Abstract
Purpose
This study aimed to study the difference in test results of online visual acuity (VA) test under different devices and screen brightness conditions and to compare online VA test with Early Treatment Diabetic Retinopathy Study (ETDRS).
Methods
Healthy volunteers with the best corrected VA of 0.0 LogMAR or higher were recruited. VAs under ETDRS were tested first, and then online VA test (the Stanford Acuity Test, StAT) visual acuities using iPad Air2 and Microsoft Surface pro4 under 50% and 100% screen brightness were performed. The VA results and the testing times were compared between different devices and screen brightness conditions.
Results
A total of 101 eyes were included in this study. The VA results measured by the StAT were better than those of ETDRS. The VA results measured at 100% screen brightness were better than those of 50% brightness (mean difference, 0.013 logMAR at most, less than 1 letter); the VA results measured by iPad Air2 were better than those of Surface pro4 (mean difference, −0.009 logMAR at most, less than 1 letter). Significantly less time was spent on VA testing under StAT than that under ETDRS.
Conclusion
The impact of screen brightness and the device on the VA results generated by online VA tests was clinically insignificant. In addition, online VA tests are found to be reliable and more time efficient than ETDRS.

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
An accurate visual acuity (VA) measurement is the foundation of ophthalmic diagnosis [1,2,3,4]. Traditional wall-mounted VA charts, including Snellen and Early Treatment Diabetic Retinopathy Study (ETDRS) charts, are the most commonly used VA measurement tools today [5,6,7]. ETDRS is recognized as the gold standard in VA chart measurement [8,9,10].
To get an accurate VA measurement, people in need of monitoring vision changes go to hospitals and have their VA measured routinely. However, frequent hospital visits are inconvenient, particularly for the elderly and mobility-impaired patients [11, 12]. Such visits were further deterred during the Corona Virus Disease 2019 (COVID-19) pandemic, in which people avoided going to overcrowded places like hospitals [13]. The pandemic has altered many patients’ medical treatment patterns as they preferred virtual consultations over in-person appointments. Our previous study in 2015 had shown that most patients with eye disease were willing to participate in mobile health programs [14]. Therefore, to help patients adapt to this new way of receiving diagnosis, a reliable and convenient online VA testing system is necessary.
Patients face many problems on self-administered test with VA charts at home. Firstly, a standard VA chart is difficult to obtain. Secondly, it is difficult for people to have the standard lighting required for an accurate VA examination. Thirdly, it is difficult to determine when to end the tests, how to score VA, and measure low VA on the chart [15]. Studies have shown that the results of measuring VA with traditional VA charts vary greatly and have poor repeatability [16, 17]. The participant’s inherent memory of the answer will also significantly impact test results.
Since the prevalence of telemedicine and virtual care has rapidly increased during the pandemic [4, 18,19,20,21,22,23], automated digital VA tests using electronic devices have gradually emerged [1, 4, 7, 24,25,26,27,28,29,30,31,32,33,34,35]. The random display of letters in different sizes greatly reduces the chance of memorizing [10]. However, many automated digital VA tests have not been validated in clinical trials and thus do not have guaranteed accuracy, and they are also not free. In order to investigate the effect of a self-administered online VA test, the Stanford Acuity Test (StAT) was selected for this study. This online VA test is free and allows people to complete it at home, which lightens their financial burden. Similar to other online VA tests (which have a high degree of reliability and agreement with traditional VA chart tests) [1, 4, 10, 24,25,26, 29, 34, 36,37,38], Piech et al. found that the StAT had reduced errors significantly compared with traditional VA chart [39]. However, most online VA tests, including StAT, do not provide guidance on how to select the appropriate device and screen brightness. Moreover, studies that discuss the effect of different devices and screen brightness on the results of online VA tests are limited. This study aimed to compare the online VA tests with ETDRS and study the difference in test results under different devices and screen brightness conditions.
Methods
Recruitment
The healthy subjects who underwent eye examinations in Zhongshan Ophthalmic Center of Sun Yat-sen University from May to September 2021 were recruited. The study received approval from the Zhongshan Ophthalmic Center’s Ethical Review Committee and was conducted in accordance with the tenets of the Declaration of Helsinki. Written informed consent was obtained from all participants in this study.
All participants underwent complete ophthalmic evaluation, including manifest refraction, slit-lamp biomicroscopy, dilated indirect ophthalmoscopy, fundus photography, and Humphrey SITA (Swedish Interactive Threshold Algorithm) standard 24–2 or 30–2 visual field testing.
Considering that the incidence of ocular and systemic diseases increases with age, which would make the test results biased, we set the inclusion criteria as follows: (1) age between 18 and 40 years old; (2) best corrected visual acuity (BCVA) 20/20 or better; (3) no history of ocular disease, or current evidence of ocular disease or systemic disease; (4) refractive error not exceeding ± 6 diopters (D) spherical equivalent (hyperopia or myopia), cylinder ≤ 2.0 D (astigmatism); (5) proficient in mobile phone operation.
Stanford Acuity Test
The StAT is an online test (https://myeyes.ai) developed by Piech and his colleagues. It is a new type of vision test based on an improved acuity model and an intelligent inference process. It can make decisions based on intelligent probabilistic models and display letters of any size adaptively, which compensates for the shortcomings of traditional printed VA charts.
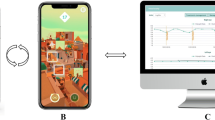
The StAT mainly relied on two devices: a computer and a smart phone. The letter “E” was displayed on the computer in four different orientations; 20 letters were displayed by default for each eye test; and only one letter was displayed at a time. The smart phone was controlled by the participant, and the answer was recorded by swiping across the screen in the same direction as the arm of the letter “E” [39].
There were four steps in the StAT. First, the participant needed to calibrate the screen size by following the prompts. Second, they needed to enter the measure distance between their position and the computer screen (the distance can be customized) and then followed the prompts to connect the smart phone to the computer. Next, they would submit answers on their phones when the computer screen randomly displayed the letter “E” of different sizes in four orientations. Then, the algorithm would adjust the size of the letter displayed next according to previous answers. As the test progressed, the algorithm was able to generate a more reliable estimate about the result [39, 40]. The results would be shown on the computer screen after the test.
Visual acuity measurements
All subjects wearing their habitual refractive correction underwent VA testing on the same day using the ETDRS and StAT in a controlled testing environment. All VA measurements were taken with a room luminance between 589 to 651 lx. If the subject’s two eyes met the inclusion criteria, the VA of both eyes would be measured; otherwise, only the eligible eye would be measured. While measuring one eye, full closure of the other eye was ensured by using an eye patch. Subjects were given at least a 1-min break between each test. A single ophthalmologist (L.C.) performed all the VA measurements. Two ophthalmologists (L.C. and S.P.) recorded the VA results and the testing time of each vision test.
The StAT (https://myeyes.ai) was performed on two different tablet computers, and the screen brightness of both tablets would switch between 50% brightness and 100% brightness. The two tablets were Microsoft Surface pro4 (SURFACE, windows10, 12.3-inch, PixelSense™ touchscreen display) and iPad Air2 (IPAD, iPadOS15, 9.7-inch, Liquid Retina display). The pixel resolution of two tablets had been uniformly set to 2048 × 1536. The static contrast ratio of the SURFACE’s screen was 1020:1, while the IPAD’s screen was 1126:1, both of which were very high. We measured the screen luminance values at the four corners and the center of the screen, a total of five points, to measure the average screen luminance values. At 100% screen brightness, the average SURFACE’s screen luminance was 360 cd/m2, and the IPAD’s was 358.4 cd/m2. At 50% screen brightness, the SURFACE had an average screen luminance of 180 cd/m2, and the IPAD had 179.2 cd/m2. The screen luminance of each device in this study met the standard requirements (range: 80–320 cd/m2) [15].
The VA tests were performed in the following sequence: (1) tested VA with ETDRS chart. The light box brightness of the 4-m ETDRS chart was 300 cd/m2. The subjects were instructed to point in the direction that the letter “E” was facing, and the ophthalmologist recorded the results based on the smallest line that four or more optotypes were correctly identified; (2) performed StAT on IPAD, measured VA at 50% screen brightness. Subjects stood at the StAT’s default standard test distance of 6.1 m and submitted the answers by swiping across the smart phone screen; (3) adjusted screen brightness to 100%, run StAT again on IPAD to repeat vision measurement; (4) performed StAT on SURFACE, measured VA at 50% screen brightness; (5) adjusted screen brightness to 100%, run StAT again on SURFACE to repeat vision measurement.
The different VA measurement methods were split into two categories: traditional ETDRS chart test (the ETDRS group) and online StAT (the StAT group). The StAT group was further divided into the following groups based on different tablet devices (two tablet computers: SURFACE and IPAD) and screen brightness (two screen brightness: 50% and 100%):
-
(1)
SURFACE50%: running StAT with SURFACE at 50% screen brightness;
-
(2)
SURFACE100%: running StAT with SURFACE at 100% screen brightness;
-
(3)
IPAD50%: running StAT with IPAD at 50% screen brightness;
-
(4)
IPAD100%: running StAT with IPAD at 100% screen brightness.
Data analysis
VA was converted to log minutes of arc (logMAR) for analysis. Comparisons of VA were performed in different group settings. For paired comparisons, the mean difference of VA was calculated, as well as the 95% confidence interval (CI) and the 95% limit of agreement (LOA). Bland–Altman plots were used to illustrate the agreement of VA test results across groups at different devices and screen brightness conditions. The mean testing time between ETDRS and StAT was compared using paired t tests. The above data were analyzed using SPSS v26.0 software (IBM, IL, USA). A p-value of < 0.05 was considered statistically significant.
Results
A total of 56 healthy subjects (101 eyes) participated in this study, including 17 males and 39 females. Eleven subjects had only one eye that satisfied the inclusion criteria; hence, only the data from their included eye were obtained, while their fellow eyes were excluded. The mean age was 26.70 ± 3.57 years old. No adverse events or complications occurred during the testing period. The mean VA of the ETDRS for all eyes tested (20/20 or better BCVA) was − 0.05 ± 0.07 logMAR.
Comparison of StAT and ETDRS on VA measurement
Compared with the traditional ETDRS chart, the VA results of the online VA test StAT were better (Table 1). The mean VA when using the ETDRS was − 0.05 ± 0.07 logMAR, and the mean VA using the StAT ranged from − 0.07 ± 0.09 logMAR to − 0.09 ± 0.10 logMAR for different devices and brightness conditions. Although the VA results were significantly different between the StAT and ETDRS (all P < 0.05), the maximum mean difference was only 0.032 logMAR, which was about 2 letters. Given that the clinically significant change was defined at 0.2 logMAR or greater (equivalent to ≥ 2 lines of acuity) [41], the difference of VA results between ETDRS and StAT had no clinical significance.
Comparison of StAT VAs under different brightness conditions
The mean VA results of StAT were better at 100% screen brightness than at 50% screen brightness (Table 2). In these two different brightness conditions, the VA results of StAT only had significant differences when IPAD was used (P = 0.009). However, the mean difference between IPAD50% and IPAD100% was 0.013 logMAR, which was equivalent to less than 1 letter and was clinically insignificant.
There was a high agreement and a small difference of averages between 50 and 100% screen brightness on IPAD (0.013 logMAR; 95% LOA, − 0.081 to 0.107, Fig. 1A), as well as on SURFACE (0.007 logMAR; 95% LOA, − 0.088 to 0.102, Fig. 1B).
Bland–Altman plots for StAT VA measurements by the IPAD and SURFACE in two different screen brightness (50% and 100%). A Agreement between IPAD50% brightness and IPAD100% brightness. B Agreement between SURFACE50% brightness and SURFACE100% brightness. C Agreement between IPAD50% brightness and SURFACE50% brightness. D Agreement between IPAD100% brightness and SURFACE100% brightness. E Agreement between IPAD50% brightness and SURFACE100% brightness. F Agreement between IPAD100% brightness and SURFACE50% brightness. The x-axis displays the average logMAR acuity, and the y-axis displays the difference in logMAR acuity of the two pairwise comparison groups. The black solid line represents the mean difference of VA between two pairwise comparison groups, black densely dashed line indicates 95% confidence interval (CI) of mean difference. The gray dashed lines represent the limits of agreement (LOA) (± 2 SD of the mean VA difference)
Comparison of StAT VAs under different devices
The results revealed that the mean VA results on IPAD were slightly better than those on SURFACE (whether performing StAT under 50% or 100% screen brightness), but the difference was not significant (all P > 0.05) (Table 3).
Figure 1C displays the high agreement of VA results of StAT between IPAD and SURFACE under 50% screen brightness. The mean difference was − 0.003 logMAR (equivalent to less than 0.2 letters) (95% LOA, − 0.019 to 0.103). Figure 1D illustrates that the agreement of VA results between IPAD and SURFACE under 100% screen brightness was also promising, with a mean difference of − 0.009 logMAR (equivalent to less than 1 letter) (95% LOA, − 0.100 to 0.084).
Comparison of StAT VAs on different devices and brightnesses
Table 4 shows the differences in VA results of StAT when the device and screen brightness were both different. The VA results of SURFACE100% were better than IPAD50% with an insignificant mean difference of 0.004 logMAR (equivalent to about 0.2 letters). However, IPAD100% had better VA results and a significant difference from SURFACE50% (mean difference, − 0.016 logMAR) (P = 0.005), but the mean difference was clinically insignificant because it was equivalent to less than 1 letter.
IPAD50% showed high agreement with SURFACE100% in VA results (Fig. 1E), the 95% LOA ranged from − 0.007 to 0.051. Agreement of VA results between the IPAD100% and SURFACE50% (Fig. 1F) was also good, with 95% LOA of − 0.123 to 0.091. Overall, the effects of different devices and screen brightness conditions on StAT VAs were not significant from a clinical perspective. Screen brightness might play a major role among these subtle effects, because higher screen brightness resulted in better test results no matter which device was used.
Comparison of testing time between StAT and ETDRS
The comparison of the mean testing time of each group is shown in Table 5. All StAT groups used significantly less time on average (48.95 s at most) than ETDRS (56.54 s) (all P < 0.001), with the IPAD100% group having the shortest mean testing time (47.04 s). Among the StAT groups, the difference of testing time was only significant between SURFACE50% and IPAD100% (48.95 s vs. 47.04 s, P < 0.05).
Discussion
Web-based VA tests provide various advantages. They provide a practical and high-quality vision test for patients who reside in distant places and require long-term eye monitoring, notably during the COVID-19 pandemic. However, there is little evidence to support the accuracy of a self-administered online VA test. In this study, StAT was utilized to investigate the differences between the online VA test and the ETDRS vision measurement, as well as the differences in test results under differed device and screen brightness conditions.
In the current study, we compared the online VA test with the traditional ETDRS chart and found that the VA results of the online VA test were better, although this difference did not have a significant impact from a clinical perspective. When we compared the effects of different devices and screen brightness on the VAs of the online VA test, the VA results measured at 100% screen brightness were better than those at 50% brightness, and the VA results measured by IPAD were better than SURFACE. Nevertheless, VA results of the online VA test did not differ significantly between these different conditions (all less than 1 letter).
Table 6 shows previous studies comparing traditional VA charts with online VA tests. The mean difference of VA results between the traditional VA charts and various online VA tests was equivalent to 1 letter to 1 line, which was clinically insignificant. Similarly, StAT also has a high agreement with the gold-standard ETDRS chart (the difference was less than two letters), so the selection of StAT as the research object in this study is representative to a certain extent.
Although SURFACE offers higher pixel density and image quality than IPAD, IPAD has a better overall screen layout due to the Retina Display’s fully laminated display technology and anti-reflective surface coating. The test results of several screens under the same brightness settings were strongly correlated in this study, and there was little difference in test results under the same screen resolution. This was in line with previous studies on the visual effects of various devices on people with low vision, which discovered no discernible difference between the effects of head-mounted displays and vertical displays on patients’ reading acuity [42].
However, the impacts of different devices on the results of online VA tests still exist. In the current study, performing an online VA test using IPAD under 100% brightness had the best VA results. Combined with the fact that IPAD50% could achieve a very similar effect as SURFACE100%, while SURFACE50% could not achieve a similar effect as IPAD100%, we infer that the unique material of the IPAD screen had a positive impact on the results. Consequently, the material of the electronic screen may be one of the factors affecting the testing effect.
Many studies have suggested that different screen brightness might affect the visual results. It has been reported that the agreement between the observers’ diagnostic results of carotid plaque duplex ultrasound images was poor at 50% and 100% brightness [43]. Another study found that raising screen brightness could boost readers’ speed and character recognition accuracy [44]. Furthermore, screen brightness aggravated blurred vision symptoms in computer vision syndrome [45, 46]. However, the VA results of the same device under different brightness had a good agreement in our study. Therefore, the difference in screen brightness may not have a noticeable impact on the results of the online VA test.
It has been proved that the “crowding effect” is constantly present in ETDRS [47], which may underestimate acuity measured in people with normal vision. In the Peek Acuity test, a box was set around the tumbling “E” to simulate the “crowding effect” [26, 48]. However, only a single optotype “E” appeared on the screen when testing StAT, which reduced the “crowding effect” and made the optotype look clearer [47, 49]. This may be one of the reasons why StAT had better VA results than ETDRS.
In previous studies, it took an average of 77 s to complete a vision test using Peek Acuity, which was 5 s faster than the Snellen chart (P = 0.13) [26, 48]. Also, in this study, the testing time of StAT was significantly shorter than ETDRS. StAT presents just one randomly orientated “E”, which can prevent the consequences of crowding effects and the potential for sequence learning if the same chart is used repeatedly. Compared to the ETDRS chart, it offers a simpler testing scenario for the tester. Furthermore, the StAT only requires the tester to observe a total of 20 letters for each eye, which is significantly less than the ETDRS chart test. These reasons may explain why the online VA test is more efficient.
There are limitations in this study. To ensure that the test results are uniform and unbiased, we excluded patients with a history of eye disease or those with decreased contrast sensitivity. As a result, the conclusions of this study may not be applicable to a large number of ophthalmic patients, thereby limiting its generalizability. However, we will explore the effect of online VA tests on ophthalmic patients in future studies.
Overall, the online VA tests were comparable to ETDRS in terms of the agreement and accuracy while taking much less time. It is critical to determine the accuracy of online VA tests because inaccurate and unreliable measures can lead to delayed treatment and management of ocular disorders. By studying StAT, this study proved the test validity of online VA tests and demonstrated that they could also have a high level of accuracy.
Conclusion
Our study demonstrated that the online VA test had the same high efficiency as the ETDRS chart and was more time-saving. Both screen brightness and the device had a clinically insignificant effect on online VA test’s results. Furthermore, using the IPAD tablet and a brighter screen resulted in better VA results of online VA test.
References
Habtamu E, Bastawrous A, Bolster NM et al (2019) Development and validation of a smartphone-based contrast sensitivity test. Transl Vis Sci Technol 8:2–11. https://doi.org/10.1167/tvst.8.5.13
Wang X, Lamoureux E, Zheng Y et al (2014) Health burden associated with visual impairment in Singapore: the Singapore epidemiology of eye disease study. Ophthalmology 121:1837–1842. https://doi.org/10.1016/j.ophtha.2014.03.017
Ou WC, Lesmes LA, Christie AH et al (2021) Normal- and low-luminance automated quantitative contrast sensitivity assessment in eyes with age-related macular degeneration. Am J Ophthalmol 226:148–155. https://doi.org/10.1016/j.ajo.2021.01.017
Ritchie A, Atamian S, Shah N et al (2021) Can visual acuity be reliably measured at home? Validation of telemedicine remote computerised visual acuity measurements. Br Irish Orthop J 17:119–126. https://doi.org/10.22599/bioj.179
Bailey IL, Lovie JE (1976) New design principles for visual acuity letter charts. Optom Vis Sci 53:740–745. https://doi.org/10.1097/00006324-197611000-00006
Mathew JA, Shah SA, Simon JW (2011) Varying difficulty of Snellen letters and common errors in amblyopic and fellow eyes. Arch Ophthalmol 129:184–187. https://doi.org/10.1001/archophthalmol.2010.369
Chen AH, Norazman F, Buari N (2012) Comparison of visual acuity estimates using three different letter charts under two ambient room illuminations. Indian J Ophthalmol 60:101–104. https://doi.org/10.4103/0301-4738.90489
Told R, Baratsits M, Garhöfer G, Schmetterer L (2013) ETDRS (Early Treatment Diabetic Retinopathy Study)-Visus. Ophthalmologe 110:960–965. https://doi.org/10.1007/s00347-013-2813-2
Koenig S, Tonagel F, Schiefer U et al (2014) Assessing visual acuity across five disease types: ETDRS charts are faster with clinical outcome comparable to Landolt Cs. Graefe’s Arch Clin Exp Ophthalmol 252:1093–1099. https://doi.org/10.1007/s00417-014-2670-y
Pang Y, Sparschu L, Nylin E (2020) Validation of an automated-ETDRS near and intermediate visual acuity measurement. Clin Exp Optom 103:663–667. https://doi.org/10.1111/cxo.13018
Gower EW, Silverman E, Cassard SD et al (2013) Barriers to attending an eye examination after vision screening referral within a vulnerable population. J Health Care Poor Underserved 24:1042–1052. https://doi.org/10.1353/hpu.2013.0134
Anjou MD, Boudville AI, Taylor HR (2013) Correcting Indigenous Australians’ refractive error and presbyopia. Clin Exp Ophthalmol 41:320–328. https://doi.org/10.1111/j.1442-9071.2012.02886.x
Burke BL, Hall RW, Dehnel PJ et al (2015) Telemedicine: pediatric applications. Pediatrics 136:e293–e308. https://doi.org/10.1542/peds.2015-1517
Dai M, Xu J, Lin J et al (2017) Willingness to use mobile health in glaucoma patients. Telemed e-Health 23:822–827. https://doi.org/10.1089/tmj.2016.0254
Ferris FL, Bailey I (1996) Standardizing the measurement of visual acuity for clinical research studies: guidelines from the Eye Care Technology Forum. Ophthalmology 103:181–182. https://doi.org/10.1016/S0161-6420(96)30742-2
Pathipati AS, Wood EH, Lam CK et al (2016) Visual acuity measured with a smartphone app is more accurate than Snellen testing by emergency department providers. Graefe’s Arch Clin Exp Ophthalmol 254:1175–1180. https://doi.org/10.1007/s00417-016-3291-4
Haupt PS (2008) Visual acuity testing in the emergency department: education and competency for emergency nurses. J Emerg Nurs 34:233–235. https://doi.org/10.1016/j.jen.2007.09.001
Stewart C, Coffey-Sandoval J, Souverein EA et al (2022) Provider-to-provider synchronous telemedical consultations in ophthalmology: advice for implementation. Digit Health 8:20552076221117744. https://doi.org/10.1177/20552076221117744
Mahajan V, Singh T, Azad C (2020) Using telemedicine during the COVID-19 pandemic. Indian Pediatr 57:652–657. https://doi.org/10.1007/s13312-020-1894-7
Liao CT, Chang WT, Yu WL, Toh HS (2020) Utility of telemedicine in the COVID-19 era. Rev Cardiovasc Med 21:583. https://doi.org/10.31083/j.rcm.2020.04.188
Lukas H, Xu C, Yu Y, Gao W (2020) Emerging telemedicine tools for remote COVID-19 diagnosis, monitoring, and management. ACS Nano 14:16180–16193. https://doi.org/10.1021/acsnano.0c08494
Bokolo A Jr (2020) Use of telemedicine and virtual care for remote treatment in response to COVID-19 pandemic. J Med Syst 44. https://doi.org/10.1007/s10916-020-01596-5
Ohannessian R, Duong TA, Odone A (2020) Global telemedicine implementation and integration within health systems to fight the COVID-19 pandemic: a call to action. JMIR Public Health Surveill 6:e18810. https://doi.org/10.2196/18810
Aslam TM, Parry NRA, Murray IJ et al (2016) Development and testing of an automated computer tablet-based method for self-testing of high and low contrast near visual acuity in ophthalmic patients. Graefe’s Arch Clin Exp Ophthalmol 254:891–899. https://doi.org/10.1007/s00417-016-3293-2
Aslam TM, Tahir HJ, Parry NRA et al (2016) Automated measurement of visual acuity in pediatric ophthalmic patients using principles of game design and tablet computers. Am J Ophthalmol 170:223–227. https://doi.org/10.1016/j.ajo.2016.08.013
Bastawrous A, Rono HK, Livingstone IAT et al (2015) Development and validation of a smartphone-based visual acuity test (peek acuity) for clinical practice and community-based fieldwork. JAMA Ophthalmol 133:930–937. https://doi.org/10.1016/j.yoph.2016.02.028
Black JM, Jacobs RJ, Phillips G et al (2013) An assessment of the iPad as a testing platform for distance visual acuity in adults. BMJ Open 3:5–7. https://doi.org/10.1136/bmjopen-2013-002730
Bokinni Y, Shah N, Maguire O, Laidlaw DAH (2015) Performance of a computerised visual acuity measurement device in subjects with age-related macular degeneration: Comparison with gold standard ETDRS chart measurements. Eye (Basingstoke) 29:1085–1091. https://doi.org/10.1038/eye.2015.94
Faria BM, Duman F, Zheng CX et al (2015) Evaluating contrast sensitivity in age-related macular degeneration using a novel computer-based test, the spaeth/richman contrast sensitivity test. Retina 35:1465–1473. https://doi.org/10.1097/IAE.0000000000000474
Kollbaum PS, Jansen ME, Kollbaum EJ, Bullimore MA (2014) Validation of an iPad test of letter contrast sensitivity. Optom Vis Sci 91:291–296. https://doi.org/10.1097/OPX.0000000000000158
Liu JL, Jason McAnany J, Wilensky JT et al (2017) M&S Smart System contrast sensitivity measurements compared with standard visual function measurements in primary open-angle glaucoma patients. J Glaucoma 26:528–533. https://doi.org/10.1097/IJG.0000000000000659
Lodhia V, Karanja S, Lees S, Bastawrous A (2016) Acceptability, usability, and views on deployment of peek, a mobile phone mhealth intervention for eye care in Kenya: qualitative study. JMIR Mhealth Uhealth 4:e30. https://doi.org/10.2196/mhealth.4746
Pang Y, Sparschu L, Wang J (2021) Repeatability of an automated ETDRS contrast threshold measurement. Ophthalmic Physiol Opt 41:896–899. https://doi.org/10.1111/opo.12829
Wisse RPL, Muijzer MB, Cassano F et al (2019) Validation of an independent web-based tool for measuring visual acuity and refractive error (the manifest versus online refractive evaluation trial): prospective open-label noninferiority clinical trial. J Med Internet Res 21:e14808. https://doi.org/10.2196/14808
Zhang Z-T, Zhang S-C, Huang X-G, Liang L-Y (2013) A pilot trial of the iPad tablet computer as a portable device for visual acuity testing. J Telemed Telecare 19:55–59. https://doi.org/10.1177/1357633X12474964
Brady CJ, Eghrari AO, Labrique AB (2015) Smartphone-based visual acuity measurement for screening and clinical assessment. JAMA 314:2682–2683
Han X, Scheetz J, Keel S et al (2019) Development and validation of a smartphone-based visual acuity test (vision at home). Transl Vis Sci Technol 8. https://doi.org/10.1167/tvst.8.4.27
Perera C, Chakrabarti R, Islam FMA, Crowston J (2015) The Eye Phone Study: reliability and accuracy of assessing Snellen visual acuity using smartphone technology. Eye (Basingstoke) 29:888–894. https://doi.org/10.1038/eye.2015.60
Piech C, Malik A, Scott LM et al (2020) The stanford acuity test: a precise vision test using Bayesian techniques and a discovery in human visual response. Proc AAAI Conf Artif Intell 34:471–479. https://doi.org/10.1609/aaai.v34i01.5384
Wang M (2020) Eye, robot: artificial intelligence dramatically improves accuracy of classic eye exam. Science 1979:6–10. https://doi.org/10.1126/science.abc4226
Bellsmith KN, Gale MJ, Yang S et al (2022) Validation of home visual acuity tests for telehealth in the COVID-19 era. JAMA Ophthalmol 140:465. https://doi.org/10.1001/jamaophthalmol.2022.0396
Virgili G, Acosta R, Bentley SA et al (2018) Reading aids for adults with low vision. Cochrane Database Syst Rev 2018. https://doi.org/10.1002/14651858.CD003303.pub4
Kakkos SK, Nicolaides AN, Geroulakos G et al (2011) Effect of computer monitor brightness on visual (subjective) carotid plaque characterization. J Clin Ultrasound 39:497–501. https://doi.org/10.1002/jcu.20871
Pan J, Sheu J, Massimo L et al (2021) Learning experience design in health professions education: a conceptual review of evidence for educators. AEM Educ Train 5. https://doi.org/10.1002/aet2.10505
Shantakumari N, Eldeeb R, Sreedharan J, Gopal K (2014) Computer use and vision-related problems among university students in Ajman, United Arab Emirate. Ann Med Health Sci Res 4:258. https://doi.org/10.4103/2141-9248.129058
Kozeis N (2009) Impact of computer use on children’s vision. Hippokratia 13:230–231
Danilova MV, Bondarko VM (2007) Foveal contour interactions and crowding effects at the resolution limit of the visual system. J Vis 7:1–18. https://doi.org/10.1167/7.2.25
Rono HK, Bastawrous A, Macleod D et al (2018) Smartphone-based screening for visual impairment in Kenyan school children: a cluster randomised controlled trial. Lancet Glob Health 6:e924–e932. https://doi.org/10.1016/S2214-109X(18)30244-4
Wang T, Huang PJ, Chen C et al (2021) A comparison of visual acuity measured by ETDRS chart and standard logarithmic visual acuity chart among outpatients. Int J Ophthalmol 14:536–540. https://doi.org/10.18240/ijo.2021.04.09
Acknowledgements
We would like to acknowledge that the Chinese government provided financial support in the form of the National Natural Science Foundation of China, the Guangdong provincial government provided financial support in the form of the Natural Science Foundation of Guangdong Province in China, and we would like to thank the financial support by Guangzhou Municipal Science and Technology Bureau in China, Health Commission of Guangdong Province in China.
Funding
This work was supported by the National Natural Science Foundation of China (No. 82271081), the Natural Science Foundation of Guangdong Province in China (No. 2022A1515010302), the Research Grant from Guangzhou Municipal Science and Technology Bureau in China (No. 202201020268), and the Research Grant from Health Commission of Guangdong Province in China (No. C2021044).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Ethics approval
Approval was obtained from the Ethical Review Committee of the Zhongshan Ophthalmic Center (2020KYPJ196). The procedures used in this study adhere to the tenets of the Declaration of Helsinki.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Lu Cheng and Shi Peng are the co-first authors of the article.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Cheng, L., Peng, S., Hao, H. et al. Effect of different screen brightness and devices on online visual acuity test. Graefes Arch Clin Exp Ophthalmol 262, 641–649 (2024). https://doi.org/10.1007/s00417-023-06206-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-023-06206-x