] showed that Sur1KO β cells have a similar Ca2+-dependent K+ current that is inhibited when [Ca2+]c is reduced using D600, an l-type Ca2+ channel blocker, and stimulated using BayK 8644, a Ca2+ channel opener. KATP channels control oscillations of Vm and [Ca2+]c in wild-type β cells, but a secondary oscillatory mechanism must exist in Sur1KO cells. We presume the two mechanisms are not active in parallel because blocking KATP channels acutely with 100 μM tolbutamide does not induce oscillations in [Ca2+]c [128].
Multiple compensatory mechanisms have been suggested to explain the large difference in glucose homeostasis between the HI neonates and the rodent models. Interestingly, several mouse models that exhibit partial loss of SUR1/KIR6.2 channel activity exhibit hypoglycemic phenotypes, which more nearly approximate the human disorder [64, 85].
The incretin response is impaired in Sur1KO mice
Glucagon-like peptide 1 (GLP-1), secreted in response to feeding, is known to potentiate glucose-stimulated insulin secretion via an increase in cyclic adenosine monophosphate (cAMP). Shiota et al. [137] showed that Sur1KO mice failed to increase their plasma insulin in response to exogenous GLP-1, and Nakazaki et al. [106] demonstrated that, whereas GLP-1, gastric inhibitory peptide (GIP), and exendin 4 increased the cAMP level in isolated islets, their potentiation of glucose-stimulated insulin release was reduced. The impaired incretin response was secondary to a blunted response to elevated cAMP acting via a protein kinase A (PKA)-independent pathway [48, 106]. The impaired response was specific for cAMP, and Sur1KO islets were stimulated by carbachol, a nonhydrolyzable analog of acetylcholine, and by tissue plasminogen activator (TPA), a protein kinase C (PKC) activator. In low glucose, stimulation by carbachol and TPA was more pronounced in Sur1KO vs wild-type islets, presumably due to the elevated oscillating [Ca2+]c. Using a yeast two-hybrid approach, Ozaki et al. [114] demonstrated an interaction between a fragment of SUR1 containing NBD1 and Epac-2 (cAMP-GEFII), a cAMP-binding guanine-nucleotide exchange factor [39, 77] and showed that Epac-2 interacted with Rim2, a member of a family of proteins that promote priming of granules for release in neurons (see 135 for review). These findings, coupled with the observation that the membranes of insulin containing dense core vesicles are rich in KATP channels [57], has led to models in which interactions between SUR1, Epac-2, RIM2, and various other proteins serve bridging functions between the plasma membrane and dense core vesicles (for example, 48, 135). These models are attractive as a means to explain how cAMP can potentiate exocytosis and why there is a blunted response to cAMP in Sur1KO animals. We have attempted to extend these results and have confirmed the interaction between NBD1 and Epac-2 (Fig. 4). However, we have been unable to demonstrate an interaction between Epac-2 and full-length SUR1 or SUR1/KIR6.2, suggesting either that the interaction with a single NBD is nonspecific or that other proteins are involved.
Interaction of SUR1 NBD1, but not full-length SUR1, with Epac2. (a) Immunoprecipitation (IP) of myc-tagged SUR1 NBD1 with HA-tagged Epac2, a kind gift from Professor Johannes Bos. Constructs were expressed in COSm6 cells in combination as indicated, Triton X-100 (0.1%) cleared lysates were prepared and immunoprecipitated with an anti-myc antibody, solubilized in SDS, and blotted with anti-HA antibody. (b) Equivalent lysates were added to cAMP-agarose beads or precipitated with anti-myc antibodies. The beads or precipitates were washed, solubilized, separated by SDS–PAGE, then blotted with either anti-myc or anti-HA antibodies. NBD1 from mrp1 is given as a control. (c) COSm6 cells were transfected with HA-Epac2 and full-length myc-tagged SUR1. Cleared lysates were prepared as above and either precipitated with anti-myc antibodies or cAMP agarose beads. The beads or precipitates were washed, solubilized, separated by SDS–PAGE, then blotted with either anti-myc or anti-HA antibodies. (d) COSm6 cells were transfected with SUR1 or SUR1 plus HA-Epac2. SUR1 was specifically affinity-labeled with 125I-azidoglibenclamide [34], and cleared lysates were prepared as above and incubated with cAMP agarose beads. The starting material (Tot), unbound fraction (Un), and bound material (Bd) were collected, separated by SDS–PAGE, and subject to autoradiography. There is a strong interaction with NBD1 (same fragment as 114), a weak interaction with NBD2, and no detectable interaction with NBD1 from MRP1 or with full-length SUR1
Catecholamine response in Sur1KO mice
Sieg et al. [141] explored the idea that elevated epinephrine might act to suppress insulin release in Sur1KO mice. Others have implied that the inhibitory action of epinephrine on insulin secretion might involve activation of KATP channels, but exogenous epinephrine hyperpolarized Sur1KO β cells via an α2-adrenoceptor mechanism, thus inhibiting insulin secretion from isolated islets and suppressing carbachol-induced insulin release in Sur1KO mice. The molecular nature of the low conductance, BaCl2-sensitive K+ channels regulated by pertussis-sensitive G proteins associated with β-cell hyperpolarization is not known [141]. Preliminary measurements of catecholamine levels in Sur1KO vs wild-type mice have not uncovered any significant differences (unpublished data); therefore, we tentatively conclude that suppression of insulin release via elevated epinephrine does not tonically suppress insulin secretion in the knockout animals, but further study is warranted.
Acetylcholine and amino acids
Shiota et al. [137] showed that fasted Sur1KO mice increase their insulin level in response to feeding, suggesting that neural stimulation is an important factor. Doliba et al. [41] and Nakazaki et al. [106] reported that acetylcholine and carbachol stimulate insulin release from Sur1KO islets even in low glucose. Doliba et al. [41] argue secretion is impaired in the Sur1KO mice and suggest acetylcholine, released in response to feeding, enhances insulin secretion, thus contributing to their euglycemia. Amino acids are also known to potentiate insulin secretion, and several studies have reported amino acids stimulate insulin release from Sur1KO islets [65, 87, 105].
KATP channels are part of a brain–liver circuit that modulates hepatic glucose production
SUR1/KIR6.2 channels are known to be present throughout the CNS and are implicated in neuroprotection during periods of anoxia (reviewed in 16). Here we focus on their role(s) in glucose homeostasis, particularly in the hypothalamus. Early electrophysiological studies identified a reciprocal response of hypothalamic neurons to applied glucose [3, 111, 112]. In the ventromedial hypothalamus (VMH), a majority of responding neurons increased their firing rate (glucose-responsive or glucose-stimulated), whereas in the lateral hypothalamus (LH), a majority reduced their activity (glucose-sensitive or glucose-inhibited). These results have been elegantly confirmed and extended by more recent studies, for example [142, 145]. Several reports and experiments on KIR6.2KO mice (98; see 28, 86, 125 for review) indicate that glucose-stimulated neurons in the VMH underlie the counterregulatory response to hypoglycemia, although Yang et al. [155] have reported that glucose-inhibited neurons are involved. The behavior of glucose-stimulated neurons is consistent with a β-cell-type regulation of KATP channels in the sense that increased glucose metabolism reduces channel activity and, thus, increases the neuronal firing rate secondary to membrane depolarization. During hypoglycemia, the firing rate drops and is presumed to reduce an inhibitory effect on glucagon release.
Three recent articles delineate a novel brain–liver circuit involving neurons in the LH in which activation of KATP channels is implicated in the control of hepatic glucose production. The activity of these neurons is presumed to suppress hepatic glucose production and increased hypothalamic insulin [116], free fatty acids [84], and glucose [83] via intracerebroventricular (ICV) infusion, resulting in reduced blood glucose levels. These effects are mimicked by diazoxide alone and blocked by coinfusion of glibenclamide. Consistent with their lack of SUR1/KIR6.2 KATP channels, Sur1KO mice maintained their hepatic glucose output when infused with fatty acids [84] or insulin [116].
It is not known whether the hypothalamic neurons involved in the brain–liver circuit are glucose-inhibited or glucose-stimulated, but based on the observation that the effect of increased glucose can be mimicked by diazoxide, a KATP channel activator, we tentatively conclude they are glucose-inhibited. In this case, the metabolic control of their membrane potential is distinctly at odds with the conventional β-cell paradigm in which increased fuel metabolism reduces KATP channel activity and would be mimicked by sulfonylureas rather than diazoxide, which stimulates KATP channels. The metabolic control of firing rate in these neurons is poorly understood; three mechanisms, summarized schematically in Fig. 5, have been suggested: (1) Oomura and colleagues [113] proposed that increasing activity of the electrogenic sodium pump (Na+-/K+-ATPase), secondary to increased glucose metabolism, can hyperpolarize glucose-inhibited neurons. This would be consistent with the [Na+]i and [K+]i determinations of Silver and Erecińska [142] on glucose-inhibited neurons, and both insulin and long-chain acyl CoAs are reported to stimulate the sodium pump. (2) Song et al. [145] proposed metabolic activation of a Cl− influx as the basis for hyperpolarization of glucose-inhibited (GI) neurons in the ventromedial nucleus. (3) The activation of KATP channels by LC-CoA is a potential mechanism. The cytosolic concentration of LC-CoA is expected to rise when fatty acids are elevated and with increased glucose metabolism due to a rise in malonyl-CoA, an inhibitor of CPT1 (carnitine-palmitoyl transferase 1), which transports LC-CoA into mitochondria (reviewed in 35, 40). Understanding metabolic control in these neurons and the role of KATP channels presents a clear challenge.
Glucose-stimulated vs glucose-inhibited hypothalamic neurons. The left panel illustrates a β-cell-like mechanism of KATP channel regulation in a glucose-stimulated neuron in the VMH. Glucose metabolism increases the ATP/ADP ratio, reducing channel activity, thus depolarizing the neuron to increase its firing rate. The preferential role for NADH equivalents derived from glycolysis and hypothesized role for creatine phosphate (CrP) and creatine kinase (CK) described in the text are shown. The firing of glucose-stimulated VMH neurons is presumed to attenuate glucagon release from pancreatic α cells when blood glucose is elevated and reduced firing during periods of brain hypoglycemia leads to increased glucagon secretion as part of the counterregulatory response (reviewed in 28, 86, 125). The right panel illustrates three potential mechanisms whereby glucose metabolism is hypothesized to hyperpolarize glucose-inhibited neurons and decrease their firing rate. Song et al. [145] have suggested metabolic activation of an inward chloride (Cl−) flux would result in hyperpolarization as diagramed in the lower left side of the right panel. Following the astrocyte-neuron lactate shuttle model [33, 76, 115] and Lam et al. [83], glucose metabolism in astrocytes leads to shuttling of lactate (Lac) into neurons via monocarboxylate transporters (MCTs), where it is converted to pyruvate (Pyr) and metabolized in mitochondria. The malonyl-CoA/LC-CoA model of glucose-stimulated insulin secretion holds that during glucose stimulation, increased TCA cycle activity in pancreatic β cells elevates malonyl-CoA via increased citrate production (reviewed in 35, 40). The inhibition of carnitine–palmitoyl transferase 1 (CPT-1) by malonyl–CoA subsequently leads to an increase in LC-CoAs that can activate KATP channels as illustrated in the lower right. Finally, early studies by Oomura and colleagues [113] implicated activation of the electrogenic sodium pump in the reduced firing rate of glucose-inhibited neurons. This hypothesis is supported by measurements of Vm, [Na+]i, and [K+ ]i by Silver and Ereciñska [142], and the stimulation of pump activity by insulin via a multistep process involving insulin receptors (IRs) (reviewed in 146). Both glucokinase (GK) and the Glut2 glucose transporter have been implicated in regulation of VMH neurons (reviewed in 125)
Summary
Adenosine-triphosphate-sensitive K+ channels present a unique use of ABC proteins as regulators of ion channels rather than transporters in their own right. Continuing analyses of the role of these channels in human genetic disease have provided better understanding of disorders of glucose homeostasis and their treatment and have validated the dual role nucleotides play in the regulation of channel activity. Understanding how HI and ND mutations inhibit and stimulate channel activity promises further insight into the molecular control of channel gating, whereas studies on KATP channel knockout mice continue to provide novel insights into their function.
References
Aguilar-Bryan L, Bryan J (1999) Molecular biology of adenosine triphosphate-sensitive potassium channels. Endocr Rev 20:101–135
Aguilar-Bryan L, Clement JP IV, Gonzalez G, Kunjilwar K, Babenko A, Bryan J (1998) Toward understanding the assembly and structure of KATP channels. Physiol Rev 78:227–245
Anand BK, Chhina GS, Sharma KN, Dua S, Singh B (1964) Activity of single neurons in the hypothalamic feeding centers: effect of glucose. Am J Physiol 207:1146–1154
Ashfield R, Gribble FM, Ashcroft SJ, Ashcroft FM (1999) Identification of the high-affinity tolbutamide site on the SUR1 subunit of the KATP channel. Diabetes 48:1341–1347
Babenko AP (2005) KATP channels “vingt ans apres”: ATG to PDB to mechanism. J Mol Cell Cardiol 39:79–98
Babenko AP, Bryan J (2002) SUR-dependent modulation of KATP channels by an N-terminal KIR6.2 peptide. Defining intersubunit gating interactions. J Biol Chem 277:43997–44004
Babenko AP, Bryan J (2003) SUR domains that associate with and gate KATP pores define a novel gatekeeper. J Biol Chem 278:41577–41580
Babenko AP, Gonzalez G, Aguilar-Bryan L, Bryan J (1999) Sulfonylurea receptors set the maximal open probability, ATP sensitivity and plasma membrane density of KATP channels. FEBS Lett 445:131–136
Babenko AP, Gonzalez G, Bryan J (1999) The N terminus of KIR6.2 limits spontaneous bursting and modulates the ATP-inhibition of KATP channels. Biochem Biophys Res Commun 255:231–238
Babenko AP, Gonzalez G, Bryan J (1999) The tolbutamide site of SUR1 and a mechanism for its functional coupling to KATP channel closure. FEBS Lett 459:367–376
Babenko AP, Gonzalez G, Bryan J (1999) Two regions of sulfonylurea receptor specify the spontaneous bursting and ATP inhibition of KATP channel isoforms. J Biol Chem 274:11587–11592
Babenko AP, Polak M, Cavé H, Busiah K, Czernichow P, Scharfmann R, Bryan J, Aguilar-Bryan L, Vaxillaire M, Froguel P (2006) Activating mutations in ABCC8 cause neonatal diabetes mellitus. N Engl J Med (in press)
Babenko AP, Vassort G (1997) Purinergic facilitation of ATP-sensitive potassium current in rat ventricular myocytes. Br J Pharmacol 120:631–638
Bakos E, Evers R, Calenda G, Tusnady GE, Szakacs G, Varadi A, Sarkadi B (2000) Characterization of the amino-terminal regions in the human multidrug resistance protein (MRP1). J Cell Sci 113(Pt 24):4451–4461
Bakos E, Evers R, Szakacs G, Tusnady GE, Welker E, Szabo K, de Haas M, van Deemter L, Borst P, Varadi A, Sarkadi B (1998) Functional multidrug resistance protein (MRP1) lacking the N-terminal transmembrane domain. J Biol Chem 273:32167–32175
Ballanyi K (2004) Protective role of neuronal KATP channels in brain hypoxia. J Exp Biol 207:3201–3212
Bancila V, Cens T, Monnier D, Chanson F, Faure C, Dunant Y, Bloc A (2005) Two SUR1-specific histidine residues mandatory for zinc-induced activation of the rat KATP channel. J Biol Chem 280:8793–8799
Bancila V, Nikonenko I, Dunant Y, Bloc A (2004) Zinc inhibits glutamate release via activation of pre-synaptic K channels and reduces ischaemic damage in rat hippocampus. J Neurochem 90:1243–1250
Baukrowitz T, Fakler B (2000) KATP channels gated by intracellular nucleotides and phospholipids. Eur J Biochem 267:5842–5848
Baukrowitz T, Schulte U, Oliver D, Herlitze S, Krauter T, Tucker SJ, Ruppersberg JP, Fakler B (1998) PIP2 and PIP as determinants for ATP inhibition of KATP channels. Science 282:1141–1144
Bienengraeber M, Olson TM, Selivanov VA, Kathmann EC, O’Cochlain F, Gao F, Karger AB, Ballew JD, Hodgson DM, Zingman LV, Pang YP, Alekseev AE, Terzic A (2004) ABCC9 mutations identified in human dilated cardiomyopathy disrupt catalytic KATP channel gating. Nat Genet 36:382–387
Bloc A, Cens T, Cruz H, Dunant Y (2000) Zinc-induced changes in ionic currents of clonal rat pancreatic b-cells: activation of ATP-sensitive K+ channels. J Physiol 529(Pt 3):723–734
Branstrom R, Aspinwall CA, Valimaki S, Ostensson CG, Tibell A, Eckhard M, Brandhorst H, Corkey BE, Berggren PO, Larsson O (2004) Long-chain CoA esters activate human pancreatic beta-cell KATP channels: potential role in type 2 diabetes. Diabetologia 47:277–283
Branstrom R, Corkey BE, Berggren PO, Larsson O (1997) Evidence for a unique long chain acyl-CoA ester binding site on the ATP-regulated potassium channel in mouse pancreatic beta cells. J Biol Chem 272:17390–17394
Branstrom R, Leibiger IB, Leibiger B, Corkey BE, Berggren PO, Larsson O (1998) Long chain coenzyme A esters activate the pore-forming subunit (Kir6. 2) of the ATP-regulated potassium channel. J Biol Chem 273:31395–31400
Bryan J, Crane A, Vila-Carriles WH, Babenko AP, Aguilar-Bryan L (2005) Insulin secretagogues, sulfonylurea receptors and KATP channels. Curr Pharm Des 11:2699–2716
Bryan J, Vila-Carriles WH, Zhao G, Babenko AP, Aguilar-Bryan L (2004) Toward linking structure with function in ATP-sensitive K+ channels. Diabetes 53(Suppl 3):S104–S112
Burdakov D, Luckman SM, Verkhratsky A (2005) Glucose-sensing neurons of the hypothalamus. Philos Trans R Soc Lond B Biol Sci 360:2227–2235
Campbell JD, Sansom MS, Ashcroft FM (2003) Potassium channel regulation. EMBO Rep 4:1038–1042
Cartier EA, Conti LR, Vandenberg CA, Shyng SL (2001) Defective trafficking and function of KATP channels caused by a sulfonylurea receptor 1 mutation associated with persistent hyperinsulinemic hypoglycemia of infancy. Proc Natl Acad Sci USA 98:2882–2887
Chan KW, Zhang H, Logothetis DE (2003) N-terminal transmembrane domain of the SUR controls trafficking and gating of Kir6 channel subunits. EMBO J 22:3833–3843
Chang G (2003) Structure of MsbA from Vibrio cholera: a multidrug resistance ABC transporter homolog in a closed conformation. J Mol Biol 330:419–430
Chih CP, Roberts EL Jr (2003) Energy substrates for neurons during neural activity: a critical review of the astrocyte-neuron lactate shuttle hypothesis. J Cereb Blood Flow Metab 23:1263–1281
Clement JP IV, Kunjilwar K, Gonzalez G, Schwanstecher M, Panten U, Aguilar-Bryan L, Bryan J (1997) Association and stoichiometry of KATP channel subunits. Neuron 18:827–838
Corkey BE, Deeney JT, Yaney GC, Tornheim K, Prentki M (2000) The role of long-chain fatty acyl–CoA esters in beta-cell signal transduction. J Nutr 130:299S–304S
Crane A, Aguilar-Bryan L (2004) Assembly, maturation, and turnover of KATP channel subunits. J Biol Chem 279:9080–9090
Crawford RM, Ranki HJ, Botting CH, Budas GR, Jovanovic A (2002) Creatine kinase is physically associated with the cardiac ATP-sensitive K+ channel in vivo. FASEB J 16:102–104
D’Hahan N, Jacquet H, Moreau C, Catty P, Vivaudou M (1999) A transmembrane domain of the sulfonylurea receptor mediates activation of ATP-sensitive K+ channels by K+ channel openers. Mol Pharmacol 56:308–315
de Rooij J, Zwartkruis FJ, Verheijen MH, Cool RH, Nijman SM, Wittinghofer A, Bos JL (1998) Epac is a Rap1 guanine-nucleotide-exchange factor directly activated by cyclic AMP. Nature 396:474–477
Deeney JT, Prentki M, Corkey BE (2000) Metabolic control of beta-cell function. Semin Cell Dev Biol 11:267–275
Doliba NM, Qin W, Vatamaniuk MZ, Li C, Zelent D, Najafi H, Buettger CW, Collins HW, Carr RD, Magnuson MA, Matschinsky FM (2004) Restitution of defective glucose-stimulated insulin release of sulfonylurea type 1 receptor knockout mice by acetylcholine. Am J Physiol Endocrinol Metab 286:E834–E843
Doyle DA, Morais Cabral J, Pfuetzner RA, Kuo A, Gulbis JM, Cohen SL, Chait BT, MacKinnon R (1998) The structure of the potassium channel: molecular basis of K+ conduction and selectivity. Science 280:69–77
Drain P, Li L, Wang J (1998) KATP channel inhibition by ATP requires distinct functional domains of the cytoplasmic C terminus of the pore-forming subunit. Proc Natl Acad Sci USA 95:13953–13958
Düfer M, Haspel D, Krippeit-Drews P, Aguilar-Bryan L, Bryan J, Drews G (2004) Oscillations of membrane potential and cytosolic Ca2+ concentration in SUR1−/− beta cells. Diabetologia 47:488–498
Düfer M, Krippeit-Drews P, Drews G (2002) Inhibition of mitochondrial function affects cellular Ca2+ handling in pancreatic B-cells. Pflugers Arch 444:236–243
Dukes ID, McIntyre MS, Mertz RJ, Philipson LH, Roe MW, Spencer B, Worley JF III (1994) Dependence on NADH produced during glycolysis for beta-cell glucose signaling. J Biol Chem 269:10979–10982
Dunne MJ, Kane C, Shepherd RM, Sanchez JA, James RF, Johnson PR, Aynsley-Green A, Lu S, Clement JP IV, Lindley KJ, Seino S, Aguilar-Bryan L (1997) Familial persistent hyperinsulinemic hypoglycemia of infancy and mutations in the sulfonylurea receptor. N Engl J Med 336:703–706
Eliasson L, Ma X, Renstrom E, Barg S, Berggren PO, Galvanovskis J, Gromada J, Jing X, Lundquist I, Salehi A, Sewing S, Rorsman P (2003) SUR1 regulates PKA-independent cAMP-induced granule priming in mouse pancreatic B-cells. J Gen Physiol 121:181–197
Emanuele E, Falcone C, Carabela M, Minoretti P, D’Angelo A, Montagna L, Geroldi D (2003) Absence of Kir6.1/KCNJ8 mutations in Italian patients with abnormal coronary vasomotion. Int J Mol Med 12:509–512
Eto K, Suga S, Wakui M, Tsubamoto Y, Terauchi Y, Taka J, Aizawa S, Noda M, Kimura S, Kasai H, Kadowaki T (1999) NADH shuttle system regulates KATP channel-dependent pathway and steps distal to cytosolic Ca2+ concentration elevation in glucose-induced insulin secretion. J Biol Chem 274:25386–25392
Eto K, Tsubamoto Y, Terauchi Y, Sugiyama T, Kishimoto T, Takahashi N, Yamauchi N, Kubota N, Murayama S, Aizawa T, Akanuma Y, Aizawa S, Kasai H, Yazaki Y, Kadowaki T (1999) Role of NADH shuttle system in glucose-induced activation of mitochondrial metabolism and insulin secretion. Science 283:981–985
Fan Z, Makielski JC (1997) Anionic phospholipids activate ATP-sensitive potassium channels. J Biol Chem 272:5388–5395
Fernandez SB, Hollo Z, Kern A, Bakos E, Fischer PA, Borst P, Evers R (2002) Role of the N-terminal transmembrane region of the multidrug resistance protein MRP2 in routing to the apical membrane in MDCKII cells. J Biol Chem 277:31048–31055
Florez JC, Sjogren M, Burtt N, Orho-Melander M, Schayer S, Sun M, Almgren P, Lindblad U, Tuomi T, Gaudet D, Hudson TJ, Daly MJ, Ardlie KG, Hirschhorn JN, Altshuler D, Groop L (2004) Association testing in 9,000 people fails to confirm the association of the insulin receptor substrate-1 G972R polymorphism with type 2 diabetes. Diabetes 53:3313–3318
Fournet JC, Junien C (2004) Genetics of congenital hyperinsulinism. Endocr Pathol 15:233–240
Franklin I, Gromada J, Gjinovci A, Theander S, Wollheim CB (2005) Beta-cell secretory products activate alpha-cell ATP-dependent potassium channels to inhibit glucagon release. Diabetes 54:1808–1815
Geng X, Li L, Watkins S, Robbins PD, Drain P (2003) The insulin secretory granule is the major site of KATP channels of the endocrine pancreas. Diabetes 52:767–776
Gilon P, Henquin JC (1992) Influence of membrane potential changes on cytoplasmic Ca2+ concentration in an electrically excitable cell, the insulin-secreting pancreatic B-cell. J Biol Chem 267:20713–20720
Gloyn AL, Pearson ER, Antcliff JF, Proks P, Bruining GJ, Slingerland AS, Howard N, Srinivasan S, Silva JM, Molnes J, Edghill EL, Frayling TM, Temple IK, Mackay D, Shield JP, Sumnik Z, van Rhijn A, Wales JK, Clark P, Gorman S, Aisenberg J, Ellard S, Njolstad PR, Ashcroft FM, Hattersley AT (2004) Activating mutations in the gene encoding the ATP-sensitive potassium-channel subunit Kir6.2 and permanent neonatal diabetes. N Engl J Med 350:1838–1849
Gloyn AL, Weedon MN, Owen KR, Turner MJ, Knight BA, Hitman G, Walker M, Levy JC, Sampson M, Halford S, McCarthy MI, Hattersley AT, Frayling TM (2003) Large-scale association studies of variants in genes encoding the pancreatic beta-cell KATP channel subunits Kir6.2 (KCNJ11) and SUR1 (ABCC8) confirm that the KCNJ11 E23K variant is associated with type 2 diabetes. Diabetes 52:568–572
Goforth PB, Bertram R, Khan FA, Zhang M, Sherman A, Satin LS (2002) Calcium-activated K+ channels of mouse beta-cells are controlled by both store and cytoplasmic Ca2+: experimental and theoretical studies. J Gen Physiol 120:307–322
Gopel SO, Kanno T, Barg S, Eliasson L, Galvanovskis J, Renstrom E, Rorsman P (1999) Activation of Ca2+-dependent K+ channels contributes to rhythmic firing of action potentials in mouse pancreatic beta cells. J Gen Physiol 114:759–770
Hani EH, Boutin P, Durand E, Inoue H, Permutt MA, Velho G, Froguel P (1998) Missense mutations in the pancreatic islet beta cell inwardly rectifying K+ channel gene (KIR6.2/BIR): a meta-analysis suggests a role in the polygenic basis of type II diabetes mellitus in Caucasians. Diabetologia 41:1511–1515
Hashimoto N, Kido Y, Uchida T, Matsuda T, Suzuki K, Inoue H, Matsumoto M, Ogawa W, Maeda S, Fujihara H, Ueta Y, Uchiyama Y, Akimoto K, Ohno S, Noda T, Kasuga M (2005) PKCl regulates glucose-induced insulin secretion through modulation of gene expression in pancreatic beta cells. J Clin Invest 115:138–145
Haspel D, Krippeit-Drews P, Aguilar-Bryan L, Bryan J, Drews G, Düfer M (2005) Crosstalk between membrane potential and cytosolic Ca2+ concentration in beta cells from Sur1−/− mice. Diabetologia 48:913–921
Hattersley AT (2004) Unlocking the secrets of the pancreatic beta cell: man and mouse provide the key. J Clin Invest 114:314–316
Henquin JC (2000) Triggering and amplifying pathways of regulation of insulin secretion by glucose. Diabetes 49:1751–1760
Henquin JC (2004) Pathways in beta-cell stimulus-secretion coupling as targets for therapeutic insulin secretagogues. Diabetes 53(Suppl 3):S48–S58
Hibino H, Kurachi Y (2006) A new insight into the pathogenesis of coronary vasospasm. Circ Res 98:579–581
Inagaki N, Gonoi T, Seino S (1997) Subunit stoichiometry of the pancreatic beta-cell ATP-sensitive K+ channel. FEBS Lett 409:232–236
Ishihara H, Maechler P, Gjinovci A, Herrera PL, Wollheim CB (2003) Islet beta-cell secretion determines glucagon release from neighbouring alpha-cells. Nat Cell Biol 5:330–335
Jahangir A, Terzic A (2005) KATP channel therapeutics at the bedside. J Mol Cell Cardiol 39:99–112
Kane C, Shepherd RM, Squires PE, Johnson PR, James RF, Milla PJ, Aynsley-Green A, Lindley KJ, Dunne MJ (1996) Loss of functional KATP channels in pancreatic beta-cells causes persistent hyperinsulinemic hypoglycemia of infancy. Nat Med 2:1344–1347
Kane GC, Liu XK, Yamada S, Olson TM, Terzic A (2005) Cardiac KATP channels in health and disease. J Mol Cell Cardiol 38:937–943
Karwatsky J, Daoud R, Cai J, Gros P, Georges E (2003) Binding of a photoaffinity analogue of glutathione to MRP1 (ABCC1) within two cytoplasmic regions (L0 and L1) as well as transmembrane domains 10-11 and 16-17. Biochemistry 42:3286–3294
Kasischke KA, Vishwasrao HD, Fisher PJ, Zipfel WR, Webb WW (2004) Neural activity triggers neuronal oxidative metabolism followed by astrocytic glycolysis. Science 305:99–103
Kawasaki H, Springett GM, Mochizuki N, Toki S, Nakaya M, Matsuda M, Housman DE, Graybiel AM (1998) A family of cAMP-binding proteins that directly activate Rap1. Science 282:2275–2279
Koster JC, Marshall BA, Ensor N, Corbett JA, Nichols CG (2000) Targeted overactivity of beta cell KATP channels induces profound neonatal diabetes. Cell 100:645–654
Koster JC, Sha Q, Shyng S, Nichols CG (1999) ATP inhibition of KATP channels: control of nucleotide sensitivity by the N-terminal domain of the Kir6.2 subunit. J Physiol 515(Pt 1):19–30
Krippeit-Drews P, Bäcker M, Düfer M, Drews G (2003) Phosphocreatine as a determinant of KATP channel activity in pancreatic beta-cells. Pflugers Arch 445:556–562
Krippeit-Drews P, Düfer M, Drews G (2000) Parallel oscillations of intracellular calcium activity and mitochondrial membrane potential in mouse pancreatic B-cells. Biochem Biophys Res Commun 267:179–183
Kuo A, Gulbis JM, Antcliff JF, Rahman T, Lowe ED, Zimmer J, Cuthbertson J, Ashcroft FM, Ezaki T, Doyle DA (2003) Crystal structure of the potassium channel KirBac1.1 in the closed state. Science 300:1922–1926
Lam TK, Gutierrez-Juarez R, Pocai A, Rossetti L (2005) Regulation of blood glucose by hypothalamic pyruvate metabolism. Science 309:943–947
Lam TK, Pocai A, Gutierrez-Juarez R, Obici S, Bryan J, Aguilar-Bryan L, Schwartz GJ, Rossetti L (2005) Hypothalamic sensing of circulating fatty acids is required for glucose homeostasis. Nat Med 11:320–327
Lantz KA, Vatamaniuk MZ, Brestelli JE, Friedman JR, Matschinsky FM, Kaestner KH (2004) Foxa2 regulates multiple pathways of insulin secretion. J Clin Invest 114:512–520
Levin BE, Routh VH, Kang L, Sanders NM, Dunn-Meynell AA (2004) Neuronal glucosensing: what do we know after 50 years? Diabetes 53:2521–2528
Li C, Buettger C, Kwagh J, Matter A, Daikhin Y, Nissim IB, Collins HW, Yudkoff M, Stanley CA, Matschinsky FM (2004) A signaling role of glutamine in insulin secretion. J Biol Chem 279:13393–13401
Light P (1996) Regulation of ATP-sensitive potassium channels by phosphorylation. Biochim Biophys Acta 1286:65–73
Long SB, Campbell EB, Mackinnon R (2005) Voltage sensor of Kv1.2: structural basis of electromechanical coupling. Science 309:903–908
MacDonald MJ (1990) Elusive proximal signals of beta-cells for insulin secretion. Diabetes 39:1461–1466
Mason DL, Michaelis S (2002) Requirement of the N-terminal extension for vacuolar trafficking and transport activity of yeast Ycf1p, an ATP-binding cassette transporter. Mol Biol Cell 13:4443–4455
Matsuo M, Kimura Y, Ueda K (2005) KATP channel interaction with adenine nucleotides. J Mol Cell Cardiol 38:907–916
Matsuo M, Kioka N, Amachi T, Ueda K (1999) ATP binding properties of the nucleotide-binding folds of SUR1. J Biol Chem 274:37479–37482
Matsuo M, Tanabe K, Kioka N, Amachi T, Ueda K (2000) Different binding properties and affinities for ATP and ADP among sulfonylurea receptor subtypes, SUR1, SUR2A, and SUR2B. J Biol Chem 275:28757–28763
Mertz RJ, Worley JF, Spencer B, Johnson JH, Dukes ID (1996) Activation of stimulus-secretion coupling in pancreatic beta-cells by specific products of glucose metabolism. Evidence for privileged signaling by glycolysis. J Biol Chem 271:4838–4845
Michelsen K, Yuan H, Schwappach B (2005) Hide and run. Arginine-based endoplasmic-reticulum-sorting motifs in the assembly of heteromultimeric membrane proteins. EMBO Rep 6:717–722
Mikhailov MV, Campbell JD, de Wet H, Shimomura K, Zadek B, Collins RF, Sansom MS, Ford RC, Ashcroft FM (2005) 3-D structural and functional characterization of the purified KATP channel complex Kir6.2-SUR1. EMBO J 24:4166–4175
Miki T, Liss B, Minami K, Shiuchi T, Saraya A, Kashima Y, Horiuchi M, Ashcroft F, Minokoshi Y, Roeper J, Seino S (2001) ATP-sensitive K+ channels in the hypothalamus are essential for the maintenance of glucose homeostasis. Nat Neurosci 4:507–512
Miki T, Seino S (2005) Roles of KATP channels as metabolic sensors in acute metabolic changes. J Mol Cell Cardiol 38:917–925
Miki T, Suzuki M, Shibasaki T, Uemura H, Sato T, Yamaguchi K, Koseki H, Iwanaga T, Nakaya H, Seino S (2002) Mouse model of Prinzmetal angina by disruption of the inward rectifier Kir6.1. Nat Med 8:466–472
Minami K, Miki T, Kadowaki T, Seino S (2004) Roles of ATP-sensitive K+ channels as metabolic sensors: studies of Kir6.x null mice. Diabetes 53(Suppl 3):S176–S180
Moreau C, Gally F, Jacquet-Bouix H, Vivaudou M (2005) The size of a single residue of the sulfonylurea receptor dictates the effectiveness of KATP channel openers. Mol Pharmacol 67:1026–1033
Moreau C, Jacquet H, Prost AL, D’Hahan N, Vivaudou M (2000) The molecular basis of the specificity of action of KATP channel openers. EMBO J 19:6644–6651
Moreau C, Prost AL, Derand R, Vivaudou M (2005) SUR, ABC proteins targeted by KATP channel openers. J Mol Cell Cardiol 38:951–963
Muñoz A, Hu M, Hussain K, Bryan J, Aguilar-Bryan L, Rajan AS (2005) Regulation of glucagon secretion at low glucose concentrations: evidence for adenosine triphosphate-sensitive potassium channel involvement. Endocrinology 146:5514–5521
Nakazaki M, Crane A, Hu M, Seghers V, Ullrich S, Aguilar-Bryan L, Bryan J (2002) cAMP-activated protein kinase-independent potentiation of insulin secretion by cAMP is impaired in SUR1 null islets. Diabetes 51:3440–3449
Neagoe I, Schwappach B (2005) Pas de deux in groups of four—the biogenesis of KATP channels. J Mol Cell Cardiol 38:887–894
Nenquin M, Szollosi A, Aguilar-Bryan L, Bryan J, Henquin JC (2004) Both triggering and amplifying pathways contribute to fuel-induced insulin secretion in the absence of sulfonylurea receptor-1 in pancreatic beta-cells. J Biol Chem 279:32316–32324
Nichols CG, Shyng SL, Nestorowicz A, Glaser B, Clement JP IV, Gonzalez G, Aguilar-Bryan L, Permutt MA, Bryan J (1996) Adenosine diphosphate as an intracellular regulator of insulin secretion. Science 272:1785–1787
Nishida M, MacKinnon R (2002) Structural basis of inward rectification: cytoplasmic pore of the G protein-gated inward rectifier GIRK1 at 1.8Å resolution. Cell 111:957–965
Oomura Y, Kimura K, Ooyama H, Maeno T, Iki M, Kuniyoshi M (1964) Reciprocal activities of the ventromedial and lateral hypothalamic areas of cats. Science 143:484–485
Oomura Y, Ono T, Ooyama H, Wayner MJ (1969) Glucose and osmosensitive neurones of the rat hypothalamus. Nature 222:282–284
Oomura Y, Ooyama H, Sugimori M, Nakamura T, Yamada Y (1974) Glucose inhibition of the glucose-sensitive neurone in the rat lateral hypothalamus. Nature 247:284–286
Ozaki N, Shibasaki T, Kashima Y, Miki T, Takahashi K, Ueno H, Sunaga Y, Yano H, Matsuura Y, Iwanaga T, Takai Y, Seino S (2000) cAMP-GEFII is a direct target of cAMP in regulated exocytosis. Nat Cell Biol 2:805–811
Pellerin L, Pellegri G, Bittar PG, Charnay Y, Bouras C, Martin JL, Stella N, Magistretti PJ (1998) Evidence supporting the existence of an activity-dependent astrocyte-neuron lactate shuttle. Dev Neurosci 20:291–299
Pocai A, Lam TK, Gutierrez-Juarez R, Obici S, Schwartz GJ, Bryan J, Aguilar-Bryan L, Rossetti L (2005) Hypothalamic KATP channels control hepatic glucose production. Nature 434:1026–1031
Polak M, Shield J (2004) Neonatal and very-early-onset diabetes mellitus. Semin Neonatol 9:59–65
Proks P, Lippiat JD (2006) Membrane ion channels and diabetes. Curr Pharm Des 12:485–501
Prost AL, Bloc A, Hussy N, Derand R, Vivaudou M (2004) Zinc is both an intracellular and extracellular regulator of KATP channel function. J Physiol 559:157–167
Quast U, Stephan D, Bieger S, Russ U (2004) The impact of ATP-sensitive K+ channel subtype selectivity of insulin secretagogues for the coronary vasculature and the myocardium. Diabetes 53(Suppl 3):S156–S164
Rapedius M, Soom M, Shumilina E, Schulze D, Schonherr R, Kirsch C, Lang F, Tucker SJ, Baukrowitz T (2005) Long chain CoA esters as competitive antagonists of phosphatidylinositol 4,5-bisphosphate activation in Kir channels. J Biol Chem 280:30760–30767
Riedel MJ, Boora P, Steckley D, de Vries G, Light PE (2003) Kir6.2 polymorphisms sensitize beta-cell ATP-sensitive potassium channels to activation by acyl CoAs: a possible cellular mechanism for increased susceptibility to type 2 diabetes? Diabetes 52:2630–2635
Riedel MJ, Light PE (2005) Saturated and cis/trans unsaturated acyl CoA esters differentially regulate wild-type and polymorphic beta-cell ATP-sensitive K+ channels. Diabetes 54:2070–2079
Riedel MJ, Steckley DC, Light PE (2005) Current status of the E23K Kir6.2 polymorphism: implications for type-2 diabetes. Hum Genet 116:133–145
Routh VH (2002) Glucose-sensing neurons: are they physiologically relevant? Physiol Behav 76:403–413
Sagen JV, Raeder H, Hathout E, Shehadeh N, Gudmundsson K, Baevre H, Abuelo D, Phornphutkul C, Molnes J, Bell GI, Gloyn AL, Hattersley AT, Molven A, Sovik O, Njolstad PR (2004) Permanent neonatal diabetes due to mutations in KCNJ11 encoding Kir6.2: patient characteristics and initial response to sulfonylurea therapy. Diabetes 53:2713–2718
Sanchez JA, Gonoi T, Inagaki N, Katada T, Seino S (1998) Modulation of reconstituted ATP-sensitive K+-channels by GTP-binding proteins in a mammalian cell line. J Physiol 507(Pt 2):315–324
Santos RM, Barbosa RM, Silva AM, Antunes CM, Rosario LM (1992) High external Ca2+ levels trigger membrane potential oscillations in mouse pancreatic beta-cells during blockade of KATP channels. Biochem Biophys Res Commun 187:872–879
Santos RM, Rosario LM, Nadal A, Garcia-Sancho J, Soria B, Valdeolmillos M (1991) Widespread synchronous [Ca2+]i oscillations due to bursting electrical activity in single pancreatic islets. Pflugers Arch 418:417–422
Schulze D, Rapedius M, Krauter T, Baukrowitz T (2003) Long-chain acyl-CoA esters and phosphatidylinositol phosphates modulate ATP inhibition of KATP channels by the same mechanism. J Physiol 552:357–367
Schwanstecher C, Meyer U, Schwanstecher M (2002) KIR6.2 polymorphism predisposes to type 2 diabetes by inducing overactivity of pancreatic beta-cell ATP-sensitive K+ channels. Diabetes 51:875–879
Schwappach B, Zerangue N, Jan YN, Jan LY (2000) Molecular basis for KATP assembly: transmembrane interactions mediate association of a K+ channel with an ABC transporter. Neuron 26:155–167
Seghers V, Nakazaki M, DeMayo F, Aguilar-Bryan L, Bryan J (2000) Sur1 knockout mice. A model for KATP channel-independent regulation of insulin secretion. J Biol Chem 275:9270–9277
Seino S, Miki T (2003) Physiological and pathophysiological roles of ATP-sensitive K+ channels. Prog Biophys Mol Biol 81:133–176
Seino S, Shibasaki T (2005) PKA-dependent and PKA-independent pathways for cAMP-regulated exocytosis. Physiol Rev 85:1303–1342
Sharma N, Crane A, Clement JP IV, Gonzalez G, Babenko AP, Bryan J, Aguilar-Bryan L (1999) The C terminus of SUR1 is required for trafficking of KATP channels. J Biol Chem 274:20628–20632
Shiota C, Larsson O, Shelton KD, Shiota M, Efanov AM, Hoy M, Lindner J, Kooptiwut S, Juntti-Berggren L, Gromada J, Berggren PO, Magnuson MA (2002) Sulfonylurea receptor type 1 knock-out mice have intact feeding-stimulated insulin secretion despite marked impairment in their response to glucose. J Biol Chem 277:37176–37183
Shyng S, Nichols CG (1997) Octameric stoichiometry of the KATP channel complex. J Gen Physiol 110:655–664
Shyng SL, Ferrigni T, Shepard JB, Nestorowicz A, Glaser B, Permutt MA, Nichols CG (1998) Functional analyses of novel mutations in the sulfonylurea receptor 1 associated with persistent hyperinsulinemic hypoglycemia of infancy. Diabetes 47:1145–1151
Shyng SL, Nichols CG (1998) Membrane phospholipid control of nucleotide sensitivity of KATP channels. Science 282:1138–1141
Sieg A, Su J, Munoz A, Buchenau M, Nakazaki M, Aguilar-Bryan L, Bryan J, Ullrich S (2004) Epinephrine-induced hyperpolarization of islet cells without KATP channels. Am J Physiol Endocrinol Metab 286:E463–E471
Silver IA, Erecińska M (1998) Glucose-induced intracellular ion changes in sugar-sensitive hypothalamic neurons. J Neurophysiol 79:1733–1745
Slingerland AS, Hattersley AT (2005) Mutations in the Kir6.2 subunit of the KATP channel and permanent neonatal diabetes: new insights and new treatment. Ann Med 37:186–195
Solbach TF, Konig J, Fromm MF, Zolk O (2006) ATP-binding cassette transporters in the heart. Trends Cardiovasc Med 16:7–15
Song Z, Levin BE, McArdle JJ, Bakhos N, Routh VH (2001) Convergence of pre- and postsynaptic influences on glucosensing neurons in the ventromedial hypothalamic nucleus. Diabetes 50:2673–2681
Sweeney G, Klip A (1998) Regulation of the Na+/K+-ATPase by insulin: why and how? Mol Cell Biochem 182:121–133
Tanabe K, Tucker SJ, Ashcroft FM, Proks P, Kioka N, Amachi T, Ueda K (2000) Direct photoaffinity labeling of Kir6.2 by g-32P]ATP-g4-azidoanilide. Biochem Biophys Res Commun 272:316–319
Tanabe K, Tucker SJ, Matsuo M, Proks P, Ashcroft FM, Seino S, Amachi T, Ueda K (1999) Direct photoaffinity labeling of the Kir6.2 subunit of the ATP-sensitive K+ channel by 8-azido-ATP. J Biol Chem 274:3931–3933
Taschenberger G, Mougey A, Shen S, Lester LB, LaFranchi S, Shyng SL (2002) Identification of a familial hyperinsulinism-causing mutation in the sulfonylurea receptor 1 that prevents normal trafficking and function of KATP channels. J Biol Chem 277:17139–17146
Tucker SJ, Gribble FM, Zhao C, Trapp S, Ashcroft FM (1997) Truncation of Kir6.2 produces ATP-sensitive K+ channels in the absence of the sulphonylurea receptor. Nature 387:179–183
Vanoye CG, MacGregor GG, Dong K, Tang L, Buschmann AS, Hall AE, Lu M, Giebisch G, Hebert SC (2002) The carboxyl termini of KATP channels bind nucleotides. J Biol Chem 277:23260–23270
Vaxillaire M, Populaire C, Busiah K, Cave H, Gloyn AL, Hattersley AT, Czernichow P, Froguel P, Polak M (2004) Kir6.2 mutations are a common cause of permanent neonatal diabetes in a large cohort of French patients. Diabetes 53:2719–2722
Wang X, Wu J, Li L, Chen F, Wang R, Jiang C (2003) Hypercapnic acidosis activates KATP channels in vascular smooth muscles. Circ Res 92:1225–1232
Yamada M, Ishii M, Hibino H, Kurachi Y (2004) Mutation in nucleotide-binding domains of sulfonylurea receptor 2 evokes Na-ATP-dependent activation of ATP-sensitive K+ channels: implication for dimerization of nucleotide-binding domains to induce channel opening. Mol Pharmacol 66:807–816
Yang XJ, Kow LM, Pfaff DW, Mobbs CV (2004) Metabolic pathways that mediate inhibition of hypothalamic neurons by glucose. Diabetes 53:67–73
Yuan H, Michelsen K, Schwappach B (2003) 14-3-3 dimers probe the assembly status of multimeric membrane proteins. Curr Biol 13:638–646
Zerangue N, Schwappach B, Jan YN, Jan LY (1999) A new ER trafficking signal regulates the subunit stoichiometry of plasma membrane KATP channels. Neuron 22:537–548
Zingman LV, Alekseev AE, Bienengraeber M, Hodgson D, Karger AB, Dzeja PP, Terzic A (2001) Signaling in channel/enzyme multimers: ATPase transitions in SUR module gate ATP-sensitive K+ conductance. Neuron 31:233–245
Acknowledgement
This work was supported by grants from the Deutsche Forschungsgemeinschaft (Dr225/6-1 and Du425/1-1) and the US National Institutes of Health (DK52771, DK44311, and JDRF 1-2005-950). There are no conflicts of interest in this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bryan, J., Muñoz, A., Zhang, X. et al. ABCC8 and ABCC9: ABC transporters that regulate K+ channels. Pflugers Arch - Eur J Physiol 453, 703–718 (2007). https://doi.org/10.1007/s00424-006-0116-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00424-006-0116-z