Abstract
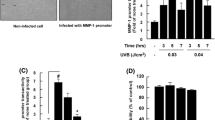
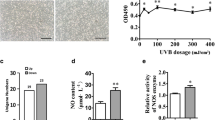
Upregulation of TNF-α is a key early response to ultraviolet B (UVB) by keratinocytes (KCs), and represents an important component of the inflammatory cascade in skin. UVB irradiation induces TNF-α expression in both KCs and dermal fibroblasts, with TNF-α mRNA induction seen as early as 1.5 h after UVB. We previously reported that the effects are wavelength-specific: TNF-α expression and secretion are induced by UVB (290–320 nm), but not by UVA (320–400 nm). Moreover, we found that IL-1α, a cytokine also present in irradiated skin, substantially and synergistically enhances the induction of TNF-α by UVB, and the induction of TNF-α by this combination of UVB with IL-1α is mediated through increased TNF-α gene transcription. We investigated the molecular mechanism for UVB-induction of the TNF-α gene with a series of TNF-α promoter constructs, ranging from 1.2 kbp (from −1179 to +1 with respect to the TNF-α transcription initiation site) down to 0.1 kbp (−109 to +1), each driving expression of a CAT reporter. Our results showed a persistent nine to tenfold increase of CAT activity in all TNF-α promoter/reporter constructs in response to UVB (30 mJ/cm2) exposure. These results indicate the presence of UVB-responsive cis-element(s) located between −109 and +1 of the TNF-α promoter, a region that contains a putative AP-1 site and a putative NFkB site. UVB-induction was abolished when the TNF-α promoter was mutated by one base pair at the AP-1 binding site. Cells treated with SP600125, an AP-1 inhibitor that inhibits JNK (c-Jun N-terminal kinase), also showed suppression of the 0.1 kbp TNF-α promoter/reporter construct. The authentic endogenous gene in untransfected cells was also blocked by the inhibitor. Electrophoretic Mobility Shift Assay indicated new complexes from UVB-treated nuclear extracts and anti-phospho-c-Jun, a regulatory component of the AP-1 transcription factor, creating a supershift indicating increased phosphorylation of c-Jun and hence higher AP-1 activity. Keratinocyte-derived TNF-α is a component of the early induction phase of the inflammatory cascade.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
TNF-α has a myriad of pro-inflammatory effects on the skin. There is evidence that ultraviolet light induces early TNF-α release from keratinocytes (KCs) in both normal and skin of cutaneous lupus erythematosus (CLE). Recent data related to the molecular mechanisms of UVB induction of KC TNF-α will be reviewed. There is a polymorphism of TNF-α associated with subacute cutaneous LE, as well as other autoimmune diseases. There are synergistic interactions between pro-inflammatory cytokines produced in the skin and in synergy with irradiated KCs, leading to later augmentation of TNF-α production. Different cytokines in combination with UVB have specific effects on chemokine production by UV-irradiated KCs. Finally, the most recent data characterizing the mechanism of the molecular sensor responsible for UV-induced activation of the TNF-α promoter will be reviewed. Clearly there is a large interplay of proteins and other skin-derived molecules that lead to the induction of inflammation in irradiated skin.
TNF-α effects in skin
There is excellent evidence that TNF-α in the skin induces adhesion molecules and chemokines in the skin, leading to attachment of inflammatory cells to vessels, rolling, emigration, and eventually chemotaxis into the skin (See Fig. 1) [7, 17, 30]. In addition, UVB induces inducible nitric oxide synthase (iNOS) activity in dermal endothelial cells, which plays an important role in UVB-induced inflammation in human skin, through a TNF-α-dependent pathway, as well as apoptosis [27, 29, 36, 37]. These inflammatory cells secrete additional cytokines that form a positive feedback loop in further upregulating TNF-α and downstream TNF-α-induced chemokines, cytokines, and other pro-inflammatory pathways.
Evidence for TNF-α production by keratinocytes and fibroblasts
There is evidence that UV-irradiation of both normal and cutaneous LE skin induces TNF-α at the protein and mRNA level [3, 9, 14, 26]. In addition, irradiation of KCs by UVB induces TNF-α mRNA and protein production [8]. IL-1α induces a synergistic induction of TNF-α by both UVB-irradiated KCs and fibroblasts (FBs), and UVB-irradiated FBs produce minimal TNF-α in the absence of IL-1α [11, 33]. In the presence of IL-1α, UVB-irradiated KCs begin to produce significant amounts of TNF-α protein between 3 and 4 h, with a peak by 24 h (Fig. 2a). There is evidence that induction of TNF-α by KCs and FBs is seen with UVB, but not UVA [33].
Synergistic effects of UVB and IL-1α on keratinocytes. Cells were treated with sham, sham + IL-1α (10 ng/ml), UVB 30 mJ/cm2 and UVB + IL-1α. a Supernatant samples were collected at the indicated times and analyzed by ELISA. There is a synergistic increase of TNF-α protein in UVB + IL-1α-treated keratinocytes. b RNA samples were collected at the indicated times and analyzed by real-time PCR. Results were normalized to cyclophilin A mRNA (housekeeping gene control) and presented as fold expression. IL-1α synergistically increases TNF-α mRNA induction by UVB-irradiated neonatal keratinocytes
Molecular mechanisms of UVB induction of KC TNF-α
The TNF-α gene is present on chromosome 6, located between lymphotoxin-β and Lymphotoxin-α (Fig. 3). The exact molecular mechanism for UV-induced TNF-α secretion from skin cells has been unknown, although there has been evidence that transcriptional effects are important [4, 6]. Normal human epidermal KCs released TNF-α in the medium after a single dose of UVB [35]. Recent studies demonstrate that TNF-α mRNA is induced in UVB-irradiated KCs treated with IL-1α by 1.5 h, with a peak at 8 h [4], followed by a steady decrease for 72 h (Fig. 2b). Nuclear run-off experiments demonstrate the UVB effect on TNF-α gene induction to be transcriptional in both macrophages and KCs [4, 6]. There was no effect of IL-1α on TNF-α mRNA half-life, suggesting that the increased TNF-α mRNA seen is predominantly due to transcriptional effects [4]. Previous studies have demonstrated that the UVB-signaling pathway in KCs is distinct from that seen with LPS, and mutations of each of the NFκB sites did not affect the UVB responsiveness of TNF-α promoter constructs [6, 22].
TNF-α promoter polymorphisms
There is an association of the -308A TNF-α promoter polymorphism with one form of subacute cutaneous LE [34]. This polymorphism is associated with an extended HLA A*01, B*08, DRB1*0301 haplotype, and the role of the polymorphism in terms of its role in etiology or simply disease association is still unclear [13]. Some studies have demonstrated an increase in levels of transcription, but the effects are highly context specific in terms of the cells type and stimulus, as well as the features of the promoter construct utilized [1, 13, 15, 16, 24]. Based on the susceptibility to UVB-induced impairment of contact hypersensitivity, it was proposed that polymorphism of the TNF-α region attributed to deleterious effects of UVB radiation in both mice and human [23].
Skin cytokine effects on epidermal TNF-α
After inflammatory cells enter the skin, they secrete numerous cytokines that can further increase epidermal production of TNF-α. There is evidence that TNF-α and IL-1α induce large increases of TNF-α mRNA expression in KCs [18]. However, clustering and internalization of TNF receptors may lessen the response to TNF-α protein over time, accounting for why persistent TNF-α in culture supernatant does not sustain TNF-α mRNA upregulation over time. Interferon -γ (IFN-γ) with IL-1α, but not IFN-α can further augment TNF-α expression by KCs [20].
Cytokines in the skin have differential effects on chemokine induction
There is evidence that UV-irradiated KCs in the presence of interferon-gamma leads to CCL5 and CCL22 induction. On the other hand, UVB in the presence of TNF-α and IL-1β induces CCL20, and CXCL8 in KCs. These chemokines are mainly regulated by IL-1α and TNF-α, UVB-induced primary proinflammatory cytokines [21].
Molecular sensor of UV in keratinocytes
A number of transcription factors are induced by UV light. Two of these UV-regulated transcription factors [10], AP-1 and NFκB, have known binding sites in the TNF-α promoter. There are, in fact, four NFκB binding sites and one AP-1 binding site (Fig. 3) [6]. The nature of the photoreceptor that senses UV light in the TNF-α promoter is not known. LPS stimulates TNF-α gene transcription in macrophages via NFκB, but site-directed mutations of the NFκB elements in the TNF-α promoter failed to disrupt its induction by UV irradiation [6]. There are broad regions of transcripitional factor binding sites in the TNF-α promoter that have positive and negative response elements unrelated to UV [6]. The proximal 120 bp portion of the TNF-α promoter region possesses binding sites for NF-kB, C/EBP (CCAAT-enhancer binding protein α) and AP-1 (c-Jun) transcription factors. Transient transfection of a 120-bp TNF-α promoter-reporter construct simultaneously transfected with a plasmid expressing the wild-type version of each of these transcription factors contributed to TNF-α promoter activation [19] (Fig. 4).
Map of human TNF-α and flanking genes on chromosome 6. The human TNF-α gene is located on chromosome 6 and is flanked by lymphotoxin α and β genes. The position and direction of transcription of the TNF-α, lymphotoxin α, and lymphotoxin β genes is shown by the black thick arrows. The exons are shown as checked boxes. The TNF-a, b, c, d, e, and f extended haplotype genetic markers are shown
Schematic diagram of human TNF-α promoter showing NF-κB and AP-1 sites. The human TNF-α promoter has four NF-κB and one AP-1 binding sites. Four different promoter/reporter constructs were designed containing different NF-κB site. The construct designed from the proximal part of the TNF-α promoter contains one NF-κB and AP-1 site, highlighted with circles
TNF-α promoter/CAT reporter deletion constructs have been made that demonstrate that the UV response element is contained between −109 and +1, in the very proximal aspect of the TNF-α promoter [4]. This proximal part of the hTNF-α promoter contains an AP-1 binding site (TGAGCTTA) at −106 to −99. AP-1 is a sequence-specific transcriptional activator, composed of the c-JUN/FOS heterodimer. In human skin, UV radiation elevates the expression of c-JUN, while FOS is constitutively expressed [31, 32]. Loss of the UVB response occurs by a G to T point mutation in the AP-1 binding site of the 1.2-kb TNF-α promoter [4]. Furthermore, inhibition of c-Jun N-terminal kinase, a stress-activated serine threonine protein kinase that phosphorylates c-Jun, results in a near-total block of the UVB induction of several TNF-α/CAT reporter promoter fragments when they are transfected into human KCs. This includes a small fragment of the proximal promoter that contains the AP-1 binding site and just one of the four NFκB binding site [4]. In addition, nuclear proteins were isolated from irradiated KCs and incubated with 32P-labeled oligonucleotide containing the AP-1 binding site of the human TNF-α promoter. This complex was then separated on a non-denatured polyacrylamide gel and demonstrated a supershift in mobility on EMSA when antibody against phosphorylated c-Jun was added. This also suggests a role for AP-1 binding to the TNF-α promoter as part of the UV response.
Activation of c-Jun N-terminal kinase is a KC specific UVB response, which in turn activates Elk-1 and AP-1 [2]. Studies in our lab showed AP-1 is a major regulator of TNF-α upregulation in response to UVB exposure [5]. TNF-α in turn has been shown to activate the NF-kB pathway via IKK-β the active subunit of IKK.
Suppression of TNF-α in cutaneous LE
It is clear that TNF-α has a pro-inflammatory role in the skin, as discussed above. However, blockade of TNF-α is complex in terms of cutaneous LE. Patients treated with anti-TNF-α agents show increased expression of interferon-regulated genes [25]. Suppression of TNF-α can induce skin disease. In addition, there is evidence that TNF-α has regulatory effects on B cell differentiation [12].
Conclusion
TNF-α plays an important pro-inflammatory role in the skin, both due to direct effects of ultraviolet light and to indirect effects of inflammatory cells that chemotax to the skin. It is clear that UV- and inflammatory cell-derived cytokines further enhance TNF-α gene transcription in human KCs and FBs. Recent studies suggest that AP-1 plays a critical role in increasing TNF-α transcription in UVB-irradiated KCs. IL-1 further augments TNF-α transcription through mechanisms independent of AP-1. Blockade of TNF-α in lupus has complex effects because of augmentation of interferon-regulated genes.
Abbreviations
- KCs:
-
Keratinocytes
- FBs:
-
Fibroblasts
- UVB:
-
Ultraviolet B
- TNF-α:
-
Tumor necrosis factor-α
References
Abraham LJ, Kroeger KM (1999) Impact of the -308 TNF promoter polymorphism on the transcriptional regulation of the TNF gene: relevance to disease. J Leukoc Biol 66:562–566
Adachi M, Gazel A, Pintucci G, Shuck A, Shifteh S, Ginsburg D et al (2003) Specificity in stress response: epidermal keratinocytes exhibit specialized UV-responsive signal transduction pathways. DNA Cell Biol 22:665–677. doi:10.1089/104454903770238148
Barkauskaite V, EK M, Popovic K, Harris HE, Wahren-Herlenius M, Nyberg F (2007) Translocation of the novel cytokine HMGB1 to the cytoplasm and extracellular space coincides with the peak of clinical activity in experimentally UV-induced lesions of cutaneous lupus erythematosus. Lupus 10:794–802. doi:10.1177/0961203307081895
Bashir MM, Sharma M, Werth VP (2006) UVB-induction of TNF-α gene transcription requires a response element, overlapping the AP-1-binding site, of the proximal promoter. J Invest Dermatol 126:277. doi:10.1038/sj.jid.5700067
Bashir M, Sharma M, Werth VP (2007) Mechanism of induction of TNF-α in response to UVB and IL-1α. J Invest Dermatol 127:S139
Bazzoni F, Kruys V, Shakhov A, Jongeneel CV, Beutler B (1994) Analysis of tumor necrosis factor promoter responses to ultraviolet light. J Clin Invest 93:56–62. doi:10.1172/JCI116984
Briscoe DM, Cotran RS, Pober JS (1992) Effects of tumor necrosis factor, lipopolysaccharide, and IL-4 on the expression of vascular cell adhesion molecule-1 in vivo. Correlation with CD3 + T cell infiltration. J Immunol 149:2954–2960
Clingen PH, Berneburg M, Petit-Frere C, Woollons A, Lowe JE, Arlett CF et al (2001) Contrasting effects of an ultraviolet B and an ultraviolet A tanning lamp on interleukin-6, tumour necrosis factor-alpha and intercellular adhesion molecule-1 expression. Br J Dermatol 145:54–62. doi:10.1046/j.1365-2133.2001.04281.x
de Kossodo S, Cruz PD Jr, Dougherty I, Thompson P, Silva-Valdez M (1995) Expression of the tumor necrosis factor gene by dermal fibroblasts in response to ultraviolet irradiation or lipopolysaccharide. J Invest Dermatol 104:318–322. doi:10.1111/1523-1747.ep12665361
Fisher GJ, Datta SC, Talwar HS, Wang Z-Q, Varani J, Kang S et al (1996) Molecular basis of sun-induced premature skin ageing and retinoid antagonism. Nature 379:335–339. doi:10.1038/379335a0
Fujisawa H, Wang B, Kondo S, Shivji GM, Sauder DN (1997) Costimulation with ultraviolet B and interleukin-1 alpha dramatically increase tumor necrosis factor-alpha production in human dermal fibroblasts. J Interferon Cytokine Res 17:307–313
Kashiwa H, Wright SC, Bonavida B (1987) Regulation of B cell maturation and differentiation. I. Suppression of pokeweed mitogen-induced B cell differentiation by tumor necrosis factor (TNF). J Immunol 138:1383–1390
Knight JC (2005) Regulatory polymorphisms underlying complex disease traits. J Mol Med 83:97–109. doi:10.1007/s00109-004-0603-7
Kock A, Schwarz T, Kirnbauer R, Urbanski A, Perry P, Ansel JC et al (1990) Human keratinocytes are a source for tumor necrosis factor alpha: evidence for synthesis and release upon stimulation with endotoxin or ultraviolet light. J Exp Med 172:1609–1614. doi:10.1084/jem.172.6.1609
Kroeger KM, Carville KS, Abraham LJ (1997) The -308 tumor necrosis factor-alpha promoter polymorphism effects transcription. Mol Immunol 34:391–399. doi:10.1016/S0161-5890(97)00052-7
Kroeger KM, Steer JH, Joyce DA, Abraham LJ (2000) Effects of stimulus and cell type on the expression of the -308 tumour necrosis factor promoter polymorphism. Cytokine 12:110–119. doi:10.1006/cyto.1999.0529
Krutmann J, Kock A, Schauer E, Parlow F, Moller A, Kapp A et al (1990) Tumor necrosis factor beta and ultraviolet radiation are potent regulators of human keratinocyte ICAM-1 expression. J Invest Dermatol 95:127–131. doi:10.1111/1523-1747.ep12477839
Lisby S, Hauser C (2002) Transcriptional regulation of tumor necrosis factor-alpha in keratinocytes mediated by interleukin-1beta and tumor necrosis factor-alpha. Exp Dermatol 11:592–598. doi:10.1034/j.1600-0625.2002.110612.x
Liu H, Sidiropoulos P, Song G, Pagliari LJ, Birrer MJ, Stein B et al (2000) TNF-alpha gene expression in macrophages: regulation by NF-kappa B is independent of c-Jun or C/EBP beta. J Immunol 164:4277–4285
Matsuura K, Otsuka F, Fujisawa H (1998) Effects of interferons on tumour necrosis factor alpha production from human keratinocytes. Cytokine 10:500–505. doi:10.1006/cyto.1997.0326
Meller S, Winterberg F et al (2005) Ultraviolet radiation-induced injury, chemokines, and leukocyte recruitment: an amplification cycle triggering cutaneous lupus erythematosus. Arthritis Rheum 52:1504–1516. doi:10.1002/art.21034
Millard TP, Kondeatis E, Cox A, Wilson AG, Grabczynska SA, Carey BS et al (2001) A candidate gene analysis of three related photosensitivity disorders: cutaneous lupus erythematosus, polymorphic light eruption and actinic prurigo. Br J Dermatol 145:229–236. doi:10.1046/j.1365-2133.2001.04339.x
Niizeki H, Inoki H, Streilein JW (2002) Polymorphisms in the TNF region confer susceptibiilty to UVB-induced impairment of contact hypersensitivity induction in mice and humans. Methods 28:46–54. doi:10.1016/S1046-2023(02)00211-6
Pachman LM, Liotta-Davis MR, Hong DK, Kinsella TR, Mendez EP, Kinder JM et al (2000) TNFalpha-308A allele in juvenile dermatomyositis: association with increased production of tumor necrosis factor alpha, disease duration, and pathologic calcifications. Arthritis Rheum 43:2368–2377. doi:10.1002/1529-0131(200010)43:10<2368::AID-ANR26>3.0.CO;2-8
Palucka AK, Blanck JP, Bennett L, Pascual V, Banchereau J (2005) Cross-regulation of TNF and IFN-alpha in autoimmune diseases. Proc Natl Acad Sci USA 102:3372–3377. doi:10.1073/pnas.0408506102
Popovic K, EK M, Espinosa A, Padyukov L, Harris HE, Wahren-Herlenius M, Nyberg F (2005) Increased expression of the novel proinflammatory cytokine high mobility group box chromosomal protein 1 in skin lesions of patients with lupus erthematosus. Arthritis Rheum 52:3639–3645. doi:10.1002/art.21398
Schwarz A, Bhardwaj R, Aragane Y, Mahnke K, Riemann H, Metze D et al (1995) Ultraviolet-B-induced apoptosis of keratinocytes: evidence for partial involvement of tumor necrosis factor-alpha in the formation of sunburn cells. J Invest Dermatol 104:922–927. doi:10.1111/1523-1747.ep12606202
Solt LA, Madge LA, Orange JS, May MJ (2007) Interleukin-1-induced NF-κB activation is NEMO-dependent but does not require IKKbeta. JBC 282:8724–8733
Suschek CV, Mahotka C, Schnorr O, Kolb-Bachofen V (2004) UVB radiation-mediated expression of inducible nitric oxide synthase activity and the augmenting role of co-induced TNF-alpha in human skin endothelial cells. J Invest Dermatol 123:950–957. doi:10.1111/j.0022-202X.2004.23422.x
Swerlick RA, Lee KH, Li KLJ, Sepp NT, Caughman SW, Lawley TJ (1992) Regulation of vascular cell adhesion molecule 1 on human dermal microvascular endothelial cells. J Immunol 149:698–705
Tanos T, Marinessen MJ, Leskow FC, Hochbaum D, Martinetto H, Gutkind JS et al (2005) Phosphorylation of c-Fos by members of the p38 MAPK family. Role in the AP-1 response to UV light. J Biol Chem 280:18842–18852. doi:10.1074/jbc.M500620200
Wan YS, Wang ZQ, Voorhees J, Fisher G (2001) EGF receptor crosstalks with cytokine receptors leading to activation of c-Jun kinase in response to UV irradiation in human keratinocytes. Cell Signal 13:139–144. doi:10.1016/S0898-6568(00)00146-7
Werth VP, Zhang W (1999) Wavelength-specific synergy between ultraviolet radiation and interleukin-1 alpha in the regulation of matrix-related genes: mechanistic role for tumor necrosis factor-alpha. J Invest Dermatol 113:196–201. doi:10.1046/j.1523-1747.1999.00681.x
Werth VP, Zhang W, Dortzbach K, Sullivan K (2000) Association of a promoter polymorphism of TNFalpha with subacute cutaneous lupus erythematosus and distinct photoregulation of transcription. J Invest Dermatol 115:726–730. doi:10.1046/j.1523-1747.2000.00118.x
Yarosh D, Both D, Kibitel J, Anderson C, Elmets C, Brash D et al (2000) Regulation of TNFalpha production and release in human and mouse keratinocytes and mouse skin after UV-B radiation. Photodermatol Photoimmunol Photomed 16:263–270. doi:10.1034/j.1600-0781.2000.160606.x
Zhuang L, Wang B, Shinder GA, Shivji GM, Mak TW, Sauder DN (1999) TNF receptor p55 plays a pivotal role in murine keratinocyte apoptosis induced by ultraviolet B irradiation. J Immunol 162:1440–1447
Zhuang L, Wang B, Sauder DN (2000) Molecular mechanism of ultraviolet-induced keratinocyte apoptosis. J Interferon Cytokine Res 20:445–454. doi:10.1089/10799900050023852
Acknowledgment
The work is supported by a V.A. Merit Review Grant (V.P.W).
Conflict of interest statement
The authors have no potential conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bashir, M.M., Sharma, M.R. & Werth, V.P. TNF-α production in the skin. Arch Dermatol Res 301, 87–91 (2009). https://doi.org/10.1007/s00403-008-0893-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00403-008-0893-7