Abstract
Purpose
Reoperations (R-PTX) for primary hyperparathyroidism (pHPT) are challenging, since they are associated with increased failure and morbidity rates. The aim was to evaluate the results of reoperations over two decades, the latter considering the implementation of Tc99msestamibi-SPECT (Mibi/SPECT), intraoperative parathormone (IOPTH) measurement, and intraoperative neuromonitoring (IONM).
Patients and methods
Data of 1,363 patients who underwent surgery for pHPT were retrospectively analyzed regarding reoperations. Causes of persistent (p) pHPT or recurrent (r) pHPT, preoperative imaging studies, surgical findings, and outcome were analyzed. Data of patients who underwent surgery between 1987 and 1997 (group 1; G1) and between 1998 and 2008 (group 2; G2) with the use of Mibi/SPECT, IOPTH, and IONM were evaluated.
Results
One hundred twenty-five patients with benign ppHPT (n = 108) or rpHPT (n = 17) underwent reoperations (R-PTX). Group 1 included 54, group 2 71 patients. Main cause of ppHPT (G1 = 65 % vs. G2 = 53 %) and rpHPT (G1 = 80 % vs. G2 = 60 %) was the failed detection of a solitary adenoma (p = 0.2). Group 1 patients had significantly less unilateral/focused neck re-explorations (G1 = 23 % vs. G2 = 57 %, p = 0.0001), and more sternotomies (G1 = 35 vs. G2 = 14 %, p = 0.01). After a median follow-up of 4 (range 0.9–23.4) years, reversal of hypercalcemia was achieved in 91 % (G1) and in 98.6 % in group 2 (p = 0.08, OR 7.14 [0.809–63.1]). The rates of permanent recurrent laryngeal nerve palsy (G1 = G2 = 9 %, p = 1) and of postoperative permanent hypoparathyroidism (G1 = 9 % vs. G2 = 6 %, p = 0.5) were not significantly different. Other complications such as wound infection, postoperative bleeding, and pneumonia were significantly lower in group 2 (p < 0.001).
Conclusion
Nowadays, cure rates of R-PTX are nearly the same as in primary operations for pHPT. These results can be achieved in high-volume centers by routine use of well-established preoperative Mibi/SPECT and US in combination with IOPTH. However, morbidity is still considerably high.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Short summary
Routine use of Tc99msestamibi-SPECT and intraoperative parathormone (IOPTH) measurement in reoperative parathyroid surgery can provide the same cure rates as primary operations, although the morbidity is still considerably high.
Purpose
Reoperations (R-PTX) for persistent (p) or recurrent (r) primary hyperparathyroidism (pHPT) are challenging, since they are related with high rates of recurrent laryngeal nerve palsy (RLNP up to 15 %) and postoperative hypoparathyroidism (up to 20 %), which is considered worse than mild hypercalcemia [1–4]. High morbidity and complication rates in reoperations are due to an intensive scarring, resulting in difficulties to identify abnormal parathyroid glands and to preserve the recurrent laryngeal nerve(s) and normal parathyroid glands. Thus, the decision to perform a reoperation depends on the balance between the risks, the severity of the disease, and the likelihood of a curative operation. Focused approaches seem to be associated with significant advantages in reoperations, especially lower morbidity rates [5, 6]. Admittedly, the success of a focused approach is dependent on accurate preoperative imaging [7]. During the past decade, preoperative localisation procedures, especially Tc99msestamibi scintigraphy with single-photon emission computed tomography (Mibi/SPECT) and high-resolution ultrasonography (US), have significantly improved [6, 7]. Thus, minimal invasive parathyroidectomy became the treatment of choice in patients with preoperatively localized sporadic pHPT [8, 9]. The implementation of intraoperative parathyroid hormone (IOPTH) measurement has been demonstrated to be an excellent predictor of cure [10, 11] and proved to be helpful in reoperations for persistent or recurrent HPT in some studies [6, 12]. Furthermore, intraoperative venous sampling (IVS) from both jugular veins with rapid PTH measurement seems to be an additional promising adjunct to regionalize the source of increased PTH secretion during R-PTX [13]. Moreover, several new localization procedures, like the 11C-methionine-positron-emission-tomography (met-PET), ultrasound-guided fine-needle aspiration (FNA) of suspected tumors or preoperative selective venous sampling with rapid PTH measurement (SVS with Quick-PTH) with high sensitivity and accuracy rates have been developed [6].
The current study was conducted to verify that advancements in imaging methods led to a higher success rate and a reduction of perioperative morbidity and complications in R-PTX. Furthermore, our aim was to show that high success rates can be achieved using commonly available and approved Mibi/SPECT and US.
Patients and methods
Data of 1,344 patients with benign pHPT who underwent PTX at the Department of Surgery, Philipps-University Marburg, between May 1987 and December 2008 were retrospectively analyzed to identify 125 patients undergoing 147 R-PTX for persistent (ppHPT) or recurrent (rpHPT) disease. Preoperative clinical symptoms and laboratory data, including serum calcium (Ca), parathyroid hormone (PTH), phosphate (PO4), blood urea nitrogen (BUN), creatinine, alkaline phosphatase (AP), preoperative localisation studies, surgical treatment (PTX), intraoperative findings, histopathological results, and outcomes were analyzed. Postoperative PTH (normal range 11–65 pg/l) and calcium (normal range 2.1–2.6 mmol/l) levels were obtained at day 3, and 6 and 12 months postoperatively, thereafter annually via outpatient visits or contacting the personal physician. All patients underwent laryngoscopy by an otolaryngologist before reoperation at our hospital and before discharge to evaluate the vocal cord function. Logopaedic therapy was initiated and the laryngoscopy was repeated 3–6 months after surgery if necessary.
PpHPT was defined as hypercalcemia within 6 months after the initial PTX. RpHPT was defined as hypercalcemia that re-occurred more than 6 months after initial PTX. Discrimination between solitary adenoma and multiglandular disease (MGD) was dependent on one or more abnormal parathyroid glands that were removed. Permanent hypoparathyroidism was defined as hypocalcemia (Ca < 2.2 mmol/l) with PTH levels < 11 pg/ml more than 6 months after R-PTX.
Before reoperation, the diagnosis of ppHPT/rpHPT was unequivocally confirmed and the indication for reoperation was reconsidered. R-PTX was recommended in patients with HPT-specific symptoms, like renal stones or severe bone alterations and pain, or highly elevated Ca levels (0.25 mmol/l above the upper normal range). In addition, previous surgical and histopathological reports as well as results of all imaging studies available were carefully reviewed. Surgical approaches included focused PTX (minimally invasive parathyroidectomy (MIP) or the unilateral neck exploration), the bilateral cervical exploration (BCE), or the mediastinal approach via median sternotomy, respectively. None of the patients underwent a thoracoscopic removal of an enlarged ectopic gland.
Preoperative localisation studies included high resolution ultrasonography (US) using a linear transducer. Initially Technetium–thallium (Tc–Tl) scintigraphy was performed, which was replaced by the Tc99msestamibi scintigraphy (Mibi) since the 1990s. In some patients, both Tc–Tl scintigraphy as well as Tc99msestamibi was performed. However, since 1998, additional SPECT technology was available for the first time. Dual-phase single-photon emission computed tomography was performed after injection of 1,000-Mbq Tc99msestamibi.
Generally, at least two localisation studies should have been done before R-PTX, since 1999 routinely Mibi/SPECT and US. When imaging was considered concordant positive, additional studies were generally not obtained.
Selected patients underwent computed tomography (CT), magnetic resonance imaging (MRI) and/or cervical angiography with selective venous sampling (SVS) with PTH measurement. Cervical-CT with intravenous contrast was performed using helical acquisition (3.5-mm image thickness before 1998 and image thickness 1.5 mm at present). Multiplanar, multisequence neck MRI was performed with and without intravenous contrast. Interpretation of imaging results (i.e., true positive) were determined as described previously [4, 14].
Since 1998, IOPTH analysis was frequently used to monitor the success of R-PTX. PTH levels were determined before skin incision, as well as after excision of the presumed hyperfunctioning parathyroid gland. Until 2006, our criteria for a successful R-PTX was a drop of more than 50 % at 5 min after excision and drop into normal range after 15 min. compared to the baseline value. Since then, we expected a drop of more than 50 % after 10 min [4, 8].
In some patients, an IVS from both jugular veins was performed to identify the side with the highest PTH value using rapid IOPTH measurement. Two blood samples were drawn from each jugular vein, one as far proximal and one as far distal as possible, which allowed determining the quadrant of PTH secretion in some patients. IVS was performed in patients with inconclusive preoperative imaging results and in patients with positive preoperative imaging results in order to evaluate the significance of this emerging technique.
For IONM, different techniques were used over the years, including the indirect stimulation of the RLN at risk via the vagal nerve and the direct stimulation of the RLN if technically feasible.
All R-PTX were performed by experienced endocrine surgeons (>100 HPT operations), all trained under the same surgical philosophy. In all surgeries, clips and sutures were used, but none was performed with vessel sealing devices. Cure was defined as permanent elimination of the potentially life threatening hypercalcemia.
A comparative analysis was performed between patients who underwent R-PTX between 1987 and 1997 (group 1), and patients who underwent R-PTX between 1998 and 2008 (group 2) when Mibi/SPECT, IOPTH, and IONM were available.
Statistical analysis was performed by using the Fisher’s exact test for two-group comparisons with exact 95 % confidence intervals (CI) for the odds ratio (OR), the unpaired Student t test for two-group comparisons, and 95 % Blyth–Still–Casella confidence intervals for diagnostic quality measures. All continuous variables were reported as median and range. A p value <0.05 was considered to be statistical significant, not adjusting for multiple testing.
Results
Overall, 125 patients underwent R-PTX, including 54 (43 %) patients in group 1 and 71 (57 %) patients in group 2 (Tables 1 and 3). In five of 23 (22 %) patients with initial surgery in Marburg and in 57 of 102 (56 %) patients who underwent initial surgery elsewhere, reoperation was necessary due to an undetected solitary parathyroid adenoma (p = 0.005, OR 4.56, [1.57–13.2]). Evaluation of surgical and pathology reports prior to R-PTX revealed that 47 of 168 (28 %) abnormal parathyroid glands and 52 normal parathyroid glands have been excised during initial PTX elsewhere.
Localization studies
Results of all localization studies are summarized in Table 2. All but five patients of group 1 had preoperative localization studies. Two had undergone neck exploration elsewhere, but no parathyroid tissue could be identified. Both patients were cured after bilateral cervical R-PTX in the early postoperative period. One patient suffered from persistent pHPT after a 3 1/2 gland resection and underwent resection of the clip marked remnant 12 months later. The remaining two patients had their initial unsuccessful surgery at our institution. Both underwent successful reoperation for MGD within the same hospital stay. However, all patients of group 2 underwent at least two localization procedures.
In 13 patients of group 1, neither a Tl–Tc nor a Tc99msestamibi scintigraphy was performed. Except the five patients of group 1 who did not undergo any localization procedure before R-PTX, in another eight patients preoperative CT or MRI imaging was performed instead of a scintigraphy. CT was false positive in three and false negative in one of these patients, while MRI scans were true positive in four patients. In 12 patients, both Tl–Tc scintigraphy and Tc99msestamibi scintigraphy without SPECT were performed with concordant results in 10 patients.
Mibi/SPECT together with IVS showed the lowest rate of false positive results (6 %).
Operative findings
One hundred twenty-five patients with previous parathyroid surgery underwent a total of 147 R-PTX, including 127 reoperations in 108 patients with ppHPT and 20 reoperations in 17 patients with rpHPT.
One hundred twenty-nine of 147 reoperations were done in our hospital, including 75 (58 %) BCE and 54 (42 %) unilateral or focused explorations.
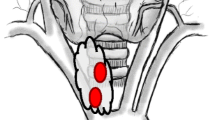
In total, 96 (77 %) patients had a single abnormal gland removed, 14 (11 %) had two abnormal glands, and 9 (7 %) patients had three or more abnormal glands excised during R-PTX. All three patients with parathyreomatosis underwent en bloc excision of the tumor bearing-tissue and in six patients (4 %) no abnormal gland could be identified. The majority of abnormal glands were identified during R-PTX in normal anatomic positions (69 %), which was not significantly different between groups 1 and 2 (73 % vs. 66 %, p = 0.38). Exact location of the parathyroid tumors removed is shown in Fig. 1.
IOPTH monitoring and IVS for regionalization
IOPTH was routinely available since 1999 and used in 45 (63 %) patients of group 2 and all patients were cured. In six cases with MGD, it directly influenced the course of the operation and prompted the need to explore the contralateral side. Overall, IOPTH had a sensitivity of 100 % [93.0–100 %] for predicting biochemical cure. In 33 patients, IVS was used, and revealed true positive results in 24 patients (sensitivity 77.4 % [60.7–90.3 %], accuracy 72.7 % [54.9–85.3 %]). IVS failed to regionalize the site of parathormone excess in seven patients (21 %) and was incorrect in two patients, respectively.
Results of surgery
Surgical results and complications are summarized in Table 3. There were no perioperative deaths, but morbidity of R-PTX was high in both groups (54 %).
Cryopreservation was performed in 25 (46 %) patients of group 1 and 35 (49 %) patients of group 2 who underwent R-PTX in our hospital, namely in all patients with more than one R-PTX, MGD or additional thyroid resection during the initial surgery. In 11 patients (six of group 1 and five of group 2), an autotransplantation of cryopreserved parathyroid tissue was performed 6 to 12 months after R-PTX and all 11 patients became normocalcemic.
Five (9 %) patients of group 1 and one patient of group 2 (1.4 %) remained hypercalcemic after R-PTX and require careful review.
Discussion
In pHPT, all efforts should be made to achieve definitive long-term cure within a successful initial operation, since reoperations for persistent or recurrent pHPT are challenging and associated with high morbidity [4, 15–19].
A thorough knowledge of the parathyroid anatomy and experience in parathyroid surgery, the unequivocal confirmation of the diagnosis of ppHPT/rpHPT, and definite exclusion of other causes for hypercalcemia are prerequisite for a successful R-PTX [1, 4, 16, 20, 21]. Mitchell et al. have shown that significantly more parathyroid reoperations originating from low-volume centers are avoidable compared with those performed at high-volume centers [22]. Thus, parathyroid surgery should preferably be performed by experienced endocrine surgeons [1, 2, 6, 17, 23]. This request is underlined by the fact that reoperation was necessary due to an undetected solitary parathyroid adenoma in the majority of patients who underwent initial surgery elsewhere.
Once the diagnosis is confirmed, the indications for reoperation must be reconsidered [1–4, 17, 23]. In our series, all patients met the strict criteria for reoperative surgery, either because of severe symptomatic pHPT or high serum calcium levels. Nevertheless, six patients (5 %) remained hypercalcemic after R-PTX in our hospital. None of these patients suffered from familial hypocalciuric hypercalcemia. Two patients with sporadic ppHPT underwent R-PTX before 1998, despite negative imaging and no parathyroid tumor could be detected during the initial or R-PTX. Admittedly, nowadays both patients would be good candidates for medical therapy instead of R-PTX, although both patients suffered from recurrent nephrolithiasis. Only one patient (1 %) of group 2 still remains mildly hypercalcemic despite four neck explorations. The latest R-PTX, including sternotomy, was done in our hospital due to severe hypercalcemia with Ca levels above 3 mmol/l and bone pain, but no parathyroid tumor could be detected. Current Mibi/SPECT and US results suggest a parathyroid tumor in the neck. However, we do not recommend another R-PTX in favor of a medical therapy to prevent RLNP or permanent hypoparathyroidism.
A careful personal and family history should be taken, since it might reveal a potential inherited disease. In the presented series, nine (7 %) patients underwent R-PTX for MEN1 associated pHPT, which was not diagnosed at the time of initial surgery.
In addition, histopathological specimens and previous operative reports have to be re-evaluated before R-PTX to determine the number of the remaining parathyroid glands and the presence of MGD [6, 19, 23]. Our detailed evaluation suggests that less than 30 % of the suspected abnormal parathyroid glands, but 52 normal parathyroid glands have been excised during initial PTX elsewhere.
No R-PTX should be undertaken without the attempt to preoperatively localize the source of the PTH secretion. Mibi and US are the most frequently used localization methods for parathyroid disease over the past two decades.
Mibi is considered the most sensitive noninvasive imaging modality for detecting pathological cervical and mediastinal glands with a sensitivity of up to 77 % [19, 24, 25]. SPECT can further improve the sensitivity and specificity, especially in patients with concomitant goiter [4–6, 11, 14, 23]. In the present study, the results of Mibi together with SPECT improved also over time with a sensitivity of 62 % in group 1 vs. 76 % in group 2 and an accuracy of 57 % in group 1 vs. 71 % in group 2.
However, equal results of Tl–Tc scintigraphy and Tc99msestamibi scintigraphy in 10 out of 12 patients of group 1 suggest that implementation of Tc99msestamibi scintigraphy alone does not explain the considerable increase of sensitivity and accuracy. This refers to the high significance of SPECT, which was performed in all but one patient of group 2 before R-PTX.
US also provides anatomical information and reveals possible concomitant thyroid pathologies. Results of US are strongly dependent on the skill of the investigator. Sensitivities for the detection of parathyroid tumors are very variable and range from 22 to 82 % [1, 3, 4, 6, 11, 18, 26]. In the present study, comparing results of the two decades, US improved with a sensitivity of 80 % and accuracy of 75 % in group 2 (Table 2).
In group 2, almost all patients underwent preoperative US (68/71, 96 %). Five patients had US examination elsewhere. Adding these true-positive results to our data, sensitivity and accuracy rates of US will increase to 82 and 76 %, respectively. Only three patients were reoperated with CT or MRI imaging instead of US.
If US and Mibi/SPECT show discordant or negative results, further noninvasive localization procedures like MRI rather than CT scans should be considered. Although both techniques improved over the years, overall results remain poor to average with sensitivity rates of 62 % (MRI) and only 44 % (CT) in the present study (group 2). These poor results may be due to the fact that MRI and CT scans were used just in cases with inconclusive results in US or Mibi/SPECT.
Preoperative SVS is a valuable localization/regionalization procedure with high sensitivity rates [1, 4, 13, 16, 19, 26]. It is an appropriate tool in patients with negative results in noninvasive imaging techniques. However, it requires a high level of technical expertise; it is time- and cost-intensive and bears the potential risk of major complications like adverse reactions to the applied contrast agent or bleeding [13]. In our series, we did not observe any complications and sensitivity rates were impressively high (see Table 2).
In addition, we were able to report on 33 patients with intraoperative venous sampling (IVS), as an user-optimized procedure. With significant PTH gradients between both sides of the neck, IVS can regionalize the source of PTH excess and, if positive, allows a focused R-PTX [4, 27]. In the present study, IVS showed a sensitivity of 71 % and an accuracy of 77 %. Interestingly, IVS correctly regionalized the source of PTH excess in six of seven patients with negative preoperative imaging results, and no complications were observed performing IVS.
Intraoperative PTH measurement (IOPTH) in R-PTX can be helpful to avoid unnecessary extension of the neck exploration by indicating an adequate decrease of PTH levels after resection of a parathyroid tumor [4, 6, 10, 11, 27]. In the current study, IOPTH directly influenced the course of the operation in six patients with multiglandular disease, since the lack of PTH decrease after excision of one or two unilateral pathological parathyroid glands prompted the surgeon to explore the contralateral side, which was the key for cure.
Data show that there is an increase of imaging methods over the years particularly regarding Tc99msestamibi (from 43 % up to 99 %). While Tc99msestamibi was available since the early 1990s and performed in patients of both groups, additional SPECT was only performed in group 2 patients.
Furthermore, US imaging increased significantly from 83 % up to 96 % and SVS was performed in only five patients (9 %) of group 1, whereas 35 patients of group 2 (49 %) underwent this invasive preoperative imaging procedure (p < 0.001). IVS, like SPECT, was performed in group 2 patients only. MRI studies increased about 9 %, while the frequency of CT scans dropped by 30 % (see Table 2).
The authors were able to show a considerable increase in sensitivity and accuracy rates of US (62/64 % vs. 82/76 %), scintigraphy after implementation of SPECT (62/57 % vs. 76/71 %), and MRI (39/33 % vs. 62/55 %) within two decades of R-PTX. The significance of noninvasive localization procedures in parathyroid surgery is supported by the fact that ppHPT occurs in only 1.8 % after minimal invasive parathyroidectomy for benign pHPT in our hospital, provided that preoperative imaging was positive and IOPTH showed an adequate decrease of PTH levels. The increase in sensitivity and accuracy rates in combination with the additional implementation of highly efficient invasive pre- and intraoperative localization tools like SVS (80/69 %) and IVS (77/73 %) sufficiently explain the marked improvement in success rates (91 vs. 98.6 %, p = 0.08). Our results might obviate the need for additional cost expensive and invasive localization tools, like met-PET, FNA, and SVS with Quick-PTH recommended by Hessman et al. [6].
Improved preoperative imaging and the availability of IOPTH led to significant more focused/targeted R-PTX in the last decade (57 % group 2 vs. 23 % group 1, p = 0.0001). Focused R-PTX might be associated with a lower morbidity rate than bilateral cervical exploration [4, 19, 23, 24, 27]. However, the overall complication rate (54 %) was still considerably high in both groups.
In the present series, the higher frequency of sternotomies in patients of group 1 was not related to the experience of the surgeon, but most likely to the imaging modalities. All R-PTX were performed by very experienced endocrine surgeons. This is underscored by the fact that the majority of abnormal glands were identified during R-PTX in normal anatomic positions (69 %), which was not significantly different between group 1 and 2 (73 vs. 66 %, p = 0.38). Nowadays, a positive Tc99msestamibi-SPECT scan is able to exclude a retrosternal location, whereas in the majority of cases of group 1 a possible retrosternal location could only be excluded by surgical exploration. Moreover, the rate of true positive Mibi results improved from less than 60 % before routine use of Mibi/SPECT to more than 70 %, while the false-negative results dropped from 35 % (group 1) to 23 % in group 2.
The significantly reduced rate of sternotomies in group 2 (14 %) vs. group 1 (35 %, p = 0.0095) led to a significant reduction of complications such as pneumonia, bleeding, pneumothorax, and markedly reduced general health status in group 2 (p = 0.0013). However, the rate of RLNP remained constantly high (9 %) over time, despite implementation, and routine use of IONM in the last decade (group 2). Thus, we cannot confirm the excellent low RLNP rates of around 1 % reported by others [1, 4, 5, 17, 23]. Richards et al. [5] showed excellent results concerning permanent RLNP and hypoparathyroidism. This is potentially due to a limited extent of the reoperation, and is achieved at the expense of a significantly lower success rate of 89 % compared to 98.6 % in our series (p = 0.02). A method to avoid preparation in severely fibrotic tissue is to lateralize the vascular sheath and enter the thyroid region via a lateral approach [4, 6].
The rate of permanent postoperative hypoparathyroidism tended to be lower in the last decade (20 % group1 vs. 13 % group 2, p = 0.2) This is most likely due to the fact that we were able to perform more focused operations in group 2. The current rate of permanent hypoparathyroidism after R-PTX is in accordance with those reported in the literature (2 to 41 %) [4, 5, 17, 28]. One important issue with regard to permanent hypoparathyroidism is the need for cryopreservation of parathyroid tissue during R-PTX. In the present study, autotransplantation of cryopreserved parathyroid tissue was able to reverse hypocalcemia in six of 11 patients of group 1 and five of nine patients of group 2, resulting in a rate of permanent hypocalcemia after all interventions of 9.2 % (group 1) and 5.6 % (group 2).
In conclusion, the presented data demonstrate that cure rates of R-PTX for ppHPT and rpHPT are almost equal the cure rates of primary operations in expert centers. Cost expensive additional localization techniques like methionin PET or fine-needle aspiration do not necessarily have to be implemented before R-PTX, if experienced sonographers, Mibi/SPECT and IOPTH/IVS are available. Localization studies before R-PTX are obligatory and all efforts should be made to identify the abnormal parathyroid tissue to make a targeted approach possible. If imaging is negative, the morbidity risk of a bilateral R-PTX has to be balanced seriously with medical treatment options, such as calcimimetics.
References
Grant CS, Herden JA, Charboneau JW, James EM, Reading CC (1986) Clinical management of persistent and/or recurrent primary hyperparathyroidism. World J Surg 10:555–565
Akerström G, Rudberg C, Grimelius L, Johannsson H, Lundström B, Rastad J (1992) Causes of failed primary exploration and technical aspects of re-operation in primary hyperparathyroidism. World J Surg 16:562–568
Jaskowiak N, Norton JA, Alexander HR, Doppman JL, Shawker T, Skarulis M, Marx S, Spiegel A, Fraker DL (1986) A prospective trial evaluating a standard approach to reoperation for missed parathyroid adenoma. Ann Surg 224(3):308–320
Karakas E, Zielke A, Dietz C, Rothmund M (2005) Reoperations for primary hyperparathyroidism. Chirurg 76:207–216
Richards ML, Thompson GB, Farley DR, Grant CS (2008) Reoperative parathyroidectomy in 228 patients during the era of minimal-access surgery and intraoperative parathyroid hormone monitoring. Am J Surg 196:937–943
Hessman O, Stalberg P, Sundin A, Garske U, Rudberg C, Eriksson L-G, Hellman P, Akerström G (2008) High success rate of parathyroid reoperation may be achieved with improved localization diagnosis. World J Surg 32:774–781
Henry JF, Sebag F, Cherenko M, Ippolito G, Taieb D, Vaillant J (2008) Endoscopic parathyroidectomy: why and when? World J Surg 32:2509–2515
Bergenfelz A, Kanngiesser V, Zielke A, Nies C, Rothmund M (2005) Conventional bilateral cervical exploration versus open minimally invasive parathyroidectomy under local anaesthesia for primary hyperparathyroidism. Br J Surg 92(2):190–197
Udelsman R, Lin Z, Donovan P (2011) The superiority of minimally invasive parathyroidectomy based on 1650 consecutive patients with primary hyperparathyroidism. Ann Surg 253:585–591
Miura D, Wada N, Arici C, Morita E, Duh Q-Y, Clark OH (2002) Does intraoperative parathyroid hormone assay improve the results of parathyroidectomy? World J Surg 26:926–930
Siperstein A, Berber E, Mackey R, Alghoul M, Wagner K, Milas M (2004) Prospective evaluation of sestamibi scan, ultrasonography, and rapid PTH to predict the success of limited exploration for sporadic primary hyperparathyroidism. Surgery 136:872–880
Udelsman R, Aruny JE, Donovan P, Sokoll LJ, Santos F, Donabedian R, Venbrux AC (2002) Rapid parathyroid hormone analysis during venous localization. Ann Surg 237(5):714–721
Reidel MA, Schilling T, Graf S, Hinz U, Nawroth P, Büchler MW, Weber T (2006) Localization of hyperfunctioning parathyroid glands by selective venous sampling in reoperation for primary or secondary hyperparathyroidism. Surgery 140:907–913
Gotthardt M, Lohmann B, Behr TM, Bauhofer A, Franzius C, Schipper ML, Wagner M, Höffken H, Sitter H, Rothmund M, Joseph K, Nies C (2004) Clinical value of parathyroid scintigraphy with technetium-99m methoxybutylisnitrile: discrepancies in clinical data and a systematic metaanalysis of the literature. World J Surg 28:100–107
Grant C, Thompson G, Farley D, Heerden JV (2005) Primary hyperparathyroidism surgical management since the introduction of minimally invasive parathyroidectomy. Arch Surg 140:472–479
Jaskowiak N, Norton JA, Alexander HR, Doppman JL, Shawker T, Skarulis M, Marx S, Spiegel A, Fraker DL (1996) A prospective trial evaluating a standard approach to reoperation for missed parathyroid adenoma. Ann Surg 224(3):308–320
Brennan MF, Norton JA (1985) Reoperation for persistent and recurrent hyperparathyroidism. Ann Surg 201(1):40–44
Cheung PS, Borgstrom A, Thompson NW (1989) Strategy in reoperative surgery for hyperparathyroidism. Arch Surg 124(6):676–680
Shen W, Duren M, Morita E, Higgins C, Duh QY, Siperstein A, Clark OH (1996) Reoperation for persistent or recurrent primary hyperparathyroidism. Arch Surg 131(8):861–867
Akerström G, Malmaeus J, Bergström R (1984) Surgical anatomy of human parathyroid glands. Surgery 95:14–21
Van Heerden JA, Grant CS (1991) Surgical treatment of primary hyperparathyroidism: an institutional perspective. World J Surg 15(6):688–692
Mitchell J, Milas M, Barbosa G, Sutton J, Berber E, Siperstein A (2008) Avoidable reoperations for thyroid and parathyroid surgery: effect of hospital volume. Surgery 144(5):899–906
Henry JF (2010) Reoperation for primary hyperparathyroidism: tips and tricks. Langenbecks Arch Surg 395:103–109
Sebag F, Shen W, Brunaud L, Kebebew E, Duh QY, Clark OH (2003) Intraoperative parathyroid hormone assay and parathyroid reoperations. Surgery 134:1049–1056
Fayet P, Hoeffel C, Fulla Y, Legmann P, Hazebroucq V, Luton JP, Chapuis Y, Richard B, Bonnin A (1997) Technetium-99m sestamibi scintigraphy, magnetic resonance imaging and venous blood sampling in persistent and recurrent hyperparathyroidism. Brit J Radiol 70:459–464
Jones JJ, Bruneaud L, Dowd CF, Duh QY, Morita E, Clark OH (2002) Accuracy of selective venous sampling for intact parathyroid hormone in difficult patients with recurrent or persistent hyperparathyroidism. Surgery 132:944–951
Irvin GL III, Molinari AS, Figueroa C, Carneiro DM (1999) Improved success rate in reoperative parathyroidectomy with intraoperative PTH assay. Ann Surg 229:874–879
Powell AC, Alexander HR, Chang R, Marx SJ, Skarulis M, Pingpank JF, Bartlett DL, Hughes M, Weinstein LS, Simonds WF, Collins MF, Shawker T, Chen CC, Reynolds J, Cochran C, Steinberg SM, Libutti SK (2009) Reoperation for parathyroid adenoma: a contemporary experience. Surgery 146:1144–1155
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Karakas, E., Müller, HH., Schlosshauer, T. et al. Reoperations for primary hyperparathyroidism—improvement of outcome over two decades. Langenbecks Arch Surg 398, 99–106 (2013). https://doi.org/10.1007/s00423-012-1004-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-012-1004-y