Abstract
Introduction
To determine whether immobilization after arthroscopic rotator cuff repair improved tendon healing compared with early passive motion.
Materials and methods
A systematic electronic literature search was conducted to identify randomized controlled trials (RCTs) comparing early passive motion with immobilization after arthroscopic rotator cuff repair. The primary outcome assessed was tendon healing in the repaired cuff. Secondary outcome measures were range of motion (ROM) and American Shoulder and Elbow Surgeons (ASES) shoulder scale, Simple Shoulder Test (SST), Constant, and visual analog scale (VAS) for pain scores. Pooled analyses were performed using a random effects model to obtain summary estimates of treatment effect with 95 % confidence intervals. Heterogeneity among included studies was quantified.
Results
Three RCTs examining 265 patients were included. Meta-analysis revealed no significant difference in tendon healing in the repaired cuff between the early-motion and immobilization groups. A significant difference in external rotation at 6 months postoperatively favored early motion over immobilization, but no significant difference was observed at 1 year postoperatively. In one study, Constant scores were slightly higher in the early-motion group than in the immobilization group. Two studies found no significant difference in ASES, SST, or VAS score between groups.
Conclusion
We found no evidence that immobilization after arthroscopic rotator cuff repair was superior to early-motion rehabilitation in terms of tendon healing or clinical outcome. Patients in the early-motion group may recover ROM more rapidly.
Level of evidence
Level II; systematic review of levels I and II studies.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Arthroscopic rotator cuff repair has become the most popular surgical treatment for rotator cuff pathology in the last two decades, and it now provides largely good clinical results. However, despite the advancement and refinement of arthroscopic techniques, the non-healing rate after rotator cuff repair remains 20–94 % [1, 2]. Some studies have documented better results of rotator cuff repair when tendon healing is successful [3–7]; thus, the achievement of such healing can reasonably be considered a primary objective of this surgery.
Many factors affect whether a tendon will successfully heal to a bony tuberosity after repair [7–13]. Early motion rehabilitation, usually recommended to prevent postoperative stiffness, may be one such factor. Some animal studies have suggested that early motion causes strain or micromotion at the repair site, compromising healing, whereas immobilization of the shoulder after rotator cuff repair improves tendon-to-bone healing [14–16]. In contrast, another animal study found that continuous passive motion enhanced tendon–bone recovery after rotator cuff repair [17]. Thus, animal studies have not successfully identified the optimal rehabilitation method for tendon healing. Similarly, comparative clinical studies have yielded conflicting results; some have demonstrated that a postoperative immobilization period improved the rate of tendon healing [18–20], whereas others found that immobilization after rotator cuff repair had no effect on the healing rate compared with early passive motion [21].
To our knowledge, no systematic review or meta-analysis on this topic has been published. The present meta-analysis of data from randomized controlled trials (RCTs) was conducted to provide an evidence-based appraisal of the effects of immobilization after arthroscopic rotator cuff repair. We postulated that the rate of cuff healing would be higher in patients treated with immobilization than in those who followed an early-motion rehabilitation protocol.
Methods
Search strategy
We searched the PubMed and Embase electronic databases and the Cochrane Central Register of Controlled Trials to identify published reports of rehabilitation for rotator cuff repair. The search strategy is presented in Table 1. Reference lists of relevant articles were manually searched to identify additional trials. We imposed no language restriction on the search, and included articles published through 2 Dec 2013.
Inclusion criteria
Two authors independently reviewed each article to determine the eligibility for inclusion based on the following criteria: (1) RCT, (2) analysis of arthroscopic repair of rotator cuff tears, (3) comparison of early passive motion with postoperative immobilization as rehabilitation protocol, and (4) follow-up period ≥1 year. Disagreements were resolved by discussion until consensus was reached. When the two reviewers could not reach consensus, a third reviewer was asked to provide a final opinion.
Outcome measures
The primary outcome assessed was tendon healing in the repaired cuff. Secondary outcome measures were the range of motion (ROM) and American Shoulder and Elbow Surgeons (ASES) shoulder scale, Simple Shoulder Test (SST), Constant, and visual analog scale (VAS) for pain scores.
Data extraction and assessment of risk of bias
Two reviewers independently extracted data from each trial. The risk of bias in the studies was assessed independently using the Cochrane criteria [22], which comprise seven features of interest: (1) sequence generation, (2) allocation concealment, (3) blinding of participants and personnel, (4) blinding of outcome assessment, (5) incomplete outcome data, (6) elective outcome reporting, and (7) other sources of bias.
Statistical analysis
The incidence of tendon healing was treated as a dichotomous variable, expressed as a risk ratio (RR) with a 95 % confidence interval (CI) for each study. ROM parameters (forward flexion and external rotation) were treated as continuous variables. For continuous variables, means and standard deviations were used to calculate weighted mean differences (WMDs) and 95 % CIs in the meta-analysis. Heterogeneity among studies was quantified using the I 2 statistic, which is a quantitative measure of inconsistency across studies. An I 2 value of 0 % represents no heterogeneity, and values of 25, 50, and ≥75 % represent low, moderate, and high degrees of heterogeneity, respectively [23]. Data from eligible studies were pooled using a random effects model because of anticipated heterogeneity among study populations, surgical treatment protocols, and durations of immobilization. Analyses were conducted using Review Manager Software (ver. 5.1; The Nordic Cochrane Centre, The Cochrane Collaboration, Copenhagen, Denmark).
Results
Study characteristics
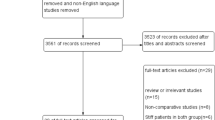
Three of 912 articles identified in the literature search met the inclusion criteria (Fig. 1) [19–21]. These studies involved a total of 265 patients (early motion, n = 138; immobilization, n = 127). General data from the three studies are summarized in Table 2.
The risk of bias in these studies is summarized in Fig. 2. The use of randomization was mentioned in two of the three trials; randomization was table generated in one case [19] and the method was not described in the other case [20]. Allocation concealment was adequate in two studies [19, 21], which was confirmed in one case by contacting the author [21]. One study [19] used triple blinding, whereas blinding was not used or not clearly described in two studies [20, 21]. Regarding incomplete outcome data, one article [20] reported an exclusion rate exceeding 15 %. No publication clearly discussed reporting bias or any other source of bias.
Primary outcome: tendon healing
All three articles reported information on tendon healing [19–21]. Meta-analysis revealed no significant difference in the incidence of repaired cuff healing between the early-motion and immobilization groups (RR = 0.98, 95 %, CI = 0.88–1.09, P = 0.67) and no heterogeneity (I 2 = 0 %; Fig. 3).
Forest plot of tendon healing. Individual studies are listed on the left, with healing events and number of patients in each study arm. A visual representation of the risk ratio for each study is plotted on the right with a diamond. The large diamond at the bottom represents the pooled treatment effect of all studies. It crosses the midline, representing no significant difference between the early-motion and immobilization groups
Secondary outcomes
Range of motion
ROM data from two of the three studies could be pooled [20, 21]. Cuff and Pupello [19] published ranges instead of standard deviations, preventing the inclusion of these data. Meta-analysis revealed no significant difference in forward flexion between the early-motion and immobilization groups at 6 months (WMD = 5.97, 95 % CI = −1.43 to 13.38, P = 0.11, I 2 = 0 %) or 1 year (WMD = 5.79, 95 % CI = −0.55 to 12.12, P = 0.07, I 2 = 0 %) postoperatively. A significant difference in external rotation favored the early-motion group at 6 months postoperatively (WMD = 8.29, 95 % CI = 2.97–13.61, P = 0.002, I 2 = 0 %), but no significant difference was observed at 1 year postoperatively (WMD = 5.62, 95 % CI = −2.53 to 13.76, P = 0.18, I 2 = 43 %; Figs. 4, 5, 6, 7).
Forest plot of forward flexion at 6 months postoperatively. Individual studies are listed on the left, with forward flexion (mean and standard deviation) and number of patients in each study arm. The pooled treatment effect, represented by the black diamond, demonstrates no significant difference between the early-motion and immobilization groups
Functional outcome measures
Two studies compared ASES and SST scores from the immobilization and early-motion groups. Kim et al. [21] found significant improvements in SST, Constant, and ASES scores in both groups after arthroscopic rotator cuff repair, with no significant difference between groups at 6 or 12 months postoperatively. Similarly, Cuff and Pupello [19] reported no significant difference in SST or ASES scores between groups at 1 year postoperatively. We could not pool data for mean differences in functional outcome measures, as means but not standard deviations were reported in one article [19]. Arndt et al. [20] reported that the mean Constant score was slightly higher in the early-motion group than in the immobilization group at 1 year postoperatively (P = 0.045).
VAS scores
Two articles [20, 21] provided pain data for both groups. Arndt et al. [20] reported a significant reduction in VAS pain scores during the follow-up period, with no significant difference between groups. Similarly, Kim et al. [21] reported no significant difference in VAS scores between groups at 1 year postoperatively.
Discussion
The structural integrity of a repaired cuff critically influences the clinical outcome of surgical treatment [3–7]. Recurrent tears at the insertion site are common after repair, occurring in 20–94 % of cases [1, 2]. Because of the high rate of repair failure, much research has focused on identifying strategies to improve rotator cuff healing following surgical repair. Bey et al. [14] suggested that early motion may compromise healing by creating strain. Gimbel et al. [15] found that shoulder immobilization after rotator cuff repair improved tendon-to-bone healing, characterized by increased organization of collagen, followed by increased mechanical properties. Thomopoulos et al. [16] reported superior structural, compositional, and quasilinear viscoelastic properties in shoulders that were immobilized after cuff repair than in those that were exercised. However, in a rabbit model, Li et al. [17] found that continuous passive motion can enhance type III collagen synthesis at the tendon–bone interface in the early stage of repair following acute rupture of the supraspinatus tendon, thereby contributing to tendon–bone recovery after rotator cuff injury.
To our knowledge, this meta-analysis is the first to explore the role of rehabilitation in cuff healing. The results contradicted our hypothesis that immobilization would increase tendon healing compared with an early-motion rehabilitation protocol, as structural outcomes were similar in the two groups 1 year after the arthroscopic repair of rotator cuff tears. Despite the use of different methods to diagnose postoperative tendon healing, no heterogeneity was found among the analyzed studies (I 2 = 0 %). We speculate that rehabilitation is not the sole factor affecting tendon–bone recovery; the effects of other factors, such as older age [8], fatty degeneration [9], larger tears [7, 10], and surgical technique [11–13], may outweigh those of the rehabilitation protocol.
Postoperative stiffness is another devastating complication of rotator cuff repair. Its incidence has not been established, with reported values ranging 4.9–32.7 % [24, 25]. Efforts to avoid stiffness led to the popularization of early passive ROM protocols after rotator cuff repair [26–28]. However, several authors have recently reported that immobilization for a certain period after surgical repair did not lead to postoperative shoulder stiffness [29, 30]. The most appropriate rehabilitation protocol to maximize the clinical outcome remains unclear and controversial. In this study, we demonstrated that subjects in the early-motion group regained ROM more rapidly, with more external rotation at 6 months and a similar functional outcome compared with the immobilization group. We speculate that immobilization leads to early stiffness due to the formation of fibrotic scar adhesions in the shoulder.
Limitations
Our literature review revealed that very few RCTs on this topic have been published. Thus, the main limitation of this review is the small number of RCTs included, which compromised the ability to draw strong conclusions. In addition, some clinical heterogeneity among trials was detected, as one study included partial-thickness tears. The strength of this systematic review is the exclusive analysis of RCTS, which helped to reduce the systematic error inherent in retrospective and some prospective cohort studies. A meta-analysis is most persuasive when data from high-quality RCTs are pooled. Nevertheless, further large-scale, well-designed RCTs on this topic are needed.
Conclusion
We found no evidence that immobilization after arthroscopic rotator cuff repair was superior to early-motion rehabilitation in terms of tendon healing or clinical outcome. Patients in the early-motion group may recover ROM more rapidly.
References
Boileau P, Brassart N, Watkinson DJ, Carles M, Hatzidakis AM, Krishnan SG (2005) Arthroscopic repair of full-thickness tears of the supraspinatus: does the tendon really heal? J Bone Joint Surg Am 87:1229–1240
Galatz LM, Ball CM, Teefey SA, Middleton WD, Yamaguchi K (2004) The outcome and repair integrity of completely arthroscopically repaired large and massive rotator cuff tears. J Bone Joint Surg Am 86-A:219–224
Flurin PH, Landreau P, Gregory T, Boileau P, Brassart N, Courage O et al (2005) Arthroscopic repair of full-thickness cuff tears: a multicentric retrospective study of 576 cases with anatomical assessment. Rev Chir Orthop Reparatrice Appar Mot 91:31–42
Kluger R, Bock P, Mittlbock M, Krampla W, Engel A (2011) Long-term survivorship of rotator cuff repairs using ultrasound and magnetic resonance imaging analysis. Am J Sports Med 39:2071–2081
Vastamaki M, Lohman M, Borgmastars N (2013) Rotator cuff integrity correlates with clinical and functional results at a minimum 16 years after open repair. Clin Orthop Relat Res 471:554–561
Lafosse L, Brozska R, Toussaint B, Gobezie R (2007) The outcome and structural integrity of arthroscopic rotator cuff repair with use of the double-row suture anchor technique. J Bone Joint Surg Am 89:1533–1541
Huijsmans PE, Pritchard MP, Berghs BM, van Rooyen KS, Wallace AL, de Beer JF (2007) Arthroscopic rotator cuff repair with double-row fixation. J Bone Joint Surg Am 89:1248–1257
Tashjian RZ, Hollins AM, Kim HM, Teefey SA, Middleton WD, Steger-May K et al (2010) Factors affecting healing rates after arthroscopic double-row rotator cuff repair. Am J Sports Med 38:2435–2442
Goutallier D, Postel JM, Gleyze P, Leguilloux P, Van Driessche S (2003) Influence of cuff muscle fatty degeneration on anatomic and functional outcomes after simple suture of full-thickness tears. J Shoulder Elbow Surg 12:550–554
Sugaya H, Maeda K, Matsuki K, Moriishi J (2007) Repair integrity and functional outcome after arthroscopic double-row rotator cuff repair. A prospective outcome study. J Bone Joint Surg Am 89:953–960
Mihata T, Watanabe C, Fukunishi K, Ohue M, Tsujimura T, Fujiwara K et al (2011) Functional and structural outcomes of single-row versus double-row versus combined double-row and suture-bridge repair for rotator cuff tears. Am J Sports Med 39:2091–2098
Tudisco C, Bisicchia S, Savarese E, Fiori R, Bartolucci DA, Masala S et al (2013) Single-row vs. double-row arthroscopic rotator cuff repair: clinical and 3 Tesla MR arthrography results. BMC Musculoskelet Disord 14:43
Duquin TR, Buyea C, Bisson LJ (2010) Which method of rotator cuff repair leads to the highest rate of structural healing? A systematic review. Am J Sports Med 38:835–841
Bey MJ, Ramsey ML, Soslowsky LJ (2002) Intratendinous strain fields of the supraspinatus tendon: effect of a surgically created articular-surface rotator cuff tear. J Shoulder Elbow Surg 11:562–569
Gimbel JA, Van Kleunen JP, Williams GR, Thomopoulos S, Soslowsky LJ (2007) Long durations of immobilization in the rat result in enhanced mechanical properties of the healing supraspinatus tendon insertion site. Biomech Eng 129:400–404
Thomopoulos S, Williams GR, Soslowsky LJ (2003) Tendon to bone healing: differences in biomechanical, structural, and compositional properties due to a range of activity levels. J Biomech Eng 125:106–113
Li S, Min SX, Zhang H, Fu GJ, Wang PC, Jin AM (2010) Effect of continuous passive motion on basic fibroblast growth factor expression during tendon-bone repair after surgical repair of acute rupture of the supraspinatus tendon in rabbits. Nan Fang Yi Ke Da Xue Xue Bao 30:1020–1023
Parsons BO, Gruson KI, Chen DD, Harrison AK, Gladstone J, Flatow EL (2010) Does slower rehabilitation after arthroscopic rotator cuff repair lead to long-term stiffness? J Shoulder Elbow Surg 19:1034–1039
Cuff DJ, Pupello DR (2012) Prospective randomized study of arthroscopic rotator cuff repair using an early versus delayed postoperative physical therapy protocol. J Shoulder Elbow Surg 21:1450–1455
Arndt J, Clavert P, Mielcarek P, Bouchaib J, Meyer N, Kempf JF (2012) Immediate passive motion versus immobilization after endoscopic supraspinatus tendon repair: a prospective randomized study. Orthop Traumatol Surg Res 98:S131–138
Kim YS, Chung SW, Kim JY, Ok JH, Park I, Oh JH (2012) Is early passive motion exercise necessary after arthroscopic rotator cuff repair? Am J Sports Med 40:815–821
Higgins JP, Altman DG, Gotzsche PC, Juni P, Moher D, Oxman AD et al (2011) The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ 343:d5928
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327:557–560
Huberty DP, Schoolfield JD, Brady PC, Vadala AP, Arrigoni P, Burkhart SS (2009) Incidence and treatment of postoperative stiffness following arthroscopic rotator cuff repair. Arthroscopy 25:880–890
Seo SS, Choi JS, An KC, Kim JH, Kim SB (2012) The factors affecting stiffness occurring with rotator cuff tear. J Shoulder Elbow Surg 21:304–309
Millett PJ, Wilcox RB 3rd, O’Holleran JD, Warner JJ (2006) Rehabilitation of the rotator cuff: an evaluation-based approach. J Am Acad Orthop Surg 14:599–609
Franceschi F, Ruzzini L, Longo UG, Martina FM, Zobel BB, Maffulli N et al (2007) Equivalent clinical results of arthroscopic single-row and double-row suture anchor repair for rotator cuff tears: a randomized controlled trial. Am J Sports Med 35:1254–1260
Aydin N, Kocaoglu B, Guven O (2010) Single-row versus double-row arthroscopic rotator cuff repair in small- to medium-sized tears. J Shoulder Elbow Surg 19:722–725
Peltz CD, Dourte LM, Kuntz AF, Sarver JJ, Kim SY, Williams GR et al (2009) The effect of postoperative passive motion on rotator cuff healing in a rat model. J Bone Joint Surg Am 91:2421–2429
Sarver JJ, Peltz CD, Dourte L, Reddy S, Williams GR, Soslowsky LJ (2008) After rotator cuff repair, stiffness–but not the loss in range of motion–increased transiently for immobilized shoulders in a rat model. J Shoulder Elbow Surg 17:108S–113S
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Shen, C., Tang, ZH., Hu, JZ. et al. Does immobilization after arthroscopic rotator cuff repair increase tendon healing? A systematic review and meta-analysis. Arch Orthop Trauma Surg 134, 1279–1285 (2014). https://doi.org/10.1007/s00402-014-2028-2
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-014-2028-2