Abstract
Purpose
The Stokes–Einstein equation predicts that diffusion is inversely correlated with viscosity of the medium. This predicts that diffusion fluxes should be lower in vitreous humour than in saline solution with lower viscosity. We test this hypothesis, which has implications for vitrectomy.
Methods
Diffusion cells were used, with a middle chamber filled with saline solution with different concentrations of hyaluronic acid (0 µg/ml, 30 µg/ml, 90 µg/ml and 180 µg/ml) or porcine vitreous humour, between cellophane membranes. HPLC was used to measure the concentration of the diffusing molecule, dexamethasone, and calculate the flux through the chamber filled with the various media. The diffusion coefficients were calculated, using Fick's law. Viscosity was measured with a Brookfield digital DV-I+viscometer.
Results
The diffusion coefficient for dexamethasone in vitreous humour is 0.065 ± 0.022 cm2/hour, 0.26 ± 0.12 cm2/hour for saline alone, 0.17 ± 0.04 cm2/hour for saline with 30 µg/ml hyaluronan, 0.076 ± 0.009 cm2/hour with 90 µg/ml hyaluronan, and with 180 µg/ml hyaluronan 0.072 ± 0.0018 cm2/hour (p < 0.001). The viscosity of liquid vitreous is 6.29 ± 2.3 cp, and the viscosity of saline alone is 1.01 ± 0.008 cp. For saline with 30 µg/ml of hyaluronan the viscosity is 1.04 ± 0.015, with 90 µg/ml hyaluronan is 1.06 ± 0.01, and with 180 µg/ml hyaluronan is 1.08 ± 0.014 (p < 0.001).
Conclusions
Dexamethasone diffuses four times faster through saline solution than vitreous humour. Liquid vitreous humour is about six times more viscous than saline. The results indicate that diffusion is faster in saline solution than in vitreous humour, in accordance to the Stokes–Einstein equation. This finding can help explain some of the physiological, pharmacological and clinical consequences of vitrectomy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The vitreous humour fills the vitreous cavity of the eye and modulates the diffusion of all molecules, such as drugs, oxygen and growth factors. The laws of Stokes–Einstein, Fick and Hagen–Poiseuille postulate that the rate of transport of any substance by diffusion or in convection currents is inversely related to the viscosity of the medium [1].
The vitreous humour is a clear aqueous gel where the matrix-forming polymer system consists mainly of collagen and hyaluronic acid. The collagen fibrils create a self-sustained collagen fibrillar network [2–4]. The hyaluronic acid, also called hyaluronan, is believed to participate in the stabilization of the collagen fibrillar network [2, 5]. The water content of vitreous is about 99% [2]. The vitreous humour is not homogenous and has a number of anatomical regions including the central vitreous, the basal vitreous, the vitreous cortex, the canal of Cloquet, the vitroretinal interface and zonule. Some of these regions possess different densities of collagen fibrils [4, 6].
In vitrectomy, when the vitreous humour is removed and replaced with saline soluiton, the viscosity of the medium decreases significantly, and the diffusion coefficient and rate of transport by diffusion or convection within the vitreous cavity is increased. This change influences the transport of all molecules, and may have various physiological, pharmacological and clinical consequences [1]. After vitrectomy, hyaluronic acid reforms to some extent, thus restoring hyaluronic levels somewhat after vitrectomy [6, 7].
Diffusion is described by Fick’s first law and the Stokes–Einstein equation. Fick’s first law states that the flux, J, is proportional to the concentration gradient (dC/dx) of the compound within a given medium:
where D is the diffusion coefficient or diffusivity of the diffusion molecules and dx is the distance traveled. The concentration C, depends among other things on the solubility of the substance in the medium.
The diffusion coefficient is described by the Stokes–Einstein equation:
where R is the molar gas constant, T is the temperature in Kelvin, η is the viscosity of the medium, r is the radius of the diffusion molecules and N is the Avogadro’s number [8].
The Hagen–Poiseuille law describes convection currents in liquids, and these are also inversely related to viscosity. The transport of a molecule by convection, J, would be the flux of a fluid multiplied by the concentration of the substance in the fluid, C, and thus the flux of a dissolved molecule in a fluid current would be:
where r is the radius and L is its length of the vessel, ΔP is the pressure gradient between two ends of the vessel and η is the viscosity of the medium [8].
The key issue is that both transport of molecules by convection currents and transport by diffusion are inversely related to the viscosity of the medium. This study was designed to investigate these changes in molecular transport by diffusion in vitreous humour compared with saline solution. We also investigated the changes in molecular transport when saline solution was mixed with different concentrations of hyaluronan, to try to reflect upon the situation in the vitreous cavity after vitrectomy.
Materials and methods
Diffusion studies
The diffusion studies were performed in two groups:
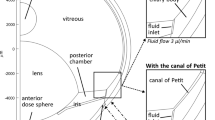
Diffusion cells were used (PermeGear, Inc, Hellertown, PA, USA: Fig. 1), with two or three chambers. A donor chamber was filled with 2 ml of a 5% hydroxypropyl-β-Cyclodextrin solution containing the reference molecule, dexamethasone (saturated, 3.76 mg/ml). A middle chamber was filled with 0.5 ml of either porcine vitreous humour or saline solution (0.9%). A receptor chamber was filled with ∼12 ml 5% hydroxypropyl-β-Cyclodextrin solution as well. The three chambers were separated by cellophane membranes MWCO (molecular weight cut off) 12,000–14,000. A 0.1 ml sample was drawn at 4, 8 and 12 hour intervals from the receptor chamber (chamber filled up to ∼12 ml after drawing each sample). A reference study with a double layer of the cellophane membranes alone was performed as a reference, in order to calculate the diffusion through the vitreous humour or saline solution only (middle chamber removed).
A schematic drawing of a diffusion cell with a middle chamber filled with either saline solution with different concentrations of hyaluronan or vitreous humour (0.5 ml). The donor chamber has a 3.76 or 4.51 mg/ml saturated solution of dexamethasone in 5% hydroxypropyl-β-cyclodextrin solution (2 ml). The receptor chamber has a 5% hydroxypropyl-β-cyclodextrin solution (∼12 ml); two cellophane membranes encapsule the middle chamber (MWCO 12,000–14,000)
The second part of the diffusion studies was performed using the same method.
The donor chamber was filled with 2 ml of a 5% hydroxypropyl-β-Cyclodextrin solution containing dexamethasone (saturated, 4.51 mg/ml). The middle chamber was filled with 0.5 ml of different concentrations of hyaluronic acid (hyaluronic acid sodium salt from bovine vitreous humor, Sigma-Aldrich) mixed in saline solution (0 µg/ml, 30 µg/ml, 90 µg/ml and 180 µg/ml). The receptor chamber was filled with ∼12 ml 5% hydroxypropyl- β -Cyclodextrin solution, and the three chambers were separated by cellophane membranes MWCO 12,000–14,000 as before. A 0.1-ml sample was drawn at 3, 6, 9 and 12 hour intervals from the receptor chamber (chamber filled up to ∼12 ml after drawing each sample). A reference study with a double layer of the cellophane membranes alone was also performed here as a reference, except that the samples were drawn at 90, 180, 270 and 360 minutes intervals.
HPLC (high-performance liquid chromatography) was used to measure the concentration of dexamethasone in the receptor chamber. We calculated the flux through the vitreous humour or saline solution filled chamber under standardized conditions. The diffusion coefficient of the vitreous humour and saline solution were calculated, using Fick´s law.
Porcine eyes were obtained from an abattoir, dissected, the vitreous humour removed and placed in the middle chamber of the diffusion cell (Fig. 1). Each eye could be utilized in two cells, 0.5 ml in each cell. The saline solution had a concentration of 9 mg/ml NaCl.
Calculations
Fick’s first law was used to calculate the diffusion, where the resistance of the cellophane membranes were subtracted from the mean flux. Fick’s first law states that the flux, J, is proportional to the concentration gradient (dC/dx) of the compound within a given medium:
The amount (M) of compound flowing through a unit cross-section (S) of a flow barrier in unit time (t) is equal to the flux, J:
Plotting the amount of drug in the receptor chamber (M) vs time (t) divided by the cross section (S) will give the flux (J). The flux can also be displayed as:
Where C0 is the concentration of dexamethasone in the donor chamber (assuming zero concentration in the receptor chamber). By subtracting the resistance (R) of the double membranes from the resistance (R), where the vitreous or saline solution are encapsulated within two membranes, we find the resistance for the vitreous humour or saline solution alone and calculate the permeability coefficient (P) as:
Now we can use the permeability coefficient to calculate the calculated flux (J*) through vitreous gel or saline:
We find the diffusion coefficient (D) according to Fick’s first law, rewritten as follows:
Viscosity measurements
The viscosity of the porcine vitreous humour and the saline solution with different concentrations of hyaluronic acid was measured with a Brookfield digital DV-I+rotational viscometer (Brookfield Engineering Laboratories, Inc., Middleboro, MA, USA). Porcine eyes were cut through the equatorial bulbus, and great care was taken to ensure that the aqueous humour would not contaminate the specimen. The vitreous humour was then removed, and two different components of the vitreous measured separately (the vitreous humour was divided into “liquid” vitreous and “gel” vitreous). Both components of the vitreous were measured with three different speeds of spindle in the viscometer; the gel vitreous was measured with 0.3, 0.6 and 1.5 rounds per minute (rpm), and the liquid vitreous with 6, 12 and 30 rpm. The measurement of the liquid vitreous at spindle speed 6 rpm was used as a reference according to the Brookfield guide and operating instructions [9, 10]. With thicker solutions (non-watery), we want to use the lowest spindle speed which is significant according to the viscometer, and in our case it is the speed of 6 rpm.
Statistical analysis was performed with commercial software (SPSS for Windows; SPSS Inc., Chicago, IL, USA). To test if there was a significant difference between the vitreous humour and saline solution results, Student’s t-test was performed. To test if there was a significant difference between both diffusion and viscosity of the saline solutions mixed with different concentrations of hyaluronan and the vitreous, one-way ANOVA was performed, with a Tukey HSD test as a post-Hoc multiple comparison, except when the saline solutions were compared with the vitreous, when a Students t-test was performed.
Results
The measured concentration of the dexamethasone in the receptor chamber in the first part of the study, after 12 hours, was 0.049 ± 0.008 mg/ml for the vitreous humour and 0.087 ± 0.006 mg/ml for the saline solution. For the double membrane, the measured concentration in the receptor chamber after 12 hours was 0.13 ± 0.009 mg/ml. The amount of dexamethasone in the receptor chamber was calculated for each interval (4, 8 and 12 hours), and the results are displayed in Fig. 2. These results were used to calculate the flux, the resistance, the diffusion and permeability coefficients. The data is displayed in Table 1, along with the results of the viscosity measurements for the liquid vitreous humour and saline solution, and p-values calculated for statistical analysis.
Shows the amount (mg) of dexamethasone in the receptor chamber at intervals (4, 8 and 12 hours). The media in the middle chamber, were vitreous humour (n = 8) and saline solution (n = 10) encapsulated between two layers of cellophane membranes. Double membrane (two layers of cellophane membranes, with no middle chamber) was used as a reference to calculate the resistance of substances tested (n = 10). The lines represent a regression line
Student’s t-test revealed a significant difference for all variables between the saline solution and vitreous humour (Table 1, p < 0.001).
In the second part of the study, the measured concentration of dexamethasone in the receptor chamber after 12 hours was 0.11 ± 0.016 mg/ml for the saline solution (0 µg/ml hyaluronan), 0.097 ± 0.007 mg/ml for the saline solution mixed with 30 µg/ml hyaluronan, 0.073 ± 0.004 mg/ml with 90 µg/ml hyaluronan, and 0.068 ± 0.008 mg/ml with 180 µg/ml of hyaluronan. For the double membrane reference, the concentration of dexamethasone in the receptor chamber was 0.080 ± 0.01 mg/ml after 6 hours. The amount of dexamethasone in the receptor chamber was calculated for each interval (3, 6, 9 and 12 hours, or 1.5, 3, 4.5 and 6 hours) and the results are displayed in Fig. 3. These results were used to calculate the flux, the resistance, the diffusion and permeability coefficients as before. The data is displayed in Table 2, along with the results of the viscosity measurements for each concentration of the hyaluronan tested and the p-value calculated for statistical analysis.
Shows the amount (mg) of dexamethasone in the receptor chamber at intervals (3, 6, 9 and 12 hours). The filling in the middle chamber, were saline solutions mixed with different concentrations of hyaluronic acid, 0 µg/ml (n = 4), 30 µg/ml (n = 6), 90 µg/ml (n = 6), 180 µg/ml (n = 6) encapsulated between two layers of cellophane membranes. Double membrane (two layers of cellophane membranes, with no middle chamber) was used as a reference to calculate the resistance of substances tested (n = 6). The lines represent a regression line
One-way ANOVA revealed a significant difference between the diffusion of dexamethasone in the vitreous and that for saline 0 and 30 µg/ml hyaluronan (p < 0.001), but no significant difference between the flux in the vitreous and that for saline 90 and 180 µg/ml hyaluronan (p = 0.963 and p = 0.995). There is no significant difference between the concentrations 0 and 30 µg/ml of hyaluronan (p = 0.07) and between 90 and 180 µg/ml (p = 1.0). But there is a significant difference between the concentrations of 0 µg/ml and 90 µg/ml (p < 0.001), 0 µg/ml and 180 µg/ml (p < 0.001), 30 µg/ml and 90 µg/ml (p = 0.003) and 30 µg/ml and 180 µg/ml (p = 0.002).
The calculated diffusion coefficient for all concentrations of hyaluronan and vitreous is shown in Fig. 4.
Shows the calculated diffusion coefficient of the saline solution with different amounts of hyaluronic acid (0, 30, 90 and 180 µg/ml, n = 6 for each substance tested, except for concentration 0 where n = 4) and the diffusion coefficient of the vitreous gel (n = 8) (p < 0.001). The bars represent error bars
The viscosity measurements of the vitreous, both the liquid vitreous and the gel vitreous, are displayed in Fig. 5. The viscosity measurements of different concentrations of hyaluronan are displayed in Fig. 6.
Student’s t-test revealed a significant difference between the viscosity measured in both components of the vitreous and that for all concentrations of hyaluronan (p < 0.001). One-way ANOVA revealed a significant difference between all concentrations of hyaluronan (p < 0.001) except between the concentrations of hyaluronan 90 µg/ml and 180 µg/ml (p = 0.08).
Discussion
The results in the first part of the study indicate that diffusion is faster in physiological saline solution than in vitreous humour (Table 1 and Fig. 4). According to our results, dexamethasone diffuses about four times faster through saline solution than vitreous humour. This indicates that the diffusion coefficient is four times higher in vitreous humour than in saline. This effect should be similar in the diffusion of all molecules, including growth factors, oxygen and other drugs. This suggests that the flux of molecules within the vitreous cavity will change dramatically when the vitreous humour is replaced with saline solution.
The liquid vitreous humour is about six times more viscous than saline solution (Table 1). When the calculated diffusion coefficient is compared with the viscosity measurements of the liquid vitreous, this complies roughly with the relationship between the viscosity of the medium and the diffusion coefficient as predicted by the Stokes–Einstein equation.
When the viscosity of vitreous is measured with a rotational viscometer, the vitreous, being a non-newtonian fluid, shows a shear thinning effect (Fig. 5), which means that with time and increased speed of spindle, the viscosity decreases.
The delicate structure of the vitreous humour is destroyed by the rotational viscometer in the measurement process, thus decreasing the viscosity (Fig. 5) [11, 12].
Our data suggest that diffusion takes place preferentially through the liquid vitreous, due to the higher diffusion coefficient in liquid than in gel vitreous. For this reason we use liquid vitreous viscosity measurements in our analysis.
The vitreous humour is a clear aqueous gel where the matrix-forming polymer system consists mainly of collagen and hyaluronic acid. The collagen fibrils occur predominantly in parallel bundles of two or more fibrils, with fibrils or bundle of fibrils frequently breaking off to join other bundles and, thus, creating a self-sustained collagen fibrillar network [2–4]. The fibers run in an antero-posterior direction [4, 13], forming canals of at least one wavelength to minimize light scattering [14].
Tuteja and Mackay [15] reported a successful, direct measurement of the diffusion coefficients of sub-10 nm diameter nanoparticles in polymer liquid by using X-ray photon correlations spectroscopy, and found that the Stokes–Einstein relation between viscosity and diffusion was not applicable with such small particles. The reason for this is because when the molecule is extremely small (sub-10 nm diameter), it most likely diffuses through the vitreous humour in the canals between the collagen polymer chains, and therefore the viscosity of the gel vitreous humour might not be relevant to the diffusion of these sub-10 nm diameter molecules.
Previous studies of human and porcine vitreous humour have shown some similarities in viscosity and composition of macromolecules such as hyaluronan and collagen compared to other species [12, 16–18]. We conclude that the use of porcine vitreous is a good candidate to represent the human eye, taking into consideration the differences.
Lee et al. [12, 16, 17] and Soman & Banerjee [19] have studied the viscosity of porcine, bovine and humans vitreous humour and its replacements. They found that the viscosity of vitreous humour is between 300 and 2000 cp. At the same time, the viscosity of water is only 1 cp. This means that when the vitreous humour is removed and replaced with saline solution, the viscosity of the medium in the vitreous cavity would reduce 300–2000 fold, and the transport of molecules through the vitreous cavity would therefore increase accordingly. The higher diffusion coefficient in saline solution compared to vitreous humour will also mean that for a given flux the concentration gradient will be smaller, meaning that concentration gradients in the vitreous cavity will become flatter after vitrectomy [1].
Lee et al. [17] studied the viscosity of porcine vitreous humour and compared it to the viscosity of human vitreous humour, and found out that some regions of the pig vitreous appeared to be a “thicker” gel, whereas the human gel more often presented a “thinner” consistency. Some of the anterior and the central human samples appeared “watery”. Samples obtained from the pig central region also often presented a “thinner” consistency. There was not a significant difference between the central region of the porcine vitreous humour and the central region of the human vitreous humour. In the viscosity measurements performed by Lee et al., the thicker gel part of the vitreous humour is included in the measurements, and they therefore display a much higher viscosity than our results.
Barton et al. [20] argue that the Stokes–Einstein equation only describes the effect of the viscosity on the rate of diffusion in a liquid; however, our results indicate otherwise. The liquid vitreous viscosity measurements we performed are in accordance with the diffusion coefficient we calculated. On the other hand, the viscosity measurements performed by Lee et al. [12, 16, 17] show a much higher viscosity, which indicates that the relationship between viscosity and diffusion could be more complicated.
After vitrectomy, it is believed that hyaluronan can re-synthezise partly or even fully [6, 7, 21]. In order to simulate the post-vitrectomy situation, we measured the diffusion and viscosity of various concentrations of hyaluronic acid mixed in saline. We choose the concentration of 30 µg/ml, because it reflects the concentration of hyaluronic acid in the post-vitrectomized eye after an average of 9 days [7, 21], the concentration 90 µg/ml, because it reflects the concentration in the aged eye [21] as well as in the porcine eye [6], and finally the concentration 180 µg/ml, because it reflects the concentration of hyaluronan in the adult eye [6].
If we look at the results of the second part of the diffusion studies (Table 2 and Fig. 4), we see that there is a decrease in the diffusion of dexamethasone with increased levels of hyaluronic acid. There is no significant difference between the concentrations 0 and 30 µg/ml of hyaluronan (p = 0.07) and between concentrations of 90 and 180 µg/ml (p = 1.0). But there is a significant difference between all other concentration pairs.
There is a significant difference between the diffusion of dexamethasone in the vitreous and that in 0 and 30 µg/ml hyaluronan (p < 0.001). The concentration of 30 µg/ml is close to the concentration of hyaluronan measured in the post-vitrectomized eye [7, 21], so even though the hyaluronan reforms to some extent the diffusion is still greater than in normal vitreous, as expected.
There is no significant difference between the diffusion of dexamethasone in the vitreous and that in 90 and 180 µg/ml hyaluronan (p = 0.963 and p = 0.995). This shows that the concentration of hyaluronan is probably a big factor in changing the diffusion of small molecules like dexamethasone.
If we look at the viscosity (Table 2 and Fig. 6), there is a significant difference between the viscosity of all of the hyaluronic acid/saline solution concentrations, except between concentrations 90 and 180 µg/ml of hyaluronan. This is in accordance with the diffusion studies.
After vitrectomy, there is no three-dimensional structure of collagen fibers that serves as a scaffold for high molecular weight hyaluronan, and hyaluronan molecules may fail to connect with each other [21]. This may explain why there is no significant difference between concentrations of 90 and 180 µg/ml of hyaluronan, both in diffusion and viscosity.
If we compare the viscosity of the liquid vitreous with the viscosity of the saline solutions with different concentrations of hyaluronic acid, the difference is significant (p < 0.001). The difference in viscosity is around six-fold in all concentrations of hyaluronan mixed in saline (5.8-fold to 6.2-fold) compared to the liquid vitreous. These results indicate a great difference in viscosity between normal vitreous and post-vitrectomized eyes.
Replacement of the vitreous humour with lower viscosity saline or aqueous humour speeds up the transport of molecules within the eye [22]. Dexamethasone molecules diffuse faster through the vitrectomized vitreous cavity to the retina, while at the same time the clearance of dexamethasone from the vitreous cavity is faster in vitrectomized eyes.
Changes in transport of other molecules could explain various physiological and clinical effects that have been documented following vitrectomy. This change in transport within the vitreous cavity can supply hypoxic areas of the retina with oxygen [23], can lead to cataract formation [24] and can influence the physiology of the eye following vitrectomy in various ways [25].
Pharmacologic vitreolysis is a new approach to improving vitreo-retinal surgery, which can increase vitreous diffusion coefficients [13]. While viscosity has not been measured following pharmacologic vitreolysis, it is very likely that it decreases viscosity and the increased diffusion reflects the Stokes–Einstein equation.
Removal of the vitreous humour influences the physiology of the eye. The diffusion characteristics of small molecules in the vitreous cavity are changed dramatically by the removal of vitreous humour and its replacement with saline solution. This effect is predicted by the Stokes–Einstein equation. When the vitreous humour is replaced with saline solution in vitrectomy, the chemical change is minor, as the vitreous humour is 99% water, but there is an enormous change in viscosity [1]. Our results imply that when the vitreous humour has been replaced with water, the diffusion of small molecules within the area increases about 4–5 times.
The Stokes–Einstein equation sheds light on the physiological and clinical consequences of vitreous removal and possibly posterior vitreous detachment [25].
References
Stefansson E, Loftsson T (2006) The Stokes-Einstein equation and the physiological effects of vitreous surgery. Acta Ophthalmol Scand 84(6):718–719. doi:10.1111/j.1600-0420.2006.00778.x
Bos KJ et al (2001) Collagen fibril organisation in mammalian vitreous by freeze etch/rotary shadowing electron microscopy. Micron 32:301–306. doi:10.1016/S0968-4328(00)00035-4
Gelse K, Pöschl E, Aigner T (2003) Collagens - structure, function, and biosynthesis. Adv Drug Deliv Rev 55:1531–1546. doi:10.1016/j.addr.2003.08.002
Bishop PN (2000) Structural macromolecules and supramolecular organisation of the vitreous gel. Prog Retin Eye Res 19(3):323–344. doi:10.1016/S1350-9462(99)00016-6
Ihanamäki T, Pelliniemi LJ, Vuorio E (2004) Collagens and collagen-related matrix components in the human and mouse eye. Prog Retin Eye Res 23:403–434. doi:10.1016/j.preteyeres.2004.04.002
Sebag J (1989) The vitreous: structure, function, and pathobiology. Springer-Verlag, New York, p 173
Itakura H et al (2005) Vitreous collagen metabolism before and after vitrectomy. Graefes Arch Clin Exp Ophthalmol 243(10):994–998. doi:10.1007/s00417-005-1150-9
Sinko P (2006) Martin’s physical pharmacy and pharmaceutical sciences. Lippincott Williams & Wilkins, Philadelphia
Brookfield Engineering Labs Education. More solutions to sticky problems. Brookfield Engineering Labs, Inc., Middleboro, MA, USA
Brookfield Engineering Labs Education. Brookfield Digital Viscometer Model DV-1+ Operating Instructions. Brookfield Engineering Labs, Inc., Middleboro, MA, USA
Weber H, Landwehr G (1982) A new method for the determination of the mechanical properties of the vitreous. Ophthalmic Res 14(5):326–334
Lee B, Litt M, Buchsbaum G (1992) Rheology of the vitreous body. Part I: Viscoelasticity of human vitreous. Biorheology 29(5–6):521–533
Sebag J, Ansari RR, Suh KI (2007) Pharmacologic vitreolysis with microplasmin increases vitreous diffusion coefficients. Graefes Arch Clin Exp Ophthalmol 245(4):576–580. doi:10.1007/s00417-006-0394-3
Sebag J (2005) Molecular biology of pharmacologic vitreolysis. Trans Am Ophthalmol Soc 103:473–494
Tuteja A et al (2007) Breakdown of the continuum stokes-einstein relation for nanoparticle diffusion. Nano Lett 7(5):1276–1281. doi:10.1021/nl070192x
Lee B, Litt M, Buchsbaum G (1994) Rheology of the vitreous body: part 3. Concentration of electrolytes, collagen and hyaluronic acid. Biorheology 31(4):339–351
Lee B, Litt M, Buchsbaum G (1994) Rheology of the vitreous body: Part 2. Viscoelasticity of bovine and porcine vitreous. Biorheology 31(4):327–338
Lee B (1992) Comparative rheological studies of the vitreous body of the eye. University of Pennsylvania dissertation, p 306
Soman N, Banerjee R (2003) Artificial vitreous replacements. Biomed Mater Eng 13(1):59–74
Barton KA et al (2007) Comment on: the Stokes-Einstein equation and the physiological effects of vitreous surgery. Acta Ophthalmol Scand 85(3):339–340. doi:10.1111/j.1600-0420.2007.00902.x
Itakura H et al (2009) Decreased vitreal hyaluronan levels with aging. Ophthalmologica 223(1):32–35. doi:10.1159/000165682
Stefansson E, Landers MB 3rd, Wolbarsht ML (1981) Increased retinal oxygen supply following pan-retinal photocoagulation and vitrectomy and lensectomy. Trans Am Ophthalmol Soc 79:307–334
Stefansson E, Novack RL, Hatchell DL (1990) Vitrectomy prevents retinal hypoxia in branch retinal vein occlusion. Invest Ophthalmol Vis Sci 31(2):284–289
Holekamp NM, Shui YB, Beebe DC (2005) Vitrectomy surgery increases oxygen exposure to the lens: a possible mechanism for nuclear cataract formation. Am J Ophthalmol 139(2):302–310. doi:10.1016/j.ajo.2004.09.046
Stefansson E (2009) Physiology of vitreous surgery. Graefes Arch Exp Clin Ophthalmol 247:147–163
Acknowledgments
This work was supported by grants from the Icelandic Fund for Prevention of Blindness, University of Iceland Research Fund and Helga Jónsdóttir and Sigurliði Kristjánsson Memorial Fund.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gisladottir, S., Loftsson, T. & Stefansson, E. Diffusion characteristics of vitreous humour and saline solution follow the Stokes Einstein equation. Graefes Arch Clin Exp Ophthalmol 247, 1677–1684 (2009). https://doi.org/10.1007/s00417-009-1141-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-009-1141-3