Abstract
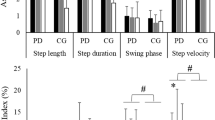
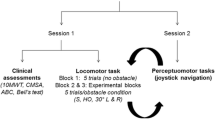
Patients with Parkinson’s disease (PD) have difficulties in performing complex bimanual movements. Here we have examined acquisition and performance of a bilateral obstacle stepping task to see whether these difficulties are also present during bipedal movements. Subjects had to minimize foot clearance when repeatedly stepping on a treadmill over randomly approaching obstacles on either side. The subjects had full vision and received acoustic feedback information about task performance. Foot clearance improved in healthy and PD subjects during the acquisition of the task. However, PD subjects showed a slower improvement and achieved a poorer performance level. Thus, in contrast to unilateral obstacle stepping, where no deficits in performance after task repetition were found in PD subjects, bilateral obstacle stepping was poorer in these subjects compared to healthy subjects. The present results extend findings from upper to lower limb movements, namely that PD subjects have difficulties in the performance of bilateral motor tasks.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Almeida QJ, Wishart LR, Lee TD (2002) Bimanual coordination deficits with Parkinson’s disease: the influence of movement speed and external cueing. Mov Disord 17:30–37
Bloem BR, van Vugt JP, Beckley DJ (2001) Postural instability and falls in Parkinson’s disease. Adv Neurol 87:209–223
Burleigh-Jacobs A, Horak FB, Nutt JG, Obeso JA (1997) Step initiation in Parkinson’s disease: influence of levodopa and external sensory triggers. Mov Disord 12:206–215
Demirci M, Grill S, McShane L, Hallett M (1997) A mismatch between kinesthetic and visual perception in Parkinson’s disease. Ann Neurol 41:781–788
Erni T, Dietz V (2001) Obstacle avoidance during human walking: learning rate and cross-modal transfer. J Physiol 534:303–312
Flament D, Vaillancourt DE, Kempf T, Shannon K, Corcos DM (2003) EMG remains fractionated in Parkinson’s disease, despite practice-related improvements in performance. Clin Neurophysiol 114:2385–2396
Georgiou N, Bradshaw JL, Iansek R, Phillips JG, Mattingley JB, Bradshaw JA (1994) Reduction in external cues and movement sequencing in Parkinson’s disease. J Neurol Neurosurg Psychiatry 57:368–370
Georgiou N, Iansek R, Bradshaw JL, Phillips JG, Mattingley JB, Bradshaw JA (1993) An evaluation of the role of internal cues in the pathogenesis of parkinsonian hypokinesia. Brain 116(Pt 6):1575–1587
Horstink MW, Berger HJ, van Spaendonck KP, van den Bercken JH, Cools AR (1990) Bimanual simultaneous motor performance and impaired ability to shift attention in Parkinson’s disease. J Neurol Neurosurg Psychiatry 53:685–690
Jackson GM, Jackson SR, Hindle JV (2000) The control of bimanual reachto- grasp movements in hemiparkinsonian patients. Exp Brain Res (Experimentelle Hirnforschung) 132:390–398
Krebs HI, Hogan N, Hening W, Adamovich SV, Poizner H (2001) Procedural motor learning in Parkinson’s disease. Exp Brain Res (Experimentelle Hirnforschung) 141:425–437
Krystkowiak P, Delval A, Dujardin K, Bleuse S, Blatt JL, Bourriez JL, Derambure P, Destee A, Defebvre L (2006) Gait abnormalities induced by acquired bilateral pallidal lesions: a motion analysis study. J Neurol 253:594–600
Lazarus A, Stelmach GE (1992) Interlimb coordination in Parkinson’s disease. Mov Disord 7:159–170
Longstaff MG, Mahant PR, Stacy MA, Van Gemmert AW, Leis BC, Stelmach GE (2003) Discrete and dynamic scaling of the size of continuous graphic movements of parkinsonian patients and elderly controls. J Neurol Neurosurg Psychiatry 74:299–304
Majsak MJ, Kaminski T, Gentile AM, Flanagan JR (1998) The reaching movements of patients with Parkinson’s disease under self-determined maximal speed and visually cued conditions. Brain 121(Pt 4):755–766
Marchese R, Bove M, Abbruzzese G (2003) Effect of cognitive and motor tasks on postural stability in Parkinson’s disease: a posturographic study. Mov Disord 18:652–658
Miyai I, Fujimoto Y, Ueda Y, Yamamoto H, Nozaki S, Saito T, Kang J (2000) Treadmill training with body weight support: its effect on Parkinson’s disease. Arch Phys Med Rehabil 81:849–852
Miyai I, Fujimoto Y, Yamamoto H, Ueda Y, Saito T, Nozaki S, Kang J (2002) Long-term effect of body weightsupported treadmill training in Parkinson’s disease: a randomized controlled trial. Arch Phys Med Rehabil 83:1370–1373
Morris M, Iansek R, Smithson F, Huxham F (2000) Postural instability in Parkinson’s disease: a comparison with and without a concurrent task. Gait Posture 12:205–216
Morris ME, Iansek R, Matyas TA, Summers JJ (1994) The pathogenesis of gait hypokinesia in Parkinson’s disease. Brain 117(Pt 5):1169–1181
Pfann KD, Buchman AS, Comella CL, Corcos DM (2001) Control of movement distance in Parkinson’s disease. Mov Disord 16:1048–1065
Rocchi L, Chiari L, Mancini M, Carlson- Kuhta P, Gross A, Horak FB (2006) Step initiation in Parkinson’s disease: influence of initial stance conditions. Neurosci Lett 406:128–132
Rogers MW (1996) Disorders of posture, balance, and gait in Parkinson’s disease. Clin Geriatr Med 12:825–845
Rogers MW, Kukulka CG, Soderberg GL (1987) Postural adjustments preceding rapid arm movements in parkinsonian subjects. Neurosci Lett 75:246–251
Shimizu N, Yoshida M, Nagatsuka Y (1987) Disturbance of two simultaneous motor acts in patients with parkinsonism and cerebellar ataxia. Adv Neurol 45:367–370
Smiley-Oyen AL, Worringham CJ, Cross CL (2003) Motor learning processes in a movement-scaling task in olivopontocerebellar atrophy and Parkinson’s disease. Exp Brain Res (Experimentelle Hirnforschung) 152:453–465
Swinnen SP, Van Langendonk L, Verschueren S, Peeters G, Dom R, De Weerdt W (1997) Interlimb coordination deficits in patients with Parkinson’s disease during the production of two-joint oscillations in the sagittal plane. Mov Disord 12:958–968
Thaut MH, McIntosh GC, Rice RR, Miller RA, Rathbun J, Brault JM (1996) Rhythmic auditory stimulation in gait training for Parkinson’s disease patients. Mov Disord 11:193–200
van Hedel HJ, Biedermann M, Erni T, Dietz V (2002) Obstacle avoidance during human walking: transfer of motor skill from one leg to the other. J Physiol 543:709–717
van Hedel HJ, Dietz V (2004) The influence of age on learning a locomotor task. Clin Neurophysiol 115:2134–2143
van Hedel HJ, Dietz V (2004) Obstacle avoidance during human walking: effects of biomechanical constraints on performance. Arch Phys Med Rehabil 85:972–979
van Hedel HJ, Waldvogel D, Dietz V (2006) Learning a high-precision locomotor task in patients with Parkinson’s disease. Mov Disord 21:406–411
Verschueren SM, Swinnen SP, Dom R, De Weerdt W (1997) Interlimb coordination in patients with Parkinson’s disease: motor learning deficits and the importance of augmented information feedback. Exp Brain Res (Experimentelle Hirnforschung) 113:497–508
Winogrodzka A, Wagenaar RC, Booij J, Wolters EC (2005) Rigidity and bradykinesia reduce interlimb coordination in Parkinsonian gait. Arch Phys Med Rehabil 86:183–189
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Michel, J., Benninger, D., Dietz, V. et al. Obstacle stepping in patients with Parkinson’s disease. J Neurol 256, 457–463 (2009). https://doi.org/10.1007/s00415-009-0114-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-009-0114-0