Abstract
Background
To evaluate the effects and side-effects of serial sub-conjunctival injections of 5-fluorouracil (5-FU) in early postoperative period for recurrent anophthalmic contracted socket.
Methods
Retrospective comparative case series at tertiary eye care centre including fifteen adult patients with features of postoperative recurrent socket contraction after buccal mucosal graft. Group A comprised eight patients treated with 10 mg weekly sub-conjunctival injection of 5–FU in the fornices. Group B comprised seven patients taken as control. Main outcome measures were: superior fornix depth (SFD), inferior fornix depth (IFD), and socket volume (SV) at 6 months follow up. Patients were re-evaluated clinically for recurrence at last follow-up.
Results
The mean ± SD values in group A versus group B were as follows: 10 ± 1.6 mm vs 5.1 ± 0.9 mm (p < 0.005) for SFD, 6.7 ± 1.5 mm vs 3.5 ± 0.5 mm (p = 0.02) for IFD; and 2 ± 0.55 ml versus 0.27 ± 0.06 ml (p = 0.005) for SV at 6 months. There was significant improvement in depth of fornices and volume of socket in seven patients in group A. One patient in group A did not benefit from 5-FU treatment. The beneficial effects of 5-FU were observed when first injection was given within 4 weeks after socket reconstruction. There was no recurrence (in six cases) and no side-effects seen in group A at final follow-up of 18.2 (12–24) months.
Conclusions
Weekly injections of 5-FU are effective for stopping the progression of recurrent contracted socket following primary reconstructive surgery. It provides early rehabilitation, and avoids repetitive surgery.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Contracted socket is defined as decrease in the depth of fornices and orbital volume caused by shrinkage and shortening of orbital tissues, and leads to inability to retain prosthesis. It causes considerable functional and psychological morbidity. Whatever the technique/graft used for reconstruction, the primary aim of management is to create a socket so as to maintain prosthesis with a good cosmetic appearance. Even after careful planning and meticulous surgery, the repeated contraction of socket can occur, causing shortening of the conjunctival fornices. Some cases may become recalcitrant, with inability to retain prosthesis because of extensive fibrosis, and only option remaining for such cases is optical methods to improve the appearance [1].
Postoperative prevention of scarring of socket is a key to success. Recurrent socket contraction is observed due to contracture of surgical bed, and requires repeated surgery [2]. But multiple surgeries can further accentuate scarring and render a case inoperable. The use of anti-fibrotic agents in glaucoma surgery to prevent postoperative fibrosis has become common practice [3]. 5-Fluorouracil (5-FU) is an effective inhibitor of fibroblast growth, interferes with collagen lattice contraction, and is used to modify the wound-healing pathway [5]. The purpose of this study is to describe the use of serial sub-conjunctival injections of 5-FU in the early postoperative period for managing recurrent contraction of socket seen after buccal mucosal graft.
Material and methods
This is a retrospective comparative case series involving 15 adult patients with features of recurrent socket contraction after reconstructive surgery with buccal mucosa graft between July 2009 and January 2012. All cases included in study showed progressive shallowing of fornices after socket reconstruction with buccal mucosal graft. The research adhered to the tenets of the Declaration of Helsinki. Informed consent for the use of 5-FU was obtained from all patients in group A.
Group A comprised eight patients who received serial subconjunctival 5-FU, and group B comprised seven patients taken as control. None of the patients had had a previous implant in the socket. The anophthalmic contracted socket was classified according to the classification by Krishna G [5].
All patients underwent socket reconstruction and adequate size full-thickness buccal mucosal graft from lower lip was used for surface area augmentation in the usual manner [6]. The graft was oversized by 50 % in all cases, and also included some fat component for volume enhancement [7]. The conjunctiva was incised from canthus to canthus, cicatricial bands were excised and removed. The buccal graft was sewn to the conjunctival margins, and stab incisions were given to prevent any collection beneath the graft. Fornix-forming sutures were placed over bolster in superior and inferior fornices. Adequate size conformer was placed into the socket, and tarsorrhaphy done. Orbital implant was not placed in any case. There were no intra-operative complications. Postoperative management included socket hygiene, antibiotics, and tarsorrhaphy removal at 1 week. The fornix forming sutures were removed at 3 weeks. These cases showed progressive loss of fornices, with difficulty in placing conformer in early postoperative period.
Superior and inferior fornix depth was measured by placing a Bowman probe vertically in the center, and socket volume by putting drop-by-drop saline in socket with the patient lying in a prone position. Each patient in group A received 10 mg sub-conjunctival injection of 5-FU (Fluracil, Biochem, India) in the superior and inferior fornices at weekly intervals, with a total of four injections. One patient required an additional injection in the lateral fornix. In group B, patients were observed conservatively.
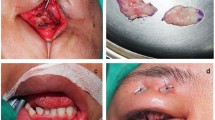
Injection technique (Fig. 1): 0.5 % proparacaine (Paracain, Sunways, India) was instilled in the socket to anesthetize the mucosa and conjunctiva. The socket was cleaned with 5 % povidone–iodine solution. The desired amount of 5-FU (10 mg, i.e., 0.2 ml of 50 mg/ml solution) was loaded in a 1-ml tuberculin syringe with 30-gauge needle. The drug was given as a single injection in the fornices. The needle was entered into the sub-mucosal plane from either temporal or nasal side up to the hub, and then the drug was injected very slowly while simultaneously withdrawing the needle to spread it in the entire fornix. This was quickly followed by firm pressure over the entry site by cotton applicator to limit leakage of the drug. In one case in group A there was severe conjunctival shortening; fornices were formed by buccal mucosa graft, and therefore the drug was injected beneath it. In all other cases, the drug was actually injected in sub-conjunctival space in the fornix. Postoperative treatment included topical antibiotics and oral analgesic for pain as required. Patients were then evaluated for customized prosthesis between 6 and 8 weeks.
Outcome assessment: the main outcome measures were increase in superior fornix depth (SFD), inferior fornix depth (IFD), and socket volume (SV) between the two groups at the 6-month follow-up. The ability to place a larger conformer and eventually prosthesis with acceptable cosmesis was also taken into consideration. In group A, patients were reviewed for post-treatment measurements (i.e., after first injection) at 1st week, 4th week, 3rd month, and 6th month, and again at final follow-up (ranging from 12–24 months) for evidence of recurrence of contraction such as entropion, forniceal shallowing, and tightness or fall of prosthesis, and any complications were noted. The statistical analysis was carried out using t-test, and significance was defined with p value less than 0.05.
Results
Patient characteristics: mean age was 25.6 ± 4.8 years and 26.2 ± 4.3 years, with average socket grading of 3.25 and 3.14 (p = 0.77) in group A and group B respectively. All patients previously had contracted socket where enucleation was done. The most common cause for enucleation in both groups was trauma. In group A, two cases had history of chemical injury causing anophthalmic contracted socket.
Table 1 shows the measurement of SFD, IFD, and SV at various follow-up visits for group A patients treated with serial sub-conjunctival 5-FU injection. In group A, the pre- and post-treatment (6 months after first injection) mean ± SD values were as follows: 5.1 mm and 10 mm for SFD (p < 0.005), 3.6 mm and 6.7 mm for IFD (p < 0.005), and 0.43 ml and 2 ml for SV (p < 0.005). Thus, there was significant average increase in all three parameters following the treatment. Individually, all cases in group A except case 4 showed significant improvement in fornices and socket volume, and were fitted with customised prosthesis with good cosmesis (Fig. 2, 3, and 4). In case number 3, lower eyelid entropion persisted at 12 months of follow-up without any difficulty in placing prosthesis (Fig. 5). In case 4, there was no statistical as well as clinical response observed with the treatment (p = 0.22, paired t-test). This patient also developed upper and lower eyelid entropion, and socket was fitted with small size prosthesis with acceptable cosmesis (Fig. 6).
In group A, a customized prosthesis was fitted 1 week after the last sub-conjunctival injection, i.e., around 8 weeks. In group B, all of the cases were tried for customized prosthesis at 6 weeks, but due to severe foreshortening of fornices, only one case could be fitted with a small-size prosthesis and acceptable cosmesis.
Total administered dose of 5-FU was 80 mg/case in seven cases and 90 mg in one case (where an additional injection in lateral fornix was given) in group A. The beneficial effects of 5-FU were observed when first injection was given within 4 weeks after socket reconstruction surgery. Case 4, which received 5-FU injection from the 5th week onwards, failed to show improvement.
There were no local and systemic side-effects observed with 5-FU in group A. Five out of eight cases experienced tolerable pain during the injection, and patients required oral analgesic for 1 day. There was no complaint of pain for subsequent days.
The final follow-up period in group A ranged from 12 to 24 months with average of 18.2 months. Except for case 3 (where lower eyelid entropion persisted) and case 4 (where no clinical improvement was seen), all of the rest cases did not show any recurrence. In group B, final follow-up period ranged from 9–15 months, with an average of 11.4 months.
Discussion
Following treatment with 5-FU, there was significant improvement in the depth of fornices and volume of socket in seven out of eight patients, leading to the placement of larger conformer and eventually prosthesis with good cosmetic outcome. Weekly injections of 5-FU, as noted in seven patients, were found to be very effective in dealing with the problem of recurrent fibrosis and contraction following the reconstructive surgery. Traditionally, any major reconstruction is performed in socket if there has been no cicatricial activity for 9 months [6]. Moreover, multiple surgeries can cause traumatic dissection of the orbital tissues, with eventual extensive scarring and contraction. The methods usually utilized for recurrence are trial of dermis-fat graft [8], or total excision of socket with closure of lids [5]. The use of silicone fixative has also been described for socket maintenance following reconstructive surgery [9]. Demicri and associates [2] described an operative technique using rigid nylon foil-anchored polytetrafluoroetyhlene (Gore-Tex) sheet for reconstruction of fornices, with the aim of preventing postoperative scarring, and obtained good results. But all these techniques require either autogenous or artificial graft for reconstruction.
The 5-FU has been previously used for many purposes in ophthalmic practice [4]. It is a pyrimidine analogue with anti-proliferative effects. The drug is most commonly used as serial sub-conjunctival injections, but may also be used as single intra-operative application in cases with failure of trabeculectomy blebs, or even in topical form for ocular squamous neoplasia [10]. Although ocular complications are not a concern for its use in anophthalmic socket, sub-conjunctival injections have been reported to cause squamous metaplastic changes and nuclear atypia during short-term follow-up [11]. In contrast, 5-FU is used as an anti-cancer drug for the treatment of pre-malignant and malignant ocular surface lesions [10, 12]. However, we believe that if an anticancer drug induces malignancy itself, then such malignancies will not be responsive to the inducing agent, and the patient should be warned of this effect.
Some of the local side-effects described with 5-FU are hyperaemia, chemosis, or foreign body [13]. Some systemic side-effects of local 5-FU administration need to be mentioned. Systemic absorption of the drug has been noted after intravitreal infusion, but usually the dose in ophthalmic practice is very small [14], and therefore concerns concerning infertility and teratogenicity will be rare. Hoehn and associates described a case of generalized tonic–clonic seizure after subconjunctival 5-FU because of neurotoxicity [15]. The authors stated the probable reason to be reduced synthesis of adenosine triphosphate, thiamine deficiency, or inherited deficiency of dihydropyrimidine dehydrogenase (DPD), which metabolizes majority of 5-FU. The spread of sub-conjunctival drug in cerebrospinal fluid can occur via sub-conjunctival space or optic nerve sheath and therefore, the possibility of seizure should be discussed with the patient. Although in our patients we did not measure DPD activity, it could be included in work-up. In our patients, the drug was very slowly delivered in sub-conjunctival space in the fornix, and the site was away from the fundus of the socket where the optic nerve is present. With this technique, we did not observe any local and systemic side-effects during the average follow-up period of 18.2 months.
Recent surgery can accelerate postoperative fibrosis and scarring. Partial thickness and larger size mucosal graft are more susceptible to contracture and fibrosis [16]. Associated conjunctivitis, mucous discharge, raw area, chemical injury, and history of radiation can also predispose to socket contraction after grafting [5, 17]. In our series, we harvested 50 % oversized graft along with fat from lower lip. The increased thickness due to inclusion of fat might have predisposed the graft to shrinkage and contraction due to increased demand of vascular supply. Also, the primary event leading to the loss of the eye was trauma (in nine cases) and chemical injury (two cases), which have contributed to recurrent contraction. The loss of fornices was observed in our cases from 3 to 5 weeks onwards. Krishna G also noted early shrinkage of graft in seven cases (13 %) after 4–6 weeks of socket reconstruction, and used pressure conformer. In addition to graft shrinkage, our cases showed progressive forniceal foreshortening and socket volume reduction, which made placement of conformer difficult despite best efforts.
5-FU acts on actively dividing cells, and therefore its beneficial effects are expected to be seen when the drug is used in the early postoperative period [3]. In our series, 5-FU was injected when the socket was in the healing and contraction phase. The seven out of eight patients who showed significant clinical improvement received the drug within 3–4 weeks of surgery. One patient who received 5-FU after 5 weeks in the same group did not show a clinical response. 5-FU not only stopped the progression, but also resulted in the regression of contraction, leading to larger fornices and increased socket volume.
We used a fixed dosing regimen in all cases, but individuals can have variable response to anti-fibrotic effects of 5-FU, and accordingly dose and frequency of injections can be modified and adjusted to keep them at a minimum according to the response [3]. This can be convenient for the patient in terms of less pain or minimal side-effects if any.
A retrospective non-comparative study from Priel and associates [18] found the use of antimetabolites to be effective in severe contracted socket reconstruction. Their series included five patients with a history of multiple socket operations where prophylactic antimetabolite (either mitomycin-C or 5-FU) was used as adjunct. 5-FU was used in three patients: one received an injection in the fornices intraoperatively, and all received 2-weekly injections of 5 mg/0.1 ml drug postoperatively. All cases were able to retain the prosthesis at final follow-up. In our comparative series, we used weekly injections of 5-FU in the fornices when the signs of socket contraction appeared in early postoperative period. Moreover, all cases had socket contraction after primary surgery.
A further study to evaluate the effect of titrated dose in this regard would be beneficial. Our study has some limitations due to small sample size and being retrospective. The measurements of fornix depth and socket volume were compared between the two groups at the 6-month follow-up. At final follow-up, only a clinical examination was done to look for any recurrent forniceal shortening and prosthesis fitting. Furthermore, all patients included have primary reconstructive surgery for socket using buccal mucosa, and therefore the role of 5-FU for second or multiple reconstructive procedures may be difficult to comment on from our study. However, initial results with sub-conjunctival 5-FU observed in our series are very encouraging, and suggest that it may be used for preventing recurrent socket contraction in early postoperative period following primary socket reconstruction with buccal mucosa . Its advantages include: low cost and convenience of injection, avoiding major surgery, and providing early rehabilitation.
To conclude, weekly sub-conjunctival injections of 5-FU are effective for stopping the progression of recurrent contracted socket if used within the early postoperative period after reconstructive surgery. However, titrated dose of serial sub-conjunctival 5-FU injections and their long-term effects need prospective evaluation.
References
Rycroft BW (1962) An operation for the treatment of severe contraction of the socket. Br J Ophthalmol 46:21–26
Demirci H, Elner SG, Elner VM (2010) Rigid nylon foil-anchored polytetrafluoroetyhlene (Gore-Tex) sheet stenting for conjunctival fornix reconstruction. Ophthalmology 117:1736–1742
Lama PJ, Fechtner RD (2003) Antifibrotics and wound healing in glaucoma surgery. Surv Ophthalmol 48:314–346
Abraham LM, Selva D, Casson R, Leibovitch I (2007) The clinical applications of fluorouracil in ophthalmic practice. Drugs 67:237–255
Krishna G (1980) Contracted sockets—I (aetiology and types). Indian J Ophthalmol 28:117–120
Schaefer DP (1998) Evaluation and management of the anophthalmic socket and socket reconstruction. In: Nesi FA, Lisman RD, Levine MR, Brazzo BG, Gladstone GJ (eds) Smith’s ophthalmic plastic and reconstructive surgery. Mosby, St. Louis, pp 1079–1124
Molgat YM, Hurwitz JJ, Webb MC (1993) Buccal mucous membrane-fat graft in the management of the contracted socket. Ophthal Plast Reconstr Surg 9:267–272
Wojno T, Tenzel RR (1986) Dermis grafts in socket reconstruction. Ophthal Plast Reconstr Surg 2:7–14
Mavrikakis I, Malhotra R, Shelley MJ, Sneddon KJ (2006) Surgical management of the severely contracted socket following reconstruction. Orbit 25:215–219
Parrozzani R, Lazzarini D, Alemany-Rubio E, Urban F, Midena E (2011) Topical 1% 5-fluorouracil in ocular surface squamous neoplasia: a long-term safety study. Br J Ophthalmol 95:355–359
Simsek T, Firat P, Citirik M, Ozdamar Y, Elgin U (2010) Short-term effects of subconjunctival injections of 5-fluorouracil on conjunctival epithelium. Cornea 29:727–731
de Keizer RJ, de Wolff-Rouendaal D, van Delft JL (1986) Topical application of 5-fluorouracil in premalignant lesions of cornea, conjunctiva and eyelid. Doc Ophthalmol 64:31–42
Huhtala A, Rönkkö S, Teräsvirta M, Puustjärvi T, Sihvola R, Vehanen K, Laukkanen A, Anttila J, Urtti A, Pohjonen T, Uusitalo H (2009) The effects of 5-fluorouracil on ocular tissues in vitro and in vivo after controlled release from a multifunctional implant. Invest Ophthalmol Vis Sci 50:2216–2223
Creten O, Spileers W, Stalmans P (2006) Systemic absorption of 5-fluorouracil during vitrectomy. Am J Ophthalmol 142:194–196
Hoehn R, Lamparter J, Pfeiffer N, Vossmerbaeumer U (2011) Seizures following subconjunctival 5-FU therapy. Graefes Arch Clin Exp Ophthalmol 249:145–146
Lee AC, Fedorovich I, Heinz GW, Kikkawa DO (2002) Socket reconstruction with combined mucous membrane and hard palate mucosal grafts. Ophthalmic Surg Lasers 33:463–468
Krishna G (1981) Contracted sockets—II. Indian J Ophthalmol 29:75–79
Priel A, Oh SR, Whipple KM, Korn BS, Kikkawa DO (2012) Use of antimetabolites in the reconstruction of severe anophthalmic socket contraction. Ophthal Plast Reconstr Surg 28:409–412
Conflicts of interest and source of funding
None
Author information
Authors and Affiliations
Corresponding author
Additional information
Authors have no financial disclosure.
Presented in part as poster at British Oculoplasty Surgery Society annual meeting, 2012, Leicester, United Kingdom
The authors have full control of all primary data, and they agree to allow Graefe's Archive for Clinical and Experimental Ophthalmology to review their data upon request.
Rights and permissions
About this article
Cite this article
Kamal, S., Kumar, S., Goel, R. et al. Serial sub-conjunctival 5-Fluorouracil for early recurrent anophthalmic contracted socket. Graefes Arch Clin Exp Ophthalmol 251, 2797–2802 (2013). https://doi.org/10.1007/s00417-013-2478-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-013-2478-1