Abstract
Stabilin-2, the hepatic hyaluronan receptor, has recently been cloned by us. Together with stabilin-1, stabilin-2 constitutes a novel family of fasciclin-like hyaluronan receptor homologues. Here, we analyzed expression of stabilin-2 (mStab-2) in a broad array of C57BL/6 mouse organs and tissues. While northern blot analysis showed positive expression of mStab-2 mRNA confined to liver and spleen, immunohistochemistry demonstrated mStab-2 protein expression in the endothelial sinuses of liver, lymph nodes, spleen, and bone marrow, and in specialized structures of eye, heart, brain, and kidney. Expression of mStab-2 was detected in corneal and lens epithelium, in mesenchymal cells of the heart valves, in the ependymal cells lining the ventricles in the brain, and in the prismatic epithelial cells covering the renal papillae. In pathological conditions, such as tumor growth or wound healing processes, mStab-2 was not expressed in the newly formed vasculature or other tissue components. Based on these results, we suggest that mStab-2 might be involved in the clearance of hyaluronan from the lymph or the blood circulation via the network of endothelial sinuses. At the other mStab-2-positive tissues sites that are either avascular and/or demarcate a solid/liquid interface, mStab-2 may serve to maintain tissue integrity by supporting extracellular matrix turnover or it may contribute to maintaining fluidity of bodily liquids by resorption of hyaluronan.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Stabilin-1 and -2 represent a novel family of high molecular weight transmembrane proteins, recently cloned by us in both human and mice. The stabilin genes code for homologous proteins featuring seven fasciclin-like adhesion domains, 18–20 epidermal growth factor domains, one X-link domain, and three to six B-(X7)-B hyaluronan (HA)-binding motifs (Politz et al. 2002). Stabilin-1 was first identified by monoclonal antibody MS-1 (Goerdt et al. 1991) and was shown to be expressed by sinusoidal endothelial cells in human spleen and liver as well as by non-continuous and angiogenic endothelial cells in wound healing processes and malignant tumors, and by alternatively activated macrophages (Goerdt et al. 1993).
Stabilin-2 was purified from rat hepatic sinusoidal endothelial cells as an HA-binding protein which functions as an endocytic receptor clearing the blood from the large amounts of HA released during steady state tissue remodeling (McCourt et al. 1999; Politz et al. 2002). HA is a non-sulfated member of the glycosaminoglycan family of polysaccharides (Laurent and Fraser 1992), and was first isolated and described as the mucus of the vitreous body of the eye (Meyer and Palmer 1934). HA is widely distributed throughout the extracellular matrix (ECM), and it has some general biological functions as an extracellular filling material and lubricant, as well as more specific effects including migration, differentiation, and phagocytosis (Turley 1992; Knudson and Knudson 1993; Toole 1997). HA is important in development (Gakunga et al. 1997; Camenisch et al. 2000), angiogenesis (West et al. 1985; Deed et al. 1997), wound healing (Chen and Abatangelo 1999), and tumor growth and metastasis (Rooney et al. 1995; Toole 2002).
The presence of human stabilin-2 has been demonstrated on the mRNA level in organs such as liver, spleen, and lymph nodes (Politz et al. 2002). In addition, the presence of an HA-binding protein corresponding to stabilin-2 was demonstrated in rat liver, spleen, and lymph nodes by the use of a monoclonal antibody (Weigel et al. 2003). Our study was motivated by the fact that the distribution of stabilin-2 in the mouse, the most frequently used laboratory animal, is unknown, and more importantly, that expression of this protein in tissues other than liver, spleen, and lymph nodes has not yet been thoroughly analyzed. By the use of a novel peptide antibody toward the carboxyl terminal part of mouse stabilin-2 (mStab-2), we performed an immunohistochemical study of mStab-2 protein expression in a broad range of tissues of the C57BL/6 mouse.
Materials and methods
Mice
Specific pathogen-free C57BL/6 female mice about 8–10 weeks of age were purchased from Harlan, UK. Mice were housed under conventional conditions. The experimental protocols were approved by the German Ethics Committee for Research on Animals.
Cells
The murine melanoma cell line B16F1 was obtained from American Type Culture Collection (Rockville, MD, USA). The cells were cultured in Dulbecco’s modified Eagle’s medium (Sigma, Taufkirchen, Germany) supplemented with 10% fetal calf serum, 100 U/ml penicillin, 100 μg/ml streptomycin, and 2 mM glutamine in a humidified atmosphere of 5% CO2 at 37°C and passaged twice a week.
Animal protocols
The animals were deeply anesthetized by inhalation of ethyl ether. A long incision on the abdominal region was made through the skin and musculature. The intestines were retracted to expose the superior mesenteric vein, which was cut. Brain, eyes, lymph nodes, lungs, liver, heart, thymus, thyroid gland, stomach, small intestine, spleen, kidneys, pancreas, adrenal glands, skeletal muscles, bone marrow, ovary, tail, and skin were removed, embedded in OCT compound (Sakura Finetek Europe, Zoeterwounde, The Netherlands), and snap-frozen in liquid nitrogen. All tissues were stored at −80°C until further use.
For the wound healing model, 15 mice were anesthetized by injection of intraperitoneal Rompun/Hostaket (16 mg/kg and 120 mg/kg, respectively), the skin on the neck was shaved, and one excisional dermal wound on every mouse neck was made using a 4-mm biopsy punch (Stiefel Laboratorium, Offenbach am Main, Germany). At day 3, 5, 7, 9, and 12, three mice each were killed and the wounded skin was removed. For induction of intradermal tumors, B16F1 cells were harvested by a brief trypsinization (0.25% trypsin/0.02% EDTA), washed three times, and resuspended in Dulbecco’s modified Eagle’s medium at a density of 1×107 cells/ml. The suspension of tumor cells was kept on ice for a maximum of 60 min before inoculation, and was warmed to room temperature just before administration. Nine animals received a single injection of 5×105 viable tumor cells intradermal in the abdomen. At day 5, 10, and 15, three mice each were killed and the tumors were removed. The wounded skin and tumor samples were embedded in OCT compound and snap-frozen in liquid nitrogen. The experiments were repeated twice.
Anti-mouse stabilin-2 antibody production
The peptide TNPLYETSTPAAPEPSCDPFTDSGERELE representing amino acids 2521–2549 of mStab-2 (accession number AF364951) was synthesized and coupled to carrier protein (KLH). The coupled protein was mixed with Freund’s complete adjuvant (Sigma) and used to immunize a rabbit. The injections were repeated three times in a biweekly period. Finally, approximately 100 ml serum and 4 ml preimmune serum were collected. The crude serum was used as polyclonal mStab-2 antibody. All services were performed by Peptide Speciality Laboratories (PSL), Heidelberg, Germany.
To confirm the specificity of the anti-mStab-2 peptide antibody, a blocking experiment was performed by incubating a 1:1,000 dilution of the respective antibody 1:1 with a 10 μg/ml dilution of the purified mStab-2 peptide (PSL) for 30–45 min followed by immunohistochemistry on mouse spleen as described below.
Immunohistochemistry
Cryostat sections (7 μm) were air dried, acetone fixed at −20°C for 10 min, and stained using EnVision+System, Peroxidase AEC kit (Dako, Carpinteria, CA, USA). Sections were pretreated with a solution of 0.03% hydrogen peroxide containing 2% sodium azide to inhibit endogenous peroxidase activity, incubated sequentially with polyclonal mStab-2 peptide antibody at a dilution of 1:500 and 1:1,000, and with peroxidase-labeled polymer conjugated to a goat anti-rabbit antibody in TRIS-HCl buffer for 30 min each step in a humidified chamber at room temperature; at least three PBS washes were performed between the single steps. Sections were developed with 3-amino-9-ethylcarbazole containing hydrogen peroxide, counterstained with hematoxylin (Merck, Darmstadt, Germany), mounted with Aqueous Mounting Medium (Dako), and immediately analyzed. Images were captured using a Leica DCRE microscope with Leica DC500 camera and Leica IM50 Image Manager software (Leica Microsystems, Wetzlar, Germany).
Parallel to staining with the mStab-2 peptide antibody, wounded skin samples and melanomas were stained with primary rat anti-mouse CD31 (PECAM-1) monoclonal antibody (BD Pharmingen, Heidelberg, Germany) and secondary goat anti-rat IgG, horseradish peroxidase linked whole antibody (Amersham Biosciences Europe, Freiburg, Germany) to detect the blood vasculature.
Northern blot analysis
Mouse Northern LIGTH blots (Panomics, Redwood City, CA, USA) were used for investigation of gene expression. The blot contained 2 μg purified mRNA from brain, heart, liver, lungs, spleen, stomach, testis, and skeletal muscles. A mStab-2-specific probe was PCR generated using the primers mStab-2, 951 forward (5′ CTG CCA AAC CAG CTA TGG AAA C 3′) and mStab-2, 1965 reverse (5′ ACG TTG TTT GCC AGA ATC TGC C 3′). The PCR product was purified (Mini Elute PCR purification kit; Qiagen, Hilden, Germany) and labeled with α32P-dCTP (Amersham Biosciences Europe). The membrane was hybridized in Express-Hyb solution (BD Biosciences Clontech, Heidelberg, Germany) at high stringency (65°C) for 4 h. After hybridization the membrane was washed twice at 65°C for 20 min in 2×SSC/0.5% SDS and in 0.2×SSC/0.5% SDS, respectively. The membrane was exposed to BioMax MR films (Eastman Kodak, Rochester, NY, USA) for a period of 7 days at −80°C.
Results
Expression of mStab-2 mRNA in mouse tissues
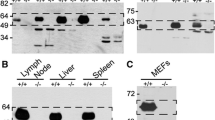
In order to establish overall similarity of mStab-2 mRNA expression in mouse tissues as compared to human and rat, northern blotting was done using a specific mStab-2 probe and a β-actin probe as a loading control. As expected, a strong 8-kb mRNA band was detected in liver and spleen (Fig. 1).
Tissue distribution of mStab-2 protein
Immunohistochemistry using the mStab-2 peptide antibody, preimmune serum as a control was carried out on a wide range of mouse organs and tissues including brain, eyes, lymph nodes, liver, lungs, heart, thymus, thyroid gland, stomach, small intestine, spleen, kidneys, pancreas, adrenal glands, skeletal muscles, bone marrow, ovary, tail, and skin. mStab-2 protein expression was noticed in special structures in liver, lymph nodes, spleen, bone marrow, eyes, heart, brain, and kidneys, whereas all other tissues tested were negative (Table 1).
In order to confirm the specificity of the anti-mStab-2 peptide antibody, preadsorption was performed using the immunogenic peptide, which resulted in blocking of mStab-2 staining in the spleen (Fig. 2). In addition to normal mouse organs, wound healing tissue and melanoma metastases were also analyzed; blood vessels in both types of specimens were shown to be negative for mStab-2, but positive for the endothelial cell marker CD31 (results not shown).
Blocking of mStab-2 antibody staining by preadsorption. Mouse spleen was stained by using either a 1:1,000 dilution of mStab-2 peptide antibody (A), a 1:1,000 dilution of mStab-2 antibody preadsorbed with the same quantity of a 10 μg/ml dilution of the immunogenic mstab-2 peptide (B), or a 1:1,000 dilution of the preimmune serum (C). Scale bars indicate 100 μm
mStab-2 protein expression in organs with endothelial sinuses
Expression of mStab-2 protein was predominantly found in organs with endothelial sinuses such as liver, lymph node, spleen, and bone marrow (Table 1). In the liver, mStab-2 was strongly expressed in flat, elongated hepatic endothelial cells lining the sinuses (Fig. 3A). In mouse lymph nodes, expression of mStab-2 protein was detected in lymphatic endothelial cells lining the subcapsular/marginal sinuses as well as the intermediate and medullary sinuses (Fig. 3C). In the spleen, mStab-2 was strongly and specifically present in the sinusoidal endothelium of the red pulp (Fig. 3E, F). Weak staining was also observed in the marginal sinus endothelium (Fig. 3E, F). The normal endothelial vessels, for example the central arteries of the white pulp, were negative for mStab-2 antibody staining (Fig. 3E, F). Similarly, mStab-2 antibody detected a system of sinusoidal vascular structures in mouse bone marrow (Fig. 3G).
mStab-2 expression in organs with endothelial sinuses. Liver (A, B), lymph node (C, D), spleen (E, F), and bone marrow (G, H) tissue sections were labeled with a novel mStab-2 peptide antibody (A, C, E–G) or preimmune serum as a control (B, D, H), using immunoperoxidase (red reaction product) and hematoxylin as a counterstain (blue). In the liver, strong expression of mStab-2 protein (red) is seen in the flat, elongated hepatic endothelial cells lining the sinuses (A). In mouse lymph nodes, mStab-2 protein was detected in the lymphatic endothelial cells lining the subcapsular/marginal sinuses as well as the intermediate and medullary sinuses (C). Strong and specific expression of mStab-2 protein was present in the sinusoidal endothelium of the red pulp in mouse spleen, while the normal endothelial vessels were negative (E, F). Sinusoidal vascular structures in mouse bone marrow were also detected by mStab-2 antibody (G). Scale bars indicate 100 μm (A, C, D, F, H) and 200 μm (B, E, G)
mStab-2 protein expression in avascular tissues and in tissues with a solid/liquid interface
Distribution of mStab-2 was also found in avascular tissues known to be rich in HA and/or proteoglycans (Table 1). In the eye, expression of mStab-2 was found on the outer surface of the cornea which consists of stratified squamous epithelium (Fig. 4A), and in the anterior part of the lens which is covered by a single layer of cuboidal epithelium (results not shown). In the heart, mStab-2 expression was restricted to mesenchymal cells in the avascular heart valves (Fig. 4C). Regarding solid/liquid interfaces, strong mStab-2 expression was found in the ependymal cells lining the ventricles of the brain, whereas the ependymal cells of the choroid plexuses were less intensely stained (Fig. 4E). In the kidney, the single layer of cuboidal epithelial cells covering the renal papillae was strongly stained by mStab-2 antibody, while the transitional multilayered epithelium of the ureter was not stained (Fig. 4G, H).
mStab-2 protein expression in avascular tissues and tissues with a solid/liquid interface. Cornea (A, B), heart valve (C, D), brain (E, F), and kidney (G, H) tissue sections were labeled with a novel mStab-2 peptide antibody (A, C, E, G, H) or preimmune serum as a control (B, D, F) using immunoperoxidase (red reaction product) and hematoxylin as a counterstain (blue). Strong expression of mStab-2 was found on the outer surface of the cornea, which consists of stratified squamous epithelium (A), in mesenchymal cells of the heart valve (C), in ependymal cells lining the ventricles of the mouse brain (E), and in the single layer of cuboidal epithelial cells covering the renal papillae in the kidney (G, H). Scale bars indicate 100 μm (A–F, H) and 250 μm (G)
Discussion
In this study we sought to gain a closer insight into the function of mStab-2 by studying its pattern of expression. Using a novel mStab-2 peptide antibody specifically recognizing the C-terminus of mStab-2, a histological analysis of a wide range of mouse tissues was performed. Staining of mStab-2 was detected in organs with predominant endothelial sinuses such as liver, lymph nodes, spleen, and bone marrow. In addition, mStab-2 was observed in specialized cells in the eye, heart, brain, and kidney. In contrast to liver and spleen however, immunohistochemical results obtained in these latter tissues could not be confirmed by northern blotting of whole tissue extracts due to the fact that the percentage of these specialized endothelial/epithelial cells is too small to be detectable by such a crude approach.
mStab-2 was identified in rat hepatic sinusoidal endothelial cells as an HA-binding protein (McCourt et al. 1999). The largest concentrations of HA are found within the skin and musculoskeletal system (>50% of a total body HA), and this is also the tissue site where ECM turnover leads to local liberation of HA (Laurent and Fraser 1992). In contrast, degradation of HA does not occur locally, but within the regional lymph nodes, where approximately 90% of HA is degraded by sinusoidal endothelial cells and macrophages (Fraser et al 1988; Fraser and Laurent 1989). There is some evidence that a minor portion of HA is taken up on its way to the lymph nodes by the endothelial cells of the lymphatic vessels. In this process, lymphatic vessel endothelial HA receptor-1 (LYVE-1) may be involved (Prevo et al. 2001). In contrast to LYVE-1, we show here that stabilin-2 is not expressed in lymphatic endothelial cells outside the lymph nodes indicating that these latter cells differ from lymph node sinusoidal endothelia. Furthermore, strong expression of mStab-2 in the endothelial cells of the lymph node sinus network in contrast to the lymph node blood vascular endothelium indicates that the HA clearance function of the lymph nodes is specific to the sinusoidal endothelium. HA (10–15%) not metabolized in the lymph nodes exits via the efferent lymphatics to the blood vasculature, where it is rapidly removed by the liver, spleen, and bone marrow (Fraser et al. 1981, 1983, 1986). Removal of HA from the blood stream is crucial for maintaining the blood at an acceptable viscosity; in this respect, the clearance function of hepatic sinusoidal endothelium has long been established (Eriksson et al. 1983; Smedsrød et al. 1984; Laurent et al. 1986).
It has previously been claimed that mouse spleen lacks endothelial sinuses (Snook 1950). In contrast to this, we show here strong expression of mStab-2 in splenic red pulp sinusoidal endothelium and weak expression in marginal sinus endothelium, whereas mStab-2 is negative in normal endothelial cells of other splenic blood vessels. This finding demonstrates the existence of sinuses also in mouse spleen. Our results thus confirm the study of Balazs et al. (2001) who for the first time reported morphological evidence for the occurrence of sinuses in postnatal mouse spleen.
In this study, we also demonstrate for the first time the expression of mStab-2 in the venous sinusoids of the bone marrow. Mouse bone marrow consists of a meshwork of vascular sinuses in which the endothelium forms a continuous layer, whereas the basement membrane is discontinuous and creates an essential element of the bone marrow–blood barrier (Inoue and Osmond 2001). The bone marrow–blood barrier is important in regulating the exit of stem cell-derived peripheral blood cells to the circulation (Petrides and Dittmann 1990).
In this study, we also demonstrate partially overlapping expression of mStab-2 in avascular tissues such as cornea, lens, and heart valves as well as in tissues with a solid/liquid interface such as cornea, lens, ependymal cells, and renal papillae. In addition to HA, stabilin-2 has been shown to bind and clear proteoglycans such as chondroitin sulfate proteoglycan, and serglycin from the circulation (Smedsrød et al. 1985; Øynebråten et al. 2000). HA and proteoglycans are highly expressed in ocular tissues, where they, for example, contribute to the stromal transparency of the cornea (Tanihara et al. 2002). The cornea consists of a stromal layer, which is covered at its external surface by epithelium in contact with tear fluid, and at its inner surface by an endothelium in contact with aqueous fluid in the anterior chamber. HA has been ultrastructurally histolocalized to both epithelium and endothelium, as well as to corneal stroma in the rat and human cornea (Eggli and Graber 1993; Lerner et al. 1998). Regarding the lens, chondroitin sulfate proteoglycan has been shown to be expressed during the early stages of morphogenesis. During this processes, it supports epithelial invagination and fusion leading to lens vesicle formation (Gato et al. 2001). HA and lumican, a keratan sulfate proteoglycan core protein, have been shown to be expressed by quiescent and proliferating mouse and human lens epithelial cells; both molecules may be involved in the epithelial–mesenchymal transition process of lens epithelial cells and in the development of posterior capsule opacification after injury (Saika et al. 1998, 2003). As both cornea and lens lack a direct blood supply and are located at a solid/liquid interface, stabilin-2 may play a role in stabilizing the preocular tear film as well as in regulating hydration of corneal epithelium and it may support ECM turnover by clearing the anterior chamber from macromolecular waste.
Similar to cornea and lens, the heart valves represent another type of avascular tissue. The heart valves are composed of fibroelastic tissue and covered by flat endothelium. The formation of functional valves from the embryonic endocardial cushions involves a series of morphologic events that includes epithelial–mesenchymal transformation, cushion cellularization and fusion, cell differentiation, and valve-leaflet remodeling. There is evidence that HA is required for heart valve morphogenesis by contributing to the formation of the acellular ECM (cardiac jelly), which facilitates migration of the cells of the endocardium and promotes prevalvular mesenchyme transformation (Camenisch et al. 2000; Walsh and Stainier 2001). In the developing mouse heart, the chondroitin sulfate proteoglycan versican is also associated with valvulogenesis (Henderson and Copp 1998). The formation of the HA/versican-rich pericellular matrix has also been shown to be important in the proliferation and migration of human aortic smooth muscle cells in vitro (Evanko et al. 1999). Since cardiac expression of mStab-2 was restricted to mesenchymal cells in the avascular heart valves, it may also play a crucial role in maintaining tissue integrity by supporting ECM metabolism.
Ependymal cells form a liquid/solid barrier lining the ventricles and the central canal of the spinal cord, forming a sheet of cuboidal cells which are in direct contact with the cerebrospinal fluid. Many of these cells are ciliated, and they are responsible for the propulsion of the cerebrospinal fluid (CSF) from the ventricles to the subarachnoid space. In addition, ependymal cells serve to protect the neural tissue from potentially harmful CSF substances (Bruni 1998). In addition to cilia, these ependymal cells have apical microvilli which may have absorptive and secretory functions. HA is present in CSF on a steady state level, and its concentration significantly increases after head injury and in various diseases such as meningitis, brain cysts, and cerebral tumor metastasis (Burke et al. 1994; Laurent et al. 1996). Strong expression of mStab-2 protein in ependymal cells lining the ventricles of mouse brain may indicate a crucial role for this scavenger receptor in maintaining the fluidity of CSF.
During mammalian kidney development, the collecting system arises by branching morphogenesis of the ureteric bud (UB) and reciprocal interactions between the UB and the metanephric mesenchyme (Lechner and Dressler 1997; al-Awqati and Goldberg 1998; Pohl et al. 2000b). There is evidence that HA, hyaluronidase, and CD44, another important cell surface receptor for HA, are involved in epithelial branching morphogenesis of UB cells in vitro (Pohl et al. 2000a). The highest concentrations of HA in healthy mammalian kidneys were found in the inner medulla of the renal papilla (Farber and van Praag 1970; Kresse and Grossmann 1970; Pitcock et al. 1988; Wells et al. 1990). In this location, HA is believed to provide mechanical support for tubules and blood vessels. Due to its unique water-binding capacity, it may furthermore influence the water transport within the inner medulla and maintain the necessary concentration gradient (Hansell et al. 1999; Knepper et al. 2003). Degradation of HA in the kidney mainly occurs in the urine, under the physiological control of an acid-active hyaluronidase (Csoka et al. 1997, 2001). In the kidney, the single layer of cuboidal epithelial cells covering the renal papillae was strongly stained by mStab-2 antibody, while the transitional multilayered epithelium of the ureter was not stained suggesting that mStab-2 may contribute to maintaining urine fluidity by resorption of HA.
In summary, we have shown that mStab-2 is constitutively expressed in tissues with predominant endothelial sinuses, such as liver, lymph nodes, spleen, and bone marrow, where it may been involved in clearance of HA from the lymphatic and blood vascular circulation. At the other mStab-2-positive tissue sites that are either avascular (cornea, lens, heart valves) and/or demarcate a solid/liquid interface (cornea, lens, brain-liquor barrier, renal papillae), stabilin-2 may serve to maintain tissue integrity by supporting ECM turnover or it may contribute to maintaining fluidity of bodily liquids by resorption of HA and other macromolecular waste molecules by endocytosis.
References
al-Awqati Q, Goldberg MR (1998) Architectural patterns in branching morphogenesis in the kidney. Kidney Int 54:1832–1842
Balazs M, Horvath G, Grama L, Balogh P (2001) Phenotypic identification and development of distinct microvascular compartments in the postnatal mouse spleen. Cell Immunol 212:126–137
Bruni JE (1998) Ependymal development, proliferation, and functions: a review. Microsc Res Tech 41:2–13
Burke EJ, Mehlhorn U, Allen SJ (1994) Hyaluronan in cerebrospinal fluid after head injury. Acta Neurol 16:103–109
Camenisch TD, Spicer AP, Brehm-Gibson T, Biesterfeldt J, Augustine ML, Calabro A Jr, Kubalak S, Klewer SE, McDonald JA (2000) Disruption of hyaluronan synthase-2 abrogates normal cardiac morphogenesis and hyaluronan-mediated transformation of epithelium to mesenchyme. J Clin Invest 106:349–360
Chen WY, Abatangelo G (1999) Functions of hyaluronan in wound repair. Wound Repair Regen 7:79–89
Csoka TB, Frost GI, Wong T, Stern R (1997) Purification and microsequencing of hyaluronidase isozymes from human urine. FEBS Lett 417:307–310
Csoka AB, Frost GI, Stern R (2001) The six hyaluronidase-like genes in the human and mouse genomes. Matrix Biol 20:499–508
Deed R, Rooney P, Kumar P, Norton JD, Smith J, Freemont AJ, Kumar S (1997) Early-response gene signalling is induced by angiogenic oligosaccharides of hyaluronan in endothelial cells. Inhibition by non-angiogenic, high-molecular-weight hyaluronan. Int J Cancer 71:251–256
Eggli PS, Graber W (1993) Ultrastructural distribution of hyaluronan in rat cornea. Exp Eye Res 56:693–699
Eriksson S, Fraser JR, Laurent TC, Pertoft H, Smedsrød B (1983) Endothelial cells are a site of uptake and degradation of hyaluronic acid in the liver. Exp Cell Res 144:223–228
Evanko SP, Angello JC, Wight TN (1999) Formation of hyaluronan- and versican-rich pericellular matrix is required for proliferation and migration of vascular smooth muscle cells. Arterioscler Thromb Vasc Biol 19:1004–1013
Farber SJ, van Praag D (1970) Composition of glycosaminoglycans (mucopolysaccharides) in rabbit renal papillae. Biochim Biophys Acta 208:219–226
Fraser JR, Laurent TC (1989) Turnover and metabolism of hyaluronan. Ciba Found Symp 143:41–59
Fraser JR, Laurent TC, Pertoft H, Baxter E (1981) Plasma clearance, tissue distribution and metabolism of hyaluronic acid injected intravenously in the rabbit. Biochem J 200:415–424
Fraser JR, Appelgren LE, Laurent TC (1983) Tissue uptake of circulating hyaluronic acid. A whole body autoradiographic study. Cell Tissue Res 233:285–293
Fraser JR, Engstrom-Laurent A, Nyberg A, Laurent TC (1986) Removal of hyaluronic acid from the circulation in rheumatoid disease and primary biliary cirrhosis. J Lab Clin Med 107:79–85
Fraser JR, Kimpton WG, Laurent TC, Cahill RN, Vakakis N (1988) Uptake and degradation of hyaluronan in lymphatic tissue. Biochem J 256:153–158
Gakunga P, Frost G, Shuster S, Cunha G, Formby B, Stern R (1997) Hyaluronan is a prerequisite for ductal branching morphogenesis. Development 124:3987–3997
Gato A, Martin C, Alonso MI, Martinez-Alvarez C, Moro JA (2001) Chondroitin sulphate proteoglycan is involved in lens vesicle morphogenesis in chick embryos. Exp Eye Res 73:469–478
Goerdt S, Walsh LJ, Murphy GF, Pober JS (1991) Identification of a novel high molecular weight protein preferentially expressed by sinusoidal endothelial cells in normal human tissues. J Cell Biol 113:1425–1437
Goerdt S, Bhardwaj R, Sorg C (1993) Inducible expression of MS-1 high-molecular-weight protein by endothelial cells of continuous origin and by dendritic cells/macrophages in vivo and in vitro. Am J Pathol 142:1409–1422
Hansell P, Maric C, Alcorn D, Goransson V, Johnsson C, Hallgren R (1999) Renomedullary interstitial cells regulate hyaluronan turnover depending on growth media osmolality suggesting a role in renal water handling. Acta Physiol Scand 165:115–116
Henderson DJ, Copp AJ (1998) Versican expression is associated with chamber specification, septation, and valvulogenesis in the developing mouse heart. Circ Res 83:523–322
Inoue S, Osmond DG (2001) Basement membrane of mouse bone marrow sinusoids shows distinctive structure and proteoglycan composition: a high resolution ultrastructural study. Anat Rec 264:294–304
Knepper MA, Saidel GM, Hascall VC, Dwyer T (2003) Concentration of solutes in the renal inner medulla: interstitial hyaluronan as a mechano-osmotic transducer. Am J Physiol Renal Physiol 284:433–446
Knudson CB, Knudson W (1993) Hyaluronan-binding proteins in development, tissue homeostasis, and disease. FASEB J 7:1233–1241
Kresse H, Grossmann A (1970) Comparative study of the mucopolysaccharide and collagen content in different topographical zones of the kidney of rat, dog and pig. Z Klin Chem Klin Biochem 8:420–424
Laurent TC, Fraser JR (1992) Hyaluronan. FASEB J 6:2397–2404
Laurent TC, Fraser JR, Pertoft H, Smedsrød B (1986) Removal of hyaluronic acid from the circulation in rheumatoid disease and primary biliary cirrhosis. J Lab Clin Med 107:79–85
Laurent TC, Laurent UB, Fraser JR (1996) The structure and function of hyaluronan: An overview. Immunol Cell Biol 74:1–7
Lechner MS, Dressler GR (1997) The molecular basis of embryonic kidney development. Mech Dev 2:105–120
Lerner LE, Schwartz DM, Hwang DG, Howes EL, Stern R (1998) Hyaluronan and CD44 in the human cornea and limbal conjunctiva. Exp Eye Res 67:481–484
McCourt PA, Smedsrød B, Melkko J, Johansson S (1999) Characterization of a hyaluronan receptor on rat sinusoidal liver endothelial cells and its functional relationship to scavenger receptors. Hepatology 30:1276–1286
Meyer K, Palmer JW (1934) The polysaccharide of the vitreous humor. J Biol Chem 107:629–634
Øynebråten I, Hansen B, Smedsrød B, Uhlin-Hansen L (2000) Serglycin secreted by leukocytes is efficiently eliminated from the circulation by sinusoidal scavenger endothelial cells in the liver. J Leukoc Biol 67:183–188
Petrides PE, Dittmann KH (1990) How do normal and leukemic white blood cells egress from the bone marrow? Morphological facts and biochemical riddles. Blut 61:3–13
Pitcock JA, Lyons H, Brown PS, Rightsel WA, Muirhead EE (1988) Glycosaminoglycans of the rat renomedullary interstitium: ultrastructural and biochemical observations. Exp Mol Pathol 49:373–387
Pohl M, Sakurai H, Stuart RO, Nigam SK (2000a) Role of hyaluronan and CD44 in in vitro branching morphogenesis of ureteric bud cells. Dev Biol 224:312–325
Pohl M, Stuart RO, Sakurai H, Nigam SK (2000b) Branching morphogenesis during kidney development. Annu Rev Physiol 62:595–620
Politz O, Gratchev A, McCourt PA, Schledzewski K, Guillot P, Johansson S, Svineng G, Franke P, Kannicht C, Kzhyshkowska J, Longati P, Velten FW, Johansson S, Goerdt S (2002) Stabilin-1 and -2 constitute a novel family of fasciclin-like hyaluronan receptor homologues. Biochem J 362:155–164
Prevo R, Banerji S, Ferguson DJ, Clasper S, Jackson DG (2001) Mouse LYVE-1 is an endocytic receptor for hyaluronan in lymphatic endothelium. J Biol Chem 276:19420–19430
Rooney P, Kumar S, Ponting J, Wang M (1995) The role of hyaluronan in tumour neovascularization. Int J Cancer 60:632–636
Saika S, Kawashima Y, Miyamoto T, Okada Y, Tanaka S, Yamanaka O, Ohnishi Y, Ooshima A, Yamanaka A (1998) Immunolocalization of hyaluronan and CD44 in quiescent and proliferating human lens epithelial cells. J Cataract Refract Surg 24:1266–1270
Saika S, Miyamoto T, Tanaka S, Tanaka T, Ishida I, Ohnishi Y, Ooshima A, Ishiwata T, Asano G, Chikama T, Shiraishi A, Liu CY, Kao CW, Kao WW (2003) Response of lens epithelial cells to injury: role of lumican in epithelial-mesenchymal transition. Invest Ophthalmol Vis Sci 44:2094–2102
Smedsrød B, Pertoft H, Eriksson S, Fraser JR, Laurent TC (1984) Studies in vitro on the uptake and degradation of sodium hyaluronate in rat liver endothelial cells. Biochem J 223:617–626
Smedsrød B, Kjellen L, Pertoft H (1985) Endocytosis and degradation of chondroitin sulphate by liver endothelial cells. Biochem J. 229:63–71
Snook T (1950) A comparative study of the vascular arrangements in mammalian spleens. Am J Anat 87:31–78
Tanihara H, Inatani M, Koga T, Yano T, Kimura A (2002) Proteoglycans in the eye. Cornea 21:62–69
Toole BP (1997) Hyaluronan in morphogenesis. J Intern Med 242:35–40
Toole BP (2002) Hyaluronan promotes the malignant phenotype. Glycobiology 12:37–42
Turley EA (1992) Molecular mechanisms of cell motility. Cancer Metastasis Rev 11:1–3
Walsh EC, Stainier DY (2001) UDP-glucose dehydrogenase required for cardiac valve formation in zebrafish. Science 293:1670–1673
Weigel JA, Raymond RC, McGary C, Singh A, Weigel PH (2003) A blocking antibody to the hyaluronan receptor for endocytosis (HARE) inhibits hyaluronan clearance by perfused liver. J Biol Chem 278:9808–9812
Wells AF, Larsson E, Tengblad A, Fellstrom B, Tufveson G, Klareskog L, Laurent TC (1990) The localization of hyaluronan in normal and rejected human kidneys. Transplantation 50:240–243
West DC, Hampson IN, Arnold F, Kumar S (1985) Angiogenesis induced by degradation products of hyaluronic acid. Science 228:1324–1326
Acknowledgements
This work was supported by the Deutsche Forschungsgemeinschaft (DFG), the Dr. Mildred-Scheel Stiftung für Krebsforschung, and the Tumorzentrum Heidelberg/Mannheim.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Falkowski, M., Schledzewski, K., Hansen, B. et al. Expression of stabilin-2, a novel fasciclin-like hyaluronan receptor protein, in murine sinusoidal endothelia, avascular tissues, and at solid/liquid interfaces. Histochem Cell Biol 120, 361–369 (2003). https://doi.org/10.1007/s00418-003-0585-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00418-003-0585-5