Abstract
Background and aim
Scandinavian Quality Register for Thyroid and Parathyroid Surgery is an on-line web-based database with the aim to improve the quality of thyroid and parathyroid surgery. Preliminary data from surgery for primary hyperparathyroidism are reported here.
Materials and methods
Fifteen departments registered 806 operations, with 639 women (79.7%) and 167 men. The median age of the patients was 62 years.
Results
Approximately 95.4% of the patients had sporadic disease and first time operation was performed in 93.8% of the patients. Localization examinations were performed in 524 patients (65%); sestamibi scintigraphy in 413 patients, with a true positive adenoma localization in 64.4% and ultrasound in 293 patients with adenoma localization in 61.1%. Bilateral neck exploration was performed in 66.8%, unilateral exploration in 16.1%, and focused minimal invasive surgery in 17.1%. In 301 patients planned for limited parathyroid exploration, conversion to bilateral neck surgery occurred in 11%. The cure rate, based on short follow-up, was 91.9%. Postoperative hypocalcemia occurred in 11.4% of the patients, and was associated with reoperation, concomitant thyroid operation, and the weight of excised parathyroid tissue.
Conclusion
Localization examinations are performed in 2/3 of the patients, but limited neck exploration was performed in only approximately 1/3 of the operations. The cure rate was lower and postoperative hypocalcemia was more frequent than expected.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Primary hyperparathyroidism (pHPT) is a common disease. Thus, recent studies have suggested a prevalence of up to 3.4% [1] with the majority of patients being elderly women and concomitant cardiovascular disease is common [2]. The gold standard for treatment of the disease was, for many years, bilateral neck exploration with excision of the enlarged gland(s). With this strategy, more than 95% of the patients are reported cured by specialized centers [3]. However, with better preoperative localization procedures for enlarged parathyroid glands, most notably sestamibi scintigraphy [4] and ultrasound, and with the event of intraoperative monitoring of parathyroid hormone (iOPTH) [5–8], bilateral neck exploration has been challenged during the last decade by a variety of minimal invasive procedures [9]. The efficacy of these new strategies, especially on a national level and incorporating specialized as well as nonspecialized departments, is not known. This is of importance because the number of operations for pHPT seems to be increasing. Thus, in Sweden with a population of about 9 million at present, approximately 900 patients undergo parathyroidectomy on a yearly basis.
Scandinavian Quality Register for Thyroid and Parathyroid Surgery is an on-line database with the aim to improve the quality of diagnostics, surgical treatment, and follow-up for patients with surgical disease in the thyroid and parathyroid glands. The register also supports clinical research. We now report the first preliminary results from the audit of parathyroid surgery.
Materials and methods
Database
Scandinavian Quality Register for Thyroid and Parathyroid Surgery (http://www.thyroid-parathyroidsurgery.com) was launched 2004 as part of a regional, EU funded, healthcare cooperation project between Lund University Hospital and the University Hospital of Copenhagen, Rigshospitalet.
During the years, acceptance was gained from several professional organizations, most notably the Swedish and Danish Associations of Endocrine Surgeons as well as the Swedish Association of Otorhinolaryngeology, Head and Neck Surgery. The database is recognized by the Swedish National Board for Health and Social Welfare, as the national registry within the field. However, the register is open to participation by all departments within Scandinavia that carry out surgical treatment in this field. The register operates within the medico-legal framework of respective country. Thus, participating departments are responsible for compliance with national legislation regulating register participation, including information and acceptance of patients where applicable.
Patients
The register is an on-line database and the present report is based on 806 consecutively registered operations by 15 participating departments up to April 3, 2006. Follow-up was performed 1–6 weeks after surgery and is scheduled for 6–12 months postoperatively.
Registered variables
Preoperatively
Department, surgeon (consultant vs assisted), gender, age, symptoms (yes/no), serum calcium level, previous thyroid operation, type of operation (primary vs reoperation), localization procedure (performed vs not performed and type of procedure), hereditary, or sporadic disease.
Peroperatively
Date of operation, type of exploration (bilateral neck exploration, unilateral neck exploration, focused operation), video assisted operation (yes/no), conversion rate by minimal-invasive surgery, type of anesthesia, number of identified and excised parathyroid glands, autotransplantation of parathyroid glands (yes/no), other operations performed, identification of recurrent laryngeal nerves and noted nerve damage (yes/no), and intraoperative parathyroid hormone (PTH) (yes/no and result).
A focused approach is defined as parathyroidectomy performed by minimal incision (<25 mm) with excision of a solitary parathyroid tumor, but without dissection for the identification of an ipsilateral parathyroid gland; a unilateral approach is an operation performed with an incision >25 mm with unilateral dissection for the excision of a solitary parathyroid tumor and the identification or excision of a normal ipsilateral parathyroid gland; a limited operation is parathyroidectomy performed either as a focused or a unilateral approach. Video assisted operation is defined as an endoscopically performed or assisted parathyroidectomy. For the purpose of the database, a consultant surgeon is defined as neck surgeon with specialist diploma in general surgery or ENT
Postoperatively
Complications, results of laryngoscopy and voice recording, histology and gland weight, and calcium status at first follow-up [<6 weeks postoperatively; strictly normocalcemic, calcium below the reference range without treatment, i.e., regarded as asymptomatic, hypocalcemia, and in treatment with calcium and/or vitamin D analogue therapy, spontaneous hypercalcemia and reoperated for pHPT (yes/no)]. Furthermore, the actual serum calcium level at this follow-up was recorded.
Results of localization procedures
The results of localization procedures were compared to the results of neck exploration, definitive histology, and postoperative calcium status at the first follow-up after discharge and graded as follows: true preoperative localization of solitary adenoma (TP), false preoperative localization of solitary adenoma (FP), correct position of one pathologic gland, but multiglandular disease not predicted, false prediction of multiglandular disease in solitary adenoma, correct prediction of multiglandular disease, and lastly, negative/inconclusive preoperative examination. For the results of venous sampling, a modified report was used: true lateralization of solitary adenoma (TP), false lateralization of solitary parathyroid adenoma (FP), one gradient correct-bilateral multiglandular disease not predicted, multiglandular disease correctly predicted by bilateral gradients, and multiglandular disease falsely predicted in solitary parathyroid adenoma.
Sestamibi scintigraphy
For the departments that used sestamibi scintigraphy as a preoperative localization modality, the type of investigation (wash-out or subtraction scintigraphy) was reported, as well as the dosage of sestamibi technetium (MBq) and the use of single photon emission computed tomography (SPECT).
Intraoperative PTH
For departments that used intraoperative PTH (iOPTH), the cut-of limit for the decrease of PTH levels to predict successful operation was reported. The results from iOPTH were graded as follows: correct iOPTH (TP), incorrect iOPTH/persistent pHPT in spite of “adequate” decline in PTH levels (FP), and misleading/insufficient decline in iOPTH in spite of adequate operation (FN).
Statistics
For continuous variables, the results are reported as median and range if not stated otherwise. For nominal variables, numbers and percentage are given. For statistical evaluation of differences between groups, the Mann–Whitney U test or Kruskal–Wallis test (for analysis of differences between three groups or more) was used. For categorical data, statistical significance was analyzed by the chi-squared test and by the Fischer’s exact test when expected frequencies were less than 5. Stepwise logistic regression analyses was used to assess the additional variance by including in the full model, in addition to age and sex, variables that had initial shown an univariate association with a p-value of less than 0.20 with the dependent variable.
Results
Preoperative variables
There were 806 operations registered—167 of the patients were males (20.3%) and 639 (79.7%) were females. The median age of the patients was 62 years (range 17–94 years). The median preoperative serum calcium level was 2.85 mmol/l and 593 (75.6%) of the patients were regarded as symptomatic. Thirty-seven of the patients had known hereditary disease (4.6%). The surgical intervention was performed as reoperation in 50 patients (6.2%), and 39 patients (4.8%) had undergone previous thyroid surgery. Preoperative localization procedures were used in 524 patients (65%), 165 patients (19.4%) were planned for focused parathyroid surgery, and 136 (16.9%) for unilateral neck exploration.
Surgical exploration and histology
At surgery, a focused operation was performed in 138 patients (17.1%), unilateral neck exploration in 130 patients (16.1%), and bilateral neck exploration in 538 patients (66.8%). Furthermore, in a total of 25.2% of the operations, more than one parathyroid gland was excised. The surgical procedure was performed under local anesthesia only in 5 patients (0.6%).
Twenty-seven of 165 patients with planned focused operation were converted (unilateral exploration 6 patients and bilateral exploration 21 patients) for a total conversion rate of 16.4%.
Twelve of 136 patients with planned unilateral neck exploration were converted to bilateral neck surgery, with a conversion rate of 8.8%. Thus, of the 301 patients planned for limited parathyroid exploration, conversion to bilateral neck surgery occurred in 11%. Video-assisted operation was performed in 30 patients (3.7%), and in 18/138 (13%) of the patients operated with a focused approach.
Concomitant thyroid operation was performed in 85 patients (10.5%); 66 of 538 patients with bilateral exploration (12.3%), 18/130 patients with unilateral neck exploration (13.8%), and only 1/138 patients with focused operation (0.7%). Thymus operation was registered in 79 patients (9.8%) and autotransplantation of a parathyroid gland(s) in 11 patients (1.4%). Only 1 patient (0.1%) was operated with sternotomy.
Complication to surgery included rebleeding with operation in five patients (0.7%), wound infection treated with drainage and/or antibiotics in eight patients (1.2%), and unilateral paresis of the recurrent laryngeal nerve was reported in 11 patients (1.4%). Voice recording was performed postoperatively in 95 patients, and showed sign of paresis of the superior laryngeal nerve in one patient (1.1%).
Histology from the operation showed solitary parathyroid adenoma in 680 patients (84.4%), multiglandular disease in 93 patients (11.5%), parathyroid cancer in two patients (0.2%), and in 31 patients (3.9%), the exploration was negative.
The median excised gland weight was 0.61 g (range 0.05–42.0 g) for all patients, and for patients with the diagnosis of solitary parathyroid adenoma, the median weight was 0.61 g; 25% quartile 0.33 g; and 75% quartile 1.06 g.
Results from localization procedures
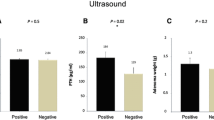
The results from the preoperative localization procedures performed compared to intraoperative findings and histology, are shown in Table 1. In general, the sensitivity to correctly localize a solitary parathyroid adenoma (TP) was modest; for sestamibi scintigraphy 64.4% and for ultrasound 61.1%, with a false positive (FP) rate of 7.7% and 7.2%, respectively. Multiglandular disease was never correctly predicted by sestamibi scintigraphy and only in three patients with ultrasonography.
For the 266 patients with TP localization of a solitary parathyroid adenoma with sestamibi scintigraphy, limited parathyroid exploration was performed in 185 patients (69.5%), focused operation in 109 patients (41%), and unilateral exploration in 76 patients (28.5%).
For the 179 patients with TP localization of parathyroid adenoma with ultrasonography, limited exploration was performed in 107 patients (59.8%), focused operation in 46 patients (25.7%), and unilateral exploration in 61 patients (34.1%).
The patients with a histological diagnosis of a solitary parathyroid tumor and a correct sestamibi scintigraphy, did not differ in gender (p = 0.594), age (p = 0.417), or preoperative serum calcium value (p = 0.990). There was also no difference between patients with and without previous thyroid operation (p = 0.337). In patients undergoing reoperation for pHPT, the sensitivity to correctly localize a solitary parathyroid tumor was somewhat higher than for patients undergoing primary operation (88.8 vs 75.9%), but failed to meet the level of significance (p = 0.126). Furthermore, there was no difference between investigations done with the washout technique vs subtraction scintigraphy (p = 0.536) and with and without SPECT (p = 0.144).
However, patients with a negative scintigraphy had smaller adenomas (mean weight 0.51 ± 0.39 g) than patients with positive scintigraphy (mean weight 1.31 ± 3.1 g) (p < 0.0001). Furthermore, patients with higher dose of administered technetium sestamibi (500 MBq; 68.3% TP vs 700 MBq; 84.8% TP vs 1,000 MBq; 85.7% TP) had a higher sensitivity (p = 0.0015). Variables with a value of p < 0.2 as well as age and gender were included in a stepwise logistic regression analyses. The results showed, that gland weight was the only variable independently associated with a correct preoperative localization by sestamibi scintigraphy (p = 0.0010).
Results of iOPTH
The cut-of limit to define a successful excision of a solitary adenoma was in all cases a decrease of PTH by 50% from baseline value at 10 min after gland excision. In addition, two departments also used a threshold value of 60% at 15 min.
IOPTH was used in 187/806 patients (23.2%). The result compared to intraoperative findings and postoperative calcium levels was correct in 180/187 patients (96.3%), and FN result, leading to unnecessary bilateral exploration, occurred in seven patients (3.7%). FP results were not reported.
Results from first postoperative follow-up
The first planned follow-up after discharge was performed <6 weeks after operation. No data was available in 41 patients (5.1%). Of the remaining 765 patients, 55 patients presented with hypercalcemia at the first follow-up and 15 patients (2%) were reoperated within 6 weeks after surgery and seven of these patients were cured. Thus, the initial cure rate among the 765 patients that could be followed (including patients undergoing reoperation and with hereditary disease) was 91.9%. In the univariate analysis of cure rate, patients undergoing reoperation had a lower cure rate (76.6%) than for first time surgery (92.9%) (p < 0.0001). Furthermore, the identification of four parathyroid glands or more had higher cure rate (97.4%; p = 0.0262). The use of preoperative localization procedures, iOPTH, and type of neck exploration did not influence the reported cure rate, nor did gender, hereditary disease, previous thyroid operation, age, or preoperative serum calcium levels.
Reported number of identified parathyroid glands and reoperation as well as gender and age in a logistic regression analysis showed that only reoperation was independently associated with a lower cure rate (p = 0.0024).
Calcium status as presented at the scheduled follow-up, is shown in Table 2. As can be shown, almost 10% of the patients were treated with oral calcium and/or Vitamin D at the first follow-up.
The risk for postoperative low calcium level and/or substitution with calcium and/or Vitamin D was analyzed. Thereby, the following variables were associated with hypocalcemia: assisted surgeon (lower risk; p = 0.0184), sporadic disease (lower risk; p < 0.0001), reoperation (higher risk; p = 0.0073), the use of preoperative localization examination (lower risk; p = 0.0023), the use of iOPTH (lower risk; p = 0.0263), type of neck exploration (lower for limited exploration; p = 0.0193), autotransplantation of parathyroid gland(s) (higher risk; p = 0.0003), number of identified parathyroid glands (higher risk; p = 0.0143), thymus operation (higher risk; p = 0.0051), concomitant thyroid operation (higher risk; p < 0.0001), postoperative local infection (higher risk; p = 0.0003), rebleeding with operation (higher risk; p = 0.0220). Furthermore, preoperative low serum calcium level (p = 0.1007), the number of excised parathyroid glands (p = 0.0537) as well as excised gland weight (p = 0.0554), reached borderline significance. These variables, as well as gender and age in a stepwise logistic regression analysis, showed that concomitant thyroid operation (p = 0.0496), reoperation (p = 0.0237), and the weight of excised pathological tissue (p = 0.0427), were independently associated with increased rate of hypocalcemia.
Discussion
In the era of evidence-based medicine and with the growing economic pressure on the healthcare systems, it is of utmost importance to monitor the efficacy of new methods and strategies being introduced for disease treatment. Ideally, knowledge should come from the collection of well-designed randomized trials. However, differences can often be expected to be small. The more successful a standard treatment is, the more difficult it is to prove that a particular new strategy is superior. This is certainly true in the surgical treatment of pHPT, where only marginal effects of new techniques can be expected.
Collecting large number of patients, from several different types of centers by the means of audit for the quality assurance within a particular field is one answer to this problem. The present report is the first preliminary analysis of data from the Scandinavian Quality Register for Thyroid and Parathyroid Surgery encompassing surgery for pHPT.
For the patients registered, the cure rate was lower, and the rate of hypocalcemia was higher than expected. Furthermore, the results provide evidence for several problems within modern pHPT surgery:
-
1.
Moderate sensitivity of all employed localization procedures with essentially no predictability for multiglandular disease.
-
2.
Limited neck exploration, even in patients with TP localization of a solitary parathyroid adenoma is performed in only 60–70% of the patients.
-
3.
The conversion rate for patients planned for focused parathyroid surgery to bilateral neck exploration is in excess of 10%.
Of the issues identified, one of the key problems is without doubt the astonishing low sensitivity to correctly localize a solitary parathyroid adenoma, especially surprising for sestamibi scintigraphy in the light of previously published studies with reported sensitivity around 85–90% [4, 10–13]. However, a recent metaanalysis did note wide differences in reported sensitivity [14]. The reason for these differences is not clear. Technical aspects might play a role. However, in the present investigation, neither the type of sestamibi scintigraphy (washout vs subtraction), SPECT, or the dose given (MBq), was independently associated with the sensitivity of the investigation. Instead, gland weight was the only predictor of a correct localization of a single parathyroid tumor. Other biological factors might contribute, such as PTH levels [15–17] and thyroid disease. However, confounding factors are also possible, and of those referral and publication bias are probably most important, i.e., patients with a positive sestamibi scintigraphy are more likely to be referred for surgery and, furthermore, “positive” results are more likely to get published than “negative” results. Regardless of the reason, due to costs and the fact that many patients are “unnecessarily” exposed to an investigation with radioactive material, other modalities, alternatively, a more selective approach should be sought. Attention should also be drawn to surgeon performed ultrasound [18, 19], as a cheap and comparatively sensitive investigation. Furthermore, the results underscore the critical role of iOPTH during minimal invasive surgery [20, 21].
A targeted operation with small incision, probably improves cosmesis and might facilitate short stay surgery. Furthermore, randomized trials have shown that operation under local anesthesia reduces operating time [22] and unilateral exploration reduces early symptomatic hypocalcemia [23]. However, in these investigations, as in the present study, no difference in hypocalcemia was seen after 4–6 weeks. Therefore, if cost is an issue, the discrepancy between the number of localization procedures and the number of patients undergoing limited parathyroid exploration as well as the conversion rate for planned minimal-invasive procedures, is in the negative balance for the new techniques. The reason for this result can, at present, only be speculated upon, but will be an important part of future analysis. For instance, it cannot be ruled out that the specific localization procedure was requested by the referring physician and depending on the preferred strategy, for instance bilateral neck exploration, the result was considered of little consequence for the surgeon. On the other hand, albeit with a short follow-up, there was no indication that a minimal invasive approach might reduce the change of cure by surgery.
There are some important limitation in the present investigation (thus the term “preliminary report”). For instance, about 5% of the patients could not be followed. These patients could change the overall cure rate somewhat, but probably not the general picture. Another important factor could be the differential diagnosis in the patients with persistent hypercalcemia, for example FHH.
Most importantly however, data were retrieved consecutively. Thus, because different departments joined the database at different time points, a direct comparison to evaluate the effect of center and volume, is, as yet, not possible. This analysis is not only important to evaluate “center effect”, but also to identify and analyse “benchmark” departments to increase the overall quality of parathyroid surgery, and especially if embarking on the new minimal invasive techniques [24–26]. The latter is of interest considering the high conversion rate for minimal invasive surgery found in the present investigation. Furthermore, for meaningful comparisons between centers, it is of utmost importance to perform an objective validation of data, both with regard to missing data and data correctness. Such validation will be performed by an open audit of participating departments.
Conclusion
Presently used localization procedures have moderate sensitivity and only a minority of patients is operated with limited parathyroid exploration. The audit furthermore shows that the overall cure rate is lower than reported in literature and the rate of hypocalcemia somewhat higher. General complications are, however, rare.
References
Lundgren E, Hagstrom EG, Lundin J, Winnerback K, Roos J, Ljunghall S, Rastad J (2002) Primary hyperparathyroidism revisited in menopausal women with serum calcium in the upper normal range at population-based screening 8 years ago. World J Surg 26:931–936
Hedback GM, Oden AS (2002) Cardiovascular disease, hypertension and renal function in primary hyperparathyroidism. J Intern Med 251:476–483
van Heerden JA, Grant CS (1991) Surgical treatment of primary hyperparathyroidism: an institutional perspective. World J Surg 15:688–692
Bergenfelz A, Tennvall J, Valdermarsson S, Lindblom P, Tibblin S (1997) Sestamibi versus thallium subtraction scintigraphy in parathyroid localization: a prospective comparative study in patients with predominantly mild primary hyperparathyroidism. Surgery 121:601–605
Bergenfelz A, Norden NE, Ahren B (1991) Intraoperative fall in plasma levels of intact parathyroid hormone after removal of one enlarged parathyroid gland in hyperparathyroid patients. Eur J Surg 157:109–112
Westerdahl J, Lindblom P, Bergenfelz A (2002) Measurement of intraoperative parathyroid hormone predicts long-term operative success. Arch Surg 137:186–190
Irvin GL 3rd, Prudhomme DL, Deriso GT, Sfakianakis G, Chandarlapaty SK (1994) A new approach to parathyroidectomy. Ann Surg 219:574–579 (Discussion 579–581)
Irvin GL 3rd, Deriso GT 3rd (1994) A new, practical intraoperative parathyroid hormone assay. Am J Surg 168:466–468
Sackett WR, Barraclough B, Reeve TS, Delbridge LW (2002) Worldwide trends in the surgical treatment of primary hyperparathyroidism in the era of minimally invasive parathyroidectomy. Arch Surg 137:1055–1059
Mazzeo S, Caramella D, Lencioni R, Molea N, De Liperi A, Marcocci C, Miccoli P, Iacconi P, Bossio GB, Viacava P, Lazzeri E, Bartolozzi C (1996) Comparison among sonography, double-tracer subtraction scintigraphy, and double-phase scintigraphy in the detection of parathyroid lesions. AJR Am J Roentgenol 166:1465–1470
Haber RS, Kim CK, Inabnet WB (2002) Ultrasonography for preoperative localization of enlarged parathyroid glands in primary hyperparathyroidism: comparison with (99m) technetium sestamibi scintigraphy. Clin Endocrinol (Oxf) 57:241–249
Clark PB, Case D, Watson NE Jr, Perrier ND, Morton KA (2003) Enhanced scintigraphic protocol required for optimal preoperative localization before targeted minimally invasive parathyroidectomy. Clin Nucl Med 28:955–960
Pattou F, Huglo D, Proye C (1998) Radionuclide scanning in parathyroid diseases. Br J Surg 85:1605–1616
Gotthardt M, Lohmann B, Behr TM, Bauhofer A, Franzius C, Schipper ML, Wagner M, Hoffken H, Sitter H, Rothmund M, Joseph K, Nies C (2004) Clinical value of parathyroid scintigraphy with technetium-99m methoxyisobutylisonitrile: discrepancies in clinical data and a systematic metaanalysis of the literature. World J Surg 28:100–107
Parikshak M, Castillo ED, Conrad MF, Talpos GB (2003) Impact of hypercalcemia and parathyroid hormone level on the sensitivity of preoperative sestamibi scanning for primary hyperparathyroidism. Am Surg 69:393–398 (Discussion 399)
Westerdahl J, Bergenfelz A (2004) Sestamibi scan-directed parathyroid surgery: potentially high failure rate without measurement of intraoperative parathyroid hormone. World J Surg 28:1132–1138
Biertho LD, Kim C, Wu HS, Unger P, Inabnet WB (2004) Relationship between sestamibi uptake, parathyroid hormone assay, and nuclear morphology in primary hyperparathyroidism. J Am Coll Surg 199:229–233
Solorzano CC, Carneiro-Pla DM, Irvin GL 3rd (2006) Surgeon-performed ultrasonography as the initial and only localizing study in sporadic primary hyperparathyroidism. J Am Coll Surg 202:18–24
Solorzano CC, Lee TM, Ramirez MC, Carneiro DM, Irvin GL (2005) Surgeon-performed ultrasound improves localization of abnormal parathyroid glands. Am Surg 71:557–562 (Discussion 562–553)
Chen H, Mack E, Starling JR (2005) A comprehensive evaluation of perioperative adjuncts during minimally invasive parathyroidectomy: which is most reliable? Ann Surg 242:375–380 (Discussion 380–373)
Chen H, Pruhs Z, Starling JR, Mack E (2005) Intraoperative parathyroid hormone testing improves cure rates in patients undergoing minimally invasive parathyroidectomy. Surgery 138:583–587 (Discussion 587–590)
Bergenfelz A, Kanngiesser V, Zielke A, Nies C, Rothmund M (2005) Conventional bilateral cervical exploration versus open minimally invasive parathyroidectomy under local anaesthesia for primary hyperparathyroidism. Br J Surg 92:190–197
Bergenfelz A, Lindblom P, Tibblin S, Westerdahl J (2002) Unilateral versus bilateral neck exploration for primary hyperparathyroidism: a prospective randomized controlled trial. Ann Surg 236:543–551
Henry JF, Sebag F, Tamagnini P, Forman C, Silaghi H (2004) Endoscopic parathyroid surgery: results of 365 consecutive procedures. World J Surg 28:1219–1223
Miccoli P, Berti P, Materazzi G, Massi M, Picone A, Minuto MN (2004) Results of video-assisted parathyroidectomy: single institution’s six-year experience. World J Surg 28:1216–1218
Udelsman R (2002) Six hundred fifty-six consecutive explorations for primary hyperparathyroidism. Ann Surg 235:665–670 (Discussion 670–662)
Acknowledgements
The present investigation was supported by grants from: European Union (Interreg. IIIA) and Swedish National Board for Health and Social Welfare. The following departments are currently participating in the Scandinavian Quality Register for Thyroid and Parathyroid Surgery: Department of Breast and Endocrine Surgery, Copenhagen University Hospital Rigshospitalet; Department of Surgery, Central Hospital, Kristianstad; Organkirurgisk Afdelning, Horsens Sygehus; Department of Surgery, Helsingborg Hospital; Department of Surgery, University Hospital of Uppsala; Center for Metabolism and Endocrinology, Karolinska University Hospital-Huddinge; Department of Surgery, Central Hospital, Halmstad; Department of Surgery, Falu Hospital; Department of Surgery, Ljungby Hospital; Department of Surgery, Växjö Central; Hospital Department of Surgery, Södersjukhuset; Department of Surgery, Västerås Central Hospital; Department of Surgery,Vendsyssel Hospital; Department of Otorhinolaryngeology, Lund University Hospital; Department of Surgery, Karolinska University Hospital; Department of Surgery, Sunderby Hospital; Department of Surgery and Transplantation, Sahlgrenska University Hospital; Department of Surgery, Kalmar Central Hospital; Department of Surgery, Randers Central Hospital; Department of Surgery, Nyköping Hospital; Department of Surgery, University Hospital of Umeå; Deparment of Surgery A,Odense University Hospital; Department of Surgery, Norra Älvsborgs Länssjukhus; and Department of Surgery, Lund University Hospital.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bergenfelz, A., Jansson, S., Mårtensson, H. et al. Scandinavian quality register for thyroid and parathyroid surgery: audit of surgery for primary hyperparathyroidism. Langenbecks Arch Surg 392, 445–451 (2007). https://doi.org/10.1007/s00423-006-0097-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-006-0097-6