Abstract
Background
The choice of appropriate therapeutic plans for primary endocervical adenocarcinomas (ECA) and endometrial adenocarcinomas (EMA) depends on the tumor’s site of origin. Some panels of antibodies help to distinguish primary ECA from EMA. However, unexpected expressions of those markers often exist, which causes this diagnostic dilemma to be still unresolved. In this study, we investigate five commonly used monoclonal antibodies (p53, TTF1, CK7, CK20, and CK34βE12) to evaluate their potential use in distinguishing between these two gynecologic malignancies.
Methods
A tissue microarray was constructed using paraffin-embedded, formalin-fixed tissues from 35 hysterectomy specimens, including 14 ECA and 21 EMA. Utilizing the avidin–biotin (ABC) technique, tissue array sections were immunostained with the five aforementioned commercially available antibodies.
Results
Immunohistochemical (IHC) expressions of p53, TTF1, CK7, CK20, and CK34βE12 were all nonsignificant (P > 0.05) in frequency differences between the immunostaining results (positive vs. negative) in tumors from both the two primary adenocarcinomas (ECA vs. EMA).
Conclusion
It is still uncertain which markers or panels would be the most appropriate for making diagnoses; hence, exploration of other useful markers, which make a definitive distinction between ECA and EMA merits further studies. This study, however, uncovered that the five commonly used monoclonal antibodies (p53, TTF1, CK7, CK20, and CK34βE12) are of no beneficial value in distinguishing between primary ECA and EMA.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background
Although careful morphologic examination usually allows for a confident diagnosis, the distinction between primary ECA and EMA may be difficult with small biopsied or curetted tissue specimens, based on hematoxylin and eosin (H&E) staining. It is important to ascertain the site of origin of these cancers, since the treatment plans may differ substantially [1, 2].
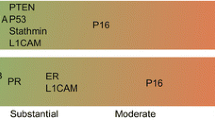
In our previous report, we discovered that five specific markers, including PR, ER, Vim, CEA and p16INK4a and their respective panels, are helpful in distinguishing between these two gynecologic malignancies (ECA vs. EMA) [3–5]. However, unexpected aberrant expressions of these markers often occurred which were not characteristic of either primary site [3, 4, 6–10]. Therefore, it is still worthwhile to identify other novel discriminating markers for the differential diagnosis between ECA and EMA. In this extension study, we explore five other markers, including p53, TTF1, CK7, CK20, and CK34βE12, that may possibly assist in distinguishing between these two gynecologic malignancies. These five markers are commonly used to help make an accurate diagnosis of many other kinds of tumors in pathological examinations. Our rationale for using these markers as possible candidates for distinguishing between ECA and EMA are summarized as follows: (1) after reviewing the literatures on PubMed, we found that p53 expression only correlates significantly with status differentiation in EMA but not in ECA [11, 12]; (2) TTF-1 immunoreactivity has been reported in tumors other than those originating in the lung or the thyroid, and the occasional expression of this marker has been found in many major histologic subtypes of gynecologic tumors [13]; (3) the differential expression patterns of CK7 and CK20 have been widely used in the discrimination between different origins of specific adenocarcinomas, such as colon versus lung, as well as colon versus ovary. Owing to the existing limiting factor of the overlap in staining positivity, CK 7 and CK 20 have been reported to be of no use in discriminating primary ECA from EMA in only a small number of cases [7, 9, 14]; and (4) CK34betaE12, which reacts with cytokeratins 1, 5, 10, and 14, has diagnostic utility for prostatic adenocarcinomas. However, its pathologic significance in ECA and EMA has not been systematically studied.
However, it was still interesting for us. In the current extension study, our aim was to reappraise the expression of these five commonly used markers in order to view their potential diagnostic values in distinguishing between doubtful cases of these two gynecologic malignancies (ECA vs. EMA) by means of tissue microarray (TMA) and immunohistochemistry (IHC) in Taiwanese women.
Methods
Study materials
The study material consisted of slides and selected formalin-fixed, paraffin-embedded tissue blocks from 35 hysterectomy specimens retrieved from the archives of the Tissue Bank of the Clinical Trial Center at Chung-Shan Medical University Hospital. These endocervical or endometrial specimens were accessioned between 2004 and 2008. The cases studied included endometrioid type endometrial adenocarcinomas (n = 21) as well as endocervical type endocervical adenocarcinomas (n = 14). Two board-certified pathologists (C.-P. Han and L.-F. Kok) carefully reviewed all the H&E stained slides for these cases. A slide with a representative tumor was selected from each case, and the tumor area of interest was circled. In the next step, the area corresponding to the selected area on the slide was also circled on the block with an oil marker. All of the donors’ tissue blocks were sent to Bio-Chiefdom International Co. Ltd, Taiwan for TMA slide construction. They were cored with a 1.5-mm diameter needle and transferred to a recipient paraffin block. The recipient block was sectioned at 5 μm, and transferred to silanized glass slides.
Immunohistochemical staining
Using the avidin–biotin complex (ABC) technique, slides were stained with monoclonal antibodies, whose main characteristics are summarized in Table 1. Briefly, formalin-fixed and paraffin-embedded tissue array specimens with 1.5-mm, 5 μm individual cores were deparaffinized in xylene, rehydrated through serial dilutions of alcohol and washed in PBS (pH 7.2), the buffer which was used for all subsequent washes. Slides were stained with the following monoclonal antibodies: 1:100 dilution; p53 (NCL-p53-DO7, Leica Microsystems), 1:100 dilution; TTF1 (NCL-TTF-1 SPT24, Leica Microsystems), 1:100 dilution; CK7 (NCL-L-CK7-560, Leica Microsystems), 1:100 dilution; CK20 (NCL-L-CK20-561, Leica Microsystems), 1:200 dilution; CK34ßE12 (NCL-CK34BE12, Leica Microsystems), prediluted, low pH antigen retrieval (Table 1). Negative controls were obtained by leaving out the primary antibody. Appropriate positive controls were performed. These slides were mounted with gum for examination, and images were captured by the Olympus BX51 microscopic/DP71 Digital Camera System for study comparison (Table 2).
Scoring of immunostaining
In this study, the tissue microarray (TMA) slides were simultaneously reviewed and scored in agreement by the aforementioned pathologists, using the Olympus BX51 two-headed microscope. Despite numerous scoring methods found in literature, both nucleic and cytoplasmic IHC scoring algorithms have not yet been optimized and standardized. Some computer-based programs have been specifically designed for the quantitative analysis of IHC. However, the accuracy of computer-based programs has not significantly improved clinical outcome measures compared with the conventional analysis by pathologists [15–18]. As a result, we interpreted the expressions of p53, TTF1, CK7, CK20, and CK34βE12 by using the German semi-quantitative scoring system in considering the staining intensity and area extent. The intensity of marker expression was quantified using the following scores: 0 = negative, 1 = weakly positive, 2 = moderately positive, 3 = strongly positive. The extent of marker expression was quantified by evaluating the percentage of the positive staining areas in relation to the whole cancer area in the core, where a score of 0 points was given for 0% reactivity, 1 point was assigned for 1–10% reactivity, 2 points were assigned for 11–50% reactivity, 3 points were given for 51–80% reactivity, and 4 points were given for 81–100% reactivity. The final immunoreactive score was determined by multiplying the intensity of positivity and the area extent of positivity scores, yielding a range from 0 to 12. The threshold for differentiating between final positive and negative immunostaining was set at 4 for interpretation. In this study, this optimal cut-off value was determined by using receiver operating characteristic (ROC) curve analysis [19, 20]. The scoring results can be expressed by dividing cases into scores of 0–3 (essentially negative) and 4–12 (at least moderately positive in at least 11–50% of cells). This method of assessment has been widely accepted and used in previous studies [3–9, 21–25].
Statistical analysis
A Chi-square or Fisher’s exact test was performed to test the frequency difference of immunostaining (positive vs. negative) between each immunohistochemical biomarker and the two groups of adenocarcinomas (ECA vs. EMA), where a negative staining was classified as having an immunostaining score of 0–3, and a positive staining was classified as having an immunostaining score of 4–12. The Mann–Whitney U test, a nonparametric analysis technique, was used to test the immunostaining raw scores between the two adenocarcinomas, given the fact that the analytical IHC scores were not normally distributed. All analyses were performed using SPSS statistical software (SPSS, Inc., Chicago, IL, USA). All tests were two-sided and the significance level was 0.05.
Results
We have already reported that five immunomarkers (ER, PR, Vim, CEA, and p16INK4a) showed significant frequency differences between ECA and EMA tissue immunostaining (P < 0.05) [3–5]. In this extension study, H&E and immunoreactivities for p53, TTF1, CK7, CK20, and CK34βE12 in representative cases of ECA and EMA are identified in Fig. 1. Using a score of ≧4 points as a cutoff, the IHC scores were expressed by dividing cases into scores of 0–3 (negative) and 4–12 (positive). All of the markers p53, TTF1, CK7, CK20, and CK34βE12 showed nonsignificant frequency differences in ECA and EMA tissue immunostains (P > 0.05). The IHC staining results for these five markers are presented as follows: (1) The p53-marker stained positive in 5 out of 14 (35.7%) ECA tumors with a median staining score of 1.50 and a range of 0–6. The p53-marker stained positive in 9 out of 21 (42.9%) EMA tumors (P = 0.673) with a median staining score of 3.00 and a range of 0–12 (P = 0.182). (2) The TTF1-marker stained positive in 1 out of 14 (7.1%) ECA tumors with a median staining score of 0.00 and a range of 0–4. The TTF1-marker stained positive in 2 out of 21 (9.5%) EMA tumors (P = 1.000) with a median staining score of 0.00 and a range of 0–6 (P = 0.720). (3) The CK7-marker stained positive in 14 out of 14 (100%) ECA tumors with a median staining score of 8.00 and a range of 4–12. The CK7-marker stained positive in 21 out of 21 (100%) EMA tumors (P > 0.05) with a median staining score of 8.50 and a range of 4–12 (P = 0.537). (4) The CK20-marker stained positive in 0 out of 14 (0%) ECA tumors with a median staining score of 0.00 and a range of 0–2. The CK20-marker stained positive in 1 out of 21 (4.8%) EMA tumors (P = 1.000) with a median staining score of 0.00 and a range of 0–6 (P = 0.491). (5) The CK34βE12-marker stained positive in 6 out of 14 (42.9%) ECA tumors with a median staining score of 2.00 and a range of 0–12. The CK20-marker stained positive in 8 out of 21 (38.1%) EMA tumors (P = 1.000), with a median staining score of 2.50 and a range of 0–6 (P = 0.535).
H&E and immunohistochemical stains for p53, TTF1, CK7, CK20, and CK34βE12 identified in ECA and EMA. a1 H&E stain of endocervical type endocervical adenocarcinoma. a2 H&E stain of endometrioid type endometrial adenocarcinoma. b1 A representative case of ECA showing a positive p53 IHC result, which was determined by multiplying the intensity of 2 points and the extent of 3 points, yielding a final score of 6. b2 A representative case of EMA showing a positive p53 IHC result, which was determined by multiplying the intensity of 3 points and the extent of 2 points, yielding a final score of 6. c1 A representative case of ECA showing a positive TTF1 IHC result, which was determined by multiplying the intensity of 2 points and the extent of 2 points, yielding a final score of 4. c2 A representative case of EMA showing a positive TTF1 IHC result, which was determined by multiplying the intensity of 3 points and the extent of 2 points, yielding a final score of 6. d1 A representative case of ECA showing a positive CK7 IHC result, which was determined by multiplying the intensity of 2 points and the extent of 4 points, yielding a final score of 8. d2 A representative case of EMA showing a positive CK7 IHC result, which was determined by multiplying the intensity of 3 points and the extent of 4 points, yielding a final score of 12. e1 A representative case of ECA showing a negative CK20 IHC result, which was determined by multiplying the intensity of 0 points and the extent of 0 points, yielding a final score of 0. e2 A representative case of EMA showing a positive CK20 IHC result, which was determined by multiplying the intensity of 3 points and the extent of 2 points, yielding a final score of 6. f1 A representative case of ECA showing a positive CK34βE12 IHC result, which was determined by multiplying the intensity of 3 points and the extent of 4 points, yielding a final score of 12. f2 A representative case of EMA showing a positive CK34βE12 IHC result, which was determined by multiplying the intensity of 3 points and the extent of 2 points, yielding a final score of 6. All photomicrographs including a1–f2 were taken with medium-powered fields, ×200
Discussion
Distinguishing between ECA and EMA before planning the patient treatment is clinically important. When there is doubt and indistinguishable primaries, immunohistochemistry (IHC) may be of assistance. However, IHC should always be interpreted along with the gross and microscopic histomorphology. In general, panels of antibodies should be used rather than relying on a single antibody, as there is no single antibody that is totally specific for any one neoplasm [3–9, 21–25]. McCluggage et al. [8] proposed that the conventional 3-marker IHC panel (ER, Vim and CEA) generally allows confident preoperative distinction between a primary endometrial and endocervical adenocarcinoma [8]. We also reported previously that the five immunomarkers (ER, PR, Vim, CEA, and p16INK4a) show significant frequency differences (P < 0.05), and the p16INK4a-marker does not add value to the 4-marker panel (ER, Vim, CEA, and PR) performance in distinguishing between primary ECA and EMA [3–5]. However, immunoprofiles are not always definitive in all cases, and a result overlap may exist. Unexpected “aberrant” expressions can often occur, which causes this diagnostic dilemma to be still unresolved [3, 4, 6–9, 14, 21–25].
ECA and EMA have not been studied in large numbers for the possible application of the five monoclonal antibodies directed against p53, TTF1, CK7, CK20, and CK34βE12. In this extension study, we evaluated these five commonly used markers for their possible use in the distinction between these two gynecologic cancers (ECA vs. EMA) by means of TMA and IHC techniques in Taiwanese women. As there is limited information in literature, our negative results and findings can still be helpful in the referral and management of such cases worldwide for the following reasons: (1) The role of p53 in EMA has been investigated extensively, and many studies have reported a significant survival disadvantage in patients, whose tumors demonstrate p53 over-expression [11, 12, 26]. Staining for p53 seems to offer additional prognostic information for EMA but not so in ECA. Based on our data, p53 was positive in 5 out of 14 ECA and 9 out of 21 EMA. The data for p53 expression did not show a significant frequency difference between ECA and EMA (P > 0.05). (2) Thyroid transcription factor-1 (TTF-1) has been widely used as a relatively specific marker for the diagnosis of lung and thyroid carcinomas, but there have been reports of TTF-1 immunoreactivity in tumors other than those originating in the lung or thyroid. Based on our data, TTF1 was essentially negative in the majority of EMA (19/21) and ECA (13/14) cases, except for 1 out of 14 (7.1%) ECA and 2 out of 21 (9.5%) EMA were positive. Although the data do not show a significant frequency difference between ECA and EMA (P > 0.05), the occasional expression of TTF-1 in both gynecologic tumors should be kept in mind when evaluating neoplasms of uncertain origin. This immunostaining may also lead to an erroneous interpretation or conclusion of an ECA or EMA lesion to be a primary lung cancer metastasis. On the other hand, the evaluation of adenocarcinomas involving the lung in patients with a history of a gynecologic malignancy should also take this immunostaining into consideration [13, 27–29]. (3) It is known that staining for CK7 and CK20 can aid in differentiating between primary endometrial or endocervical adenocarcinomas from secondary adenocarcinomas of colorectal origin [7, 9, 14, 30]. Based on our data, CK7 was positive in all 14 (100%) ECA and in 21 (100%) EMA cases, and CK20 was positive in 0 out of 14 (0%) ECA cases and 1 out of 21 (4.8%) EMA cases, which displayed a positive score of 6 points. The expression status of both CK7 and CK20 did not show significant frequency differences between ECA and EMA (P > 0.05). Our results also exhibited a reproducibility of the same differential expression of the CK7+/CK20− immunophenotype as that of other female genital tract tumors. (4) The NCL-CK34βE12 marker is intended for the qualitative identification of human high molecular weight cytokeratins 1, 5, 10, and 14. It has often been used to stain basal cells in prostatic glands, while the loss of basal cells is a characteristic diagnostic criterion for a prostate adenocarcinoma. It can also be used to differentiate in situ cancers of the breast. Lobular carcinoma in situ (LCIS) exhibits perinuclear staining with CK34βE12. Ductal carcinoma in situ (DCIS) does not stain for CK34βE12 [29, 31]. Based on our data, CK34βE12 was positive in 6 out of 14 (42.9%) ECA and 8 out of 21 (38.1%) EMA. CK34βE12 expression did not show a significant frequency difference between ECA and EMA (P > 0.05).
In summary, for all the antibodies tested (such as p53, TTF1, CK7, CK20, and CK34βE12) in this extension study, there was no significant difference in immunostaining between cervical and endometrial adenocarcinomas. However, it is still uncertain which markers or panels would be more appropriate in practice; hence, investigating other useful markers that will help to make a definitive distinction between these two gynecologic malignancies (ECA vs. EMA) still merits further study.
Conclusion
According to our data, when histomorphological and clinical doubt exists as to the primary site of origin, appropriate panels of antibodies can help to make an accurate diagnosis. In spite of the limited number of cases, the negative findings of this extension study still provide a valuable reference and encourage us to further investigate other markers and panels for making a definitive diagnostic distinction between primary ECA and EMA.
References
Lurain JR, Bidus MA, Elkas JC (2007) Uterine cancer, cervical and vaginal cancer. In: Berek RS (ed) Novak’s gynecology, 14th edn. Lippincott Williams & Wilkins (LWW), Philadelphia, pp 1343–1402
Schorge JO, Knowles LM, Lea JS (2004) Adenocarcinoma of the cervix. Curr Treat Options Oncol 5:119–127
Yao CC, Kok LF, Lee MY, Wang PH, Wu TS, Tyan YS et al (2009) Ancillary p16(INK4a) adds no meaningful value to the performance of ER/PR/Vim/CEA panel in distinguishing between primary endocervical and endometrial adenocarcinomas in a tissue microarray study. Arch Gynecol Obstet [Epub ahead of print]
Han CP, Lee MY, Kok LF, Ruan A, Wu TS, Cheng YW et al (2009) Aditional 3-marker (ER/Vim/CEA) panel engenders no supplemental benefit in distinguishing between primary endocervical and endometrial adenocarcinomas in a tissue microarray study. Int J Gynecol Pathol (in publication)
Han CP, Kok LF, Wang PH, Wu TS, Tyan YS, Cheng YW, Lee MY, Yang SF (2009) Scoring of p16(INK4a) immunohistochemistry based on independent nuclear staining alone can sufficiently distinguish between endocervical and endometrial adenocarcinomas in a tissue microarray study. Mod Pathol [Epub ahead of print]
Dabbs DJ, Sturtz K, Zaino RJ (1996) Distinguishing endometrial from endocervical adenocarcinoma. Hum Pathol 27:172–177
Castrillon DH, Lee KR, Nucci MR (2002) Distinction between endometrial and endocervical adenocarcinoma: an immunohistochemical study. Int J Gynecol Pathol 21:4–10
McCluggage WG, Sumathi VP, McBride HA, Patterson A (2002) A panel of immunohistochemical stains, including carcinoembryonic antigen, vimentin, and estrogen receptor, aids the distinction between primary endometrial and endocervical adenocarcinomas. Int J Gynecol Pathol 21:11–15
Alkushi A, Irving J, Hsu F, Dupuis B, Liu CL, Rijn M, Gilks CB (2003) Immunoprofile of cervical and endometrial adenocarcinomas using a tissue microarray. Virchows Arch 442:271–277
Wehling M (2008) Translational medicine: science or wishful thinking? J Transl Med 6:31
McHugh M (1995) P53 expression in endocervical and endometrial adenocarcinomas. Int J Surg Pathol 2:269–273
McCluggage G, McBride H, Maxwell P, Bharucha H (1997) Immunohistochemical detection of p53 and bcl-2 proteins in neoplastic and non-neoplastic endocervical glandular lesions. Int J Gynecol Pathol 16:22–27
Siami K, McCluggage WG, Ordonez NG, Euscher ED, Malpica A, Sneige N, Silva EG, Deavers MT (2007) Thyroid transcription factor-1 expression in endometrial and endocervical adenocarcinomas. Am J Surg Pathol 31:1759–1763
Park KJ, Bramlage MP, Ellenson LH, Pirog EC (2009) Immunoprofile of adenocarcinomas of the endometrium, endocervix, and ovary with mucinous differentiation. Appl Immunohistochem Mol Morphol 17:8–11
Remmele W, Schicketanz KH (1993) Immunohistochemical determination of estrogen and progesterone receptor content in human breast cancer. Computer-assisted image analysis (QIC score) vs. subjective grading (IRS). Pathol Res Pract 189:862–866
Matos LL, Stabenow E, Tavares MR, Ferraz AR, Capelozzi VL, Pinhal MA (2006) Immunohistochemistry quantification by a digital computer-assisted method compared to semiquantitative analysis. Clinics 61:417–424
Camp RL, Chung GG, Rimm DL (2002) Automated subcellular localization and quantification of protein expression in tissue microarrays. Nat Med 8:1323–1327
Cregger M, Berger AJ, Rimm DL (2006) Immunohistochemistry and quantitative analysis of protein expression. Arch Pathol Lab Med 130:1026–1030
Zweig MH, Campbell G (1993) Receiver-operating characteristic (ROC) plots: a fundamental evaluation tool in clinical medicine. Clin Chem 39:561–577
Metz CE (1978) Basic principles of ROC analysis. Semin Nucl Med 8:283–298
Han CP, Lee MY, Tzeng SL, Yao CC, Wang PH, Cheng YW, Chen SL, Wu TS, Tyan YS, Kok LF (2008) Nuclear Receptor Interaction Protein (NRIP) expression assay using human tissue microarray and immunohistochemistry technology confirming nuclear localization. J Exp Clin Cancer Res 27:25
Koo CL, Kok LF, Lee MY, Wu TS, Cheng YW, Hsu JD, Ruan A, Chao KC, Han CP (2009) Scoring mechanisms of p16INK4a immunohistochemistry based on either independent nucleic stain or mixed cytoplasmic with nucleic expression can significantly signal to distinguish between endocervical and endometrial adenocarcinomas in a tissue microarray study. J Transl Med 7:25
Kamoi S, AlJuboury MI, Akin MR, Silverberg SG (2002) Immunohistochemical staining in the distinction between primary endometrial and endocervical adenocarcinomas: another viewpoint. Int J Gynecol Pathol 21:217–223
Khoury T, Tan D, Wang J, Intengan M, Yang J, Alrawi S, Yan P, Byrd JC (2006) Inclusion of MUC1 (Ma695) in a panel of immunohistochemical markers is useful for distinguishing between endocervical and endometrial mucinous adenocarcinoma. BMC Clin Pathol 6:1
Reid-Nicholson M, Iyengar P, Hummer AJ, Linkov I, Asher M, Soslow RA (2006) Immunophenotypic diversity of endometrial adenocarcinomas: implications for differential diagnosis. Mod Pathol 19:1091–1100
Vallmanya Llena FR, Laborda Rodríguez A, Lloreta Trull J, Cortadellas Angel R, Placer Santos J, Mas Gelabert A (2006) Immunohistochemical expression of p53, p21, p16, and cyclin D1 in superficial bladder cancer. A tissue microarray study. Actas Urol Esp 30:754–762
Zhang PJ, Gao HG, Pasha TL, Litzky L, Livolsi VA (2009) TTF-1 expression in ovarian and uterine epithelial neoplasia and its potential significance, an immunohistochemical assessment with multiple monoclonal antibodies and different secondary detection systems. Int J Gynecol Pathol 28:10–18
Grayson W (2003) Mini-Symposium: immunohistologyingynaecological pathology: application of immunohistochemistry in the evaluation of neoplastic epithelial lesions of the uterine cervix and endometrium. Current Diagn Pathol 9:19–25. http://download.journals.elsevierhealth.com/pdfs/journals/0968-6053/PIIS0968605302901523.pdf
Hadi Y, Allen MG (2001) Immunohistochemical analysis of gynecologic tumors. Int J Gyn Pathol 20:64–78
Wang NP, Zee S, Zarbo RJ, Bacchi CE, Gown AM (1995) Coordinate expression of cytokeratins 7 and 20 defines unique subsets of carcinomas. Appl Immunohistochem 3:99–107
Yeh IT, Mies C (2007) Application of immunohistochemistry to breast lesions. Arch Pathol Lab Med 132:349–358
Acknowledgments
This work was supported in parts by grants from Department of Health (DOH98-PAB-1001-E and DOH98-PAB-1009-I) and Chung-Shan Medical University, Taiwan, ROC.
Conflict of interest statement
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding authors
Additional information
C.-P. Han, L.-F. Kok and M.-Y. Lee have equally contributed to this article.
Rights and permissions
About this article
Cite this article
Han, CP., Kok, LF., Lee, MY. et al. Five commonly used markers (p53, TTF1, CK7, CK20, and CK34βE12) are of no use in distinguishing between primary endocervical and endometrial adenocarcinomas in a tissue microarray extension study. Arch Gynecol Obstet 281, 317–323 (2010). https://doi.org/10.1007/s00404-009-1115-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-009-1115-z