Abstract
Background
Status epilepticus (SE) treatment ranges from small benzodiazepine doses to coma induction. For some SE subgroups, it is unclear how the risk of an aggressive therapeutic approach balances with outcome improvement. We recently developed a prognostic score (Status Epilepticus Severity Score, STESS), relying on four outcome predictors (age, history of seizures, seizure type and extent of consciousness impairment), determined before treatment institution. Our aim was to assess whether the score might have a role in the treatment strategy choice.
Methods
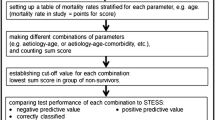
This cohort study involved adult patients in three centers. For each patient, the STESS was calculated before primary outcome assessment: survival vs. death at discharge. Its ability to predict survival was estimated through the negative predictive value for mortality (NPV). Stratified odds ratios (OR) for mortality were calculated considering coma induction as exposure; strata were defined by the STESS level.
Results
In the observed 154 patients, the STESS had an excellent negative predictive value (0.97). A favorable STESS was highly related to survival (P < 0.001), and to return to baseline clinical condition in survivors (P < 0.001). The combined Mantel-Haenszel OR for mortality in patients stratified after coma induction and their STESS was 1.5 (95 % CI: 0.59–3.83).
Conclusion
The STESS reliably identifies SE patients who will survive. Early aggressive treatment could not be routinely warranted in patients with a favorable STESS, who will almost certainly survive their SE episode. A randomized trial using this score would be needed to confirm this hypothesis.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
(1993) Guidelines for epidemiologic studies on epilepsy. Commission on Epidemiology and Prognosis, International League Against Epilepsy. Epilepsia 34:592–596
Aminoff MJ (1998) Do nonconvulsive seizures damage the brain? – No. Arch Neurol 55:119–120
Cavaliere R, Farace E, Schiff D (2006) Clinical implications of status epilepticus in patients with neoplasms. Arch Neurol 63:1746–1749
Claassen J, Hirsch LJ, Emerson RG, Mayer SA (2002) Treatment of refractory status epilepticus with pentobarbital, propofol, or midazolam: a systematic review. Epilepsia 43:146–153
Claassen J, Lokin JK, Fitzsimmons BF, Mendelsohn FA, Mayer SA (2002) Predictors of functional disability and mortality after status epilepticus. Neurology 58:139–142
Coeytaux A, Jallon P, Galobardes B, Morabia A (2000) Incidence of status epilepticus in French-speaking Switzerland: (EPISTAR). Neurology 55:693–697
Corsellis JA, Bruton CJ (1983) Neuropathology of status epilepticus in humans. Adv Neurol 34:129–139
DeGiorgio CM, Tomiyasu U, Gott PS, Treiman DM (1992) Hippocampal pyramidal cell loss in human status epilepticus. Epilepsia 33:23–27
DeLorenzo RJ, Hauser WA, Towne AR, Boggs JG, Pellock JM, Penberthy L, Garnett L, Fortner CA, Ko D (1996) A prospective, population-based epidemiologic study of status epilepticus in Richmond, Virginia. Neurology 46:1029–1035
Drislane FW (1999) Evidence against permanent neurologic damage from nonconvulsive status epilepticus. J Clin Neurophysiol 16:323–331; discussion 353
Hesdorffer DC, Logroscino G, Cascino G, Annegers JF, Hauser WA (1998) Incidence of status epilepticus in Rochester, Minnesota, 1965–1984. Neurology 50:735–741
Holtkamp M (2007) The anaesthetic and intensive care of status epilepticus. Curr Opin Neurol 20:188–193
Jordan KG, Hirsch LJ (2006) In nonconvulsive status epilepticus (NCSE), treat to burst-suppression: pro and con. Epilepsia 47(Suppl 1):41–45
Kaplan PW (2000) No, some types of nonconvulsive status epilepticus cause little permanent neurologic sequelae (or: “the cure may be worse than the disease”). Neurophysiol Clin 30:377–382
Knake S, Rosenow F, Vescovi M, Oertel WH, Mueller HH, Wirbatz A, Katsarou N, Hamer HM (2001) Incidence of status epilepticus in adults in Germany: a prospective, population-based study. Epilepsia 42:714–718
Logroscino G, Hesdorffer DC, Cascino G, Annegers JF, Hauser WA (1997) Short-term mortality after a first episode of status epilepticus. Epilepsia 38:1344–1349
Lowenstein DH, Alldredge BK (1998) Status epilepticus. N Engl J Med 338:970–976
Nohria V, Lee N, Tien RD, Heinz ER, Smith JS, DeLong GR, Skeen MB, Resnick TJ, Crain B, Lewis DV (1994) Magnetic resonance imaging evidence of hippocampal sclerosis in progression: a case report. Epilepsia 35:1332–1336
Rossetti AO, Hurwitz S, Logroscino G, Bromfield EB (2006) Prognosis of status epilepticus: role of aetiology, age, and consciousness impairment at presentation. J Neurol Neurosurg Psychiatry 77:611–615
Rossetti AO, Logroscino G, Bromfield EB (2006) A clinical score for prognosis of status epilepticus in adults. Neurology 66:1736–1738
Shneker BF, Fountain NB (2003) Assessment of acute morbidity and mortality in nonconvulsive status epilepticus. Neurology 61:1066–1073
Shorvon S (2001) The management of status epilepticus. J Neurol Neurosurg Psychiatry 70(Suppl 2):II22–27
Tien RD, Felsberg GJ (1995) The hippocampus in status epilepticus: demonstration of signal intensity and morphologic changes with sequential fast spin-echo MR imaging. Radiology 194:249–256
Towne AR, Pellock JM, Ko D, DeLorenzo RJ (1994) Determinants of mortality in status epilepticus. Epilepsia 35:27–34
Treiman DM (1995) Electroclinical features of status epilepticus. J Clin Neurophysiol 12:343–362
Treiman DM WN, Collins JF (1999) Treatment of status epilepticus if first drug fails. Epilepsia 40:243
Vignatelli L, Rinaldi R, Galeotti M, de Carolis P, D’Alessandro R (2005) Epidemiology of status epilepticus in a rural area of northern Italy: a 2-year population-based study. Eur J Neurol 12:897–902
Vignatelli L, Tonon C, D’Alessandro R (2003) Incidence and short-term prognosis of status epilepticus in adults in Bologna, Italy. Epilepsia 44:964–968
Young GB, Jordan KG (1998) Do nonconvulsive seizures damage the brain? – Yes. Arch Neurol 55:117–119
Zarovnaya EL, Jobst BC, Harris BT (2007) Propofol-associated fatal myocardial failure and rhabdomyolysis in an adult with status epilepticus. Epilepsia 48:1002–1006
Author information
Authors and Affiliations
Corresponding author
Additional information
This paper was presented in part at the 61st Annual Meeting of the American Epilepsy Society, Nov. 30–Dec. 4, 2007, in Philadelphia, PA, USA.
Rights and permissions
About this article
Cite this article
Rossetti, A.O., Logroscino, G., Milligan, T.A. et al. Status Epilepticus Severity Score (STESS). J Neurol 255, 1561–1566 (2008). https://doi.org/10.1007/s00415-008-0989-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-008-0989-1