Abstract
Introduction
In this paper the SpinalMouse, a new computerised external device for measuring sagittal spinal range of motion (ROM), was tested for inter-rater reliability and use in clinical practice.
Materials and methods
To assess inter-rater reliability, two investigators each measured 111 subjects.
Results
Correlation coefficients were found to be r=0.90 for flexion, r=0.85 for extension and r=0.90 for total inclination. Intra-class coefficients were 0.95 for flexion, 0.92 for extension and 0.95 for total inclination. A poor agreement (kappa=0.22) was found for the presence of outliers from normal values for intersegmental ROM.
Conclusion
We conclude the device is a useful, reliable tool for measuring sagittal spinal ROM in clinical practice, considering the small load it confers on patients and the short amount of time the measurement involves. The SpinalMouse might be more accurate after following the recommendations we make.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
During the past 30 years, numerous studies have been published about spinal range of motion (ROM), and many methods of measurement have been described. One of the most frequently used methods involves radiological analysis which can be performed in multiple ways (CT, plain and biplanar radiography) [4, 6, 8, 10, 11, 12, 19, 22, 24]. A limitation of this method is the relatively high dose of radiation it requires, which precludes the use of the radiograph as a routine measurement in clinical practice. Therefore, many non-invasive, external methods have been developed: goniometers, skin markers, inclinometers, spondylometers, measurement of back surface curvature and opto-electronic systems, some of them computer aided, each with its specific characteristics [2, 9, 14, 16, 17, 21, 22]. External methods for measuring spinal ROM are now commonly used because they are easy to apply, non-invasive and take little clinical time [21].
We used the SpinalMouse to measure sagittal spinal ROM. It is a non-invasive electronic computer-aided device, which is manually guided paravertebrally along the spinal column. It measures spinal ROM as well as intersegmental ROM. A relatively unique feature of the device is that it measures thoracic, lumbar and sacral/hip mobility separately. Data about the SpinalMouse have not yet been published.
This study was designed to test the SpinalMouse’s inter-rater reliability as well as to judge the device on its merits in clinical practice.
Materials and methods
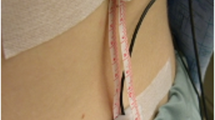
Measurement of spinal ROM was done with the SpinalMouse (Idiag, Volkerswill, Switzerland), an electronic computer-aided measuring device, which measures sagittal spinal ROM and intersegmental angles in a non-invasive way, a so-called surface-based technique (Fig. 1). The device is connected radiographically via an analog-digital converter to a standard PC. After supplying basic data of the patient, including height, weight, sex and age, the SpinalMouse is run paravertebrally along the spinal column from C7 to the rima ani (S3). The patient is asked to take three consecutive positions: erect, in maximal flexion and maximal extension of the spine. In each position a measurement is performed.
When manually guided paravertebrally along the spine of a subject, the system records the outline of the skin over the spinal column in the sagittal plane. The local angle or inclination relative to a perpendicular line is given at any position by an internal pendulum connected to a potentiometer. An ‘intelligent recursive algorithm’ computes information concerning the relative position of the vertebral bodies of the underlying bony spinal column. Raw data of the SpinalMouse measurements are the superficial back length from C7 to S3 and the local angle of each point of this length relative to the plumb line. In this manner, spinal ROM and 17 segments (Th1/2-L5/S1) are evaluated.
All measurements are summarised in a table, which consists of six columns: the first three columns contain the values for posture in the sequence upright, flexion and extension (kyphotic angles are expressed as positive values, lordotic angles as negative values). The last three columns refer to the calculated mobility in the sequence flexion minus upright, upright minus extension, and flexion minus extension (the latter being equal to ROM). At the foot the contribution of the thoracic spine, lumbar spine and sacral spine/hip to total mobility is expressed, as well as length of the back (in mm) and inclination (inclination as flexion minus extension is similar to total inclination) (Table 1). Figure 2 shows the superficial back shape; in the right corner the inclination is drawn, which represents full mobility of the trunk, composed of thoracic, lumbar and sacral/hip mobility.
Sagittal shape of the back and inclination in flexed, upright and extended positions (same patient as Table 1)
The developer of the SpinalMouse claims to have measured 180 healthy volunteers without a history of back complaints (using a preliminary version of the device) and so created a database of age- and gender-specific normal values for intersegmental ROM. The SpinalMouse software (version 2.3) supplies a graph in which the calculated intersegmental ROM is compared with these normal values (Fig. 3).
Graphic demonstration of the calculated measurements of intersegmental ROM as shown in Table 1, compared to age- and gender-specific normal values
Study group
The study group consisted of 111 subjects aged between 21 and 60 years old (mean age 39.2 years, mean height 1.78 m, mean weight 79.3 kg, mean BMI 24.7 kg/m2; 75 men, 36 women). Forty-two were healthy volunteers, 69 subjects had sustained a spinal fracture (35 treated conservatively and 34 treated surgically). The spinal fracture patients were included because we used their ROM in another study [23]. All spinal fracture patients sustained their fracture at least 1.5 years previously, none of them had any neurological deficit.
Measurement
To assess inter-rater reliability, two investigators (RBP and VJML) measured the patients in succession. Observer one completed a full measurement (patient upright, in flexion and extension) after which observer two performed a full measurement. Subjects were asked to try to touch their toes with their fingers with their knees straight, with the neck slightly flexed and their feet approximately 30 cm apart. For extension, subjects were asked to extend their back as far as possible, without external help. The SpinalMouse was placed at C7 (found by palpation after instructing the patient to bend the head slightly to the chest) and manually guided to the rima ani in a paravertebral manner. No ‘warming up’ was performed before the measurement. The following was tested for inter-rater reliability: inclination in flexion; inclination in extension; total inclination; measured length of the back as flexion minus extension. Also, the presence of outliers from normal values for intersegmental ROM was tested for inter-rater reliability.
Statistical analysis
Statistical analysis was done with SPSS version 10 (SPSS Chicago, IL, USA). Length of the back and inclination were tested by means of the intra-class correlation coefficient (ICC) and Pearson’s correlation coefficient r [20, 25]; mean values measured by the two investigators were compared by means of the paired t-test. No universally acceptable levels have been adopted for expressing the reliability of measurements when ICC values are calculated [13]. However, one proposed scheme for defining the amount of reliability with ICCs has the following values: 0.99–0.90 high reliability; 0.89–0.80 good reliability; 0.79–0.70 fair reliability and 0.69 and below poor reliability [18]. The presence of outliers from normal values for intersegmental ROM was tested by means of Cohen’s kappa. Cohen’s kappa measures the agreement between the evaluations of two raters when both are rating the same object. A value of 1 indicates perfect agreement, a value of 0 indicates that agreement is no better than chance. A p-value of 0.05 was considered significant.
Results
Correlation coefficients and ICC are shown in Table 2, as well as mean values measured by the two observers.
For inclination (total inclination, flexion and extension) ICCs were 0.92 and 0.95; all Pearson’s correlation coefficients were significant (p<0.001). The relationship between total inclination as measured by observer one and observer two is shown in Fig. 4. Observer one measured a higher mean total inclination than observer two (p<0.05), and mean extension as measured by observer one was higher than that measured by observer two (p<0.05). There was no significant difference between mean flexion as measured by both observers (p=0.830).
Reliability for measurement of the length of the back as flexion−extension was as follows: r=0.61 (p<0.001), ICC=0.76. Mean values measured by observer one were higher than those measured by observer two (p<0.05). Figure 5 shows the relationship between measured length of the back (flexion–extension) between observer one and observer two.
Cohen’s kappa for the presence of outliers from normal values for intersegmental ROM was 0.22.
Discussion
This study was designed to test a new device for measuring sagittal spinal ROM. We chose to do this by means of inter-rater reliability. We did not assess intra-rater reliability, because that would mean patients would have to bow and extend two more times, and should be done on separate days, which was not possible for time and logistic reasons.
Inclination in flexion, inclination in extension and total inclination were found to be highly reliable; however, some differences were found between the mean results. When taking into account that both measurements were done successively (so the first measurement might influence the second), and the fact that patients might not take exactly the same position during two consecutive measurements, some differences in results were to expected. As mentioned by Portek et al., subject repeatability is a major contributing factor in the measurement of spinal mobility [22]. A significant difference for extension and total inclination was found. Considering extension, a large part of our study group encountered problems (e.g. maintaining balance) when standing in extension. As reported in the literature, extension in standing is uncomfortable, and the subject may find it difficult to maintain balance [3, 21]. This might explain the mean difference for extension (2.4 deg) found between the two investigators. Besides this subject repeatability, the difference might also result from the device itself, or a cumulative effect of these two entities. For total inclination, a similar difference was found (2.1 deg). However, it can be questioned whether such a small difference is a clinically important finding.
Inter-rater reliability for the difference of the back’s length from flexion to extension was found to be fair. There was a small but significant difference between the two investigators (6.8 mm). As pointed out by Mayer et al. in a previous study, variability among examiners in locating bony landmarks is a major contributing factor in the external measurement of spinal ROM [15]. When performing one complete measurement, C7 needs to be palpated three times and has to be stopped at S3 three times, which makes a total of six possible errors per measurement. Accumulation of these possible errors might be an explanation for the difference found in measured length. Considering this, a possibility might be to mark C7 and S3 with a skin marker after palpating both precisely. By doing so, the length of the back might be measured more accurately. However, during flexion these skin markers will shift in relation to the underlying vertebra. Another possible explanation for the difference found is a slightly different pathway taken along the spinal curvature.
A poor agreement was found for the presence of outliers from normal values for intersegmental ROM (kappa 0.22). We cannot, however, ascertain whether the developer’s graph with normal intersegmental ROM data was obtained in a reliable way, since no accompanying publication is available. For now, we conclude that the SpinalMouse is not very reliable in measuring intersegmental ROM.
Comparison of our results with the literature is difficult because no studies have been published concerning the SpinalMouse so far. In a study by Keeley et al., using a two-inclinometer technique that is to some extent comparable, inter-rater correlation was found to be good: r=0.92 (p<0.001) [7]. However, in that study only lumbar and hip mobility were measured, whereas thoracic mobility was not. Chen found a computerised single-sensor inclinometer to have a poor inter-rater reliability (ICC 0.39 for extension and ICC 0.69 for flexion) [1]. In another study the inter-rater reliability for the CA-6000 spine motion analyzer (a computerized potentiometer) was as follows: flexion r=0.76; extension r=0.84; flexion+extension r=0.84; compared with these data our results seem favourable. However, only lumbar ROM was measured in that study [5].
The data we report for sagittal spinal ROM cannot be seen as normal values. First, we measured patients with a spinal fracture in the past as well as healthy volunteers. In addition, we used inclination for comparison, which, as pointed out before, consists of thoracic, lumbar as well as sacral/hip mobility. For assessment of inter-rater reliability, this is not important, but it should be taken into account when comparing data with earlier studies, which mostly report on lumbar mobility. Mellin reports on thoracolumbar ROM in his study concerning the Myrin inclinometer, but he did not measure hip mobility, and his population consisted of 25 healthy volunteers, so comparison of our data to his data is not reliable [17]. To validate the ability of the device to measure sagittal spinal ROM and intersegmental ROM, a comparison between the SpinalMouse’s data and radiographs could have been made. It is questionable, however, whether radiographs should be chosen as the ‘gold standard’. The use of radiographs is probably unjustifiable in terms of patient risk and cost (especially when, as in this study, the whole spinal column needs to be assessed). Because of this, and the fact that 2/3 of our study group consisted of patients with a spinal fracture in the past, we have not been able to validate the SpinalMouse.
Clinical use
When using the SpinalMouse, we encountered a number of pitfalls. When measuring subjects much taller than the investigator, it is difficult to place the SpinalMouse exactly on C7 and to see the LED on the mouse, which indicates that the device is ready for use. To overcome these problems, it might be useful to have a little stool for the investigator to stand on. Another problem we encountered was controlling the skin surface in lumbar lordosis in extension. Sometimes, the SpinalMouse could not pass the lumbar angle properly because the angle was too sharp, and the wheels of the mouse slipped as a result.
Concerning the clinical time and the user-friendliness, we are fairly satisfied. One complete measurement takes about 1 min, the device is not velocity sensitive, and after some training the SpinalMouse is rather simple to use.
Of course, there are some limitations concerning this study. Investigators were not blinded to the subjects’ diagnosis. Another issue that should be kept in mind is that comparison with the literature is not possible, since no publication concerning the SpinalMouse is available.
Conclusion
The SpinalMouse seems to be a good, reliable device for measuring sagittal spinal ROM, as tested by inter-rater reliability. After following the recommendations we made, the device might be more accurate. Correlation coefficients found were fair to good; there was a significant difference between mean total inclination as well as mean extension as measured by the two investigators, but this difference was so small that it would not be of major influence in clinical practice. For measuring intersegmental ROM, the SpinalMouse does not seem to be a reliable tool yet. Considering the short clinical time needed for measurement and the low health risk posed to the patient, the SpinalMouse could be used as a reliable objective tool for measuring sagittal spinal ROM. Intra-rater reliability needs to be assessed in a further study.
References
Chen SP, Samo DG, Chen EH, Crampton AR, Conrad KM, Egan L, Mitton J (1997) Reliability of three lumbar sagittal motion measurement methods: surface inclinometers. J Occup Environ Med 39:217–223
Chiou WK, Lee YH, Chen WJ, Lin YH (1996) A non invasive protocol for the determination of lumbar spine mobility. Clin Biomech 11:474–480
Dillard J, Trafimow J, Andersson GB, Cronin K (1991) Motion of the lumbar spine. Reliability of two measurement techniques. Spine 16:321–324
Dodd CA, Fergusson CM, Pearcy MJ, Houghton GR (1986) Vertebral motion measured using biplanar radiography before and after Harrington rod removal for unstable thoracolumbar fractures of the spine. Spine 11:452–455
Dopf CA, Mandel SS, Geiger DF, Mayer PJ (1994) Analysis of spine motion variability using a computerized goniometer compared to physical examination. A prospective clinical study. Spine 19:586–595
Johnsson R, Selvik G, Stromqvist B, Sunden G (1990) Mobility of the lower lumbar spine after posterolateral fusion determined by roentgen stereophotogrammetric analysis. Spine 15:347–350
Keeley J, Mayer TG, Cox R, Gatchel RJ, Smith J, Mooney V (1986) Quantification of lumbar function. Part 5. Reliability of range-of-motion measures in the sagittal plane and an in vivo torso rotation measurement technique. Spine 11:31–35
Knop C, Fabian HF, Bastian L, Blauth M (2001) Late results of thoracolumbar fractures after posterior instrumentation and transpedicular bone grafting. Spine 26:88–99
Lee YH, Chiou WK, Chen WJ, Lee MY, Lin YH (1995) Predictive model of intersegmental mobility of lumbar spine in the sagittal plane from skin markers. Clin Biomech 10:413–420
Leferink VJM, Zimmerman KW, Veldhuis EFM, Vergert EM ten, Duis HJ ten (2001) Thoracolumbar spinal fractures: radiological results of transpedicular fixation combined with transpedicular cancellous bone graft and posterior fusion in 183 patients. Eur Spine J 10:517–523
Lim TH, Eck JC, An HS, McGrady LM, Harris GF, Haughton VM (1997) A noninvasive, three-dimensional spinal motion analysis method. Spine 22:1996–2000
Lindsey RW, Dick W, Nunchuck S, Zach G (1993) Residual intersegmental spinal mobility following limited pedicle fixation of thoracolumbar spine fractures with the fixateur interne. Spine 18:474–478
Madson TJ, Youdas JW, Suman VJ (1999) Reproducibility of lumbar spine range of motion measurements using the back range of motion device. J Orthop Sports Phys Ther 29:470–477
Mannion A, Troke M (1999) A comparison of two motion analysis devices used in the measurement of lumbar spinal mobility. Clin Biomech 14:612–619
Mayer RS, Chen IH, Lavender SA, Trafimow JH, Andersson GB (1995) Variance in the measurement of sagittal lumbar spine range of motion among examiners, subjects, and instruments. Spine 20:1489–1493
Mayer TG, Kondraske G, Beals SB, Gatchel RJ (1997) Spinal range of motion. Accuracy and sources of error with inclinometric measurement. Spine 22:1976–1984
Mellin G (1986) Measurement of thoracolumbar posture and mobility with a Myrin inclinometer. Spine 11:759–762
Meyers CR, Blesh TE (1962) Measurement in physical education. Ronald Press, New York
Miyasaka K, Ohmori K, Suzuki K, Inoue H (2000) Radiographic analysis of lumbar motion in relation to lumbosacral stability. Investigation of moderate and maximum motion. Spine 25:732–737
Muller R, Buttner P (1994) A critical discussion of intraclass correlation coefficients. Stat Med 13:2465–2476
Ng JK, Kippers V, Richardson CA, Parnianpour M (2001) Range of motion and lordosis of the lumbar spine: reliability of measurement and normative values. Spine 26:53–60
Portek I, Pearcy MJ, Reader GP, Mowat AG (1983) Correlation between radiographic and clinical measurement of lumbar spine movement. Br J Rheumatol 22:197–205
Post RB, Leferink VJM (2003) Sagittal range of motion after a spinal fracture; does ROM correlate with functional outcome? Eur Spine J (in press)
Schlegel JD, Smith JA, Schleusener RL (1996) Lumbar motion segment pathology adjacent to thoracolumbar, lumbar, and lumbosacral fusions. Spine 21:970–981
Shrout PE, Fleiss JL (1979) Intraclass correlations: uses in assessing rater reliability. Psychol Bull 86:420–428
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Post, R.B., Leferink, V.J.M. Spinal mobility: sagittal range of motion measured with the SpinalMouse, a new non-invasive device. Arch Orthop Trauma Surg 124, 187–192 (2004). https://doi.org/10.1007/s00402-004-0641-1
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-004-0641-1