Abstract
Aquaporin-3 (AQP3) is a water/glycerol transporting protein expressed strongly at the plasma membrane of keratinocytes. There is evidence for involvement of AQP3-facilitated water and glycerol transport in keratinocyte migration and proliferation, respectively. Here, we investigated the involvement of AQP3 in keratinocyte differentiation. Studies were done using AQP3 knockout mice, primary cultures of mouse keratinocytes (AQP3 knockout), neonatal human keratinocytes (AQP3 knockdown), and human skin. Cells were cultured with high Ca2+ or 1α,25-dihydroxyvitamin D3 (VD3) to induce differentiation. The expression of differentiation marker proteins and differentiating responses were comparable in control and AQP3-knockout or knockdown keratinocytes. Topical application of all-trans retinoic acid (RA), a known regulator of keratinocyte differentiation and proliferation, induced comparable expression of differentiation marker proteins in wildtype and AQP3 null epidermis, though with impaired RA-induced proliferation in AQP3 null mice. Immunostaining of human and mouse epidermis showed greater AQP3 expression in cells undergoing proliferation than differentiation. Our results showed little influence of AQP3 on keratinocyte differentiation, and provide further support for the proposed involvement of AQP3-facilitated cell proliferation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The aquaporins (AQPs) are a family of small, integral membrane proteins that transport water and in some cases small solutes such as glycerol, termed aquaglyceroporins (AQPs 3, 7 and 9) [14, 23]. Phenotype analysis of AQPs knockout mice has revealed multiple physiological roles of AQPs. AQP-facilitated water transport is involved in the urinary concentrating mechanism, epithelial fluid secretion, brain edema, neural signal transduction, and cell migration [24]. Aquaglyceroporin-facilitated glycerol transport is involved in metabolic pathways, such as adipose AQP7 in obesity [10] and AQP9 in glycerol metabolism [19].
In mammalian epidermis, AQP3 is strongly expressed in plasma membranes of keratinocytes [15, 21]. AQP3-deficient mouse skin has reduced stratum corneum water content and elasticity compared to that of wildtype mice [8, 15]. These defects were found to result from deficiency of AQP3-facilitated glycerol transport, reducing stratum corneum and epidermal cell glycerol content and hence humectant properties [9]. Recent data implicated AQP3 function as a novel determinant in cutaneous wound healing and tumorigenesis. AQP3-facilitated water transport is involved in cell migration, accelerating wound healing [11]. AQP3-facilitated glycerol transport is involved in keratinocyte proliferation, in which AQP3 knockout mice are resistant to tumor formation by a mechanism that may involve reduced cell glycerol content and ATP energy for cell growth and tumorigenesis [12].
A study using mouse primary cultured keratinocytes has also suggested the involvement of AQP3 in keratinocyte differentiation [3]. AQP3 overexpression increased the expression of differentiation markers, though decreased that of a proliferation marker. Phosphatidylglycerol (PG), which is involved in keratinocyte differentiation and thought to be produced by AQP3-mediated glycerol and phospholipase D2 (PLD2), inhibited DNA synthesis, suggesting a PLD2/AQP3 ‘signaling module’ as a regulator of keratinocyte differentiation. Involvement of AQP3 in keratinocyte differentiation would represent a major new role of AQP3 in skin, with potentially broad consequences regarding normal epidermal differentiation and disease pathophysiology.
The aim of this study is to investigate the involvement of AQP3 in keratinocyte differentiation. We utilized AQP3 knockout mice and primary keratinocyte cultures derived therefrom, neonatal human keratinocytes (NHK) after AQP3 knockdown, and human skin. Keratinocyte differentiation was induced in cell cultures by treatments with Ca2+ or VD3 [2, 5], and mouse skin was treated with all-trans retinoic acid (RA), a known regulator of keratinocyte differentiation and proliferation [6]. To assess keratinocyte differentiation, we measured the expression of differentiation marker proteins, cornified cell envelope (CE) formation, and transglutaminase (TGase) activity. The data showed no effect of AQP3 on keratinocyte differentiation markers or the response in each of these systems, providing strong evidence that keratinocyte differentiation does not depend on AQP3. Furthermore, immunostaining of mouse and human skin showed AQP3 expression in cells undergoing proliferation rather than differentiation, supporting the involvement of AQP3 in keratinocyte proliferation rather than differentiation.
Materials and methods
Mice
AQP3 null mice (hairless and CD1 genetic background) were generated by targeted gene disruption as described [16]. All animal experiments were approved by the Committee on Animal Research of Kyoto University.
Primary culture of mouse keratinocytes
Full-thickness skin from 1 to 3-day-old mice was incubated in dispase (Invitrogen Life Technologies, Carlsbad, CA, USA) for 7 h at 4°C. The epidermis was separated from the dermis, cut into fragments, and incubated in 0.25% trypsin/0.1% EDTA for 10 min. Keratinocytes were seeded on collagen type I plates (BD Biosciences, Franklin Lakes, NJ, USA) at a density of 105 per cm2, and cultured in keratinocyte growth medium containing 0.15 mM calcium (Cambrex, Walkersville, MD, USA). To induce cell differentiation, keratinocytes were cultured with 1.5 mM calcium for 4 days (high Ca) or 1 μM 1α,25-dihydroxyvitamin D3 for 3 days (VD3) after confluence.
CE assay was performed as described [22]. Briefly, cells were harvested by trypsinization, and 1 × 105 cells were washed twice with phosphate-buffered saline (PBS) (pH 7.5) and treated with 50 μl of 2% sodium dodecyl sulfate (SDS), containing 20 mM dithiothreitol (DTT), and then heat-treated for 5 min at 100°C. Detergent- and reducing agent-resistant CEs were counted in a hemocytometer under phase optics. TGase activity was measured by protein-bound fluorescence after incorporation of monodansylcadaverine into casein (Sigma, St Louis, MO, USA) as described [17].
Human keratinocyte cell cultures
Neonatal human keratinocytes (Kurabo industries Ltd, Osaka, Japan) were grown in keratinocyte growth medium containing 0.15 mM calcium (Cascade Biologics. Portland, OR, USA). NHK were transfected with AQP3 siRNA or RISC-free siRNA (Dharmacon, Lafayette, CO, USA) at 40–50% confluence using Lipofectamine 2000™ (Invitrogen). To induce cell differentiation, keratinocytes were cultured in 1.5 mM calcium (high Ca) for 6 days after confluence. AQP3 expression was assessed by immunofluorecence using a polyclonal AQP3 antibody (Chemicon, Temecula, CA, USA, 1:200) and anti-rabbit Cy3-conjugated IgG secondary antibody (Sigma).
Retinoic acid-induced cell proliferation and differentiation in mouse epidermis
Dorsal skin of mice was treated with four applications of all-trans retinoic acid (Sigma, 0.0125%, 100 μl ethanol) or vehicle, and skin was excised at 24 h after final treatment. For measurement of epidermal cell proliferation, mice were injected intraperitoneally with BrdU (100 μg/g body weight; Sigma-Aldrich) at 1 h prior to sacrifice. Paraffin-embedded sections were stained with hematoxylin and eosin, or anti-BrdU antibody (ABcam, Cambridge, MA, USA, 1:20) with biotinylated anti-rat IgG and HRP-conjugated ABC reagent (Vector Laboratories Inc.). BrdU positive cells were counted, with >200 basal cells examined per mouse.
For immunoblot analysis, epidermal sheets were separated from dermis by heat-split, and homogenized in lysis buffer including 0.1 M Tris hydroxymethyl aminomethane–HCl (pH 9), 6 M urea, 1% 2-mercaptoethanol, 1% SDS, 1 mM EDTA and 0.1 mM PMSF. The supernatant (10,000g, 10 min, 4°C) was used for immunoblotting as described below.
Immunoblot analysis
Keratinocytes were lysed and homogenated in cell lysis buffer (Cell Signaling Technology, Boston, MA, USA). The supernatant (10,000g, 10 min, 4°C) was used for immunoblotting with primary antibodies against involucrin (Covance for mice, Emeryville, CA, USA, 1:1,000; Abcam for human 1:1,000), filaggrin (Covance 1:1,000), loricrin (Covance 1:1,000), keratin 5 (Lab Vision, Fremont, CA, USA, 1:500), keratin 10 (Chemicon 1:1,000), keratin 14 (Chemicon 1:200) and β-actin (Sigma 1:2,000). Horseradish peroxidase-conjugated secondary anti-rabbit IgG antibody (Cell Signaling Technology) or anti-mouse IgG antibody (DAKO, Carpinteria, CA, USA) was used for detection by enhanced chemiluminescence (Amersham Pharmacia, Piscataway, NJ, USA).
Immunostaining of human and mice skin
After receiving informed consent, we obtained abdominal skin samples from normal human adults undergoing plastic surgery. Tissues were fixed in formalin for paraffin sectioning. After deparaffinization, section was treated in sodium citrate buffer (10 mM sodium citrate, pH 6.0) for 20 min at 95–100°C for antigen retrieval, and stained with anti-keratin 14 (Chemicon 1:10), keratin 10 (Chemicon 1:100), keratin 6 (Lab Vision 1:100) or AQP3 (Chemicon 1:200).
Statistical analysis
Statistical analysis was performed with a two-tailed indirect Student’s t test or ANOVA.
Results
Comparable cell differentiation in control and AQP3-deficient keratinocytes
To investigate if AQP3 gene deletion affected keratinocyte differentiation, we used primary cultured keratinocytes from epidermis of wildtype and AQP3 null mice. Keratinocytes were cultured with low Ca2+ (0.15 mM) until confluence, and then treated with high Ca2+ (1.5 mM) for 4 days or VD3 for 3 days to induce differentiation. Involucrin, a marker of intermediate differentiation [5], was increased with high Ca2+ and VD3 in both wildtype and AQP3 null keratinocyte (Fig. 1a). Keratin 10, a marker of early differentiation, was also increased with high Ca2+. A decrease was found in keratin 5, a marker of basal proliferating cells, indicated suppressed proliferation in both wildtype and AQP3 null keratinocytes. Figure 1b shows a summary of the results, showing comparable changes in differentiation markers in wildtype and AQP3 null keratinocytes, suggesting AQP3-independent keratinocyte differentiation in response to high Ca2+ and VD3 treatments. To compare high Ca2+-induced keratinocyte differentiation between wildtype and AQP3 null keratinocytes further, CE formation and TGase activity were assayed. We found comparable increases in CE formation and TGase activity in response to high Ca2+, indicating no effect of AQP3 on high Ca2+-induced differentiation (Fig. 1c, d).
Comparable cell differentiation induced by high concentrated Ca2+ and VD3 in wildtype and AQP3-deficient mouse primary cultured keratinocytes. a Immunoblot analysis using antibodies against involucrin, keratin 10, keratin 5, and β-actin. Keratinocytes from wildtype and AQP3 null mouse epidermis were cultured with 0.15 mM Ca2+ for 4 days (control). After confluence cells were treated with 1.5 mM Ca2+ for 4 days (high Ca) or 1 mM VD3 for 3 days (VD3). b Immunoblots were quantified as the ratio to β-actin using NIH image. The values shown are the mean ± SEM of 3–4 separate experiments performed in duplicate (*P < 0.01). c CE formation and d TGase activity. Keratinocytes were cultured with control or high Ca2+ medium described in (a). Data are expressed as the ratio to wildtype control (n = 4, *P < 0.01)
Keratinocyte differentiation was also studied in neonatal human keratinocytes (NHKs). To knockdown AQP3 expression, NHKs were transfected with siRNA-AQP3 or RISC-free siRNA at 40–50% confluence, and then cultured in low Ca2+ media until confluence (low Ca2+). To induce differentiation, NHKs were treated with 1.5 mM Ca2+ medium for 6 days (high Ca2+). Immunostaining assay confirmed AQP3 expression in confluent and high Ca2+-induced differentiated NHKs (Fig. 2a, upper). Transfection of siRNA-AQP3 consistently reduced AQP3 protein expression by ~95% (Fig. 2a, lower). In this setting, differentiation markers were compared between control and AQP3 knocked down cells by immunobloting. We found no significant differences in the increases of involucrin, loricrin and keratin 10, or the decrease in keratin 5 in high Ca2+ treated control and AQP3 knockdown NHKs (Fig. 2b). As summarized in Fig. 2c, comparable increases in differentiation markers were found in control and AQP3 knockdown NHKs, providing evidence against involvement of AQP3 in keratinocyte differentiation.
Cell differentiation induced by Ca2+ in AQP3-knock-down human keratinocytes. a AQP3 immunostaining of neonatal human keratinocytes (control) and AQP3-siRNA-treated keratinocytes (AQP3 RNAi). Keratinocytes were cultured with 0.15 mM Ca2+ for 4 days (low Ca), and replaced with 1.5 mM Ca2+ and cultured for 6 days (high Ca). Bar 20 μm. b Immunoblot analysis using antibodies against involucrin, loricrin, keratin 10, keratin 5, and β-actin in RISC-free siRNA-treated (control) and AQP3-siRNA-treated (RNAi) keratinocyte. c Immunoblots were quantified as the ratio to β-actin using NIH image. The values shown are the mean ± SEM of 4–5 separate experiments performed in three separate sets of experiments (*P < 0.01)
RA induces comparable epidermal differentiation in wildtype and AQP3 null skin
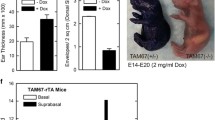
To investigate the role of AQP3 in keratinocyte differentiation and proliferation in vivo, dorsal skin of mice was topically treated with RA [6]. RA is potent stimulator of keratinocyte proliferation, which is mediated by heparin-binding epidermal growth factor-like growth factor [18, 25]. RA was also found to modulate differentiation, as seen as an increase in involucrin in vivo, consistent with our findings here, though it suppresses terminal differentiation in cultured cells [7, 20]. Figure 3a shows greater hyperplasia after four RA treatments in wildtype than in AQP3 null epidermis. To account for the difference in hyperplasia, epidermal cell proliferation was significantly greater in wildtype mice than in AQP3 null mice, as shown by the greater percentage of BrdU positive epidermal cells following RA treatment (Fig. 3b). To further study RA-mediated cell differentiation, the expressions of several differentiation marker proteins were examined by immunoblotting. Despite the marked differences in the cell proliferation, RA treatment produced comparable expression in involucrin, loricrin and filaggrin between wildtype and AQP3 null epidermis, indicating comparable differentiation responses to RA application (Fig. 3c, upper). RA altered the expression of keratin 5 and 14, which is likely related to the involvement of AQP3 in keratinocyte proliferation rather than differentiation (Fig. 3c, lower).
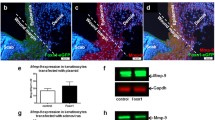
Retinoic acid-induced cell proliferation and differentiation in AQP3 null epidermis. Dorsal skin of wildtype and AQP3 null mice were treated topically with vehicle or four applications of retinoic acid (RA). a Hematoxylin and eosin staining of skin treated with RA. Bar 50 μm. b (left) BrdU staining of epidermis following four RA applications. (right) Percentage of BrdU positive cells in epidermal basal layer (SE n = 3, *P < 0.05). c Immunoblot analysis using antibodies against involucrin, loricrin, filaggrin, keratin14, keratin 5 and β-actin. Epidermis was excised at 24 h after final treatment with vehicle or RA. d AQP3 immunostaining of epidermis treated with vehicle or four RA applications. Bar 20 μm. e Immunostaining of AQP3 (red) and keratin 14, 10 or 6 (green) in RA-treated epidermis of wildtype and AQP3 null mice. Bar 20 μm
AQP3 is expressed more strongly in the basal than the upper layer of differentiated keratinocyte in mouse epidermis [15]. To further investigate the possible involvement of AQP3 in keratinocyte differentiation, AQP3 localization was examined in RA-treated epidermis. As shown in Fig. 3d, RA treatment increased AQP3 expression compared to control epidermis, and as found previously in human keratinocytes [1, 4]. AQP3 was found to be expressed not only in basal layer but also in the middle layer of epidermis in RA treated skin. Co-labeling with anti-keratin antibodies showed that AQP3 expression was greater in proliferating, keratin 14 positive cells, than in differentiating, keratin 10 positive cells (Fig. 3e). AQP3 was also found to be expressed in keratin 6 positive cells, hyperproliferative cells, in the upper layer of RA treated epidermis. These in vivo experiments suggest that AQP3 facilitates keratinocyte proliferation rather than differentiation.
Localization of AQP3 in normal human epidermis
Last, we examined AQP3 localization in human skin from abdomen with normal structure (Fig. 4a). As shown in Fig. 4b, AQP3 was expressed more strongly in basal and suprabasal layers than in upper layers of normal epidermis. Co-labeling showed greater AQP3 localization in keratin-14 positive cells, a marker of basal cell proliferation (Fig. 4b). AQP3 was partly expressed in the lower part of keratin 10 and involucrin positive cell layer, early differentiating cells. These observations further support the involvement of AQP3 in cell proliferation rather than differentiation.
Discussion
We used several biochemical and immunohistochemical approaches to examine the involvement of AQP3 in keratinocyte differentiation. In all assays using different systems, including genetically modified AQP3 null mice, we found no effect of AQP3 expression on keratinocyte differentiation. First, we found no significant differences in the expression patterns of differentiation marker proteins, CE formation, and TGase activity between keratinocytes from control and AQP3 deficient mice during in vitro differentiation induced by high Ca2+- or VD3. Second, control and AQP3 knock-down human keratinocytes equally expressed differentiation markers upon high Ca2+-treatment. Third, RA-induced cell differentiation did not differ in intact epidermis from wildtype and AQP3 null mice, though impaired cell proliferation was found in RA-treated AQP3 null epidermis. The impaired RA-mediated proliferation in AQP3 deficiency, with comparable differentiation, provides evidence that AQP3 is involved in proliferation, but not differentiation, during hyperproliferation. The data are consistent with previous results showing impaired mitogen induced cell proliferation in AQP3 deficient keratinocyte following treatment with phorbol ester (TPA), EGF and wounding [11, 12]. Last, immunostaining of mouse and human epidermis indicated greater AQP3 expression in cells undergoing proliferation than differentiation. The RA-induced increase in AQP3 expression, which localized mainly to proliferating cells, supports the involvement of AQP3 in proliferation.
Our data do not support recent reports using mouse keratinocytes suggesting the requirement of AQP3 in keratinocyte differentiation. Zheng et al. [26] reported colocalization of AQP3 with phospholipase D2 (PLD2) in caveolin-rich membrane microdomains in keratinocytes. In a separate report, the same group found that glycerol was utilized by PLD2 to generate phosphatidylglycerol (PG), which was modulated by the differentiation agent high Ca2+, suggesting that PG is an important signaling lipid for keratinocyte differentiation [27]. A more recent study reported that inhibition of AQP3 glycerol transport by acidic medium reduced PG synthesis [3]. From these results the authors suggested that AQP3 participates with PLD2 in a glycerol-phosphotidylglycerol signalling module, which promote keratinocyte differentiation. They showed that AQP3 overexpression stimulated differentiation responses such as promoter activity of keratin 10 and involucrin. However, our present study utilizing multiple systems found no effect of AQP3 expression on keratinocyte differentiation responses.
In conclusion, our data showed little involvement of AQP3 in keratinocyte differentiation. Our findings and previous studies [13] suggest that AQP3 plays an important role in keratinocyte proliferation and migration, rather than in differentiation, in epidermal homeostasis and skin disorders such as tumorigenesis and wound healing. Further work is needed to elucidate the precise mechanism of AQP3-mediated cell proliferation, which is likely of relevance to human skin disorders associated with epidermal hyperproliferation and inflammation.
Abbreviations
- AQP:
-
Aquaporin
- RA:
-
All-trans retinoic acid
- VD3 :
-
1α,25-Dihydroxyvitamin D3
References
Bellemère G, Von Stetten O, Oddos T (2008) Retinoic acid increases aquaporin 3 expression in normal human skin. J Invest Dermatol 128:542–548
Bikle DD, Ng D, Tu CL, Oda Y, Xie Z (2001) Calcium- and vitamin D-regulated keratinocyte differentiation. Mol Cell Endocrinol 177:161–171. doi:10.1016/S0303-7207(01)00452-X
Bollag WB, Xie D, Zheng X, Zhong X (2007) A potential role for the phospholipase D2-aquaporin-3 signaling module in early keratinocyte differentiation: production of a phosphatidylglycerol signaling lipid. J Invest Dermatol 127:2823–2831. doi:10.1038/sj.jid.5700692
Cao C, Wan S, Jiang Q, Amaral A, Lu S, Hu G, Bi Z, Kouttab N, Chu W, Wan Y (2008) All-trans retinoic acid attenuates ultraviolet radiation-induced down-regulation of aquaporin-3 and water permeability in human keratinocytes. J Cell Physiol 215:506–516. doi:10.1002/jcp.21336
Eckert RL, Crish JF, Robinson NA (1997) The epidermal keratinocyte as a model for the study of gene regulation and cell differentiation. Physiol Rev 77:397–424
Fisher GJ, Voorhees JJ (1996) Molecular mechanisms of retinoid actions in skin. FASEB J 10:1002–1013
Griffiths CE, Rosenthal DS, Reddy AP, Elder JT, Astrom A, Leach K, Wang TS, Finkel LJ, Yuspa SH, Voorhees JJ et al (1992) Short-term retinoic acid treatment increases in vivo, but decreases in vitro, epidermal transglutaminase-K enzyme activity and immunoreactivity. J Invest Dermatol 99:283–288. doi:10.1111/1523-1747.ep12616626
Hara M, Ma T, Verkman AS (2002) Selectively reduced glycerol in skin of aquaporin-3-deficient mice may account for impaired skin hydration, elasticity, and barrier recovery. J Biol Chem 277:46616–46621. doi:10.1074/jbc.M209003200
Hara M, Verkman AS (2003) Glycerol replacement corrects defective skin hydration, elasticity, and barrier function in aquaporin-3-deficient mice. Proc Natl Acad Sci USA 100:7360–7365. doi:10.1073/pnas.1230416100
Hara-Chikuma M, Sohara E, Rai T, Ikawa M, Okabe M, Sasaki S, Uchida S, Verkman AS (2005) Progressive adipocyte hypertrophy in aquaporin-7-deficient mice: adipocyte glycerol permeability as a novel regulator of fat accumulation. J Biol Chem 280:15493–15496. doi:10.1074/jbc.C500028200
Hara-Chikuma M, Verkman AS (2008) Aquaporin-3 facilitates epidermal cell migration and proliferation during wound healing. J Mol Med 86:221–231. doi:10.1007/s00109-007-0272-4
Hara-Chikuma M, Verkman AS (2008) Prevention of skin tumorigenesis and impairment of epidermal cell proliferation by targeted aquaporin-3 gene disruption. Mol Cell Biol 28:326–332. doi:10.1128/MCB.01482-07
Hara-Chikuma M, Verkman AS (2008) Roles of aquaporin-3 in epidermis. J Invest Dermatol 128:2145–2151. doi:10.1038/jid.2008.70
King LS, Kozono D, Agre P (2004) From structure to disease: the evolving tale of aquaporin biology. Nat Rev Mol Cell Biol 5:687–698. doi:10.1038/nrm1469
Ma T, Hara M, Sougrat R, Verbavatz JM, Verkman AS (2002) Impaired stratum corneum hydration in mice lacking epidermal water channel aquaporin-3. J Biol Chem 277:17147–17153. doi:10.1074/jbc.M200925200
Ma T, Song Y, Yang B, Gillespie A, Carlson EJ, Epstein CJ, Verkman AS (2000) Nephrogenic diabetes insipidus in mice lacking aquaporin-3 water channels. Proc Natl Acad Sci USA 97:4386–4391. doi:10.1073/pnas.080499597
Puszkin EG, Raghuraman V (1985) Catalytic properties of a calmodulin-regulated transglutaminase from human platelet and chicken gizzard. J Biol Chem 260:16012–16020
Rittié L, Varani J, Kang S, Voorhees JJ, Fisher GJ (2006) Retinoid-induced epidermal hyperplasia is mediated by epidermal growth factor receptor activation via specific induction of its ligands heparin-binding EGF and amphiregulin in human skin in vivo. J Invest Dermatol 126:732–739. doi:10.1038/sj.jid.5700202
Rojek A, Praetorius J, Frøkjaer J, Nielsen S, Fenton RA (2008) A current view of the mammalian aquaglyceroporins. Annu Rev Physiol 70:301–327. doi:10.1146/annurev.physiol.70.113006.100452
Rosenthal DS, Griffiths CE, Yuspa SH, Roop DR, Voorhees JJ (1992) Acute or chronic topical retinoic acid treatment of human skin in vivo alters the expression of epidermal transglutaminase, loricrin, involucrin, filaggrin, and keratins 6 and 13 but not keratins 1, 10, and 14. J Invest Dermatol 98:343–350. doi:10.1111/1523-1747.ep12499802
Sougrat R, Morand M, Gondran C, Barré P, Gobin R, Bonté F, Dumas M, Verbavatz JM (2002) Functional expression of AQP3 in human skin epidermis and reconstructed epidermis. J Invest Dermatol 118:678–685. doi:10.1046/j.1523-1747.2002.01710.x
Takahashi H, Ibe M, Kinouchi M, Ishida-Yamamoto A, Hashimoto Y, Iizuka H (2003) Similarly potent action of 1, 25-dihydroxyvitamin D3 and its analogues, tacalcitol, calcipotriol, and maxacalcitol on normal human keratinocyte proliferation and differentiation. J Dermatol Sci 31:21–28. doi:10.1016/S0923-1811(02)00136-6
Verkman AS, Mitra AK (2000) Structure and function of aquaporin water channels. Am J Physiol Renal Physiol 278:F13–F28
Verkman AS (2005) Novel roles of aquaporins revealed by phenotype analysis of knockout mice. Rev Physiol Biochem Pharmacol 155:31–55. doi:10.1007/3-540-28217-3_2
Xiao JH, Feng X, Di W, Peng ZH, Li LA, Chambon P, Voorhees JJ (1999) Identification of heparin-binding EGF-like growth factor as a target in intercellular regulation of epidermal basal cell growth by suprabasal retinoic acid receptors. EMBO J 18:1539–1548. doi:10.1093/emboj/18.6.1539
Zheng X, Bollinger Bollag W (2003) Aquaporin 3 colocates with phospholipase d2 in caveolin-rich membrane microdomains and is downregulated upon keratinocyte differentiation. J Invest Dermatol 121:1487–1495. doi:10.1111/j.1523-1747.2003.12614.x
Zheng X, Ray S, Bollag WB (2003) Modulation of phospholipase D-mediated phosphatidylglycerol formation by differentiating agents in primary mouse epidermal keratinocytes. Biochim Biophys Acta 1643:25–36. doi:10.1016/j.bbamcr.2003.08.006
Acknowledgments
We thank Maiko Yusa for mouse breeding. This work was supported in part by grant R37 DK35124 from the National Institutes of Health to ASV.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hara-Chikuma, M., Takahashi, K., Chikuma, S. et al. The expression of differentiation markers in aquaporin-3 deficient epidermis. Arch Dermatol Res 301, 245–252 (2009). https://doi.org/10.1007/s00403-009-0927-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00403-009-0927-9