Abstract
Background and aims
Cigarette smoking is linked to thromboembolic events; however, a relationship between nicotine exposition and thrombosis has not been established. Thus, we intended to study the effect of acute and chronic nicotine application in an in vivo mouse model.
Materials and methods
In microvessels of the dorsal skin fold chamber, light-dye-induced thrombus formation was analyzed using intravital fluorescence microscopy. Male and female C57BL/6J mice received nicotine chronically via the drinking water (100 μg/ml) for 8 weeks. An additional series of experiments was performed with acute iv nicotine treatment (3 mg/kg body weight).
Results
No significant differences in microvascular thrombus formation were detected after chronic nicotine application in male and female animals when compared with controls. Accordingly, flow cytometric analysis did not show significant effects on platelet activity. Chronic nicotine treatment resulted in a significantly reduced endothelial activation in male, but not in female mice. In contrast, acute iv application of nicotine revealed significantly shorter thrombosis times in arterioles of female mice and a significantly increased endothelial P-selectin expression in mice of both genders.
Conclusion
Chronic nicotine application does not promote microvascular thrombus formation in mice of either gender, whereas acute high-dose iv administration caused a significant increase of arteriolar thrombosis in female animals probably via a synergistic effect of increased endothelial P-selectin expression and female hormone levels. A gender-dependency of acute nicotine action can be presumed.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cigarette smoking is the leading cause of preventable premature death in the developed world [1]. It promotes atherosclerosis and is associated with an increased risk of cardiac death, myocardial infarction, angina pectoris, peripheral vascular disease, and stroke [2]. This predisposition for atherosclerotic diseases is based on the damaging effects of cigarette smoke on the endothelium [3], increased platelet activation [4, 5], increased fibrinogen and thrombin levels, and an activation of plasmatic coagulation [6, 7]. Nicotine is the addiction-causing agent in cigarette fume and has been suspected to contribute to some of the negative effects of smoking. For example, acute local exposure to nicotine was associated with an impaired response to endothelium-derived nitric oxide in human veins [8]. However, a causal role of nicotine for these cardiovascular disorders has not been proven [9, 10]. In fact, nicotine, at concentrations seen in smokers, has been shown to exert an inhibitory effect on platelet activation in vitro [11]. Furthermore, nicotine substitution therapy is considered as a safe aid to smoking cessation and did not increase adverse cardiac events in a randomized, double-blind placebo-controlled trial in patients with transdermal nicotine replacement and cardiac disease [12].
To further address this ambiguous issue, we studied the effect of chronic nicotine treatment on microvascular thrombus formation in an in vivo mouse model applying intravital fluorescence microcopy of the dorsal skinfold chamber. Concomitantly, in vitro experiments were conducted to investigate the influence of nicotine on endothelial cell function and platelet reactivity. All experiments were performed in animals of either sex to address the gender differences in the prognosis after ischemic coronary events [13]. Smoking appears to be the crucial factor for the increased prothrombotic risk in the context of oral contraceptive use, underlining a potential coherence with female sex hormone levels [14, 15]. Finally, we did not only study the effects of chronic nicotine exposure but also chose high-dose intravenous nicotine exposition to address the immediate toxicity of nicotine.
Materials and methods
Mouse dorsal skinfold chamber
Upon approval by the local government, all experiments were carried out in accordance with the German legislation on protection of animals and the National Institutes of Health ‘Guide for the Care and Use of Laboratory Animals’ (Institute of Laboratory Animal Resources, National Research Council). C57BL/6J mice with a body weight (bw) of 23–27 g were anesthetized by an intraperitoneal injection of ketamine (90 mg/kg bw) and xylazine (25 mg/kg bw).
For the study of microvascular thrombus formation, we used the dorsal skinfold chamber, as originally described by Lehr et al. [16] in mice. Before the preparation, animals were placed on a heating pad coupled to a rectal probe. Briefly, a double skin layer on the back on the animal was implanted between two symmetric titanium frames. One skin layer was then completely removed in a circular area of 15 mm in diameter, and the remaining layers (consisting of striated skin muscle, subcutaneous tissue, and skin) were covered with a glass coverslip incorporated into one of the titanium frames (Fig. 1a–c). Animals tolerated the chamber well and showed no signs of discomfort or changes of sleeping and feeding habits. Before intravital microscopy, animals were allowed a recovery period of 3 days.
a Dorsal skinfold chamber preparation with b the observation window, allowing the c direct visualization of the striated muscle microcirculation. d–f Developing venular microvascular thrombus (arrow heads) at three different time points after light-dye-induced endothelial damage (magnification ×630)
In vivo thrombosis model
On day 4, after the skinfold chamber preparation, thrombus formation was induced in randomly chosen venules (n = 3–4 per preparation) and arterioles (n = 1–2 per preparation). After injection of 0.1 ml fluorescein isothiocyanate (FITC)-labeled dextran (2%; MW 150000, Sigma-Aldrich, Munich, Germany) into the retro-orbital venous plexus and subsequent circulation for 30 s, microcirculation of the striated muscle tissue was visualized by intravital fluorescence microscopy using a Zeiss microscope (Axiotech vario, Zeiss, Jena, Germany). The microscopic procedure was performed at a constant room temperature of 21–23°C. The epi-illumination setup included a 100-W HBO mercury lamp and a blue filter (450–490/>520 nm excitation/emission wavelength). Microscopic images were recorded by a charge-coupled device video camera (FK 6990A-IQ, Pieper, Schwerte, Germany) and stored on videotapes for off-line evaluation (S-VHS Panasonic AG 7350-E, Matsushita, Tokyo, Japan). Using a ×20 water immersion objective (Achroplan ×20/0.50 W, Zeiss), baseline blood flow was monitored in individual arterioles (diameter range 15–30 μm) and venules (diameter range 20–40 μm). Subsequently, photochemical thrombus formation was induced by continuous local exposure of filtered light (450–490/>520 nm excitation/emission wavelength) and a ×63 water immersion objective (Achroplan ×63/0.95 W, Zeiss) to the individual microvessels (Fig. 1d–f), as described previously [17–19]. The light/dye thrombosis model used is based on endothelial injury by phototoxicity induced by exposure of FITC to excitation light. The phenomenon is mediated by reactive oxygen species, in particular singlet oxygen, generated by excitation of the fluorochrom. Microvascular thrombosis in this model involves endothelial injury, although not widespread denudation. Thrombi are primarily composed of platelets and a smaller number of leukocytes [20]. Light exposure was discontinued after blood flow in the vessel ceased for at least 60 s due to complete vessel occlusion.
Microcirculation analysis
Intravascular thrombus formation, i.e., change of inner luminal vessel diameter due to platelet and/or leukocyte adherence to the endothelium of the vessel wall, and microcirculatory parameters (blood flow velocity, vessel diameter) were quantified off-line by analysis of the videotaped images using a computer-assisted image analysis system (CapImage, Zeintl Software, Heidelberg, Germany). Analysis included the following parameters: thrombus formation with determination of the time periods until (1) first cell deposition (platelets, leukocytes) was observed along the endothelial lining, (2) the inner diameter of the microvessel was reduced to 50% by the growing thrombus, (3) initial occurrence of stasis (at least 5-s duration), and (4) sustained cessation of blood flow due to vessel occlusion. Microcirculatory analysis further included the determination of vascular wall shear rates based on the Newtonian definition γ = 8 × V/D (V represents the red blood cell centerline velocity divided by 1.6 according to the Baker–Wayland factor [21], and D represents the individual inner vessel diameter).
Experimental design
To closely resemble the usual way of nicotine uptake, male and female C57BL/6J mice received nicotine chronically via the drinking water (100 μg/ml) for 8 weeks. Oral intake of nicotine at this dosage has been shown to induce cotinine levels, the stable major metabolite of nicotine, similar to those seen in chronic smokers in previous studies in mice [22, 23]. Additionally, plasma levels of cotinine were determined to ensure appropriate levels in this particular study. Control animals of both genders received normal drinking water. As nicotine content of the drinking water with possible alterations in taste and smell might theoretically deter mice from consuming this water, drinking bottles were weighted for both treatment groups to demonstrate an equal amount of fluid intake over a representative time period of 7 days. To study the effects of acute nicotine application on microvascular thrombus formation, additional male and female mice were injected with nicotine (3 mg/kg iv) 5 min before the beginning of the experiments.
Determination of cotinine levels by gas chromatography
Two hundred microliter serum was filled in tubes spiked with 1 μl of internal standards solution for cotinine-d3 (2 μg/ml). Then, samples were vortexed, allowed to equilibrate for 5 min, and alkalinized with 100 μl 2.0 M potassium carbonate. One hundred microliter of a mixture of trichlormethane, acetonitrile, and ethyl acetate (4:3:2) were added. Samples were capped and mixed for 5 min on the vortex mixer and then centrifuged. The organic phase was used for injection into the GC-MS (Hewlett Packard GC 6890 Series II with 5971 MSD, Column 12 m Ultra 1, Hewlett Packard, Boblingen, Germany). For quantification of cotinine, 98/101 m/z was used. The analyte concentrations in the samples were determined using five-point calibration lines with cotinine concentrations ranging from 0 to 100 ng/ml. Linearity of the calibration lines was good, with typical r 2 values of 0.997. The limit of quantification was 4.9 ng/ml.
Preparation of murine platelet rich plasma
For in vitro testing of platelet function, 0.5–1 ml blood was drawn from the retro-orbital venous plexus of untreated mice with 1.5-cm glass capillaries and collected into a tube containing 300 μl Tyrode buffer solution (TBS) and heparin (20 U/ml). The sample was centrifuged for 5 min at 750×g, followed by recentrifugation of the supernatant for 6 min at 150×g, yielding platelet rich plasma (PRP). PRP was centrifuged again for 5 min at 1,825×g, and the cell pellet was resuspended in 1 ml TBS with 1 μM prostacyclin and 10 U/ml heparin for subsequent incubation at 37°C for 10 min. Centrifugation (5 min at 1,825×g) and resuspension were repeated twice. Finally, the platelet pellet was resuspended in 450 μl TBS with 2 μl apyrase [24]. Platelet suspensions were transferred into a 37°C water bath for 30 min of resting to eliminate isolation-induced platelet activation. Then, platelets were incubated with nicotine (50 nM) for additional 30 min in water followed by exposure to thrombin (20 U/ml) and incubation with saturating amounts of the appropriate antibody. The nicotine concentration of 50 nM nicotine is comparable to levels in chronic smokers [11]. Platelets from control animals were kept continuously at 37°C without addition of nicotine.
Flow cytometric analysis of P-selectin and CD107a expression
For evaluation of receptor expression under resting conditions, 5 μl of specific rat anti-mouse P-selectin (Emfret Analytics, Eibelstadt, Germany) and CD107a (BD Biosciences, Heidelberg, Germany) or negative control antibodies and 25 μl platelet suspension were combined and incubated for 15 min at room temperature. The reaction was stopped by addition of 400 μl PBS. Analysis was performed within the subsequent 30 min. In addition, the same set of experiments was carried out after exposure to thrombin for maximal platelet activation (20 U/ml).
FACScan flowcytometer (Becton Dickinson) was calibrated with fluorescent standard microbeads (CaliBRITE Beads, Becton Dickinson) for accurate instrument setting. Platelets were identified by their characteristic forward and sideward light scatter and selectively analyzed for their fluorescence properties using the CellQuest program (Becton Dickinson) with assessment of 20.000 events per sample. The relative fluorescence intensity of a given sample was calculated by subtracting the signal obtained when cells were incubated with the isotype specific control antibody from the signal generated by cells incubated with the test antibody.
Enzyme-linked immunosorbent assay of circulating endothelial markers
Plasma concentrations of circulating, i.e., soluble (s) sP-selectin, sE-selectin, intercellular adhesion molecule-1 (sICAM-1), and vascular cell adhesion molecule-1 (sVCAM-1), were determined using the respective enzyme immunoassay kits (R&D Systems, Minneapolis, MN, USA). Blood samples were prepared by centrifugation for 10 min at 2,000×g and room temperature (GS-6R Centrifuge, Beckman Coulter, Fullerton, CA, USA).
Histology and immunohistochemistry
At the end of each experiment, a cross-section tissue block of the dorsal skinfold chamber was fixed in 4% phosphate buffered formalin for 2–3 days and embedded in paraffin. From the paraffin-embedded tissue blocks, 4-μm sections were cut and stained with hematoxylin and eosin (HE) for histological analysis. For immunohistochemical demonstration of P-selectin, ICAM-1, and PAF-R expression, sections collected on poly-l-lysine-coated glass slides were treated by microwave for antigen unmasking. For evaluation of PAI-1 expression, sections were treated by proteinase K. Goat anti-P-selectin (1:100), anti-PAF-R (1:400), anti-ICAM-1 (1:200), and anti-PAI-1 (1:100, all Santa Cruz Biotechnology, Heidelberg, Germany) were used as primary antibodies and incubated for 90–120 min at room temperature. This was followed by a horseradish peroxidase-conjugated donkey anti-goat antibody (1:25; Santa Cruz Biotechnology) and development using DAB (P-selectin) and ACE (PAF-R, ICAM-1, PAI-1) substrate as chromogen. The sections were counterstained with hematoxylin and examined by light microscopy (Zeiss Axioscop 40, Zeiss, Jena, Germany).
Statistical analysis
After proving the assumption of normality and equal variance across groups, differences between groups were assessed using one-way analysis of variance followed by the appropriate post-hoc comparison test. All data were expressed as means±SEM, and overall statistical significance was set at p < 0.05. Statistics and graphics were performed using the software packages SigmaStat and SigmaPlot (Jandel Corporation, San Rafael, CA, USA).
Results
Influence of nicotine content on intake of drinking water and cotinine plasma levels
Consumption of drinking water over a time period of 7 days was −9.2 ± 0.5% of the initial bottle weight for nicotinated water and −9.1 ± 0.4% for unaltered water (p = not significant), implying an equal amount of fluid intake irrespective of nicotine content. Nicotine intake calculated from the animals’ body weights and usage of drinking water averaged ∼15 mg kg−1 day−1. Cotinine plasma levels amounted to >100 ng/ml in nicotine-treated mice and <10 ng/ml in control mice. These data are very similar to those obtained by other groups, and the model appears to be suitable for exposing experimental animals to nicotine for several weeks [25].
Chronic nicotine treatment does not influence microvascular thrombus formation in vivo
Red blood cell (RBC) velocities and wall shear rates did not differ significantly between chronic nicotine treatment and controls in mice of either gender (Table 1). In male controls, light-dye mediated thrombus formation induced complete occlusion of arterioles and venules after 577 ± 78 and 520 ± 89 s, respectively. After chronic nicotine treatment, complete occlusion of arterioles and venules did not differ significantly from these values (arterioles, 640 ± 96 s; venules, 427 ± 51 s; Fig. 2a and b). In parallel, thrombus formation in female mice was not significantly influenced by chronic nicotine treatment. Arteriolar and venular vessels were found clogged at an average time of 866 ± 24 and 459 ± 61 s in female controls and at 715 ± 130 and 493 ± 79 s in nicotine-treated females (Fig. 2a and b). In addition to this, we did not observe differences in thrombus formation between males and females either with or without nicotine treatment.
Occlusion times of arterioles (a) and venules (b) upon light-dye-induced thrombus formation in male (M-con; n = 8) and female (F-con; n = 6) controls (normal drinking water) and after chronic nicotine treatment of male (M-nic; n = 7) and female (F-nic; n = 6) mice [nicotine via drinking water for 8 weeks (100 μg/ml)]. Values are given as means±SEM; p=not significant
Nicotine exposition does not effect murine platelet P-selectin and CD107a expression
We studied the effect of nicotine application at a concentration of 50 nM on murine platelet activation. Thrombin-stimulation resulted in a marked increase of the expression of P-selectin and a slight increase of CD107a on the platelet surface of normal and nicotine-exposed platelets indicated by an increase in mean fluorescence. In vitro nicotine exposure did not significantly affect spontaneous platelet P-selectin and CD107a expression when compared to controls. In line with this, thrombin-induced expression of these two platelet activation markers also was not significantly influenced by nicotine neither in male nor in female mice (data not shown).
Chronic nicotine application reduces circulation of endothelial activation markers in male, but not in female mice
To characterize the effect of chronic nicotine exposure on endothelial cell activation, we determined circulating (soluble) endothelial activation markers. In male mice, nicotine exposure for 8 weeks resulted in a significant reduction of sP-selectin and sE-selectin when compared to controls (Fig. 3a and b). This effect was not seen in female mice, although a tendency towards a reduction could be observed. sICAM-1 was significantly elevated in female control mice when compared to male control mice, but nicotine treatment did not affect sICAM-1 circulation in mice of either sex (Fig. 3c). There were no substantial differences concerning sVCAM-1 (Fig. 3d). However, although chronic nicotine exposition did not significantly reduce the circulation of endothelial activation markers in female mice, it did, at least, not elicit an increase of these markers.
Plasma concentrations of circulating sP-selectin (a) and sE-selectin (b), sICAM-1 (c), and sVCAM-1 (d) in male (M-con) and female (F-con) controls (normal drinking water) and after chronic nicotine treatment of male (M-nic) and female (F-nic) mice [nicotine via drinking water for 8 weeks (100 μg/ml)]. n = 6–8 animals per group. Values are given as means±SEM; *p < 0.05 vs M-con
Chronic nicotine application dampens endothelial activation predominantly in male mice
In general, adhesion molecules were found expressed within the endothelium of arterioles and venules, whereas little, if any, immunoreactivity was detected within the surrounding subcutaneous and muscle tissue of the dorsal skinfold chamber. Endothelial expression of these molecules was assessed as percentage of positively stained vessels. Interestingly, chronic nicotine treatment caused a significant reduction of the endothelial expression of P-selectin, PAF-R, and PAI-1 in male mice when compared to controls (Fig. 4a,b and d). In contrast to this, a significant reduction in female mice was merely seen for PAI-1 after nicotine treatment when compared to female controls (Fig. 4d). Once again, the expression of ICAM-1 was not influenced by nicotine in mice of both genders (Fig. 4c). Of note, the expression of PAF-R was significantly higher in female mice compared to male mice after nicotine treatment (Fig. 4b).
Immunohistological analysis and exemplary microscopic images of female mice of the endothelial expression of P-selectin (a), PAF-R (b), ICAM-1 (c), and PAI-1 (d) in male (M-con) and female (F-con) controls (normal drinking water) and after chronic nicotine treatment of male (M-nic) and female (F-nic) mice [nicotine via drinking water for 8 weeks (100 μg/ml)]. n = 6–8 animals per group. Values are given as means±SEM. *p < 0.05 vs M-con, # p < 0.05 vs F-con, § p < 0.05 vs M-nic
Acute application of high-dose nicotine acts prothrombotic in arterioles of female mice
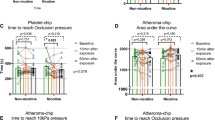
To test the direct effect of nicotine on the endothelium and on thrombogenicity in vivo, we injected nicotine at a dose of 3 mg/kg iv 5 min before thrombus induction. Of note, the average dose during chronic oral nicotine application amounted to ∼15 mg kg−1 day−1 or approximately 0.01 mg kg−1 min−1. In males, light-dye mediated thrombus formation induced complete occlusion of arterioles and venules after 419 ± 90 and 334 ± 31 s, respectively (Fig. 5a and b). Thrombosis times did not differ significantly from control mice. In contrast to this, arteriolar occlusion in female mice occurred significantly faster after acute nicotine application than in controls (arterioles, 302 ± 63 s; p < 0.05 vs controls, 832 ± 39 s), whereas acute nicotine exposure did not affect venular thrombus formation in female mice (Fig. 5b).
Occlusion times of arterioles (a) and venules (b) upon light-dye-induced thrombus formation in male (M-conac; n = 8) and female (F-conac; n = 8) controls (saline exposure) and after acute nicotine treatment of male (M-nicac; n = 4) and female (F-nicac; n = 6) mice (nicotine 3 mg/kg iv at −5 min). Values are given as means±SEM; # p < 0.05 vs F-conac
Acute application of high-dose nicotine boosts endothelial activation
According to the primary study design, we determined circulating (soluble) endothelial activation molecules after acute nicotine application. Briefly, we did not observe a reduction of the circulation of these four markers, but rather an increase of sP-selectin (Fig. 6a), sE-selectin (Fig. 6b), and sVCAM-1 (Fig. 6d) in both male and female mice. sICAM-1 was markedly reduced in both sexes (Fig. 6c). Immunohistochemistry confirmed this proneness for endothelial activation as a result of acute nicotine exposition, in particular for endothelial P-selectin expression (Fig. 7a) and, to a lesser extent, for PAF-R (Fig. 7b) and ICAM-1 (Fig. 7c). However, PAI-1 expression was found to be reduced in these mice (Fig. 7d). In summary, acute high-dose nicotine exposition in general exerted activating effects on the vascular endothelium.
Plasma concentrations of circulating sP-selectin (a) and sE-selectin (b), sICAM-1 (c), and sVCAM-1 (d) in male (M-conac) and female (F-conac) controls (saline exposure) and after acute nicotine treatment of male (M-nicac) and female (F-nicac) mice (nicotine 3 mg/kg iv at −5 min). n = 6–8 animals per group. Values are given as means±SEM; *p < 0.05 vs M-conac; # p < 0.05 vs F-conac, § p < 0.05 vs M-nicac
Immunohistological analysis and exemplary microscopic images of female mice of the endothelial expression of P-selectin (a), PAF-R (b), ICAM-1 (c), and PAI-1 (d) in male (M-conac) and female (F-conac) controls (saline exposure) and after acute nicotine treatment of male (M-nicac) and female (F-nicac) mice (nicotine 3 mg/kg iv at −5 min). n = 6–8 animals per group. n = 6–8 animals per group. Values are given as means±SEM. *p < 0.05 vs M-conac, # p<0.05 vs F-conac
Discussion
The major findings of the present study are that chronic oral nicotine exposition in a comparable extent as seen in smokers does not promote microvascular thrombus formation in vivo in animals of either gender. This might, at least in part, be due to the fact that nicotine did not cause an increase of spontaneous or thrombin-induced platelet activation in vitro. Furthermore, endothelial activation, as represented by endothelial expression and blood circulation of endothelial activation markers, was largely found to be abridged after 8 weeks of chronic nicotine uptake. This effect predominantly occurred in male mice, except for the expression of PAI-1 which was significantly reduced in both male and female animals. In contrast to this, we found a significantly increased thrombus formation in arterioles of female mice after acute high-dose exposure of nicotine, which was associated with a tendency towards enhanced expression of PAF-R and ICAM-1 and a significant increase in endothelial P-selectin expression. Male mice did not exhibit accelerated thrombosis times after iv application of nicotine despite similar effects on endothelial activation. Based on these data, acute nicotine application at a high concentration has prothrombotic properties predominantly in females, implying a gender-dependency of acute nicotine action.
Cigarette smoking continues to be one of the world’s most serious public health problems, being the major risk factor of ischemic heart disease and thrombo–embolic events [26]. Being aware that the smoke of a cigarette contains more than 4,000 potential noxious substances, numerous studies have been conducted attempting to identify the harmful agent in cigarette smoke. Nicotine exerts sympathomimetic effects and leads to vasoconstriction and hypertension [9]. On the other hand, other components of the cigarette smoke, among them tar, carbon monoxide, polycyclic aromatic hydrocarbons, cyanide, and cadmium, might have detrimental effects, as these have been shown to increase platelet activation, fibrinogen levels, and leukocyte adhesion [5, 12, 27]. Thus, it has to be differentiated between the possible effects of cigarette smoke and nicotine itself. Cigarette smoking has, in most cases, been shown to elicit negative effects on platelet and endothelial function. A clinical study in smokers showed an impairment of endothelial nitric oxide production with the possible consequence of increased thrombogenicity [28]. Cigarette smoke caused leukocyte adhesion to the vascular endothelium and increase of xanthine oxidase activity in hamsters, which could be attenuated by pretreatment with superoxide dismutase [29]. Platelets from chronic smokers express significantly more P-selectin in a resting state and bind more fibrinogen via the GP IIb–IIIa receptor after activation when compared to platelets from non-smokers [5]. Additionally, platelet-dependent thrombin generation is enhanced in smokers [7]. However, concerning the intrinsic effects of nicotine as the addiction-causing substance itself on endothelial and platelet activation and thrombus formation, in vitro data are controversial, and in vivo studies are scarce.
It has become common assumption that nicotine substitution to quit smoking is safe. In a placebo-controlled double-blind study using nicotine nasal spray in a smoking cessation program, cardiovascular risk factor could be significantly reduced without negative effects caused by nicotine substitution [30]. This is in line with a study showing a rapid decrease of the circulation of the endothelial adhesion molecules sICAM-1, sCD44v5, and sCD44v6 during chronic nicotine replacement therapy after smoking cessation [31]. In contrast to this, chronic nicotine application enhanced focal ischemic brain injury and reduced tissue plasminogen activator (t-PA) in a middle cerebral artery occlusion model in rats [32] and increased the production of PAI-1 by human brain endothelial cells in cell cultures [33]. In line with the effects caused by cigarette smoke in previous studies [29], acute nicotine application enhanced selectin-dependent rolling of leukocytes on nicotine-exposed microvessels of lung allografts [34]. Nicotine impaired endothelium-dependent dilatation in human veins in vivo, implying a defective endothelial function [8]. However, studies dealing with the effects of nicotine on platelet function revealed a reduced susceptibility of platelets to shear stress after nicotine exposition [35] and a 75% decline of the shear-dependent platelet activation [11]. Thus, a rather protective effect of nicotine on platelet reactivity has been proposed.
The results of this study now indicate that chronic nicotine consumption does not convey prothrombogenic effects in vivo. Concordantly, negative side effects are not observed with long-term transdermal nicotine substitution in the clinical setting. This might partly be due to the fact that endothelial activation was found to be reduced and that there was no significant impact on platelet function in both genders.
In a second step, we questioned whether acute intravenous nicotine application with a rapid rise in plasma nicotine levels might have different effects on microvascular thrombus formation and endothelial activation than constant uptake of nicotine. A steep increase of plasma nicotine concentration has been associated with adverse cardiac events due to its sympathomimetic properties [12]. In fact, cigarette smoking with deep inhalation of fume results in a rapid absorption of nicotine over the lungs occurring at a rate similar to that after iv administration [36]. The acute application of nicotine on HUVECS in in vitro studies resulted in an increased expression of ICAM-1 and VCAM-1 via a second messenger pathway involving PKC and p38 MAPK-mediated activation of NF-kappaB and AP-1 [37]. Moreover, acute nicotine exposure induced MAPK-mediated P-selectin and E-selectin-dependent leukocyte adhesion in allograft lung microvessels in vivo [34].
Based on our results, it can be presumed that a rapid increase in nicotine levels leads to an increase of endothelial activation. Therefore, it is possible that not the mere presence of nicotine in the blood, but rather speed and dose of nicotine exposure is crucial for its prothrombotic effects. Although the prothrombogenic effect of acute nicotine administration was seen in mice of both genders in this study, microvascular thrombus formation was solely increased in female mice. An in vitro study investigating platelet adhesion in patients prone to arterial and venous thrombosis in dependence to gender and smoking revealed that higher platelet activation occurs in men, ex-smokers and current smokers [38]. However, this study did not show an increased platelet reactivity in females. On the other side, numerous clinical and experimental studies link female hormone treatment to a generally increased risk for thrombotic and ischemic events [39, 40]. These adverse effects in particular occurred in smoking women [41]. We now show that gender differences exist in the context of acute nicotine application and would like to propose an increased, possibly MAPK-mediated, expression of endothelial P-selectin in combination with female hormone levels as underlying mechanism for the prothrombogenic effect of nicotine in arterioles of female mice. While P-selectin does not mediate platelet–platelet interaction, P-selectin provides an anchoring source for leukocytes on activated platelets and, thus, may play a very important role in determining the size and stability of the platelet aggregates in the developing thrombus [42]. In light of the fact that increased microvascular thrombosis was observed only in female, but not in male, mice despite a comparable rise in endothelial P-selectin expression after acute nicotine application, a relevant impact of female hormones can be assumed.
In general, unharmful effects of nicotine, independent of acute or chronic application, were mostly seen in male mice, whereas microvascular thrombus formation was only found to be accelerated in female mice.
Conclusion
Chronic continuous nicotine application does not promote microvascular thrombus formation on mice of either gender, which is supported by the fact that a general reduction of endothelial activation and a lack of impact on platelet activation were observed. In contrast to this, acute high-dose iv administration of nicotine caused a significant increase of arteriolar thrombus formation in female, but not in male animals, and boosted endothelial P-selectin expression in mice of both genders. Based on these data, acute nicotine application at a high concentration acts prothrombogenic particularly in females, probably implying a synergistic effect between increased endothelial P-selectin-expression and the presence of female hormones.
References
US Department of Health and Human Services (1990) The health benefits of smoking cessation. US Department of Health and Human Services, Public Health Service, Centers for Disease Control, Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health, Washington, DC. DHHS Publication No. (CDC) 90–8416
US Department of Health and Human Services (1983) The health consequences of smoking: cardiovascular disease: a report of the surgeon general. US Department of Health and Human Services, Public Health Service, Centers for Disease Control, Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health, Washington, DC. DHHS Publication No: (PHS) 84–50204
Zeiher AM, Schachinger V, Minners J (1995) Long-term cigarette smoking impairs endothelium-dependent coronary arterial vasodilator function. Circulation 92:1094–1100
Fuster V, Chesebro JH, Frye RL, Elveback LR (1981) Platelet survival and the development of coronary artery disease in the young adult: effects of cigarette smoking, strong family history and medical therapy. Circulation 63:546–551
Nair S, Kulkarni S, Camoens HM, Ghosh K, Mohanty D (2001) Changes in platelet glycoprotein receptors after smoking—a flow cytometric study. Platelets 12:20–26
Fitzgerald GA, Oates JA, Nowak J (1988) Cigarette smoking and hemostatic function. Am Heart J 115:267–271
Hioki H, Aoki N, Kawano K, Homori M, Hasumura Y, Yasumura T, Maki A, Yoshino H, Yanagisawa A, Ishikawa K (2001) Acute effects of cigarette smoking on platelet-dependent thrombin generation. Eur Heart J 22:56–61
Chalon S, Moreno H Jr, Benowitz NL, Hoffman BB, Blaschke TF (2000) Nicotine impairs endothelium-dependent dilatation in human veins in vivo. Clin Pharmacol Ther 67:391–397
Benowitz NL (1988) Pharmacologic aspects of cigarette smoking and nicotine addition. N Engl J Med 319:1318–1330
Benowitz NL (1997) Systemic absorption and effects of nicotine from smokeless tobacco. Adv Dent Res 11:336–341
Ramachandran J, Rubenstein D, Bluestein D, Jesty J (2004) Activation of platelets exposed to shear stress in the presence of smoke extracts of low-nicotine and zero-nicotine cigarettes: the protective effect of nicotine. Nicotine Tob Res 6:835–841
Joseph AM, Norman SM, Ferry LH, Prochazka AV, Westman EC, Steele BG, Sherman SE, Cleveland M, Antonnucio DO, Hartman N, McGovern PG (1996) The safety of transdermal nicotine as an aid to smoking cessation in patients with cardiac disease. N Engl J Med 335:1792–1798
Vaccarino V, Parsons L, Every NR, Barron HV, Krumholz HM (1999) Sex-based differences in early mortality after myocardial infarction. National registry of myocardial infarction 2 participants. N Engl J Med 341:217–225
Roy S (1999) Effects of smoking on prostacyclin formation and platelet aggregation in users of oral contraceptives. Am J Obstet Gynecol 180:S364–368
Holschermann H, Terhalle HM, Zakel U, Maus U, Parviz B, Tillmanns H, Haberbosch W (1999) Monocyte tissue factor expression is enhanced in women who smoke and use oral contraceptives. Thromb Haemost 82:1614–1620
Lehr HA, Leunig M, Menger MD, Nolte D, Messmer K (1993) Dorsal skinfold chamber technique for intravital microscopy in nude mice. Am J Pathol 143:1055–1062
Thorlacius H, Vollmar B, Seyfert UT, Vestweber D, Menger MD (2000) The polysaccharide fucoidan inhibits microvascular thrombus formation independently from P-and L-selectin function in vivo. Eur J Clin Investig 30:804–810
Vollmar B, Schmits R, Kunz D, Menger MD (2001) Lack of in vivo function of CD31 in vascular thrombosis. Thromb Haemost 85:160–164
Roesken F, Ruecker M, Vollmar B, Boeckel N, Morgenstern E, Menger MD (1997) A new model for quantitative in vivo microscopic analysis of thrombus formation and vascular recanalisation: the ear of the hairless (hr/hr) mouse. Thromb Haemost 78:1408–1414
Rumbaut RE, Randhawa JK, Smith CW, Burns AR (2004) Mouse cremaster venules are predisposed to light/dye-induced thrombosis independent of wall shear rate, CD18, ICAM-1, or P-selectin. Microcirculation 11:239–247
Baker M, Wayland H (1974) On-line volume flow rate and velocity profile measurements for blood in microvessels. Microvasc Res 7:131–143
Suner IJ, Espinosa-Heidmann DG, Marin-Castano ME, Hernandez EP, Pereira-Simon S, Cousins SW (2004) Nicotine increases size and severity of experimental choroidal neovascularization. Investig Ophthalmol Vis Sci 45:311–317
Heeschen C, Jang JJ, Weis M, Pathak A, Kaji S, Hu RS, Tsao PS, Johnson FL (2001) Nicotine stimulates angiogenesis and promotes tumor growth and atherosclerosis. Nat Med 7:833–839
Nieswandt B, Schulte V, Bergmeier W (2004) Flow-cytometric analysis of mouse platelet function. Methods Mol Biol 272:255–268
Rowell PP, Hurst HE, Marlowe C, Bennett BD (1983) Oral administration of nicotine: its uptake and distribution after chronic administration to mice. J Pharmacol Methods 9:249–261
McBride PE (1992) The health consequences of smoking. Cardiovascular diseases. Med Clin North Am 76:333–353
Howard G, Wagenknecht LE, Burke GL, Diez-Roux A, Evans GW, McGovern P, Nieto FJ, Tell GS (1998) Cigarette smoking and progression of atherosclerosis: The Atherosclerosis Risk in Communities (ARIC) Study. JAMA 279:119–124
Barua RS, Ambrose JA, Eales-Reynolds LJ, DeVoe MC, Zervas JG, Saha DC (2001) Dysfunctional endothelial nitric oxide biosynthesis in healthy smokers with impaired endothelium-dependent vasodilatation. Circulation 104:1905–1910
Lehr HA, Kress E, Menger MD, Friedl HP, Hubner C, Arfors KE, Messmer K (1993) Cigarette smoke elicits leukocyte adhesion to endothelium in hamsters: inhibition by CuZn-SOD. Free Radic Biol Med 14:573–581
Ludviksdottir D, Blondal T, Franzon M, Gudmundsson TV, Sawe UJ (1999) Effects of nicotine nasal spray on atherogenic and thrombogenic factors during smoking cessation. J Intern Med 246:61–66
Palmer RM, Stapleton JA, Sutherland G, Coward PY, Wilson RF, Scott DA (2002) Effect of nicotine replacement and quitting smoking on circulating adhesion molecule profiles (sICAM-1, sCD44v5, sCD44v6). Eur J Clin Investig 32:852–857
Wang L, Kittaka M, Sun N, Schreiber SS, Zlokovic BV (1997) Chronic nicotine treatment enhances focal ischemic brain injury and depletes free pool of brain microvascular tissue plasminogen activator in rats. J Cereb Blood Flow Metab 17:136–146
Zidovetzki R, Chen P, Fisher M, Hofman FM, Faraci FM (1999) Nicotine increases plasminogen activator inhibitor-1 production by human brain endothelial cells via protein kinase C-associated pathway. Stroke 30:651–655
Sikora L, Rao SP, Sriramarao P (2003) Selectin-dependent rolling and adhesion of leukocytes in nicotine-exposed microvessels of lung allografts. Am J Physiol Lung Cell Mol Physiol 285:L654–L663
Rubenstein D, Jesty J, Bluestein D (2004) Differences between mainstream and sidestream cigarette smoke extracts and nicotine in the activation of platelets under static and flow conditions. Circulation 109:78–83
Tutka P, Mosiewicz J, Wielosz M (2005) Pharmacokinetics and metabolism of nicotine. Pharmacol Rep 57:143–153
Ueno H, Pradhan S, Schlessel D, Hirasawa H, Sumpio BE (2006) Nicotine enhances human vascular endothelial cell expression of ICAM-1 and VCAM-1 via protein kinase C, p38 mitogen-activated protein kinase, NF-kappaB, and AP-1. Cardiovasc Toxicol 6:39–50
Lilienberg G, Venge P (1998) Platelet adhesion in patients prone to arterial and venous thrombosis: the impact of gender, smoking and heredity. Scand J Clin Lab Invest 58:279–286
Helmerhorst FM, Bloemenkamp KW, Rosendaal FR, Vandenbroucke JP (1997) Oral contraceptives and thrombotic disease: risk of venous thromboembolism. Thromb Haemost 78:327–333
Tanis BC, Rosendaal FR (2003) Venous and arterial thrombosis during oral contraceptive use: risks and risk factors. Semin Vasc Med 3:69–84
Chasan-Taber L, Stampfer MJ (1998) Epidemiology of oral contraceptives and cardiovascular disease. Ann Intern Med 128:467–477
Merten M, Thiagarajan P (2000) P-selectin expression on platelets determines size and stability of platelet aggregates. Circulation 102:1931–1936
Acknowledgments
The authors kindly thank Berit Blendow, Doris Butzlaff, Dorothea Frenz, Maren Nerowski, and Kathrin Sievert, Institute for Experimental Surgery, University of Rostock for their excellent technical assistance. This study is supported by a grant from the Deutsche Forschungsgemeinschaft, Bonn-Bad Godesberg, Germany (Vo 450/8-1).
Author information
Authors and Affiliations
Corresponding author
Additional information
Best abstracts — Surgical Forum 2007
Rights and permissions
About this article
Cite this article
Lindenblatt, N., Platz, U., Hameister, J. et al. Distinct effects of acute and chronic nicotine application on microvascular thrombus formation and endothelial function in male and female mice. Langenbecks Arch Surg 392, 285–295 (2007). https://doi.org/10.1007/s00423-007-0173-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-007-0173-6