Abstract
Cardiac uptake of long-chain fatty acids (FA) is mediated predominantly by two membrane-associated proteins, the 43-kDa plasma membrane fatty acid-binding protein (FABPpm) and the 88-kDa fatty acid translocase/CD36 (FAT/CD36). While FABPpm is present constitutively in the sarcolemma, FAT/CD36 is recycled between an intracellular membrane compartment and the sarcolemma. Since the amount of sarcolemmal FAT/CD36 is a major determinant of cellular FA uptake, understanding of the regulation of its recycling is likely to provide new insights into altering substrate preference of the heart. FAT/CD36 recycling displays a remarkable similarity with that of the two glucose transporters (GLUT) in the heart, GLUT1 and GLUT4. Translocation of all three transporters is induced by insulin and by contraction, which stimuli activate distinct signalling cascades. The insulin pathway involves phosphatidylinositol-3 kinase (PI3K) whilst the contraction pathway is dependent on AMP-activated protein kinase (AMPK). For the identification of additional protein components involved in the regulation of FAT/CD36 recycling, valuable lessons can be learned from GLUT1 and GLUT4 recycling. Especially GLUT4 recycling is an intensively studied process in which a number of signalling proteins, both upstream and downstream from PI3 K and AMPK, have been identified, as well as proteins that are part of the translocation machinery involving Rab GTPases and soluble N-ethylmaleimide attachment protein receptors (SNAREs). Comparison of the magnitude of the effects of insulin and contraction on substrate uptake and on transporter appearance in the sarcolemma have revealed that FAT/CD36 recycling resembles GLUT1 recycling more closely than that of GLUT4. This pinpoints the recycling compartment and excludes a pre-endosomal storage compartment as the intracellular storage site for FAT/CD36. Further research will probably establish whether FAT/CD36 translocation is (partly) coupled to that of one or both GLUTs or, alternatively, whether it is a distinct process that also can be induced independently of GLUT1 or GLUT4 movement. In the latter case, a unique set of proteins would be dedicated to FAT/CD36 recycling, which would then provide an attractive target for manipulating cardiac substrate preference.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Long-chain fatty acids (FA) and glucose are the major substrates with which the heart sustains mechanical performance [122]. Currently, there is renewed interest in the regulation of cardiac utilization of these substrates because novel regulatory sites have been identified. Glucose uptake has been established firmly as the rate-limiting step in glucose utilization by muscle cells [102]. Internalized glucose is phosphorylated rapidly to glucose-6-phosphate, maintaining intracellularly sequestered glucose at a low level even when exogenous glucose concentrations are high. As a consequence, the outside-to-inside glucose gradient across the sarcolemma will remain steep and drives glucose towards cellular uptake. Similarly, FA uptake is governed by the FA gradient across the sarcolemma [122]. Even so, the first step in cellular FA metabolism, the thiolinkage of FA with coenzyme A to form acyl-CoA is a rapid event [86, 122]. Indeed, this rapid trapping of FA following cellular entry ensures that at high exogenous FA concentrations, i.e. at levels beyond which FA uptake is saturated, the intracellular level of free (i.e. non-metabolized) FA does not rise [67]. The fact that for both substrates—glucose and FA—transsarcolemmal transport appears to be the rate-limiting step implies that cardiac substrate preference is determined mainly at the level of the sarcolemma rather than by competition for oxidation, as proposed by Randle et al. [94]. For a better understanding of the interplay between FA uptake and glucose uptake at the sarcolemmal level, unravelling of the molecular mechanisms underlying these processes is of pivotal importance. Newer studies have indicated that specific membrane proteins are involved in the regulation of both cellular FA and glucose uptake.
This article begins with a review of the initial studies that identified the proteins involved in cardiac FA uptake. One of these putative FA transporters, the fatty acid translocase/CD36 (FAT/CD36), recycles between the sarcolemma and intracellular stores and its translocation to the cell surface appears to be crucial for regulation of cardiac FA uptake. To unmask the components of the cellular FAT/CD36 translocation machinery and to obtain insight into the regulation of cardiac substrate preference, it is helpful to compare this event with what is already known about the translocation of GLUT1 and GLUT4, the major cardiac glucose transporters. Because GLUT4 recycling has been studied in more detail in skeletal muscle and adipose tissue, the mechanisms disclosed in these tissues will be discussed where appropriate. We realize that care must be taken in extrapolating findings from skeletal muscle to a cardiac setting, given the subtle differences in cardiac and skeletal muscle metabolism. But overall, the similarities far outweigh the differences. Moreover, GLUT4 translocation has been best investigated in adipocytes, which share with heart and skeletal muscle the ability to respond metabolically to insulin but, in contrast, lack, of course, exercise metabolism. Finally, an attempt has been made to integrate the various findings into an overall scheme of regulation of cardiac substrate transport by intracellular recycling of glucose and FA transporters.
Regulation of cardiac FA uptake
Cellular FA uptake has long been considered to be a passive mechanism, dependent on the metabolic rate and governed by physicochemical properties of these lipophilic substrates [98]. Especially partitioning of FA between albumin and plasma membranes has been postulated to be dependent on K off rates for albumin and K on rates for phospholipid bilayers [38]. However, the saturable nature of the FA uptake process, as observed in isolated cardiac myocytes, and its sensitivity to competitive inhibition suggest that a protein component is involved in cellular FA uptake [67, 68, 110]. The use of a variety of transport inhibitors with different modes of action has indicated that the protein component is responsible for the majority of FA uptake. While, in theory, all kinetic evidence could still be explained by saturability of metabolism [39], the observation that transport inhibition and substrate competition also occur in giant vesicles derived from the sarcolemma of cardiac myocytes, in which FA metabolism is entirely absent, adds powerful evidence in favour of the dependence of the heart on sarcolemmal proteins that act as FA transporters or FA transport facilitators [68]. The residual FA uptake, i.e. the non-inhibitable component (20–30% of total FA uptake), then most likely would be due to passive diffusion. While the list of proteins that have been proposed to act as putative transporters for FA is still growing, there is functional evidence for four of them. These are the 40-kDa plasma membrane FA binding protein (FABPpm) [48], the 88-kDa FAT/CD36 [47] and two members of the family of FA transport proteins (FATPs), the 63-kDa FATP1 [100] and the 70-kDa FATP6 [34]. All these putative transporters have been detected in the heart at both the mRNA and protein levels [68, 124]. In addition, all these transporters are localized at the sarcolemma, a prerequisite for their functioning in the cellular uptake of FA. Cellular FA uptake rates and relative abundance correlate positively for FAT/CD36 and FABPpm in white and red skeletal muscle and heart but not for FATP1 [68]. This may argue against a functional role for FATPs in the bulk FA uptake by the heart, but does not exclude a more specific function in the heart, for instance in preferential uptake of FA occurring at lower concentrations or in coupling FA uptake directly to a certain metabolic process. It also does not exclude a significant contribution of FATPs to bulk FA uptake in non-muscle tissues. Interestingly, the FATPs possess acyl-coenzyme A synthetase activity [16], so that these proteins may increase FA uptake by metabolic trapping.
The sulpho-N-succinimidylesters of FA have been proven a valuable tool for studying the role of FAT/CD36 in cellular FA uptake, because they do not influence other uptake processes nor do they interfere with the action of the other putative FA transporters [17]. Sulpho-N-succinimidyloleate (SSO) inhibits cardiac FA uptake by ~80%, which is similar to the inhibitory potential of a polyclonal anti-FABPpm antiserum. Since, however, this antiserum and SSO together do not inhibit FA uptake further [68], i.e. both agents act non-additively, not only at maximally inhibiting concentrations but also at partially inhibiting concentrations, both FABPpm and FAT/CD36 would seem to act as two components of a single FA uptake system [68]. Assessment of the membrane topology of both transporters has revealed that FABPpm is a peripheral membrane protein at the outer leaflet [112], while FAT/CD36 is an integral membrane protein with one or two membrane spanning regions [1, 87]. It is likely that in this putative uptake system FABPpm acts as a receptor for FA, facilitating the diffusion of the FA-albumin complex through the unstirred fluid layer, and that FAT/CD36 mediates the transmembrane passage of FA, possibly by facilitating a flip-flop across the bilayer. Whether FABPpm and FAT/CD36 are, at some stage, in physical contact with each other remains to be established (Fig. 1).
Transporters involved in the uptake of long-chain fatty acids (FA) and glucose across the sarcolemma of cardiac myocytes and their subsequent intracellular transport to their sites of metabolic conversion. For FA the scheme is as follows. Following the dissociation of FA from plasma albumin, FA could either partition directly into the phospholipid bilayer or be bound by plasma membrane FA binding protein (FABPpm), FA translocase (FAT/CD36) or FA transport protein (FATP). The subsequent transmembrane migration of FA could take place either without the involvement of membrane proteins (passive diffusion), or with a membrane protein acting solely as an acceptor for FA (FABPpm) or as a true translocator (FAT, FATP). At the inner side of the sarcolemma, FA binds to cytoplasmic (intracellular) FA binding proteins (FABPc) before entering metabolic or other pathways after activation to fatty acyl-coenzyme A (acyl-CoA) and subsequent transport by acyl-coenzyme A binding protein (ACBP). FATP is involved in the uptake and simultaneous activation of FA. For glucose the scheme is as follows. Unlike FA, glucose, by virtue of its hydrophilic properties, does not need soluble carrier proteins, but is dependent on the presence of glucose transporters (GLUT)-1 and GLUT4 for transmembrane migration. Its intracellular arrival is rapidly followed by phosphorylation to glucose-6-phosphate (G-6-P) and subsequent entrance into metabolic pathways
Our studies on the influence of short-term contractile activity on FA uptake into skeletal muscle have provided the first data showing that FA uptake is subject to short-term regulation [6]: the induction of tetanic contraction markedly enhances muscle FA uptake. Because this increase is sensitive to inhibition by SSO, it appears to involve FAT/CD36. Because there was no de novo protein synthesis of FAT/CD36 during this contraction period, the acute increase in FA uptake can only be explained by either an increase in intrinsic activity of FAT/CD36 through a covalent modification or translocation to the sarcolemma from previously unrecognized intracellular membrane stores. This latter mechanism has been shown to occur in contracting muscle, and bears striking resemblance to the up-regulation of glucose uptake by the well-described translocation of GLUT4 [6]. These initial findings prompted us to investigate the possibility that cardiac FA uptake is also regulated by FAT/CD36 translocation. As a starting point for the identification of possible cellular components involved in FAT/CD36 translocation in cardiac myocytes, we speculated that valuable lessons could be learned from knowledge of GLUT4 translocation in the heart. We will therefore first review the present status of knowledge on the regulation of cardiac glucose uptake.
Regulation of cardiac glucose uptake
Cellular uptake of glucose is primarily a protein-mediated process because of the inability of hydrophilic compounds to traverse phospholipid bilayers. This facilitated transport is mediated by members of the GLUT family that belong to a much larger superfamily of 12-transmembrane segment transporters. Twelve GLUT isoforms have been described to date [51, 111]. The major isoforms present in heart and skeletal muscle are GLUT1 and GLUT4 (Fig. 1). A key mechanism in short-term regulation of glucose uptake is the translocation of both glucose transporters from intracellular stores to the sarcolemma through vesicular trafficking. Insulin and contraction are the two major physiological stimuli of cardiac glucose transport. Of these transporters, the translocation of GLUT4 is by far the most intensively investigated, especially in response to insulin. We will thus first review the signalling pathways and vesicular trafficking components involved in the translocation of GLUT4 in response by either of both stimuli. Subsequently, we will summarize the major findings concerning the regulation of cardiac glucose uptake by GLUT1, and finally compare the subcellular distribution of GLUT1 in cardiac myocytes with that of GLUT4.
GLUT4 and insulin
Under basal, non-stimulated conditions, the majority of GLUT4 is stored intracellularly [103, 135]. Insulin is able to translocate GLUT4 to the cell surface primarily by stimulation of exocytosis [108]. Insulin also decreases the rate of GLUT4 endocytosis approximately two- to threefold in adipose cells [44, 54]. The magnitude of the stimulatory effect of insulin on glucose uptake by cardiac myocytes is reportedly between 2- and 14-fold, and is attributable mainly to GLUT4 translocation [20, 27, 28, 29, 67, 93]. The sequence of intracellular events has been a topic of intensive research and is known to involve activation of the insulin receptor, tyrosine phosphorylation of insulin receptor substrates (IRSs) followed by their binding to and activation of phosphatidylinositol (PI)-3 kinase (PI3K) and subsequent production of PI-3,4,5-(PO4)3. Downstream from PI3K, transduction of the signal becomes more obscure, but it is recognized that protein kinase B (PKB/Akt) and atypical protein kinase C (PKC) isoforms are involved in adipose and skeletal muscle cells [25, 125]. Interestingly, insulin treatment of cardiac myocytes caused the association of PKB/Akt to GLUT4-containing vesicles [58], as has been also shown for adipocytes [11, 43]. This suggests that PKB/Akt phosphorylates component proteins of GLUT4-containing vesicles in response to insulin [62]. More recently, a novel, PI3K-independent signalling pathway with significance in insulin-induced glucose transport has been identified in adipose cells; this pathway originates in caveolae or in lipid rafts, involves tyrosine phosphorylation of the proto-oncogene c-Cbl and results in the activation of a small GTP-binding protein, TC10, a member of the Rho family [59].
The translocation machinery involved in vesicle-mediated shuttling of GLUT4 exhibits many of the features of transport of synaptic vesicles in the presynaptic nerve terminal. The specificity of the transport of these vesicles is safeguarded by soluble N-ethylmaleimide attachment protein receptor (SNARE) proteins according to the principles of the so-called SNARE hypothesis [9, 13]. The hypothesis postulates that, in vesicle trafficking events, a unique vesicle-associated protein (v-SNARE) specifically recognizes and interacts with a cognate target (t)-SNARE protein localized at the target membrane. This hypothesis also provides an attractive framework to ensure that intracellular GLUT4 vesicles, which are mobilized by insulin, are properly targeted to the plasma membrane and do not fuse randomly with other membranes. Indeed, homologues of v-SNAREs—vesicle-associated membrane protein-2 (VAMP2) and VAMP3 and the t-SNAREs syntaxin-4 and 23-kDa synaptosomal-associated protein (SNAP23)—have been identified in adipocytes and skeletal myocytes [101, 107]. Specifically VAMP2 is localized in intracellular GLUT4 containing vesicles and syntaxin-4 and SNAP23 exist almost exclusively in the plasma membrane. Disruption of the function of the syntaxin-4-SNAP23-VAMP2 SNARE complex selectively inhibits the insulin-induced translocation of GLUT4 to the cell surface but not the recruitment of GLUT1 in adipose cells [125]. VAMP3 or cellubrevin is associated with intracellular GLUT4 from endosomal nature in skeletal and cardiac muscles [101] and probably participates in the trafficking of GLUT4 within endosomes or from endosomes to the GLUT4 storage compartment. Several proteins are implicated in regulating the formation of syntaxin-4, SNARE23 and VAMP2 complex in response to insulin. Synip binds to syntaxin-4 in an insulin-dependent manner and prevents VAMP2 binding [80]. Pantophysin and vesicle-associated protein-33 (VAP33) bind to VAMP2 and prevent the association of the v-SNARE into the complex [8, 30].
Other proteins involved in the insulin-induced translocation of GLUT4 are members of the Ras-related Rab GTP-binding proteins. All Rabs bind and hydrolyse GTP, and in their cycling between GTP-bound (active) and GDP-bound (inactive) conformations these proteins act as molecular switches in vesicular trafficking [132]. Although Rabs have not been detected in the SNARE complex, they are probably required for the assembly of this complex, as has been shown in yeast [104]. Members of the Rab family are associated with distinct intracellular compartments involved in endocytic and exocytic processes, indicating that the individual Rab proteins have specialized transport functions. The non-hydrolysable GTP analogue GTPγS, which keeps GTP-binding proteins in a permanently active state, has been instrumental in establishing a role for Rab proteins in the translocation of GLUT4. In adipocytes, which had been permeabilized to allow the cellular entry of non-permeant nucleoside phosphates, the increase in Rab activity upon GTPγS addition induces the translocation of GLUT4 to the plasma membrane in an insulin-like manner [3]. These findings have been confirmed in permeabilized cardiac myocytes [5].
The few studies to date addressing the presence of rab proteins in the heart have revealed the presence of rab1, -3, -4, -5, -6 and -11 [119, 120, 128]. While rab1 and -6 are involved in antegrade and retrograde vesicular trafficking between the endoplasmic reticulum and Golgi stacks [78, 89], rab3, -4, -5 and -11 are candidates for regulating GLUT4 recycling. rab3 and -4 translocate to the plasma membrane of cardiac myocytes in response to insulin [120]. rab4, but not rab3, has been detected in immunopurified GLUT4-containing intracellular vesicles obtained from rat heart [120]. Subsequently, a functional involvement of Rab4 has been demonstrated through its over-expression in H9c2 cardiac myoblasts. Basal glucose uptake is reduced moderately in these cells but insulin-stimulated glucose uptake and surface GLUT4 content increase fourfold, indicating that Rab4 is a key player in the insulin responsiveness of GLUT4 translocation in the heart [21]. More recently, Rab11 has been found to participate in insulin-inducible GLUT4 translocation in cardiac myocytes [57]. Rab11 associates specifically with recycling endosomes in mammalian cell lines [106, 117]. Its association with GLUT4-containing vesicles suggests a role for recycling endosomes in trafficking of GLUT4. Rab5 has been localized to the plasma membrane, clathrin coated vesicles and early endosomes and is postulated to be functioning in endocytic processes, as opposed to both Rab4 and Rab11 that are more likely to be involved in exocytosis [10, 12, 115]. Interestingly, in adipocytes, microinjection of anti-Rab5 increases basal levels of GLUT4 and inhibits GLUT4 internalization upon insulin withdrawal [45]. This suggests a role for Rab5, which associates with the motor protein dynein, in the regulation of GLUT4 distribution in adipose cells.
It is now generally accepted that, in insulin-sensitive tissues, GLUT4 is found at least in two distinct intracellular compartments [2, 84, 101, 107]. In rat skeletal muscle, the insulin-responsive intracellular pool with the lowest buoyant density coincides with endosomal proteins such as the transferrin receptor, annexin II, secretory carrier membrane proteins (SCAMPs) or cellubrevin, while the heavier fraction containing the majority of intracellular GLUT4 is depleted of the transferrin receptor and is enriched in an 160-kDa insulin-responsive aminopeptidase (IRAP) and in VAMP2 [2, 84, 101]. In rat cardiac myocytes, GLUT4 is distributed in an endosomal pool that contains SCAMPs, GLUT1, insulin-like growth factor (IGF)-II receptors and into a unique non-endosomal intracellular membrane pool [4, 29]. It is likely that rab11 associates with the endosomal GLUT4 pool in rat heart [57]. Based on these observations in skeletal muscle and in cardiac myocytes, we propose that GLUT4 is distributed in two major pools: a GLUT4 storage compartment that contains most of GLUT4 and is translocated to the sarcolemma in response to insulin, and an endosomal GLUT4 compartment that may respond to other signals. The GLUT4 storage compartment is enriched in IRAP and in VAMP2 which is in keeping with the observations performed in adipose cells. [18, 53]. The mechanisms that control the generation of the GLUT4 trafficking pathway remain unknown. In this regard, muscle denervation causes a marked repression of GLUT4, but does not affect the level of expression of component proteins of intracellular vesicles such as IRAP, VAMP2, transferrin receptors, IGF-II receptors or SCAMPs [134]. In addition, in muscle from GLUT4−/− mice, trafficking of the transferrin receptor is not different from that in the wild-type, while IRAP displays an abnormal subcellular distribution and an impaired recruitment to the sarcolemma in response to insulin [49]. These findings suggest that despite the fact that GLUT4 is not involved in the expression of other component proteins, this glucose transporter has a pivotal role in defining the exocytic storage compartment. The storage compartment and its component proteins are considered to be uniquely dedicated to trafficking of GLUT4 in response to insulin. In contrast, the recycling endosomes fulfil a variety of other functions besides GLUT4 recruitment [12, 106, 115, 117].
GLUT4 and contraction
The ability to induce GLUT4 translocation is not restricted to insulin, but can also be achieved by a drop in oxygen supply (anoxia/ischaemia) and by mitochondrial inhibitors [127] and, physiologically most relevant, by an increase in mechanical activity of the heart [41]. All these factors induce GLUT4 translocation independently of insulin signalling, because inhibition of PI3K does not interfere with their ability to induce GLUT4 translocation [75, 116, 129]. The notion that these factors each induce metabolic stress suggests that they share a common signalling pathway. Recently, this pathway has been shown to include AMP-activated protein kinase (AMPK), which is activated by a stress-induced rise in intracellular AMP and a concomitant drop in ATP [40, 91]. Other evidence for an involvement of AMPK comes from studies using the cell-permeable agent 5-aminoimidazole-4-carboxyamide-1-β-d-ribofuranoside (AICAR). This adenosine analogue is taken up readily by cells and subsequently 5′-phosphorylated to ZMP, which in turn activates AMPK selectively and increases glucose uptake in a manner that is not reversible by addition of the PI3K-specific inhibitor wortmannin [42, 79]. However, the involvement of AMPK is not undisputed. For instance, AMPK activation in skeletal muscle is prevented by preloading with glycogen prior to exercise, but nonetheless contraction-inducible glucose uptake is preserved [19]. On the other hand, expression in mouse muscle of a dominant inhibitory mutant of AMPK completely blocks the stimulation of glucose uptake by AICAR or hypoxia [81]. The difficulty in establishing a causal link between AMPK activation and glucose uptake resides in the fact that a specific inhibitor of AMPK is not yet available. The downstream targets of AMPK that are involved in GLUT4 translocation await their identification. The ability of specific protein kinase C (PKC) inhibitors to inhibit contraction-inducible glucose uptake into skeletal muscle suggests an involvement of one or more PKC isoforms. Furthermore, PKCζ and components of the extracellular signal-regulated kinase (ERK) pathway have been found to be downstream from AMPK, based on the ability of their specific inhibitors myristoylated PKCζ pseudosubstrate and PD98059, respectively, to inhibit AICAR-induced GLUT4 translocation in mouse skeletal muscle [14].
GLUT1
GLUT1 has a much more ubiquitous tissue distribution than GLUT4, which is restricted mainly to insulin-sensitive, extrahepatic tissues. Compared with other tissues, the heart expresses a relatively large amount of GLUT1 [29]. In contrast to GLUT4, which is stored predominantly intracellularly, GLUT1 has a more pronounced sarcolemmal localization and has been regarded generally as mediating basal glucose uptake. However, for the heart evidence is accumulating that intracellularly stored GLUT1 can also be recruited by insulin [4, 29] and by contraction or manipulations acting on contraction signalling in perfused hearts or in isolated cardiac myocytes [4, 127]. Quantitatively, the effect of insulin on the surface appearance of GLUT1 (1.5- to 2.7-fold increase) is moderate compared with that of GLUT4 (2.6- to 5.6-fold increase; [23, 29, 95]). It is likely that some of the variability observed in the different studies stems from the utilization of perfused rat heart preparations on the one hand and isolated rat cardiomyocytes on the other. The latter model is characterized by a lower basal glucose transport rate due to a lower abundance of GLUT1 in the plasma membrane under basal conditions. In contrast to the effect of insulin, the effect of mitochondrial inhibitor rotenone (which activates contraction signalling) on the extent of translocation of GLUT1 is similar to that of GLUT4 [127]. The signalling mechanisms involved in the translocation of GLUT1 are remarkably similar to that of GLUT4 in that PI3K is involved in insulin-induced GLUT1 translocation, but not in ischemia (contraction-signalling)-induced GLUT1 translocation [23]. The effect of ischaemia [23, 131] or rotenone [4, 127] on surface GLUT1 is of a similar magnitude to that of insulin, i.e. an ~1.5-fold increase. The comparison of the effects of insulin and contraction signaling on translocation of GLUT1 and GLUT4 will be used below (see section Comparison of glucose and FA uptake) to shed light on possible similarities with recycling of FA transporters.
Intracellular storage of GLUT1 and GLUT4
Comparison of intracellular storage of GLUT4 with that of GLUT1 in non-stimulated cardiac myocytes, using immunotitration with an anti-GLUT4 antibody, has identified two distinct intracellular GLUT4 storage sites [4, 29]. One site of intracellular GLUT4 is shared with the complete intracellular population of GLUT1, and contains other endosomal proteins such as the transferrin receptor and Rab11, identifying this site as the recycling endosomes [57]. The other site is entirely devoid of GLUT1 [4] and most probably represents the GLUT4 storage compartment. Interestingly, rotenone induces GLUT1 and GLUT4 translocation mainly from the endosomal compartment, while insulin recruits GLUT4 from the storage compartment and also GLUT1 from the endosomal compartment [4]. The separation between intracellular GLUT1 and the GLUT4-specific storage compartment is further substantiated by over-expression of Rab4 in cardiac myocytes. Rab4 over-expression decreases the cell surface abundance of GLUT4, while not affecting GLUT1 distribution [21]. Moreover, a synthetic peptide corresponding to the N-terminus of VAMP2 inhibits insulin-inducible GLUT4 translocation, but not insulin-inducible GLUT1 translocation in adipocytes [77].
Taken together, these findings are compatible with the existence of a minimum of two and a maximum of three distinct glucose transporter pools in the heart. The first pool is the GLUT4 storage compartment, which contains GLUT4 but not GLUT1 and permits the translocation of GLUT4 to the plasma membrane in response to insulin. The second pool is formed by the endosomal compartment that contains both GLUT4 and GLUT1 and responds to rotenone and to insulin; rotenone recruits GLUT4 and GLUT1, whereas insulin only recruits GLUT1 from the endosomal pool. This pool may in theory permit the response to contraction. A third pool, for which there is not yet experimental support in cardiac myocytes, may be proposed: the contraction-responsive GLUT4 compartment. We propose this third compartment on the basis of observations in skeletal muscle that indicate the existence of a postendocytic, contraction-responsive GLUT4 compartment. However, we stress that this compartment may not exist in cardiac myocytes. Currently available estimates in skeletal muscle indicate that the storage pool contains 40–60% of the intracellular GLUT4.
Comparison of glucose and FA uptake
The similarities between the regulation of cardiac FA and glucose uptake are striking. Notably, both processes are up-regulated by the same physiological stimuli and, moreover, both use the same basic mechanism of regulation, i.e. recycling of substrate transporters between intracellular membrane compartments and the sarcolemma. However, subtle differences exist. These similarities and differences are being discussed alongside the following issues.
Involvement of passive diffusion
The uptake of glucose is dependent on the involvement of transporters, as the hydrophilic substrate is unable to cross the phospholipid bilayer. However, FA readily partitions in biological membranes [38, 39] and its uptake is inhibited incompletely by transport inhibitors or protein-modifying agents [68]. Since the rate of passive diffusion is governed by physicochemical properties of the phospholipid bilayer and obeys the laws of thermodynamics, the process is unlikely to be subject to acute regulation. We can assume safely that passive diffusion of FA is not affected directly by contraction or insulin, since the absolute rate of non-inhibitable FA uptake is not altered in the presence of these stimuli [70, 72]. This implies that the passive diffusion component in the FA uptake process has a damping effect on the stimulation of FA uptake by insulin or contraction.
Storage of FA and glucose transporters in non-stimulated cardiac myocytes
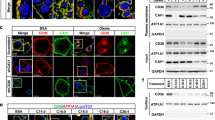
There is general agreement that the majority of GLUT4 is stored intracellularly under basal conditions (see above, GLUT4 and insulin). In concordance, our fractionation studies (Fig. 2) demonstrate a markedly (two- to threefold) greater abundance of GLUT4 in a low-density microsomal fraction (LDM; intracellular membrane fraction, presumably containing endosomes) than in a plasma membrane fraction (PM). In addition, we have confirmed that, under basal conditions, GLUT1 has a more pronounced sarcolemmal localization than GLUT4, because the amount of GLUT1 in the PM is similar to that in the LDM. Examining the presence of FAT/CD36 within these fractions, it is obvious that its equal distribution between PM and LDM more closely resembles that of GLUT1 than that of GLUT4 (Fig. 2). In addition, FAT/CD36 is present equally in both sarcolemmal and microsomal membranes in non-stimulated cardiac myocytes [83]. Moreover, Western blot analysis of immunoabsorbed GLUT4 vesicles reveals that these vesicles lack FAT/CD36, providing convincing evidence for an intracellular storage of FAT/CD36 that is different from that of GLUT4. FAT/CD36 also colocalizes with Rab11. Combining these pieces of evidence carefully pinpoints the endosomes, harbouring the complete population of intracellular GLUT1, as suitable candidates for intracellular storage of FAT/CD36. It remains to be established whether the intracellular localization of the storage compartment marker IRAP is distinct from that of FAT/CD36.
Comparison of cellular distribution of GLUT4, GLUT1 and FAT/CD36, caveolin-3 (Cav3) and the transferrin receptor (TfR) in the plasma membrane (PM) or low-density microsomal (LDM) fractions under basal (non-stimulated) conditions. GLUT1 and GLUT4 were both detected at 45 kDa, FAT/CD36 at 88 kDa, caveolin-3 at 24 kDa and the transferrin receptor at 95 kDa. It must be mentioned that, despite the assumption that the GLUT4 specific storage pool is missing in the LDM fraction, the minute presence of GLUT4 in the sarcolemma of non-stimulated cardiac myocytes, compared with that of GLUT1, still allows the conclusion that basal GLUT4 localization is more intracellular than that of GLUT1
In contrast to FAT/CD36, FABPpm is markedly more abundantly expressed in the PM than in the LDM under basal (non-stimulated) conditions, suggesting that its storage within an endosomal compartment is relatively small compared with that of other transporters. Translocation processes will thus make only a minor contribution to the regulation of the sarcolemmal content of FABPpm. As a verification of the fractionation procedure, the sarcolemmal marker caveolin-3 resides mainly in the PM fraction, and the transferrin receptor mainly in the LDM.
Regulation by insulin
While it is appreciated that insulin favours esterification of FA into cellular triacylglycerol stores in skeletal muscle [22, 71, 85] and heart [72], the ability of insulin to stimulate FA utilization at the sarcolemmal level has only been explored recently. In cardiac myocytes insulin stimulates FA uptake 1.5-fold [72]. This stimulation can be prevented by SSO and by wortmannin indicating that (i) FAT/CD36 is responsible for the increase in FA uptake and (ii) activation of PI3K is required. Furthermore, insulin decreases the amount of FAT/CD36 in the LDM fraction by 47% and simultaneously increases the amount of FAT/CD36 in the PM fraction 1.5-fold [72, 74]. It is therefore likely that insulin induces FA uptake through translocation of FAT/CD36 from intracellular stores to the sarcolemma. Apparently, insulin mobilizes FAT/CD36 to the sarcolemma, just as it mobilizes GLUT1 and GLUT4 from intracellular stores. However, the magnitude of the effect of insulin on FAT/CD36 translocation is more similar to that of GLUT1 (the surface appearance of which is also enhanced 1.5-fold) than that of GLUT4 (the surface appearance of which more than doubles). Combined with the similarity of FAT/CD36 subcellular distribution to that of GLUT1 rather than GLUT4 under basal, non-stimulated conditions (see previous section), this adds further evidence in favour of the hypothesis that storage of intracellular FAT/CD36, just as that of GLUT1, is confined to the endosomal compartment.
The involvement of insulin in the regulation of FA uptake is an entirely novel role for this hormone, and could have consequences for altered FA fluxes in syndromes of insulin deficiency or resistance. The relatively modest stimulation of FA uptake by insulin, compared with that of glucose, does not mean that this effect of insulin is functionally less significant. In this respect, intracellular FA are known to be powerful mediators of signal transduction as they are the main physiological ligands of the peroxisome proliferator-activated receptors [33]. Furthermore, intracellular FA and metabolites are more toxic to cells than glucose and its metabolites. For instance, high levels of intracellular “free” FA exert detergent-like effects on biological membranes and inhibit the catalytic activity of many enzymes [35] and accumulation of certain FA metabolites, such as acyl-CoA and acyl-carnitine, cause arrhythmias and can impair cardiac functioning severely [63]. This implies that cellular systems cannot allow the intracellular FA concentration to fluctuate to the same extent as with glucose.
Regulation by contraction
While the consequences of an increase in workload on cardiac energy metabolism have been investigated extensively [66, 113], the impact of an increase in contractile activity on FA uptake by cardiac myocytes has been explored only poorly. When cardiac myocytes are stimulated electrically at varying stimulation frequencies, both FA uptake and glucose uptake rise with stimulation frequency. At 4 Hz, this increase is 1.5-fold for both substrates [70]. The contraction-induced increase in FA uptake is blocked completely by SSO. The increase in FA uptake in the presence of contraction is thus linked causally to increased involvement of FAT/CD36. In the search for a signal transduction pathway, we can exclude a role for PI3K since wortmannin does not inhibit contraction-inducible FA uptake [72], indicating that different mechanisms are involved in contraction-inducible and insulin-inducible FA uptake. We can also exclude a role for cyclic AMP-dependent protein kinase A, because manipulations increasing intracellular cyclic AMP, e.g. the membrane-permeant cyclic AMP analogue dibutyryl cyclic AMP, the β-agonist isoproterenol and the phosphodiesterase III inhibitor amrinone, all fail to alter FA uptake into cardiac myocytes [73].
Another attractive candidate signalling enzyme for the mediation of contraction-inducible FA uptake is AMPK, because it is already known to be involved in another aspect of cardiac FA utilization. An important target for AMPK is namely acetyl-CoA carboxylase, which AMPK inhibits by phosphorylation, resulting in a drop in intracellular malonyl-CoA levels and a de-inhibition of carnitine palmitoyltransferase-I (CPT-I) [65]. The combined induction of FA uptake and of CPT-I activity through AMPK activation is then likely to be metabolically efficient, as this allows the extra incoming FA to be channelled preferentially into mitochondrial β-oxidation. In addition, as mentioned earlier, AMPK is known to be involved in stimulation of glucose uptake by translocation of GLUT4 to the sarcolemma (see above: GLUT4 and contraction). Indeed, electrical stimulation of cardiac myocytes elevates the intracellular AMP/ATP ratio 1.9-fold and stimulates AMPK activity 3.3-fold [74]. Pharmacological evidence for the involvement of AMPK in contraction-inducible FA uptake has been provided by studying the effects on FA uptake of the mitochondrial inhibitor oligomycin and the cell-permeable adenosine analogue AICAR, both of which stimulate glucose uptake and GLUT4 translocation (see above: GLUT4 and contraction). Both oligomycin and AICAR stimulate AMPK activity markedly (more than fivefold) and FA uptake up to twofold [74]. Moreover, 4-Hz stimulation loses its enhancing effect on FA uptake into cardiac myocytes when the latter are treated simultaneously with either oligomycin or AICAR, indicating a common mechanism. Additional evidence for a common mechanism in the stimulating effects of contractions, oligomycin and AICAR on FA uptake is the observation that the PI3K inhibitor oligomycin is unable to block either action. The mechanism has been shown to involve a translocation of FAT/CD36 from intracellular stores to the sarcolemma. In this respect, subcellular fractionation experiments indicate that activation of AMP kinase by oligomycin results in a 49% depletion of FAT/CD36 from an intracellular membrane compartment and a concomitant 1.5-fold increase at the sarcolemma [74]. Remarkably, the relative extent of up-regulation of FAT/CD36 at the cell surface by AMPK activation is very similar to that of GLUT1 and GLUT4. Since both contraction-inducible GLUT1 and GLUT4 are stored in the recycling endosomes, it may be speculated that they share this intracellular storage site with contraction-inducible FAT/CD36. Thus, these recycling endosomes harbour FAT/CD36 that is mobilized by contraction-induced activation of AMPK as well as by insulin-induced activation of PI3K (see previous section). Because insulin and contraction are likely to operate independently of each other, this implies that there must be distinct sorting mechanisms, to respond to either stimulus, present within the recycling endosomes. However, because a specific inhibitor of AMPK is not yet available, a causal relationship between AMPK activation and FAT/CD36 translocation, just as with GLUT4 translocation, is difficult to establish. To date, the strongest evidence for such a relationship comes from the ability of 5-iodotubercidin, an adenosine kinase inhibitor that prevents the conversion of AICAR to ZMP, to block the AICAR-induced increase in FA uptake completely [74].
Differential effects of various mitochondrial inhibitors on uptake of FA and glucose
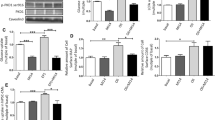
Mitochondrial inhibitors have been used frequently to mimic pharmacologically the effect of contraction on ATP utilization. Accordingly, rotenone, 2,4-dinitrophenol (DNP) and oligomycin all similarly enhance the AMP level twofold (Fig. 3), leading to activation of AMPK. In addition all of them have proven successful in stimulating glucose uptake and GLUT4 translocation (Fig. 3, see also [5, 31, 127]). However, only oligomycin enhances FA uptake, whereas DNP and rotenone inhibit this process rather substantially (Fig. 3). Remarkably, the underlying mechanisms between DNP and rotenone must be different, since these inhibitors exert opposite effects on FA oxidation (Fig. 3).
Effects of mitochondrial inhibitors on cardiomyocyte AMP levels, glucose uptake and FA uptake and oxidation by cardiac myocytes: comparison with electrical stimulation. Cell suspensions were incubated for 15 min in the absence of additions (control, Ctrl), in the presence of electrical field stimulation at 200 V and 4 Hz (4 Hz), or with 10 μM 2,4-dinitrophenol (DNP), 3 μM rotenone (ROT), or 30 μM oligomycin (Oli) prior to the metabolic measurements. Cardiomyocyte AMP levels are normalized to those of ATP, which does not change significantly in the presence of the different manipulations [74]. The cellular content of adenosine phosphates was determined by HPLC according to [121]. Determination of deoxyglucose uptake (3 min), palmitate uptake (3 min) and oxidation (30 min) was carried out as described earlier [67]. Means±SD, n=4 experiments on different cardiomyocyte preparations. *P<0.05 vs. control
With respect to rotenone, its blockade of the electron transport chain arrests the Krebs’ cycle and thus reduces FA oxidation. Our earlier work suggested that palmitate uptake and oxidation are tightly coupled. For example, treatment of cardiac myocytes with the CPT-I inhibitor etomoxir completely arrests FA oxidation and inhibits FA uptake by 50% [67]. In addition, etomoxir has no direct effect on FA uptake, i.e. at the level of the sarcolemma [36], indicating that the etomoxir-imposed inhibition of FA uptake is secondary to the fall in FA oxidation. Likewise, rotenone inhibits FA uptake through a blockade of FA oxidation.
The fall in palmitate uptake by cardiac myocytes treated with the uncoupling agent DNP, however, is not due to an arrest of aerobic metabolism. Accordingly, despite the decrease in FA uptake FA oxidation in the presence of DNP is increased. This indicates that the reduction in FA uptake is compensated for by more efficient channelling of FA into oxidative pathways, probably at the expense of esterification into cellular lipid pools. This channelling is then made possible by the AMPK-induced phosphorylation and inhibition of acetyl-CoA carboxylase and a concomitant increase in mitochondrial β-oxidation [65]. As an explanation for its inhibitory action on FA uptake, we speculate that this mitochondrial uncoupler has non-specific side effects on proton gradients across other membranes at the cellular level, and consequently destroys the membrane potential at the level of the sarcolemma. Since FA uptake is reportedly dependent on the membrane potential [24, 126], DNP’s inhibitory effect on FA uptake is then caused through this mechanism.
Of all tested mitochondrial inhibitors, oligomycin mimics most closely the effects of contraction on substrate utilization by myocytes in that it enhances both FA and glucose uptake. Oligomycin is a potent inhibitor of the mitochondrial F1F0-ATPase and, as such, has long been used to inhibit state-3 respiration in isolated mitochondria [37]. Because of the tight coupling between FA oxidation and FA uptake, oligomycin would be expected to reduce FA uptake under these anaerobic conditions rather than to stimulate it. However, a recent study has demonstrated that the concentration of oligomycin required for 50% inhibition (IC50) of the mitochondrial F1F0-ATPase is fivefold lower than its IC50 for inhibition of electron flux through the respiratory chain [130]. This discrepancy opens a window of oligomycin concentrations at which the intracellular AMP is elevated while, simultaneously, oxygen consumption is not inhibited. Accordingly, at concentrations of 5–100 μM, oligomycin elevates intracellular AMP and simultaneously enhances FA uptake and oxidation [74].
In conclusion, DNP and oligomycin share with contractile activity the ability to efficiently channel FA upon its cellular entry towards oxidative metabolism. It remains to be established whether the AMP-enhancing action of rotenone, despite its mitigating action on FA oxidation, is still sufficient to trigger translocation of FAT/CD36 to the cell surface. If so, the coupling between translocation of the GLUTs and translocation of FAT/CD36 would be retained, despite the opposite effects of rotenone on FA and glucose uptake (see above, GLUT1).
Mutual dependence of FA transporters: comparison with glucose transporters
As mentioned above (Regulation of cardiac FA uptake), FAT/CD36 and FABPpm together are responsible for 70–80% of the FA influx into the heart. However, FAT/CD36- and FABPpm-mediated FA uptakes are not additive. In contrast, glucose uptake into adipose and muscle tissues is regarded as the sum of the transport actions of GLUT1 and GLUT4 [82]. Hence, the two cardiac FA transporters have a different mutual relationship than the two cardiac glucose transporters. The two cardiac glucose transporters GLUT1 and GLUT4, although translocated to the sarcolemma by the same stimuli, operate independently of each other and, therefore in parallel. In contrast, the two FA transporters FAT/CD36 and FABPpm most probably act as two components of a single transport system, and thus are positioned in series. As a putative receptor for FA, FABPpm is present constitutively at the cell surface, while FAT/CD36 recycles between endosomes and the sarcolemma. Of these two transporters, FAT/CD36 is the major site of flux control. This notion is based on the following lines of evidence. First, in heart and other tissues FABPpm is an abundantly expressed protein [133] so that its availability is unlikely to be rate limiting. Second, there is a better relationship between the amount of sarcolemmal FAT/CD36 and FA uptake rates into giant vesicles derived from different mammalian tissues than between sarcolemmal FABPpm and giant vesicle FA uptake rates, both under basal [61, 68] and pathological conditions [7]. Third, the relative increase in FA uptake into cardiac myocytes elicited by insulin or contraction is similar to the increases in the sarcolemmal content of FAT/CD36 due to translocation from endosomal sources [72, 74]. Hence, insulin or the onset of contraction activates signalling events resulting in translocation of FAT/CD36 to the sarcolemma, after which, supposedly, an interaction will be established with FABPpm. Whether specific sarcolemmal microdomains exist that may act as docking sites for endosomally delivered FAT/CD36 and simultaneously harbour significant populations of FABPpm is an intriguing possibility that remains to be established. An interesting candidate domain could be presented by the caveolae that are known to accommodate a number of receptors and transporters. These 100-nm, flask-shaped invaginations of the sarcolemma are abundant in cardiac myocytes [26, 64]. In addition, cardiac myocytes express relative large quantities of caveolin-3, the major constituent of caveolae [105]. Interestingly, it has been established that cholesterol-complexing agents that disrupt the structural integrity of caveolae markedly reduce FA uptake into hepatoma cells [90]. These findings suggest an important role for caveolae in cellular FA uptake. With respect to glucose uptake and GLUT4 recycling, there are also indications for an involvement of caveolae, although this still is a controversial issue. For instance, caveolin-3 does not colocalize with GLUT4 at the cell surface of skeletal muscle fibres [92]. In adipocytes, however, insulin induces the translocation of GLUT4 to caveolae [55, 76]. Furthermore, adipocytic caveolae are known to play a crucial role in internalization of GLUT4 upon insulin withdrawal [97]. Whether caveolae play comparable roles in GLUT4 and FAT/CD36 recycling is another intriguing research question.
Integrated model for recycling of FA and glucose transporters in cardiac myocytes
The available evidence suggests that intracellular FAT/CD36 is stored in a single endosomal pool. We propose that this intracellular pool is identical to the endosomal compartment that contains both GLUT4 and GLUT1, and that this compartment responds to AMPK activation and to insulin signalling. As a consequence, the FAT/CD36-containing pool represents an endosomal population and also contains both GLUT1 and GLUT4. The additivity of AMPK activation and insulin signalling with respect to FA and glucose uptake [72, 74, 75, 116, 129] indicates that within this endosomal compartment there must be (at least) two independently operating sorting mechanisms for recruitment of FAT/CD36 and GLUTs, most probably involving different SNARE proteins and Rabs. A candidate Rab protein in insulin-inducible transporter translocation from this compartment could be Rab11, because it is associated with both GLUT4 and FAT/CD36 and redistributes to the sarcolemma upon insulin stimulation [57, 83, 106, 117]. Its counterpart involved in AMPK-inducible transporter translocation is still hypothetical.
FAT/CD36 storage resembles that of GLUT1 more closely that that of GLUT4, since GLUT4 is also stored in a unique insulin-sensitive compartment. GLUT1, and probably also FAT/CD36, lack this kind of intracellular storage. This makes the insulin-inducible recruitment of GLUT4 a magnitude greater than its contraction-inducible recruitment, or recruitment of FAT/CD36 or GLUT1 by insulin or contraction. We do not know yet whether GLUT4, GLUT1 and FAT/CD36 travel together within the same recycling endosomal vesicles or whether they are stored in independent subcompartments, but still use the same signalling processes for their recruitment. A hypothetical model for FAT/CD36 recycling in relation to that of GLUT1 and GLUT4 is depicted in Fig. 4.
Hypothetical model of FAT/CD36 translocation in relation to that of GLUT1 and GLUT4. FAT/CD36, just as the transferrin receptor, GLUT1 and a minor portion of GLUT4, migrates upon activation of AMP-activated protein kinase (AMPK, through muscle contraction) or phosphatidylinositol-3 kinase [PI3K, initiated by insulin binding to the insulin receptor (IR)] from an endosomal compartment (recycling endosomes) to the sarcolemma. AMPK-dependent mobilization is assisted by RabX, a hypothetical member of the Rab family involved in contraction-dependent recycling, whereas PI3K-dependent mobilization is presumably mediated by Rab11. In parallel, the majority of GLUT4 present in the exocytotic storage compartment together with Rab4 and an insulin-responsive aminopeptidase (IRAP) is moved in response to insulin to the sarcolemma. We speculate that the segregation of intracellular FAT/CD36 from the majority of intracellular GLUT4 present in the storage compartment is extended to the level of the sarcolemma. In agreement with this view, surface GLUT4 derived from the storage compartment, is confined to a specific sarcolemmal region that is distinct from the surface docking site for recycling proteins. Both docking sites possess unique target soluble N-ethylmaleimide attachment protein receptors (t-SNAREs) (tRE t-SNARE involved in docking of recycling endosomes, tSC t-SNARE involved in docking of vesicles from the storage compartment) for binding to their cognate vesicle-SNAREs (v-SNAREs) at the recycling endosomes (vRE) or the storage compartment (vSC), respectively. Based on this, we envisage two systems, the first being the continuum between the recycling endosomes and their surface docking sites, and the second being vesicular trafficking between the storage compartment and its surface docking site. These systems may operate independently of each other, which precludes a mixing between their putative intracellular and sarcolemmal pools of transporters
Future perspectives
It is becoming increasingly evident that translocation events play a more common role in the regulation of substrate utilization than previously realized after the initial discovery of GLUT4 recycling in adipocytes [56, 60]. This was followed by the observation that another glucose transporter, GLUT1, also shuttles between intracellular stores and the cell surface [99]. At present, we should take into consideration that transporter recycling is also involved in the regulation of FA uptake. While we have established recently that contraction and insulin induce the translocation of FAT/CD36 in skeletal muscle and heart [6, 71, 72, 74], other FA transporters, e.g. FATP-1 and -4, are translocated to the cell surface in adipocytes in response to insulin [109]. Interestingly, in skeletal muscle insulin is able to induce the sodium-dependent uptake of neutral amino acids by translocation of the amino acid transport system A to the sarcolemma [46]. It is indeed possible that recycling of transporters is the standard, while their constitutive presence at the sarcolemma, in case of FABPpm (see above: Storage of FA and glucose transporters in non-stimulated cardiac myocytes) and also in case of the cardiac monocarboxylate transporter MCT1 [50], is the exception to the rule.
Cardiac disease has often been linked to a change in substrate preference. For example, cardiac hypertrophy is associated with a shift in the utilization from FA to glucose [52, 123], while on the other hand the diabetic heart prefers FA at the expense of glucose [96, 102, 118]. In obese Zucker rats, a rodent model for insulin resistance and obesity, FA uptake into the heart is increased twofold [69]. This increase is not accompanied by a change in protein expression of FAT/CD36 or FABPpm, but is paralleled by an increased abundance of FAT/CD36 at the sarcolemma at the expense of intracellular storage. At present, we do not know whether this permanent relocation of FAT/CD36 to the sarcolemma is a normal physiological response to elevated circulating insulin levels, as observed in obese Zucker rats, or otherwise is due to chronic alterations in the FAT/CD36 translocation machinery. It is therefore of pivotal importance to unravel the molecular mechanisms of FAT/CD36 translocation, notably the rate-limiting step in FA utilization. Especially the differences with the regulation of translocation of glucose transporters can help to identify therapeutic strategies to allow selective manipulation of substrate transporter recruitment and/or internalization, and therefore restore the cardiac substrate balance. It is expected that normalization of cardiac substrate utilization will lead to improvement of cardiac functioning.
An attractive therapeutic target is possibly represented by the endosomal compartment that is involved in storage of FAT/CD36 and GLUTs. These endosomes constitute a highly organized subcellular structure in which a multitude of trafficking processes involved in sorting of proteins or other macromolecules with different destinations are carried out with a remarkable degree of specificity. Alongside the unmasking of the components involved in vesicular trafficking of GLUT4 and the transferrin receptor, it is becoming evident that this sorting is safeguarded by unique molecular mechanisms that we now are just beginning to understand. It will be the challenge in future research to find the specific v-SNAREs and t-SNAREs, Rabs and other proteins involved in vesicle fission and fusion, that are dedicated to trafficking of FAT/CD36 between the cell surface and its intracellular compartment.
Abbreviations
- AICAR :
-
5-aminoimidazole-4-carboxyamide-1-β-d-ribofuranoside, cell-permeable activator of AMPK
- AMPK :
-
AMP-activated protein kinase
- amrinone :
-
specific inhibitor of phosphodiesterase III
- CPT-I :
-
carnitine palmitoyl transferase I
- dibutyryl cyclic AMP :
-
cell-permeable analogue of cyclic AMP, mimics cyclic AMP-activated signalling
- DNP :
-
2,4-dinitrophenol, mitochondrial uncoupling agent
- ERK :
-
extracellular signal-regulated kinase
- etomoxir :
-
specific inhibitor of CPT-I
- FA :
-
long-chain fatty acid(s)
- FABPpm :
-
plasma membrane fatty acid-binding protein
- FAT/CD36 :
-
fatty acid translocase/CD36
- GTPγS :
-
guanosine 5′-O-(3-thiotriphosphate), non-hydrolysable GTP analogue, locks Rab proteins in a persistently active state
- IGF-II :
-
insulin-like growth factor II
- 5-iodotubercidin :
-
specific inhibitor of adenosine kinase, prevents conversion of AICAR into ZMP
- IRAP :
-
insulin-responsive aminopeptidase
- IRS :
-
insulin receptor substrate
- isoproterenol :
-
potent β-agonist
- myristoylated PKCζ pseudosubstrate :
-
cell-permeable, specific inhibitor of atypical PKCs
- oligomycin :
-
potent inhibitor of mitochondrial F1F0-ATPase
- PD98059 :
-
specific inhibitor of mitogen-activated protein kinase signalling
- PI3K :
-
phosphatidylinositol-3 kinase
- PKB (PKB/Akt):
-
protein kinase B
- PKC :
-
protein kinase C
- rotenone :
-
inhibitor of electron transfer in mitochondria
- SCAMP :
-
secretory carrier membrane protein
- SNAP23 :
-
synaptosomal-associated protein (23 kDa)
- SNARE :
-
soluble N-ethylmaleimide attachment protein receptor
- SSO :
-
sulpho-N-succinimidyloleate, specific inhibitor of transport function of FAT/CD36
- VAMP2 (-3):
-
vesicle-associated membrane protein-2 (-3)
- VAP33 :
-
vesicle-associated protein 33
- wortmannin :
-
inhibitor of PI3K
- ZMP :
-
5′-monophosphate of AICAR
References
Abumrad NA, el-Maghrabi MR, Amri EZ, Lopez E, Grimaldi PA (1993) Cloning of a rat adipocyte membrane protein implicated in binding or transport of long-chain fatty acids that is induced during preadipocyte differentiation. Homology with human CD36. J Biol Chem 268:17665–17668
Aledo JC, Lavoie L, Volchuk A, Keller SR, Klip A, Hundal HS (1997) Identification and characterization of two distinct intracellular GLUT4 pools in rat skeletal muscle: evidence for an endosomal and an insulin-sensitive GLUT4 compartment. Biochem J 325:727–732
Baldini G, Hohman R, Charron MJ, Lodish HF (1991) Insulin and nonhydrolyzable GTP analogs induce translocation of GLUT 4 to the plasma membrane in alpha-toxin-permeabilized rat adipose cells. J Biol Chem 266:4037–4040
Becker C, Sevilla L, Tomas E, Palacin M, Zorzano A, Fischer Y (2001) The endosomal compartment is an insulin-sensitive recruitment site for GLUT4 and GLUT1 glucose transporters in cardiac myocytes. Endocrinology 142:5267–5276
Bergemann C, Loken C, Becker C, Graf B, Hamidizadeh M, Fischer Y (2001) Inhibition of glucose transport by cyclic GMP in cardiomyocytes. Life Sci 69:1391–1406
Bonen A, Luiken JJFP, Arumugam Y, Glatz JFC, Tandon NN (2000) Acute regulation of fatty acid uptake involves the cellular redistribution of fatty acid translocase. J Biol Chem 275:14501–14508
Bonen A, Luiken JJ, Glatz JFC (2002) Regulation of fatty acid transport and membrane transporters in health and disease. Mol Cell Biochem 239:181–192
Brooks CC, Scherer PE, Cleveland K, Whittemore JL, Lodish HF, Cheatham B (2000) Pantophysin is a phosphoprotein component of adipocyte transport vesicles and associates with GLUT4-containing vesicles. J Biol Chem 275:2029–2036
Bryant NJ, Govers R, James DE (2002) Regulated transport of the glucose transporter GLUT4. Nat Rev Mol Cell Biol 3:267–277
Bucci C, Parton RG, Mather IH, Stunnenberg H, Simons K, Hoflack B, Zerial M (1992) The small GTPase rab5 functions as a regulatory factor in the early endocytic pathway. Cell 70:715–728
Calera MR, Martinez C, Liu H, Jack AK, Birnbaum MJ, Pilch PF (1998) Insulin increases the association of Akt-2 with Glut4-containing vesicles. J Biol Chem 273:7201–7204
Chavrier P, Parton RG, Hauri HP, Simons K, Zerial M (1990) Localization of low molecular weight GTP binding proteins to exocytic and endocytic compartments. Cell 62:317–329
Cheatham B (2000) GLUT4 and company: SNAREing roles in insulin-regulated glucose uptake. Trends Endocrinol Metab 11:356–361
Chen HC, Bandyopadhyay G, Sajan MP, Kanoh Y, Standaert M, Farese RV Jr, Farese RV (2002) Activation of the ERK pathway and atypical protein kinase C isoforms in exercise- and aminoimidazole-4-carboxamide-1-beta-d-riboside (AICAR)-stimulated glucose transport. J Biol Chem 277:23554–23562
Coderre L, Kandror KV, Vallega G, Pilch PF (1995) Identification and characterization of an exercise-sensitive pool of glucose transporters in skeletal muscle. J Biol Chem 270:27584–27588
Coe NR, Smith AJ, Frohnert BI, Watkins PA, Bernlohr DA (1999) The fatty acid transport protein (FATP1) is a very long chain acyl-CoA synthetase. J Biol Chem 274:36300–36304
Coort SLM, Willems J, Coumans WA, van der Vusse GJ, Bonen A, Glatz JFC, Luiken JJFP (????) Sulfo-N-succinimidyl esters of long chain fatty acids specifically inhibit fatty acid translocase (FAT/CD36)-mediated cellular fatty acid uptake. Mol Cell Biochem 239:213–219
Cormont M, Tanti JF, Zahraoui A, Van Obberghen E, Tavitian A, Le Marchand-Brustel Y (1993) Insulin and okadaic acid induce Rab4 redistribution in adipocytes. J Biol Chem 268:19491–19497
Derave W, Ai H, Ihlemann J, Witters LA, Kristiansen S, Richter EA, Ploug T (2000) Dissociation of AMP-activated protein kinase activation and glucose transport in contracting slow-twitch muscle. Diabetes 49:1281–1287
Donthi RV, Huisamen B, Lochner A (2000) Effect of vanadate and insulin on glucose transport in isolated adult rat cardiomyocytes. Cardiovasc Drugs Ther 14:463–470
Dransfeld O, Uphues I, Sasson S, Schurmann A, Joost HG, Eckel J (2000) Regulation of subcellular distribution of GLUT4 in cardiomyocytes: Rab4A reduces basal glucose transport and augments insulin responsiveness. Exp Clin Endocrinol Diabetes 108:26–36
Dyck DJ, Steinberg G, Bonen A (????) Insulin increases FA uptake and esterification but reduces lipid utilization in isolated contracting muscle. Am J Physiol 281:E600–E607
Egert S, Nguyen N, Schwaiger M (1999) Myocardial glucose transporter GLUT1: translocation induced by insulin and ischemia. J Mol Cell Cardiol 31:1337–1344
Elsing C, Kassner A, Gajdzik L, Graf J, Stremmel W (1998) Electrogenicity of hepatocellular fatty acid uptake. Eur J Med Res 3:393–396
Farese RV (2002) Function and dysfunction of aPKC isoforms for glucose transport in insulin-sensitive and insulin-resistant states. Am J Physiol 283:E1–E11
Feron O, Zhao YY, Kelly RA (1999) The ins and outs of caveolar signaling. m2 muscarinic cholinergic receptors and eNOS activation versus neuregulin and ErbB4 signaling in cardiac myocytes. Ann NY Acad Sci 874:11–19
Fischer Y, Rose H, Kammermeier H (1991) Highly insulin-responsive isolated rat heart muscle cells yielded by a modified isolation method. Life Sci 49:1679–1688
Fischer Y, Kamp J, Thomas J, Popping S, Rose H, Carpene C, Kammermeier H (1996) Signals mediating stimulation of cardiomyocyte glucose transport by the alpha-adrenergic agonist phenylephrine. Am J Physiol 270:C1211–C1220
Fischer Y, Thomas J, Sevilla L, Munoz P, Becker C, Holman G, Kozka IJ, Palacin M, Testar X, Kammermeier H, Zorzano A (1997) Insulin-induced recruitment of glucose transporter 4 (GLUT4) and GLUT1 in isolated rat cardiac myocytes. Evidence of the existence of different intracellular GLUT4 vesicle populations. J Biol Chem 272:7085–7092
Foster LJ, Weir ML, Lim DY, Liu Z, Trimble WS, Klip A (2000) A functional role for VAP-33 in insulin-stimulated GLUT4 traffic. Traffic 1:512–521
Fryer LG, Hajduch E, Rencurel F, Salt IP, Hundal HS, Hardie DG, Carling D (2000) Activation of glucose transport by AMP-activated protein kinase via stimulation of nitric oxide synthase. Diabetes 49:1978–1985
Gao J, Ren J, Gulve EA, Holloszy JO (1994) Additive effect of contractions and insulin on GLUT-4 translocation into the sarcolemma. J Appl Physiol 77:1597–1601
Gervois P, Torra IP, Fruchart JC, Staels B (2000) Regulation of lipid and lipoprotein metabolism by PPAR activators. Clin Chem Lab Med 38:3–11
Gimeno RE, Ortegon AM, Patel S, Punreddy S, Ge P, Sun Y, Lodish HF, Stahl A (2003) Characterization of a heart-specific fatty acid transport protein. J Biol Chem 278:16039–16044
Glatz JF, van der Vusse GJ (1989) Intracellular transport of lipids. Mol Cell Biochem 88:37–44
Glatz JF, Luiken JJ, Bonen A (2001) Involvement of membrane-associated proteins in the acute regulation of cellular fatty acid uptake. J Mol Neurosci 16:123–132
Groen AK, Wanders RJ, Westerhoff HV, van der Meer R, Tager JM (1982) Quantification of the contribution of various steps to the control of mitochondrial respiration. J Biol Chem 257:2754–2757
Hamilton JA (1998) Fatty acid transport: difficult or easy? J Lipid Res 39:467–481
Hamilton JA, Kamp F (1999) How are free fatty acids transported in membranes? Is it by proteins or by free diffusion through the lipids? Diabetes 48:2255–2269
Hardie DG, Carling D (1997) The AMP-activated protein kinase--fuel gauge of the mammalian cell? Eur J Biochem 246:259–273
Hayashi T, Wojtaszewski JF, Goodyear LJ (1997) Exercise regulation of glucose transport in skeletal muscle. Am J Physiol 273:E1039–E1051
Hayashi T, Hirshman MF, Kurth EJ, Winder WW, Goodyear LJ (1998) Evidence for 5’ AMP-activated protein kinase mediation of the effect of muscle contraction on glucose transport. Diabetes 47:1369–1373
Heller-Harrison RA, Morin M, Guilherme A, Czech MP (1996) Insulin-mediated targeting of phosphatidylinositol 3-kinase to GLUT4-containing vesicles. J Biol Chem 271:10200–10204
Holman GD, Lo Leggio L, Cushman SW (1994) Insulin-stimulated GLUT4 glucose transporter recycling. A problem in membrane protein subcellular trafficking through multiple pools. J Biol Chem 269:17516–17524
Huang J, Imamura T, Olefsky JM (2001) Insulin can regulate GLUT4 internalization by signaling to Rab5 and the motor protein dynein. Proc Natl Acad Sci USA 98:13084–13089
Hyde R, Peyrollier K, Hundal HS (2002) Insulin promotes the cell surface recruitment of the SAT2/ATA2 system A amino acid transporter from an endosomal compartment in skeletal muscle cells. J Biol Chem 277:13628–13634
Ibrahimi A, Sfeir Z, Magharaie H, Amri EZ, Grimaldi P, Abumrad NA (1996) Expression of the CD36 homolog (FAT) in fibroblast cells: effects on fatty acid transport. Proc Natl Acad Sci USA 93:2646–2651
Isola LM, Zhou SL, Kiang CL, Stump DD, Bradbury MW, Berk PD (1995) 3T3 fibroblasts transfected with a cDNA for mitochondrial aspartate aminotransferase express plasma membrane fatty acid-binding protein and saturable fatty acid uptake. Proc Natl Acad Sci USA 92:9866–9870
Jiang H, Li J, Katz EB, Charron MJ (2001) GLUT4 ablation in mice results in redistribution of IRAP to the plasma membrane. Biochem Biophys Res Commun 284:519–525
Johannsson E, Nagelhus EA, McCullagh KJ, Sejersted OM, Blackstad TW, Bonen A, Ottersen OP (1997) Cellular and subcellular expression of the monocarboxylate transporter MCT1 in rat heart. A high-resolution immunogold analysis. Circ Res 80:400–407
Joost HG, Bell GI, Best JD, Birnbaum MJ, Charron MJ, Chen YT, Doege H, James DE, Lodish HF, Moley KH, Moley JF, Mueckler M, Rogers S, Schurmann A, Seino S, Thorens B (2002) Nomenclature of the GLUT/SLC2A family of sugar/polyol transport facilitators. Am J Physiol 282:E974–E976
Kagaya Y, Kanno Y, Takeyama D, Ishide N, Maruyama Y, Takahashi T, Ido T, Takishima T (1990) Effects of long-term pressure overload on regional myocardial glucose and free fatty acid uptake in rats. A quantitative autoradiographic study. Circulation 81:1353–1361
Kandror KV, Pilch PF (1994) gp160, a tissue-specific marker for insulin-activated glucose transport. Proc Natl Acad Sci USA 91:8017–8021
Kandror KV, Pilch PF (1996) Compartmentalization of protein traffic in insulin-sensitive cells. Am J Physiol 271:E1–E14
Karlsson M, Thorn H, Parpal S, Stralfors P, Gustavsson J (2002) Insulin induces translocation of glucose transporter GLUT4 to plasma membrane caveolae in adipocytes. FASEB J 16:249–251
Karnieli E, Hissin PJ, Simpson IA, Salans LB, Cushman SW (1981) A possible mechanism of insulin resistance in the rat adipose cell in streptozotocin-induced diabetes mellitus. Depletion of intracellular glucose transport systems. J Clin Invest 68:811–814
Kessler A, Tomas E, Immler D, Meyer HE, Zorzano A, Eckel J (2000) Rab11 is associated with GLUT4-containing vesicles and redistributes in response to insulin. Diabetologia 43:1518–1527
Kessler A, Uphues I, Ouwens DM, Till M, Eckel J (2001) Diversification of cardiac insulin signaling involves the p85 alpha/beta subunits of phosphatidylinositol 3-kinase. Am J Physiol 280:E65–E74
Khan AH, Pessin JE (2002) Insulin regulation of glucose uptake: a complex interplay of intracellular signalling pathways. Diabetologia 45:1475–1483
Kono T (1982) Recycling of the insulin-sensitive glucose transport mechanism in fat-cells. Biochem Soc Trans 10:9–10
Koonen DPY, Coumans WA, Arumugam Y, Bonen A, Glatz JFC, Luiken JJFP (2002) Giant membrane vesicles as a model to study cellular substrate uptake dissected from metabolism. Mol Cell Biochem 239:121–130
Kupriyanova TA, Kandror KV (1999) Akt-2 binds to Glut4-containing vesicles and phosphorylates their component proteins in response to insulin. J Biol Chem 274:1458–1464
Lango R, Smolenski RT, Narkiewicz M, Suchorzewska J, Lysiak-Szydlowska W (2001) Influence of L-carnitine and its derivatives on myocardial metabolism and function in ischemic heart disease and during cardiopulmonary bypass. Cardiovasc Res 51:21–29
Lasley RD, Smart EJ (2001) Cardiac myocyte adenosine receptors and caveolae. Trends Cardiovasc Med 11:259–263
Lopaschuk GD (2001) Malonyl CoA control of fatty acid oxidation in the diabetic rat heart. Adv Exp Med Biol 498:155–165
Lopaschuk GD (2002) Metabolic abnormalities in the diabetic heart. Heart Fail Rev 7:149–159
Luiken JJFP, van Nieuwenhoven FA, America G, van der Vusse GJ, Glatz JFC (1997) Uptake and metabolism of palmitate by isolated cardiac myocytes from adult rats: involvement of sarcolemmal proteins. J Lipid Res 38:745–758
Luiken JJFP, Turcotte LP, Bonen A (1999) Protein-mediated palmitate uptake and expression of fatty acid transport proteins in heart giant vesicles. J Lipid Res 40:1007–1016
Luiken JJFP, Arumugam Y, Dyck DJ, Bell RC, Pelsers MM, Turcotte LP, Tandon NN, Glatz JFC, Bonen A (2001) Increased rates of fatty acid uptake and plasmalemmal fatty acid transporters in obese Zucker rats. J Biol Chem 276:40567–40573
Luiken JJFP, Willems J, van der Vusse GJ, Glatz JFC (2001) Electrostimulation enhances FAT/CD36-mediated long-chain fatty acid uptake by isolated rat cardiac myocytes. Am J Physiol 281:E704–E712
Luiken JJFP, Dyck DJ, Han XX, Tandon NN, Arumugam Y, Glatz JFC, Bonen A (2002) Insulin induces the translocation of the fatty acid transporter FAT/CD36 to the plasma membrane. Am J Physiol 282:E491–E495
Luiken JJFP, Koonen DP, Willems J, Zorzano A, Becker C, Fischer Y, Tandon NN, Van Der Vusse GJ, Bonen A, Glatz JFC (2002) Insulin stimulates long-chain fatty acid utilization by rat cardiac myocytes through cellular redistribution of FAT/CD36. Diabetes 51:3113–3119
Luiken JJFP, Willems J, Coort SLM, Coumans WA, Bonen A, Van Der Vusse GJ, Glatz JFC (2002) Effects of cAMP modulators on long-chain fatty-acid uptake and utilization by electrically stimulated rat cardiac myocytes. Biochem J 367:881–887
Luiken JJFP, Coort SLM, Willems J, Coumans WA, Bonen A, van der Vusse GJ, Glatz JFC (2003) Contraction-induced FAT/CD36 translocation in rat cardiac myocytes is mediated through AMP-activated protein kinase signaling. Diabetes 52:1627–1634
Lund S, Holman GD, Schmitz O, Pedersen O (1995) Contraction stimulates translocation of glucose transporter GLUT4 in skeletal muscle through a mechanism distinct from that of insulin. Proc Natl Acad Sci USA 92:5817–5821
Malide D, Ramm G, Cushman SW, Slot JW (2000) Immunoelectron microscopic evidence that GLUT4 translocation explains the stimulation of glucose transport in isolated rat white adipose cells. J Cell Sci 113:4203–4210
Martin LB, Shewan A, Millar CA, Gould GW, James DE (1998) Vesicle-associated membrane protein 2 plays a specific role in the insulin-dependent trafficking of the facilitative glucose transporter GLUT4 in 3T3-L1 adipocytes. J Biol Chem 273:1444–1452
Martinez O, Antony C, Pehau-Arnaudet G, Berger EG, Salamero J, Goud B (1997) GTP-bound forms of rab6 induce the redistribution of Golgi proteins into the endoplasmic reticulum. Proc Natl Acad Sci USA 94:1828–1833
Merrill GF, Kurth EJ, Hardie DG, Winder WW (1997) AICA riboside increases AMP-activated protein kinase, fatty acid oxidation, and glucose uptake in rat muscle. Am J Physiol 273:E1107–E1112
Min J, Okada S, Kanzaki M, Elmendorf JS, Coker KJ, Ceresa BP, Syu LJ, Noda Y, Saltiel AR, Pessin JE (1999) Synip: a novel insulin-regulated syntaxin 4-binding protein mediating GLUT4 translocation in adipocytes. Mol Cell 3:751–760
Mu J, Brozinick JT Jr, Valladares O, Bucan M, Birnbaum MJ (2001) A role for AMP-activated protein kinase in contraction- and hypoxia-regulated glucose transport in skeletal muscle. Mol Cell 7:1085–1094
Mueckler M (1994) Facilitative glucose transporters. Eur J Biochem 219:713–725
Muller H, Deckers K, Eckel J (2002) The fatty acid translocase (FAT)/CD36 and the glucose transporter GLUT4 are localized in different cellular compartments in rat cardiac muscle. Biochem Biophys Res Commun 293:665–669
Munoz P, Mora S, Sevilla L, Kaliman P, Tomas E, Guma A, Testar X, Palacin M, Zorzano A (1996) Expression and insulin-regulated distribution of caveolin in skeletal muscle. Caveolin does not colocalize with GLUT4 in intracellular membranes. J Biol Chem 271:8133–8139
Muoio DM, Dohm GL, Tapscott EB, Coleman RA (1999) Leptin opposes insulin’s effects on fatty acid partitioning in muscles isolated from obese ob/ob mice. Am J Physiol 276:E913–E921
Oram JF, Wenger JI, Neely JR (1975) Regulation of long chain fatty acid activation in heart muscle. J Biol Chem 250:73–78
Pearce SF, Wu J, Silverstein RL (1994) A carboxyl terminal truncation mutant of CD36 is secreted and binds thrombospondin: evidence for a single transmembrane domain. Blood 84:384–389
Ploug T, van Deurs B, Ai H, Cushman SW, Ralston E (1998) Analysis of GLUT4 distribution in whole skeletal muscle fibers: identification of distinct storage compartments that are recruited by insulin and muscle contractions. J Cell Biol 142:1429–1446
Plutner H, Cox AD, Pind S, Khosravi-Far R, Bourne JR, Schwaninger R, Der CJ, Balch WE (1991) Rab1b regulates vesicular transport between the endoplasmic reticulum and successive Golgi compartments. J Cell Biol 115:31–43
Pohl J, Ring A, Stremmel W (2002) Uptake of long-chain fatty acids in HepG2 cells involves caveolae: analysis of a novel pathway. J Lipid Res 43:1390–1399
Ponticos M, Lu QL, Morgan JE, Hardie DG, Partridge TA, Carling D (1998) Dual regulation of the AMP-activated protein kinase provides a novel mechanism for the control of creatine kinase in skeletal muscle. EMBO J 17:1688–1699
Ralston E, Ploug T (1999) Caveolin-3 is associated with the T-tubules of mature skeletal muscle fibers. Exp Cell Res 246:510–515
Ramrath S, Tritschler HJ, Eckel J (1999) Stimulation of cardiac glucose transport by thioctic acid and insulin. Horm Metab Res 31:632–635
Randle PJ, Garland PB, Newsholme EA, Hales CN (1965) The glucose fatty acid cycle in obesity and maturity onset diabetes mellitus. Ann NY Acad Sci 131:324–333
Rett K, Wicklmayr M, Dietze GJ, Haring HU (1996) Insulin-induced glucose transporter (GLUT1 and GLUT4) translocation in cardiac muscle tissue is mimicked by bradykinin. Diabetes 45:S66–S69
Rodrigues B, Cam MC, McNeill JH (1998) Metabolic disturbances in diabetic cardiomyopathy. Mol Cell Biochem 180:53–57
Ros-Baro A, Lopez-Iglesias C, Peiro S, Bellido D, Palacin M, Zorzano A, Camps M (2001) Lipid rafts are required for GLUT4 internalization in adipose cells. Proc Natl Acad Sci USA 98:12050–12055
Rose H, Hennecke T, Kammermeier H (1990) Sarcolemmal fatty acid transfer in isolated cardiomyocytes governed by albumin/membrane-lipid partition. J Mol Cell Cardiol 22:883–892
Saltis J, Habberfield AD, Egan JJ, Londos C, Simpson IA, Cushman SW (1991) Role of protein kinase C in the regulation of glucose transport in the rat adipose cell. Translocation of glucose transporters without stimulation of glucose transport activity. J Biol Chem 266:261–267
Schaffer JE, Lodish HF (1994) Expression cloning and characterization of a novel adipocyte long chain fatty acid transport protein. Cell 79:427–436
Sevilla L, Tomas E, Munoz P, Guma A, Fischer Y, Thomas J, Ruiz-Montasell B, Testar X, Palacin M, Blasi J, Zorzano A (1997) Characterization of two distinct intracellular GLUT4 membrane populations in muscle fiber. Differential protein composition and sensitivity to insulin. Endocrinology 138:3006–3015
Shulman GI (2000) Cellular mechanisms of insulin resistance. J Clin Invest 106:171–176
Slot JW, Geuze HJ, Gigengack S, James DE, Lienhard GE (1991) Translocation of the glucose transporter GLUT4 in cardiac myocytes of the rat. Proc Natl Acad Sci USA 88:7815–7819
Sogaard M, Tani K, Ye RR, Geromanos S, Tempst P, Kirchhausen T, Rothman JE, Sollner T (1994) A rab protein is required for the assembly of SNARE complexes in the docking of transport vesicles. Cell 78:937–948
Song KS, Scherer PE, Tang Z, Okamoto T, Li S, Chafel M, Chu C, Kohtz DS, Lisanti MP (1996) Expression of caveolin-3 in skeletal, cardiac, and smooth muscle cells. Caveolin-3 is a component of the sarcolemma and co-fractionates with dystrophin and dystrophin-associated glycoproteins. J Biol Chem 271:15160–15165
Sonnichsen B, De Renzis S, Nielsen E, Rietdorf J, Zerial M (2000) Distinct membrane domains on endosomes in the recycling pathway visualized by multicolor imaging of Rab4, Rab5, and Rab11. J Cell Biol 149:901–914
St.Denis JF, Cushman SW (1998) Role of SNAREs in the GLUT4 translocation response to insulin in adipose cells and muscle. J Basic Clin Physiol Pharmacol 9:153–165
Stagsted J, Olsson L, Holman GD, Cushman SW, Satoh S (1993) Inhibition of internalization of glucose transporters and IGF-II receptors. Mechanism of action of MHC class I-derived peptides which augment the insulin response in rat adipose cells. J Biol Chem 268:22809–22813
Stahl A, Evans JG, Pattel S, Hirsch D, Lodish HF (2002) Insulin causes fatty acid transport protein translocation and enhanced fatty acid uptake in adipocytes. Dev Cell 2:477–488
Stremmel W (1988) Fatty acid uptake by isolated rat heart myocytes represents a carrier-mediated transport process. J Clin Invest 81:844–852
Stuart Wood I, Trayhurn P (2003) Glucose transporters (GLUT and SGLT): expanded families of sugar transport proteins. Br J Nutr 89:3–9
Stump DD, Zhou SL, Berk PD (1993) Comparison of plasma membrane FABP and mitochondrial isoform of aspartate aminotransferase from rat liver. Am J Physiol 265:G894–G902
Taegtmeyer H, Goodwin GW, Doenst T, Frazier OH (1997) Substrate metabolism as a determinant for postischemic functional recovery of the heart. Am J Cardiol 80:3A–10A
Tomas E, Sevilla L, Palacin M, Zorzano A (2001) The insulin-sensitive GLUT4 storage compartment is a postendocytic and heterogeneous population recruited by acute exercise. Biochem Biophys Res Commun 284:490–495
Trischler M, Stoorvogel W, Ullrich O (1999) Biochemical analysis of distinct Rab5- and Rab11-positive endosomes along the transferrin pathway. J Cell Sci112:4773–4783
Tsakiridis T, Vranic M, Klip A (1995) Phosphatidylinositol 3-kinase and the actin network are not required for the stimulation of glucose transport caused by mitochondrial uncoupling: comparison with insulin action. Biochem J 309:1–5
Ullrich O, Reinsch S, Urbe S, Zerial M, Parton RG (1996) Rab11 regulates recycling through the pericentriolar recycling endosome. J Cell Biol 135:913–924
Unger RH, Orci L (2001) Diseases of liporegulation: new perspective on obesity and related disorders. FASEB J 15:312–321
Uphues I, Kolter T, Goud B, Eckel J (1994) Insulin-induced translocation of the glucose transporter GLUT4 in cardiac muscle: studies on the role of small-molecular-mass GTP-binding proteins. Biochem J 301:177–182
Uphues I, Chern Y, Eckel J (1995) Insulin-dependent translocation of the small GTP-binding protein rab3C in cardiac muscle: studies on insulin-resistant Zucker rats. FEBS Lett 377:109–112
Van der Vusse GJ, Coumans WA, Van der Veen E, Drake AJ, Flameng W, Suy R (1984) ATP, creatine phosphate and glycogen content in human myocardial biopsies: markers for the efficacy of cardioprotection during aorto-coronary bypass surgery. Vasc Surg 18:127–134
Van der Vusse GJ, Glatz JF, Stam HC, Reneman RS (1992) Fatty acid homeostasis in the normoxic and ischemic heart. Physiol Rev 72:881–940
Van der Vusse GJ, van Bilsen M, Glatz JFC (2000) Cardiac fatty acid uptake and transport in health and disease. Cardiovasc Res 45:279–293
Van Nieuwenhoven FA, Willemsen PHM, Van der Vusse GJ, Glatz JFC (1999) Co-expression in rat heart and skeletal muscle of four genes coding for proteins implicated in long-chain fatty acid uptake. Int J Biochem Cell Biol 31:489–498
Watson RT, Pessin JE (2001) Subcellular compartmentalization and trafficking of the insulin-responsive glucose transporter, GLUT4. Exp Cell Res 271:75–83
Weisiger RA, Fitz JG, Scharschmidt BF (1989) Hepatic oleate uptake. Electrochemical driving forces in intact rat liver. J Clin Invest 83:411–420
Wheeler TJ, Fell RD, Hauck MA (1994) Translocation of two glucose transporters in heart: effects of rotenone, uncouplers, workload, palmitate, insulin and anoxia. Biochim Biophys Acta 1196:191–200
Wu G, Yussman MG, Barrett TJ, Hahn HS, Osinska H, Hilliard GM, Wang X, Toyokawa T, Yatani A, Lynch RA, Robbins J, Dorn GW 2nd (2001) Increased myocardial Rab GTPase expression: a consequence and cause of cardiomyopathy. Circ Res 89:1130–1137
Yeh JI, Gulve EA, Rameh L, Birnbaum MJ (1995) The effects of wortmannin on rat skeletal muscle. Dissociation of signaling pathways for insulin- and contraction-activated hexose transport. J Biol Chem 270:2107–2111
Ylitalo K, Ala-Rami A, Vuorinen K, Peuhkurinen K, Lepojarvi M, Kaukoranta P, Kiviluoma K, Hassinen I (2001) Reversible ischemic inhibition of F1F0-ATPase in rat and human myocardium. Biochim Biophys Acta 1504:329–339
Young LH, Renfu Y, Russell R, Hu X, Caplan M, Ren J, Shulman GI, Sinusas AJ (1997) Low-flow ischemia leads to translocation of canine heart GLUT-4 and GLUT-1 glucose transporters to the sarcolemma in vivo. Circulation 95:415–422
Zerial M, Stenmark H (1993) Rab GTPases in vesicular transport. Curr Opin Cell Biol 5:613–620
Zhou SL, Potter BJ, Stump D, Sorrentino D, Berk PD (1990) Quantitation of plasma membrane fatty acid-binding protein by enzyme dilution and monoclonal antibody based immunoassay. Mol Cell Biochem 98:183–189
Zhou M, Sevilla L, Vallega G, Chen P, Palacin M, Zorzano A, Pilch PF, Kandror KV (1998) Insulin-dependent protein trafficking in skeletal muscle cells. Am J Physiol 275:E187–E196
Zorzano A, Sevilla L, Camps M, Becker C, Meyer J, Kammermeier H, Munoz P, Guma A, Testar X, Palacin M, Blasi J, Fischer Y (1997) Regulation of glucose transport, and glucose transporters expression and trafficking in the heart: studies in cardiac myocytes. Am J Cardiol 80:65A–76A
Acknowledgements
Work in the authors’ laboratories is supported by the Netherlands Heart Foundation, grant 2000.156, and by the Heart and Stroke Foundation of Ontario. Joost Luiken is the recipient of a VIDI-Innovational Research grant from the Netherlands Organisation for Scientific Research (NWO-ZonMw grant No. 016.036.305). Arend Bonen is a Canada Research Chair in Metabolism and Health. Jan Glatz is Netherlands Heart Foundation Professor of Cardiac Metabolism.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Luiken, J.J.F.P., Coort, S.L.M., Koonen, D.P.Y. et al. Regulation of cardiac long-chain fatty acid and glucose uptake by translocation of substrate transporters. Pflugers Arch - Eur J Physiol 448, 1–15 (2004). https://doi.org/10.1007/s00424-003-1199-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00424-003-1199-4