Abstract
Background
Inhibins and activins are important regulators of the female reproductive system. Recently, two novel inhibin subunits, named betaC and betaE, have been identified and shown to be expressed in several human tissues. However, only limited data on the expression of these novel inhibin subunits in normal human endometrial tissue and endometrial adenocarcinoma cell lines exist.
Materials and methods
Samples of proliferative and secretory human endometrium were obtained from five premenopausal, non-pregnant patients undergoing gynecological surgery for benign diseases. Normal endometrial tissue and Ishikawa endometrial adenocarcinoma cell lines were analyzed by immunohistochemistry, immunofluorescence and RT-PCR.
Results
Expression of the inhibin betaC and betaE subunits could be demonstrated at the protein level by means of immunohistochemical evaluation and at the transcriptional level by establishing a betaC- and betaE-specific RT-PCR analysis in normal human endometrial tissue and the parental Ishikawa cell line. Interestingly, in a highly de-differentiated subclone of the Ishikawa cell line lacking estrogen receptor expression, the expression of the inhibin-betaC subunit appeared strongly reduced.
Discussion
Here, we show for the first time that the novel inhibin/activin-betaC and -betaE subunits are expressed in normal human endometrium and the estrogen receptor positive human endometrial carcinoma cell line Ishikawa using RT-PCR and immunohistochemical detection methods. Interestingly, the Ishikawa minus cell line (lacking estrogen receptor expression) demonstrated no to minimal expression of the betaC subunit as observed with immunofluorescence and RT-PCR, suggesting a possible hormone- dependency of this subunit in human endometrial cancer cells. Moreover, because the Ishikawa cell line minus is thought to be a more malignant endometrial cell line than its estrogen receptor positive counterpart, inhibin-betaC subunit might be substantially involved in the pathogenesis and malignant transformation in human endometrium.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Inhibin/activin proteins belong to the transforming growth factor-β (TGF-β) family of growth and differentiation factors and were primarily isolated from the gonads [1–3]. Activins are homo- or heterodimers composed of two different β subunits (βA, βB), each encoded by a single gene. These β-subunits can either form activins by dimerization with a second β-subunit, or alternatively inhibins by dimerizing with a α-subunit. Thus, depending on the subunit combination, there are two forms of inhibin [namely inhibin A (α-βA) and inhibin B (α-βB)] and three isoforms of activin [namely activin A (βA–βA), activin B (βB–βB) and activin AB (βA–βB)] [1–3].
Recently, three additional β-subunits have been identified, determined as βC [4], βD [5] and βE [6]. Whereas the βD-subunit has only been detected in Xenopus, expression of the βC and βE genes could also be identified in humans [4, 7]. This two novel subunits share 82 and 61% amino acid sequence similarity of the mature peptides from rat and mouse, respectively [8, 9]. The inhibin/activin-βC protein was primarily found to be in human liver and prostate [10], while inhibin/activin-βE mRNA was predominantly expressed in human liver with low levels in heart, testis, leukocytes, skeletal muscle and placenta [7].
The expression of inhibin/activin subunits has been described in different gynecological organs, including normal and pathological human endometrium [11–16], suggesting different roles, such as paracrine modulators of endometrial cell function regulating endometrial maturation, decidualization and implantation processes [17] and malignant transformation [15, 16, 18, 19].
However, only limited data on the expression of the inhibin-βC and -βE subunits in human endometrial tissue exist. Therefore, aims of the present study were to evaluate the synthesis of the novel inhibin-βC and -βE subunits in normal human endometrium and the human endometrial cancer cell line Ishikawa.
Materials and methods
Tissue samples
Samples of human endometrium were obtained from five premenopausal, non-pregnant patients undergoing gynecological surgery either by D&C or hysterectomy for benign diseases, mainly uterine leiomyomata, at the 1st Department of Obstetrics and Gynaecology of the Ludwig-Maximilians-University Munich. Endometrium samples were classified according to anamnestic and histologic dating into proliferative (n = 5) and secretory phase (n = 5).
Generation of a polyclonal inhibin-βE peptide antibody
Anti-inhibin βE polyclonal antibodies were generated as custom-made antibodies in rabbits against a polypeptide of 16 amino acids of inhibin-βE [polypeptide-sequence: NH2-CRWGPRRRRQGSRTLL-COOH; amino acid position 144–158; accession number: AAH05161] as previously described by BioGenes (Berlin, Germany) [20]. A primary dose of 200 μg activin βE polypeptide was solubilized in Freund’s complete adjuvant (Sigma-Aldrich, Germany) and administered subcutaneously in rabbits. Three doses of the peptide solubilized in Freund’s incomplete adjuvant were administrated at intervals of 6 weeks. After the third booster injection (14 days), blood was collected from the rabbit, and the serum was separated. Antibodies were isolated by column chromatography with a protein A column (Amersham Pharmacia Biotech, Freiburg, Germany).
Immunohistochemistry
Immunohistochemistry was performed using a combination of pressure cooker heating and the standard streptavidin–biotin peroxidase complex using the goat IgG-Vectastain Elite ABC kit and rabbit IgG-Vectastain Elite ABC kit for the inhibin-βC and -βE subunits, respectively (both kits obtained from Vector Laboratories, Burlingame, CA, USA) as previously described [20] with slight modifications.
Briefly, paraffin-fixed tissue sections were dewaxed using xylol for 15 min and rehydrated in 100% of ethanol twice. Endogenous peroxidase activity was quenched by immersion in 3% hydrogen peroxide (Merck, Darmstadt, Germany) in methanol for 20 min. After washing, slides were subjected to antigen retrieval for 5 min in a pressure cooker using sodium citrate buffer (pH 6.0), containing 0.1 M citric acid and 0.1 M sodium citrate in distilled water. After cooling to room temperature, sections were washed twice in phosphate-buffered saline (PBS). Non-specific binding was blocked by incubating the sections with Ultra-V-Block (Lab Vision, Fremont, USA) for 45 min at room temperature. Sections were then incubated at 4°C over night with the inhibin-βC polyclonal goat antibody (R&D Systems, Wiesbaden, Germany) at a dilution of 1:50 in Ultra-V-Block (Lab Vision, Fremont, USA) or the inhibin-βE polyclonal rabbit antibody at a dilution of 1:4,000 in Ultra-V-Block (Lab Vision, Fremont, USA). After washing with PBS, sections were incubated with biotinylated secondary anti-rabbit antibody (provided by Vector Laboratories) for 30 min at room temperature. After incubation with the avidin–biotin peroxidase complex (diluted in 10 ml PBS; Vector Laboratories) for 30 min and repeated washing steps with PBS, visualization was performed with ABC substrate buffer (Vectastain Elite ABC kit, Vector Laboratories, Burlingame, CA, USA) and chromogen 3,3′-diaminobenzidine (DAB; Dako, Glostrup, Denmark) at 1 mg/ml concentration for 2 min. Sections were then counterstained with Mayer’s acidic hematoxylin and dehydrated in an ascending series of alcohol (50–98%). After xylol treatment, sections were mounted. Negative controls were performed by replacing the primary antibody with normal goat IgG or rabbit IgG as isotype control in the same dilution compared to the primary antibody, respectively. Immunohistochemical staining was performed using human liver tissue as an appropriate positive control. Positive cells showed a brownish color and negative controls as well as unstained cells were stained blue.
Cells and cell culture
The endometrial adenocarcinoma cell line Ishikawa has been established as a well-differentiated human endometrial adenocarcinoma cell line with estrogen receptor expression [21]. From this cell line (Ishikawa plus), several undifferentiated cell strains developed that lost estrogen receptor expression (Ishikawa minus) [21]. Cells were grown in Quantum 263 medium (PAA, Pasching, Austria) supplemented with antibiotics at 37°C in a humidified atmosphere with 5% CO2 as previously described [22].
Immunofluorescence analysis
Cells grown on glass cover slips were fixed with acetone for 10 min at room temperature and washed twice with PBS. Non-specific binding was blocked by incubating the sections with Ultra-V-Block (Lab Vision, Fremont, USA) for 15 min at room temperature. Thereafter, slides were incubated with inhibin-βC antibody (1:50 in dilution medium provided by DAKO, Glostrup, Denmark) or inhibin-βE antibody (1:2,000 in dilution medium provided by DAKO, Glostrup, Denmark) over night at 4°C, followed by a 1:500 diluted Cy3-conjugated donkey-anti-goat antibody (Dianova, Hamburg, Germany) for inhibin-βC or a 1:500 diluted Cy3-conjugated goat-anti-rabbit antibody (Dianova, Hamburg, Germany) for inhibin-βE, respectively. The slides were finally embedded in mounting buffer containing 4,6-diamino-2-phenylindole (DAPI) resulting in blue staining of the nuclei. Slides were embedded with Vectashield mounting medium (Axxora, Lörrach, Germany) and examined with a Zeiss (Jena, Germany) Axiophot photomicroscope. Digital images were obtained with a digital camera system (Axiocam, Zeiss) and saved on a computer.
RT-PCR analysis
RNA was extracted from cells using the Nucleospin RNA II kit (Macherey–Nagel, Düren, Germany). Reverse transcription was performed with M-MLV reverse transcriptase and oligo-dT (Promega, Mannheim, Germany) as recommended by the supplier. PCR was performed in an Eppendorf Mastercycler with GoTaq (Promega, Mannheim, Germany). PCR cycling was performed after a 5 min initiation at 94°C with 32 cycles of 1 min at 94°C, 1 min at 57°C, 2 min at 72°C, followed by a 5 min extension at 72°C. Primer sequences are listed in Table 1. Actin primers (661 bp amplification product) were from Stratagene, The Netherlands.
Results
Expression of inhibin-βC and -βE in normal human secretory endometrial tissue
To test the reactivity of the βC and βE subunit antibody, an evaluation of the immunohistochemical staining reaction was performed using appropriate positive controls including normal human liver specimens. A positive staining reaction for inhibin-βC and -βE expression could be demonstrated in normal human liver tissue (Fig. 1), confirming previous results [7, 20, 23]. In normal proliferative and secretory endometrial tissues, inhibin-βC and -βE was primarily detected in endometrial glandular epithelial cells, while immunostaining reaction in the stromal compartment was weaker (Fig. 2a–d). The staining intensity was slightly less intense in proliferative samples compared to secretory endometrial tissue (Fig. 2a–d).
Immunohistochemical staining reaction of inhibin-βC and -βE in normal liver tissue. The inhibin-βC subunit demonstrated a positive staining reaction in normal human liver tissue (a ×400). The inhibin-βE subunit also showed a positive staining reaction in normal human liver tissue, although with a lesser intensity compared to the βC subunit (b ×400)
Immunohistochemical staining reaction of inhibin-βC and -βE subunit in normal human secretory endometrial tissue. Proliferative endometrium demonstrated a positive immunohistochemical staining reaction against inhibin-βC (a ×250) and -βE (b ×250) antibodies. In normal secretory endometrial tissues, inhibin-βC (c ×400) and -βE (d ×400) was primarily detected in endometrial glandular epithelial cells, while the immunostaining reaction in the stromal compartment was weaker compared to the glandular epithelial cells
Expression of inhibin-βC and-βE in the human endometrial adenocarcinoma cell line Ishikawa
The endometrial adenocarcinoma cell line Ishikawa is a malignant cell line derived from invasive endometrial adenocarcinoma. We therefore tested the expression of inhibin-βC and -βE in this cell line, demonstrating an expression of both novel subunits at the protein level, being primarily in the cytoplasma (Fig. 3a, b). Interestingly, the Ishikawa minus cell line with no estrogen receptor expression demonstrated no to minimal expression of the βC subunit, whereas the inhibin-βE could also be demonstrated in this cell line (Fig. 3c, d).
Localization of inhibin-βC and -βE expression in endometrial Ishikawa cells. The endometrial adenocarcinoma cell line Ishikawa was analyzed by immunofluorescence for the expression of inhibin-βC and -βE, showing a positive cytoplasmic staining reaction for both subunits in Ishikawa plus cancer cells (a, b ×400). The labeling intensity appeared stronger in mitotic cells (arrows). Interestingly, the Ishikawa minus cell line, demonstrated no to minimal expression of the βC subunit, whereas the inhibin-βE could also be demonstrated in this cell line (c, d ×400)
RT-PCR analysis
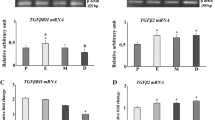
To analyze the inhibin-βC and -βE subunit expression at the transcriptional level, RNA was extracted from normal human endometrium and cells of the human endometrial cancer cell line Ishikawa, transcribed into cDNA, and analyzed by PCR analysis using specific primers. Figure 4a, b demonstrates that the mRNAs of the inhibin subunits βC and βE are expressed in Ishikawa cells. Interestingly, the Ishikawa minus cell line (with no estrogen receptor expression) demonstrated no to minimal expression of the βC subunit mRNA, whereas the inhibin-βE could also be demonstrated in this cell line (Fig. 4b).
Inhibin-βC and -βE mRNA expression in the endometrium and endometrial Ishikawa cells. Normal human endometrium (a) and the endometrial adenocarcinoma cell line Ishikawa were analyzed by RT-PCR analysis for the expression of the inhibin-βC and -βE subunits (b). The used marker was pBR328 (Carl Roth, Karlsruhe)
Discussion
Inhibins and activins were initially characterized as endocrine and paracrine hormonal regulators of the hypothalamic-pituitary–gonadal axis. Meanwhile, it is clear that they are expressed in a wide range of female reproductive tissues including normal and pathological human endometrium [11–14, 16, 19, 24]. In this preliminary study, we have demonstrated an immunohistochemical staining reaction of the novel subunits inhibin/activin-βC and -βE subunits in normal human endometrium and the human endometrial carcinoma cell line Ishikawa using RT-PCR and immunohistochemical detection methods.
Although the precise physiologic roles of endometrial inhibins/activins are still unclear, possible functions in stem cell biology [25] and reproductive biology by influencing ovarian and placental hormone secretion [2, 26] have been suggested. Additionally, they seem to have important roles in endometrial decidualization [27], trophoblast differentiation [28], immunomodulary function [29, 30], systemic inflammation [31, 32], endometrial repair [33] and apoptosis [34].
The inhibin/activin-βC subunit was demonstrated to be predominantly expressed in hepatocytes [4, 9], prostate, ovary, testes and pituitary [10, 35]. Although the precise role of this subunit is still not elucidated yet, several possible functions have been suggested, including apoptosis [36, 37] and increasing the rate of DNA synthesis in primary rat hepatocytes [38], leading to mitosis in a subset of hepatocytes [35]. Moreover, it was demonstrated that activin C (βC–βC) does not activate activin A (βA–βA)-responsive promoters, suggesting a regulative role of the βC subunit to the levels of bioactive activin A (βA–βA) through the formation of signaling incompetent activin AC heterodimers [39–41]. Therefore, βC-subunit might function as an antagonist of activin function [10, 39]. Moreover, human testis, liver and prostate cancers also synthesize this βC subunit, suggesting a possible role in the pathogenesis and carcinogenesis of these cancers [41]. If these functions are also applicable in normal or malignant endometrial tissue still remains to be clarified.
The βE subunit is also predominantly expressed in hepatocytes [7, 37]. Interestingly, inhibin/activins-βE mRNA expression was transiently up-regulated after partial hepatectomy or portal vein branch ligation [23, 42]. When ectopically expressed in HepG2 or Hep3B hepatoma cells or in the murine hepatocyte cell line AML12, activin βE reduced the cell number and increased apoptosis rates [37, 38]. Moreover, transient overexpression of βE by non-viral gene transfer in the mouse liver inhibited regenerative DNA synthesis [36]. These observations suggest that activin E may have a growth-limiting function similar to activin A [43]. However, the apoptotic function of the βE subunit is also still unclear in human endometrial tissue. Moreover, the function of this novel subunit and the formation of putative inhibins and/or activins are still unclear and warrant further research.
In conclusion, we have demonstrated an immunohistochemical staining reaction of the novel subunits inhibin-βC and -βE subunits in normal human endometrium and the human endometrial carcinoma cell line Ishikawa using RT-PCR and immunohistochemical detection methods. Interestingly, the Ishikawa minus cell line (laking estrogen receptor expression) demonstrated no to minimal expression of the βC subunit as observed with immunofluorescence and RT-PCR, suggesting a possible hormone-dependent dependency of this subunit in human endometrial cancer cells. Moreover, because the Ishikawa cell line minus is thought to be a more malignant endometrial cell line than its estrogen receptor positive counterpart [21], inhibin-βC subunit might be substantially involved in the pathogenesis and malignant transformation in human endometrium.
References
Vale W, Rivier C, Hsueh A, Campen C, Meunier H, Bicsak T, Vaughan J, Corrigan A, Bardin W, Sawchenko P et al (1988) Chemical and biological characterization of the inhibin family of protein hormones. Recent Prog Horm Res 44:1–34
de Kretser DM, Hedger MP, Loveland KL, Phillips DJ (2002) Inhibins, activins and follistatin in reproduction. Hum Reprod Update 8:529–541
Xia Y, Schneyer AL (2009) The biology of activin: recent advances in structure, regulation and function. J Endocrinol 202:1–12
Hötten G, Neidhardt H, Schneider C, Pohl J (1995) Cloning of a new member of the TGF-beta family: a putative new activin beta C chain. Biochem Biophys Res Commun 206:608–613
Oda S, Nishimatsu S, Murakami K, Ueno N (1995) Molecular cloning and functional analysis of a new activin beta subunit: a dorsal mesoderm-inducing activity in Xenopus. Biochem Biophys Res Commun 210:581–588
Fang J, Yin W, Smiley E, Wang SQ, Bonadio J (1996) Molecular cloning of the mouse activin beta E subunit gene. Biochem Biophys Res Commun 228:669–674
Hashimoto O, Tsuchida K, Ushiro Y, Hosoi Y, Hoshi N, Sugino H, Hasegawa Y (2002) cDNA cloning and expression of human activin betaE subunit. Mol Cell Endocrinol 194:117–122
Fang J, Wang SQ, Smiley E, Bonadio J (1997) Genes coding for mouse activin beta C and beta E are closely linked and exhibit a liver-specific expression pattern in adult tissues. Biochem Biophys Res Commun 231:655–661
Vejda S, Cranfield M, Peter B, Mellor SL, Groome N, Schulte-Hermann R, Rossmanith W (2002) Expression and dimerization of the rat activin subunits betaC and betaE: evidence for the formation of novel activin dimers. J Mol Endocrinol 28:137–148
Mellor SL, Cranfield M, Ries R, Pedersen J, Cancilla B, de Kretser D, Groome NP, Mason AJ, Risbridger GP (2000) Localization of activin beta(A)-, beta(B)-, and beta(C)-subunits in humanprostate and evidence for formation of new activin heterodimers of beta(C)-subunit. J Clin Endocrinol Metab 85:4851–4858
Leung PH, Salamonsen LA, Findlay JK (1998) Immunolocalization of inhibin and activin subunits in human endometrium across the menstrual cycle. Hum Reprod 13:3469–3477
Petraglia F, Florio P, Luisi S, Gallo R, Gadducci A, Vigano P, Di Blasio AM, Genazzani AR, Vale W (1998) Expression and secretion of inhibin and activin in normal and neoplastic uterine tissues. High levels of serum activin A in women with endometrial and cervical carcinoma. J Clin Endocrinol Metab 83:1194–1200
Mylonas I, Jeschke U, Winkler L, Makovitzky J, Richter DU, Briese V, Friese K (2003) Immunohistochemical expression of inhibin-alpha in human endometrium and the in vitro secretion of inhibin, estradiol and cortisol in cultured human endometrial glandular cells. Arch Gynecol Obstet 268:142–150
Mylonas I, Makovitzky J, Fernow A, Richter DU, Jeschke U, Briese V, Gerber B, Friese K (2005) Expression of the inhibin/activin subunits alpha (alpha), beta-A (betaA) and beta-B (betaB) in benign human endometrial polyps and tamoxifen-associated polyps. Arch Gynecol Obstet 272:59–66
Mylonas I, Jeschke U, Wiest I, Hoeing A, Vogl J, Shabani N, Kuhn C, Schulze S, Kupka MS, Friese K (2004) Inhibin/activin subunits alpha, beta-A and beta-B are differentially expressed in normal human endometrium throughout the menstrual cycle. Histochem Cell Biol 122:461–471
Worbs S, Shabani N, Mayr D, Gingelmaier A, Makrigiannakis A, Kuhn C, Jeschke U, Kupka MS, Friese K, Mylonas I (2007) Expression of the inhibin/activin subunits (-alpha, -betaA and -betaB) in normal and carcinogenic endometrial tissue: Possible immunohistochemical differentiation markers. Oncol Rep 17:97–104
Jones RL, Findlay JK, Salamonsen LA (2006) The role of activins during decidualisation of human endometrium. Aust N Z J Obstet Gynaecol 46:245–249
Risbridger GP, Schmitt JF, Robertson DM (2001) Activins and inhibins in endocrine and other tumors. Endocr Rev 22:836–858
Mylonas I, Worbs S, Shabani N, Kuhn C, Kunze S, Schulze S, Dian D, Gingelmaier A, Schindlbeck C, Bruning A, Sommer H, Jeschke U, Friese K (2009) Inhibin-alpha subunit is an independent prognostic parameter in human endometrial carcinomas: Analysis of inhibin/activin-alpha, -betaA and -betaB subunits in 302 cases. Eur J Cancer 45:1304–1314
Mylonas I, Makovitzky J, Shabani N, Gingelmaier A, Dian D, Kuhn C, Schulze S, Kunze S, Jeschke U, Friese K (2009) Development and characterisation of an antibody for the immunohistochemical detection of inhibin/activin betaE (betaE) in normal human ovarian and placental tissue. Acta Histochem 111:366–371
Nishida M (2002) The Ishikawa cells from birth to the present. Hum Cell 15:104–117
Brüning A, Makovitzky J, Gingelmaier A, Friese K, Mylonas I (2009) The metastasis-associated genes MTA1 and MTA3 are abundantly expressed in human placenta and chorionic carcinoma cells. Histochem Cell Biol 132:33–38
Lau AL, Kumar TR, Nishimori K, Bonadio J, Matzuk MM (2000) Activin betaC and betaE genes are not essential for mouse liver growth, differentiation, and regeneration. Mol Cell Biol 20:6127–6137
Mylonas I, Makovitzky J, Hoeing A, Richter DU, Vogl J, Schulze S, Jeschke U, Briese V, Friese K (2006) Inhibin/activin subunits beta-A (-betaA) and beta-B (-betaB) are differentially localised in normal, hyperplastic and malignant human endometrial tissue. Acta Histochem 108:1–11
Beattie GM, Lopez AD, Bucay N, Hinton A, Firpo MT, King CC, Hayek A (2005) Activin A maintains pluripotency of human embryonic stem cells in the absence of feeder layers. Stem Cells 23:489–495
Welt CK (2002) The physiology and pathophysiology of inhibin, activin and follistatin in female reproduction. Curr Opin Obstet Gynecol 14:317–323
Jones RL, Salamonsen LA, Findlay JK (2002) Activin A promotes human endometrial stromal cell decidualization in vitro. J Clin Endocrinol Metab 87:4001–4004
Caniggia I, Lye SJ, Cross JC (1997) Activin is a local regulator of human cytotrophoblast cell differentiation. Endocrinology 138:3976–3986
Keelan JA, Zhou RL, Mitchell MD (2000) Activin A exerts both pro- and anti-inflammatory effects on human term gestational tissues. Placenta 21:38–43
Robson NC, Wei H, McAlpine T, Kirkpatrick N, Cebon J, Maraskovsky E (2009) Activin-A attenuates several human natural killer cell functions. Blood 113:3218–3225
Jones KL, de Kretser DM, Patella S, Phillips DJ (2004) Activin A and follistatin in systemic inflammation. Mol Cell Endocrinol 225:119–125
Phillips DJ, de Kretser DM, Hedger MP (2009) Activin and related proteins in inflammation: not just interested bystanders. Cytokine Growth Factor Rev 20:153–164
Kaitu’u-Lino TJ, Phillips DJ, Morison NB, Salamonsen LA (2009) A new role for activin in endometrial repair after menses. Endocrinology 150:1904–1911
Chen YG, Lui HM, Lin SL, Lee JM, Ying SY (2002) Regulation of cell proliferation, apoptosis, and carcinogenesis by activin. Exp Biol Med (Maywood) 227:75–87
Gold EJ, Zhang X, Wheatley AM, Mellor SL, Cranfield M, Risbridger GP, Groome NP, Fleming JS (2005) BetaA- and betaC-activin, follistatin, activin receptor mRNA and betaC-activin peptide expression during rat liver regeneration. J Mol Endocrinol 34:505–515
Chabicovsky M, Herkner K, Rossmanith W (2003) Overexpression of activin beta(C) or activin beta(E) in the mouse liver inhibits regenerative deoxyribonucleic acid synthesis of hepatic cells. Endocrinology 144:3497–3504
Vejda S, Erlach N, Peter B, Drucker C, Rossmanith W, Pohl J, Schulte-Hermann R, Grusch M (2003) Expression of activins C and E induces apoptosis in human and rat hepatoma cells. Carcinogenesis 24:1801–1809
Wada W, Medina JJ, Kuwano H, Kojima I (2005) Comparison of the function of the beta(C) and beta(E) subunits of activin in AML12 hepatocytes. Endocr J 52:169–175
Mellor SL, Ball EM, O’Connor AE, Ethier JF, Cranfield M, Schmitt JF, Phillips DJ, Groome NP, Risbridger GP (2003) Activin betaC-subunit heterodimers provide a new mechanism of regulating activin levels in the prostate. Endocrinology 144:4410–4419
Butler CM, Gold EJ, Risbridger GP (2005) Should activin betaC be more than a fading snapshot in the activin/TGFbeta family album? Cytokine Growth Factor Rev 16:377–385
Gold E, Jetly N, O’Bryan MK, Meachem S, Srinivasan D, Behuria S, Sanchez-Partida LG, Woodruff T, Hedwards S, Wang H, McDougall H, Casey V, Niranjan B, Patella S, Risbridger G (2009) Activin C antagonizes activin A in vitro and overexpression leads to pathologies in vivo. Am J Pathol 174:184–195
Takamura K, Tsuchida K, Miyake H, Tashiro S, Sugino H (2005) Activin and activin receptor expression changes in liver regeneration in rat. J Surg Res 126:3–11
Rodgarkia-Dara C, Vejda S, Erlach N, Losert A, Bursch W, Berger W, Schulte-Hermann R, Grusch M (2006) The activin axis in liver biology and disease. Mutat Res 613:123–137
Acknowledgments
We would like to thank Mrs. I. Krienke, Mrs. S. Kunze, Mrs S. Schulze, Mrs. S. Hoffmann and Mrs. I. Wiest for their excellent work with endometrial samples.
Conflict of interest statement
None.
Author information
Authors and Affiliations
Corresponding author
Additional information
T. Kimmich and A. Brüning contributed equally to this manuscript.
Rights and permissions
About this article
Cite this article
Kimmich, T., Brüning, A., Käufl, S.D. et al. Inhibin/activin-betaC and -betaE subunits in the Ishikawa human endometrial adenocarcinoma cell line. Arch Gynecol Obstet 282, 185–191 (2010). https://doi.org/10.1007/s00404-009-1310-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-009-1310-y