Abstract
Introduction
Patients with central retinal vein occlusion (CRVO) may experience reduced vision in the morning. This may be due to increased cystoid macular oedema (CMO), which can be measured on optical coherence tomography (OCT).
Methods
A prospective study was performed on ten patients. Retinal thickness measurements were made with the Topcon 3D OCT-1000: at 9 a.m., 11 a.m., 1 p.m., 3 p.m., 5 p.m. In addition, at 9 a.m. and 5 p.m. visual acuity was recorded using ETDRS LogMAR.
Results
There were seven males and three females with average age of 59.4 years (range 40–80 years). The average duration of symptoms was 5.4 months (range 3–9 months). In eyes with CRVO, median central macular thickness (CMT) significantly reduced from 571 µm at 9 a.m. to 475 µm at 5 p.m. (p < 0.05). Comparison of CMT at 9 a.m. to each of the subsequent time intervals found that there was a significant reduction in the central macula thickness late in the day (p < 0.05). There was no statistical difference in the visual acuity and change in macular thickness did not correlate with change in visual acuity in eyes affected by CRVO.
Discussion
Patients with CRVO demonstrate increase in CMO in morning compared with late morning and afternoon. Possible causes are diurnal variation in blood pressure, retinal metabolism and erect posture. Interventions designed to influence these factors could be used to try to reduce CMO severity
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
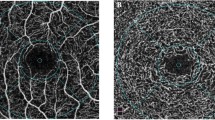
Central retinal vein occlusion (CRVO) is a common retinal vascular disease and usually carries a poor visual outcome [1]. The major complications associated with decrease in visual acuity are retinal hemorrhage over the fovea, foveal ischemia and cystoid macular oedema (CMO), with CMO being the commonest cause of visual loss [2]. Optical coherence tomography (OCT) is a noninvasive method for measuring the central macular thickness (CMT) which provides quantitative and reproducible measurements of macular thickness.
Patients with CMO from diabetes mellitus may show substantial variability during the course of the day, with macular thickening being at its maximum on awakening and then tending to decrease throughout the day [3–8]. A variety of mechanisms may be postulated to explain this phenomenon, such as arterial pressure, neuronal activity, or other metabolic and/or endocrine factors [9–11].
We designed the current study to evaluate changes in CMT measured by OCT throughout the day in eyes with CMO and CRVO.
Method & materials
Ten patients with CRVO in one eye, either ischaemic or non-ischaemic, who complained of worsening of vision on awakening were included in the study. All subjects underwent a complete eye examination before enrollment, including biomicroscopic fundoscopy and refracted visual acuity testing using ETDRS LogMAR chart at 3 m.
To be eligible, a subject was required to have retinal thickening due to CRVO based on clinical examination involving the centre of the macula, pupil dilation of 5 mm or larger and CRVO of less than 1 year duration. All patients were included consecutively. Subjects were excluded if there was a history of diabetes.
Epidemiological data including age, sex, duration of symptoms and medical history was recorded. Retinal thickness measurements were made with the Topcon 3D OCT-1000: at 9 a.m., 11 a.m., 1 p.m., 3 p.m., 5 p.m. Central macular zone thickness, defined as the central-most zone of the 9 zones defined by the ETDRS protocol was measured. In addition, at 9 a.m. and 5 p.m. visual acuity was recorded using ETDRS LogMAR.
SPSS version 13.0 was used for statistical analysis of data. As the sample was small, and did not demonstrate a normal distribution, Friedman test was used for repeated measures analysis and Wilcoxon signed rank test for pair-wise comparison to assess at which time points there was significant change in central macula thickness. All tests were two-tailed and a p value (asymptotic value) of less than 0.05 was considered significant.
As the unaffected eye in each subject was used as the control, and therefore cannot be considered to be truly independent, the difference between the maximum and minimum values of CMT in the unaffected and affected eyes were compared to determine if there was a significant change in the disease eye unrelated to subject variations.
Hospital ethics committee approval was obtained for the study. Before recruitment, a full explanation of the nature of this procedure was conveyed to the patient (in accordance with the Helsinki declaration).
Results
Table 1 indicates patient demographics. There were seven males and three females with average age of 59.4 years (range 40–80 years). The average duration of symptoms was 5.4 months (range 3–9 months). Seven patients were on treatment for hypertension and four patients were on treatment for increased serum cholesterol. One patient was on treatment for primary open angle glaucoma(POAG), and the rest had no associated ocular history.
Table 2 and Figs. 1 and 2 show visual acuity and central macular thickness in eyes with CRVO. In eyes with CRVO median CMT changed from 571 µm (25th centile 377, 75th centile 631.8) at 9 a.m. to 475 µm (242,562) at 5 p.m. The other corresponding values were: at 11 a.m. 542.5 µm (325.3, 627.3), 1 p.m. 505.5 µm (322.8, 562.3), and 3 p.m. 472.0 µm (308, 508). Median visual acuity at 9 a.m. was 1.00 (0.79, 1.02) and at 5 p.m. 0.93 (0.81, 1.00)
Comparison of CMT at 9.00 A.M. to each of the subsequent time intervals found that there was a significant change in the CMT (the absolute p value between 9 and 11 a.m. was 0.032, and 0.005 between subsequent 9–1 p.m., 9–3 p.m. and 9–5 p.m. intervals). The decrease in CMT was also found to be significant between each 2-hour time interval except the time interval between 3 p.m. and 5 p.m..
In the unaffected eyes, the median CMT at 9 a.m. was 218.0 μm (197.8, 247.3) CMT at 5 p.m. was 203.06 μm (191.5, 231.5). The other corresponding values were: at 11 a.m. 216.0 µm (196.0, 252.0), 1 p.m. 211.5 µm (192.5, 252.5), and 3 p.m. 207.0 µm (191.5, 245.0). Median visual acuity at 9 a.m. and 5 p.m. was 0.00 (−0.05, 0.08). It was found that there was a small but significant difference in CMT at 3 p.m. (p = 0.04) and 5 p.m. (p = 0.04) compared to 9 a.m.
As the decrease in CMT was also found in normal eyes of the subject, it was important to ascertain that the degree of variability in the affected eye was significant and not due to subject factors. To do this, the difference between the maximum and minimum values in the CRVO (median difference 86.5 μm) and unaffected eye (median difference 6.75 μm) was compared (p = 0.0074) which showed that there is an exaggerated increase in CMT in affected eyes.
Wilcoxon rank test was used to assess the differences in visual acuity at the two time points in the CRVO eyes. There was no statistical difference found at the 95% level of significance (p = 0.06), and change in macular thickness did not correlate significantly with a change in visual acuity (p = 0.27) in eyes affected by CRVO.
Discussion
The objective of our study was to evaluate changes in CMT measured by OCT throughout the day in eyes with CMO and CRVO. All patients in our series had a significantly higher CMT at 9 a.m., which gradually reduced over the course of the day.
In previous studies reduction in CMT during the day has been shown in diabetic patients. Frank et al. [3] in a study of ten subjects, measured retinal thickness at 8 a.m., 11 a.m., 2:00 p.m., and 5:00 p.m. Subset analysis revealed temporal variation in thickness with greater oedema in the morning and less late in the day in patients with an initial macular thickness of more than 400 um. A study by Larsen et al. [4] of 12 diabetic patients showed an overnight increase in CMT of an average of 6.3%, with no change in seven control subjects. The patients with diabetic macular oedema also demonstrated a mean loss of 5 ETDRS letters of acuity overnight. Polito et al. [5] studied the effect of posture on diurnal variation in diabetic CMO. The average relative decrease in foveal thickening was 20.6% in upright position and 6.2% in recumbent position between 9 a.m. and 6 p.m.
In our study, there was an average decrease in CMT of approximately 17.6% which was measured at five points of time during the day. Even the fellow unaffected eyes showed a small decrease in CMT over the day. Our findings are in agreement with the study by Paques et al. [8] who reported significant reduction (p < 0.001) in macular thickness and visual acuity (p < 0.002) between 7 a.m. and 7 p.m. in 16 eyes with CRVO.
A number of mechanisms may be involved in reducing CMO in CRVO during the day, for example hydrostatic pressure gradient [12] and a gravitational effect with change in posture. Erect posture during the day may increase venous drainage. Indeed, in diabetics CMO has been shown to decrease in relation to erect posture during the day [6, 7]. Variation in CMO may also be driven by variations of retinal metabolism. The oxygen consumption rate by the retina of experimental animals is higher in the dark-adapted state, e.g. overnight [9–11]. In a hypoxic retina, the effects of ischemia may be more severe during the night because of increased metabolism activating pathways which may cause worsening of CMO. In addition, in most healthy individuals there is a nocturnal decline in mean systolic blood pressure (SBP) of at least 10% from daytime values [13]. Paques et al. [8] recently demonstrated that there was correlation between variations in systolic and diastolic pressure and CMT, i.e., loss of the normal pressure dip during the night was correlated with an increase in CMT in the morning.
If the trigger factor for increased CMO in the morning can be identified, than strategies to reduce CMO can be devised, e.g., erect posture, blood pressure reduction in hypertensive patients or hyperbaric oxygen [14] to aid metabolism in the ischemic retina. We understand one of the weakness of this study is the small number (n = 10). Further studies are needed to investigate these factors in diurnal variation in CMO.
In conclusion, patients with CRVO demonstrate an increase in CMO in the morning compared with late morning and afternoon. Possible causes are postural changes, hypertension and retinal metabolism overnight.
References
Williamson TH (1997) Central retinal vein occlusion: what’s the story? Br J Ophthalmol 81:698–704
Weinberg DV (2000) Venous occlusive disease of the retina. In: Albert DM, Jakobiec FA, Azar DT et al (eds) Principles and practice of ophthalmology, 2nd edn. WB Saunders Co, Philadelphia, PA, pp 1887–1900
Frank RN, Schulz L, Abe K, Iezzi R (2004) Temporal variation in diabetic macular edema measured by optical coherence tomography. Ophthalmology 111:211–217, doi:10.1016/j.ophtha.2003.05.031
Larsen M, Wang M, Sander B (2005) Overnight thickness variation in diabetic macular oedema. Invest Ophthalmol Vis Sci 46:2313–2316, doi:10.1167/iovs.04-0893
Polito A, Polini G, Chiodini RG, Isola M, Soldano F, Bandello F (2007) Effect of posture on the diurnal variation in clinically significant diabetic macular oedema. Invest Ophthalmol Vis Sci 48:3318–3323, doi:10.1167/iovs.06-1526
Polito A, Del Borrello M, Polini G, Furlan F, Isola M, Bandello F (2006) Diurnal variation in clinically significant diabetic macular edema measured by the stratus OCT. Retina 26:14–20, doi:10.1097/00006982-200601000-00003
Diabetic Retinopathy Clinical Research Network (2006) Diurnal variation in retinal thickening measurement by optical coherence tomography in center-involved diabetic macular oedema. Arch Ophthalmol 124:1701–1707
Paques M, Massin P, Sahel JA, Gaudric A, Bergmann JF, Azancot S, Lévy BI, Vicaut E (2005) Circadian fluctuations of macular oedema in patients with morning vision blurring: correlation with arterial pressure and effect of light deprivation. Invest Ophthalmol Vis Sci 46:4707–4711, doi:10.1167/iovs.05-0638
Braun RD, Linsenmeier RA, Goldstick TK (1995) Oxygen consumption in the inner and outer retina of the cat. Invest Ophthalmol Vis Sci 36:542–554
Linsenmeier RA (1986) Effects of light and darkness on oxygen distribution and consumption in the cat retina. J Gen Physiol 88:521–542, doi:10.1085/jgp.88.4.521
Cringle SJ, Yu DY, Yu PK, Su EN (2002) Intraretinal oxygen consumption in the rat in vivo. Invest Ophthalmol Vis Sci 43:1922–1927
Ganong WF (1989) Review of medical physiology, 14th edn. Appleton & Lange, Norwalk, CT, p 498
Millar-Craig MW, Bishop CN, Raftery EB (1978) Circadian variation of blood-pressure. Lancet 1:795–797, doi:10.1016/S0140-6736(78)92998-7
Chang YH, Chen PL, Tai MC, Chen CH, Lu DW, Chen JT (2006) Hyperbaric oxygen therapy ameliorates the blood—retinal barrier breakdown in diabetic retinopathy. Clin Experiment Ophthalmol 34:584–589, doi:10.1111/j.1442-9071.2006.01207.x
Author information
Authors and Affiliations
Corresponding author
Additional information
Ethical Committee: Guys and St Thomas’ Hospital Ethic Committee Approval
Rights and permissions
About this article
Cite this article
Gupta, B., Grewal, J., Adewoyin, T. et al. Diurnal variation of macular oedema in CRVO: prospective study. Graefes Arch Clin Exp Ophthalmol 247, 593–596 (2009). https://doi.org/10.1007/s00417-008-1011-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-008-1011-4