Abstract
In bacterial empyema the pleural mesothelium is constantly exposed to microorganisms. Staphylococcus aureus (S. aureus) is one of the most frequent pathogens associated with empyema. In an earlier study we demonstrated that S. aureus induced barrier dysfunction in pleural mesothelial cell monolayers. In the present study we report that S. aureus activates the early response genes c-fos and c-jun and activator protein-1 (AP-1), and induces proapoptosis genes Bad and Bak in primary mouse pleural mesothelial cells (PMCs). Our data indicate that in PMCs S. aureus induces apoptosis in a time- and multiplicity of infection (MOI)-dependent manner. Staphylococcus aureus induced Bcl 2, Bcl-X L, c-fos, c-jun, and AP-1 expression in PMCs during the initial phase of infection. In S. aureus-infected PMCs, Bad and Bak gene expression was increased and correlated with DNA fragmentation and cytochrome-c release. Bcl 2 and Bcl-X L gene expression was significantly lower in S. aureus-infected PMCs than in uninfected PMCs 12 h postinfection. We conclude that at the initial stage of infection S. aureus modulates expression of early response genes c-fos and c-jun, and in the late phase of infection S. aureus induces expression of proapoptotic genes Bak and Bad in PMCs. Silencing AP-1 significantly inhibited S. aureus-induced Bak and Bad expression in PMCs. The upregulation of early response genes during the early phase of infection may contribute to the activation of proapoptotic genes Bak and Bad and release of cytochrome-c, caspase-3 thereby resulting in apoptosis in PMCs.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Staphylococcus aureus is a leading cause of the development of parapneumonic effusions in pleural space [1]. Empyema is a serious complication of pulmonary parenchymal infection associated with the presence of bacteria in the pleural space and rarely resolves without appropriate medical therapy. Staphylococcusaureus accounts for a large number of cases of pediatric empyema [2]and is a significant cause (19.7%) of bacterial pneumonia in patients with acquired immunodeficiency syndrome [3]. It is estimated that 0.8% of childhood pneumonia progresses to empyema, affecting 3.3% per 100,000 children [4, 5]. Early diagnosis of infected pleural effusion and rapid drainage is necessary to reduce the morbidity and mortality in patients with empyema [6].
In empyema the pleura is exposed to invading pathogens. In earlier studies we demonstrated that S. aureus induces an acute inflammatory response in the pleural space [7] and compromises pleural mesothelial cell (PMC) barrier function [8]. Pleural mesothelial integrity is necessary for maintenance of barrier function [7]. It is unclear if S. aureus has any deleterious effect on PMCs. Interaction of S. aureus with host cells often results in the internalization of bacteria [9, 10], and intracellular S. aureus induces apoptosis in epithelial and endothelial cells [11–13]. However, the pathway through which S. aureus induces apoptosis is not clear.
Apoptosis is an active cellular process of gene-directed self-destruction [14]. The process of apoptosis is regulated mainly by two gene family members, namely, the Bcl 2-related genes and caspases. Caspases are a family of cysteine proteases that are activated during apoptosis [15]. The Bcl 2 family regulates apoptosis by controlling the activity of caspases via cytochrome-c from mitochondria [16]. The members of this family are separated functionally into two groups, apoptotic agonists (Bad, Bix, Bak) and apoptotic antagonists (Bcl 2, Bcl-X L, Bcl-w). Proapoptotic and antiapoptotic family members mediate their proapoptotic or antiapoptotic signals through their relative abundance. They dimerize through their Bcl 2 homology domains, neutralizing each other’s function [17]. Bad regulates the execution of apoptosis and Bak promotes cell death and counteracts the protection from apoptosis provided by Bcl 2 [18].
Recent studies revealed that cells undergoing apoptosis express the early response genes c-fos and c-jun, which code for transcriptional factors [19, 20]. The fos/jun early response genes encode proteins that are major components of the AP-1 transcription factor. These proteins are members of the bZIP family of transcription factors, capable of forming homo- and heterodimeric AP-1 complexes with each other as well as with other nuclear factors [21]. AP-1 is a key regulator of major biological processes, including cell proliferation, differentiation, and apoptosis [22]. Although S. aureus is known to induce apoptosis in a variety of cell types, the underlying mechanisms by which S. aureus induces apoptosis in PMCs have not been investigated. In the present study we evaluated the mechanisms of S. aureus-induced apoptosis in primary cultures of mice PMCs. Our data indicate that S. aureus induces the early response genes c-fos and c-jun; moreover, the expression of antiapoptotic genes Bcl 2 and Bcl-X L spiked at 12 h at the initial stage of infection. S. aureus induced the expression of proapoptotic genes Bak and Bad of the Bcl 2 family and cytochrome-c release in the later phase of infection.
Material and Methods
Reagents
Fetal bovine serum (FBS) was purchased from Atlanta Biologicals (Norcross, GA). F12K media, AP-1 stealth RNAi, and the primers for Bcl-X L, Bcl 2, Bak, and Bad were synthesized by Invitrogen (Carlsbad, CA). An in situ Apoptag labeling kit was obtained from Oncor (Gaithersburg, MD). Biodyne® nylon membranes were purchased from Pierce Biotechnology (Rockford, IL). c-fos- and c-jun-specific polyclonal antibodies were obtained from Oncogene (Boston, MA). The cytochrome-c-specific monoclonal antibody and caspase-3-specific cellular activity kits were from Calbiochem (SanDiego, CA) and the chemiluminescence ECL kit was from Amersham Pharmacia Biotech (Piscataway, NJ).
Isolation and Characterization of Primary Cultures of Mice PMCs
Female mice with C57BL/6 background (5–6 weeks of age) were obtained from The Jackson Laboratory (Bar Harbor, ME). PMCs from normal healthy (control) animals were obtained by collagenase digestion of visceral and parietal pleura as reported earlier [23]. Briefly, the pleural surfaces were exposed to collagenase (10 mg/ml) and PMCs were harvested, resuspended in F12K culture medium, and grown to confluence in tissue culture flasks. The PMCs were characterized by the presence of classic cobblestone morphology [24], the absence of factor VIII antigen, and the presence of cytokeratin [25].
Assessment of Viable Intracellular S. aureus
PMCs were grown to confluence in 24-well tissue culture plates. Staphylococcus aureus with various multiplicities of infection (MOI) (1:1, 1:10, and 1:100) was added to each well and incubated for 3–72 h. At the end of the incubation period, uningested bacteria were removed by washing three times with HBSS. The bacteria that were not ingested but attached to PMCs were removed by lysing with Lysostaphin (10 μg/ml for 20 min in HBSS). PMC culture was lysed by treating it with hypotonic buffer; the number of viable intracellular S. aureus (colony-forming units, CFU) was then estimated. The cell culture was vortex agitated briefly to disperse S. aureus clumps. Appropriate dilutions were performed on each sample, and duplicate aliquots of each dilution were plated on tryptic soy agar (TSA; Difco Labs, Detroit, MI) spread plates. Spread plates were incubated at 37°C for 24 h and the colonies were counted. Each experiment was performed three times in duplicates.
Preparation of S. aureus Culture and PMC Stimulation
A mouse virulent strain of S. aureus (ATCC) was cultured as reported earlier [8]. The bacteria were harvested by centrifugation, washed twice in phosphate-buffered saline (PBS), and resuspended in F12K serum-free media (SFM). PMCs (5 × 105/ml) were incubated in the presence of S. aureus with various MOI (1:1, 1:10, and 1:100, PMC : S. aureus) in SFM for 6, 12, 24, and 48 h at 37°C in 5% CO2. The induction of apoptosis was determined with all three MOI. Further experiments were performed using 1:10 MOI.
Quantitative Detection of Apoptosis by TUNEL Assay
Mice PMCs were cultured in chambered glass slides and were incubated with either SFM or S. aureus for a desired period of time. The PMC culture was fixed with 4% paraformaldehyde. PMC apoptosis was estimated by the TUNEL method (In situ Apoptag Labeling kit, Oncor, Gaithersburg, MD) as reported earlier [27]. The percentage of apoptotic cells (percent positively stained nuclei to total nuclei) was determined by counting a total of 100 cells per slide and at least three slides per group.
Determination of Apoptotic DNA (Ladder) by Electrophoresis
DNA extraction and electrophoresis were performed as described earlier [28]. In brief, 5 × 106 PMCs were incubated with either SFM or S. aureus (1:10 MOI, PMC : S. aureus) for 6, 12, 24, and 48 h. The isolated DNA was subjected to electrophoresis in 1.6% agarose gel at a concentration of 12 μg per lane and visualized after ethidium bromide staining.
Western Blot Analysis for Estimation of c-fos, c-jun, and Cytochrome-c
PMCs after activation with S. aureus were washed three times by centrifugation. The cell pellet was lysed and nuclear lysates were used to detect the expression of early response genes. Nuclear lysates (106cells/sample) were subjected to SDS-PAGE on gels containing 12% (wt/vol) acrylamide under reducing conditions. Separated proteins were transferred to Biodyne® nylon membranes (Pierce). c-fos and c-jun expression was detected by c-fos/c-jun-specific polyclonal antibodies obtained from Oncogene (Boston, MA). The cytochrome-c expression was detected by using a monoclonal antibody specific to cytochrome-c (Calbiochem, San Diego, CA). Specific protein detection was performed by chemiluminescence using an ECL kit (Amersham Pharmacia Biotech, Piscataway, NJ). The relative densities of c-fos, c-jun, and cytochrome-c were estimated using Quantity One software on GS-710 calibrated imaging densitometer (BioRad, Hercules, CA).
Estimation of AP-1 by Electrophoretic Mobility Shift Assay
Nuclear extracts were prepared as described previously [29]. LightShift (Chemiluminescent EMSA kit; Pierce, Rockford, IL) was used according to the manufacturer’s instructions. In brief, for each sample, 50 μM biotin-labeled (biotin 3′ end DNA labeling kit; Pierce) double-stranded oligonucleotide sequence for AP-1 (Promega, Madison, WI) was incubated with 6 μg of nuclear extract. To assess the binding specificity, an excess of unlabeled AP-1/DNA complexes was added to appropriate tubes at the start of the binding reaction. Protein-DNA complexes were quantified as above.
Stealth RNAi and Transfection of PMCs
Stealth RNAi targeting the transcription factor AP-1 sense GGUGUGGUGGAAGUGUACCGCGUAA, anti-sense UUACGCGGUACACUUCCACCACACC, and scrambled (control) RNAi were designed using Block-iT RNAi Designer (Invitrogen, Carlsbad, CA) and synthesized. PMCs were plated in a 60-mm culture dish and incubated at 37°C in 5% CO2 for 24 h. The transfection of PMCs with RNAi (100 nm) was performed using lipofectamine-2000 (Invitrogen). After 4 h of transfection the culture was incubated at 37°C in 5% CO2 in media containing 10% serum. Twenty-four hours after transfection the PMCs were infected with S. aureus but some cultures were left uninfected. The total RNA was extracted for quantitative PCR.
Total RNA Extraction and Quantitative Real-Time PCR Analysis
Total RNA from PMCs was isolated by using a highly pure RNA isolation kit (Roche Applied Science, Indianapolis, IN). RNA samples were diluted with RNase-free water to 100 ng/μl, and 10 μl of each sample with 1 μl of 3.5 μM anchored oligo(dT)23 (Sigma, St. Louis, MO) were denatured at 70°C for 10 min followed by 2 min of incubation on ice. The cDNA strand was generated using AMV reverse transcriptase and 20 units of RNase inhibitor. The reaction mix was incubated for 50 min at 42°C, followed by an enzyme inactivation step of 15 min at 70°C. For PCR, 50 μl of reaction mix contained cDNA, 25 μl of SYBR Green JumpStart Taq ReadyMix, 0.5 μl of internal reference dye, and 14.5 μl of corresponding oligonucleotide primers (80 nM final concentration). The Bcl 2, Bcl-X L, Bak, and Bad primer pairs were purchased from R & D Systems (Minneapolis, MN). Amplification and detection were performed using the SYBR Green method and the Applied Biosystems (Foster City, CA) 7500 Real-Time PCR System with the following profile: 1 cycle at 94°C for 2 min, 40 cycles at 94°C for 15 s, 60°C for 1 min, 72°C for 1 min. The fluorescence resulted from the incorporation of SYBR Green dye into the double-stranded DNA that was produced during the PCR reaction, and emission data were quantified using the threshold cycle (CT) value.
Caspase-3 Cellular Activity Assay
Caspase-3 activity was measured in PMC extracts as recommended by the manufacturer (Calbiochem, San Diego, CA). In brief, mouse PMCs (20 × 106/ml) were grown to confluence and infected with S. aureus (1:10, PMC : S. aureus) or left uninfected. Cell lysates were prepared in ice-cold lysis buffer, left on ice for 10 min, and centrifuged. The protein concentrations of the cell lysates were determined using the BCA reagent method. Supernatants were collected and frozen at −70°C until use. Before starting the assay, the plate conversion factor was determined. The enzyme activity was expressed as pmol substrate/min. Standard substrate p-nitroaniline (pNA) (50 μM) was used. The samples were run in triplicate and 10 μl of caspase-3 inhibitor (Ac-DEVD-CHO) was added to prepare the inhibitor-treated samples. To 10 μl of test samples 40 μl of assay buffer and 50 μl of caspase-3 substrate I (Ac-DEVE-pNA) were added and incubated at 37°C for 30 min. The absorbance was read at 405-nm excitation and 460-nm emission using a plate reader. The data were collected from 5 to 120 min and analyzed using following equation:
The caspase-3 activity was expressed as pmol/min/μg protein.
Statistical Analysis
Data were analyzed using SigmaStat statistical software (Apple Computer, Cupertino, CA). Results are expressed as mean ± SE. The data were analyzed by analysis of variance (ANOVA) with the use of the Student-Newman-Keuls test for multiple comparisons and was considered significant if p < 0.05.
Results
Intracellular S. aureus Viability in PMCs over Time
The live intracellular bacteria were determined by counting CFUs. The infected cells were lysed and plated on agar plates. We enumerated the number of intracellular bacteria at 3, 6, 12, 24, 48, and 72 h after infection with S. aureus using 1:1, 1:10, and 1:100 MOI. The intracellular CFUs increased with increasing MOI. Each MOI demonstrated a distinct and significantly increased CFU after 6 h. After 12 h of infection a significant increase in CFUs was noted with both 1:10 and 1:100 MOI. The intracellular viability of S. aureus increased over time until 24 h, after which it plateaued (Fig. 1).
Intracellular viable S. aureus (CFU) in pleural mesothelial cells over time. PMC cultures were incubated with 1, 10, or 100 MOI of S. aureus per mesothelial cell for 3, 6, 12, 24, 48, and 72 h. The data represent mean ± SE CFU of three separate experiments run as duplicates. The data also compared in each MOI over time and the p values are indicated as * p < 0.001 compared with 1:1 MOI and # p < 0.001 compared with 1:10 MOI
S. aureus Infection with Increasing MOI Demonstrated Increased Apoptosis in PMCs
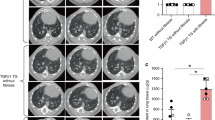
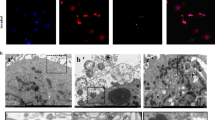
To evaluate the percentage of apoptosis of PMCs, cells were infected with S. aureus or left uninfected for 6, 12, 24, and 48 h. The in situ detection of apoptotic DNA was estimated by TUNEL, which is based on the specific staining of the 3′ hydroxyl ends of the fragmented DNA within apoptotic cells. We estimated the percentage of apoptotic cells over time after infection with S. aureus using 1:1, 1:10, and 1:100 MOI (PMC : S. aureus). Staphylococcus aureus induced apoptosis in PMCs in a time-dependent manner, and the percentage of apoptotic cells increased with increasing MOI (Fig. 2A). In S. aureus-infected PMCs (1:10 MOI), the percentage of apoptosis was 15.08 ± 1.58% after 12 h, which is statistically significant (p < 0.001) compared to that of uninfected PMCs. After 24 h of S. aureus infection a further increase in apoptosis (32.49 ± 2.05%) was noted; however, no apoptosis was noted in uninfected PMCs. The percentage of apoptotic cells at 48 h in S. aureus-infected and uninfected PMCs were 41.49 ± 3.9% and 7.28 ± 0.91%, respectively. Figure 2B is a representative example of in situ TUNEL labeling of apoptotic cells in S. aureus-infected and uninfected PMCs at 24 h. TUNEL positive staining was observed in nuclei and nuclear fragments with the morphologic characteristics of apoptosis in S. aureus-infected PMCs compared to uninfected PMCs. The identification of stained apoptotic bodies was confirmed by nuclear condensation and cytoplasmic compaction.
S. aureus-induced pleural mesothelial cell apoptosis as estimated by TUNEL. A Increasing S. aureus MOI induced PMC apoptosis over time. PMC cultures were incubated with 1, 10, or 100 CFU of S. aureus per mesothelial cell and stained by TUNEL as described in the Methods section. *p < 0.001 compared to uninfected and S. aureus-infected PMCs with listed MOI. The data also compared in each MOI over time and the p values are indicated as !p < 0.001 compared with 6 h, #p < 0.001 compared with 12 h, and @p < 0.001 compared with 24 h. Data are presented as mean ± SE of three separate experiments estimated at three different times. B Representative image of TUNEL positive staining to demonstrate PMC apoptosis. PMCs incubated in the presence of SFM or S. aureus (1:10, PMC : S. aureus) for 24 h. PMC apoptosis was detected in situ by TUNEL-immunoperoxidase reaction. The data shown are single representatives of three independent experiments. Magnification: × 400. Scale bar = 50 μm
S. aureus Induces DNA Fragmentation in PMCs
DNA fragmentation is a hallmark of apoptosis. DNA fragmentation was evaluated by ladder analysis in agarose gels. Total DNA extracted from PMCs infected with S. aureus and uninfected PMCs was visualized (Fig. 3). Six hours after S. aureus infection, the laddering pattern was observed and it increased over time. No DNA laddering was noted in uninfected PMCs.
Staphylococcus aureus-induced DNA fragmentation in PMCs. The data presented are DNA gels stained with ethidium bromide demonstrating the typical apoptosis laddering pattern. PMCs cultured in the presence of SFM or S. aureus (1:10, PMC : S. aureus). Lane M = 100-bp DNA ladder. Lanes 1–4 are 6, 12, 24, and 48 h of exposure, respectively. The data shown are representative of three independent experiments
S. aureus Induces the Expression of c-fos and c-jun
The expression of early response genes c-fos and c-jun increased in S. aureus-treated PMCs from 3 to 12 h. We noted a steady increase in both c-fos and c-jun expression in S. aureus-infected PMCs up to 12 h. The maximum expression of c-fos and c-jun was noted at 12 h. However, after 24 h a significant decrease in the expression of c-fos and c-jun was noted in S. aureus-infected PMCs (Fig. 4). There was no significant c-fos expression noted in uninfected PMCs; however, there was some faint expression of c-jun but it was 12-fold lower than S. aureus-induced response (Fig. 5). The housekeeping gene β-actin was used to demonstrate equal loading of protein.
Staphylococcus aureus-induced c-fos expression in PMCs. Western Blot analysis of resting and S. aureus-infected PMC nuclear lysates. Upper panel: relative optical densities, middle panel = autoradiograph showing c-fos expression, lower panel = autoradiograph showing β-actin expression demonstrating equal sample loading. Data shown are representative of three independent experiments. Relative OD = relative optical density as estimated by densitometry. *p < 0.001 compared with uninfected PMCs
Staphylococcus aureus-induced c-jun expression in PMCs. Western Blot analysis of resting and S. aureus-infected PMC nuclear lysates. Upper panel = relative optical densities, middle panel = autoradiograph showing c-jun expression, lower panel = autoradiograph showing β-actin expression demonstrating equal sample loading. Data shown are representative of three independent experiments. Relative OD = relative optical density as estimated by densitometry. *p < 0.001 compared with uninfected PMCs
S. aureus Induces AP-1 DNA Binding Protein Expression
The effect of S. aureus on AP-1 DNA binding activity in PMCs was estimated by gel shift assay. PMCs were incubated for 12 h in the presence or absence of S. aureus and then the cells were harvested for nuclear protein. In cells treated with S. aureus a significant increase in AP-1 DNA binding complex was noted. The DNA binding complex was completely inhibited by coincubation of nuclear extracts, with an excess of unlabeled AP-1 oligonucleotide. The pretreatment of nuclear lysate with anti-c-fos and anti-c-jun antibodies decreased the expression of AP-1 DNA binding complex (Fig. 6).
AP-1 DNA binding activity in S. aureus-infected and uninfected PMCs. Nuclear protein extracts were prepared from uninfected control (SFM) or S. aureus-infected PMCs for 12 h. Protein-DNA complex was resolved by nondenaturing gel electrophoresis and visualized by autoluminograph. Formation of a specific AP-1 DNA-protein complex was completely inhibited by coincubation with a 50-fold molar excess unlabeled AP-1 oligonucleotide. The pretreatment of nuclear lysate with antibodies specific to c-fos and c-jun decreased the expression of AP-1 DNA complex
S. aureus Induces Proapoptosis Genes in PMCs
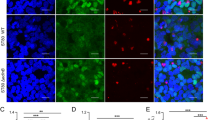
S. aureus infection induced significantly higher expression of proapoptotic genes compared to the antiapoptotic genes Bcl2 and Bcl-XL in PMCs. In S. aureus-infected PMCs Bcl2 and Bcl-XL gene expression spiked at 12 h; however, this response was short-lived and declined to basal levels thereafter (Fig. 7A, B). In contrast, there was no significant increase in Bak and Bad gene expression 12 h of S. aureus infection. However, there was a significant increase in Bak and Bad gene expression in S. aureus-infected PMCs after 24 and 48 h (Fig. 7C, D). In uninfected PMCs Bcl-XL gene expression was threefold higher, whereas Bcl2 expression was fivefold higher than in S. aureus-infected cultures at 24 and 48 h. In uninfected PMCs both Bcl-XL and Bcl2 expression was maintained and remained higher than that in S. aureus-infected PMCs after 24 h.
Relative proapoptotic and antiapoptotic gene expression in resting and S. aureus-infected PMCs as estimated by real-time quantitative PCR. PMCs were infected with S. aureus or left untreated for 0, 6, 12, 24, and 48 h. A Bcl-X L and B Bcl 2 (antiapoptotic genes). C Bak and D Bad (proapoptotic genes). The data are mean ± SE of three independent experiments. *p < 0.001 for S. aureus-infected PMCs vs. SFM (serum-free medium)
To understand the role of AP-1 in the regulation of proapoptotic genes Bak and Bad, PMCs were transfected with AP-1 stealth RNAi (100 μM) or scrambled RNAi (RNAi-Sc) and infected with S. aureus for 24 h. Silencing the AP-1 gene with Ap1-RNAi significantly inhibited the S. aureus-induced expression of the proapoptotic Bak and Bad genes in PMCs compared to scrambled RNAi-treated PMCs (Fig. 8). This suggests that AP-1 plays a key role in the regulation of proapoptotic genes during S. aureus-induced PMC apoptosis.
Silencing AP-1 expression inhibits S. aureus-induced proapoptotic gene expression in PMCs. Pleural mesothelial cells were infected for 24 h with S. aureus in the presence and absence of AP-1 RNAi, and Bak and Bad gene expression was estimated by quantitative PCR as discussed in the Methods section. The data are mean ±SE of three independent experiments. *p < 0.001 compared with uninfected PMCs and # p < 0.001 compared with S. aureus-induced response
S. aureus Infection Induces Cytochrome-c Release in PMCs
Staphylococcus aureus infection enhanced cytochrome-c release in PMCs. In uninfected PMCs there was no evidence of cytochrome-c release throughout the study period. In S. aureus-infected PMCs a significant increase in the cytochrome-c release was noted as early as 6 h and maximum cytochrome-c release was noted after 12 h of S. aureus infection. However, this response plateaued 24 h after S. aureus infection (Fig. 9).
Cytochrome-c response in S. aureus-infected and uninfected PMCs. Pleural mesothelial cell lysates were subjected to SDS-PAGE and Western blot analysis as described in the Methods section. Upper panel = relative optical densities, middle panel = autoradiograph showing cytochrome-c expression, lower panel = autoradiograph showing β-actin expression demonstrating equal sample loading. Data presented are representative of three independent observations. Relative OD = relative optical density as estimated by densitometry. *p < 0.001 compared with uninfected PMCs
S. aureus Infection Induces Caspase-3 Activity in PMCs
Caspase-3 activity was estimated in PMCs 12 h after S. aureus infection along with parallel uninfected PMC cultures. In S. aureus-infected PMCs a significant increase in the caspase-3 activity was noted. In uninfected PMCs there was no evidence of caspase-3 activity. We also monitored the kinetics of caspase-3 activity in S. aureus-infected and uninfected PMCs. We noted a significant increase in the caspase-3 activity as early as 10 min in S. aureus-infected PMCs and maximum activity was noted after 1 h; the activity decreased thereafter. However, this response was significantly inhibited in caspase-3 inhibitor-treated samples, indicating a caspase-3-specific response. These results suggest that S. aureus induces apoptosis in PMCs in a caspase-3-dependent manner (Fig. 10).
Staphylococcus aureus induces caspase-3 expression in pleural mesothelial cells. Pleural mesothelial cells were infected with S. aureus for 12 h and caspase-3 activity was estimated. The data represent mean ± SE of three independent experiments. *p < 0.001 compared with uninfected PMCs and #p < 0.001 compared with S. aureus-induced response in the absence of caspase-3 inhibitor
Discussion
Staphylococcus aureus is a leading cause of the development of complicated parapneumonic effusions, especially in children. Early diagnosis and rapid drainage of infected pleural effusions is necessary to reduce the morbidity and mortality in empyema. The pleural mesothelial cells play a critical role in pleural integrity, and loss of pleural mesothelial integrity secondary to infection leads to pleural barrier dysfunction. In empyema, pleural mesothelial cells are constantly exposed to invading microbial pathogens. In earlier studies from this laboratory, we reported that S. aureus induced acute inflammatory responses in the pleural space via induction of murine KC and MIP-2 [7]. We also demonstrated that S. aureus infection results in pleural mesothelial barrier dysfunction [8]. We now provide evidence that S. aureus infection induces apoptosis in PMCs via induction of c-fos and c-jun early response genes that regulate downstream modulators of the apoptosis pathway. S. aureus induced apoptosis in PMCs in a time- and MOI-dependent manner as evaluated by TUNEL assay and apoptotic DNA ladder analysis. The number of intracellular bacteria in PMCs increased dramatically after 3 h of infection. This increased intracellular survival of S. aureus was directly correlated with PMC apoptosis as evidenced by TUNEL staining. S. aureus infection induced expression in PMCs of the proapoptotic genes Bad and Bak. Concomitantly, the expression of the antiapoptotic genes Bcl2 and Bcl-XL was inhibited in these cells. We also noted an increase in cytochrome-c release in S. aureus-infected PMCs, which directly correlated with apoptosis.
During bacterial infection internalized pathogens multiply in the cytoplasm of the cell and are transmitted from cell to cell and thus achieve the infection-growth cycle [30]. In epithelial and endothelial cells, intracellular survival of S. aureus was noted to induce apoptosis [11, 13]. It is evident that apoptosis of S. aureus-infected PMCs is due to intracellular bacterial growth over time. It is possible that free and multiplying bacteria in the cytoplasm may be responsible for inducing proapoptosis signals in PMCs. Increased expression of the early response genes c-fos and c-jun has been related to the development of apoptosis [31, 32]. In addition, signaling pathways for apoptosis have been linked to activation of specific signaling cascades and early accumulation of c-fos, c-jun, and c-myc [33–35]. Our data demonstrate that S. aureus induced expression of c-fos and c-jun early response genes in the early phase of infection in primary mouse PMCs. In uninfected PMCs no significant increase in c-fos and c-jun expression was noted. In a similar study with IL-2-dependent mouse melanoma cells, interleukin deprivation induced apoptosis via c-fos and c-jun induction, and inhibition of c-fos and c-jun expression by anti-sense oligonucleotides in these cells protected them from apoptosis induced by interleukin deprivation [33]. Preston et al. [36] demonstrated that c-fos gene expression causes apoptosis. High levels of c-fos were observed in mouse tissue in which apoptosis was part of normal development [35]. In addition, S. aureus infection was noted to induce c-jun expression in normal mouse osteoblasts [37]. A study on lymphoid cell lines also demonstrated that increased expression of c-jun induced apoptosis in response to various stimuli [33]. The mitogen-activated protein kinases (MAPK) and extracellular signal regulated protein kinases (ERK1 and ERK2) are activated during the invasion of bacteria, including S. aureus [37, 38]. MAPK-activated JNK phosphorylates the c-jun, which in turn enhances transcription of FasL and TNF-α genes which results in apoptosis [31]. In addition, JNK activation was also implicated as essential for induction of apoptosis because it is known to induce c-jun transcription [39]. During S. aureus infection the induction of early response genes c-fos and c-jun may regulate downstream events leading to apoptosis in PMCs.
AP-1 is considered the nuclear decision-maker that determines survival or cell death in response to extracellular stimuli. Cell death induced by Fas ligand (FasL) and its cell surface receptor Fas is a classical example of apoptosis induced by external signal. The FasL and TNF-α genes contain AP-1 binding sites. The combination of c-fos and c-jun to form the AP-1 complex is essential for the apoptotic process. We noted increased expression of c-fos and c-jun in S. aureus-infected cells after 6 and 12 h of infection. When we measured the AP-1 protein DNA binding with c-fos/c-jun in PMCs, we noticed an increase in AP-1 DNA binding complex in the S. aureus-infected PMCs. In addition, pretreatment of nuclear lysate with anti-c-fos and anti-c-jun antibodies significantly decreased the expression of AP-1 DNA binding complex. In S. aureus-infected PMCs the expression of AP-1 DNA binding complex directly correlated with the expression of c-fos and c-jun. These components of AP-1 are involved in apoptosis; AP-1 is known to modulate apoptosis and the upregulation of c-fos and c-jun correlated with increased apoptosis [40]. S. aureus-induced apoptosis in PMCs was multiplicity-of-infection dependent. In PMCs the intracellular growth of S. aureus was directly correlated with the expression of c-fos and c-jun early response genes. Taken together, these data indicate that uncontrolled growth of bacteria in PMCs induces c-fos/c-jun genes via activation transcription activator factor AP-1. In addition, silencing AP-1 gene expression with RNAi-inhibited S. aureus induced Bak and Bad gene expression, suggesting that AP-1 activation initiates the apoptotic pathway during S. aureus infection in PMCs. Thus, during S. aureus infection the expression of AP-1 complex may reflect a functional role in activating putative downstream genes involved in later apoptosis events in PMC.
The apoptosis process is controlled mainly by Bcl 2 family proteins [18]. Bcl 2 and Bcl-X L function as death antagonists and Bad and Bax function as apoptotic agonists within the apoptosis pathway [18, 41]. We noted significantly higher Bcl 2 and Bcl-X L gene expression in resting PMCs than in S. aureus-infected PMCs. Interestingly, after 12 h of S. aureus infection a spike in Bcl 2 and Bcl-X L gene expression was noticed. S. aureus-induced expression of Bcl 2 and Bcl-X L during the initial phase of infection may be related to a survival mechanism to counter the infection. In contrast, Bad and Bak mRNA expression was significantly higher in S. aureus-infected PMCs than in resting PMCs. Bcl 2 is a mitochondrial protein and when expressed it inhibits the cell to undergo apoptosis [42], whereas Bak expression accelerates proapoptotic activity in cells [43]. Our data suggest that S. aureus infection modulates expression of pro- and antiapoptotic genes, especially by selective induction of the proapoptotic genes that mediate apoptosis in PMCs.
Mitochondria play a major role in cell death by releasing the proapoptotic proteins into cytosol. The cytochrome-c is released from mitochondria complexes with apoptosis protease-activating factor-1 (Apaf-1) and activates caspase-9 that eventually results in caspase-3 activation [44]. In cells undergoing apoptosis, caspase-3 activation is required for DNA fragmentation [45]. Caspases are primary effector molecules of apoptosis [15]. A recent study reported that in peritoneal mesothelial cells S. aureus induced apoptosis in the caspase-3-independent pathway [46]. However, we noted significant increases in caspase-3 activity in S. aureus-infected PMCs. This indicates that S. aureus infection induces distinct apoptotic pathways in pleural mesothelial and peritoneal mesothelial cells. In addition, Bak and Bax directly mediate the release of cytochrome-c into the cytoplasm to initiate apoptosis [47, 48]. In the late phase of S. aureus infection we noted an increase in Bak and Bad expression. Our results indicate that during S. aureus infection Bak and Bad expression is implicated in the PMC apoptosis and it is in agreement with previous studies [49–51].
In conclusion, the present data demonstrate that invading bacteria (S. aureus) induce early response genes c-fos and c-jun and proapoptosis genes Bad and Bak that lead to PMC apoptosis. The higher risk of morbidity in patients with empyema may, in part, be due to pathogen-induced pleural mesothelial apoptosis and loss of mesothelial monolayer integrity. However, further studies are needed to understand the role of the c-fos and c-jun early response genes in the regulation of proapoptosis and antiapoptosis genes during S. aureus infection in PMCs.
References
Ashbaugh DG (1991) Empyema thoracis. Factors influencing morbidity and mortality. Chest 99:1162–1165
Freij BJ, Kusmiesz H, Nelson JD , McCracken GH Jr (1984) Parapneumonic effusions and empyema in hospitalized children: a retrospective review of 227 cases. Pediatr Infect Dis 3:578–591
Afessa B, Green B (2000) Bacterial pneumonia in hospitalized patients with HIV infection: the Pulmonary Complications, ICU Support, and Prognostic Factors of Hospitalized Patients with HIV (PIP) Study. Chest 117:1017–1022
Hardie W, Bokulic R, Garcia VF, Reising SF, Christie CD (1996) Pneumococcal pleural empyemas in children. Clin Infect Dis 22:1057–1063
Satpathy SK, Behera CK, Nanda P (2005) Outcome of parapneumonic empyema. Indian J Pediatr 72:197–199
Strange C, Sahn SA (1999) The definitions and epidemiology of pleural space infection. Semin Respir Infect 14:3–8
Mohammed KA, Nasreen N, Ward MJ, Antony VB (2000) Induction of acute pleural inflammation by Staphylococcus aureus. I. CD4+ T cells play a critical role in experimental empyema. J Infect Dis 181:1693–1699
Mohammed KA, Nasreen N, Hardwick J, Logie CS, Patterson CE, Antony VB (2001) Bacterial induction of pleural mesothelial monolayer barrier dysfunction. Am J Physiol Lung Cell Mol Physiol 281:L119–L125
Hamill RJ, Vann JM, Proctor RA (1986) Phagocytosis of Staphylococcus aureus by cultured bovine aortic endothelial cells: model for postadherence events in endovascular infections. Infect Immun 54:833–836
Ogawa SK, Yurberg ER, Hatcher VB, Levitt MA, Lowy FD (1985) Bacterial adherence to human endothelial cells in vitro. Infect Immun 50:218–224
Bayles KW, Wesson CA, Liou LE, Fox LK, Bohach GA, Trumble WR (1998) Intracellular Staphylococcus aureus escapes the endosome and induces apoptosis in epithelial cells. Infect Immun 66:336–342
Esen M, Schreiner B, Jendrossek V, Lang F, Fassbender K, Grassme H, Gulbins E (2001) Mechanisms of Staphylococcus aureus induced apoptosis of human endothelial cells. Apoptosis 6:431–439
Menzies BE, Kourteva I (1998) Internalization of Staphylococcus aureus by endothelial cells induces apoptosis. Infect Immun 66:5994–5998
Thompson CB (1995) Apoptosis in the pathogenesis and treatment of disease. Science 267:1456–1462
Cohen GM (1997) Caspases: the executioners of apoptosis. Biochem J 326(Pt 1):1–16
Henkart PA, Grinstein S (1996) Apoptosis: mitochondria resurrected? J Exp Med 183:1293–1295
Chittenden T, Harrington EA, O’Connor R, Flemington C, Lutz RJ, Evan GI, Guild BC (1995) Induction of apoptosis by the Bcl-2 homologue Bak. Nature 374:733–736
Adams JM, Cory S (2001) Life-or-death decisions by the Bcl-2 protein family. Trends Biochem Sci 26:61–66
Datta R, Kharbanda S, Kufe D (1990) Regulation of jun-B gene expression by 1-beta-D-arabinofuranosyl-cytosine in human myeloid leukemia cells. Mol Pharmacol 38:435–439
Kharbanda SM, Sherman ML, Kufe DW (1990) Transcriptional regulation of c-jun gene expression by arabinofuranosylcytosine in human myeloid leukemia cells. J Clin Invest 86:1517–1523
Angel P, Karin M (1991) The role of Jun, Fos and the AP-1 complex in cell-proliferation and transformation. Biochim Biophys Acta 1072:129–157
Piechaczyk M, Blanchard JM (1994) c-fos proto-oncogene regulation and function. Crit Rev Oncol Hematol 17:93–131
Mohammed KA, Nasreen N, Ward MJ, Antony VB (1999) Helper T cell type 1 and 2 cytokines regulate C-C chemokine expression in mouse pleural mesothelial cells. Am J Respir Crit Care Med 159:1653–1659
Andrews PM, Porter KR (1973) The ultrastructural morphology and possible functional significance of mesothelial microvilli. Anat Rec 177:409–426
Connell ND, Rheinwald JG (1983) Regulation of the cytoskeleton in mesothelial cells: reversible loss of keratin and increase in vimentin during rapid growth in culture. Cell 34:245–253
Mohammed KA, Nasreen N, Ward MJ, Antony VB (1998) Macrophage inflammatory protein-1alpha C-C chemokine in parapneumonic pleural effusions. J Lab Clin Med 132:202–209
Nasreen N, Mohammed KA, Dowling PA, Ward MJ, Galffy G, Antony VB (2000) Talc induces apoptosis in human malignant mesothelioma cells in vitro. Am J Respir Crit Care Med 161:595–600
Nicoletti I, Migliorati G, Pagliacci MC, Grignani F, Riccardi C (1991) A rapid and simple method for measuring thymocyte apoptosis by propidium iodide staining and flow cytometry. J Immunol Methods 139:271–279
Heintz NH, Janssen YM, Mossman BT (1993) Persistent induction of c-fos and c-jun expression by asbestos. Proc Natl Acad Sci U S A 90:3299–3303
Tilney LG, Portnoy DA (1989) Actin filaments and the growth, movement, and spread of the intracellular bacterial parasite, Listeria monocytogenes. J Cell Biol 109:1597–1608
Hess J, Angel P, Schorpp-Kistner M (2004) AP-1 subunits: quarrel and harmony among siblings. J Cell Sci 117:5965–5973
Eferl R, Wagner EF (2003) AP-1: a double-edged sword in tumorigenesis. Nat Rev Cancer 3:859–868
Colotta F, Polentarutti N, Sironi M, Mantovani A (1992) Expression and involvement of c-fos and c-jun protooncogenes in programmed cell death induced by growth factor deprivation in lymphoid cell lines. J Biol Chem 267:18278–18283
Grassilli E, Carcereri de Prati A, Monti D, Troiano L, Menegazzi M, Barbieri D, Franceschi C, Suzuki H (1992) Studies of the relationship between cell proliferation and cell death. II. Early gene expression during concanavalin A-induced proliferation or dexamethasone-induced apoptosis of rat thymocytes. Biochem Biophys Res Commun 188:1261–1266
Smeyne RJ, Vendrell M, Hayward M, Baker SJ, Miao GG, Schilling K, Robertson LM, Curran T, Morgan JI (1993) Continuous c-fos expression precedes programmed cell death in vivo. Nature 363:166–169
Preston GA, Lyon TT, Yin Y, Lang JE, Solomon G, Annab L, Srinivasan DG, Alcorta DA, Barrett JC (1996) Induction of apoptosis by c-Fos protein. Mol Cell Biol 16:211–218
Ellington JK, Elhofy A, Bost KL, Hudson MC (2001) Involvement of mitogen-activated protein kinase pathways in Staphylococcus aureus invasion of normal osteoblasts. Infect Immun 69:5235–5242
Tang P, Rosenshine I, Finlay BB (1994) Listeria monocytogenes, an invasive bacterium, stimulates MAP kinase upon attachment to epithelial cells. Mol Biol Cell 5:455–464
Verheij M, Bose R, Lin XH, Yao B, Jarvis WD, Grant S, Birrer MJ, Szabo E, Zon LI, Kyriakis JM, Haimovitz-Friedman A, Fuks Z, Kolesnick RN (1996) Requirement for ceramide-initiated SAPK/JNK signalling in stress-induced apoptosis. Nature 380:75–79
Karin M, Liu Z, Zandi E (1997) AP-1 function and regulation. Curr Opin Cell Biol 9:240–246
Reed JC (1996) Mechanisms of Bcl-2 family protein function and dysfunction in health and disease. Behring Inst Mitt (97):72–100
Ibrado AM, Huang Y, Fang G, Bhalla K (1996) Bcl-xL overexpression inhibits taxol-induced Yama protease activity and apoptosis. Cell Growth Differ 7:1087–1094
Zhang M, Liu H, Guo R, Ling Y, Wu X, Li B, Roller PP, Wang S, Yang D (2003) Molecular mechanism of gossypol-induced cell growth inhibition and cell death of HT-29 human colon carcinoma cells. Biochem Pharmacol 66:93–103
Green DR, Kroemer G (2004) The pathophysiology of mitochondrial cell death. Science 305:626–629
Janicke RU, Sprengart ML, Wati MR, Porter AG (1998) Caspase-3 is required for DNA fragmentation and morphological changes associated with apoptosis. J Biol Chem 273:9357–9360
Haslinger-Loffler B, Wagner B, Bruck M, Strangfeld K, Grundmeier M, Fischer U, Volker W, Peters G, Schulze-Osthoff K, Sinha B (2006) Staphylococcus aureus induces caspase-independent cell death in human peritoneal mesothelial cells. Kidney Int 70:1089–1098
Yamasaki E, Wada A, Kumatori A, Nakagawa I, Funao J, Nakayama M, Hisatsune J, Kimura M, Moss J, Hirayama T (2006) Helicobacter pylori vacuolating cytotoxin induces activation of the proapoptotic proteins Bax and Bak, leading to cytochrome c release and cell death, independent of vacuolation. J Biol Chem 281:11250–11259
Jurgensmeier JM, Xie Z, Deveraux Q, Ellerby L, Bredesen D, Reed JC (1998) Bax directly induces release of cytochrome c from isolated mitochondria. Proc Natl Acad Sci U S A 95:4997–5002
Wesson CA, Deringer J, Liou LE, Bayles KW, Bohach GA, Trumble WR (2000) Apoptosis induced by Staphylococcus aureus in epithelial cells utilizes a mechanism involving caspases 8 and 3. Infect Immun 68:2998–3001
Baran J, Weglarczyk K, Mysiak M, Guzik K, Ernst M, Flad HD, Pryjma J (2001) Fas (CD95)-Fas ligand interactions are responsible for monocyte apoptosis occurring as a result of phagocytosis and killing of Staphylococcus aureus. Infect Immun 69:1287–1297
Urnowey S, Ansai T, Bitko V, Nakayama K, Takehara T, Barik S (2006) Temporal activation of anti- and pro-apoptotic factors in human gingival fibroblasts infected with the periodontal pathogen, Porphyromonas gingivalis: potential role of bacterial proteases in host signalling. BMC Microbiol 6:26
Acknowledgment
This work was supported in part by grant NIH RO1 AI41877-04 from the National Institutes of Health and by a Veterans Affairs merit review grant.
Author information
Authors and Affiliations
Corresponding author
Additional information
Kamal A. Mohammed, Najmunnisa Nasreen contributed equally to this work.
Rights and permissions
About this article
Cite this article
Mohammed, K.A., Nasreen, N. & Antony, V.B. Bacterial Induction of Early Response Genes and Activation of Proapoptotic Factors in Pleural Mesothelial Cells. Lung 185, 355–365 (2007). https://doi.org/10.1007/s00408-007-9046-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00408-007-9046-6