Abstract
Background
Artificial intelligence (AI) has influenced all aspects of human life and neurology is no exception to this growing trend. The aim of this paper is to guide medical practitioners on the relevant aspects of artificial intelligence, i.e., machine learning, and deep learning, to review the development of technological advancement equipped with AI, and to elucidate how machine learning can revolutionize the management of neurological diseases. This review focuses on unsupervised aspects of machine learning, and how these aspects could be applied to precision neurology to improve patient outcomes. We have mentioned various forms of available AI, prior research, outcomes, benefits and limitations of AI, effective accessibility and future of AI, keeping the current burden of neurological disorders in mind.
Discussion
The smart device system to monitor tremors and to recognize its phenotypes for better outcomes of deep brain stimulation, applications evaluating fine motor functions, AI integrated electroencephalogram learning to diagnose epilepsy and psychological non-epileptic seizure, predict outcome of seizure surgeries, recognize patterns of autonomic instability to prevent sudden unexpected death in epilepsy (SUDEP), identify the pattern of complex algorithm in neuroimaging classifying cognitive impairment, differentiating and classifying concussion phenotypes, smartwatches monitoring atrial fibrillation to prevent strokes, and prediction of prognosis in dementia are unique examples of experimental utilizations of AI in the field of neurology. Though there are obvious limitations of AI, the general consensus among several nationwide studies is that this new technology has the ability to improve the prognosis of neurological disorders and as a result should become a staple in the medical community.
Conclusion
AI not only helps to analyze medical data in disease prevention, diagnosis, patient monitoring, and development of new protocols, but can also assist clinicians in dealing with voluminous data in a more accurate and efficient manner.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
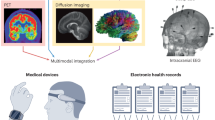
In 1956, an American computer scientist John McCarthy first introduced the term and principles of ‘artificial intelligence (AI)’ [1, 2]. The term AI is used to describe ‘machines’ capable of demonstrating cognitive functions that humans associate with other human minds such as ‘learning’ and ‘problem solving’ [3]. The foundation of AI is ‘machine learning’, a form of intelligence based on the compilation of a complex algorithm and software that mimics the human mind to decipher critical problems that include visual perception, speech recognition, and decision-making [4]. Similarly, ‘deep learning’ is described as a class of artificial neural networks that learn in a supervised and unsupervised manner [5] (Fig. 1).
In health care, AI uses this ability to analyze medical data in disease prevention, diagnosis, patient monitoring, and development of new protocols [6]. Clinicians today are drowning in voluminous data, but AI gives the hope of easing the burden [7]. After the digitization of health-care data beginning in the mid-1960s until the incorporation of the electronic health record (EHR) in the American Recovery and Reinvestment Act 2009 [8], the increasing availability and progress of analytical techniques are opening new doors in health care [9]. AI is helping clinicians assess only clinically relevant information buried under massive amounts of data.
Neurological disorders comprise structural, biochemical or electrical abnormalities of the brain, spinal cord and nerves. With increasing population and aging, the burden of chronic neurological disorders has increased substantially despite a decrease in mortality due to stroke and other communicable neurological diseases [10]. In 2014, nine of the most common neurological disorders—dementia, stroke, epilepsy, Parkinson's disease, multiple sclerosis, migraine, and tension-type headache—cost the US economy nearly $789 billion [11]. In 2015, neurological disorders caused 250.7 million disability-adjusted life years (DALYs), which comprised 10.2% of global DALYs and 9.4 million deaths, and16.8% of global deaths [12]. Today, neurology faces multiple challenges in the field of diagnostic and management modalities. This ranges from simple issues like identification of healthy sleep patterns to more complicated issues like early detection and reduction in the duration of rehabilitation of acute ischemic stroke diagnosis of rare subtypes of epilepsy and prevention of sudden unexpected death in epilepsy (SUDEP), or considering multiple attributes of epilepsy and inter-observer variability of reading EEG. The vast amount of data compiled in neurology every year requires deep learning to structuralize the data to help neurologists in making an early diagnosis and improving care [13]. Artificial Intelligence has gained a lot of attention in the realms of detecting, diagnosing, and even preventing irreversible outcomes due to neurological disorders [13].
The founding principle of precision medicine is AI, which will eventually be part of neurological management. It is an emerging approach for disease treatment and prevention that takes multiple variables such as gene, environment, and lifestyle into account. It has the potential to work at an unprecedented rate by using massive computer power without any human programming [14]. The future of AI in every field is reassuring, especially in neurology from the prediction of outcomes of seizure disorder, grading of brain tumors, upskilling neurosurgical procedures, rehabilitation of stroke patients to smartphone apps monitoring patient symptoms and progress, the future seems promising [15]. During the last two decades, multiple gadgets equipped with artificial intelligence have been invented and researched to improve the functionality, diagnostic efficiency, and prognosis in patients suffering from neurological disorders. Few examples of such include the Apple Watch monitoring tremors and asymptomatic arrhythmia; iPad devices monitoring patient drawing capability with suspected movement disorders; CT scans and MRI equipped with AI to help radiologists diagnose complicated images; AI health applications to improve patient medication adherence; EpiFinder application to identify seizure types and epilepsy syndromes for triage [16]. A new horizon is emerging in neurology in the form of artificial intelligence, helping patients to improve their prognosis.
The primary objective of this narrative review is to highlight the emerging AI technologies that are creating new ways of neurological disorder management and improvement of patients’ overall functional outcomes. We have described various forms of AI used and available for use, as well as prior research, outcomes, benefits, and limitations of AI, effective accessibility and future of AI, keeping the current burden of neurological disorders in mind.
Discussion
Types of AI and prior research
In spite of the voluminous research helping to diagnose a complex spectrum of diseases, the translation into clinical practice has been challenging. Machine learning (ML) may be able to bridge the gap between translation of relevant clinical data and accurate clinical diagnosis [7]. Smart devices with AI technology, including smartwatches, smartphones, and tablets are being used by researchers not only to identify and stratify complex movement disorders [17] or arrhythmias including atrial fibrillation [18], but also to predict aspiration pneumonia in patients with swallowing difficulties secondary to stroke and dementia [19] and to improve medication compliance in patients on anticoagulation therapy [20]. Epileptologists are using smart devices with wrist annotated sensors to detect seizure activity [12, 21] and AI-enabled iPads to come up with a differential diagnosis and therapeutic approaches for rare epilepsy syndromes [22]. These studies could further pave a way to a better understanding of the pathophysiology involved in SUDEP [21]. Table 1 lists various types of AI technology and their clinical applications in neurological disorders.
Different algorithms play an integral part in ML. ML algorithms such as random forest that use neuroimaging data in small sample data with high-dimensional parameter spaces are more stable than other algorithms and have been successful not only in classification of dementia, including mild cognitive impairment (MCI) [23] and Alzheimer’s [24], but also in other disorders including psychogenic non-epileptic seizures (PNES) [23, 25], Parkinson's disease [26, 27], and schizophrenia. In the same note, different algorithms have been used in the classification of similar disorders such as dementia [23, 25, 28]. Algorithms of the self-organizing map have been used by a group of researchers to identify distinctive phenotypes among concussive patients [29]. Deep learning algorithms are being used to predict the time since stroke onset (TSS) to help clinicians come up with better tools to guide stroke treatment [19]. EpiFinder algorithms help in diagnosing seizure in adult patients with spells [22]. These tools can help diagnose elusive disorders and prevent delay in diagnosis and treatment. Prior studies, utilizing the role of AI in neurological care, are mentioned in Table 2.
Stroke
Stroke is the leading cause of disability and the fifth leading cause of death in the USA (102). Each year 795,000 Americans experience a new or recurrent stroke [30], and an estimated 24 billion dollars is spent annually on direct medical expenses [30]. Only 5% or fewer receive intravenous thrombolytic therapy in spite of the urgent need to administer it to preserve tissue in acute ischemic stroke [31, 32]. This can be due to lack of physician experience in administering thrombolytics, risk of 6% hemorrhage with thrombolytics, patients living in rural areas with limited resources, and strokes are unwitnessed or wake-up strokes [31,32,33,34]. Thus, there is an urgent need to streamline care and improve technology to solve this complex issue and bring down the rising costs [35]. ML has shown that it not only predicts the risk of recurrent stroke within 1 year after a TIA or minor stroke [36], but also predicts time since stroke onset (TSS) and is a better alternative than current DWI–FLAIR mismatch [37,38,39,40,41,42] in patients with unknown TSS (wake-up strokes or unwitnessed strokes); thus, it guides physicians to make better therapeutic approaches [19]. Smart devices with apps, using techniques like photoplethysmography, and handheld electrocardiograph recorders with greater accuracy are being used to check the heart rate and heart rate variability and to screen for asymptomatic atrial fibrillation which helps to prevent embolic stroke [18].
Epilepsy
Given its varied clinical manifestations, the rates of misdiagnosis are 26% in epilepsy centers and 20–40% in community settings. This often leads to unwarranted investigations and treatments [43]. Machine learning applications in epilepsy ranges from diagnosis of epilepsy [22, 44], PNES [45], and rare subtypes of epilepsy to the prevention of SUDEP and minimizing inter-observer variability of EEG interpretation.
Rajagopalan et al. showed that ML can diagnose temporal epilepsy by detecting microstate alterations than depending on ictal or interictal charges on repeated scalp EEG [44]. These, in turn, are affected by a multitude of factors such as medications, sleep deprivation, and inter-observer variability [46]. ML-detected alterations in microstate C shows a possible reflection of the inappropriate activation of alpha activity [47,48,49] with 76.1% accuracy, even in the absence of a visible interictal epileptiform (IED) discharges on EEG [44]. The EpiFinder algorithm used in a tertiary center was able to generate a differential of seizure types and epilepsy syndromes from other spells [22].
A pilot study using wristband sensors detected increased EDA, i.e., epidermal activity in epileptic seizures. The increase in EDA was proportionally higher in generalized tonic–clonic seizures (GTCS) versus complex partial seizures (CPS) [21]. Similar observations have been noted by Van Buren in 1958 [50], and elevated plasma catecholamines following GTCS support this assumption [51, 52]. They propose that this autonomic instability of sympathetic surge during seizures could play a role in SUDEP [21].
Psychogenic non-epileptic seizures (PNES) resemble epileptic seizures and consist of episodes of paroxysmal behavioral manifestations including a range of motor, sensory, and behavioral manifestations [53, 54]. 20% of the epilepsy patients referred to a tertiary center are eventually diagnosed with PNES using the gold standard video electroencephalography (vEEG); hence, there is a need to identify better, quicker, and affordable tests to reduce the significant chronic disability, lost wage hours, multiple hospitalizations, and associated risk of morbidity and mortality [53,54,55,56,57].
A group from Italy was able to identify PNES using ML with multivariate neuroimaging analysis and also secondarily locate brain regions within the limbic and the right inferior frontal cortex (IFC) [45]. IFC has also been implicated in other disorders such as compulsive–impulsive disorders, Tourette syndrome, and Parkinson's disease with levodopa-induced dyskinesia [58]. The EpiFinder algorithm used in a tertiary center was able to differentiate epileptic seizures from PNES [22].
Concussion
Concussion is another multidimensional problem with no validated criteria for diagnosis, leading to inter-examiner variability [59,60,61,62]. Its clinical presentation varies from cognitive to non-cognitive domains including sleep and balance [62,63,64,65,66]. Prior studies have focused on scans, symptoms, and cognitive testing [62, 65, 66] despite its varied symptomatology.
ML has not only been able to differentiate concussed and control subjects, and improve diagnosis based on individual data including conventional imaging, cognitive domains, eye movement, and clinical presentation [66,67,68,69,70,71,72,73,74], but has also made it possible to look into less understood and complex pathologies such as vestibular impairments [75,76,77,78,79], to better understand and identify varied phenotypes like cognitive problems, oculomotor dysfunction, affective disturbances, cervical spine disorders, headaches, and cardiovascular and vestibular anomalies [29, 80].
Dementia
Frontotemporal dementia (FTD) is a neurodegenerative disorder that accounts for 20% of young-onset dementia and has a high rate of misdiagnosis [81, 82]. This often leads to poor patient satisfaction and well-being, unnecessary laboratory tests, clinic visits, and imaging, and addition to the health-care costs [28, 83]. It has the worst prognosis and reduced life expectancy when compared to other dementias [12]. A study in the UK has shown that deep learning algorithms can reduce unnecessary investigations and improve costs and patient satisfaction through better clinical practice guidelines [28].
Movement disorders
The diagnosis of the two most common movement disorders, Parkinson’s disease (PD) and essential tremor (ET), is challenging and based primarily on clinical criteria [84]. Researchers are using novel methods to synchronize data into deep learning from tremor characteristics in varied environments, questionnaires addressing non-motor issues, and Archimedean spirals drawn to identify newer phenotypes [17]. Prior studies have used each of these characteristics individually to diagnose movement disorders [85].
Outcomes and limitations
As discussed above, AI has played an important role in identifying neurological disorders [13]. It has been transformational in converting the voluminous data collected into those of clinical relevance [13]. For all the benefits, however, there are huge limitations and unknown legal ramifications.
First, there is a lack of data standards and open data repositories in machine learning [7, 86]. For example, limitations in the integration of already available commercial medical devices such as Parkinson’s Kinetigraph TM into routine health care have been secondary to non-integration of motor and nonmotor characteristics, lacking open data storages and open programs [87]. Varghese et al. have overcome the limitations mentioned by not only integrating motor and non-motor phenomena, but also by using large data models with massive infrastructure like Medical-Data Models Portal (MDM), and combining affordable devices with customizable apps and SDS (smart device systems) that can be programmed by any Apple-based App developer [17]. This can help reach the level of data required to quicken the regulatory steps and rollout devices sooner with improved diagnostic accuracy [17, 84, 88] (Table 3).
Moreover, deep learning will never be 100% complete, especially with inter-examiner differences and varied environments [17]. Studies reveal that data entered by specialists improve performance in deep learning methods especially with pattern recognition [17].
In ML, there is some literature that the size of the samples should be a multiple of the number of input and output variables [19] nonetheless studies were affected by small sample size [17, 44, 45].
ML’s clinical application in confounding groups with similar neurological, psychological, or pathological presentation is limited [45]: for instance, ML’s application in distinguishing PNES not only from patients with epilepsy, but also with similar psychopathological presentation such as major depression [45], or ML’s ability to distinguish epilepsy from healthy controls [44] versus application in patients with panic disorder [89], schizophrenia [90], drug-induced, and memory deficit with similar alterations in microstate C [44].
AI or deep learning uses different reasoning methods to diagnose a disease. A systematic review by Arani et al. in multiple sclerosis showed different reasoning methods or a combination of methods, e.g., case based, rule based, model based, fuzzy logic, genetic algorithms, natural language processing, and neural networks were used by different computers and each method had its own capabilities and limitations [91]. The efficiency of each method varied, and, hence, affected its applicability in the diagnosis of rare and complicated disease such as multiple sclerosis [91]. Nonetheless, they can play a major role in helping patients and physicians with timely clinical diagnosis [91].
It is impossible to account for all potential positive or negative side effects even with the best algorithms [28]. Deep learning algorithms tend to avoid negative side effects and confounding factors like test results to achieve its goal, and thus in turn can affect patient safety and outcomes [28, 92].
Mobile apps are currently being used to monitor paroxysmal AF and long-term anticoagulation (39) and have shown to be effective tools in monitoring and screening of arrhythmias [18], but this has often led to a large number of false positives and in turn to expensive and unnecessary testing [18, 93]. This inadvertently raises the medico-legal aspect and logistics for governments and public health bodies with regard to systematic and opportunistic screening, cost-effectiveness, and management of newly identified patients with AF [18]; hence, a better understanding of local screening guidelines is required, e.g., European Heart Rhythm Association Consensus guidelines on screening AF.
Lastly, the ethical and legal ramifications are beyond the scope of this paper, but sustaining patient trust would be the key in promoting collaboration and implementation of AI [94].The black box scenario is that decisions made by AI-enabled computer-aided diagnosis (CAD) systems [95] cannot be explained. The legal ramifications of a misdiagnosis are unclear, especially with regard to whether the fault lies with the manufacturer or the physician [95,96,97]. We need to develop standard practices for evaluation of AI tools [98]. It is debatable whether AI will replace physicians, but AI will definitely be playing a greater role in integrating health care [94].
Future directions
Deep brain stimulation (DBS) is an effective surgical treatment option and improves quality of life in patients with tremor manifestation, including Parkinson’s (PD) and essential tremor (ET) [99,100,101,102]. Currently, determination of DBS leads is done by a neurologist, and is therefore affected by interpersonal variability. AI may help in this regard to make an objective evaluation, subject to fulfilling the regulatory requirements and getting medical clearance [17].
Using open data portals can be in the best shared interest to develop data standards and smart devices [86]. Some researchers have made the study models, frameworks, codes, and anonymized data samples open source, which makes it easier to reproduce in future studies [17]. Using devices that are affordable with customizable apps that are available to the masses increases their applicability [17]. For example, Kardiaband app by AliveCor is the first FDA-cleared smartwatch-based ECG reader [103].
Standard auditing and statistics only can test known hypotheses, but newer algorithms can test multiple hypotheses in a reasonable time frame and make a priori assumptions [28] beyond the scope of human capabilities. This has the potential to be applied across other diseases and specialties [28]. ML specifically is able to analyze large datasets at much quicker speeds and at higher accuracy to investigate unexplained phenomena [15]. ML algorithms like self-organizing map (SOM) can be extended to include non-vestibular parameters, including previous concussions, neuropsychological outcomes, and multiple other variables to validate studies in a more complicated context [29]. This also help to improve diagnostic criteria by identifying features among varied patient populations [16].
Conclusion
The current neurological care not only places a burden on the US economy by imposing higher overall costs, but also affects disability-adjusted life years. The ability of AI and ML to analyze medical data in disease prevention, diagnosis, patient monitoring, and development of new protocols will help clinicians to deal with voluminous data in a more accurate and efficient manner. AI has the ability to limit inter-observer variability, screen for asymptomatic atrial fibrillation, diagnose epilepsy, PNES, concussions, and movement disorders, and identify abnormal autonomic functions to prevent SUDEP. Though AI utilization is limited for a wide variety of reasons including physician’s reluctance to adopt novel technology, billing and reimbursement issues, pan-USA licensing problems, malpractice lawsuits, and the initial cost of technological establishment, it has the potential to serve as a powerful tool for neurological care.
References
Cukier K (2019) Ready for Robots? How to think about the future of AI. Foreign Affairs 98:192
Myers A (2011) Stanford's John McCarthy, seminal figure of artificial intelligence, dies at 84. Stanford Report. https://news.stanford.edu/news/2011/october/john-mccarthy-obit-102511.html. Accessed 14 Jul 2019
Russell SJ, Norvig P (2010) Artificial intelligence—a modern approach, 3rd edn. Pearson Education Inc, Upper Saddle River, New Jersey
Konar A (1999) Artificial intelligence and soft computing—behavioral and cognitive modeling of the human brain. CRC Press, Boca Raton. https://doi.org/10.1201/9781315219738
Deng L, Yu D (2014) Deep learning: methods and applications. Found Trends Signal Process 7(3–4):197–387. https://doi.org/10.1561/2000000039
Pantelopoulos A, Bourbakis NG (2010) A survey on wearable sensor-based systems for health monitoring and prognosis. IEEE Trans Syst Man Cybern Part C 40(1):1–12. https://doi.org/10.1109/TSMCC.2009.2032660
D A (2018) Artificial intelligence for authentic engagement. Syneos health communications. https://syneoshealthcommunications.com/perspectives/artificial-intelligence. Accessed 4 Apr 2018
Henricks WH (2011) "Meaningful use" of electronic health records and its relevance to laboratories and pathologists. J Pathol Inform 2:7. https://doi.org/10.4103/2153-3539.76733
Flores M, Glusman G, Brogaard K, Price ND, Hood L (2013) P4 medicine: how systems medicine will transform the healthcare sector and society. Personal Med 10(6):565–576. https://doi.org/10.2217/pme.13.57
Murray CJ, Vos T, Lozano R, Naghavi M, Flaxman AD, Michaud C, Ezzati M, Shibuya K, Salomon JA, Abdalla S, Aboyans V, Abraham J, Ackerman I, Aggarwal R, Ahn SY, Ali MK, Alvarado M, Anderson HR, Anderson LM, Andrews KG, Atkinson C, Baddour LM, Bahalim AN, Barker-Collo S, Barrero LH, Bartels DH, Basanez MG, Baxter A, Bell ML, Benjamin EJ, Bennett D, Bernabe E, Bhalla K, Bhandari B, Bikbov B, Bin Abdulhak A, Birbeck G, Black JA, Blencowe H, Blore JD, Blyth F, Bolliger I, Bonaventure A, Boufous S, Bourne R, Boussinesq M, Braithwaite T, Brayne C, Bridgett L, Brooker S, Brooks P, Brugha TS, Bryan-Hancock C, Bucello C, Buchbinder R, Buckle G, Budke CM, Burch M, Burney P, Burstein R, Calabria B, Campbell B, Canter CE, Carabin H, Carapetis J, Carmona L, Cella C, Charlson F, Chen H, Cheng AT, Chou D, Chugh SS, Coffeng LE, Colan SD, Colquhoun S, Colson KE, Condon J, Connor MD, Cooper LT, Corriere M, Cortinovis M, de Vaccaro KC, Couser W, Cowie BC, Criqui MH, Cross M, Dabhadkar KC, Dahiya M, Dahodwala N, Damsere-Derry J, Danaei G, Davis A, De Leo D, Degenhardt L, Dellavalle R, Delossantos A, Denenberg J, Derrett S, Des Jarlais DC, Dharmaratne SD, Dherani M, Diaz-Torne C, Dolk H, Dorsey ER, Driscoll T, Duber H, Ebel B, Edmond K, Elbaz A, Ali SE, Erskine H, Erwin PJ, Espindola P, Ewoigbokhan SE, Farzadfar F, Feigin V, Felson DT, Ferrari A, Ferri CP, Fevre EM, Finucane MM, Flaxman S, Flood L, Foreman K, Forouzanfar MH, Fowkes FG, Fransen M, Freeman MK, Gabbe BJ, Gabriel SE, Gakidou E, Ganatra HA, Garcia B, Gaspari F, Gillum RF, Gmel G, Gonzalez-Medina D, Gosselin R, Grainger R, Grant B, Groeger J, Guillemin F, Gunnell D, Gupta R, Haagsma J, Hagan H, Halasa YA, Hall W, Haring D, Haro JM, Harrison JE, Havmoeller R, Hay RJ, Higashi H, Hill C, Hoen B, Hoffman H, Hotez PJ, Hoy D, Huang JJ, Ibeanusi SE, Jacobsen KH, James SL, Jarvis D, Jasrasaria R, Jayaraman S, Johns N, Jonas JB, Karthikeyan G, Kassebaum N, Kawakami N, Keren A, Khoo JP, King CH, Knowlton LM, Kobusingye O, Koranteng A, Krishnamurthi R, Laden F, Lalloo R, Laslett LL, Lathlean T, Leasher JL, Lee YY, Leigh J, Levinson D, Lim SS, Limb E, Lin JK, Lipnick M, Lipshultz SE, Liu W, Loane M, Ohno SL, Lyons R, Mabweijano J, MacIntyre MF, Malekzadeh R, Mallinger L, Manivannan S, Marcenes W, March L, Margolis DJ, Marks GB, Marks R, Matsumori A, Matzopoulos R, Mayosi BM, McAnulty JH, McDermott MM, McGill N, McGrath J, Medina-Mora ME, Meltzer M, Mensah GA, Merriman TR, Meyer AC, Miglioli V, Miller M, Miller TR, Mitchell PB, Mock C, Mocumbi AO, Moffitt TE, Mokdad AA, Monasta L, Montico M, Moradi-Lakeh M, Moran A, Morawska L, Mori R, Murdoch ME, Mwaniki MK, Naidoo K, Nair MN, Naldi L, Narayan KM, Nelson PK, Nelson RG, Nevitt MC, Newton CR, Nolte S, Norman P, Norman R, O'Donnell M, O'Hanlon S, Olives C, Omer SB, Ortblad K, Osborne R, Ozgediz D, Page A, Pahari B, Pandian JD, Rivero AP, Patten SB, Pearce N, Padilla RP, Perez-Ruiz F, Perico N, Pesudovs K, Phillips D, Phillips MR, Pierce K, Pion S, Polanczyk GV, Polinder S, Pope CA 3rd, Popova S, Porrini E, Pourmalek F, Prince M, Pullan RL, Ramaiah KD, Ranganathan D, Razavi H, Regan M, Rehm JT, Rein DB, Remuzzi G, Richardson K, Rivara FP, Roberts T, Robinson C, De Leon FR, Ronfani L, Room R, Rosenfeld LC, Rushton L, Sacco RL, Saha S, Sampson U, Sanchez-Riera L, Sanman E, Schwebel DC, Scott JG, Segui-Gomez M, Shahraz S, Shepard DS, Shin H, Shivakoti R, Singh D, Singh GM, Singh JA, Singleton J, Sleet DA, Sliwa K, Smith E, Smith JL, Stapelberg NJ, Steer A, Steiner T, Stolk WA, Stovner LJ, Sudfeld C, Syed S, Tamburlini G, Tavakkoli M, Taylor HR, Taylor JA, Taylor WJ, Thomas B, Thomson WM, Thurston GD, Tleyjeh IM, Tonelli M, Towbin JA, Truelsen T, Tsilimbaris MK, Ubeda C, Undurraga EA, van der Werf MJ, van Os J, Vavilala MS, Venketasubramanian N, Wang M, Wang W, Watt K, Weatherall DJ, Weinstock MA, Weintraub R, Weisskopf MG, Weissman MM, White RA, Whiteford H, Wiebe N, Wiersma ST, Wilkinson JD, Williams HC, Williams SR, Witt E, Wolfe F, Woolf AD, Wulf S, Yeh PH, Zaidi AK, Zheng ZJ, Zonies D, Lopez AD, AlMazroa MA, Memish ZA (2012) Disability-adjusted life years (DALYs) for 291 diseases and injuries in 21 regions, 1990–2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet 380(9859):2197–2223. https://doi.org/10.1016/s0140-6736(12)61689-4
Gooch CL, Pracht E, Borenstein AR (2017) The burden of neurological disease in the United States: a summary report and call to action. Ann Neurol 81(4):479–484. https://doi.org/10.1002/ana.24897
Onorati F, Regalia G, Caborni C, Migliorini M, Bender D, Poh MZ, Frazier C, Kovitch Thropp E, Mynatt ED, Bidwell J, Mai R, LaFrance WC Jr, Blum AS, Friedman D, Loddenkemper T, Mohammadpour-Touserkani F, Reinsberger C, Tognetti S, Picard RW (2017) Multicenter clinical assessment of improved wearable multimodal convulsive seizure detectors. Epilepsia 58(11):1870–1879. https://doi.org/10.1111/epi.13899
Wahl B, Cossy-Gantner A, Germann S, Schwalbe NR (2018) Artificial intelligence (AI) and global health: how can AI contribute to health in resource-poor settings? BMJ Glob Health 3(4):e000798. https://doi.org/10.1136/bmjgh-2018-000798
Mesko B (2017) The role of artificial intelligence in precision medicine. Expert Rev Precis Med Drug Dev 2(5):239–241. https://doi.org/10.1080/23808993.2017.1380516
Hassabis D, Kumaran D, Summerfield C, Botvinick M (2017) Neuroscience-inspired artificial intelligence. Neuron 95(2):245–258. https://doi.org/10.1016/j.neuron.2017.06.011
Ganapathy K, Abdul SS, Nursetyo AA (2018) Artificial intelligence in neurosciences: a clinician's perspective. Neurol India 66(4):934–939. https://doi.org/10.4103/0028-3886.236971
Varghese J, Niewohner S, Soto-Rey I, Schipmann-Miletic S, Warneke N, Warnecke T, Dugas M (2019) A smart device system to identify new phenotypical characteristics in movement disorders. Front Neurol 10:48. https://doi.org/10.3389/fneur.2019.00048
Li KHC, White FA, Tipoe T, Liu T, Wong MC, Jesuthasan A, Baranchuk A, Tse G, Yan BP (2019) The current state of mobile phone apps for monitoring heart rate, heart rate variability, and atrial fibrillation: narrative review. JMIR mHealth uHealth 7(2):e11606. https://doi.org/10.2196/11606
Ho KC, Speier W, Zhang H, Scalzo F, El-Saden S, Arnold CW (2019) A machine learning approach for classifying ischemic stroke onset time from imaging. IEEE Trans Med Imaging. https://doi.org/10.1109/tmi.2019.2901445
Labovitz DL, Shafner L, Reyes Gil M, Virmani D, Hanina A (2017) Using artificial intelligence to reduce the risk of nonadherence in patients on anticoagulation therapy. Stroke 48(5):1416–1419. https://doi.org/10.1161/strokeaha.116.016281
Poh MZ, Loddenkemper T, Swenson NC, Goyal S, Madsen JR, Picard RW (2010) Continuous monitoring of electrodermal activity during epileptic seizures using a wearable sensor. Conf Proc IEEE Eng Med Biol Soc 2010:4415–4418. https://doi.org/10.1109/iembs.2010.5625988
Okazaki EM, Yao R, Sirven JI, Crepeau AZ, Noe KH, Drazkowski JF, Hoerth MT, Salinas E, Csernak L, Mehta N (2018) Usage of EpiFinder clinical decision support in the assessment of epilepsy. Epilepsy Behav 82:140–143. https://doi.org/10.1016/j.yebeh.2018.03.018
Sarica A, Cerasa A, Quattrone A (2017) Random forest algorithm for the classification of neuroimaging data in Alzheimer's disease: a systematic review. Front Aging Neurosci 9:329. https://doi.org/10.3389/fnagi.2017.00329
Rathore S, Habes M, Iftikhar MA, Shacklett A, Davatzikos C (2017) A review on neuroimaging-based classification studies and associated feature extraction methods for Alzheimer's disease and its prodromal stages. NeuroImage 155:530–548. https://doi.org/10.1016/j.neuroimage.2017.03.057
Breiman L (2001) Random forests. Mach Learn 45(1):5–32. https://doi.org/10.1023/a:1010933404324
Salvatore C, Cerasa A, Castiglioni I, Gallivanone F, Augimeri A, Lopez M, Arabia G, Morelli M, Gilardi MC, Quattrone A (2014) Machine learning on brain MRI data for differential diagnosis of Parkinson's disease and Progressive Supranuclear Palsy. J Neurosci Methods 222:230–237. https://doi.org/10.1016/j.jneumeth.2013.11.016
Amoroso N, La Rocca M, Monaco A, Bellotti R, Tangaro S (2018) Complex networks reveal early MRI markers of Parkinson’s disease. Med Image Anal 48:12–24. https://doi.org/10.1016/j.media.2018.05.004
Brzezicki MA, Kobetić MD, Neumann S, Pennington C (2019) Diagnostic accuracy of frontotemporal dementia. An artificial intelligence-powered study of symptoms, imaging and clinical judgement. Adv Med Sci 64(2):292–302. https://doi.org/10.1016/j.advms.2019.03.002
Visscher RMS, Feddermann-Demont N, Romano F, Straumann D, Bertolini G (2019) Artificial intelligence for understanding concussion: Retrospective cluster analysis on the balance and vestibular diagnostic data of concussion patients. PLoS ONE 14(4):e0214525. https://doi.org/10.1371/journal.pone.0214525
Benjamin EJ, Virani SS, Callaway CW, Chamberlain AM, Chang AR, Cheng S, Chiuve SE, Cushman M, Delling FN, Deo R, Ferranti SDd, Ferguson JF, Fornage M, Gillespie C, Isasi CR, Jiménez MC, Jordan LC, Judd SE, Lackland D, Lichtman JH, Lisabeth L, Liu S, Longenecker CT, Lutsey PL, Mackey JS, Matchar DB, Matsushita K, Mussolino ME, Nasir K, O’Flaherty M, Palaniappan LP, Pandey A, Pandey DK, Reeves MJ, Ritchey MD, Rodriguez CJ, Roth GA, Rosamond WD, Sampson UKA, Satou GM, Shah SH, Spartano NL, Tirschwell DL, Tsao CW, Voeks JH, Willey JZ, Wilkins JT, Wu JH, Alger HM, Wong SS, Muntner P (2018) Heart Disease and stroke statistics—2018 update: a report from the American Heart Association. Circulation 137(12):e67–e492. https://doi.org/10.1161/CIR.0000000000000558
Al Kasab S, Adams RJ, Debenham E, Jones DJ, Holmstedt CA (2017) Medical University of South Carolina Telestroke: a telemedicine facilitated network for stroke treatment in SOUTH CAROLINA-a progress report. Telemed J e-health 23(8):674–677. https://doi.org/10.1089/tmj.2016.0229
Zhai YK, Zhu WJ, Hou HL, Sun DX, Zhao J (2015) Efficacy of telemedicine for thrombolytic therapy in acute ischemic stroke: a meta-analysis. J Telemed Telecare 21(3):123–130. https://doi.org/10.1177/1357633x15571357
Laghari FJ, Hammer MD (2017) Telestroke imaging: a review. J Neuroimaging 27(1):16–22. https://doi.org/10.1111/jon.12402
Moradiya Y, Janjua N (2013) Presentation and outcomes of "wake-up strokes" in a large randomized stroke trial: analysis of data from the International Stroke Trial. J Stroke Cerebrovasc Dis 22(8):e286–292. https://doi.org/10.1016/j.jstrokecerebrovasdis.2012.07.016
Kamal H, Lopez V, Sheth SA (2018) Machine Learning in Acute Ischemic Stroke Neuroimaging. Frontiers in neurology 9 (945). 10.3389/fneur.2018.00945
Chan KL, Leng X, Zhang W, Dong W, Qiu Q, Yang J, Soo Y, Wong KS, Leung TW, Liu J (2019) Early identification of high-risk TIA or minor stroke using artificial neural network. Front Neurol 10:171. https://doi.org/10.3389/fneur.2019.00171
Thomalla G, Rossbach P, Rosenkranz M, Siemonsen S, Krutzelmann A, Fiehler J, Gerloff C (2009) Negative fluid-attenuated inversion recovery imaging identifies acute ischemic stroke at 3 hours or less. Ann Neurol 65(6):724–732. https://doi.org/10.1002/ana.21651
Thomalla G, Cheng B, Ebinger M, Hao Q, Tourdias T, Wu O, Kim JS, Breuer L, Singer OC, Warach S, Christensen S, Treszl A, Forkert ND, Galinovic I, Rosenkranz M, Engelhorn T, Kohrmann M, Endres M, Kang DW, Dousset V, Sorensen AG, Liebeskind DS, Fiebach JB, Fiehler J, Gerloff C (2011) DWI-FLAIR mismatch for the identification of patients with acute ischaemic stroke within 4.5 h of symptom onset (PRE-FLAIR): a multicentre observational study. Lancet Neurol 10(11):978–986. https://doi.org/10.1016/s1474-4422(11)70192-2
Ebinger M, Galinovic I, Rozanski M, Brunecker P, Endres M, Fiebach JB (2010) Fluid-attenuated inversion recovery evolution within 12 hours from stroke onset: a reliable tissue clock? Stroke 41(2):250–255. https://doi.org/10.1161/strokeaha.109.568410
Emeriau S, Serre I, Toubas O, Pombourcq F, Oppenheim C, Pierot L (2013) Can diffusion-weighted imaging-fluid-attenuated inversion recovery mismatch (positive diffusion-weighted imaging/negative fluid-attenuated inversion recovery) at 3 Tesla identify patients with stroke at %3c4.5 hours? Stroke 44(6):1647–1651. https://doi.org/10.1161/strokeaha.113.001001
Koga M, Toyoda K, Kimura K, Yamamoto H, Sasaki M, Hamasaki T, Kitazono T, Aoki J, Seki K, Homma K, Sato S, Minematsu K (2014) THrombolysis for Acute Wake-up and unclear-onset Strokes with alteplase at 0.6 mg/kg (THAWS) Trial. Int J Stroke 9(8):1117–1124. https://doi.org/10.1111/ijs.12360
Thomalla G, Fiebach JB, Ostergaard L, Pedraza S, Thijs V, Nighoghossian N, Roy P, Muir KW, Ebinger M, Cheng B, Galinovic I, Cho TH, Puig J, Boutitie F, Simonsen CZ, Endres M, Fiehler J, Gerloff C (2014) A multicenter, randomized, double-blind, placebo-controlled trial to test efficacy and safety of magnetic resonance imaging-based thrombolysis in wake-up stroke (WAKE-UP). Int J Stroke 9(6):829–836. https://doi.org/10.1111/ijs.12011
Xu Y, Nguyen D, Mohamed A, Carcel C, Li Q, Kutlubaev MA, Anderson CS, Hackett ML (2016) Frequency of a false positive diagnosis of epilepsy: a systematic review of observational studies. Seizure 41:167–174. https://doi.org/10.1016/j.seizure.2016.08.005
Kr V, Rajagopalan SS, Bhardwaj S, Panda R, Reddam VR, Ganne C, Kenchaiah R, Mundlamuri RC, Kandavel T, Majumdar KK, Parthasarathy S, Sinha S, Bharath RD (2018) Machine learning detects EEG microstate alterations in patients living with temporal lobe epilepsy. Seizure 61:8–13. https://doi.org/10.1016/j.seizure.2018.07.007
Vasta R, Cerasa A, Sarica A, Bartolini E, Martino I, Mari F, Metitieri T, Quattrone A, Gambardella A, Guerrini R, Labate A (2018) The application of artificial intelligence to understand the pathophysiological basis of psychogenic nonepileptic seizures. Epilepsy Behav 87:167–172. https://doi.org/10.1016/j.yebeh.2018.09.008
Javidan M (2012) Electroencephalography in mesial temporal lobe epilepsy: a review. Epilepsy Res Treat 2012:17. https://doi.org/10.1155/2012/637430
Milz P, Pascual-Marqui RD, Achermann P, Kochi K, Faber PL (2017) The EEG microstate topography is predominantly determined by intracortical sources in the alpha band. Neuroimage 162:353–361. https://doi.org/10.1016/j.neuroimage.2017.08.058
Khanna A, Pascual-Leone A, Michel CM, Farzan F (2015) Microstates in resting-state EEG: current status and future directions. Neurosci Biobehav Rev 49:105–113. https://doi.org/10.1016/j.neubiorev.2014.12.010
Pyrzowski J, Sieminski M, Sarnowska A, Jedrzejczak J, Nyka WM (2015) Interval analysis of interictal EEG: pathology of the alpha rhythm in focal epilepsy. Sci Rep 5:16230. https://doi.org/10.1038/srep16230
van Buren JM (1958) Some autonomic concomitants of ICTAL automatism: a study of temporal lobe attacks. Brain 81(4):505–528. https://doi.org/10.1093/brain/81.4.505
Simon RP, Aminoff MJ, Benowitz NL (1984) Changes in plasma catecholamines after tonic–clonic seizures. Neurology 34(2):255–257. https://doi.org/10.1212/wnl.34.2.255
Meierkord H, Shorvon S, Lightman SL (1994) Plasma concentrations of prolactin, noradrenaline, vasopressin and oxytocin during and after a prolonged epileptic seizure. Acta Neurol Scand 90(2):73–77
Lesser RP (1996) Psychogenic seizures. Neurology 46(6):1499–1507. https://doi.org/10.1212/wnl.46.6.1499
Krumholz A (1999) Nonepileptic seizures: diagnosis and management. Neurology 53(5 Suppl 2):S76–83
Bowman ES, Markand ON (1996) Psychodynamics and psychiatric diagnoses of pseudoseizure subjects. Am J Psychiatry 153(1):57–63. https://doi.org/10.1176/ajp.153.1.57
Benbadis SR (2010) Psychogenic nonepileptic "seizures" or "attacks"? It's not just semantics: attacks. Neurology 75(1):84–86. https://doi.org/10.1212/WNL.0b013e3181e6216f
Bruni A, Martino I, Borzi G, Gambardella A, De Fazio P, Labate A (2017) The mystery of unexplained traumatic sudden falls. A clinical case that adds a new feasible cause. Neurol Sci 38(6):1115–1117. https://doi.org/10.1007/s10072-017-843-7
Cerasa A, Fasano A, Morgante F, Koch G, Quattrone A (2014) Maladaptive plasticity in levodopa-induced dyskinesias and tardive dyskinesias: old and new insights on the effects of dopamine receptor pharmacology. Front Neurol 5:49. https://doi.org/10.3389/fneur.2014.00049
McCrory P, Meeuwisse W, Dvorak J, Aubry M, Bailes J, Broglio S, Cantu RC, Cassidy D, Echemendia RJ, Castellani RJ, Davis GA, Ellenbogen R, Emery C, Engebretsen L, Feddermann-Demont N, Giza CC, Guskiewicz KM, Herring S, Iverson GL, Johnston KM, Kissick J, Kutcher J, Leddy JJ, Maddocks D, Makdissi M, Manley GT, McCrea M, Meehan WP, Nagahiro S, Patricios J, Putukian M, Schneider KJ, Sills A, Tator CH, Turner M, Vos PE (2017) Consensus statement on concussion in sport—the 5%3csup%3eth%3c/sup%3e international conference on concussion in sport held in Berlin, October 2016. Br J Sports Med 51(11):838. https://doi.org/10.1136/bjsports-2017-097699
Mayer AR, Quinn DK, Master CL (2017) The spectrum of mild traumatic brain injury. Neurology 89(6):623. https://doi.org/10.1212/WNL.0000000000004214
Sharp DJ, Jenkins PO (2015) Concussion is confusing us all. Prac Neurol 15(3):172. https://doi.org/10.1136/practneurol-2015-001087
Feddermann-Demont N, Echemendia RJ, Schneider KJ, Solomon GS, Hayden KA, Turner M, Dvořák J, Straumann D, Tarnutzer AA (2017) What domains of clinical function should be assessed after sport-related concussion? A systematic review. Br J Sports Med 51(11):903. https://doi.org/10.1136/bjsports-2016-097403
Al Sayegh A, Sandford D, Carson AJ (2010) Psychological approaches to treatment of postconcussion syndrome: a systematic review. J Neurol Neurosurg Psychiatry 81(10):1128–1134. https://doi.org/10.1136/jnnp.2008.170092
Silverberg ND, Hallam BJ, Rose A, Underwood H, Whitfield K, Thornton AE, Whittal ML (2013) Cognitive-behavioral prevention of postconcussion syndrome in at-risk patients: a pilot randomized controlled trial. J Head Trauma Rehabil 28(4):313–322. https://doi.org/10.1097/HTR.0b013e3182915cb5
Caplain S, Blancho S, Marque S, Montreuil M, Aghakhani N (2017) Early detection of poor outcome after mild traumatic brain injury: predictive factors using a multidimensional approach a pilot study. Front Neurol 8:666. https://doi.org/10.3389/fneur.2017.00666
Sakai K, Yamada K (2019) Machine learning studies on major brain diseases: 5-year trends of 2014–2018. Jpn J Radiol 37(1):34–72. https://doi.org/10.1007/s11604-018-0794-4
Minaee S, Wang Y, Choromanska A, Chung S, Wang X, Fieremans E, Flanagan S, Rath J, Lui YW (2018) A deep unsupervised learning approach Toward MTBI identification using diffusion MRI. Conf Proc IEEE Eng Med Biol Soc 2018:1267–1270. https://doi.org/10.1109/embc.2018.8512556
Nielson JL, Cooper SR, Yue JK, Sorani MD, Inoue T, Yuh EL, Mukherjee P, Petrossian TC, Paquette J, Lum PY, Carlsson GE, Vassar MJ, Lingsma HF, Gordon WA, Valadka AB, Okonkwo DO, Manley GT, Ferguson AR (2017) Uncovering precision phenotype-biomarker associations in traumatic brain injury using topological data analysis. PLoS ONE 12(3):e0169490. https://doi.org/10.1371/journal.pone.0169490
Vakorin VA, Doesburg SM, da Costa L, Jetly R, Pang EW, Taylor MJ (2016) Detecting mild traumatic brain injury using resting state magnetoencephalographic connectivity. PLoS Comput Biol 12(12):e1004914. https://doi.org/10.1371/journal.pcbi.1004914
Zhao X, Rangaprakash D, Yuan B, Denney TS Jr., Katz JS, Dretsch MN, Deshpande G (2018) Investigating the correspondence of clinical diagnostic grouping with underlying neurobiological and phenotypic clusters using unsupervised machine learning. Front Appl Math Stat. https://doi.org/10.3389/fams.2018.00025
Juengst SB, Switzer G, Oh BM, Arenth PM, Wagner AK (2017) Conceptual model and cluster analysis of behavioral symptoms in two cohorts of adults with traumatic brain injuries. J Clin Exp Neuropsychol 39(6):513–524. https://doi.org/10.1080/13803395.2016.1240758
Si B, Dumkrieger G, Wu T, Zafonte R, Valadka AB, Okonkwo DO, Manley GT, Wang L, Dodick DW, Schwedt TJ, Li J (2018) Sub-classifying patients with mild traumatic brain injury: a clustering approach based on baseline clinical characteristics and 90-day and 180-day outcomes. PLoS ONE 13(7):e0198741. https://doi.org/10.1371/journal.pone.0198741
Landry AP, Ting WKC, Zador Z, Sadeghian A, Cusimano MD (2018) Using artificial neural networks to identify patients with concussion and postconcussion syndrome based on antisaccades. J Neurosurg. https://doi.org/10.3171/2018.6.Jns18607
Peacock WF, Van Meter TE, Mirshahi N, Ferber K, Gerwien R, Rao V, Sair HI, Diaz-Arrastia R, Korley FK (2017) Derivation of a three biomarker panel to improve diagnosis in patients with mild traumatic brain injury. Front Neurol 8:641. https://doi.og/10.3389/fneur.2017.00641
Zhou G, Brodsky JR (2015) Objective vestibular testing of children with dizziness and balance complaints following sports-related concussions. Otolaryngol Head Neck Surg 152(6):1133–1139. https://doi.org/10.1177/0194599815576720
Corwin DJ, Wiebe DJ, Zonfrillo MR, Grady MF, Robinson RL, Goodman AM, Master CL (2015) Vestibular deficits following youth concussion. J Pediatr 166(5):1221–1225. https://doi.org/10.1016/j.jpeds.2015.01.039
Kelly KM, Kiderman A, Akhavan S, Quigley MR, Snell ED, Happ E, Synowiec AS, Miller ER, Bauer MA, Oakes LP, Eydelman Y, Gallagher CW, Dinehart T, Schroeder JH, Ashmore RC (2019) Oculomotor, vestibular, and reaction time effects of sports-related concussion: video-oculography in assessing sports-related concussion. J Head Trauma Rehabil 34(3):176–188. https://doi.org/10.1097/htr.0000000000000437
Kontos AP, Deitrick JM, Collins MW, Mucha A (2017) Review of vestibular and oculomotor screening and concussion rehabilitation. J Athl Train 52(3):256–261. https://doi.org/10.4085/1062-6050-51.11.05
Worts PR, Schatz P, Burkhart SO (2018) Test performance and test-retest reliability of the vestibular/ocular motor screening and king-devick test in adolescent athletes during a competitive sport season. Am J Sports Med 46(8):2004–2010. https://doi.org/10.1177/0363546518768750
Craton N, Ali H, Lenoski S (2017) COACH CV: the seven clinical phenotypes of concussion. Brain Sci 7(9):119
Onyike CU, Diehl-Schmid J (2013) The epidemiology of frontotemporal dementia. Int Rev Psychiatry 25(2):130–137. https://doi.org/10.3109/09540261.2013.776523
Shinagawa S, Catindig JA, Block NR, Miller BL, Rankin KP (2016) When a little knowledge can be dangerous: false-positive diagnosis of behavioral variant frontotemporal dementia among community clinicians. Dement Geriatr Cogn Disord 41(1–2):99–108. https://doi.org/10.1159/000438454
Landqvist Waldö M, Gustafson L, Passant U, Englund E (2015) Psychotic symptoms in frontotemporal dementia: a diagnostic dilemma? Int Psychogeriatr 27(4):531–539. https://doi.org/10.1017/S1041610214002580
Newman EJ, Breen K, Patterson J, Hadley DM, Grosset KA, Grosset DG (2009) Accuracy of Parkinson's disease diagnosis in 610 general practice patients in the West of Scotland. Mov Disord 24(16):2379–2385. https://doi.org/10.1002/mds.22829
Silva de Lima AL, Hahn T, Evers LJW, de Vries NM, Cohen E, Afek M, Bataille L, Daeschler M, Claes K, Boroojerdi B, Terricabras D, Little MA, Baldus H, Bloem BR, Faber MJ (2017) Feasibility of large-scale deployment of multiple wearable sensors in Parkinson's disease. PLoS ONE 12(12):e0189161. https://doi.org/10.1371/journal.pone.0189161
Feigin VL, Abajobir AA, Abate KH, Abd-Allah F, Abdulle AM, Abera SF, Abyu GY, Ahmed MB, Aichour AN, Aichour I, Aichour MTE, Akinyemi RO, Alabed S, Al-Raddadi R, Alvis-Guzman N, Amare AT, Ansari H, Anwari P, Ärnlöv J, Asayesh H, Asgedom SW, Atey TM, Avila-Burgos L, Frinel E, Avokpaho GA, Azarpazhooh MR, Barac A, Barboza M, Barker-Collo SL, Bärnighausen T, Bedi N, Beghi E, Bennett DA, Bensenor IM, Berhane A, Betsu BD, Bhaumik S, Birlik SM, Biryukov S, Boneya DJ, Bulto LNB, Carabin H, Casey D, Castañeda-Orjuela CA, Catalá-López F, Chen H, Chitheer AA, Chowdhury R, Christensen H, Dandona L, Dandona R, de Veber GA, Dharmaratne SD, Do HP, Dokova K, Dorsey ER, Ellenbogen RG, Eskandarieh S, Farvid MS, Fereshtehnejad S-M, Fischer F, Foreman KJ, Geleijnse JM, Gillum RF, Giussani G, Goldberg EM, Gona PN, Goulart AC, Gugnani HC, Gupta R, Hachinski V, Gupta R, Hamadeh RR, Hambisa M, Hankey GJ, Hareri HA, Havmoeller R, Hay SI, Heydarpour P, Hotez PJ, Jakovljevic MB, Javanbakht M, Jeemon P, Jonas JB, Kalkonde Y, Kandel A, Karch A, Kasaeian A, Kastor A, Keiyoro PN, Khader YS, Khalil IA, Khan EA, Khang Y-H, Tawfih A, Khoja A, Khubchandani J, Kulkarni C, Kim D, Kim YJ, Kivimaki M, Kokubo Y, Kosen S, Kravchenko M, Krishnamurthi RV, Defo BK, Kumar GA, Kumar R, Kyu HH, Larsson A, Lavados PM, Li Y, Liang X, Liben ML, Lo WD, Logroscino G, Lotufo PA, Loy CT, Mackay MT, El Razek HMA, El Razek MMA, Majeed A, Malekzadeh R, Manhertz T, Mantovani LG, Massano J, Mazidi M, McAlinden C, Mehata S, Mehndiratta MM, Memish ZA, Mendoza W, Mengistie MA, Mensah GA, Meretoja A, Mezgebe HB, Miller TR, Mishra SR, Ibrahim NM, Mohammadi A, Mohammed KE, Mohammed S, Mokdad AH, Moradi-Lakeh M, Velasquez IM, Musa KI, Naghavi M, Ngunjiri JW, Nguyen CT, Nguyen G, Le Nguyen Q, Nguyen TH, Nichols E, Ningrum DNA, Nong VM, Norrving B, Noubiap JJN, Ogbo FA, Owolabi MO, Pandian JD, Parmar PG, Pereira DM, Petzold M, Phillips MR, Piradov MA, Poulton RG, Pourmalek F, Qorbani M, Rafay A, Rahman M, Rahman MH, Rai RK, Rajsic S, Ranta A, Rawaf S, Renzaho AMN, Rezai MS, Roth GA, Roshandel G, Rubagotti E, Sachdev P, Safiri S, Sahathevan R, Sahraian MA, Samy AM, Santalucia P, Santos IS, Sartorius B, Satpathy M, Sawhney M, Saylan MI, Sepanlou SG, Shaikh MA, Shakir R, Shamsizadeh M, Sheth KN, Shigematsu M, Shoman H, Silva DAS, Smith M, Sobngwi E, Sposato LA, Stanaway JD, Stein DJ, Steiner TJ, Stovner LJ, Abdulkader RS, Ei Szoeke C, Tabarés-Seisdedos R, Tanne D, Theadom AM, Thrift AG, Tirschwell DL, Topor-Madry R, Tran BX, Truelsen T, Tuem KB, Ukwaja KN, Uthman OA, Varakin YY, Vasankari T, Venketasubramanian N, Vlassov VV, Wadilo F, Wakayo T, Wallin MT, Weiderpass E, Westerman R, Wijeratne T, Wiysonge CS, Woldu MA, Wolfe CDA, Xavier D, Xu G, Yano Y, Yimam HH, Yonemoto N, Yu C, Zaidi Z, El Sayed Zaki M, Zunt JR, Murray CJL, Vos T (2017) Global, regional, and national burden of neurological disorders during 1990–2015: a systematic analysis for the Global Burden of Disease Study 2015. The Lancet Neurology 16(11):877–897. https://doi.org/10.1016/S1474-4422(17)30299-5
Seeley WW (2009) Frontotemporal dementia neuroimaging: a guide for clinicians. Front Neurol Neurosci 24:160–167. https://doi.org/10.1159/000197895
Jain S, Lo SE, Louis ED (2006) Common misdiagnosis of a common neurological disorder: how are we misdiagnosing essential tremor? JAMA Neurol 63(8):1100–1104. https://doi.org/10.1001/archneur.63.8.1100
Kikuchi M, Koenig T, Munesue T, Hanaoka A, Strik W, Dierks T, Koshino Y, Minabe Y (2011) EEG microstate analysis in drug-naive patients with panic disorder. PLoS ONE 6(7):e22912. https://doi.org/10.1371/journal.pone.0022912
Nishida K, Morishima Y, Yoshimura M, Isotani T, Irisawa S, Jann K, Dierks T, Strik W, Kinoshita T, Koenig T (2013) EEG microstates associated with salience and frontoparietal networks in frontotemporal dementia, schizophrenia and Alzheimer's disease. Clin Neurophysiol 124(6):1106–1114. https://doi.org/10.1016/j.clinph.2013.01.005
Arani LA, Hosseini A, Asadi F, Masoud SA, Nazemi E (2018) Intelligent computer systems for multiple sclerosis diagnosis: a systematic review of reasoning techniques and methods. Acta Inf Med 26(4):258–264. https://doi.org/10.5455/aim.2018.26.258-264
Amodei D, Olah C, Steinhardt J, Christiano P, Schulman J, Mané D (2016) Concrete Problems in AI Safety (arXiv e-prints)
Ozcan EE, Gorenek B (2018) Lessons from the current European Heart Rhythm Association consensus document on screening for atrial fibrillation. Anatol J Cardiol 19(3):222–224. https://doi.org/10.14744/AnatolJCardiol.2018.37043
Ho CWL, Soon D, Caals K, Kapur J (2019) Governance of automated image analysis and artificial intelligence analytics in healthcare. Clin Radiol 74(5):329–337. https://doi.org/10.1016/j.crad.2019.02.005
Giger ML (2018) Machine learning in medical imaging. J Am Coll Radiol 15(3 Pt B):512–520. https://doi.org/10.1016/j.jacr.2017.12.028
Lee JG, Jun S, Cho YW, Lee H, Kim GB, Seo JB, Kim N (2017) Deep learning in medical imaging: general overview. Korean J Radiol 18(4):570–584. https://doi.org/10.3348/kjr.2017.18.4.570
Pinto A, Brunese L, Pinto F, Reali R, Daniele S, Romano L (2012) The concept of error and malpractice in radiology. Semin Ultrasound CT MR 33(4):275–279. https://doi.org/10.1053/j.sult.2012.01.009
Tang A, Tam R, Cadrin-Chenevert A, Guest W, Chong J, Barfett J, Chepelev L, Cairns R, Mitchell JR, Cicero MD, Poudrette MG, Jaremko JL, Reinhold C, Gallix B, Gray B, Geis R (2018) Canadian association of radiologists white paper on artificial intelligence in radiology. Can Assoc Radiol J 69(2):120–135. https://doi.org/10.1016/j.carj.2018.02.002
Paschen S, Deuschl G (2018) Patient evaluation and selection for movement disorders surgery: the changing spectrum of indications. Progr Neurol Surg 33:80–93. https://doi.org/10.1159/000480910
Deuschl G, Paschen S, Witt K (2013) Clinical outcome of deep brain stimulation for Parkinson's disease. Handb Clin Neurol 116:107–128. https://doi.org/10.1016/b978-0-444-53497-2.00010-3
Fasano A, Romito LM, Daniele A, Piano C, Zinno M, Bentivoglio AR, Albanese A (2010) Motor and cognitive outcome in patients with Parkinson's disease 8 years after subthalamic implants. Brain 133(9):2664–2676. https://doi.org/10.1093/brain/awq221
Deuschl G, Raethjen J, Hellriegel H, Elble R (2011) Treatment of patients with essential tremor. Lancet Neurol 10(2):148–161. https://doi.org/10.1016/s1474-4422(10)70322-7
AliveCor (2019) FDA clears first medical device accessory for Apple Watch®. AliveCor, Inc. https://www.alivecor.com/press/press_release/fda-clears-first-medical-device-for-apple-watch/. Accessed 10 Jul 2019
Funding
The study had no internal or external funding source.
Author information
Authors and Affiliations
Contributions
Conceptualization, UP; methodology: none; formal analysis and investigation, UP, AA, SS; writing—original draft preparation, KA, AA, SS, UP; writing—review and editing, PM, KP, RY, AS, MY, BR; supervision, KA; project administration, UP; resources, UP; funding acquisition, none.
Corresponding author
Ethics declarations
Conflicts of interest
The authors report no disclosures relevant to the manuscript. The authors declare that there is no conflict of interest. Robert Yao is the founder and CEO of EpiFinder, Inc.
Informed consent
This review article does not have direct or indirect involvement of humans or animals, so permission from IRB or ethics committee was not applicable or required.
Rights and permissions
About this article
Cite this article
Patel, U.K., Anwar, A., Saleem, S. et al. Artificial intelligence as an emerging technology in the current care of neurological disorders. J Neurol 268, 1623–1642 (2021). https://doi.org/10.1007/s00415-019-09518-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-019-09518-3