Abstract
Solar radiation is a very important exogenous factor in skin pathogenesis and can lead to the development of a number of skin disorders. UVB irradiation is known to induce oxidative stress, inflammation and especially DNA lesions in exposed cells. It is important, therefore, to identify agents that can offer protection against UVB-caused skin damage. Natural compounds have been studied for their possible ability to control/modulate various lifestyle-related diseases. The application of plant compounds/extracts with screening, antioxidant and anti-inflammatory activities may also successfully protect the skin against UV-caused injury. We assessed the potency of Prunella vulgaris extract (PVE) and its main phenolic acid component, rosmarinic acid (RA), to suppress UVB-induced (295–315 nm) alterations to human keratinocytes HaCaT using a solar simulator. Pre- and post-treatment of HaCaT cells with PVE (5–50 mg/l) and RA (0.18–1.8 mg/l) reduced breakage together with the apoptotic process. PVE and RA also significantly eliminated ROS production and diminished IL-6 release. Taken together, both PVE and RA prevent UVB-caused injury to keratinocytes. However their efficacy needs to be demonstrated in vivo.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Life on the earth is impossible without solar light. Plants utilize the energy in photosynthesis and many vital functions in animals and humans are associated with sunlight. However, excessive exposure to solar radiation has several adverse effects on human health. Reports in this field indicate that the UV part of sunlight is a key risk factor associated with the initiation and development of various skin diseases. Solar UV radiation on the earth’s surface comprises approximately 90–99% UVA and of 1–10% of UVB [38]. Although UVB light (280–315 nm) is largely absorbed (95%) in the protective ozone layer, the rest of the incoming UVB (295–315 nm) is a very potent genotoxic agent. UVB penetrates as far as the epidermal basal cell layer of the skin and thus affects mainly epidermal cells [31]. The basal cell layer serves as stem cells with the ability to divide and produce new cells (keratinocytes), and UVB radiation may alter the proliferation, differentiation and metabolism of these cells.
UVB light affects mainly heterocyclic bases of DNA, strongly absorbing chromophores for UVB light. Direct absorption of UVB photons leads to the formation of cyclobutane–pyrimidine dimers and pyrimidine-pyrimidone (6-4) photoproducts. UVB rays also directly interact with aromatic amino acids in proteins and their modifications may alter protein function [38]. Further, UVB participates in indirect damage to biomolecules via production of reactive oxygen and nitrogen species (RONS), which are capable of oxidizing lipids, proteins and DNA. The oxidized products, including lipid hydroperoxides, protein carbonyls and 8-hydroxydeoxyguanosine, have been proven to be implicated in the onset of skin cancers [36]. UVB light also affects the level of skin antioxidants, impairing the skin’s ability to protect itself against the RONS, and is implicated in the skin inflammatory process, which involves infiltration of inflammatory blood leucocytes (macrophages and neutrophils), increased production of prostaglandins (PGs), release of tumor necrosis factor-alpha (TNF-α), nuclear factor-kappa B (NFκB) and inflammatory cytokines (interleukins: IL-1α, IL-1β, IL-6, IL-8, IL-12) that further induce production of RONS and increase oxidative stress [9, 31].
Inadequate repair of DNA lesions, impaired skin antioxidant network, as well as other adverse biological consequences of UVB exposure may result in disruption of cell regulation, accumulation of modified and defective cells and finally in the formation of skin tumors [33]. Thus, protection of skin against excessive sunlight exposure is essential to forestall the damage [37]. Exogenous application of protective dermatological preparations containing sunscreens (organic and inorganic filters) is commonly recommended. In this regard, several natural substances or standardized plant extracts have also been investigated. These play a role in a broad range of physiological processes including protection against harmful UV radiation [5].
Prunella vulgaris L. (Labiatae) is a perennial herb that has been used as a traditional remedy in European and Chinese medicine for the treatment of sore throat and fever, for accelerating wound healing, and for dermatosis and skin allergies [14]. The organic fraction of P. vulgaris exhibits antioxidative and antimicrobial activities [25]. Phytochemical studies indicate that P. vulgaris is rich in phenolics including rosmarinic, ellagic and caffeic acids [16]. Rosmarinic acid (RA; Fig. 1), the major phenolic acid of the plant, exhibits multiple biological activities, mainly antioxidant, anti-inflammatory and antimutagenic [22]. Recent studies also suggest its usefulness in the treatment of atopic dermatitis [17] and in providing photoprotection [29]. Ellagic acid (EA; Fig. 1) in the form of ellagic acid-rich extract affects skin pigmentation in guinea pig [30] and human [12] skin. Caffeic acid (CA; Fig. 1) affords significant protection against UVA, UVB and UVC light-induced damage in vitro and in vivo [20, 27, 39].
In an earlier work we showed that post-treatment with P. vulgaris extract (PVE) and RA protects HaCaT keratinocytes against UVA-induced oxidative damage [26]. The purpose of this study was to examine PVE and RA preventive and therapeutic effects on UVB-induced damage to HaCaT.
Materials and methods
Materials
Cell proliferation ELISA BrdU (colorimetric) kit, protease inhibitor cocktail tablets Complete™ and Sybr Green were purchased from Roche Diagnostic (Germany). Dihydrorhodamine 123 was from Fluka Chemie (Germany). Caspase-3 (Ac-DEVD-AMC/Ac-DEVD-CHO) and caspase-9 (Ac-LEHD-AFC/Ac-LEHD-CHO) fluorigenic substrate/inhibitor were obtained from Bachem AG (Switzerland). Agarose for DNA electrophoresis was from Serva (Germany). Human IL-6 ELISA kit was purchased from R&D Systems (USA). The genomic DNA purification kit was obtained from Gentra Systems (USA). Western blotting luminol reagent for chemiluminescent horseradish peroxidase (HRP) detection, rabbit anti-caspase-3 primary antibody, actin (I-19) goat polyclonal primary antibody, goat anti-rabbit and rabbit anti-goat HRP-conjugated secondary antibodies were purchased from Santa Cruz Biotechnology (USA). Dulbecco’s modified Eagle’s medium (DMEM) and heat-inactivated fetal calf serum (FCS) were obtained from Invitrogen/Gibco (USA). Sterile dimethyl sulfoxide (DMSO), neutral red (NR), agarose type I and type VII, ethidium bromide and all other chemicals were purchased from Sigma-Aldrich (USA).
P. vulgaris extract and RA
Prunella vulgaris extract (batch SC 310703/11), prepared by extraction of cut dry plant material (aerial part collected in bloom), with 30% (v/v) ethanol, was kindly provided by IVAX Pharmaceuticals s.r.o. (Opava, Czech Republic). PVE was characterized by the content of RA (9.0% w/w; determined by HPLC). RA (purity 99%) was purchased from Sigma-Aldrich.
Cell culture
HaCaT keratinocytes, a spontaneously transformed human epithelial cell line developed by Petra Boukamp and Norbert Fusenig [3], were obtained from CLS (Eppelheim, Germany). Cells were grown in DMEM supplemented with FCS (10%; v/v), streptomycin (100 U/ml) and penicillin (0.1 mg/ml) in a humidified atmosphere with CO2 (5%; v/v) at 37°C. The culture medium was changed twice a week. The cells were subcultured following trypsinization. For experiments, cells were seeded at a density of 1 × 105 cells/cm2 and grown near to confluence.
Treatment of keratinocytes with PVE and RA
Cells were either pre-treated (1 h before irradiation) or post-treated (4 or 8 h after irradiation) with PVE (5–50 mg/l) and RA (0.9–9 mg/l). For all experiments, stock solutions of PVE (1–10 g/l) and RA (0.18-1.8 g/l) were prepared in DMSO. Before application, the solutions were diluted in serum-free medium so that the final concentration of DMSO in medium was 0.5% (v/v). Irradiated and non-irradiated control cells for each protocol were treated with serum-free medium containing the respective aliquot of DMSO (0.5%; v/v) instead of the test compound stock solution.
UVB irradiation
Prior to UV irradiation, cells were properly washed with PBS and covered with a thin layer of PBS. Dishes with keratinocytes were UVB irradiated (100 or 200 mJ/cm2) on ice-cold plates to eliminate UV-induced thermal stimulation. In parallel, non-irradiated cells were treated similarly and kept in the dark in an incubator. For irradiation, a solar simulator SOL-500 (Dr. Hönle UV Technology, Germany), with a spectral range (295–3,000 nm) corresponding to natural sunlight was used. For all experiments, the simulator was equipped with an H2 filter (Dr. Hönle UV Technology, Germany) transmitting wavelengths of 295–315 nm. The UVB output measured by an UVB-meter (Dr. Hönle UV Technology, Germany) in direct contact with the cell culture dish was 0.9 mW/cm2.
Activity of released LDH
The activity of LDH (EC 1.1.1.27) released into the medium via damaged membrane was measured spectrophotometrically at 340 nm, as described previously [18].
Cell proliferation
Cell proliferation was determined using a colorimetric immunoassay, based on the measurement of 5-bromo-2′-deoxyuridine (BrdU) incorporation in place of thymidine into the DNA during DNA synthesis. Proliferation was monitored using a cell proliferation ELISA BrdU (colorimetric) kit according to the manufacturer’s protocol.
DNA single-strand breaks
An alkaline version of the Comet assay was used for monitoring DNA single-strand breaks. This method is based on monitoring DNA lesions in individual cells, after sandwiching cells (approximately 10,000 cells) between thin layers of agarose and subsequent lysis and electrophoresis of cellular DNA. Damaged DNA is visualized by fluorescent stain as comet formation [34]. The assay was performed as described previously [32]. An inversion fluorescent microscope Olympus IX 70 (Olympus, Japan) was used for nuclei analysis.
DNA damage was assessed in 100 nuclei per slide area by visual scoring from 0 (undamaged, no discernible comet tail) to 4 (almost all DNA in tail, insignificant head). Each comet was given a value according to its classification to produce an overall score for each slide ranging from 0 to 400 arbitrary units. Scores were calculated using the following formula:
where N 0, N 1, N 2, N 3, and N 4 are the number of cells in each group from 0 to 4.
DNA fragmentation
DNA was extracted from the cells using the Genomic DNA purification kit (Gentra Systems, USA), as described by the manufacturer’s protocol for 3–5 × 106 cells. The pattern of DNA cleavage was analyzed by agarose gel electrophoresis. Briefly, the DNA samples mixed with loading buffer [glycerol (40%, v/v); bromophenol blue (0.25%, m/v)] 2:1 were separated by horizontal electrophoresis on 1.8% agarose gel (0.89 mol/l Tris; 0.89 mol/l H3BO3; 0.02 mol/l EDTA; pH 8.4), stained with Sybr Green and visualized under UV light.
Caspase-3 and -9 activities
Caspases activity was measured using caspase-3 (Ac-DEVD-AMC) and caspase-9 (Ac-LEHD-AFC) fluorigenic substrates [21]. The cells were washed with PBS and lysed in ice-cold lysis buffer (50 mmol/l HEPES, pH 7.4; Triton X-100 (0.5%; v/v), protease inhibitor cocktail tablet, 5 mmol/l dithiothreitol (DDT) for 15 min at 4°C). The lysate was cleared by centrifugation (14,000 rpm for 15 min at 4°C). The protein concentration was determined by a Bradford assay. The lysate was mixed with assay buffer (20 mmol/l HEPES, pH 7.1, 2 mmol/l EDTA, protease inhibitor cocktail tablet, 5 mmol/l DDT) containing respective fluorigenic substrate or inhibitor and incubated (37°C; 60 min). Fluorescence was measured at 380/450 nm (caspase-3) or 400/505 nm (caspase-9) using a microplate spectrophotometer (INFINITE M200, Tecan, Switzerland).
Caspase-3 activation (Western immunoblot)
The amount of activated caspase-3 was investigated using Western immunoblot analysis. After incubation, cells were harvested and samples were prepared as described previously [32]. The supernatant protein concentration was determined by Lowry assay. Proteins were separated by 15% SDS-polyacrylamide gel electrophoresis and transferred onto a nitrocellulose membrane. Residual binding sites on the membrane were blocked using blocking buffer (5% non-fat dried milk (w/v) in 100 mmol/l Tris-buffered saline (pH 7.5) with Tween 20 (0.05%; v/v)) for 1 h at room temperature. The membrane was then incubated with a primary antibody (rabbit anti-caspase-3 or goat anti-actin (I-19)) overnight at 4°C and then with a secondary HRP-conjugated antibody (goat anti-rabbit antibody or rabbit anti-goat antibody) for 2 h at room temperature. Caspase-3/actin expression was detected by chemiluminescence using Western blotting luminol reagent and autoradiography with XAR-5 film.
Evaluation of ROS generation
The pre-fluorescent probe dihydrorhodamine 123 was used to monitor the intracellular ROS generation induced by UVB light, as described previously [32]. Briefly, after irradiation and treatment with PVE/RA, the cells were incubated with dihydrorhodamine 123 (5 nmol/l) 20 min in the incubator at 37°C. Cells were then properly washed with PBS, scraped into 1 ml of PBS, sonicated and centrifuged (10,000 rpm for 10 min at 4°C). The fluorescence was measured using a microplate spectrophotometer (INFINITE M200, Tecan, Switzerland) at specific excitation/emission wavelengths of 500/536 nm. The protein concentration was determined by a Bradford assay [4].
Interleukin-6 determination
The amount of IL-6 was determined using a specific immunoassay kit Quantikine® (R&D Systems, USA) according to the manufacturer’s protocol. Briefly, after the incubation period, the medium was collected and samples were measured immediately or stored at −80°C. The media were mixed (1:1) with the assay diluent on the 96-well plate, covered with a specific monoclonal antibody and incubated (2 h at room temperature). The mixture was removed, wells were rinsed four times with wash buffer and the conjugate solution was added (2 h at room temperature). Then the solution was removed, the wells were rinsed four times with wash buffer and the substrate solution was added. After incubation (10 min at room temperature, in the dark), stop solution was applied and a yellow-colored product was measured at 450 nm (Sunrise, Tecan, Switzerland)).
Statistical analysis
The series of experiments were performed at least in three independent examinations with three replicates for each sample. Data were expressed as mean ± SD. Statistical comparison was performed using the Student’s t test. Statistical significance was determined at p = 0.05.
Results
Effect of PVE and RA on UVB-induced membrane disruption
Prunella vulgaris extract and rosmarinic acid at concentrations used in our experiments were not toxic to keratinocytes, as describe elsewhere [26]. Pre-treatment with PVE and RA reduced LDH release into the medium in UVB-irradiated (200 mJ/cm2) cells. Protective effect of both PVE and RA was approximately 30% for all concentrations (Fig. 2a). Post-treatment with the extract and RA diminished LDH leakage in a concentration-dependent manner. At the highest concentration, PVE and RA showed protection of 80 and 70%, respectively (Fig. 2b).
PVE and RA reduce UVB-induced LDH leakage into the medium. Keratinocytes were pre-treated (1 h; a) or post-treated (8 h; b) with PVE (5–50 mg/l) or RA (0.18–1.8 mg/l). Cells were exposed to solar UVB (295–315 nm; 200 mJ/cm2). Irradiated and non-irradiated control cells were incubated with DMSO (0.5%; v/v) under the same conditions. Data are expressed as mean ± S.D. (#) p < 0.05 and (*) p < 0.01 are statistically different from irradiated cells
Effect of PVE and RA on UVB-affected cell proliferation
Keratinocytes pre-treated with PVE and RA and exposed to UVB (100 mJ/cm2) showed a higher level of BrdU incorporation than untreated irradiated cells. Protection reached 17% (Fig. 3a). Application of PVE and RA after irradiation increased keratinocyte proliferation as well. Concentration dependence was not observed and both PVE and RA showed protection around 25% (Fig. 3b).
PVE and RA reduce UVB-induced disruption of HaCaT proliferation. Keratinocytes were pre-treated (1 h; a) or post-treated (8 h; b) with PVE (5–50 mg/l) or RA (0.18–1.8 mg/l). Cells were exposed to solar UVB (295–315 nm; 200 mJ/cm2). Irradiated and non-irradiated control cells were incubated with DMSO (0.5%; v/v) under the same conditions. Data are expressed as mean ± SD. (#) p < 0.05 and (*) p < 0.01 are statistically different from irradiated cells
PVE and RA protect keratinocyte against UVB-induced DNA breakage
Possible detrimental effect of PVE and RA on keratinocyte DNA was excluded. The number and extent of DNA damage on non-irradiated HaCaT treated with PVE (25 and 50 mg/l) and RA (4.5 and 9 mg/l) for 24 h was comparable with control cells (data not shown). Pre-treatment of keratinocytes with PVE and RA protected DNA against the formation of single strand breaks. The effect of both was concentration-dependent. However, the potency of RA was more powerful at all concentrations than that of PVE. The maximal protection of PVE and RA reached nearly 65 and 80%, respectively (Fig. 4a). In cells post-treated with PVE, DNA damage declined with increasing extract concentration and the highest protection was 65%. RA reduced DNA breakage most effectively at a concentration of 2.25 mg/l (85%). At higher concentrations, its protection was 50% (Fig. 4b).
PVE and RA decrease UVB-caused DNA single-strand breaks formation in HaCaT. Keratinocytes were pre-treated (1 h; a) or post-treated (4 h; b) with PVE (5–50 mg/l) or RA (0.18–1.8 mg/l). Cells were exposed to solar UVB (295–315 nm; 200 mJ/cm2). Irradiated and non-irradiated control cells were incubated with DMSO (0.5%; v/v) under the same conditions. To evaluate DNA damage, 100 cells (nuclei) per slide were analyzed. Total damage is expressed in arbitrary units, which range from 0 (undamaged DNA) to 400 (totally damaged DNA). Data are expressed as mean ± SD. (*) p < 0.01 is statistically different from irradiated cells
Modulation of UVB-induced apoptosis by PVE and RA
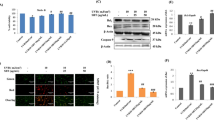
Caspase-3 activity in HaCaT pre-treated with PVE and RA was obviously reduced in comparison to untreated UVB-irradiated (200 mJ/cm2) cells (Fig. 5a). The effect of PVE was more potent than that of RA with a maximum at a concentration of 25 mg/l (52%). RA reached the most efficient protection at a concentration of 4.5 mg/l (40%). At the highest concentration, the preventive effects of both PVE and RA decreased. Application of PVE and RA after UVB exposure reduced caspase-3 activity as well. The observed effect was not concentration-dependent (Fig. 5b) and was similar for both PVE and RA. Their protection reached approximately 75% for all concentrations. Evaluation of caspase-3 activation, the cleavage of pro-caspase-3 into smaller fragments, by Western blot demonstrated a decrease in activated caspase-3 in cells treated with PVE and RA. RA was more powerful than PVE in both pre-treatment and post-treatment protocols and reduced caspase-3 activation to nearly the level of non-irradiated cells (Fig. 6).
PVE and RA reduce UVB-induced caspase-3 activity in HaCaT. Keratinocytes were pre-treated (1 h; a) or post-treated (8 h; b) with PVE (5–50 mg/l) or RA (0.18–1.8 mg/l). Cells were exposed to solar UVB (295–315 nm; 200 mJ/cm2). Irradiated and non-irradiated control cells were incubated with DMSO (0.5%; v/v) under the same conditions. Data are expressed as mean ± SD. (*) p < 0.01 is statistically different from irradiated cells
PVE and RA inhibit UVB-induced caspase-3 activation in HaCaT. Keratinocytes were pre-treated (1 h; a) or post-treated (8 h; b) with PVE (5–50 mg/l) or RA (0.18–1.8 mg/l). Cells were exposed to solar UVB (295–315 nm; 200 mJ/cm2). Irradiated and non-irradiated control cells were incubated with DMSO (0.5%; v/v) under the same conditions. Data are representative of three independent experiments
Pre-treatment of keratinocytes with PVE and RA also reduced caspase-9 activity augmented by UVB radiation (200 mJ/cm2) (Fig. 7a). The effect of PVE was most apparent at a concentration of 10–25 mg/l (80% protection). The ability of RA was maximal at a concentration of 4.5 mg/l (90%). The application of PVE after UVB exposure reduced caspase-9 activity in a concentration-dependent manner and the maximal protection was nearly 80%. RA decreased caspase-9 activity similarly at all concentrations tested and protection was approximately 70% (Fig. 7b).
PVE and RA reduce UVB-induced caspase-9 activity in HaCaT. Keratinocytes were pre-treated (1 h; a) or post-treated (8 h; b) with PVE (5–50 mg/l) or RA (0.18–1.8 mg/l). Cells were exposed to solar UVB (295–315 nm; 200 mJ/cm2). Irradiated and non-irradiated control cells were incubated with DMSO (0.5%; v/v) under the same conditions. Data are expressed as mean ± SD. (*) p < 0.01 is statistically different from irradiated cells
The hallmark of apoptotic cell death is DNA fragmentation. The application of PVE before irradiation (200 mJ/cm2) reduced DNA cleavage in keratinocytes and the most pronounced effect was observed at a concentration of 25 mg/l (Fig. 8a, line 6). At the highest concentration, its potency decreased. The effect of RA was concentration-dependent and at concentrations of 4.5–9 mg/l (Fig. 8a, line 10 and 11) DNA laddering was comparable with that in non-irradiated cells. In the post-treatment protocol, the effect of PVE and RA was determined only for the two highest concentrations. The effect of PVE and RA was similar to that observed in the pre-treatment protocol. PVE at a concentration of 25 mg/l (Fig. 8b, line 3) obviously reduced DNA cleavage, but the highest concentration was not effective. RA significantly prevented DNA fragmentation in a concentration-dependent manner (Fig. 8b, line 5 and 6).
Effect of PVE and RA on UVB-induced DNA fragmentation in HaCaT. Keratinocytes were pre-treated (1 h; a) or post-treated (8 h; b) with PVE (5–50 mg/l) or RA (0.18–1.8 mg/l). Cells were exposed to solar UVB (295–315 nm; 200 mJ/cm2). Irradiated and non-irradiated control cells were incubated with DMSO (0.5%; v/v) under the same conditions. Data are representative of three independent experiments. (a) line 1 standard; line 2 non-irradited cells; line 3 UVB (200 mJ/cm2); line 4 PVE 5 mg/l + UVB; line 5 PVE 10 mg/l + UVB; line 6 PVE 25 mg/l + UVB; line 7 PVE 50 + UVB; line 8 RA 0.18 mg/l + UVB; line 9 RA 0.45 mg/l + UVB; line 10 RA 0.9 mg/l + UVB; line 11 RA 1.8 mg/l + UVB. (b) line 1 non-irradiated cells; line 2 UVB(200 mJ/cm2); line 3 UVB + PVE 25 mg/l; line 4 UVB + PVE 50 mg/l; line 5 UVB + RA 0.9 mg/l; line 6 UVB + RA 1.8 mg/l; line 7 standard
PVE and RA ability to modulate UVB-induced ROS generation
The treatment of non-irradiated HaCaT with PVE and RA (4 h) slightly reduced ROS generation compared to untreated non-irradiated HaCaT (data not shown). Treatment with PVE and RA before irradiation prevented ROS production in irradiated (200 mJ/cm2) HaCaT (Fig. 9a). Their effect did not depend on concentration. Protection was approximately 30% (PVE) and 35% (RA). However, excellent concentration-dependent ROS decrease was found in post-treated cells (Fig. 9b). At concentrations of 25 and 50 mg/l, PVE reduced ROS level to that of control. Similarly in cells treated with RA (4.5 and 9 mg/l), the level of ROS was comparable with non-irradiated keratinocytes.
PVE and RA reduce UVB-induced ROS generation in HaCaT. Keratinocytes were pre-treated (1 h; a) or post-treated (4 h; b) with PVE (5–50 mg/l) or RA (0.18–1.8 mg/l). Cells were exposed to solar UVB (295–315 nm; 200 mJ/cm2). Irradiated and non-irradiated control cells were incubated with DMSO (0.5%; v/v) under the same conditions. Data are expressed as mean ± SD. (#) p < 0.05 and (*) p < 0.01 is statistically different from irradiated cells
Effect of PVE and RA on interleukin-6 release
Prunella vulgaris extract and rosmarinic acid attenuated IL-6 release in irradiated (200 mJ/cm2) cells, when they were applied before UVB exposure. The effects of PVE and RA were concentration-dependent with a maximal protection of 25% (Fig. 10a). In post-treated HaCaT, the ability of PVE was concentration-dependent as well (maximal protection reached 40%). The greatest potency of RA was observed at a concentration of 2.25 mg/l (54%) and at higher concentrations decreased slightly (Fig. 10b).
PVE and RA decrease UVB-induced IL-6 release from HaCaT. Keratinocytes were pre-treated (1 h; a) or post-treated (8 h; b) with PVE (5–50 mg/l) or RA (0.18–1.8 mg/l). Cells were exposed to solar UVB (295–315 nm; 200 mJ/cm2). Irradiated and non-irradiated control cells were incubated with DMSO (0.5%; v/v) under the same conditions. Data are expressed as mean ± SD. (#) p < 0.05 and (*) p < 0.01 is statistically different from irradiated cells
Discussion
The use of UV photoprotective dermatological preparations is one of the most recommended and the most common way of preventing solar UV light-caused damage to the skin. For this purpose, several photoprotective agents have been developed. The current world trend is to enhance the effect of chemical sunscreens with natural bioactive products. The use of natural compounds that absorb UV rays and protect skin against UVB and UVA radiation is of great interest. Owing to similarities in structure and absorbance spectrum profiles between polyphenolic compounds and organic UV filters, polyphenols might be effective in photoprotection [37]. Besides these attributes, polyphenolic compounds exhibit a wide range of biological activities, such as antioxidant, radical scavenging, anti-inflammatory, immunomodulatory and antitumor [5], which are essential for superior photoprotective agents. Previously, we demonstrated the protective effect of PVE and RA against UVA-caused oxidative damage in HaCaT [26]. Here, we have shown their ability to reduce UVB-induced alterations in the HaCaT cell line.
DNA bases are considered to be the main targets (chromophores) of UVB irradiation, which induces primarily two types of DNA lesion, cyclobutane–pyrimidine dimers and pyrimidine-pyrimidone (6-4) photoproducts [38]. The DNA lesions observed in the comet assay after UVB treatment are thought to be due to transient DNA breaks during the nucleotide excision repair of the photoproducts. Other mechanisms including oxidative damage to DNA due to the excess of ROS generation may also contribute to the UVB-induced comet formation [35]. We found that application of PVE and RA before and after irradiation significantly reduced UVB-caused DNA breakage, especially at the highest concentration (50 mg/l PVE; 9 mg/l RA). Post-treatment with RA was the most effective at a concentration of 0.45 mg/l. At higher concentrations, the protection slightly dropped slightly, although RA itself did not induce DNA single-strand breaks in non-irradiated cells after 24 h of treatment. The apparent lack of polyphenols/plant extract protection at higher concentrations has been described [7, 11]. The irregularity of dose–effect relationship may be linked with a pro-oxidant effect of polyphenols at high concentrations, especially under the conditions of the disrupted antioxidant/oxidant balance that occurs after treatment with ROS-generating agents such as some drugs and UV irradiation. Hanif et al. hypothesize that the pro-oxidant activity of polyphenols maybe linked to their ability to mobilize copper ions that leads to ROS generation and DNA oxidative damage [8].
Damage to chromosomal DNA is associated with cell cycle arrest, which allows the cell time to repair DNA lesions before DNA replication [19]. This manifests also as cell proliferation disruption. Both PVE and RA slightly prevented keratinocytes from UVB-caused proliferation arrest. A more pronounced effect of PVE/RA was observed in post-treatment protocol.
DNA lesion, such as cyclobutane–pyrimidine dimers, can stimulate the secretion of cytokines, e.g., IL-1, IL-6 and IL-8 in human keratinocytes [9, 23]. Application of PVE and RA to HaCaT before and after UVB exposure reduced IL-6 secretion. However, post-treatment was more powerful. In a recent study, Kim et al. showed the anti-inflammatory potency of an aqueous extract of P. vulgaris. They found that it significantly inhibited IL-6, IL-8 and TNF-α secretion from phorbol 12-myristate 13-acetate and calcium ionophore (A23187)-stimulated mast cells (HMC-1), together with suppression of NFκB activation [14].
DNA damage is also linked with apoptotic cell death. Cells with excessive or irreparable damage to nuclear DNA are eliminated by apoptosis to limit the incidence and propagation of defective cells. Apoptosis is a tightly regulated form of cell death and multifactor-related process. During apoptosis, the expression of pro-apoptotic genes up-regulates and/or the expression of anti-apoptotic genes down-regulates [15]. Caspases are mediators of apoptotic cell death. Both intrinsic and extrinsic pathways finally merge together and lead to activation of caspase-3, the critical marker for apoptosis [2]. UVB irradiation was found to induce apoptosis through both pathways and strongly increases caspase-3 activity [6]. The later stadium of apoptosis appears as cleavage of chromosomal DNA into fragments [13]. We have shown that caspase-3 and -9 activities in UVB-exposed cells were inhibited when keratinocytes were treated with PVE and RA before or after irradiation. Both PVE and RA also reduced pro-caspase-3 cleavage into active form. However, the effect of RA was more obvious. DNA laddering was prevented in pre- and post-treated HaCaT; RA was again more powerful.
The mitochondrial apoptotic pathway is activated by increased ROS generation, which is a pivotal characteristic phenomenon of UV exposure that can result in oxidative stress and biomolecules damage [28]. Pre-treatment with PVE and RA obviously reduced ROS generation in UVB-irradiated cells. The application of PVE and RA after exposure decreased the ROS levels to those of non-irradiated cells.
As we used the whole standardized ethanolic extract of P. vulgaris and not the purified simple compound, the active components responsible for the UVB preventive effect are unclear. However, in parallel with the beneficial effects of PVE on UVB-irradiated HaCaT cells, we assessed the photoprotective activity of RA, the main phenolic acid of PVE. On several parameters, RA showed similar or more pronounced ability to prevent/reduce UVB-induced alterations. We can assume that RA is an active compound of PVE. Recent reports have also shown the UVA (photo)protective power of RA. Orally administered RA inhibited cutaneous alterations caused by chronic UVA exposure in Swiss mice [29]. Topically applied RA and its structural analog caffeic acid (CA), at concentrations of both 5 and 10 mmol/l, significantly protect SKH-1 mice against UVA-caused ROS generation. However, the effectiveness of RA was higher than CA. Orally administered CA for 3 days before UV exposure significantly suppressed ROS generation in mice skin as well. Evaluation of organ and tissue distribution confirmed that orally used CA efficiently distributes in the skin and does not accumulate in the tissue [39]. Poquet et al. showed that CA and its derivative dihydrocaffeic acid significantly reduced pro-inflammatory cytokine production in UVB-irradiated HaCaT [24]. Moreover, CA protected against UVB-caused skin erythema in breast skin samples of human volunteers [27]. Ellagic acid (EA), the second most abundant polyphenol in PVE, exerted strong effects in suppressing lipid peroxide levels in random flaps of rat back skin [1]. Degradation of cutaneous elastic fibers, which constitutes the major feature of aging skin, is a well-known sign of chronically UV exposed skin. A recent study reported that EA also protects human dermal fibroblast against exogenous and endogenous enzymatic degradation of elastin as well as enhanced elastogenesis in fibroblast culture [10]. Other PVE constituents very likely contribute to the overall effects of PVE. However, due to a combination of action of several compounds with different structures, PVE could modulate various cellular pathways, which are affected during or after UVB irradiation and thus the application of the mixture may be more beneficial than the use of the single compound. Use of a mixture may also minimize any potentially adverse effects of the components, as the desired effect may be achieved at lower concentrations of the constituents.
To sum up, the results showed that PVE and RA prevent or at least moderate UVB-caused damage to keratinocytes. The (photo)protective effect of both seems to be linked to direct elimination of ROS that prevent oxidative damage of cellular molecules and apoptosis. Their ability to reduce DNA lesions, caspase-3 and -9 activity and secretion of IL-6 may also reflect their antioxidant activity. The protective activity may also be connected with their ability to absorb UV photons, as shown in the absorption spectra of PVE and RA (Fig. 11). Both PVE and RA absorb in the UVB as well as UVA region. In this way, PVE components and RA may reduce the number of photons attacking cell molecules. Further experimental work is necessary to examine the bioavailability of RA and PVE active components to the skin, to exclude any possible toxic or phototoxic effects and to clarify their photoprotective activity in vitro and in vivo.
Absorption and photostability spectra of P. vulgaris extract and rosmarinic acid. PVE (final concentration 25 mg/l) and RA (final concentration 10 μmol/l) were diluted in phosphate saline buffer (pH 7.5). The PVE or RA solution, placed in a 6-well plate (2 ml per well), was UVB irradiated (1 J/cm2, ~20 min) using a solar simulator (Dr. Hönle UV Technology, Germany). The non-irradiated samples were kept in the incubator for the irradiation period. The absorption spectrum was measured between 240 and 600 nm in UV–Vis spectrophotometer UV-2401PC (Shimadzu, Japan) immediately after UVB treatment. Non-irradiated and irradiated samples (PVE, RA) were scanned in quartz cuvette against non-irradiated and irradiated blanks (0.5% DMSO), respectively
References
Ashoori F, Suzuki S, Zhou JH, Isshiki N, Miyachi Y (1994) Involvement of lipid peroxidation in necrosis of skin flaps and its suppression by ellagic acid. Plast Reconstr Surg 94:1027–1037
Aufiero BM, Talwer H, Young C, Krishnan M, Hatfield JS, Lee HK, Wong HK, Hamzavi I, Murakawa GJ (2006) Narrow-band UVB induces apoptosis in human keratinocytes. J Photochem Photobiol B 82:132–139
Boukamp P, Petrussevska RT, Breitkreutz D, Hornung J, Markham A, Fusenig NE (1988) Normal keratinization in a spontaneously immortalized aneuploid human keratinocyte cell line. J Cell Biol 106:761–771
Bradford MM (1976) A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein–dye binding. Anal Biochem 72:248–254
Dinkova-Kostova AT (2008) Phytochemicals as protectors against ultraviolet radiation: versatility of effects and mechanisms. Planta Med 74:1548–1559
El-Mahdy MA, Zhu Q, Wang QE, Wani G, Patnaik S, Zhao Q, Arafa el-S, Barakat B, Mir SN, Wani AA (2008) Naringenin protects HaCaT human keratinocytes against UVB-induced apoptosis and enhances the removal of cyclobutane pyrimidine dimers from the genome. Photochem Photobiol 84:307–316
Fan P, Lou H (2004) Effects of polyphenols from grape seeds on oxidative damage to cellular DNA. Mol Cell Biochem 267:67–74
Hanif S, Shamim U, Ullah MF, Azmi AS, Bhat SH, Hadi SM (2008) The anthocyanidin delphinidin mobilizes endogenous copper ions from human lymphocytes leading to oxidative degradation of cellular DNA. Toxicology 249:19–25
Ishida T, Sakaguchi I (2007) Protection of human keratinocytes from UVB-induced inflammation using root extract of Lithospermum erythrorhizon. Biol Pharm Bull 30:928–934
Jimenez F, Mitts TF, Liu K, Wang Y, Hinek A (2006) Ellagic and tannic acids protect newly synthesized elastic fibers from premature enzymatic degradation in dermal fibroblast cultures. J Invest Dermatol 126:1272–1280
Kapiszewska M, Sołtys E, Visioli F, Cierniak A, Zajac G (2005) The protective ability of the Mediterranean plant extracts against the oxidative DNA damage. The role of the radical oxygen species and the polyphenol content. J Physiol Pharmacol 56:183–197
Kasai K, Yoshimura M, Koga T, Arii M, Kawasaki S (2006) Effects of oral administration of ellagic acid-rich pomegranate extract on ultraviolet-induced pigmentation in the human skin. J Nutr Sci Vitaminol (Tokyo) 52:383–388
Khodarev NN, Sokolova IA, Vaughan AT (1998) Mechanisms of induction of apoptotic DNA fragmentation. Int J Radiat Biol 73:455–467
Kim SY, Kim SH, Shin HY, Lim JP, Chae BS, Park JS, Hong SG, Kim MS, Jo DG, Park WH, Shin TY (2007) Effects of Prunella vulgaris on mast cell-mediated allergic reaction and inflammatory cytokine production. Exp Biol Med (Maywood) 232:921–926
Kulms D, Schwarz T (2002) Independent contribution of three different pathways to ultraviolet-B-induced apoptosis. Biochem Pharmacol 64:837–841
Lamaison JL, Petitjean-Freytet C, Carnat A (1991) Medicinal Laminaceae with antioxidant properties, a potential source of rosmarinic acid. Pharm Acta Helv 66:185–188
Lee J, Jung E, Koh J, Kim YS, Park D (2008) Effect of rosmarinic acid on atopic dermatitis. J Dermatol 35:768–771
Maines MD (1998) Current protocols in toxicology. Wiley, USA
Melnikova VO, Ananthaswamy NH (2005) Cellular and molecular events leading to the development of skin cancer. Mutat Res 571:91–106
Neradil J, Veselská R, Slanina J (2003) UVC-protective effect of caffeic acid on normal and transformed human skin cells in vitro. Folia Biol (Praha) 49:197–202
Ochu EE, Rothwell NJ, Waters CM (1998) Caspase mediate 6-hydroxydopamine-induced apoptosis but not necrosis in PC12 cells. J Neurochem 70:2637–2640
Petersen M, Simmonds MS (2003) Rosmarinic acid. Phytochemistry 62:121–125
Petit-Frère C, Capulas E, Lyon DA, Norbury CJ, Lowe JE, Clingen PH, Riballo E, Green MH, Arlett CF (2000) Apoptosis and cytokine release induced by ionizing or ultraviolet B radiation in primary and immortalized human keratinocytes. Carcinogenesis 21:1087–1095
Poquet L, Clifford M, Williamson G (2008) Effect of dihydrocaffeic acid on UV irradiation of human keratinocyte HaCaT cells. Arch Biochem Biophys 476:196–204
Psotová J, Kolář M, Soušek J, Švagera Z, Vičar J, Ulrichová J (2003) Biological activities of Prunella vulgaris extract. Phytother Res 17:1082–1087
Psotová J, Svobodová A, Kolářová H, Walterová D (2006) Photoprotective properties of Prunella vulgaris and rosmarinic acid on human keratinocytes. J Photochem Photobiol B 84:167–174
Saija A, Tomaino A, Trombetta D, De Pasquale A, Uccella N, Barbuzzi T, Paolino D, Bonina F (2000) In vitro and in vivo evaluation of caffeic and ferulic acids as topical photoprotective agents. Int J Pharm 199:39–47
Sander CS, Chang H, Hamm F, Elsner P, Thiele JJ (2004) Role of oxidative stress and the antioxidant network in cutaneous carcinogenesis. Int J Dermatol 43:326–335
Sánchez-Campillo M, Gabaldon JA, Castillo J, Benavente-García O, Del Baño MJ, Alcaraz M, Vicente V, Alvarez N, Lozano JA (2009) Rosmarinic acid, a photo-protective agent against UV and other ionizing radiations. Food Chem Toxicol 47:386–392
Shimogaki H, Tanaka Y, Tamai H, Masuda M (2000) In vitro and in vivo evaluation of ellagic acid on melanogenesis inhibition. Int J Cosmet Sci 22:291–303
Svobodová A, Psotová J, Walterová D (2003) Natural phenolics in the prevention of UV-induced skin damage. A review. Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub 147:137–145
Svobodová A, Zdařilová A, Mališková J, Mikulková H, Walterová D, Vostálová J (2007) Attenuation of UVA-induced oxidative damage to human keratinocytes by silymarin. J Dermatol Sci 46:21–30
Thomas-Ahner JM, Wulff BC, Tober KL, Kusewitt DF, Riggenbach JA, Oberyszyn TM (2007) Gender differences in UVB-induced skin carcinogenesis, inflammation, and DNA damage. Cancer Res 67:3468–3474
Tice RR, Andrews PW, Singh NP (1990) The single cell gel assay: a sensitive technique for evaluating intercellular differences in DNA damage and repair. Basic Life Sci 53:291–301
Tzung TY, Rünger TM (1998) Assessment of DNA damage induced by broadband and narrowband UVB in cultured lymphoblasts and keratinocytes using the comet assay. Photochem Photobiol 67:647–650
Vayalil PK, Mittal A, Hara Y, Elmets CA, Katiyar SK (2004) Green tea polyphenols prevent ultraviolet light-induced oxidative damage and matrix metalloproteinases expression in mouse skin. J Invest Dermatol 122:1480–1487
Velasco MV, Sarruf FD, Salgado-Santos IM, Haroutiounian-Filho CA, Kaneko TM, Baby AR (2008) Broad-spectrum bioactive sunscreens. Int J Pharm 363:50–57
Verschooten L, Claerhout S, Van Laethem A, Agostinis P, Garmyn M (2006) New strategies of photoprotection. Photochem Photobiol 82:1016–1023
Yamada Y, Yasui H, Sakurai H (2006) Suppressive effect of caffeic acid and its derivatives on the generation of UVA-induced reactive oxygen species in the skin of hairless mice and pharmacokinetic analysis on organ distribution of caffeic acid in ddY mice. Photochem Photobiol 82:1668–1676
Acknowledgments
This work was supported by the grant of Grant Agency of the Czech Republic (303/07/P314) and Ministry of Education of the Czech Republic (MSM 6198959216). We thank Dr. Ladislav Cvak (IVAX Pharmaceuticals, Opava, Czech Republic) for providing the P. vulgaris extract.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Vostálová, J., Zdařilová, A. & Svobodová, A. Prunella vulgaris extract and rosmarinic acid prevent UVB-induced DNA damage and oxidative stress in HaCaT keratinocytes. Arch Dermatol Res 302, 171–181 (2010). https://doi.org/10.1007/s00403-009-0999-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00403-009-0999-6