Abstract
Introduction
Accuracy in navigated surgery depends on placement and registration of stable reference markers close to the anatomic region of interest. Navigation in small and complex anatomic regions, such as the scaphoid, is challenging due to difficulties in placing a stable reference marker. In the current paper, we describe the use of a customized wrist-positioning device “Scaph-splint” with a built-in reference marker that facilitates navigated scaphoid screw insertion in combination with a 3D imaging device.
Materials and methods
Initial cadaveric feasibility study Five fresh-frozen cadaveric upper extremity specimens were utilized. Each specimen was secured onto the “Scaph-splint” with the wrist in about 90° of extension. Using a 3D fluoroscope, a series of images were taken of the carpal bones and reconstructed in axial, sagittal, and coronal planes. Navigated planning and guidance of scaphoid drilling and screw placement was performed. Next, a repeat 3D scan was taken to analyze the drill canal. The accuracy of navigated scaphoid drilling, drilling trials, and any penetration of the scaphoid outside of the planned drill trajectory were evaluated. A grading scheme was used to assess the drilling accuracy: Grade 1 <1 mm deviation, Grade 2 <2 mm deviation, Grade 3 <3 mm.
Results
Scaphoid drilling was confirmed to be completely accurate (Grade 1) in two specimens, highly accurate (Grade 2) in two specimens, and accurate (Grade 3) in one specimen. No specimen required a repeat drilling of the scaphoid. In one specimen, the proximal scaphoid pole was perforated by the drill. No registration failures or loosening of the reference marker occurred.
Conclusion
The use of the “Scaph-splint” enabled stabilization of the hand and wrist, thus adequately fixing the reference marker in relation to scaphoid for optimal navigation and screw placement without the need to directly penetrate the scaphoid with a reference marker. The use of 3D fluoroscopy further increased the accuracy and precision of scaphoid screw placement.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Screw osteosynthesis of scaphoid fractures is often based on minimally invasive operative techniques. Fracture reduction and screw insertion can be guided by wrist fluoroscopy, arthroscopy, or specially designed guiding jigs [12, 22]. Nevertheless, operative fixation of these fractures remains a challenging problem in hand surgery. Complications of scaphoid osteosynthesis such as incorrect screw placement or inadvertent damage of articular cartilage have been reported in the literature ranging from 5 to 30% [1, 8, 19–21]. Additionally, percutaneous techniques have been associated with increased intraoperative use of radiation [2, 12]. The biomechanical importance of optimal scaphoid screw placement has been emphasized in the literature [9, 18]. Recently, mobile CT and isocentric C-arm fluoroscope image intensifiers have been introduced as precise imaging modalities for intraoperative evaluation and management of fractures and osteosyntheses [15, 16]. The ISO-C3D is a 3D imaging system that collects 100 sequential radiographs within a 2-min time span around the anatomic region of interest. The images are then processed by the C-arm computer and reconstructed into sagittal, axial, and coronal planes. These images can then be transferred to a navigation system for surgical planning and further virtual placement of surgical tools. The combination of 3D imaging and Computer Assisted Surgery (CAS), such as navigation-based fracture fixation and implant placement, has been shown to be an effective tool in orthopedic surgery [4, 5, 11]. The surgeon can navigate through the anatomic region of interest in multiplanar planes to find the best possible position for screw placement. For navigation to be precise, stable, motion-free reference markers have to be placed near the anatomic region of interest and be registered by the navigation system [3, 14]. Navigation-assisted surgery in small and complex anatomic regions, such as the scaphoid, has been challenging due to difficulties with establishing such a reference marker. Navigated screw osteosynthesis for scaphoid fractures using 2D fluoroscopy imaging has been recently reported in the literature [17]. Yet given the complex anatomy of the scaphoid and the carpus, we feel that 3D imaging can better delineate the complex anatomical detail and improve surgical accuracy of scaphoid screw insertion. In the following paper, we describe the first use of a custom wrist/hand positioning device “Scaph-splint” with a built-in reference marker that would immobilize the distal upper extremity, facilitating the accurate insertion of a scaphoid screw using 3D navigation.
Materials and methods
The wrist/hand positioning device
The custom-built hand-positioning device “Scaph-splint” was made out of Polysulfon (PSU), which is radiolucent and reusable after gas sterilization. It consisted of four separate parts assembled in such a way as to provide a stable platform for both the distal forearm and the hand. The design of the splint allows for positioning of the extremity in either the volar or the dorsal positions (Fig. 1). The reference marker for the navigation system was securely fixed onto a designated slot on the hand platform. The splint was deliberately constructed such that the reference marker was 15 cm away from the center of ISO-C3D scan area. This minimizes the incidence of metal artifact while ensuring that the marker is not too far away as to affect accuracy [6, 7].
The upper extremity was then secured to the device using velcro straps with the wrist in about 90° of extension, enabling a palmar approach to the scaphoid. To prevent secondary motion additional straps were used to rigidly fix the cadaver arm onto the splint. For navigation of the 1-mm K-wire, an aiming device was utilized and fixed to a positioning arm that could be moved through all planes and fixed at a desirable position.
Cadaver study
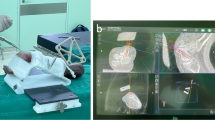
Five fresh-frozen cadaveric upper extremity specimens were utilized. Each extremity was immobilized on the “Scaph-splint” as described earlier (Fig. 2). The fixed extremity was placed on a carbon fiber table to reduce artifact. A commercially available navigation system (Brainlab, Heimstetten, Germany) and ISO-C3D fluoroscopy (Siemens, Germany) unit were used. Sequential radiographs were taken from the carpus with the fluoroscope during one automated scan and transferred to the navigation system for analysis. Surgical planning was achieved with the help of the navigation system, which visualized the drill/screw trajectory based on the multi-plane (sagittal, coronal, and frontal) reconstruction images provided by the 3D fluoroscope (Fig. 4). The trajectory was chosen by identifying the middle axis of the scaphoid in two planes (sagittal and coronal) and employing it as the optimal anatomical position. When the axis and the length of the screw had been determined virtually, insertion of the guide wire was carried out under permanent guidance of the virtual images. A 1.5 cm incision was then made over the distal pole of the scaphoid. Navigated drilling proceeded with a 2.5 mm drill bit in a distal to proximal direction over the guide wire. Finally, a cannulated Herbert screw was inserted into the drill canal with a navigated screw driver. A secondary ISO-C3D scan was performed for the final evaluation of the drill canal and screw insertion.
Cadaveric feasibility study
The accuracy of screw placement was determined by evaluation of pre- and postoperative fluoroscopic 3D images. In particular, the following parameters were evaluated:
-
1.
The accuracy of navigated scaphoid drilling, determined by comparing the planned and final drill trajectories, and graded as completely accurate (1), highly accurate (2), and accurate (3)
-
2.
Number of drilling trials
-
3.
Perforation of the scaphoid outside the planned drill trajectory. The scaphoid drill canal was examined in all three reconstruction planes by an experienced orthopedic hand surgeon who was blinded to the study.
Motion assessment between the “Scaph-splint” and scaphoid
Five fresh-frozen cadaveric upper extremity specimens were utilized. Five rounds of tests for motion analysis were performed. Assessment for movement of the scaphoid relative to the “Scaph-splint” was made possible using a 3D ultrasound motion tracking system (Model CMS 30P; Zebris Inc.; Tübingen, Germany). Drilling was simulated with a T-handle. Any relative motion was measured by the ultrasound system and analyzed accordingly (Fig. 4a). There were three microphones, i.e., triaxial sensor, with a star-adapter (made of acrylic glass). The ultrasonic microphones (cylindrical, height 10 mm, diameter 5 mm, weight 1 g, pulse frequency 50 s−1 at frequency of 40,000 Hz emit) were connected by thin electrical cables to the central unit of the measurement system of a personal computer. One of the microphones was fixed on the “Scaph-splint” with a screw and the other microphone was fixed in the scaphoid with two K-wires (Fig. 3b). The distance between the transducer (Model MH H3; Zebris Inc.; Tübingen, Germany) and the microphone was 1 m. The absolute spatial accuracy of the system was <0.25 mm at a resolution of 0.085 mm. The maximum deviation from the actual angle change was less than 1° in all three planes. This was confirmed independently by the manufacturer. The Euclidean distance from the scaphoid to the splint was used for the evaluation purposes.
First clinical case
The study was performed following the Declaration of Helsinki principles. The first patient was a 30-year-old male with a sports-related injury. He had sustained a complicated wrist injury with fractures of the scaphoid and hook of the hamate with concomitant scapholunate dissociation (Fig. 4a). The patient underwent surgery 5 days post-injury. The hand was fixed to the splint with the use of a bandage and placed on a carbon fiber hand surgery table. To acquire images an ISO-C3D system (Siemens, Erlangen, Germany) was used. The data were transferred to the navigation system (VectorVision, Brainlab, Feldkirchen, Germany). After planning the trajectory, the customized aiming device was calibrated once it had been fixed with a positioning arm to the “Scaph-splint”. Once the trajectory planning had been completed, the aiming device was aligned extracorporeally. This position was fixed using the positioning arm. A 1-mm K-wire was used to perform the drilling (Fig. 5). A repeat scan was performed post-drilling to analyze the drill path. Once the path was confirmed to be satisfactory, the Herbert screw was inserted. Treatment of the scapholunate dissociation and the fracture of the hook of the hamate were performed in a non-navigated conventional fashion.
Results
Cadaveric feasibility study
All cadaveric specimens were successfully secured on the “Scaph-splint” without any residual motion or artifacts detected by the navigation system. Scaphoid drilling was rated as completely accurate in two, highly accurate in another two, and accurate in one cadaveric specimen. No relevant artifacts of the 3D fluoroscopic scans due to the splint or the fixation straps were found (Fig. 3c). No specimen required repeated drilling of the scaphoid. However, in one specimen the proximal scaphoid pole was perforated by the drill.
Relative motion analysis
The mean change in the Euclidean distance between the scaphoid and splint across all five specimens was 0.4 mm (range 0.2–0.7 mm, standard deviation 0.2 mm). No clinically significant differences were demonstrated for the relative motion measurements from testing of the five specimens.
Clinical case
There were no technical problems encountered while performing the navigated drilling procedures. The reference marker remained stable throughout testing. Verification of registration showed accuracy to within less than 1 mm. The quality of the images was satisfactory in all cases. The postoperative X-rays confirmed a satisfactory result (Fig. 6). The complete operative time was 180 min. The time taken to acquire images for each scan was 190 s.
Discussion
Internal fixation of scaphoid fractures remains a challenging task. Central placement of the screw in the scaphoid has been shown to offer a biomechanical advantage in the internal fixation of scaphoid fractures [9, 18]. In the current study, we used 3D navigation to optimize scaphoid screw placement. Navigation and CAS have become increasingly popular in the field of orthopedic surgery, because they have been shown to improve the accuracy of surgical procedures [5, 13]. Accurate navigation requires registration of motion-free reference markers near the anatomic region of interest [7]. The small yet complex anatomy of the wrist and the carpal bones make establishing stable reference markers rather difficult. However, the “Scaph-splint” enables accurate surgical planning and placement of a scaphoid screw. With polysulfon as the base material of its structure, we were able to minimize potential signal artifacts by reducing the amount of metal in the surgical field. This is particularly important in small anatomic regions where the use of Iso-C 3D in combination with metal-containing objects can produce enough artifact to decrease the accuracy of navigated surgical planning and precision during registration [6].
Accurate evaluation and fixation of scaphoid fractures with 2D fluoroscopy can be a challenging task, even for the experienced hand surgeon. Computed tomography can provide valuable information about the anatomical details of the scaphoid, thus simplifying surgical planning [2, 10]. Liverneaux et al. [17] have previously used 2D fluoroscopy to successfully insert navigated scaphoid screws. In their study, they utilized a device to immobilize the wrist and hand for accurate screw placement. Their study, however, lacked the additional power provided by 3D fluoroscopy. The CT-like images that are produced by Iso-C 3D demonstrate the anatomy of the scaphoid in sagittal, coronal, and frontal planes, thus improving the accuracy and precision of navigated screw placement. Our results demonstrated that in four out of five specimens a highly accurate screw trajectory was achieved. In addition, no repeated drilling trials or misdirection of the screw occurred.
The limitations of this study include the use of cadaveric specimens, the number of specimens, and screw placement in intact, non-fractured scaphoids. The use of fresh cadaveric specimens was necessary because this was the first time that the “Scaph-splint” in combination with 3D fluoroscopy was used for navigated scaphoid screw placement. In our second study, we demonstrated that there was no clinically significant motion between the scaphoid and the splint. The limitations of this arm of the study were similar to those already mentioned and in addition, specimens from non-fractured scaphoids were utilized.
In its first clinical use, it was necessary to use a 1-mm K-wire. In previous studies, it was reported that a limitation of navigated drilling was the obligation to use a 2.5 mm or greater sized drill bit [13]. To address this problem we developed a custom-made navigated aiming device, which is fixed to a movable and lockable arm. The device was fixed following data acquisition, in order to reduce any imaging artifacts. The operative time was longer than usual due to the introduction of the new technology. The authors believe that subsequent cases will see a reduction in operative time due a flattening of the learning curve. Despite the complicated unstable condition of the wrist fracture being treated, we were successful in our use of the navigation system for screw replacement. This shows that the degree of immobilization of the wrist employed was sufficient in this case; however, we would need to increase the number of such cases to establish whether this system is truly beneficial and effective.
Conclusions
Despite the inherent limitations of our study, we concluded that the use of the “Scaph-splint” in combination with 3D fluoroscopy increases the accuracy of navigated scaphoid screw placement. Moreover, 3D fluoroscopy allows for an immediate intraoperative control of the screw placement in our pilot study.
References
Adams BD, Blair WF, Reagan DS, Grundberg AB (1988) Technical factors related to Herbert screw fixation. J Hand Surg Am 13:893–899
Bain GI, Bennett JD, MacDermid JC, Slethaug GP, Richards RS, Roth JH (1998) Measurement of the scaphoid humpback deformity using longitudinal computed tomography: intra- and interobserver variability using various measurement techniques. J Hand Surg Am 23:76–81
Citak M, Board TN, Sun Y, Look V, Krettek C, Hufner T, Kendoff D (2007) Reference marker stability in computer aided orthopedic surgery: a biomechanical study in artificial bone and cadavers. Technol Health Care 15:407–414
Citak M, Hufner T, Geerling J, Kfuri M Jr, Gansslen A, Look V, Kendoff D, Krettek C (2006) Navigated percutaneous pelvic sacroiliac screw fixation: experimental comparison of accuracy between fluoroscopy and Iso-C3D navigation. Comput Aided Surg 11:209–213
Citak M, Kendoff D, Kfuri M Jr, Pearle A, Krettek C, Hufner T (2007) Accuracy analysis of Iso-C3D versus fluoroscopy-based navigated retrograde drilling of osteochondral lesions: a pilot study. J Bone Joint Surg Br 89:323–326
Citak M, Kendoff D, Wanich T, Look V, Stuber V, Geerling J, Krettek C, Hufner T (2008) The influence of metal artifacts on navigation and the reduction of artifacts by the use of polyether-ether-ketone. Comput Aided Surg 13:233–239
Citak M, Kendoff D, Wanich T, Pearle A, Singhai R, Krettek C, Hufner T (2006) The influence of distance on registration in ISO-C-3D navigation: a source of error in ISO-C-3D navigation. Technol Health Care 14:473–478
Dias JJ, Wildin CJ, Bhowal B, Thompson JR (2005) Should acute scaphoid fractures be fixed? A randomized controlled trial. J Bone Joint Surg Am 87:2160–2168
Dodds SD, Panjabi MM, Slade JF 3rd (2006) Screw fixation of scaphoid fractures: a biomechanical assessment of screw length and screw augmentation. J Hand Surg Am 31:405–413
Frahm R, Lowka K, Vinee P (1992) Computerized tomography diagnosis of scaphoid fracture and pseudarthrosis in comparison with roentgen image. Handchir Mikrochir Plast Chir 24:62–66
Gebhard FT, Kraus MD, Schneider E, Liener UC, Kinzl L, Arand M (2006) Does computer-assisted spine surgery reduce intraoperative radiation doses? Spine 31:2024–2027 (discussion 2028)
Herbert TJ, Fisher WE, Leicester AW (1992) The Herbert bone screw: a ten year perspective. J Hand Surg Br 17:415–419
Hufner T, Geerling J, Oldag G, Richter M, Kfuri M Jr, Pohlemann T, Krettek C (2005) Accuracy study of computer-assisted drilling: the effect of bone density, drill bit characteristics, and use of a mechanical guide. J Orthop Trauma 19:317–322
Kendoff D, Bogojevic A, Citak M, Citak M, Maier C, Maier G, Krettek C, Hufner T (2007) Experimental validation of noninvasive referencing in navigated procedures on long bones. J Orthop Res 25:201–207
Kendoff D, Citak M, Gardner MJ, Stubig T, Krettek C, Hufner T (2009) Intraoperative 3D imaging: value and consequences in 248 cases. J Trauma 66:232–238
Kotsianos D, Wirth S, Fischer T, Euler E, Rock C, Linsenmaier U, Pfeifer KJ, Reiser M (2004) 3D imaging with an isocentric mobile C-arm comparison of image quality with spiral CT. Eur Radiol 14:1590–1595
Liverneaux PA, Gherissi A, Stefanelli MB (2008) Kirschner wire placement in scaphoid bones using fluoroscopic navigation: a cadaver study comparing conventional techniques with navigation. Int J Med Robot 4:165–173
McCallister WV, Knight J, Kaliappan R, Trumble TE (2003) Central placement of the screw in simulated fractures of the scaphoid waist: a biomechanical study. J Bone Joint Surg Am 85-A:72–77
Moran R, Curtin J (1988) Scaphoid fractures treated by Herbert screw fixation. J Hand Surg Br 13:453–455
Muller M, Chen ZB, Al Morshidy A, Germann G, Sauerbier M (2006) Postoperative CT-controlled results of renewed osteosynthesis using screw fixation for acute scaphoid fractures. Unfallchirurg 109:185–192
Tumilty JA, Squire DS (1996) Unrecognized chondral penetration by a Herbert screw in the scaphoid. J Hand Surg Am 21:66–68
Whipple TL (1995) Stabilization of the fractured scaphoid under arthroscopic control. Orthop Clin North Am 26:749–754
Conflict of interest statement
None of the authors have had any financial or personal relationships with other people or organizations that could inappropriately influence (bias) their work, within 3 years from the beginning of this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Citak, M., O’Loughlin, P.F., Kendoff, D. et al. Navigated scaphoid screw placement using customized scaphoid splint: an anatomical study. Arch Orthop Trauma Surg 130, 889–895 (2010). https://doi.org/10.1007/s00402-010-1044-0
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-010-1044-0