Abstract
Vascular permeability and endothelial glycocalyx were examined in young adult spontaneously hypertensive rats (SHR), stroke-prone SHR (SHRSP), and Wistar Kyoto rats (WKY) as a control, in order to determine earlier changes in the blood-brain barrier (BBB) in the hypothalamus in chronic hypertension. These rats were injected with horseradish peroxidase (HRP) as an indicator of vascular permeability. Brain slices were developed with a chromogen and further examined with cationized ferritin, a marker for evaluating glycocalyx. Staining for HRP was seen around vessels in the hypothalamus of SHR and SHRSP, but was scarce in WKY. The reaction product of HRP appeared in the abluminal pits of endothelial cells and within the basal lamina of arterioles, showing increased vascular permeability in the hypothalamus of SHR and SHRSP, whereas there were no leaky vessels in the frontal cortex of SHR and SHRSP, or in both areas of WKY. The number of cationized ferritin particles binding to the capillary endothelial cells was decreased in the hypothalamus of SHR and SHRSP, while the number decreased in the frontal cortex of SHRSP, compared with those in WKY. Cationized ferritin binding was preserved in some leaky arterioles, while it was scarce or disappeared in other leaky vessels. These findings suggest that BBB disruption occurs in the hypothalamus of 3-month-old SHR and SHRSP, and that endothelial glycocalyx is markedly damaged there without a close relationship to the early changes in the BBB.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Vascular dementia is a heterogeneous syndrome caused by the occlusion of large vessels or small artery disease (Hachinski et al. 1987; Parnetti et al. 1994; Roman 1996; Wallin and Blennow 1993). The pathogenesis of, and relationship between, the latter small artery lesions, i.e., lacunae and white matter lesions, and progressive cognitive impairment or dementia have been much debated. Wardlaw et al. (2003) recently reviewed the causative role of blood-brain barrier (BBB) impairment in vascular dementia, with leakage of serum components into and through the walls of cerebral small arterioles leading to neuronal and glial damage. Hypertension is one of the risk factors for cerebrovascular disease and also has a role in the development of vascular dementia. It is well known that hypertension causes BBB dysfunction and brain damage (Amenta et al. 2003; Fredriksson et al. 1987; Johansson 1980; Knox et al. 1980; O’Sullivan et al. 2003). Earlier changes in the BBB in chronic hypertension and the mechanism of BBB disruption remain unclear.
Spontaneously hypertensive rats (SHR), which are normotensive at birth and gradually develop hypertension in the first months of life, represent a model of chronic hypertension sharing several similarities with human essential hypertension (Fredriksson et al. 1985, 1988a, b; Hazama et al. 1975; Mueller 1982; Ogata et al. 1981; Okamoto and Aoki 1963; Okamoto et al. 1974; Sabbatini et al. 2000, 2002; Yamori et al. 1975). At present, it is known that in the early changes in the BBB of SHR, BBB damage occurs in the cerebral cortex, and in the deep gray matter in SHR at the age of 5 or 6 months or older, at which point tissue damage has already manifested (Fredriksson et al. 1987; Knox et al. 1980), while increased vascular permeability appears in pial arterioles of 3-month-old SHR (Knox et al. 1980). It remains to be clarified whether the BBB in parenchymal vessels has deteriorated or not in 3-month-old SHR, and also whether the BBB has deteriorated or not in the hypothalamus of SHR. The hypothalamus is a well-known autonomic regulatory region of the brain involved in integrating several behaviors, as well as cardiorespiratory activity (Kramer et al. 2000). Several studies have revealed neuronal dysfunction in the hypothalamus of hypertensive animals (Horn et al. 1998; Kramer et al. 2000). It is hypothesized that the dysfunction in the specific neuronal system in the hypothalamus has significant neurophysiological ramifications for cardiovascular dysregulation in SHR (Kramer et al. 2000). A hypothalamic defect has been suggested to be involved in mediating elevated levels of resting arterial pressure in SHR (Fukushima 1968; Yamori and Okamoto 1969). Therefore, we examined the BBB in the hypothalamus of 3-month-old SHR, which were in a hypertensive state.
The BBB damage was evaluated in terms of endothelial glycocalyx and vascular permeability, both of which are altered in acute hypertension (Nag 1984). Glycocalyx is a surface layer lining the endothelial cells and is composed of proteoglycan. Its physiological functions are multifaceted: it is a transport barrier, a porous hydrodynamic interface in the motion of red and white blood cells in microvessels, and a mechanotransducer of fluid shearing stresses to the cytoskeleton of endothelial cells. Combined cationized ferritin (CF) binding and horseradish peroxidase (HRP) histochemical labeling techniques were used to detect the surface anionic charge based on glycocalyx (Lindner et al. 1998; Thurauf et al. 1983; Vorbrodt et al. 1986) and as a sensitive method of vascular permeability (Mesulam 1978; Ueno et al. 2000, 2001a, b, 2002), respectively.
Materials and methods
Twelve-week-old male Wistar Kyoto/izumo (WKY), SHR/izumo (SHR), and stroke-prone SHR/izumo (SHRSP) rats (purchased from Japan CL, Japan) weighing 250–300 g (n=15) were used. The experimental protocol was conducted according to the Japanese Experimental Animal Research Association Standards, as defined in the Guidelines for Animal Experiments, and was approved by the Animal Research Committee at Kagawa University. Systolic and diastolic arterial pressure was measured in awake rats by the tail-cuff method. The animals were anesthetized with sodium pentobarbital (60 mg/kg body weight), and injected with diphenhydramine (0.5 mg/100 g body weight, i.p.) 30 min before the injection of HRP to avoid an anaphylactic response possibly induced by HRP. Then, the rats were injected with HRP (50 mg per rat, type VI; Sigma, St. Louis, MO, USA) via a femoral vein 5 min before perfusion fixation.
The animals were perfused transcardially with 0.01 mol/l phosphate-buffered saline and then with a fixative containing 2.5% glutaraldehyde and 2% paraformaldehyde in a 0.1 mol/l phosphate buffer, pH 7.4 (Ueno et al. 2000). The brain was removed and immersed in 1.25% glutaraldehyde and 1% paraformaldehyde in a 0.1 mol/l phosphate buffer, pH 7.4, at 4°C for 12 h. It was placed in a sucrose buffer solution consisting of 10% sucrose in a 0.1 mol/l phosphate buffer, pH 7.4, at 4°C for 12–24 h, sectioned coronally on a microslicer into sections 50 μm in thickness, and collected in a 0.1 mol/l phosphate buffer.
For light microscopic observation, some sections were further transferred to an incubation medium composed of a 0.01 mol/l acetate buffer (pH 3.3), tetramethylbenzidine (TMB), and hydrogen peroxide, as reported previously (Mesulam 1978; Ueno et al. 2001a). The sections incubated with TMB were mounted on gelatin-coated glass slides and a few sections were counterstained with hematoxylin-eosin.
For electron microscopic observation, the surface anionic sites in the vessel wall were first examined. The sections were immersed for 4 h in ice-cold 0.1 mol/l NH4Cl in a 0.1 mol/l cacodylate buffer, pH 7.3, to block free aldehyde groups. This step was followed by overnight washing in the same buffer. Then, the sections were incubated for 15 min at room temperature in a solution of CF (Sigma) in 0.1 mol/l of a cacodylate buffer, pH 7.3 (1 mg/ml), according to the procedure of Thurauf et al. (1983) with some modifications (Vorbrodt et al. 1986). Some sections were incubated under similar conditions in a solution of native ferritin (Calbiochem-Novabiochem, La Jolla, CA, USA) to evaluate non-specific binding. Then, the sections were transferred to an incubation medium of a 0.1 mol/l cacodylate buffer, pH 7.3, diaminobenzidine tetrahydrochloride (DAB), and hydrogen peroxide (Reese and Karnovsky 1967; Ueno et al. 2000). The sections were washed and fixed for 1 h in 1% OsO4 buffered with a 0.1 mol/l cacodylate buffer, pH 7.3, washed again, en bloc stained with 1% uranyl acetate for 1 h at room temperature in darkness, dehydrated in ethanol, and embedded in Epon 812. One-micrometer-thick sections were taken from each block and stained with 0.5% toluidine blue. Ultrathin sections were cut, placed on uncoated or coated grids and observed with a JEM-1200EX electron microscope. In addition, some grids were stained with uranyl acetate and Reynold’s lead citrate.
Assessment of CF binding to the microvascular glycocalyx was made from photographic prints with a final magnification of ×120,000. Glycocalyx thickness was determined at 1-cm intervals along the endothelial luminal surface by measuring the distance from the cell membrane to the farthest CF molecule (Lindner et al. 1998). Statistical analysis was performed by non-parametric group tests (Mann-Whitney U-test) using StatView II software (Abacus Concepts) on a Macintosh computer. Blood pressure was represented by the mean of five values ±SD and statistical analysis of the blood pressure among three groups was performed by non-parametric group tests (Mann-Whitney U-test). The vessels, in which the staining for HRP was seen within the basement membrane, were considered to be leaky vessels with increased vascular permeability, and statistical analysis of the percentage of leaky arterioles was done for SHRSP (or SHR) and WKY using Fisher’s exact probability test.
Results
Blood pressure (systolic/diastolic) was significantly higher in 3-month-old SHR (184±30 mmHg/143±23 mmHg) and SHRSP (216±27 mmHg/163±17mmHg) than in the same-aged WKY (124±9 mmHg/97±8 mmHg).
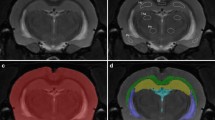
A staining reaction for HRP was seen very clearly around median eminence, a BBB-free area, in three strains of rats (Fig. 1). In addition, staining for HRP was present around vessels in anterior portions of the hypothalamus and parts of the basal forebrain, amygdala, and piriform cortex of SHR and SHRSP, while it was weak around a few WKY vessels (Fig. 1). On the contrary, no reaction product was observed in the frontal cortex of the three strains. Electron microscopic examination in capillaries of the frontal cortex and the hypothalamus revealed that there was homogeneous CF binding to the capillary endothelial cells in both areas of WKY (Fig. 2A, D), while no binding was detected with native ferritin (data not shown). The CF binding was mostly homogeneous, but partly sparse, in the frontal cortex and sparse in the hypothalamus of SHR (Fig. 2B, E). The CF binding to the endothelial cells was sparse in both areas of SHRSP (Fig. 2C, F). In quantitative analysis, the number of CF particles bound to the endothelial cells was significantly decreased in the frontal cortex of SHRSP and in the hypothalamus of SHR and SHRSP compared to those in WKY (Fig. 3). Electron microscopic examination in arterioles of both areas revealed that the reaction product of HRP was occasionally seen in the vesicular structures inside the endothelial cells in each strain. On the contrary, the extravasated reaction product was seen exclusively in arterioles of the hypothalamus of SHR and SHRSP, being localized in the vesicular structures such as abluminal pits of endothelial cells and within the basal lamina, whereas in WKY there were no vessels with increased vascular permeability. The percentage of arterioles showing increased vascular permeability was 20% (6 vessels showing increased vascular permeability/30 vessels examined, P<0.05) in SHRSP, 6.7% (2 vessels showing increased vascular permeability/30 vessels examined, P>0.05) in SHR, and 0% (0 vessel showing increased vascular permeability/30 vessels examined) in WKY. Extravascular deposition was distributed densely, but sporadically, in contact with specific endothelial cells. The CF binding to the endothelial cells was not changed and was homogenous in some arterioles showing an increased vascular permeability in SHR and SHRSP (Fig. 4B, C), while it was slightly sparse (Fig. 4D) or rare (Fig. 4E) in other arterioles showing increased vascular permeability in SHRSP. In addition, the CF binding disappeared in a few vessels, presumably venules, showing diffuse staining for HRP in the endothelial cytoplasm connected with the luminal membrane of a pit (Fig. 4F).
Light microscopic photographs showing the staining for horseradish peroxidase (HRP) with tetramethylbenzidine in Wistar Kyoto rats (WKY; A), spontaneously hypertensive rats (SHR; B), and stroke-prone SHR (SHRSP; C). The staining reaction for HRP is seen in anterior portions of the hypothalamus and parts of the amygdala and piriform cortex in SHR (B) and SHRSP (C), but is scarce in WKY (A). The areas indicated by arrows (A–C) were investigated using an electron microscope. Scale bars indicate 2 mm
Representative electron microscopic photographs of microvessels, showing capillary profiles in the frontal cortex (A–C) and the hypothalamus (D–F) of WKY (A, D), SHR (B, E), and SHRSP (C, F). The cationized ferritin (CF) binding to the endothelial cells in WKY is constant in both areas. The CF binding to the endothelial cells is mostly homogeneous, but partly sparse in the frontal cortex of SHR (B) and sparse in the hypothalamus of SHR (E). The CF binding to the endothelial cells is sparse in both areas of SHRSP (C, F). Scale bars indicate 200 nm
The mean thickness of CF particles bound to the endothelial luminal surface. The mean thickness in the hypothalamus is significantly less in SHR and SHRSP than in WKY, while the mean thickness in the frontal cortex is significantly less in SHRSP than in WKY. Values are means±SEM. * P<0.01, significantly different by the Mann-Whitney U-test compared with the corresponding value in WKY
Electron microscopic photographs of vessels in the hypothalamus of WKY (A), SHR (B), and SHRSP (C–F). No leakage of HRP is seen in arterioles of WKY, and CF binding to endothelial cells is uniformly observed (A). The reaction product for HRP is seen within the basal lamina (arrows in B) and in vesicular structures of the endothelial cytoplasm of SHR, while CF particles are uniformly observed (B). The reaction product of HRP is not seen in the junctional clefts of the endothelial cells (arrowhead in C) but in plasmalemmal vesicles, especially abluminal vesicles (arrowheads in D), of endothelial cells and within the basal lamina of arterioles (arrows in C–E) in SHRSP (C–E), indicating increased vascular permeability. The CF particles bound to the endothelial cells are uniformly observed (C), slightly sparse (D), or rare (arrowheads in E) in arterioles of SHRSP. The reaction product of HRP is diffusely seen in the cytoplasm (arrowheads in F) of the endothelial cells connected with the luminal membrane of a pit (double arrowhead in F), while the CF particles in this vessel, presumably a venule, have disappeared (F). Scale bars indicate 200 nm
Discussion
Light microscopic study revealed the staining reaction for HRP around vessels in anterior portions of the hypothalamus and parts of the basal forebrain, amygdala, and piriform cortex in SHR and SHRSP. In this study, we focused on the vascular permeability in the anterior portions of the hypothalamus, because the staining for HRP was observed strongly there.
Electron microscopic findings indicated that cerebrovascular permeability to HRP increased exclusively in arterioles of the hypothalamus in 3-month-old SHR and SHRSP. The CF binding to the capillary endothelial cells deteriorated not only in the hypothalamus of SHR and SHRSP, but also in the frontal cortex of SHRSP. Accordingly, it is likely that the endothelial dysfunction in capillaries had already occurred in widespread areas of 3-month-old SHRSP brains, while the endothelial dysfunction was not related directly to increased vascular permeability in young SHRSP. It is likely that the aggravation of endothelial dysfunction and increased vascular permeability of the arterioles may lead to hyaline and fibrinoid degeneration of the vessels in adult SHR and SHRSP (Amano 1977). The CF binding to endothelial cells was preserved in some arterioles, showing increased vascular permeability, in the hypothalamus of SHR and SHRSP (Fig. 4B–D), as was also observed in the hippocampus (Ueno et al., 2004). On the other hand, the number of CF particles bound to the endothelial cells was decreased in other leaky arterioles (Fig. 4E), as was not seen in the hippocampus. It is conceivable that the decreased CF binding to the endothelial cells of arterioles may be not closely related to increased vascular permeability and that the hypertensive state may induce the endothelial damage more remarkably in the hypothalamus than in the hippocampus.
The number of leaky arterioles showing staining for HRP within the basement membrane in SHRSP significantly increased compared with that in WKY. However, as the number of HRP-loaded vesicular structures in the arterioles was not calculated, the detailed mechanism of the vascular hyperpermeability in the endothelial cells has not yet been determined. It is well known, however, that enhanced vesicular transport appears to be a common response of the cerebral endothelium to a variety of stimuli (Cervos-Navarro et al. 1983). Caveolae-mediated transcytosis possibly contributes to vascular hyperpermeability (Pascariu et al. 2004; Simionescu et al. 1974; Stan 2002). On the other hand, the involvement of caveolae in the transcytosis of macromolecules was recently questioned by the caveolin knockout mouse model (Drab et al. 2001). Cationized ferritin binding to HRP-loaded vesicular structures was not found in the luminal membrane of endothelial cells (Fig. 4), although the binding to vesicular structures without HRP was occasionally seen in their luminal membranes (Fig. 2A). Accordingly, these findings do not necessarily suggest that the vascular hyperpermeability observed in this study results from increased caveolae-mediated transcytosis. Transport through junctional clefts of endothelial cells may contribute to increased vascular permeability; however, this was not observed in this study (Fig. 4C). The reaction product of HRP was seen not only within the basal lamina, but also occasionally in the abluminal pits of the endothelial cytoplasm of arterioles (Fig. 4D). Accordingly, it is likely that increased vascular permeability in the arterioles appears to be accounted for by enhanced vesicular transport. In addition, we found some venules showing diffuse staining of HRP in the endothelial cytoplasm without CF binding to its luminal membrane (Fig. 4F), as was not seen in the hippocampus of SHRSP (Ueno et al. 2004). The diffuse staining of HRP in the endothelial cytoplasm of venules was also seen in the hippocampus of aged senescence-accelerated mice (SAMP8; Ueno et al. 2001a) and in the corpus callosum of rats with chronic cerebral hypoperfusion (Ueno et al. 2002). It is likely that the diffuse leakage of intravascular macromolecules through endothelial cytoplasm with endothelial glycocalyx damage may occur in venules. However, future studies with another tracer are needed to confirm the diffuse leakage of macromolecules transendothelially. It remains unclear why the hypothalamic area appears to be especially susceptible to hypertension-induced hyperpermeability. It seems that the blood in this area is supplied by proximal portions of branching vessels of the major artery and accordingly the vessels in the hypothalamus may be under higher pressure than those in the others. It is conceivable that increased vascular permeability in arterioles and venules of the anterior hypothalamic area may affect norepinephrine release in this area (Carlson et al. 2001; Peng et al. 1995, 2003).
In the present study, alterations in the surface charge of the capillary endothelial cells were not necessarily related to increased vascular permeability. Nag (1984) reported that an increase in vascular permeability in acute hypertension was accompanied by a transient alteration in surface charge. The difference may result from the fact that the BBB damage at the early stage of chronic hypertension in this study was milder than that in the acute hypertensive state.
These results suggest that the chronic hypertensive state induces BBB disruption, and that endothelial glycocalyx is markedly damaged without a close relationship to BBB disruption in the hypothalamus at an early stage.
References
Amano S (1977) Vascular changes in the brain of spontaneously hypertensive rats: hyaline and fibrinoid degeneration. J Pathol 121:119–128
Amenta F, Di Tullio MA, Tomassoni D (2003) Arterial hypertension and brain damage: evidence from animal models (review). Clin Exp Hypertens 25:359–380
Carlson SH, Roysomutti S, Peng N, Wyss JM (2001) The role of the central nervous system in NaCl-sensitive hypertension in spontaneously hypertensive rats. Am J Hypertens 14:155–162
Cervos-Navarro J, Artigas J, Mrsulja BJ (1983) Morphofunctional aspects of the normal and pathological blood-brain barrier. Acta Neuropathol 8:1–19
Drab M, Verkade P, Elger M, Kasper M, Lohn M, Lauterbach B, Menne J, Lindschau C, Mende F, Luft FC, Schedl A, Haller H, Kurzchalia TV (2001) Loss of caveolae, vascular dysfunction, and pulmonary defects in caveolin-1 gene-disrupted mice. Science 293:2449–2452
Fredriksson K, Auer RN, Kalimo H, Nordborg C, Olsson Y, Johansson BB (1985) Cerebrovascular lesions in stroke-prone spontaneously hypertensive rats. Acta Neuropathol 68:284–294
Fredriksson K, Kalimo H, Westergren I, Kahrstrom J, Johansson BB (1987) Blood-brain barrier leakage and brain edema in the stroke-prone spontaneously hypertensive rats. Acta Neuropathol 74:259–268
Fredriksson K, Nordborg C, Kalimo H, Olsson Y, Johansson BB (1988a) Cerebral microangiopathy in stroke-prone spontaneously hypertensive rats. An immunohistochemical and ultrastructural study. Acta Neuropathol 75:241–252
Fredriksson K, Kalimo H, Nordborg C, Olsson Y, Johansson BB (1988b) Cyst formation and glial response in the brain lesions of stroke-prone spontaneously hypertensive rats. Acta Neuropathol 76:441–450
Fukushima M (1968) Histometric and histochemical studies of the hypothalamo-hypophyseal neurosecretory system of spontaneously hypertensive rats and rats with experimental hypertension. Jpn Circ J 32:485–516
Hachinski VC, Potter P, Merskey H (1987) Leuko-araiosis. Arch Neurol 44:21–23
Hazama F, Amano S, Haebara H, Okamoto K (1975) Changes in vascular permeability in the brain of stroke-prone spontaneously hypertensive rats studied with peroxidase as a tracer. Acta Pathol Jpn 25:565–574
Horn EM, Shonis CA, Holzwarth MA, Waldrop TG (1998) Decrease in glutamic acid decarboxylase level in the hypothalamus of spontaneously hypertensive rats. J Hypertens 16:625–633
Johansson BB (1980) The blood-brain barrier in acute and chronic hypertension. Adv Exp Med Biol 131:211–226
Knox CA, Yates RD, Chen I-L, Klara PM (1980) Effects of aging on the structural and permeability characteristics of cerebrovasculature in normotensive and hypertensive strains of rats. Acta Neuropathol 51:1–13
Kramer JM, Plowey ED, Beatty JA, Little HR, Waldrop TG (2000) Hypothalamus, hypertension, and exercise. Brain Res Bull 53:77–85
Lindner JR, Ismail S, Spotnitz WD, Skyba DM, Jayaweera AR, Kaul S (1998) Albumin microbubble persistence during myocardial contrast echocardiography is associated with microvascular endothelial glycocalyx damage. Circulation 98:2187–2194
Mesulam M-M (1978) Tetramethylbenzidine for horseradish peroxidase neurohistochemistry: a non-carcinogenic blue reaction-product with superior sensitivity for visualizing neural afferents and efferents. J Histochem Cytochem 26:106–117
Mueller SM (1982) The blood-brain barrier in young spontaneously hypertensive rats. Acta Neurol Scand 65:623–628
Nag S (1984) Cerebral endothelial surface charge in hypertension. Acta Neuropathol 63:276–281
Ogata J, Fujishima M, Tamaki K, Nakatomi Y, Ishitsuka T, Omae T (1981) Vascular changes underlying cerebral lesions in stroke-prone spontaneously hypertensive rats. Acta Neuropathol 54:183–188
Okamoto K, Aoki K (1963) Development of a strain of spontaneously hypertensive rats. Jpn Circ J 27:282–293
Okamoto K, Yamori Y, Nagaoka A (1974) Establishment of the stroke-prone spontaneously hypertensive rat (SHR). Circ Res 34:143–153
O’Sullivan C, Duggan J, Lyons S, Thornton J, Lee M, O’Brien E (2003) Hypertensive target-organ damage in the very elderly. Hypertension 42:130–135
Parnetti L, Mari D, Mecocci P, Senin U (1994) Pathogenetic mechanisms in vascular dementia. Int J Clin Lab Res 24:15–22
Pascariu M, Bendayan M, Ghitescu L (2004) Correlated endothelial caveolin overexpression and increased transcytosis in experimental diabetes. J Histochem Cytochem 52:65–76
Peng N, Meng QC, King K, Oparil S, Wyss JM (1995) Acute hypertension increases norepinephrine release in the anterior hypothalamic area. Hypertension 25:828–833
Peng N, Clark JT, Wei CC, Wyss JM (2003) Estrogen depletion increases blood pressure and hypothalamic norepinephrine in middle-aged spontaneously hypertensive rats. Hypertension 41:1164–1167
Reese TS, Karnovsky MJ (1967) Fine structural localization of blood-brain barrier to exogenous peroxidase. J Cell Biol 34:207–217
Roman GC (1996) From UBOs to Binswanger’s disease: impact of magnetic resonance imaging on vascular dementia research. Stroke 27:1269–1273
Sabbatini M, Strocchi P, Vitaioli L, Amenta F (2000) The hippocampus in spontaneously hypertensive rats: a quantitative microanatomical study. Neuroscience 100:251–258
Sabbatini M, Catalani A, Consoli C, Marletta N, Tomassoni D, Avola R (2002) The hippocampus in spontaneously hypertensive rats: an animal model of vascular dementia. Mech Ageing Dev 123:547–559
Simionescu M, Simionescu N, Palade GE (1974) Morphometric data on the endothelium of blood capillaries. J Cell Biol 60:128–152
Stan R-V (2002) Structure and function of endothelial caveolae. Microsc Res Tech 57:350–364
Thurauf N, Dermietzel R, Kalweit P (1983) Surface charges associated with fenestrated brain capillaries. I. In vitro labeling of anionic sites. J Ultrastruct Res 84:103–110
Ueno M, Akiguchi I, Hosokawa M, Kotani H, Kanenishi K, Sakamoto H (2000) Blood-brain barrier permeability in the periventricular areas of the normal mouse brain. Acta Neuropathol 99:385–392
Ueno M, Sakamoto H, Kanenishi K, Onodera M, Akiguchi I, Hosokawa M (2001a) Ultrastructural and permeability features of microvessels in the hippocampus, cerebellum and pons of senescence-accelerated mice (SAM). Neurobiol Aging 22:469–478
Ueno M, Sakamoto H, Kanenishi K, Onodera M, Akiguchi I, Hosokawa M (2001b) Ultrastructural and permeability features of microvessels in the periventricular area of senescence-accelerated mice (SAM). Microsc Res Tech 53:232–238
Ueno M, Tomimoto H, Akiguchi I, Wakita H, Sakamoto H (2002) Blood-brain barrier disruption in white matter lesions in a rat model of chronic cerebral hypoperfusion. J Cereb Blood Flow Metab 22:97–104
Ueno M, Sakamoto H, Tomimoto H, Akiguchi I, Onodera M, Huang CL, Kanenishi K (2004) Blood-brain barrier is impaired in the hippocampus of young adult spontaneously hypertensive rats. Acta Neuropathol 107:532-538
Vorbrodt AW, Lossinsky AS, Dobrogowska DH, Wisniewski HM (1986) Distribution of anionic sites and glycoconjugates on the endothelial surfaces of the developing blood-brain barrier. Dev Brain Res 29:69–79
Wallin A, Blennow K (1993) Heterogeneity of vascular dementia: mechanisms and subgroups. J Geriatr Psychiatr Neurol 6:177–188
Wardlaw JM, Sandercock PAG, Dennia MS, Starr J (2003) Is breakdown of the blood-brain barrier responsible for lacunar stroke, leukoaraiosis, and dementia? Stroke 34:806–812
Yamori Y, Okamoto K (1969) Hypothalamic tonic regulation of blood pressure in spontaneously hypertensive rats. Jpn Circ J 33:509–519
Yamori Y, Horie R, Sato M, Sasagawa S, Okamoto K (1975) Experimental studies on the pathogenesis and prophylaxis of stroke-prone spontaneously hypertensive rats (SHR). 1. Quantitative estimation of cerebrovascular permeability. Jpn Circ J 39:611–615
Acknowledgements
This research was supported by a Budget from the Ministry of Education, Culture, Sports, Science and Technology, Japan. The authors thank Ms C. Ishikawa and Ms Y. Fujiwara for technical and editorial assistance.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ueno, M., Sakamoto, H., Liao, YJ. et al. Blood-brain barrier disruption in the hypothalamus of young adult spontaneously hypertensive rats. Histochem Cell Biol 122, 131–137 (2004). https://doi.org/10.1007/s00418-004-0684-y
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00418-004-0684-y