Abstract
Background
Muscles are the primary contributors to joint loading. Loading is typically associated with the onset and progression of joint degeneration, and in turn, joint degeneration is known to affect negatively the control of muscle forces and co-ordination patterns. Nevertheless, the role of muscles in joint adaptation and degeneration has been largely ignored. Here, we review some of our research on the in vivo changes in muscular forces and joint loading in animal models of osteoarthritis and in patients with joint injury and disease. We attempt to emphasize the close dependence of muscle forces, joint loading and degeneration and, vice versa, try to point out how joint degeneration affects muscle forces and joint loading.
Material and methods
We measured the forces and electromyographic signals in normal and anterior cruciate ligament transected feline knees and measured (1) a consistent decrease in the knee extensor and ankle extensor muscle forces for weeks following intervention; (2) a corresponding decrease in the static and dynamic external ground reaction forces; and (3) a change in the electromyographic signals (in terms of the firing patterns of individual muscles and of the co-ordination of extensors and flexors during locomotion). We introduced results on the biosynthetic response of articular cartilage to controlled, in vivo, loading and discuss preliminary results from an experimental animal model of muscle weakness. In contrast to much of the published literature, loading, in our case, is introduced by controlled nerve stimulation and the corresponding muscular forces that load the joint in its in vivo configuration.
Results
We found that short-term loading (30–60 min) in the cat knee produces distinct up-regulation of mRNA of specific metalloproteinases (MMPs) and some of the MMP inhibitors. In our newly developed muscle-weakness model, we confirmed that controlled Botox injections in the rabbit knee extensor muscles cause a 60–80% decrease in muscle force, and that these changes in muscle force are associated with changes in the external ground reaction forces, and most importantly, that muscle weakness seems to be associated with degeneration of the knee in the absence of joint instability or any other intervention.
Conclusion
From the results of our research, we conclude that muscle health and muscle rehabilitation are key components for the successful prevention of, and recovery from, joint injury and disease.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
It is generally accepted that musculoskeletal tissues adapt to mechanical loading [1]. Such adaptations have been well described for bone [2, 3, 4, 5] and skeletal muscle [6, 7, 8, 9, 10]. However, the exact role of muscles in the mechanical loading of joints and the adaptive or degenerative changes in joints caused by muscular loading, remain unknown.
Joint degeneration, such as osteoarthritis, is associated with changes in the mechanical environment [11, 12, 13, 14]. For example, disruption of the normal joint mechanics through surgical removal of the anterior cruciate ligament, meniscectomy, or resection of the tibial plateau in experimental models of joint injury, have been shown to cause degenerative changes in the knee [15, 16, 17]. Similarly, excessive loading on the patellofemoral joint has been related to the onset of chondromalacia patellae and subsequent osteoarthritis [18, 19, 20, 21]. In addition, sports injuries that result in changes of the alignment of articular surfaces, such as ligament rupture, meniscal tearing, or injury of the joint capsule or articular cartilage, have been associated with an increased risk for the development of osteoarthritis [22, 23].
Despite all this experimental evidence, the relationship between joint loading and the corresponding degenerative processes remain largely unknown. There are several reasons for this state of affairs. First, it is difficult to obtain good data on the in vivo loading of joints during normal, everyday movements. Second, even if the generalized in vivo loading were known, it still would be virtually impossible to determine the corresponding instantaneous stress–strain states of the tissues that make up joints. Finally, the relationship between tissues' stress–strain states and the corresponding adaptive or degenerative biological responses remain virtually unknown, except for selected experiments on isolated tissues (e.g. articular cartilage explants) exposed to non-physiological in vitro loading conditions [24, 25, 26]. The value of these in vitro tests for predicting adaptive tissue response in vivo remains unknown. Because of the difficulty of determining the in vivo joint loading, researchers and clinicians have resorted to a variety of indirect measures. Probably, the most often used indirect measure of joint loading for human (and animal) locomotion is the ground reaction forces obtained from commercially available force platforms. A somewhat more sophisticated, but still indirect, measure of joint loading is the calculation of the resultant joint forces and moments using (commercially available) inverse dynamics software (e.g. Andrews [27]). However, the ground reaction force and the resultant joint forces and moments are global measures of joint loading. They do not provide insight into specific local loading conditions, and they cannot be associated with a specific anatomical structure of the joint. However, joint degeneration appears to be highly site-specific and local. For example, Adams [11] demonstrated that changes in articular cartilage hypertrophy in the anterior cruciate ligament-transected dog knee were site-specific. Similarly, we observed in the anterior cruciate ligament-transected cat knee, that specific areas appeared (gross morphologically and histologically) to be perfectly normal (femoral groove), while other areas showed complete erosion of the articular cartilage (medial tibial plateau), combined with a shredding of the medial meniscus and osteophyte formations [28]. These results suggest that either some parts of the joint are loaded differently than others, and thus, one observes the differential adaptive/degenerative responses, or that areas of similar loading adapt/degenerate distinctly differently for, as yet, unknown reasons.
In order to fully understand the relationship between joint adaptation/degeneration and joint loading, one should know the following in the ideal case: (1) the instantaneous stress–strain state of all joint tissues for normal, everyday movement tasks; (2) the corresponding biosynthetic short-term and long-term responses of these tissues; and (3) the short-term and long-term adaptive responses of in vivo joint tissues to altered loading conditions. We emphasize here "short-term" and "long-term" adaptive responses, as it appears likely that the biosynthetic response mechanisms of biological tissues continuously change as a tissue adapts to new loading conditions. At present, this ideal case scenario appears virtually impossible. Below, we would like to give a few examples of how we have approached this problem in previous studies, and furthermore, would like to describe preliminary results of ongoing work, and suggest future experiments. However, before doing this, we would like to consider the difficulties of associating the roles played by muscles on joint degeneration and adaptation.
The primary role of muscles is to move joints, and, while doing so, they load the joint articular surfaces. It has been argued that loads exceeding a certain threshold may lead to degenerative responses. However, before accepting this paradigm one should consider the following: (1) ground reaction forces [12, 29, 30, 31, 32], and in vivo muscle forces [33] are greatly diminished in many experimental animal models of osteoarthritis for weeks and months, but degenerative responses may be seen very early in the process. Therefore, it appears that the onset of degenerative responses may be associated with reduced loading rather than excessive loading; (2) in humans, joint swelling, pain, and stiffness, as well as joint instability are often associated with great muscle inhibition (i.e. an inability to contract maximally the muscles crossing the affected joint). Muscle inhibition is known to cause atrophy and weakness [34] and lead to a reduction in the generalized joint loading. The question now arises: is it the joint loading or the loss of muscular control that causes the onset and progression of joint degeneration? It has been shown that muscle activation patterns (as evaluated by electromyographic recordings) are severely altered following transection of the anterior cruciate ligament in the cat [33], which is a bona-fide model of knee osteoarthritis. Similarly, reduction of sensory feedback, either through sensory ablation in the knee of rats [35] or selective dorsal root ganglionectomy in dogs [36], has been associated with an increased rate of progression of joint degeneration; (3) finally, there is ample clinical and anecdotal (but, unfortunately, little systematic) evidence that muscle weakness may promote joint degeneration [37, 38, 39]. Intuitively, one would expect muscle weakness generally to unload the joint and, therefore, produce reduced loading conditions compared with normal. But muscle weakness, like joint injury or disease, may result in a diminished capacity for muscular control and may lead to premature fatigue when normal, everyday tasks are performed, such as walking, climbing stairs and getting up from chairs, and, because of the fatigue, may cause loss of fine motor control. Also, it has been argued in the past by one of the authors that, maybe, joint degeneration leading to osteoarthritis in the elderly is not exclusively an age-dependent occurrence but an issue of the well-documented, age-related loss of force and muscle control. It is well accepted that there is a substantial, and continuous, decrease in strength past the age of about 52 years [40, 41, 42, 43] and that humans [44] and rats [45] show a loss of the number of functional motor units for a given muscle. Motor units are the smallest control units of voluntary activation, and a reduction in the number of motor units may cause the age-related loss of movement control and, possibly, may cause the dramatic increase in the occurrence of joint degenerative diseases in the elderly.
Muscles, loading and the injured or diseased joint
In order to establish the possible role of muscles in joint adaptation, injury and disease, one must first establish the normal force and activation patters of muscles during standardized movements and then compare these normal values with those obtained in animals or humans with joint injury and disease. Below, we discuss some of our experimental research on in vivo muscle force and activation recordings in an animal model of osteoarthritis, relate those muscle forces to the corresponding articular cartilage contact pressures and ground reaction forces and, finally, discuss aspects of muscle inhibition in humans with joint injury and disease. These discussions occur within a framework of related studies published in the scientific literature.
There is a limited number of studies on the in vivo loading of joints. Joint pressures in the human hip have been estimated by several research groups for a variety of movement conditions, using instrumented artificial joints [46, 47, 48, 49, 50, 51, 52]. These measurements have the limitation that they measure the contact mechanics of an artificial joint rather than the mechanics that might occur in the real human hip. Furthermore, after implementation of an artificial hip, the movements, muscle activation patterns, and the mechanics of moment production by the muscles are likely to be altered, thereby causing further changes in the joint mechanics, thus questioning the usefulness of results obtained under these experimental conditions.
We have focused our efforts on the direct, in vivo measurement of muscle forces in the normal [53, 54] and the anterior cruciate ligament-transected cat [33] and have determined the in situ and in vivo patellofemoral contact pressures in the same experimental model [55, 56, 57, 58, 59]. Muscular forces in the gastrocnemius and the knee extensors (patellar tendon) are reduced to approximately 30% of the normal values following transection of the anterior cruciate ligament (Fig. 1). However, and possibly even more importantly, the muscular forces are "jerky" rather than smooth following intervention. We speculate that these jerky muscle forces are related to problems in the controlling of muscular activation after transection of the anterior cruciate ligament. Electromyographic (EMG) evidence from the vastus lateralis (VL), a knee extensor, supports this idea. EMG records of VL reveal that the peak-to-peak magnitude is similar prior to and post-transection; however, the EMG before intervention was continuous during the stance phase of gait [touchdown (TD) to paw off (PO); Fig. 1], while it was discontinuous, consisting of distinctly separated bursts, following intervention. The activation bursts of VL may be the result of two conflicting neural signals: (1) an excitatory signal preventing collapse of the knee during the stance phase of gait, and (2) an inhibitory signal, probably caused by proprioceptive feedback pathways, which suppress VL activity powerfully [60, 61]. The results shown in Fig. 1 were obtained 7 days after transection of the anterior cruciate ligament. We now have EMG evidence that such abnormal activation patterns persist for approximately 1–3 months, but then become "normal" by 6 months after intervention (unpublished results). It should be noted here that the change in EMG patterns, as well as the dramatic reduction in force, appears to be exclusively associated with the loss of the anterior cruciate ligament, as sham-surgery did not produce a decrease in muscle force or a change in EMG signals [33].
Gastrocnemius (gastroc) and quadriceps (Quad) forces and semitendinosus (ST) and VL EMGs from a representative cat before (left) and 7 days after (right) anterior cruciate ligament transection (ACLT). Results are shown for four full step cycles of slow walking. TD and PO are indicated in both panels for one step cycle and they contain the stance phase of the target hind limb. Note the decrease in force from before to after ACLT and the obvious changes in the EMG patterns
In agreement with the reduction in muscle force following the transection, the patellofemoral contact forces are also reduced. However, patellofemoral contact forces decreased by only approximately 30% (i.e. approximately 70% of the normal force), whereas muscle forces decreased by about 70% (i.e. about 30% of the normal muscle forces) within 7 to 14 days after intervention (Fig. 2). The reason that the patellofemoral contact forces are not reduced by nearly as much as the corresponding knee extensor forces is associated with the altered gait kinematics. Following transection of the anterior cruciate ligament, the knee angle was reduced by approximately 15° throughout the stance phase, and specifically, knee extension observed in the normal animal just prior to paw off was missing in the experimental hind limbs [29].
Mean (thick line) and individual (thin lines) patellofemoral contact forces from a representative animal for full step cycles, before (intact) and after anterior cruciate ligament transection (ACL-deficient). The patellofemoral contact forces were normalized relative to the mean peak force before ACL transection. 0 on the horizontal axis represents the start of the swing phase. The stance began at approximately 40% (second vertical line) and 60% (third vertical line) and lasts to the right end side of the figure for the intact and ACL-deficient limb, respectively. Note, there is an approximate 30% decrease in the peak patellofemoral contact forces 7 days after ACL transection
Consistent with the decreased muscle forces, the static (standing on a force platform) vertical ground reaction forces were also reduced in the experimental hind limb in comparison with the contralateral hind limb (Fig. 3). It is interesting to note that the static vertical ground reaction forces are decreased the most between 6 to 8 weeks following the transection and not, as one might expect, immediately after. Static ground reaction forces return to normal after approximately 4–5 months. The peak vertical ground reaction forces during locomotion are reduced the most immediately following transection (Fig. 4). They then recover steadily over a 1-year period and approximate normal (contralateral) values after approximately 6 months.
Average relative loading of the anterior cruciate ligament (ACL) transected (closed symbols) and the contralateral hind limb (open symbols) during "quiet" standing of the animals (n=6). Means were calculated for periods of standing ranging from 5–30 s for each animal in each test and were expressed relative to the sum of the vertical ground reaction forces of both hind limbs. The number of independent observations at each time point ranged from 1 to 6
Vertical ground reaction forces as a percentage of body weight for the transected (open circles) and contralateral (closed circles) hind limbs before anterior cruciate ligament transection (ACLT) and at different time points post-ACLT. Asterisks and dagger indicate significant differences from pre-transection values of the corresponding leg. The values are means (± SD) for seven cats, with multiple steps for each cat
In order for the local and site-specific mechanics in a joint to be analyzed, it is crucial for one to identify the contact pressure distributions at the articular surfaces, as it is these contact pressures that will determine the stress–strain distribution in the articular cartilage and the corresponding adaptive or degenerative responses in the cartilage and subchondral bone. Intuitively one would expect a smaller patellofemoral contact force to be associated with a smaller contact pressure. However, when two articular joint surfaces are pressed together with increasing force, the contact area also increases [58]. An example of the relationship between patellofemoral contact force and contact area is shown in Fig. 5 for five cats. Therefore, average and peak pressures may not necessarily increase with increasing joint loading, but the increased load may be accommodated by an increased contact area. The relationship between the patellofemoral contact force and the mean contact pressure is shown in Fig. 6, with the corresponding regression line. From a statistical point of view, an increase in patellofemoral contact force was associated with a significant increase in mean contact pressure; however, a fivefold increase in force (from 100 to 500 N) merely caused a 65% increase in the mean contact pressure (from 7.8 to 12.9 MPa).
Patellofemoral contact area as a function of the patellofemoral contact force (applied force) in five cat knees. Note the rapid increase in the contact area for applied forces in the normal physiological range (approximately 0–250 N). It appears, therefore, that increases in patellofemoral contact forces might be primarily accommodated by an increase in the contact area, rather than an increase in the mean contact pressure
Average contact pressure in the patellofemoral joint (pressure) as a function of the patellofemoral contact force (applied force). Note that the slope of the regression line is very small (0.0128). An increase in the patellofemoral contact force by 100 N merely increases the corresponding average contact pressure by 1.28 MPa; therefore, the average pressure in the patellofemoral joint is virtually independent of the contact force (and thus, the muscular forces), as an increase in contact force is largely accommodated by an increase in the articular contact area
On calculating the decrease in mean contact pressure for the cat patellofemoral joint before and after transection of the anterior cruciate ligament, based on the regression equation shown in Fig. 6, Hasler and Herzog [56] found the following values in an exemplar animal:
-
Peak patellofemoral contact force before transection = 133 N
-
Peak patellofemoral contact force after transection = 89 N
The corresponding mean pressure would decrease from 8.2 MPa to 7.6 MPa (before and after transection, respectively). Therefore, for a decrease in the in vivo patellofemoral contact force of 33%, the corresponding mean pressure decreased by only 7%. This example illustrates the difficulty of extrapolating from ground reaction force or muscle force measurements to the local loading of the joint and its associated structures. Needless to say, the mean pressure is only one of many possibilities that quantify joint surface loading. The peak pressure behaves quite differently from the mean pressure with increasing contact force; it increases at a greater rate than the mean pressure shown here [58].
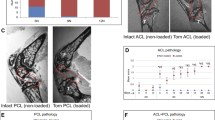
Another issue that must be considered briefly is the adaptive ability of an injured joint. For example, following transection of the anterior cruciate ligament, the stiffness of the cat knee (as determined by the force–anterior displacement or the force–internal angular displacement relationships) is dramatically reduced. However, this stiffness changes continuously in the recovery process, and is back to pre-intervention values at 4 months post-intervention (Fig. 7). Furthermore, and more importantly in the context of the present discussion, articular cartilage thickness increases in the cat knee, following transection, at all of six sites measured, and this increase over 16 weeks is most pronounced on the retro-patellar surface (102% increase) and the femoral groove (76%; n=4). Furthermore, this increase in thickness is accompanied by a decrease in stiffness of the articular cartilage surfaces [59]. These changes in articular cartilage mechanical properties can be shown theoretically to cause an increase in contact area and a decrease in peak pressure. Using articular cartilage thickness and stiffness data from experiments [59], we calculated, based on a biphasic, linear elastic, isotropic contact model, the change in contact area and pressure distribution in the "normal" and the anterior cruciate ligament-transected cat knee 16 weeks post-intervention (Fig. 8). We found that peak pressures were reduced by approximately 50% and contact radius was increased by approximately 34% in the transected joint compared with the normal joint. When we measured the peak contact pressures and contact areas in the experimental and contralateral patellofemoral joints of five cats at 16 weeks post-transection, peak pressure was decreased by 22% and contact area was increased by approximately 50% (Fig. 9) for a given patellofemoral contact force [59]. This result demonstrates that the internal, site-specific loading of a joint changes as a function of the internal geometry (not shown), bone alignment (not shown), and articular cartilage thickness and functional mechanical properties (Figs. 8, 9), even if the muscular forces and the resultant joint contact force are identical. These examples emphasize the difficulty one has in directly relating muscular forces to the site-specific loading of a joint.
Anterior–posterior stiffness of cat tibial displacement relative to the femur, before (pre), immediately after (post) and at 2 and 4 months after anterior cruciate ligament transection (n=4) for knee flexion at angles of 30° and 90°. Note that the anterior stiffness of the cat knee decreases dramatically after anterior cruciate ligament transection, but that this stiffness is back to normal at 4 months post-intervention. Similar results were observed for internal rotation stiffness of the cat tibia relative to the femur (not shown)
Theoretical predictions of the contact radius (in an axi-symmetric contact problem) and peak pressure at different times of loading (t=0, 5, and 10 s) using the exact input (cartilage thickness and material properties) obtained experimentally, and the approximate joint geometry (radius of curvature = 10 and 20 mm for the patella and patellar groove, respectively) in an analytical, biphasic model of the articular cartilage contact mechanics. Note the decreased peak pressure and increased contact radius (area) in the cartilage with the properties of the experimental knee 16 weeks after anterior cruciate ligament transection (diseased) compared with the intact contralateral control (normal)
Patellofemoral contact pressures measured with Fuji Presensor film in an intact knee and the contralateral anterior cruciate ligament transected knee at 16 weeks post-intervention. Increased pressures are represented by darker staining. Note the greater peak pressures in the intact joint and the greater contact area in the anterior cruciate ligament-transected joint (ACLT), as predicted theoretically (see Fig. 8). This result was consistent for five independent observations and for the whole range of loading conditions (not shown)
Before finishing this section on the injured and diseased joint, we would like to discuss briefly a phenomenon that is clinically important but cannot really be evaluated through animal experimentation. It is the issue of muscle inhibition. Muscle inhibition is defined here as the loss of maximal voluntary force caused by a pathological decrease in muscle activation, as assessed by the so-called superimposed twitch technique (for details of this technique please see Merton [62] or Belanger and McComas [63]). There is a great body of evidence that muscle inhibition, for example of the knee extensors, is a common adjunct of acute and chronic knee injuries. For example, patients with unilateral anterior knee pain, anterior cruciate ligament deficiency and reconstruction show muscle inhibition for months and years following first occurrence of the knee pathology [34, 64]. However, when compared with a healthy reference group, patients showed significant muscle inhibition not only in the affected leg but also in the apparently normal contralateral leg (Fig. 10). Hurley et al. [34] concluded that severe initial muscle inhibition interferes with the rehabilitation process and compromises the functional recovery of patients. Several questions arise form these clinical studies: why do knee patients often retain great muscle inhibition and strength deficits years after the initial injury? Is it possible that muscle atrophy is promoted by muscle inhibition, despite rehabilitation procedures involving strengthening exercises? And, what is (are) the mechanism(s) causing muscle inhibition in patients with joint instability, effusion and pain, and how can muscle inhibition be reduced and eliminated in patients? Clinicians and clinical scientists will need to address these questions rigorously in the future, as we believe that muscle inhibition and the associated loss of muscle mass and strength, as well as the loss of precise muscle control, may play an important role in the development of joint degeneration.
Muscle inhibition of the knee extensors in unilateral knee patients (n=88) with anterior knee pain (AP), anterior cruciate ligament deficiency (ACL-D), and anterior cruciate ligament reconstruction (ACL-R). The average muscle inhibition in the knee extensors for healthy people (no knee injuries) is 9.7% (horizontal line). Note that all patient groups have significantly elevated muscle inhibition in the affected leg (as expected) and in the "normal" unaffected contralateral leg (unexpected); therefore, in a clinical test in which the left-to-right differences are assessed, muscle inhibition would be greatly underestimated
Muscles, loading and the healthy joint
So far, we have dealt primarily with injured or diseased joints, and muscle strength, mechanical loading, or muscle coordination patterns were compared with normal, healthy joints (often the contralateral control). However, one of the puzzling questions is: how is joint degeneration initiated? What are the stimuli that predispose a joint to become osteoarthritic? It is likely that these questions do not have a unique answer. It is likely that the onset of joint degeneration leading to osteoarthritis requires a whole set of conditions to be in place, rather than just a single condition that triggers the events leading to joint degeneration.
In the past few years we have initiated pilot projects aimed at addressing the question of how joint degeneration may be initiated. Two of these approaches are briefly described below, and pilot results (as these are largely unreported findings to date) are shown.
The first approach deals with the controlled, in vivo loading of joints and the immediate (or nearly immediate) assessment of soft tissue responses to different mechanical loading protocols, using primarily molecular biology approaches. This study was motivated by a great number of studies aimed at determining the biological responses of soft tissues, loaded in vitro, under non-physiological mechanical loading conditions. For example, articular cartilage explants have been loaded in a variety of ways (static, dynamic, confined, and unconfined compression, hydrostatic loading, etc.), and molecular adaptive and degenerative responses have been reported (e.g. [24, 25, 26]). The general limitation of all these studies is that the artificial loading conditions, as produced, for example, by confined compression testing, may cause biosynthetic responses that might not be meaningful when compared with those that would be obtained if normal, in vivo joint loading were used.
In our approach the knee of NZ white rabbits is loaded by electrical (controlled) stimulation of the knee extensor muscles. The knee is either fixed (isometric contractions, Fig. 11) or moved through a specific range of motion by a motor. Contraction and muscle force can be timed, relative to the knee movement, by a computer. Force feedback is obtained though a load cell attached to the motor (Fig. 12). Preliminary results indicate that loading produces distinct biological responses that are site specific. For example, 2 s of quadriceps stimulation once every 30 s for 1 h showed a distinct and statistically significant increase in mRNA levels of metalloproteinase-3 (MMP-3) when compared with unloaded controls and unloaded contralateral knee articular cartilage (Fig. 13). Furthermore, the MMP-3 response was significantly greater in articular cartilage harvested from the loaded area of the femoral groove than that obtained from the loaded articular cartilage harvested from the retro-patellar surface. This result suggests that the same load applied to two contacting articular surfaces (where the steady-state pressure distribution must be equal, according to Newton's law of action–reaction), may produce distinctly different biological responses. This suggestion is further supported by strong evidence of a site-specific, rather than a uniform, degeneration of joints in experimental models of osteoarthritis [11, 65].
Experimental set-up of knee loading through knee extensor stimulation in a NZ white rabbit. Upon stimulation of the muscles, the knee wants to extend but this is prevented by a restraining bar that measures the knee extensor force. By measuring the moment arms from the instrumented bar to the knee and from the quadriceps tendon to the knee, we can convert the force in the instrumented bar into a knee extensor moment and a knee extensor muscle force
Force, as measured by the instrumented force bar, as a function of time for a loading protocol involving 2-s knee extensor stimulation, once every 30 s for 1 h. The knee extensor force can be controlled by adjustment of the stimulation frequency and the voltage of femoral nerve stimulation. The feedback system allows for a controlled change in the knee extensor forces during the experiment (if desired)
mRNA levels of metalloproteinase-3 for articular cartilage loaded in vivo for 2 s twice per min for 1 h (experimental), and for unloaded control cartilage obtained from the contralateral joint (contralateral) and from unloaded control joints (control). Note the increase in mRNA levels for the experimental compared with the unloaded control surfaces at both sites (peripheral and central) in the patella and femur
The second approach we would like to discuss briefly deals with an experimental animal model of muscle weakness. Suter and Herzog [66] proposed that muscle weakness might be an independent risk factor for the development of osteoarthritis. Slemenda et al. [39] showed, in a prospective study involving more than 300 women, that knee extensor weakness (relative to body weight) was associated with the onset of knee osteoarthritis over a 30-month test period. Similarly, Slemenda et al. [38] found, in a cross-sectional investigation involving almost 500 volunteers (aged 65 and older), that knee extensor strength was a significant predictor of radiographic and symptomatic osteoarthritis of the knee. However, because of the experimental design in the latter study, it is not known whether the lack of knee extensor strength caused osteoarthritis or if subjects who had developed osteoarthritis subsequently became weaker than the non-symptomatic patients because of the muscle inhibition typically associated with osteoarthritis. Thus, a direct link between muscle weakness and joint degeneration cannot be made based on this and other studies published in the scientific literature.
Recently, we developed an animal model of muscle weakness. The knee extensors of NZ white rabbits were given a single injection of 3.5–5.0 units per kg of botulinum toxin (Botox). We confirmed that injection of Botox led to a repeatable and quantifiable reduction of muscle strength of 60–80% (i.e. 20–40% strength of the contralateral control muscles; Fig. 14). This reduction in muscle strength was associated with a change in the vertical ground reaction forces and a reduction in muscle mass of approximately 30% (Fig. 15). However, and most importantly, in those animals tested to date, the experimental knee showed a reddening and fibrillation of the articular cartilage on the lateral portion of the tibial plateau that was interpreted by three independent evaluators as a first sign of joint degeneration (Fig. 16). Needless to say, these preliminary data must be viewed with caution, but it is our belief that the in vivo assessment of joint adaptive and degenerative responses to controlled, in vivo loading produced through muscular stimulation is an essential and necessary stage in gaining insight into the clinical problems of onset and progression of joint degeneration. Furthermore, we believe that the precise control of muscle forces (or the loss of muscle control through injury, muscle inhibition, reduced afferent feedback, or aging) is a factor contributing to joint degeneration leading to osteoarthritis. Finally, our pilot data suggest that muscle weakness may be a risk factor for joint degeneration. Whether the risk is associated with the actual loss of force production, or with a change in muscular control to compensate for the loss of force, will need to be addressed systematically in future studies.
Peak knee extensor torques (Nm) as a function of knee angle for an exemplar animal (NZ white rabbit) stimulated via a femoral nerve cuff at 100 Hz for 0.5 s. This animal received a single Botox injection (3.5 units/kg), and testing was done 4 weeks following injection. Note the consistent decrease in knee extensor torque in the experimental knee compared with the contralateral knee
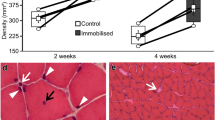
Knee extensor muscle masses of the exemplar rabbit shown in Fig. 14. One month following Botox injection (3.5 units/kg), the knee extensor muscles had atrophied by about 30% (in terms of mass) compared with the corresponding contralateral muscles
Top view of the tibial plateau harvested from an animal 4 weeks after a single Botox injection into the knee extensor muscles. There is a distinct reddening and fibrillation of the articular cartilage on the lateral tibial plateau (arrow) that was seen in three experimental animals tested to date but was not observed in the normal control animals
Conclusion
From the results of our studies we conclude that joint loading produced by muscle forces, the control of joint movements through co-ordinated muscular contraction, and joint integrity and stability, are essential factors influencing joint adaptive and degenerative responses.
References
Taber LA (1995) Biomechanics of growth, remodeling, and morphogenesis. Appl Mech Rev 48:487–545
Carter DR (1987) Mechanical loading history and skeletal biology. J Biomech 20:1095–1099
Cowin SC (1986) Wolff's law of trabecular architecture at remodeling equilibrium. J Biomech Eng 108:83–88
Goldstein SA, Matthews LS, Kuhn JL, Hollister SJ (1991) Trabecular bone remodeling: an experimental model. J Biomech 24[Suppl 1]:135–150
Huiskes R, Weinans H, Grootenboer HJ, Dalstra M, Fudala B, Sloof TJ (1987) Adaptive bone-remodeling theory applied to prosthetic-design analysis. J Biomech 20:1135–1150
Booth FW (1982) Effect of limb immobilization on skeletal muscle. J Appl Physiol 52:1113–1118
Goldberg AL, Etlinger JD, Goldspink DF, Jablecki C (1975) Mechanism of work-induced hypertrophy of skeletal muscle. Med Sci Sports Exerc 7:248–261
Simard CP, Spector SA, Edgerton VR (1982) Contractile properties of rat hind limb muscles immobilized at different lengths. Exp Neurol 77:467–482
Tabary JC, Tabary C, Tarieu C, Tarieu G, Goldspink G (1972) Physiological and structural changes in the cat's soleus muscle due to immobilization at different lengths by plaster casts. J Physiol 224:231–244
Vandenburgh HH (1982) Dynamic mechanical orientation of skeletal myofibers in vitro. Dev Biol 93:438–443
Adams ME (1989) Cartilage hypertrophy following canine anterior cruciate ligament transection differs among different areas of the joint. J Rheumatol 16:818–824
Brandt KD, Braunstein EM, Visco DM, O'Connor B, Heck D, Albrecht M (1991) Anterior (cranial) cruciate ligament transection in the dog: a bona fide model of osteoarthritis, not merely of cartilage injury and repair. J Rheumatol 18:436–446
Jurvelin J, Kiviranta F, Tammi M, Helminen HJ (1986) Softening of canine articular cartilage after immobilization of the knee joint. Clin Orthop 207:246–252
Setton LA, Mow VC, Muller FJ, Pita JC, Howell DS (1994) Mechanical properties of canine articular cartilage are significantly altered following transection of the anterior cruciate ligament. J Orthop Res 12:451–463
Pond MJ, Nuki G (1973) Experimentally-induced osteoarthritis in the dog. Ann Rheum Dis 32:387–388
McDevitt C, Gilbertson E, Muir H (1977) An experimental model of osteoarthritis; early morphological and biochemical changes. J Bone Joint Surg Br 59:24–35
Moskowitz RW, Howell DS, Goldberg VM (1979) Cartilage proteoglycan alterations in an experimentally induced model of rabbit osteoarthritis. Arthritis Rheum 22:155–163
Bandi W (1972) Chondromalacia patellae und femoro-patellare Arthrose. Aetiologie, Klinik, und Therapie. Helv Chir Acta Suppl 11:3–70
Insall J, Goldberg V, Salvati E (1972) Recurrent dislocation and the high-riding patella. Clin Orthop 88:67–69
Outerbridge RE, Dunlop JAY (1975) The problem of chondromalacia. Clin Orthop 110:177–196
Maquet PGJ (1979) Mechanics and osteoarthritis of the patellofemoral joint. Clin Orthop 144:70–73
Kettlekamp DB, Coyler RA (1984) Osteoarthritis of the knee. In: Moskowitz RW, Howell DS (eds) Osteoarthritis: diagnosis and management. Saunders, Philadelphia, pp 403–421
Mankin HJ, Brandt KD, Shulman LE (1986) Workshop on the pathogenesis of osteoarthritis: proceedings and recommendations. J Rheumatol 13:1127–1160
Wong M, Wuethrich P, Eggli P, Hunziker E (1996) Zone-specific cell biosynthetic activity in mature bovine articular cartilage: a new method using confocal microscopic stereology and quantitative autoradiography. J Orthop Res 14:424–432
Wong M, Wuethrich P, Buschmann MD, Eggli P, Hunziker E (1997) Chondrocyte biosynthesis correlates with local tissue strain in statically compressed adult articular cartilage. J Orthop Res 15:189–196
Quinn TM, Grodzinsky AJ, Hunziker EG, Sandy JD (1998) Effects of injurious compression on matrix turnover around individual cells in calf articular cartilage explants. J Orthop Res 16:490–499
Andrews JG (1974) Biomechanical analysis of human motion. Kinesiology 4:32–42
Clark A, Herzog W, Matyas JR, Barclay L, Leonard TR (2001) Proceedings of the 18th Congress of the International Society of Biomechanics, pp 162–163
Suter E, Herzog W, Leonard TR, Nguyen H. 1998. One-year changes in hindlimb kinematics, ground reaction forces and knee stability in an experimental model of osteoarthritis. J Biomech 31:511–517
Brandt KD, Myers SL, Burr D, Albrecht M (1991) Osteoarthritic changes in canine articular cartilage, subchondral bone, and synovium fifty-four months after transection of the anterior cruciate ligament. Arthritis Rheum 34:1560–1570
Vilensky JA, O'Connor BL, Brandt KD, Dunn EA, Rogers PI, DeLong CA (1994) Serial kinematic analysis of the unstable knee after transection of the anterior cruciate ligament: temporal and angular changes in a canine model of osteoarthritis. J Orthop Res 12:229–237
O'Connor BL, Visco DM, Heck D, Myers SL, Brandt KD (1989) Gait alterations in dogs after transection of the anterior cruciate ligament. Arthritis Rheum 32:1142–1147
Hasler EM, Herzog W, Leonard TR, Stano A, and Nguyen H (1998) In-vivo knee joint loading and kinematics before and after ACL transection in an animal model. J Biomech 31:253–262
Hurley MV, Jones DW, Newham DJ (1994) Arthrogenic quadriceps inhibition and rehabilitation of patients with extensive traumatic knee injuries. Clin Sci (Colch) 86:305–310
Salo PT, Seeratten RA, Erwin WM, Bray RC (2002) Evidence for a neuropathic contribution to the development of spontaneous knee osteoarthritis in a mouse model. Acta Orthop Scand 73:77–84
Visco DM, O'Connor BL, Heck D (1990) ORS meeting 1990, 36:559
Brandt KD (1997) Putting muscle into osteoarthritis. Ann Intern Med 127:154–155
Slemenda C, Brandt KD, Heilman DK, Mazzuca S, Braunstein EM, Katz BP, Wolinsky FD (1997) Quadriceps weakness and osteoarthritis of the knee. Ann Intern Med 127:97–104
Slemenda C, Heilman DK, Brandt KD, Katz BP, Mazzuca S, Braunstein EM, Byrd D (1998) Reduced quadriceps strength relative to body weight. A risk factor for knee osteoarthritis in women? Arthritis Rheum 41:1951–1959
Klitgaard H, Zhou M, Schiaffino S, Betto R, Salviati G, Saltin B (1990) Aging alters the myosin heavy chain composition of single fibres from human skeletal muscle. Acta Physiol Scand 140:55–62
Inokuchi S, Ishikawa H, Iwamoto S, Kimura T (1975) Age-related changes in the histological composition of the rectus abdominis muscle of the adult human. Hum Biol 47:231–249
Overend TJ, Cunningham DA, Paterson DH, Lefcoe MS (1992) Thigh composition in young and elderly men determined by computed tomography. Clin Physiol 12:629–640
Lexell J, Henriksson-Larsén K, Winblad B, Sjöström M (1983) Distribution of different fibre types in human skeletal muscles: effects of aging studied in whole muscle cross sections. Muscle Nerve 6:588–595
McComas AJ (1996) Skeletal muscle: form and function. Human Kinetics, Champaign, Illinois.
Campbell MJ, McComas AJ, Petito F (1973) Physiological changes in ageing muscles. J Neurol Neurosurg Psychiatry 36:174–182
Krebs DE, Elbaum L, Riley PO, Hodge WA, Mann RW (1991) Exercise and gait affects on in vivo hip contact pressures. Phys Ther 71:301–309
Strickland EM, Fares M, Krebs DE, Riley PO, Givens-Heiss DL, Hodge WA, Mann RW (1992) In vivo acetabular contact pressures during rehabilitation. I. Acute phase. Phys Ther 72:691–699
Givens-Heiss DL, Krebs DE, Riley PO, Strickland EM, Fares M, Hodge WA, Mann RW (1992) In vivo acetabular contact pressures during rehabilitation. II. Postacute phase. Phys Ther 72:700–705
Fagerson TL, Krebs DE, Harris BA, Mann RW (1995) Examining shibboleths of hip rehabilitation protocols using in vivo contact pressures from an instrumented hemiarthroplasty. Physiotherapy (London) 81:533–540
Park SS, Krebs DE, Mann RW (1999) Hip muscle co-contraction: evidence from concurrent in vivo pressure measurement and force estimation. Gait Posture 10:211–222
Kotzar GM, Davy DT, Goldberg VM, Heiple KG, Berilla J, Heiple G, Brown RH, Burstein AH (1991) Telemeterized in vivo hip joint force data: a report on two patients after total hip surgery. J Orthop Res 9:621–633
Bergmann G, Graichen F, Rohlmann A (1993) Hip joint loading during walking and running, measured in two patients. J Biomech 26:969–990
Herzog W, Leonard TR (1991) Validation of optimization models that estimate the forces exerted by synergistic muscles. J Biomech 24S:31–39
Herzog W, Leonard TR, Guimaraes ACS (1993) Forces in gastrocnemius, soleus, and plantaris tendons of the freely moving cat. J Biomech 26:945–953
Herzog W, Hasler EM, Maitland ME, Suter E, Leonard TR, Muller C (1998) In vivo mechanics and in situ stability of the anterior cruciate ligament-deficient knee. An animal model of osteoarthritis. Sportverletz Sportschaden 14.2:67–74
Hasler EM, Herzog W (1998) Quantification of in vivo patellofemoral contact forces before and after ACL transection. J Biomech 31:37–44
Herzog W, Hasler EM, Leonard TR (2000) Experimental determination of in vivo pressure distribution in biologic joints. J Musculoskeletal Res 4:1–7
Clark AL, Herzog W, Leonard TR (2002) Contact area distribution in the feline patellofemoral joint under physiologically meaningful loading conditions. J Biomech 35:53–60
Herzog W, Wu JZ, Leonard TR, Suter E, Diet S, Muller C, Mayzus P (1998) Mechanical and functional properties of cat knee articular cartilage 16 weeks post ACL transection. J Biomech 31:1137–1145
Krebs DE, Staples WH, Cuttita D, Zickel RE (1983) Knee joint angle: its relationship to quadriceps femoris activity in normal and postarthrotomy limbs. Arch Phys Med Rehabil 64:441–447
Suter E, Herzog W, Bray RC (1998) Quadriceps inhibition following arthroscopy in patients with anterior knee pain. Clin Biomech 13:314–319
Merton PA (1954) Voluntary strength and fatigue. J Physiol 123:553–564
Belanger AY, McComas AJ (1981) Extent of motor unit activation during effort. J Appl Physiol 51:1131–1135
Suter E, Herzog W, De Souza K, Bray R (1998) Inhibition of the quadriceps muscles in patients with anterior knee pain. J Appl Biomech 14:360–373
Clark A, Herzog W, Matyas JR, Barclay L, Leonard TR (2002) Proceedings of the IV World Congress of Biomechanics, Calgary, AB, Canada. CD ROM
Suter E, Herzog W (2000) Does muscle inhibition after knee injury increase the risk of osteoarthritis. Exerc Sport Sci Rev 28:15–18
Acknowledgements
The research described here has been continuously funded since 1992 by the Canadian Institutes of Health Research (formerly the Medical Research Council of Canada) and the Arthritis Society of Canada.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Herzog, W., Longino, D. & Clark, A. The role of muscles in joint adaptation and degeneration. Langenbecks Arch Surg 388, 305–315 (2003). https://doi.org/10.1007/s00423-003-0402-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-003-0402-6