Abstract
We undertook a comparative immunolocalisation study on type II collagen, aggrecan and perlecan in a number of 12- to 14-week-old human foetal and postnatal (7–19 months) ovine joints including finger, toe, knee, elbow, hip and shoulder. This demonstrated that perlecan followed a virtually identical immunolocalisation pattern to that of type II collagen in the foetal tissues, but a slightly divergent localisation pattern in adult tissues. Aggrecan was also localised in the cartilaginous joint tissues, which were clearly delineated by toluidine blue staining and the type II collagen immunolocalisations. It was also present in the capsular joint tissues and in ligaments and tendons in the joint, which stained poorly or not at all with toluidine blue. In higher power microscopic views, antibodies to perlecan also stained small blood vessels in the synovial lining tissues of the joint capsule; however, this was not discernable in low power macroscopic views where the immunolocalisation of perlecan to pericellular regions of cells within the cartilaginous rudiments was a predominant feature. Perlecan was also evident in small blood vessels in stromal connective tissues associated with the cartilage rudiments and with occasional nerves in the vicinity of the joint tissues. Perlecan was expressed by rounded cells in the enthesis attachment points of tendons to bone and in rounded cells in the inner third of the meniscus, which stained prominently with type II collagen and aggrecan identifying the chondrogenic background of these cells and local compressive loads. Flattened cells within the tendon and in the surface laminas of articular cartilages and the meniscus did not express perlecan. Collected evidence presented herein, therefore, indicates that besides being a basement membrane component, perlecan is also a marker of chondrogenic cells in prenatal cartilages. In postnatal cartilages, perlecan displayed a pericellular localisation pattern rather than the territorial or interterritorial localisation it displayed in foetal cartilages. This may reflect processing of extracellular perlecan presumably as a consequence of intrinsic biomechanical loading on these tissues or to divergent functions for perlecan and type II collagen in adult compared to prenatal tissues.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Type II collagen is the major structural fibrillar collagen of cartilage and a definitive chondrogenic marker (Eyre 2002; Eyre et al. 2006; 2002); 60% of the dry weight of articular cartilage is type II collagen. Aggrecan is also a primary chondrogenic marker and a predominant extracellular matrix (ECM) component of articular cartilages constituting 6–10% of its dry mass (Melrose et al. 2005b). Aggrecan is also expressed as a minor component in fibrocartilages where cells of a chondrogenic background exist (meniscus, intervertebral disc, tendon) (Melrose et al. 2001, 2005a; Nakano et al. 1997; Thomopoulos et al. 2002). In the course of our studies on the immunolocalisation of the heparan sulphate proteoglycan (HSPG), perlecan in tensional and weight-bearing connective tissues (Melrose et al. 2002; 2003; 2004b; 2005b; 2006), we observed that this proteoglycan displayed a very similar spatiotemporal immunolocalisation pattern to aggrecan and type II collagen, leading us to conclude that perlecan may also be a chondrogenic marker. The comparative immunolocalisations conducted in the present study on the foetal human tissues showed that perlecan immunolocalised precisely to the same cartilaginous tissues where type II collagen was immunolocalised and which were delineated by the anionic proteoglycan stain toluidine blue. Aggrecan was also a predominant matrix component in the cartilage, but was also diffusely distributed extracellularly in capsular lining tissues and ligaments and tendons in the joint compartments, which were poorly stained or not at all by toluidine blue and did not contain type II collagen. Perlecan strongly stained the pericellular matrix of rounded cells within the foetal and newborn rudimentary cartilages and the chondrocytes of the permanent articular cartilages. As we found earlier, it also stained the basement membrane of small blood vessels and nerves in the synovial lining tissues of joints (Melrose et al. 2004b) or cells of a rounded chondrocyte-like morphology within ligaments and tendons at the fibrocartilaginous enthesis attachment points of tendons to bone or the inner compressed third of menisci. This is consistent with the focal compressive load these tissue regions receive (Benjamin and Ralphs 1998, 2001) rather than the tensional load received elsewhere in the tendon or the hoop stresses generated in the outer tensional meniscal regions where the cells have an elongated fibroblastic morphology. We propose from the data generated in the present study that the comparative immunolocalisations of type II collagen, aggrecan and perlecan indicate that perlecan should also be considered a definitive early marker of the chondrogenic phenotype in prenatal tissues.
Materials and methods
Materials
Chondroitinase-ABC was obtained from Sigma-Aldrich, Castle Hill, NSW, Australia. Menzel and Glaser SuperFrost ultraPlus positively charged microscope sides were obtained from Fisher Scientific, Braunschweig, GmbH. Biotinylated anti-mouse IgG secondary antibody and horseradish peroxidase conjugate were obtained from Dako (Botany, NSW, Australia). Histochoice® was an Amresco product (Solon, OH, USA). Monoclonal antibody (MAb) to aggrecan G1 domain (clone 969D4D11) was obtained from Biosource Europe (Nivelle, Belgium through Bioclone, Sydney, Australia). Anti type II collagen (clone II-4CII) was purchased from MP Biomedicals, (Ohio, USA). Mouse MAb A76 to perlecan domain I was obtained from abcam through Sapphire Biosciences, (Redfern, Australia). NovaRED substrate was obtained from Vector Laboratories, (Burlingame, CA, USA).
Tissues
Knee, elbow, hip, shoulder, finger and toe joints from two 12-week and two 14-week-old human foetuses were obtained at the termination of pregnancy with ethical approval from the Human Care and Ethics Review Board of The Royal North Shore Hospital. Ovine hip, articular and knee tibial and femoral articular, patellar and growth plate cartilage and menisci were obtained from newborn (7 days old), and 7 and 19-month-old merino sheep with ethical approval from our institutional animal ethics committee.
Methods
Preparation of human foetal and ovine joint tissues for immunohistology
Whole foetal joints were fixed in Histochoice for 24 h (Melrose et al. 2008b). The tissues were then dehydrated in graded ethanol solutions and embedded in paraffin blocks. Four micron microtome sections were cut in vertical or coronal planes and attached to SuperFrost Plus glass microscope slides (Menzel-Glaser, Germany), de-paraffinised in xylene (2 changes × 5 min), and re–hydrated through graded ethanol washes (100–70% v/v) to water. Full thickness coronal vertical osteochondral tissue slabs (4 mm) from the mid weight-bearing regions of the tibia and femur of newborn (7 day), and 7 and 19-month-old ovine stifle joints encompassing the epiphyseal growth plates were prepared using a band saw (Melrose et al. 2004a). The bone/cartilage specimens were fixed, either in Histochoice or 10% neutral buffered formalin for 48 h then decalcified for 8 days in 10% formic acid. The specimens were then dehydrated in graded alcohols and embedded in Paraplast wax. Intact lateral and medial menisci from newborn (7 day), and 7 and 19-month-old sheep were fixed in Histochoice or 10% neutral buffered formalin for 48 h and a 3–4 mm wedge of the central region encompassing the outer to inner meniscal regions was prepared, dehydrated in sequentially graded alcohols and double embedded in paraplast wax-celloidin. Vertical 4 μm osteochondral and meniscal sections were cut on a rotary microtome and mounted on SuperFrost Plus glass slides, de-paraffinised in xylene and re-hydrated through graded ethanol washes (100–70% v/v) to water.
Histochemistry
Anionic proteoglycans were localised in tissue sections by staining for 10 min with 0.04% w/v toluidine blue in 0.1 M sodium acetate buffer, pH 4.0, followed by a 2-min counterstain in 0.1% w/v fast green FCF.
Immunohistochemistry
Incubations with primary antibodies were performed using a Sequenza vertical cover-plate immunostaining system (Melrose et al. 2005b; Melrose et al. 2003; Melrose et al. 2002; Melrose et al. 2004b). Endogenous peroxidase activity was blocked by incubating the tissue sections with 3% H2O2 for 5 min and after washing in water non-specific binding sites were blocked with 10% swine serum for 10 min. Sections destined for perlecan immunolocalisations (Melrose et al. 2005a, 2005b; Melrose et al. 2003; Melrose et al. 2002; Melrose et al. 2004b; Whitelock et al. 2008) were pre-digested with chondroitinase-ABC (0.25 U/ml) for 1 h at 37°C in 0.1 M Tris–HCl and 0.03 M sodium acetate buffer of pH 8.0. Specimens destined for aggrecan immunolocalisation (Melrose et al. 2002; 2003; 2005a, b) were pre-digested for 2 h at 37°C with 0.05 U/ml chondroitinase-ABC. Sections destined for localisation of type II collagen (Burgeson and Hollister 1979) were pre-digested with proteinase K for 6 min (DAKO S3020) followed by bovine testicular hyaluronidase (1,000 U/ml) for 1 h at 37°C in phosphate buffer of pH 5.0 prior to incubation with primary antibody. The primary Ab’s anti-aggrecan (1/20,000 dliution), anti-perlecan (1/1,000 dilution) and anti type II collagen (1/200 dilution) diluted in 50 mM Tris–HCl buffer, pH 7.2 and 0.15 M BSA were incubated with tissue sections at 4°C overnight and the tissues blocked 2 h at room temperature with Dako non-protein blocking agent. The primary Abs were subsequently localised using biotinylated anti-mouse IgG antibodies, and horseradish peroxidase conjugated streptavidin was subsequently used to visualise the tissue immune complexes using Nova RED substrate for colour development. Control sections were also prepared in which the authentic primary antibody was either omitted or replaced with an irrelevant isotype matched mouse IgG directed against Aspergillus niger glucose oxidase, an enzyme which is neither present nor inducible in mammalian tissues. The stained tissue specimens were then examined using a Leica photomicroscope linked to a DFC 480 digital camera using bright-field and Nomarski differential interference contrast microscopy.
Results
Histological examination of mid vertical longitudinal sections of 12-week-old human foetal big toe (Fig. 1a–d) and index finger (Fig. 1e–h) demonstrated the prominently stained primordial cartilages of the metatarsal and phalangeal cartilage rudiments of the toe and of the proximal, middle and distal phalanx rudiments of the finger separated by the distal, proximal interphalangeal and metacarpal phalangeal joint spaces (Fig. 1a, e). Type II collagen immunolocalisation followed a restricted expression pattern within the cartilaginous rudiments (Fig. 1b, f). Aggrecan was immunolocalised to similar regions as the toluidine blue-stained cartilaginous rudiments in the foetal big toe and first finger, but also stained periarticular structures such as the anterior tibialis tendon of the toe and flexor digitorum superficialis and extensor tendons in the finger (Fig. 1c, g). Perlecan, however, was immunolocalised precisely to the cartilage rudiments in the toe and finger displaying a similar distribution to the type II collagen immunolocalisations (Fig. 1d, h).
Toluidine blue prominently stained the cartilaginous rudiments of the shaft of the humerus and ulna in 12-week-old human foetal elbow joints (Fig. 2a, e), but did not stain a prominent ligamental attachment in the ulna (Fig. 2e). The immunolocalisation of type II collagen followed a similar distribution pattern (Fig. 2b, f). Aggrecan immunolocalisation was not confined to the cartilaginous humeral and ulna rudiments, but was also evident in periarticular structures associated with the elbow joint including capsular ligamental attachments (Fig. 2c, g). Perlecan was specifically immunolocalised to the cartilaginous rudiments of the ulna and humerus, but not to the ligamental attachments (Fig. 2h), and detected in the basement membrane of a nerve plexus adjacent to the elbow joint (Fig. 2d) and a series of small blood vessels in the looser stromal tissues surrounding the shaft of the humeral rudiment (Fig. 2d). However, in macroscopic views the predominant distribution pattern occupied by perlecan was confined to the cartilaginous rudiments to areas where type II collagen was also found.
Toluidine blue prominently stained a coronally sectioned 14-week-old human foetal shoulder joint, distinctively labelling the humeral head, acromion cartilage rudiments and cartilage canals (Fig. 3a). Type II collagen was immunolocalised precisely to the cartilage rudiments depicted by toluidine blue staining (Fig. 3b); aggrecan immunolocalisations were more widespread and its localisation extended to the surrounding ligamental tissues (Fig. 3c). This contrasted with the perlecan immunolocalisations, which precisely delineated the cartilage rudiments in a similar manner to the type II collagen immunolocalisations (Fig. 3d). Perlecan also delineated small blood vessels in the shoulder capsular tissues (Fig. 3d).
The cartilaginous femoral, tibial and patellar rudiments were prominently stained by toluidine blue in two 12-week-old foetal human knee joints (Fig. 4a, d). Whereas type II collagen immunolocalisations precisely identified the cartilage rudiments (Fig. 4b), aggrecan was present diffusely in the periarticular knee joint capsular tissues, posterior and anterior cruciate ligaments and patellar tendons, and strongly stained the cartilaginous rudiments (Fig. 4c). Immunolocalisation of perlecan was primarily in the tibial and femoral rudiments (Fig. 4e), but para-articular structures were also labelled to a lesser extent including small blood vessels in the joint capsule and stromal tissues associated with the shaft of the tibial and femoral rudiments and the inner zone of the cross-sectioned medial and lateral menisci (Fig. 4e).
Histological and immunohistological localisation of anionic proteoglycan using toluidine blue–fast green staining (a, d), type II collagen (b), aggrecan (c) and perlecan (e) in two 12-week-old human foetal knees, vertical section, macroscopic views. The serial section available for the localisation of perlecan (e) did not contain any patella, type II collagen and aggrecan localisations in the second knee and were similar to those depicted in segments (b, c, respectively) and are not shown. The femoral cartilaginous rudiment is present towards the top of each photosegment and the tibial rudiment is below this
Examination of a coronally sectioned 14-week-old human foetal knee joint (Fig. 5a–d) demonstrated similar immunolocalisation patterns to those evident in the 12-week-old knee specimens. In macroscopic views of serial sections of 12- and 14-week-old human foetal femoral head rudiments, staining with toluidine blue vividly delineated the extent of the cartilaginous rudiment and cartilage canals (Fig. 5e, i), but perichondrial regions of the femoral heads were unstained. Immunolocalisation of type II collagen delineated the same regions of the cartilage rudiments as did toluidine blue (Fig. 5f, j). Immunolocalisation of aggrecan stained a comparable area of the rudiment to that stained with toluidine blue and in which type II collagen was immunolocalised; however, aggrecan was also detected in the perichondrial regions (Fig. 5g, k). Perlecan was immunolocalised to the same regions of these tissues stained with toluidine blue and in which type II collagen was present (Fig. 5h, i).
Histological and immunohistological localisation of anionic proteoglycan using toluidine blue–fast green staining (a, e, i), type II collagen (b, f, j), aggrecan (c, g, k) and perlecan (d, h, l) in a 14-week-old human foetal knee, and 12- and 14-week-old human foetal femoral heads. Coronal sections, macroscopic views, composite images
Higher power microscopy of the perlecan immunolocalisations at magnifications conducive to viewing cellular detail demonstrated its pericellular localisation in the basement membranes around cells in the human colon (Fig. 6a) and around blood vessels in the synovial lining tissues where entrapped red blood cells were conspicuous (Fig. 6b, c). Perlecan immunolocalisation was also evident within the humerus rudiment and in a series of small blood vessels along its shaft, basement membrane of a nerve plexus and stromal blood vessels associated with the rudiments (Fig. 6d, h). Perlecan was also immunolocalised to blood vessels in the infolded synovial lining tissues, as well as pericellular staining of chondrocytes within the cartilaginous rudiments in a human foetal finger (Fig. 6e, f). Closer inspection of the cells within the flexor digitorum superficialis tendon attachment point to the metacarpophalangeal joint in a 12-week-old human foetal finger clearly identified a population of rounded perlecan positive cells within the insertion, whereas the elongated cells in the tendon were negative (Fig. 6g). Perlecan and aggrecan localisations in the interphalangeal joint between the middle and proximal phalanx of a 12-week-old finger clearly showed that the latter had a more widespread distribution in these tissues than perlecan (Fig. 7b, c). Toluidine blue staining was relatively light in the associated tendon and perichondrial regions of the cartilage rudiments, which displayed intense aggrecan localisations but diffuse perlecan staining (Fig. 7a–c). Perlecan was, however, prominently localised to the hypertrophic chondrocytes of the growth plates, blood vessels in synovial lining tissues and stromal connective tissues of the cartilage rudiments (Fig. 7c).
Immunolocalisation of perlecan in human colon (a), and blood vessels in a 12-week foetal knee (b, c), elbow (d, h) and finger (e–g). The boxed areas in segments (d and e) are presented at higher magnification in segments (h and f), respectively. Perlecan follows a prominent localisation pattern associated with the chondrocytes of the cartilaginous rudiments with up-regulated expression in the hypertrophic cells of the developing growth plates of the primary ossification centres in the ulna (d) and first finger (e). Perlecan is also strongly expressed by blood vessels in the synovial lining tissues in the 12- to 14-week-old human foetal knee (b, c respectively), elbow (d, arrows), finger (e, f) and cells of a rounded morphology dissimilar to the elongated tenocytes in the attachment region of the flexor digitorum superficialis tendon to the margins of the metacarpo-phalangeal joint between the head of the metacarpal and proximal phalanx (g, asterisk). The boxed area in segment (d) is presented at higher magnification in (h) depicting perlecan localisation in a blood vessel (BV) and the basement membrane of a nerve associated with the elbow (h). Segment (a) is a positive control slide for perlecan, depicting human colon with prominent localisation of perlecan in the basement membranes of the crypt cells in the lamina propria, which are in cross section. Red blood cells are visible in the two knee joint vessels presented in (b, c), which were visualised by perlecan staining and the red blood vessels visualised using Nomarski differential interference contrast imaging
Medium power views of localisation of anionic proteoglycan by toluidine blue–fast green staining (a) and immunolocalisation of aggrecan (b) and perlecan (c) in the proximal interphalangeal (PIP) joint-associated tissues between the middle and proximal phalanx. Aggrecan is a prominent component staining the phalangeal cartilaginous rudiments as well as the flexor digitorum superficialis and extensor tendons, which insert into the margins of the PIP joint and regions of the tendon that attach onto the shaft of the finger rudiment cartilage (b). Perlecan is prominently expressed by the chondrocytes in the cartilaginous rudiments and by blood vessels in the synovial lining and joint capsular tissues, as well as in the adjacent skin and cells of a rounded morphology dissimilar to the tenocytes in the flexor digitorum superficialis tendon attachment points to the proximal phalanx (c)
Macroscopic localisations of toluidine blue-stained proteoglycan (Fig. 8a, e, i, m), type II collagen (Fig. 8b, f, j, n), aggrecan (Fig. 8c, g, k, o) and perlecan (Fig. 8d, h, i, p) in femoral (Fig. 8a–d), tibial (Fig. 8e–h), patellar (Fig. 8i–l) and femoral hip articular and growth plate cartilages (Fig. 8m–p) of newborn (7-day-old) sheep again demonstrated that perlecan displayed similar distributions to the other chondrogenic markers in these joint tissues. Selected areas in the deep articular and femoral and tibial growth plate cartilages were also presented at higher magnification to provide detail of the perlecan localisations in relation to cellular organisation in these tissues (Figs. 9, 10). This demonstrated that perlecan (Fig. 9m-p) displayed a prominent pericellular localisation pattern similar to that of aggrecan (Fig. 9i–l) in these newborn ovine joint tissues, whilst type II collagen had a prominent extracellular distribution pattern throughout these tissues (Fig. 9e–h). Perlecan displayed a gradient in ECM localisation in the femoral and tibial growth plate cartilages of the newborn ovine knee joint with the hypertrophic chondrocytes displaying the highest levels of perlecan expression. Aggrecan and perlecan also displayed a diffuse distribution in the interterritorial matrix of the columnar and hypertrophic growth plate chondrocytes (Fig. 10a, b, e, f), whilst again type II collagen displayed an extracellular distribution (Fig. 10c, g) similar to that depicted by toluidine blue proteoglycan staining throughout the growth plate cartilages (Fig. 10d, h).
Macroscopic localisation of toluidine blue-stained proteoglycan (a, e, i, m), type II collagen (b, f, j, n), aggrecan (c, g, k, o) and perlecan (d, h, i, p) localisations in ovine newborn (7-day-old) joint tissues. Coronal vertical sections of femoral condyle (a–d) and tibial plateau (e–h), patella (horizontal section) (i–l) and femoral head (vertical section) (m–p)
Higher power localisations of toluidine blue-stained proteoglycan (a–d), type II collagen (e–h), aggrecan (i–l) and perlecan (m–p) localisations in femoral condyle (FC, a, e, i, m), tibial plateau (TP, b, f, j, n), patella (c, g, k, o) and hip (d, h, l, p) articular cartilage of ovine newborn (7-day-old) joints
Observation of the macroscopic staining patterns for toluidine blue-stained proteoglycan, type II collagen, aggrecan and perlecan in newborn 7- and 19-month-old ovine menisci showed that these components were prominent in the inner third of the menisci, particularly in the newborn menisci (Fig. 11a, d, g, j). This inner meniscal region is known to experience compressive load rather than the outer meniscal zone, which experiences tensional hoop stresses and which had considerably less staining for these components (Fig. 11a–i).
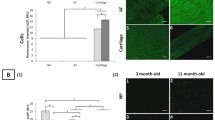
Comparative immunolocalisations of perlecan and aggrecan in full thickness femoral and tibial articular cartilages from 7- and 19-month-old ovine knee joints again showed that the former displayed a prominent pericellular localisation around cells of a rounded morphology throughout the full thickness of these articular cartilages, but little if any staining was evident in the territorial and interterritorial regions of these tissues (Fig. 12b, d, f, h). Aggrecan, however, was a prominent extracellular matrix component (Fig. 12a, c, e, g) and displayed a distribution similar to that of type II collagen in these young to mature adult cartilages.
Observation of higher magnification immunolocalisations of perlecan in the surface regions of the newborn to mature femoral and tibial articular cartilages and menisci indicated that cells of a flattened morphology did not express perlecan in any of these tissues (Fig. 13a–c, g–i, m–o), whilst cells of a rounded morphology had prominent pericellular perlecan rich matrices (Fig. 13d–f, j–l, p–r).
Comparative immunolocalisation of perlecan in the surface and deep cartilage regions in newborn, and 7-month and 19-month-old menisci (a–f) and femoral (g–l) and tibial (m–n) articular cartilages. Photosegments a–c are imaged using Nomarski differential interference contrast microscopy to visualise the laminar surface structure of the menisci. Scale bars 50 μm
Discussion
If aggrecan, type II collagen and perlecan are definitive markers of the cartilaginous phenotype, it seems reasonable to expect that they must have essential roles to play in the development, maintenance and function of cartilage. Type II collagen is the major structural collagen of cartilage and also occurs in non-cartilaginous tissues such as the vitreous fluid of the eye (Edwards 2008; Ponsioen et al. 2008), and its identity as a chondrogenic marker is beyond contention (Eyre 2002; Eyre et al. 2006; O’Driscoll et al. 1995). To determine the roles that aggrecan and perlecan play in chondrogenesis, mouse knockout or partial deletion models have been used to examine how connective tissues rich in these proteoglycans are affected by genetic manipulation, which alters the levels of these proteoglycans in the tissues.
The cartilage matrix deficiency (cmd) mouse, due to a deletion in the aggrecan gene, was the first example of a mutation of a proteoglycan gene identified in mammals (Watanabe and Yamada 2002). Cmd/cmd homozygotes display dwarf-like features, cleft palates and die shortly after birth due to respiratory failure. The cartilage of cmd/cmd mice is highly cellular, but deficient in matrix components although they contain normal levels of link protein and type II collagen. Electron microscopy of cmd homozygote cartilage shows abnormal collagen fibril formation and packing indicating that aggrecan has roles to play in collagen fibrillogenesis in chondrogenesis through its ability to act as a space-filling ECM molecule. Perlecan knockdown in mice is a lethal condition, endochondral ossification is severely impaired and the spinal rudiments do not fully develop leading to a diminished skeletal stature (Arikawa-Hirasawa et al. 1999, 2001a, b, 2002). Most of the perlecan knockout mice survive early stages of embryonic development, but by day 11.5 around 50% of them die due to cardiac failure or other cardiovascular insufficiencies. The remaining mice die shortly thereafter due to respiratory failure (Arikawa-Hirasawa et al., 1999, 2001a, b, 2002). The pups that survive to birth display short squat frames; examination of their long bones demonstrates massive disruptions in chondrogenesis (French et al. 1999) and endochondral ossification; thus, perlecan has well-established roles to play in chondrogenesis (Iozzo 1994; Iozzo et al. 1994). The chondrogenic activity of perlecan maps to its HS substituted domain-1 (French et al. 2002; Yang et al. 2006) and this has been utilised in regenerative strategies utilising matrices containing perlecan domain-1 and BMP-2 to stimulate chondrogenesis (Gomes et al. 2003; Jha et al. 2009; Yang et al. 2006). Perlecan also has roles to play in the sequestration and presentation of FGF-1, 2, 7, 9 and 18 to chondrocytes (Iozzo 1994; Iozzo et al. 1994; Knox et al. 2001, 2002; Knox and Whitelock 2006; Melrose et al. 2006; Whitelock et al. 2008) and in the organisation and stabilisation of rudimentary, articular and growth plate cartilages through its interactive properties with a diverse range of ECM molecules, which provide cell–cell and cell–ECM connections (Costell et al. 1999; Iozzo 1994, 2005; Iozzo et al. 1994; Melrose et al. 2008a; SundarRaj et al. 1995). The demonstration of FGF-2, the major ligand of perlecan, as a mechanotransductive molecule in articular cartilage (Vincent et al. 2002, 2004; Vincent and Saklatvala 2006) is consistent with the aforementioned functional properties of perlecan and also implicates it in an accessory role in the mechanosensory machinery (Vincent et al. 2007), which chondrocytes utilise to sense alterations in their biomechanical microenvironment and elicit a response in terms of matrix remodelling or synthesis in such instances to effect tissue homeostasis.
Perlecan clearly has many important roles to play in cartilage development, maintenance and function. Indeed, whilst perlecan is found in the interterritorial and pericellular matrix in rudimentary developmental and growth plate cartilages, it displays a strict pericellular localisation pattern in the chondrocytes of the permanent articular cartilages; thus, it is a definitive cell-associated chondrogenic marker (Melrose et al. 2006). This divergent localisation pattern of perlecan in the pre- and postnatal cartilages may reflect the different biomechanical loadings experienced by these tissues and more extensive processing of perlecan in the mature cartilages. Aggrecan is also a prominent extracellular molecule in cartilage and diffusely localised in capsular tissues and focal regions of ligaments and tendons subjected to compressive forces. Perlecan immunolocalisations precisely delineate rounded cartilage-like cells in these focally compressed enthesis regions of tendon complimenting the matrix-associated aggrecan localisation in this region. Thus, perlecan delineates cells of a chondrogenic background even in fibrocartilages containing a mixed population of cells of differing genetic background. We also observed that in newborn to adult ovine menisci, and in the femoral and tibial knee joint articular cartilages that whilst the rounded cells within the cartilage proper expressed perlecan, surface zone cells of an elongated morphology in these tissues did not. The cells in the surface lamina of menisci and cartilage also express proteoglycan-4 (lubricin), whereas chondrocytes do not (Gleghorn et al. 2007; Sun et al. 2006). The collected evidence presented herein therefore strongly supports our assertion that perlecan should be considered as a cell-associated chondrogenic marker. Perlecan is detectable in very early stages of cartilage development (Gustafsson et al. 2003; Hassell et al. 2002; Melrose et al. 2002, 2003, 2004b, 2008a, Roediger et al. 2009; Smith et al. 2009) and, although diminished in content in mature cartilages partly due to the age-dependant decline in cell numbers in this tissue, it is nevertheless still a readily detectable cell-associated entity (Melrose et al. 2005b, 2006). Indeed, in chondrocyte clones in osteoarthritic cartilage, perlecan expression has been shown to be focally up-regulated compared to that in the resident permanent chondrocytes (Tesche and Miosge 2004, 2005). This has led to the proposal that these cell clusters represent an adult chondro-progenitor cell population present in the surface-eroded articular cartilage, further supporting perlecan as a marker protein for the chondrogenic phenotype. The same cannot be said of aggrecan, the major cartilage proteoglycan that is focally depleted around these cell clusters in OA.
References
Arikawa-Hirasawa E, Watanabe H, Takami H, Hassell JR, Yamada Y (1999) Perlecan is essential for cartilage and cephalic development. Nat Genet 23:354–358
Arikawa-Hirasawa E, Wilcox WR, Le AH, Silverman N, Govindraj P, Hassell JR, Yamada Y (2001a) Dyssegmental dysplasia, Silverman-Handmaker type, is caused by functional null mutations of the perlecan gene. Nat Genet 27:431–434
Arikawa-Hirasawa E, Wilcox WR, Yamada Y (2001b) Dyssegmental dysplasia, Silverman-Handmaker type: unexpected role of perlecan in cartilage development. Am J Med Genet 106:254–257
Arikawa-Hirasawa E, Le AH, Nishino I, Nonaka I, Ho NC, Francomano CA, Govindraj P, Hassell JR, Devaney JM, Spranger J, Stevenson RE, Iannaccone S, Dalakas MC, Yamada Y (2002) Structural and functional mutations of the perlecan gene cause Schwartz-Jampel syndrome, with myotonic myopathy and chondrodysplasia. Am J Hum Genet 70:1368–1375
Benjamin M, Ralphs JR (1998) Fibrocartilage in tendons and ligaments—an adaptation to compressive load. J Anat 193(Pt 4):481–494
Benjamin M, Ralphs JR (2001) Entheses—the bony attachments of tendons and ligaments. Ital J Anat Embryol 106:151–157
Burgeson RE, Hollister DW (1979) Collagen heterogeneity in human cartilage: identification of several new collagen chains. Biochem Biophys Res Commun 87:1124–1131
Costell M, Gustafsson E, Aszodi A, Morgelin M, Bloch W, Hunziker E, Addicks K, Timpl R, Fassler R (1999) Perlecan maintains the integrity of cartilage and some basement membranes. J Cell Biol 147:1109–1122
Edwards AO (2008) Clinical features of the congenital vitreoretinopathies. Eye (Lond) 22:1233–1242
Eyre D (2002) Collagen of articular cartilage. Arthritis Res 4:30–35
Eyre DR, Wu JJ, Fernandes RJ, Pietka TA, Weis MA (2002) Recent developments in cartilage research: matrix biology of the collagen II/IX/XI heterofibril network. Biochem Soc Trans 30:893–899
Eyre DR, Weis MA, Wu JJ (2006) Articular cartilage collagen: an irreplaceable framework? Eur Cell Mater 12:57–63
French MM, Smith SE, Akanbi K, Sanford T, Hecht J, Farach-Carson MC, Carson DD (1999) Expression of the heparan sulfate proteoglycan, perlecan, during mouse embryogenesis and perlecan chondrogenic activity in vitro. J Cell Biol 145:1103–1115
French MM, Gomes RR Jr, Timpl R, Hook M, Czymmek K, Farach-Carson MC, Carson DD (2002) Chondrogenic activity of the heparan sulfate proteoglycan perlecan maps to the N-terminal domain I. J Bone Miner Res 17:48–55
Gleghorn JP, Jones AR, Flannery CR, Bonassar LJ (2007) Boundary mode frictional properties of engineered cartilaginous tissues. Eur Cell Mater 14:20–28 (discussion 28–29)
Gomes RR Jr, Farach Carson MC, Carson DD (2003) Perlecan-stimulated nodules undergo chondrogenic maturation in response to rhBMP-2 treatment in vitro. Connect Tissue Res 44(Suppl 1):196–201
Gustafsson E, Aszodi A, Ortega N, Hunziker EB, Denker HW, Werb Z, Fassler R (2003) Role of collagen type II and perlecan in skeletal development. Ann N Y Acad Sci 995:140–150
Hassell J, Yamada Y, Arikawa-Hirasawa E (2002) Role of perlecan in skeletal development and diseases. Glycoconj J 19:263–267
Iozzo RV (1994) Perlecan: a gem of a proteoglycan. Matrix Biol 14:203–208
Iozzo RV (2005) Basement membrane proteoglycans: from cellar to ceiling. Nat Rev Mol Cell Biol 6:646–656
Iozzo RV, Cohen IR, Grassel S, Murdoch AD (1994) The biology of perlecan: the multifaceted heparan sulphate proteoglycan of basement membranes and pericellular matrices. Biochem J 302(Pt 3):625–639
Jha AK, Yang W, Kirn-Safran CB, Farach-Carson MC, Jia X (2009) Perlecan domain I-conjugated, hyaluronic acid-based hydrogel particles for enhanced chondrogenic differentiation via BMP-2 release. Biomaterials 30:6964–6975
Knox SM, Whitelock JM (2006) Perlecan: how does one molecule do so many things? Cell Mol Life Sci 63:2435–2445
Knox S, Melrose J, Whitelock J (2001) Electrophoretic, biosensor, and bioactivity analyses of perlecans of different cellular origins. Proteomics 1:1534–1541
Knox S, Merry C, Stringer S, Melrose J, Whitelock J (2002) Not all perlecans are created equal: interactions with fibroblast growth factor (FGF) 2 and FGF receptors. J Biol Chem 277:14657–14665
Melrose J, Ghosh P, Taylor TK (2001) A comparative analysis of the differential spatial and temporal distributions of the large (aggrecan, versican) and small (decorin, biglycan, fibromodulin) proteoglycans of the intervertebral disc. J Anat 198:3–15
Melrose J, Smith S, Knox S, Whitelock J (2002) Perlecan, the multidomain HS-proteoglycan of basement membranes, is a prominent pericellular component of ovine hypertrophic vertebral growth plate and cartilaginous endplate chondrocytes. Histochem Cell Biol 118:269–280
Melrose J, Smith S, Ghosh P, Whitelock J (2003) Perlecan, the multidomain heparan sulfate proteoglycan of basement membranes, is also a prominent component of the cartilaginous primordia in the developing human fetal spine. J Histochem Cytochem 51:1331–1341
Melrose J, Smith S, Ghosh P (2004a) Histological and immunohistological studies on cartilage. In: De Ceuninck MS F, Pastoreau P (eds) Cartilage and osteoarthritis volume 2 Structure and in vivo analysis, vol 2. Humana Press, Totowa, pp 39–63
Melrose J, Smith S, Whitelock J (2004b) Perlecan immunolocalises to perichondral vessels and canals in human foetal cartilagenous promordia in early vascular and matrix remodelling events associated with diarthrodial-joint development. J Histochem Cytochem 52:1405–1413
Melrose J, Smith S, Cake M, Read R, Whitelock J (2005a) Comparative spatial and temporal localisation of perlecan, aggrecan and type I, II and IV collagen in the ovine meniscus: an ageing study. Histochem Cell Biol 124:225–235
Melrose J, Smith S, Cake M, Read R, Whitelock J (2005b) Perlecan displays variable spatial and temporal immunolocalisation patterns in the articular and growth plate cartilages of the ovine stifle joint. Histochem Cell Biol 123:561–571
Melrose J, Roughley P, Knox S, Smith S, Lord M, Whitelock J (2006) The structure, location, and function of perlecan, a prominent pericellular proteoglycan of fetal, postnatal, and mature hyaline cartilages. J Biol Chem 281:36905–36914
Melrose J, Hayes AJ, Whitelock JM, Little CB (2008a) Perlecan, the “jack of all trades” proteoglycan of cartilaginous weight-bearing connective tissues. Bioessays 30:457–469
Melrose J, Smith SM, Smith MM, Little CB (2008b) The use of Histochoice for histological examination of articular and growth plate cartilages, intervertebral disc and meniscus. Biotech Histochem 83:47–53
Nakano T, Dodd CM, Scott PG (1997) Glycosaminoglycans and proteoglycans from different zones of the porcine knee meniscus. J Orthop Res 15:213–220
O’Driscoll SW, Commisso CN, Fitzsimmons JS (1995) Type II collagen quantification in experimental chondrogenesis. Osteoarthritis Cartil 3:197–203
Ponsioen TL, van Luyn MJ, van der Worp RJ, van Meurs JC, Hooymans JM, Los LI (2008) Collagen distribution in the human vitreoretinal interface. Invest Ophthalmol Vis Sci 49:4089–4095
Roediger M, Kruegel J, Miosge N, Gersdorff N (2009) Tissue distribution of perlecan domains III and V during embryonic and fetal human development. Histol Histopathol 24:859–868
Smith S, Whitelock JM, Iozzo RV, Melrose J (2009) Topographical variation in the distributions of versican, aggrecan and perlecan in the foetal human spine reflects their diverse functional roles in spinal development. Htistochem Cell Biol 132:491–503
Sun Y, Berger EJ, Zhao C, An KN, Amadio PC, Jay G (2006) Mapping lubricin in canine musculoskeletal tissues. Connect Tissue Res 47:215–221
SundarRaj N, Fite D, Ledbetter S, Chakravarti S, Hassell JR (1995) Perlecan is a component of cartilage matrix and promotes chondrocyte attachment. J Cell Sci 108(Pt 7):2663–2672
Tesche F, Miosge N (2004) Perlecan in late stages of osteoarthritis of the human knee joint. Osteoarthritis Cartil 12:852–862
Tesche F, Miosge N (2005) New aspects of the pathogenesis of osteoarthritis: the role of fibroblast-like chondrocytes in late stages of the disease. Histol Histopathol 20:329–337
Thomopoulos S, Hattersley G, Rosen V, Mertens M, Galatz L, Williams GR, Soslowsky LJ (2002) The localized expression of extracellular matrix components in healing tendon insertion sites: an in situ hybridization study. J Orthop Res 20:454–463
Vincent T, Saklatvala J (2006) Basic fibroblast growth factor: an extracellular mechanotransducer in articular cartilage? Biochem Soc Trans 34:456–457
Vincent T, Hermansson M, Bolton M, Wait R, Saklatvala J (2002) Basic FGF mediates an immediate response of articular cartilage to mechanical injury. Proc Natl Acad Sci USA 99:8259–8264
Vincent TL, Hermansson MA, Hansen UN, Amis AA, Saklatvala J (2004) Basic fibroblast growth factor mediates transduction of mechanical signals when articular cartilage is loaded. Arthritis Rheum 50:526–533
Vincent TL, McLean CJ, Full LE, Peston D, Saklatvala J (2007) FGF-2 is bound to perlecan in the pericellular matrix of articular cartilage, where it acts as a chondrocyte mechanotransducer. Osteoarthritis Cartil 15:752–763
Watanabe H, Yamada Y (2002) Chondrodysplasia of gene knockout mice for aggrecan and link protein. Glycoconj J 19:269–273
Whitelock JM, Melrose J, Iozzo RV (2008) Diverse cell signaling events modulated by perlecan. Biochemistry 47:11174–11183
Yang W, Gomes RR, Brown AJ, Burdett AR, Alicknavitch M, Farach-Carson MC, Carson DD (2006) Chondrogenic differentiation on perlecan domain I, collagen II, and bone morphogenetic protein-2-based matrices. Tissue Eng 12:2009–2024
Acknowledgments
Funded by National Health and Medical Research Council of Australia, Project Grant 352562.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Smith, S.M., Shu, C. & Melrose, J. Comparative immunolocalisation of perlecan with collagen II and aggrecan in human foetal, newborn and adult ovine joint tissues demonstrates perlecan as an early developmental chondrogenic marker. Histochem Cell Biol 134, 251–263 (2010). https://doi.org/10.1007/s00418-010-0730-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00418-010-0730-x