Abstract
Hidradenoma papilliferum (HP) is a rare, small, benign, cystic, papillary, slow growing tumor occurring in anogenital region of adult women. The authors describe a case of large, rapidly enlarging HP of vulva in a 25-year-old woman and review the literature available on this rare condition.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Hidradenoma papilliferum (HP) is a rare, small, benign, cystic, papillary, slow growing tumor occurring in anogenital region of adult women. It may pose diagnostic difficulties with Bartholin cysts/abscesses, lipoma and some premalignant/malignant vulval lesions. The authors describe a case of a large, rapidly enlarging HP of vulva in a young woman and review the literature available on this rare condition.
Case report
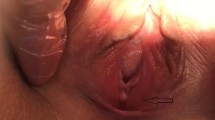
A 25-years-old para 2 woman presented to the outpatient department with a painless swelling of increasing size on the external genitalia. The woman had detected the pea sized swelling 4 months ago. Examination revealed a 8 × 6 cm sized, pedunculated, non-tender, soft swelling arising from the sulcus between the left sided labium majus and minor, at the junction of upper 3/4th and lower 1/4th (Fig. 1). Speculum and bimanual examinations were essentially normal. A provisional diagnosis of lipoma of the vulva was made.
After a complete preoperative workup, the patient underwent complete excision of the lesion with an uneventful postoperative course. Histology revealed well circumscribed dermal nodule with invaginations lined by numerous papillary projections which were, at places, lined by cells with apocrine differentiation (Fig. 2).
The woman is well after 2 years of follow-up.
Discussion
Hidradenoma Papilliferum is a rare, benign, cystic, papillary tumor that occurs primarily in vulva of Caucasian women [1]. It is believed to arise from the anogenital glands and exhibits both apocrine and eccrine differentiation, with the former being more common [2]. It tends to occur exclusively in post pubescent white women between 30 and 70 years of age, most often in the fourth decade [1]. It usually presents as a solitary, slow growing (size range: 2 mm–3 cm), painless nodule/tumor on the labia majora/minora/sulcus between them or in the perianal area. Thirty-eight percent of these cases reportedly originate from labia majora and 26% from labia minora. Occasionally, the tumor becomes elevated to form a reddish brown papillary mass and the surface may ulcerate to mimic a malignancy on gross appearance [3]. The lesions that are located on the lower aspects of labia majora/minora or in the interveining sulcus may initially be misdiagnosed as Bartholin cyst/abscess. Pain may be a feature in the event of concomitant/subsequent development of Bartholin’s abscess. Docimo et al. [1] have suggested presence of HP, particularly that originating from labia minora, to be a predisposition for development of Bartholin’s abscess. A disruption/blockade to drainage of the Bartholin’s duct by a tumor in the vicinity may also result in development of Bartholin cyst/abcess. Literature reports one such case to be that of cellular angiofibroma and another to have histologically turned out to be leiomyosarcoma, although malignant change in HP is otherwise extremely rare [4], [5]. Skene duct cysts, epidermal inclusion cysts, seborrheic dermatitis, acrochordon (fibroepithelial polyp), fibroma, fibromyoma, dermatofibroma, lipoma, syringoma, hemangioma, lymphangioma, angiokeratoma, pyogenic granuloma, papillomatosis, varicose veins and malignancy could be considered among the clinical differential diagnoses. Although considered essentially benign, there have been reports of concomitant presence of vulvar invasive squamous cell carcinoma, Paget’s disease and melanocytic neoplasia [6, 7]. Nishie et al. reported a case of vulvar HP having mixed histopathologic features of syringocystadenoma papilliferum and anogenital mammary like glands, suggesting the development of HP from these mammary like glands [8].
Histologically, the tumor represents an adenoma with apocrine differentiation and is located in the dermis with no connection to the overlying epidermis. Under low power magnification, the tumor simulates a well-differentiated adenocarcinoma [9]. Stromal compression often results in formation of a well-circumscribed pseudocapsule. Entrapment of epithelial cells within the compressed connective tissue may result in a pseudoinfiltrative appearance. Obscure tubular and cystic structures are evident within the tumor, with papillary folds projecting into the cystic spaces. The lumina are usually surrounded by a double layer of cells consisting of inner layer of secretory cells and an outer cuboidal layer with myoepithelial cells. Occasionally, the lumina may be lined by a single crest of columnar cells with oval, pale staining nuclei and faintly eosinophilic cytoplasm. HP has histological features analogous to intraductal papilloma of breast. Vazmitel et al. [10] reported a case of ductal carcinoma insitu arising in HP along with demonstration of Human Papilloma Virus-16 (HPV-16) in it, thus suggesting a probable aetiological role of the virus in development of the carcinoma. Kazakov et al. [11] reported detection of HPV in 4 of 15 cases of HP with oxyphilic metaplasia and in 3 of 16 conventional papillary hidradenomas. Of the HPV types 16, 31, 33, 53, and 56 detected in the study, the last one was the most common. A causal role of this virus in HP has been suggested but is not yet confirmed.
As the condition has a benign course most often, surgical excision has been regarded as adequate. However, the clinical presentation may become increasingly indistinct when the condition simultaneously occurs with Bartholin’s cyst/abscess or with other cystic lesions of the vulva. The report, though infrequent, association or transformation into adenocarcinoma/adenosquamous/squamous carcinoma/Paget’s disease tends to suggest surgical excision with wide margins and careful follow-up to be a more appropriate approach of management. Simple drainage of recurrent Bartholin’s abscess may not be sufficient, especially in elderly women.
The young age of the woman of Asian origin, the large size of the tumor at presentation and a short history suggestive of rapid course of progression make the present case different from the common presentations of vulval HP.
Conclusion
Hidradenoma Papilliferum, a rare lesion of the anogenital area of adult women follows a slowly progressive benign course in most cases. Infrequently, it may harbour a malignant or premalignant lesion. Recurrent Bartholin’s abscess/cysts and/or ulcerated lesions particularly in the elderly should arouse such a suspicion. A multidisciplinary management may then be tailored to include wide surgical excision, a close follow-up and screening for HPV infections.
References
Docimo S, Shon W, Elkowitz DE (2008) Bartholin’s abcess arising within hidradenoma papilliferum of the vulva: a case report. Cases J 1:282
Meeker JH, Nenbecker RD, Helwig EB (1962) Hidradenoma papilliferum. Am J Clin Pathol 37:182–195
Handa Y, Yamanaka N, Inagaki H, Tomita Y (2003) Large ulcerated perianal hidradenoma papilliferum in a young female. Dermatol Surg 29(7):790–792
Silva AC, Nascimento AG, DaSilva CS, Murta EF, Adad SJ (2005) Cellular angiofibroma of the vulva: case report with clinicopathological and immunohistochemistry study. Sao Paulo Med J 123:250–252
Dewdney S, Kennedy CM, Galask RP (2005) Leiomyosarcoma of the vulva:a case report. J Reprod Med 50:630–632
Barre C, Lorenzato M, Bourdat B, Quereux C, Durlach A (2007) Vulvar invasive squamous cell carcinoma and hidradenoma papilliferum. Case report. Gynecol Obstet Fertil 35(9):776–779
Simpson WA, Burke M, Frappell J, Cook MG (1988) Paget’s disease, melanocytic neoplasia and hidradenoma papilliferum of the vulva. Histopathology 12(6):675–679
Nishie W, Sawamura D, Mayuzumi M, Takahashi S, Shimizu H (2004) Hidradenoma papilliferum with mixed histopathologic features of syringocystadenoma papilliferum and anogenital mammary like glands. J Cutan Pathol 31(8):561–564
Wilkinson EJ, Xie D (2004) Benign disorders of the Vulva. In: Kurman RJ (ed) Blaustein’s pathology of the female genital tract, 5th ed edn. Springer, New Delhi, pp 37–98
Vazmitel M, Spagnolo DV, Nemcova J, Michal M, Kazakov DV (2008) Hidradenoma papilliferum with a ductal carcinoma in situ component: case report and review of literature. Am J Dermatopathol 30(4):392–394
Kazakov DV, Mikyskona I, Kutzner H, Simpson RH, Hes O, Mukensnabl P et al (2005) Hidradenoma papilliferum with oxyphilic metaplasia: a clinicopathological study of 18 cases, including detection of human papilloma virus. Am J Dermatopathol 27(2):102–110
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Duhan, N., Kalra, R., Singh, S. et al. Hidradenoma papilliferum of the vulva: case report and review of literature. Arch Gynecol Obstet 284, 1015–1017 (2011). https://doi.org/10.1007/s00404-010-1784-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-010-1784-7