Abstract
Thinning of the dermis is the principal histological change in atrophic skin disorders and aged skin. It is caused due to a decreased amount of collagen in the dermis. Macrolides have been reported to exert various pharmacological activities, including anti-inflammatory activity, tumor angiogenesis inhibition and growth inhibition of fibroblasts, in addition to antimicrobial activity. In this study, we investigated the effects of erythromycin A (EMA) and its new derivative EM201 on type I collagen production by cultured dermal fibroblasts. Dermal fibroblasts were cultured with 10−9 M-10−5 M EMA or EM201, and collagen production was measured by incubation with radioactive proline, SDS-polyacrylamide gel electrophoresis and fluorography. mRNA levels were measured by Northern blots analysis, and to investigate transcriptional levels luciferase assays were also performed. The results showed that both EMA and EM201 increased collagen production and type I collagen mRNA level (to a maximum of 200% with EMA and 250% with EM201) in a dose-dependent manner in cultured dermal fibroblasts. Transcription of the type I collagen gene was also increased by both macrolides. These results suggest that EMA and EM201 have the potential to improve the thinning of the dermis in atrophic skin disorders and aged skin.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Type I collagen is the principal component of the collagen fibers in the dermis, and it is produced by fibroblasts. Thus, a breakdown in the regulation of type I collagen expression in fibroblasts causes abnormalities in the amount of the dermal collagen fibers of the skin. When expression of type I collagen increases beyond the normal level, the amount of collagen fibers increases, resulting in a condition of fibrosis [18, 27]. If the expression falls below the normal level, on the other hand, the quantity of collagen fibers decreases, which causes conditions of atrophic skin disorders and wrinkles [15, 30]. Consequently, research on the regulation of the expression of type I collagen is extremely important for understanding these conditions and the mechanisms of the diseases that cause them and considering methods to treat them. Macrolides have been reported to exert various pharmacological activities, including anti-inflammatory activity [16], tumor angiogenesis inhibition [32], inhibition of in vitro malignant tumor cells proliferation [33] and inhibition of the growth of fibroblasts [24], in addition to antimicrobial activity. In this study, we investigated the effects of erythromycin A (EMA) and its new derivative EM201 on type I collagen production by cultured human dermal fibroblasts and found that these drugs have activity that increases its production.
Materials and methods
Reagents
Erythromycin A (EMA) and its new derivative EM201, a 14-membered ring macrolide compound, were synthesized at Kitasato University (Tokyo, Japan) (Fig. 1). EM201 has been shown to be almost free of antibacterial activity [34]. The macrolides were dissolved in DMSO and used at a final concentration of 10−9–10−5 M.
Fibroblast cultures
Skin sample from three healthy donors (a 1-year-old boy, an 18-year-old man and a 25-year-old woman) undergoing plastic surgery were obtained after informed consent. Fibroblast cultures were established from the skin biopsy specimens by the outgrowth method described previously [8], and the cell strains obtained were designated N-1M, N-18M and N-25F, respectively. The cultures were maintained in Dulbecco’s modified Eagle medium (DMEM) containing 10% fetal bovine serum (FBS), in a CO2 incubator at 37°C. The cells were used in each comparative study at population doubling levels (PDLs) of two to five.
Fibroblast proliferation assay [13]
We inoculated 24-well tissue culture plates with 2 × 104 fibroblasts per well, and the next day we started culturing the fibroblasts in DMEM containing 10−9–10−4M EMA or 10−9–10−4M EM201. We counted the numbers of fibroblasts after 24, 48 and 72 h A Burker-Turk hemocytometer was used to make the cell counts.
Isolation and measurement of newly synthesized collagen [11]
When the cell layers had become confluent, the cells were cultured for 48 h at 37°C in DMEM containing 0.2% FBS and supplemented with macrolides at concentrations of 10−9–10−5 M. They were then incubated with DMEM containing 5 μCi/ml 2,3-[3 H] proline (Amersham) in the presence of 50 μg/ml l-ascorbic acid 2-phosphate for 24 h. Labeled proteins secreted into the culture medium were precipitated by the addition of 5% (final concentration) trichloroacetic acid. The precipitate was dissolved in 0.05 M acetic acid, and after being digested with 0.1% pepsin was subjected to SDS-PAGE (5% polyacrylamide gel containing 3.6 M urea). Radioactive bands were detected by fluorography, and the relative amounts of collagen were quantified by densitometry.
RNA extraction and Northern blot analysis [14]
Fibroblasts were cultured to confluence in DMEM containing 10% FBS in 100 mm × 20 mm dishes, and then for 48 h in DMEM containing 0.2% FBS and macrolides at concentrations of 10−9–10−5 M. Total RNA was isolated from the fibroblasts by extraction in guanidium isothiocyanate, and an aliquot (5 μg per lane) was size-fractionated by 1% agarose gel electrophoresis and transferred to a nylon filter. Equal loading was confirmed by staining the gels with ethidium bromide. The blots were immobilized by UV cross-linking and prehybridization for 4 h at 42°C in a solution containing 50% formamide, 10% Denhardt’s solution, 5× SSC, 20 mM sodium phosphate, 0.1% SDS and 0.1 mg/ml denatured salmon sperm DNA. The hybridization was performed at 42°C overnight in the above solution in the presence of 10% dextran sulfate and cDNA probes labeled by nick translation with [α-32P] dCTP (Amersham, England). The human cDNA probes used for the Northern hybridization: were α1(I) collagen [4] and glyceraldehyde-3-phosphate dehydrogenase (GAPDH) [2]. The filter was washed in solutions of decreasing ionic strength and increasing temperature, and the final stringency of the washes was 0.1× SSC, 0.1% SDS at 65°C. Kodak X Omat film was then exposed to the filters for various periods of time, and the radioactivity was quantified by scanning the bands with a densitometer. To probe the membrane again, the membrane was washed in sterile water at room temperature, equilibrated in 2× SSC for 5 min, and then incubated in 0.1% SDS, 0.1× SSC at 95°C for 10 min to remove the preceding probe.
DNA constructs
Plasmid p2.3COL1A1Luc contains the human COL1A1 promoter region, encompassing −2.3 kb to +42 bp, fused to the luciferase gene. A Sac I- Kpn I fragment of the −2.3 kb to +42 bp region of the α(I) collagen gene from p2.3 Kα(I)CAT [23] was subcloned into the Sac I- Kpn I sites of pGEM7(+) (Promega), excised as a Sac I-Xho I fragment and subcloned into the Sac I-Xho I sites of pGL2-Basic (Promega) [17]. The CMV immediate early enhancer promoter renilla luciferase construct (phRL-CMV Vector, Promega) was used as an internal control to correct for variations in transfection efficiency between the samples.
Transient transfection and luciferase assay
A total of 5 × 105 cells were plated in 6-well tissue culture plates and cultured as described above. After 2 days, the culture medium was changed to DMEM containing 1% FBS with or without the macrolides, and the transfections were performed by using the FuGene 6 kit (Roche Applied Science) as described previously [29]. The cells were co-transfected with 1.0 μg of the human COL1A1 promoter fused to the luciferase gene and 20 ng of phRL-CMV vector. After 48 h later, the cells were harvested, and lysates were prepared using the passive lysis buffer (Promega). Luciferase activity in equal aliquots was determined with the Dual Luciferase Reporter Assay System (Promega) and a luminometer. All experiments were performed in triplicate and repeated at least three times.
Statistical analysis
The data were expressed as means ± standard error of the mean (SEM). The significance of the differences between the untreated (control) and treated cells was determined by Student’s t test. P values less than 0.05 were considered to be significant.
Results
Effect of erythromycin A (EMA) and EM201 on cell growth activity
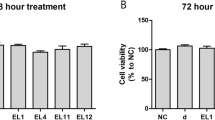
Τo determine whether EMA and EM201 have effects on cell growth activity of fibroblasts, first, we cultured the cells with the drugs and analyzed their growth curves. At the 10−4 M concentration of EMA, floating and dying cells began to be observed the day after the drug was added, and after 72 h the number of cells had fallen to approximately 68% of the number of control cells. When cultured at 10−9–10−5 M EMA, the growth curves of the fibroblasts were almost the same as the curves of the controls at every concentration (Fig. 2a). At the 10−4 M concentration of EM201 as well, floating and dying cells began to be seen the day after addition of the drug, and after 72 h the number of cells had fallen to approximately 75% of the number of control cells. When cultured at 10−9–10−5 M EM201, the growth curves of the fibroblasts were almost the same as the curves of the controls at every concentration (Fig. 2b). No effect of EMA or EM201 on fibroblast growth was observed at 10−9–10−5 M, and the 10−4 M concentration was concluded to be the toxic dose of both drugs. Two cell strains (N-18M, and N-25F) were used for these experiments. Results from the two strains were similar.
Effect of erythromycin A (EMA) and EM201 on the growth of cultured dermal fibroblasts. N-18M and N-25F fibroblast strains were examined. The data from N-18M are shown. The cell growth curve was determined by inoculating 2 × 104 fibroblasts onto 24-well tissue culture plates and adding EMA (a) or EM201 (b). The number of cells was counted 24, 48 and 72 h after the start of incubation with the macrolides
Effects of erythromycin A (EMA) and EM201 on type I collagen production
Since EMA and EM201 had been shown not to affect the growth of fibroblasts, next, we investigated their effect on type I collagen production by dermal fibroblasts. The level of synthesized type I collagen in the culture medium increased in a dose-dependent manner following the addition of EMA at concentrations in the 10−9 M–10−6 M range to the fibroblast cultures (Fig. 3a). Densitometric measurements also showed a dose-dependent increase in the production of type I collagen, and the maximal increase in the level of both the α1 and α2 chains of type I collagen reached 170% of the level in the control in the presence of the 10−7 M concentration of EMA (Fig. 3b, c). The level of synthesized type I collagen in the culture medium also increased in a dose-dependent manner following the addition of EM201 at concentrations in the 10−9–10−6 M range to the fibroblasts cultures (Fig. 4a). Densitometric measurements showed an increase in the production of type I collagen in a dose-dependent manner, and the maximal increase in the level of both the α1 and α2 chains of type I collagen was approximately 230% of their levels in the control in the presence of the 10−7 M concentration of EM201 (Fig. 4b, c).
Effect of erythromycin A (EMA) on production of type I collagen by cultured dermal fibroblasts. N-18M and N-25F fibroblast strains were examined. The cells were incubated for 48 h at 37°C in DMEM containing 0.2% FBS, supplemented with 10−9–10−5 M concentrations of EMA and then cultured for 24 h in DMEM containing 5 μCi/ml 2,3-[3H] proline (Amersham) in the presence of 50 μg/ml l-ascorbic acid 2-phosphate. Labeled proteins secreted into the culture medium were precipitated, and after dissolving in 0.05 M acetic acid and digesting with pepsin, these were subjected to SDS-PAGE (5% polyacrylamide gel containing 3.6 M urea). Radioactive bands were detected by fluorography and the relative amounts of collagen were quantified by densitometry and corrected for cell number. The fluorography of the culture from N-18M fibroblast strain is shown (a). The results of densitometry scanning of the α1 (b) and α2 (c) chains of type I collagen from cultures treated with EMA are expressed as percentages of the values in untreated control cultures. Values shown are means ± SEM of triplicate determination in each experiments. * P < 0.05 versus untreated controls. ** P < 0.01 versus untreated controls
Effect of EM201 on type I collagen production by cultured dermal fibroblasts. N-18M and N-25F fibroblast strains were examined. The cells were incubated for 24 h at 37°C in DMEM containing 0.2% FBS, supplemented with 10−7–10−5 M of EM201. The fluorography was performed as described in Fig. 3. The fluorography of the culture from N-25F fibroblast strain is shown (a). The results of densitometry scanning of the α1 (b) and α2 (c) chains of type I collagen from cultures treated with EM201 are expressed as percentages of the values in the untreated control cultures. Values shown are means ± SEM of triplicate determination in each experiments. * P < 0.05 versus untreated controls. ** P < 0.01 versus untreated controls
Effects of erythromycin A (EMA) and EM201 on type I collagen mRNA levels
Since EMA and EM201 were both shown to increase type I collagen production by fibroblasts, next, we investigated the mRNA levels in order to identify the step in collagen expression at which it was increased. The results of the Northern blot analyses revealed that the addition of EMA in the 10−9–10−6 M concentration range up-regulated the expression of α1 (I) collagen mRNA in a dose-dependent manner (Fig. 5a). Densitometric measurements and digitization of the results with correction for GAPDH values also showed a dose-dependent increase in the levels of α1 (I) collagen mRNA expression, and the expression level increased to a maximum of 150% of the level in the control in the presence of the 10−6 M concentration of EMA (Fig. 5b). The results of the Northern blot analyses revealed that the addition of EM201 in the 10−9–10−6 M concentration range up-regulated the expression of α1 (I) collagen mRNA in a dose-dependent manner (Fig. 5c). Densitometric measurements and digitization of the results with correction for GAPDH values also showed a dose-dependent increase in the α1 (I) collagen mRNA expression level, and the expression level increased to a maximum of 250% of the level of expression in the controls in the presence of the 10−6 M concentration of EM201 (Fig. 5d).
Effect of erythromycin A (EMA) or EM201 on type I collagen mRNA levels in cultured dermal fibroblasts. N-18M and N-25F fibroblast strains were examined. Fibroblasts were cultured for 48 h in DMEM containing 0.2% FBS and 10−9–10−5 M concentrations of EMA, and after isolating the total RNA from the fibroblasts by extraction in guanidium isothiocyanate, Northern blot analyses were performed. a The Northern blot of the culture from N-18M fibroblast strain is shown. b Results of densitometry scanning of α1(I) collagen m-RNA from cells treated with EMA are expressed as a percentage of the value for untreated cells. The quantity of α1(I) collagen m-RNA was normalized to the quantity of GAPDH m-RNA. Values shown are means ± SEM of three independent experiments for each fibroblast strain. * P < 0.05 versus untreated controls. ** P < 0.01 versus untreated controls. Then, fibroblasts were cultured with 10−9–10−5 M concentrations of EM201 for 48 h, and after isolating the total RNA, Northern blot analyses were performed as described above. c The Northern blot of the culture from N-25F fibroblast strain is shown. d The results of densitometry scanning of α1(I) collagen m-RNA from cells treated with EM201 are expressed as described in (b). Values shown are means ± SEM of three independent experiments by each fibroblast strains. * P < 0.05 versus untreated controls ** P < 0.01 versus untreated controls
Effects of erythromycin A (EMA) and EM201 on the α1 (I) collagen gene (COL1A1) promoter activity
It was shown that the increases in type I collagen production by both EMA and EM201 caused by the amounts of type I collagen mRNA to increase to almost the same level. Therefore, we investigated whether the increases occurred at the α1 (I) collagen gene (COL1A1) transcription level.
Following the addition of 10−7 and 10−6 M EMA to the fibroblast cultures, the transcription activity of α1 (I) collagen increased significantly to 170 and 200%, respectively, of the activity in the control cells, as determined by the luciferase assay using the human COL1A1 promoter-reporter gene construct containing 2.3 kb of the 5′ flanking sequences of COL1A1 [17] fused to the luciferase gene (Fig. 6a). Following the addition of 10−7 and 10−6 M EM201 to the fibroblast cultures, α1 (I) collagen transcription activity increased significantly to 150 and 300%, respectively, of the activity in the control cells (Fig. 6b).
Effect of erythromycin A (EMA) and EM201 on α1 (I) collagen gene (COL1A1) promoter activity in cultured dermal fibroblasts. N-1M fibroblast strain was examined. A total of 5 × 105 cells were plated in 6-well tissue culture plates. Two days later, the culture medium was changed to DMEM containing 0.2% FBS with or without the macrolides, and the transfections were performed. The cells were co-transfected with 1.0 μg of the human COL1A1 promoter fused to the luciferase gene (p2.3COL1A1Luc) and 20 ng of phRL-CMV vector. After 48 h, the cells were harvested. Lysates were prepared, and luciferase activity was determined. All experiments were performed in triplicate and repeated at least three times. a Cultures with EMA (10−7, 10−6 M) b Cultures with EM201 (10−7, 10−6 M). * P < 0.05 versus untreated controls. ** P < 0.01 versus untreated controls
Discussion
Macrolides have been reported to exert various pharmacological and antimicrobial activities, including anti-inflammatory activities [16], immuno-modulation of keratinocytes [20] and inhibition of the following: tumor angiogenesis [32], the expression of vascular endothelial growth factor (VEGF) [1], the in vitro proliferation of malignant tumor cells [33], and the growth of fibroblasts [24]. In addition, the erythromycin derivative EM703 has been recently shown to inhibit the development of bleomycin-induced pulmonary fibrosis in the mouse [22] and to inhibit type I collagen production by cultured dermal fibroblasts [17]. In the present study, we investigated the effect of EMA and its new derivative EM201 on type I collagen production by cultured dermal fibroblasts. As a result, we found that EMA and its derivative EM201 have activity that increases the expression of type I collagen by cultured normal human dermal fibroblasts. Various factors controlling collagen production from fibroblasts are widely recognized. It is known that the expression of the type I collagen gene is inhibited when fibroblasts are exposed to TNF-α [31], IFN-γ [5], EGF [21], glucocorticoids [10], or transformed with viruses [28] or chemicals such as TPA [12]. On the other hand, expression of the type I collagen gene is induced when fibroblasts are exposed to ascorbic acid [9], TGF-β [25, 26], IL-6 [6] and also to hypoxia [7].
In this study, EMA increased α1 (I) and α2 (I) collagen production by a maximum of approximately 1.7-fold, and it increased the mRNA level of α1 (I) collagen by a maximum of approximately 1.5-fold. It was also found to have efficacy that increased the transcription level of α1 (I) collagen by a maximum of twofold. On the other hand, the effect of its new derivative, EM201, in increasing expression was more potent. At the protein level, it increased the production of α1 (I) and α2 (I) collagen by a maximum of 2.2-fold, and at the mRNA level it increased α1 (I) collagen mRNA level by a maximum of approximately 2.5-fold. It also increased the production at the transcription level by a maximum of approximately threefold. Based on these results, it appears that regulation of the increase in type I collagen production by both EMA and EM201 is achieved almost entirely at the transcription level, and there appears to be a little increase as a result of an effect on mRNA stability or translation. EMA and EM201 increased type I collagen production and gene expression in a concentration-dependent manner, from 10−9 to 10−7 M or 10−9 to 10−6 M. At higher concentrations of 10−6 or 10−5 M, the rate of increase by both declined. At these concentrations, EMA and EM201 did not affect cell growth capacity, and these concentrations were not toxic doses (Fig. 2). These findings suggest that the peak concentrations of EMA and EM201 that activate expression of the type I collagen gene lies between 10−7 and 10−6 M.
We added EMA and EM201 to the cultured fibroblasts, incubated them, and examined their effect on the ability to produce collagen. In this study, we used a serum concentration of 0.2%, selected because the activity that increased collagen production was clearly shown at 0.2% than when we added reagents under 10 and 1% serum conditions in a preliminary experiment (data not shown). Efficacy was not observed when the fibroblasts were cultured under high serum concentrations, because the serum activates collagen production [3] and the values were masked by it.
In terms of clinical significance, the maximal blood concentration of a single 200 mg tablet of erythromycin administered orally was approximately 1 × 10−6 M in general clinical practice (Abbott Japan, company data). The fact that the concentration of EMA that significantly increased collagen production in this study was at least 10−6 M or less and that EM201 also significantly increased collagen production at least at 10−6 M or less mean that in the future, it may be possible to use them as drugs to treat atrophic skin diseases or wrinkles, in which the fiber component of skin is decreased.
In this study, we investigated the effects of erythromycin A (EMA) and its new derivative EM201 on type I collagen production by cultured dermal fibroblasts. Collagen fiber is constructed with not only type I collagen as the principal component, but also other types of collagens such as types III, V and VI collagen. It is known that the expression of types I and III collagen is regulated in a parallel manner in most cases, whereas type VI collagen is regulated independently from types I and III collagen in some events [19]. To get a better understanding of the role of both macrolides on the regulation of the amount of collagen fibers in the dermis, we would like to investigate the effects of both macrolides on the production of other types of dermal collagen in further experiment. Further studies also have to show the beneficial effects of the macrolides in more complex culture systems, such as three-dimensional gel, artificial skin or skin explant cultures.
References
Aoki D, Ueno S, Kubo F, Oyama T, Sakuta T, Matsushita K, Maruyama I, Aikou T (2005) Roxithromycin inhibits angiogenesis of human hepatoma cells in vivo by suppressing VEGF production. Anticancer Res 25:133–138
Arcari P, Martinelli R, Salvatore F (1984) The complete sequence of a full length cDNA for human liver glyceraldehyde-3-phosphate dehydrogenase: evidence for multiple mRNA species. Nucleic Acids Res 12:9179–9189
Bembenek ME, Willis DH Jr, Liberti JP (1982) The effect of insulin on collagen production in isolated chondrosarcoma chondrocytes. Biochem Biophys Res Commun 106:338–345
Chu ML, Myers JC, Bernard MP, Ding JF, Ramirez F (1982) Cloning and characterization of five overlapping cDNAs specific for the human pro alpha 1(I) collagen chain. Nucleic Acids Res 10:5925–5934
Czaja MJ, Weiner FR, Eghbali M, Giambrone MA, Eghbali M, Zern MA (1987) Differential effects of gamma interferon on collagen and fibronectin gene expression. J Biol Chem 262:13348–13351
Duncan MR, Berman B (1991) Stimulation of collagen and glycosaminoglycan production in cultured human adult dermal fibrolasts by recombinant human interleukin 6. J Invest Dermatol 97:686–692
Falanga V, Martin TA, Takagi H, Kirsner RS, Helfman T, Pardes J, Ochoa MS (1993) Low oxygen tension increases mRNA levels of alpha 1 (I) procollagen in human dermal fibroblasts. J Cell Physiol 157:408–412
Fleischmajer R, Perlish JS, Krieg T, Timple R (1981) Variability in collagen and fibronectin synthesis by scleroderma fibroblasts in primary culture. J Invest Dermatol 76:400–403
Geesin JC, Darr D, Kaufman R, Murad S, Pinnell SR (1988) Ascorbic acid specifically increases type I and type III procollagen messenger RNA levels in human skin fibroblast. J Invest Dermatol 90:420–424
Hamalainen L, Oikarinen J, Kivirikko KI (1985) Synthesis and degradation of type I procollagen mRNAs in cultured human skin fibroblasts and the effect of cortisol. J Biol Chem 260:720–725
Hata R, Kurata S, Shinkai H (1988) Existence of malfunctioning pro alpha2(I) collagen genes in a patient with a pro alpha2(II)-chain-defective variant of Ehlers–Danlos syndrome. Eur J Biochem 174:231–237
Hatamochi A, Aumailley M, Mauch C, Chu ML, Timpl R, Krieg T (1989) Reguration of collagen VI expression in fibroblasts: effect of cell density, cell–matrix interactions, and chemical transformation. J Biol Chem 264:3494–3499
Hatamochi A, Arakawa M, Takeda K, Ueki H (1994) Activation of fibroblast proliferation by Werner’s syndrome fibroblast-conditioned medium. J Dermatol Sci 7:210–216
Hatamochi A, Kuroda K, Shinkai H, Kohma H, Oishi Y, Inoue S (1998) Regulation of matrix metalloproteinase (MMP) expression in cutis laxa fibroblasts: upregulation of MMP-1, MMP-3 and MMP-9 genes but not of the MMP-2 gene. Br J Dermatol 38:757–762
Hildebran JN, Absher M, Low RB (1983) Altered rates of collagen synthesis in in vitro aged human lung fibroblasts. In Vitro 19:307–314
Ianaro A, Ialenti A, Maffia P, Sautebin L, Rombola L, Carnuccio R, Iuvone T, D’Acquisto F, Di Rosa M (2000) Anti-inflammatory activity of macrolide antibiotics. J Pharmacol Exp Ther 292:156–163
Ikeda H, Sunazuka T, Suzuki H, Hamasaki Y, Yamazaki S, Omura S, Hatamochi A (2008) EM703, the new derivate oferythromycin, inhibits transcription of type I collagen in normal and scleroderma fibroblast. J Dermatol Sci 49:195–205
Jimenez SA, Hitraya E, Varga J (1996) Pathogenesis of scleroderma: collagen. Rheum Dis Clin North Am 22:647–674
Kitamura Y, Namikawa H, Hayashi S, Yoshida T, Suzuki T, Hamasaki Y, Yamazaki S, Hatamochi A (2009) Effects of UVA irradiation following treatment with 8-methoxypsoralen on type I and type III collagen synthesis in normal and scleroderma fibroblast cultures. Arch Dermatol Res (in press)
Kobayashi M, Shimauchi T, Hino R, Tokura Y (2004) Roxithromycin downmodulates Th2 chemokine production by keratinocytes and chemokine receptor expression on Th2 cells: its dual inhibitory effects on the ligands and the receptors. Cell Immunol 228:27–33
Kurata S, Hata R (1991) Epidermal growth factor inhibits transcription of type I collagen genes and production of type I collagen in cultured human skin fibroblasts in the presence and absence of l-ascorbic acid 2-phosphate, a long-acting vitamin C derivative. J Biol Chem 266:9997–10003
Li YJ, Azuma A, Usuki J, Abe S, Matsuda K, Sunazuka T, Shimizu T, Hirata Y, Inagaki H, Kawada T, Takahashi S, Kudoh S, Omura S (2006) EM703 improves bleomycin-induced pulmonary fibrosis in mice by the inhibition of TGF-β signaling in lung fibroblasts. Respir Res 7:1–13
Mori K, Hatamochi A, Ueki H, Olsen A, Jimenez SA (1996) The transcription of human α1(I) procollagen gene (COL 1 A 1) is suppressed by tumor necrosis factor-α through proximal short promoter elements: evidence for suppression mechanisms mediated by two nuclear factor binding sites. Biochem J 319:811–816
Nonaka M, Pawankar R, Tomiyama S, Yagi T (1999) A macrolide antibiotic roxithromycin inhibits the growth of nasal polyp fibroblasts. Am J Rhinol 13:267–272
Raghow R, Postlethwaite AE, Keski-Oja J, Moses HL, Kang AH (1987) Transforming growth factor-beta increases steady state levels of type I procollagen and fibronectin messenger RNAs posttranscriptionally in cultured human dermal fibrobrasts. J Clin Invest 79:1285–1288
Roberts AB, Sporn MB, Assoian RK, Smith JM, Roche NS, Wakefield LM, Heine UI, Liotta LA, Falanga V, Kehrl JH et al (1986) Transforming growth factor type beta: rapid induction of fibrosis and angiogenesis in vivo and stimulation of collagen formation in vitro. Proc Natl Acad Sci USA 83:4167–4171
Saitta B, Gaidarova S, Cicchillitti L, Jimenez SA (2000) CCAAT binding transcription factor binds and regulates human COL1A1 promoter activity in human dermal fibroblasts: demonstration of increased binding in systemic sclerosis fibroblasts. Arthritis Rheum 43:2219–2229
Sandmeyer S, Gallis B, Bornstein P (1981) Coordinate transcriptional regulation of type I procollagen genes by Rous sarcoma virus. J Biol Chem 256:5022–5028
Sato M, Shegogue D, Hatamochi A, Yamazaki S, Trojanowska M (2004) Lysophosphatidic acid inhibits TGF-beta-mediated stimulation of type I collagen mRNA stability via an ERK-dependent pathway in dermal fibroblasts. Matrix Biol 23:353–361
Shuster S, Black MM, Mcvitie E (1975) The influence of age and sex on skin thickness, skin collagen and density. Br J Dermatol 93:639–642
Solis-Herruzo JA, Brenner DA, Chojkier M (1988) Tumor necrosis factor alpha: inhibits collagen gene transcription and collagen systhesis in cultured human fibroblasts. J Biol Chem 263:5841–5845
Yatsunami J, Tsuruta N, Hara N, Hayashi S (1998) Inhibition of tumor angiogenesis by roxithromycin, a 14-membered ring macrolide antibiotic. Cancer Lett 131:137–143
Yatsunami J, Fukuno Y, Nagata M, Tominaga M, Aoki S, Tsuruta N, Kawashima M, Taniguchi S, Hayashi S (1999) Antiangiogenic and antitumor effects of 14-membered ring macrolides on mouse B16 melanoma cells. Clin Exp Metastasis 17:361–367
Yoshida K, Sunazuka T, Nagai K, Sugawara A, Cho A, Nagamitsu T, Harigaya Y, Otoguro K, Akagawa (2005) Macrolides with promotive activity of monocyte to macrophage differentiation. J Antibiot 58:79–81
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Namikawa, H., Sunazuka, T., Kitamura, Y. et al. Effect of erythromycin A and its new derivative EM201 on type I collagen production by cultured dermal fibroblasts. Arch Dermatol Res 302, 341–348 (2010). https://doi.org/10.1007/s00403-009-0977-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00403-009-0977-z