Abstract
Solanezumab and Crenezumab are two humanized antibodies targeting Amyloid-β (Aβ) which are currently tested in multiple clinical trials for the prevention of Alzheimer’s disease. However, there is a scientific discussion ongoing about the target engagement of these antibodies. Here, we report the immunohistochemical staining profiles of biosimilar antibodies of Solanezumab, Crenezumab and Bapineuzumab in human formalin-fixed, paraffin-embedded tissue and human fresh frozen tissue. Furthermore, we performed a direct comparative immunohistochemistry analysis of the biosimilar versions of the humanized antibodies in different mouse models including 5XFAD, Tg4-42, TBA42, APP/PS1KI, 3xTg. The staining pattern with these humanized antibodies revealed a surprisingly similar profile. All three antibodies detected plaques, cerebral amyloid angiopathy and intraneuronal Aβ in a similar fashion. Remarkably, Solanezumab showed a strong binding affinity to plaques. We also reaffirmed that Bapineuzumab does not recognize N-truncated or modified Aβ, while Solanezumab and Crenezumab do detect N-terminally modified Aβ peptides Aβ4–42 and pyroglutamate Aβ3–42. In addition, we compared the results with the staining pattern of the mouse NT4X antibody that recognizes specifically Aβ4–42 and pyroglutamate Aβ3–42, but not full-length Aβ1–42. In contrast to the biosimilar antibodies of Solanezumab, Crenezumab and Bapineuzumab, the murine NT4X antibody shows a unique target engagement. NT4X does barely cross-react with amyloid plaques in human tissue. It does, however, detect cerebral amyloid angiopathy in human tissue. In Alzheimer mouse models, NT4X detects intraneuronal Aβ and plaques comparable to the humanized antibodies. In conclusion, the biosimilar antibodies Solanezumab, Crenezumab and Bapineuzumab strongly react with amyloid plaques, which are in contrast to the NT4X antibody that hardly recognizes plaques in human tissue. Therefore, NT4X is the first of a new class of therapeutic antibodies.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
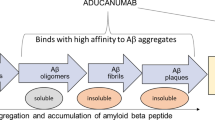
The amyloid-β hypothesis has been the most influential hypothesis for Alzheimer’s disease (AD) and an important basis for the development of novel therapeutic strategies. The hypothesis suggests that increased Aβ production or decreased Aβ clearance leads to accumulation of hydrophobic Aβ40 and Aβ42 and the formation of insoluble extracellular plaques [29]. Plaques then trigger a cascade of toxic changes eventually resulting in synapse loss, neuron loss, brain atrophy and dementia [53]. If the amyloid-β hypothesis is indeed correct, intervening in the cascade and removing Aβ from the brain should prevent neuron loss and cognitive decline. The main therapeutic intervention strategies directed at Aβ include reducing Aβ production, assisting Aβ clearance and preventing the aggregation of Aβ [55]. Active and passive immunotherapy procedures are considered to be among the most promising approaches to prevent or treat AD and over the last decade various anti-Aβ antibodies have been developed [24, 55].
Bapineuzumab was the first antibody used in a passive immunotherapy clinical trial. The humanized antibody developed by Pfizer and Johnson & Johnson targets the N-terminal region of Aβ binding fibrillar and soluble Aβ [68]. Bapineuzumab is the only antibody reported to clinically decrease the brain amyloid burden as well as reduce Tau and phosphorylated-Tau levels in the CSF in mild to moderate AD patients [9, 59]. However, large-scale phase three clinical trials were discontinued in 2012 as treatment evoked vasogenic edema and did not improve measures of cognitive decline in mild or moderate AD patients relative to placebo controls [9, 60, 69].
Several passive immunotherapy trials are currently ongoing [1]. Among them, Crenezumab (Genentech) and Solanezumab (Eli Lilly) are the leading clinical Aβ antibodies tested in multiple Phase II or III clinical trials [1]. These humanized monoclonal antibodies are highly homologous and target the mid-region of Aβ [14, 71]. Solanezumab is reported to bind preferentially to soluble monomers rather than fibrillar Aβ [65, 71]. Early clinical trials with Solanezumab showed increased CSF Aβ levels and large Phase 3 clinical trials reported that treatment with Solanezumab slowed down the cognitive decline in mild AD, but not in moderate AD patients [19, 68]. Crenezumab has a binding affinity to Aβ fibrils, oligomers and monomers [2]. The antibody, which unlike Solanezumab and Bapineuzumab is built on an IgG4 backbone, is currently being tested in several Phase II trials.
Several pre-clinical studies have demonstrated beneficial effects of passive immunotherapy against other therapeutic Aβ targets. N-truncated and modified Aβ species are highly represented in the earliest stages of AD as well as in fully developed AD and may, therefore, be potential therapy targets. For example, anti-pyroglutamate Aβ3–42 antibodies reduced the plaque burden in AD mice, in the absence of microhemorrhage or increased vascular amyloid [17, 22, 75]. Aβ4–42 is another abundant species in AD that is as toxic as AβpE3−42 and Aβ1–42 may, therefore, be a potential target for immunotherapy approaches [7].
In the present study, we performed a direct comparative immunohistochemistry analysis of the biosimilar versions of the humanized antibodies Bapineuzumab, Crenezumab and Solanezumab. The aim of the study was to investigate the binding profiles of these antibodies in different mouse models as well as in human tissue and compare the humanized antibodies with NT4X, an antibody that binds to the N-terminus of N-truncated Aβ especially Aβ4−x.
Materials and methods
Human specimens
The brains of 35 sporadic AD patients (SAD; 32 females/3 males, mean age; mean age ± SEM 81.4 ± 1.58; Braak stage 4–6; ApoE4: 17/35) and 5 non-demented control patients (1 female/4 males, mean age ± SEM 81 ± 4.65; Braak stage 0–1) were analyzed (Table 1). All human cortical brain samples were obtained from the Netherlands Brain Bank (NBB, Amsterdam, The Netherlands) [56]. NBB works with a rapid autopsy program to minimize postmortem delay (PMD). Definite diagnosis was based on established criteria and written informed consent was obtained from all subjects. The control subjects did not suffer from any primary neurological or psychiatric disease or brain metastases nor did they have a history of medication or drug treatment. The inclusion as a control donor is based both on review of medical records and on the Braak stage by the Netherlands Brain Bank. All sporadic AD patients had Reisberg Scales of four or higher. The Reisberg Scale is used by caregivers as clinical diagnostic criteria and divided into seven different stages. Stages 4–7 are dementia stages, while stages 1–3 are pre-dementia stages [57].
Animal models
In this study, five established AD-like transgenic mouse lines (Table 2) were used: Tg4-42 [10], TBA42 [77], 5XFAD [48], APP/PS1KI [12] and 3xTg [49].
Tg4-42 mice express human Aβ4–42 fused to the murine TRH signal peptide under the control of the neuronal Thy-1 promoter [10]. TBA42 mice express Aβ3Q−42 fused to the murine TRH signal peptide under the control of the neuronal Thy-1 promoter. The glutamate at position three of the Aβ amino acid sequence is mutated into glutamine to facilitate enhanced pyroglutamate formation. These mice express unmodified Aβ3Q−42, which can be readily converted to AβpE3−42 by glutaminyl cyclase [43, 77]. 5XFAD mice overexpress the 695 amino acid isoform of the human amyloid precursor protein (APP695) carrying the Swedish, London and Florida mutations under the control of the murine Thy1-promoter. In addition, human presenilin-1 (PSEN-1) carrying the M146L/L286V mutations is expressed under the control of the murine Thy1-promoter [48]. 5XFAD mice used in the current study were backcrossed for more than ten generations to C57Bl/6J wild-type mice (Jackson Laboratories, Bar Harbor, ME, USA) to obtain an incipient congenic line on a C57Bl/6J genetic background [32]. 3xTg mice (a generous gift by Dr. Wolfgang Härtig, University of Leipzig) represent a triple-transgenic model of AD harboring three mutated transgenes: PS1-M146V, APPSwe, and tauP301L [49]. The APP/PS1KI transgenic mouse model (a generous gift by Dr. Laurent Pradier, Sanofi, Paris) carries M233T/L235P knocked-in mutations in presenilin-1 and overexpresses mutated human amyloid precursor protein carrying the London and Swedish mutations under the Thy-1 promoter [12]. APP/PS1KI mice were backcrossed for more than 10 generations on a C57BL/6J genetic background.
All animal experiments were conducted in accordance with the German guidelines for animal care and approved by the local legal authorities (LAVES).
Immunohistochemistry
Mice were killed via CO2 anesthetization followed by cervical dislocation. Brain samples were carefully dissected and post-fixed in 4 % phosphate-buffered formalin at 4 °C.
Human and mouse tissue samples were processed as previously described [10, 73]. In brief, 4 μm paraffin sections were deparaffinized in xylene, followed by rehydration in a series of ethanol. After H2O2 treatment to block endogenous peroxidases, sections were boiled in 0.01 M citrate buffer for antigen retrieval, followed by a 3-min incubation in 88 % formic acid. Non-specific binding sites were blocked by treatment with skim milk and fetal calf serum in PBS, prior to the addition of the primary antibodies. The following biosimilar antibodies (BS) were used (Table 3): BapineuzumabBS (1:2500; 0.7 mg/ml), CrenezumabBS (1:2500; 0.85 mg/ml), SolanezumabBS (1:2500; 1.5 mg/ml) and NT4X (1:200; 2 mg/ml) [4, 14, 44]. Corresponding biotinylated secondary anti-human and anti-mouse antibodies (1:200) were purchased from DAKO (Glostrup, Denmark). Staining was visualized using the ABC method, with a Vectastain kit (Vector Laboratories, Burlingame, USA) and diaminobenzidine (DAB) as chromogen. Counterstaining was carried out with hematoxylin.
In addition to formalin-fixed, paraffin-embedded tissue fresh frozen cortical human brains and mouse brain hemispheres were embedded in Tissue-Tec (Sakura, Torrance, USA) and cut sagittal into entire series of 10 μm thick sections on a CM1850 UV cryostat (Leica, Wetzlar, Germany). Brains were mounted onto superfrost slides and fixed in −20 °C methanol. After hydration in PBS and H2O2 treatment to block endogenous peroxidases, sections were washed and incubated in 88 % formic acid for 3 min. Non-specific binding sites were blocked by treatment with skim milk and fetal calf serum in PBS. Prior to the addition of the antibodies the human antibodies BapineuzumabBS, CrenezumabBS and SolanezumabBS were biotinylated with a Biotinylation kit (EZ-Link Sulfo-NHS-LC-Biotinylation Kit) according to the instruction of the manufacturer (Thermo Scientific, Waltham, USA). Section was incubated over-night with biotinylated BapineuzumabBS, CrenezumabBS and SolanezumabBS as well as NT4X. Staining was visualized using the ABC method, with a Vectastain kit (Vector Laboratories, Burlingame, USA) and diaminobenzidine (DAB) as chromogen. Counterstaining was carried out with hematoxylin.
Bright field images of DAB-immunostained tissue were acquired using a BX-51 microscope equipped with a Camera (Olympus, Tokyo, Germany). The semiquantitative analysis of plaque pathology and congophilic amyloid angiopathy (CAA) in formalin-fixed and paraffin-embedded tissue was based on Aβ staining intensity according to the following scale: −: no staining; (+): barely perceptible staining; +: weak staining; ++: moderate staining; +++: intense staining. All slides were assessed by two observers with no significant inter-observer variability. Figures were created with GraphPad Prism V6 for Windows (GraphPad Software, San Diego, CA, USA).
Amyloid plaque load quantification of human brain samples
Plaque load was quantified in formalin-fixed and paraffin-embedded human brain samples diagnosed with sporadic AD. Brains were stained with BapineuzumabBS, CrenezumabBS, SolanezumabBS and NT4X. Furthermore, the pan-Aβ 2431-1 [10] was used as a control. For each of the 35 brains, four paraffin-embedded sections were stained simultaneously with DAB as chromogen. The relative Aβ load was evaluated in the frontal cortex using an Olympus BX-51 microscope equipped with an Olympus DP-50 camera and the ImageJ software (NIH, USA). Representative pictures of 20× magnification were systematically captured. Using ImageJ, the pictures were binarized to 8-bit black and white pictures and a fixed intensity threshold was applied defining the DAB staining. Measurements were performed for a percentage area covered by DAB staining. Statistics were calculated using GraphPad Prism V6 (GraphPad Software, San Diego, CA, USA) for Windows.
Results
The present report provides, to our best knowledge, the first comparative immunohistochemical analysis of BapineuzumabBS, CrenezumabBS and SolanezumabBS in human tissue and transgenic AD mouse models. The staining patterns of these humanized antibodies were also compared to the Aβ4−x-specific antibody NT4X.
Bapineuzumab, Crenezumab, Solanezumab and NT4X demonstrated abundant vascular binding activity in sporadic Alzheimer’s disease cases
To compare the staining patterns of BapineuzumabBS, CrenezumabBS, SolanezumabBS and NT4X cortical tissue sections were analyzed in 35 sporadic AD cases and five non-demented control cases.
Cerebral amyloid angiopathy (CAA) staining of blood vessel walls was seen with BapineuzumabBS, CrenezumabBS, SolanezumabBS and NT4X. All antibodies showed a comparable CAA staining pattern in parallel sections (Figs. 1, 3a–d). Vascular staining could be detected to variable degrees, using immunohistochemistry with BapineuzumabBS, CrenezumabBS and SolanezumabBS, in all of the sporadic AD cases as well as in some non-demented control case we investigated. With NT4X vascular immunoreactivity was observed in 32 of 35 SAD cases, but in none of the control cases.
Semiquantitative analysis of congophilic amyloid angiopathy (CAA) in sporadic and non-demented control cases. a List of demographic data and staining profiles of BapineuzumabBS, CrenezumabBS, SolanezumabBS and NT4X in sporadic AD patients and non-demented control cases. b Summary of CAA staining profiles of BapineuzumabBS, CrenezumabBS, SolanezumabBS and NT4X in SAD cases. Aβ staining intensity:− no staining; (+) barely perceptible staining; + weak staining; ++ moderate staining; +++ intense staining. BS Braak staging
Bapineuzumab, Crenezumab and Solanezumab demonstrated abundant plaque binding activity in sporadic Alzheimer’s disease cases
BapineuzumabBS and SolanezumabBS showed a highly comparable staining profile and displayed abundant extracellular immunoreactivity in all patients using formalin-fixed and paraffin-embedded tissue (Figs. 2, 3e, g, i, k). CrenezumabBS showed a lower Aβ staining intensity in most cases than BapineuzumabBS and SolanezumabBS, although considerable plaque pathology was present in all of the sporadic AD cases (Figs. 2, 3f, j). This is consistent with the reported lower binding affinity of Crenezumab (nM) for Aβ than the homologous antibody Solanezumab (pM).
Semiquantitative analysis of plaque pathology in sporadic and non-demented control cases. a List of demographic data and staining profiles of BapineuzumabBS, CrenezumabBS, SolanezumabBS and NT4X in sporadic AD patients and non-demented control cases. b Summary of plaque staining profiles of BapineuzumabBS, CrenezumabBS, SolanezumabBS and NT4X in SAD cases. Aβ staining intensity: − no staining; + barely perceptible staining; + weak staining; ++ moderate staining; +++ intense staining. BS Braak staging
Immunohistochemical staining pattern of sporadic AD brains. Cerebral amyloid angiopathy (CAA) visualized with BapineuzumabBS (a), CrenezumabBS (b), SolanezumabBS (c) and NT4X (d). All antibodies showed a comparable CAA staining pattern in cortical parallel sections (a–d). Abundant plaque pathology could be recognized with BapineuzumabBS (a, e, i), CrenezumabBS (b, f, j), and SolanezumabBS (c, g, k). In contrast, NT4X showed a preferential binding to blood vessels presenting CAA and barely recognized plaques (d, h, i). Scale bar a–d, i–l 100 µm; e–h 50 µm
In contrast to BapineuzumabBS, CrenezumabBS and SolanezumabBS, NT4X recognized only a minor portion of plaques in the brain tissue of AD patients. NT4X barely recognized plaques and in 68 % of the sporadic cases the antibody did not detect plaques at all (Figs. 2, 3e, l). Amyloid plaque load quantification of human brain samples confirmed these results (Fig. 4).
Plaque load quantification in sporadic AD cases. Immunostaining with BapineuzumabBS, CrenezumabBS, SolanezumabBS and the pan-Abeta antibody 2431-1 revealed no significant differences in the detection of plaques in sporadic AD cases. NT4X detected significantly less plaques in sporadic AD cases than BapineuzumabBS, CrenezumabBS, SolanezumabBS and pan-Abeta. One-way analysis of variance (ANOVA) followed by Bonferroni’s multiple comparison test; n = 35; ***p < 0.001, data presented as mean ± SEM
In addition abundant plaque pathology was also visualized with biotinylated BapineuzumabBS (Fig. 5a, e), biotinylated CrenezumabBS (Fig. 5b, f), and biotinylated SolanezumabBS (Fig. 5c, g) in fresh frozen tissue. We biotinylated the humanized antibodies to avoid any possible compromise by the secondary antibody.
Immunohistochemical staining pattern in fresh frozen tissue. Abundant plaque pathology visualized with biotinylated BapineuzumabBS (a, e), biotinylated CrenezumabBS (b, f), and biotinylated SolanezumabBS (c, g) in cortical human tissue. Only weak plaque staining with NT4X in fresh frozen human tissue (d). Abundant plaque pathology could be recognized with biotinylated BapineuzumabBS (i), biotinylated CrenezumabBS (j), biotinylated SolanezumabBS (k) and NT4X (l) in aged 5XFAD mice. No staining was observed under control conditions with ABC incubation alone (d) Scale bar a–d, j–l 100 µm; e–h 50 µm
Comparative immunohistochemical analysis in different mouse models of AD
The mouse lines Tg4-42, TBA42, APP/PS1KI, 5XFAD and 3xTg (Table 2) were analyzed with BapineuzumabBS, CrenezumabBS and SolanezumabBS as well as with NT4X. These five transgenic mouse lines express different Aβ forms or combinations of human mutant APP, PS1 and Tau. It is well known that all of these mouse models develop plaques and/or intraneuronal Aβ at different stages during their life.
Staining of 3xTg mice expressing both mutant APP and mutant Tau on a PS1 knock-in background revealed intraneuronal Aβ in the cortex of 18-month-old 3xTg mice with BapineuzumabBS, CrenezumabBS, SolanezumabBS and NT4X (Fig. 6a–d). Furthermore, abundant extracellular plaque staining was visible with all antibodies at the age of 18 months in the subiculum of the hippocampus (Fig. 6e–h). Intraneuronal Aβ and plaque staining was less abundant with CrenezumabBS and NT4X.
Immunohistochemical staining of 3xTg transgenic mice. Intraneuronal Aβ could be detected with BapineuzumabBS (a), CrenezumabBS (b), SolanezumabBS (c) and NT4X (d) in the cortex of 18-month-old 3xTg mice. Abundant extracellular plaque staining visible with all antibodies at the age of 18 months in 3xTg mice (e–h). Intraneuronal Aβ and plaque staining was less abundant with CrenezumabBS (b and f) and NT4X (d and h). m month. Scale bar a–d 50 μm; e–h 100 μm
APP/PS1KI mice overexpress human APP with the Swedish and London mutations on a mutant PS1 knock-in background. Abundant plaque pathology was observed among others in the cortex and hippocampus at 6 months of age (Fig. 7e–l). Furthermore, all four antibodies demonstrated intraneuronal Aβ accumulation and extracellular plaques in 2-month-old mice (Fig. 7a–d). Staining in APP/PS1KI was most abundant with BapineuzumabBS at both ages.
Immunohistochemical staining of hippocampal and cortical sections of APP/PS1KI transgenic mice. Immunostaining with BapineuzumabBS (a), CrenezumabBS (b), SolanezumabBS (c) and NT4X (d) demonstrating intraneuronal Aβ accumulation and extracellular plaques in 2-month-old APP/PS1KI mice. Abundant extracellular plaque staining in the hippocampus (e–h) and cortex (i–l) with all four antibodies at 6 months of age. Staining was most abundant with BapineuzumabBS. m months. Scale bar a–d 50 μm; i–l 100 μm; e–h 200 μm
To compare the staining pattern of NT4X, BapineuzumabBS, CrenezumabBS and SolanezumabBS in the well-established 5XFAD mouse model hemizygous and homozygous mice were studied using cortical and hippocampal sections, as these are the brain areas known to develop abundant intraneuronal and extraneuronal Aβ pathology. Immunostaining with all four antibodies demonstrated strong intraneuronal Aβ accumulation in 6-week-old homozygous 5XFAD (Fig. 7a–d). As expected, intraneuronal Aβ accumulation was observed in young, but not in aged 5XFAD mice. 5XFAD mice, overexpressing APP with the Swedish, Florida and London mutations combined with PSEN1 carrying the M146L and L286V mutations, showed abundant extracellular plaque staining with BapineuzumabBS in the hippocampus and cortex of 3-month-old hemizygous 5XFAD mice (Fig. 8e, i). Plaque staining in young 5XFAD mice was less abundant with SolanezumabBS (Fig. 8g, k). Only faint plaque staining was observed with CrenezumabBS and NT4X at 3 months of age (Fig. 8f, j, h, l). Furthermore, immunohistochemical detection of Aβ, using BapineuzumabBS, CrenezumabBS, SolanezumabBS and NT4X, showed an abundant plaque-associated pathology in 12-month-old 5XFAD mice (Fig. 8m–p). Abundant plaque pathology could also be recognized with biotinylated BapineuzumabBS (i), biotinylated CrenezumabBS (j), biotinylated SolanezumabBS (k) and NT4X (l) in aged 5XFAD mice in fresh frozen tissue.
Immunohistochemical staining of hippocampal and cortical sections of 5XFAD transgenic mice. Immunostaining with BapineuzumabBS (a), CrenezumabBS (b), SolanezumabBS (c) and NT4X (d) demonstrating intraneuronal Aβ accumulation in 6-week-old homozygous 5XFAD. Abundant extracellular plaque staining with BapineuzumabBS at the age 3 months in hemizygous 5XFAD (e and i). Plaque staining in 5XFAD mice was less abundant with SolanezumabBS (g and k). Only faint plaque staining was observed with CrenezumabBS (f and j) and NT4X (h and l) at 3 months of age. Abundant extracellular plaque staining with BapineuzumabBS (m), CrenezumabBS (n), SolanezumabBS (o) and NT4X (p) at the age of 12 months. m months, w weeks, hom homozygous. Scale bar a–d; i–p 50 μm; e–h 200 μm
In 3-month-old homozygous Tg4-42 mice, expressing Aβ4–42, strong intraneuronal immunoreactivity could be detected with CrenezumabBS, SolanezumabBS and NT4X. The three antibodies detected intraneuronal Aβ in the CA1 region of the hippocampus (Fig. 9b–d), where staining was most intense with SolanezumabBS. In contrast, no intraneuronal Aβ was observed with BapineuzumabBS in Tg4-42 mice (Fig. 9a). The inability of BapineuzumabBS to detect Aβ in Tg4-42 mice is consistent with the antibodies affinity for the N-terminus of Abeta 1−x in a helical conformation stabilized by hydrogen bonds involving amino acids 1–3, which are absent in this model [44].
Immunohistochemical staining of hippocampal sections of Tg4-42 and TBA42 transgenic mice. Positive intraneuronal immunoreactivity could be detected with CrenezumabBS (b), SolanezumabBS (c) and NT4X (d) in homozygous Tg4-42 mice. All three antibodies detected intraneuronal Aβ in the hippocampus of 3-month-old mice. No intraneuronal Aβ was observed with BapineuzumabBS (a). Intraneuronal Aβ in hippocampal TBA42 brain sections was only detected with SolanezumabBS (g). In contrast, BapineuzumabBS (e), CrenezumabBS (f) and NT4X (h) showed no parenchymal staining in 3-month-old TBA42 mice. hom homozygous. Scale bar a–d 50 μm; e–h 33 μm
In TBA42 mice that overexpress pyroglutamate Aβ3–42, intraneuronal Aβ has previously been reported predominately in the CA1 of the hippocampus [77]. However, intraneuronal Aβ in hippocampal TBA42 brain sections could only been detected with SolanezumabBS (Fig. 9g). In contrast, BapineuzumabBS, CrenezumabBS and NT4X showed no staining in 3-month-old TBA42 mice. This is consistent with the epitope specificities of BapineuzumabBS and NT4X. In the case of CrenezumabBS, this is likely due simply to the significantly lower affinity of this antibody relative to the homologous antibody SolanezumabBS.
Discussion
Currently, immunotherapy is considered to be among the most advanced and promising approaches to prevent or treat AD. The first evidence that antibodies are potential therapeutic agents for AD was reported in 1996. Solomon et al. [67] demonstrated that antibodies against the N-terminal region of Aβ prevented the formation of Aβ fibrils in vitro, disaggregated pre-formed fibrils and evoked neuroprotection against Aβ toxicity [66]. In 1999, Schenk and colleagues demonstrated in vivo that active immunization with pre-aggregated synthetic Aβ1–42 could prevent the onset of plaque formation in young mice and decelerate the progression of plaque formation in PDAPP mice [61]. Several other studies replicated these results in different mouse models suggesting that they could be translated to the clinic [15, 31, 72]. The first anti-Aβ clinical trial AN1792 used full-length Aβ1–42 in an active immunization trial, but was terminated in phase II as several treated patients developed a severe T cell-mediated immune response to the antigen giving rise to meningoencephalitis [21, 50].
Consequently, passive immunization was considered as a safer and more controllable alternative to active immunization. It was shown that peripheral administration of a monoclonal antibody against amyloid β-peptide (3D6 murine parent antibody of Bapineuzumab) was sufficient to reduce the amyloid load in PDAPP mice [5]. Further studies also demonstrated that the passive immunization approach significantly reduced CNS Aβ and restored memory deficits in the Morris Water Maze and object recognition in APP mice [11, 18, 33]. Due to the promising results in mice and the lack of possible Th-1 mediated autoimmunity, passive immunization was promptly moved to the clinic [76]. So far several different antibodies have been tested in clinical trials including Bapineuzumab, Crenezumab and Solanezumab.
Bapineuzumab (Pfizer and Johnson & Johnson) is a humanized IgG1 antibody directed against the N-terminus of Aβ recognizing the Aβ1–5 region. It is the first antibody tested in a passive immunization trial for AD [51, 68]. Two large clinical trials with mild to moderate AD patients revealed no significant benefits, leading to the termination of all phase III studies in 2012 [38, 51]. Despite the lack of cognitive improvements Bapineuzumab was able to stabilize the plaque burden and lower phosphorylated-tau levels in cerebrospinal fluid [44]. Bapineuzumab and its murine form 3D6 are reported to bind with a high affinity to various Aβ forms without cross-reacting with APP [5, 6, 36, 61, 78]. Bapineuzumab binds to the N-terminus of Aβ in a helical conformation. The N-terminus created by BACE cleavage is buried in the antibody surface, and the helical conformation might provide a possible mechanism for the antibody to exhibit differential binding to monomeric and aggregated pools of Aβ depending on the exhibition of this epitope [20, 44]. Well in line with previous findings we could show that Bapineuzumab binds strongly to plaques in transgenic APP mice as well as vascular amyloid and Aβ plaques in human formalin-fixed, paraffin-embedded tissue and fresh frozen tissue.
The antibodies Crenezumab (Genentech) and Solanezumab (Eli Lilly) are reported to be highly homologous in their antigen binding region [14, 71] and are currently in clinical phase II or III trials [1].
Crenezumab is derived from a mouse antibody binding to Aβ12–23 and is reported to bind Aβ monomers, oligomers and fibrils with equal high affinity [2]. In contrast to Bapineuzumab and Solanezumab, the humanized antibody is designed on an IgG4 backbone to reduce the risk of microglial-mediated pro-inflammatory effects, including vasogenic edema [2]. A phase I clinical trial proved safety of Crenezumab and the antibody is currently in phase II trial [1].
Here, we demonstrated a high binding affinity of CrenezumabBS in formalin-fixed, paraffin-embedded tissue and fresh frozen tissue to vascular amyloid and plaques in sporadic AD cases, however, the plaque staining intensity with CrenezumabBS was in most cases lower than with BapineuzumabBS and SolanezumabBS. Furthermore, abundant plaque pathology was detected in 5XFAD, 3xTg and APP/PS1KI mice.
Similar to Crenezumab, Solanezumab is targeted to an internal epitope of Aβ (13–28) [68]. The antibody is an IgG1 monoclonal antibody derived from the murine antibody 266 that preferentially binds soluble Aβ [16]. Early clinical trials with Solanezumab showed increased levels of plasma and CSF Aβ and showed little cognitive improvements in patients with moderate AD [19]. Currently, a large phase III trial with Solanezumab is ongoing.
Solanezumab is reported to recognize various forms of N-truncated Aβ [30]. Our findings are in line with these reports, as SolanezumabBS detected intraneuronal pyroglutamated Aβ3−x and Aβ4−x in TBA42 and Tg4-42 mice in formalin-fixed, paraffin-embedded tissue, respectively. Importantly, these mice do only express N-truncated Aβ variants pyroglutamated Aβ3−x and Aβ4−x and not APP.
Surprisingly, SolanezumabBS detected abundant plaque pathology in all of the 35 analyzed sporadic AD cases and in two of the control cases in formalin-fixed and paraffin-embedded tissue as well as in fresh frozen tissue. Furthermore, the antibody also detected plaques in 5XFAD, APP/PS1KI and 3xTg mice. In contrast to these results, it has previously been reported that the antibody inhibits fibril formation [37] by synthetic Aβ and only detects soluble monomeric Aβ [46]. Solanezumab has nearly the same sequence of amino acids interacting with Aβ as Crenezumab suggesting that the two antibodies bind Aβ in the same manner [14]. Interestingly, while Solanezumab is not reported to bind aggregated forms of Aβ its murine parent was reported to do so [65]. Seubert et al. showed that ‘antibody 266 (IgG1 isotype) recognizes a central epitope of Aβ residues 16–24 and much less effectively binds amyloid plaques, as compared to 3D6’.
Next to Aβ starting with aspartate as the first amino acid, a variety of modified and N-truncated Aβ variants has been characterized [34]. N-truncated Aβ can be found plaque associated as well as intraneuronal in AD mouse models [25] and it has been demonstrated that N-terminal deletions enhance aggregation of β-amyloid into neurotoxic, β-sheet fibrils. Such peptides may initiate and/or nucleate the pathological deposition of Aβ into plaques [52]. Furthermore, Sergeant et al. [64] demonstrated that amino-truncated Aβ species represent a large portion of all Aβ species in fully developed AD as well as at the earliest stage of AD pathology and are only detected during disease progression [7]. It was concluded that therapy specifically targeting these pathological amino-truncated species of Aβx−42 might be therapeutically advantageous.
Several pre-clinical studies already showed beneficial effects of passive immunization against pyroglutamate Aβ3−x. Pyroglutamated Aβ3−x mAbs reduced plaque depositions while limiting the side effects of vaccination. For example, passive immunization of 5XFAD mice with the 9D5 antibody that detects low molecular weight pyroglutamate Aβ oligomers reduced Aβ plaque load and AβpE3−x levels in mice [75]. Another anti-pyroglutamated Aβ3−x antibody (mAb07/1) significantly reduced plaque burden after passive immunization of APPswe/PS1dE9 transgenic mice without increasing vascular amyloid or microhemorrhage [23]. Similarly, De Mattos and colleagues reported that passive immunization of PDAPP mice reduced pre-existing plaques without inducing microhemorrhage in a dose-dependent manner [17].
Here, we tested the binding affinity of BapineuzumabBS, CrenezumabBS and SolanezumabBS to pyroglutamated Aβ3−x in TBA42 mice in formalin-fixed and paraffin-embedded tissue. This mouse model expresses only Aβ3Q-42 starting with an N-terminal glutamine (Q) residue at position three of Aβ as glutamine is a better substrate for both the spontaneous and enzymatically catalyzed conversion of Aβ3–42 into AβpE3–42 [43, 77]. Therefore, TBA42 mice do not express human APP or other Aβ variants. Only SolanezumabBS was able to detect intraneuronal Aβ in the CA1 of the hippocampus in these mice, while the highly homologous CrenezumabBS did not detect Aβ in this mouse model. This is likely not a consequence of specificity, but of binding affinity, consistent with the three orders of magnitude lower binding affinity of CrenezumabBS for Aβ relative to SolanezumabBS. As expected, BapineuzumabBS showed no parenchymal staining in TBA42 mice as it has been previously shown that Bapineuzumab is not able to recognize N-terminally modified or truncated Aβ species [44]. The crystal structure of a Bapineuzumab Fab-Aβ peptide complex revealed that it captured Aβ in a monomeric helical conformation at the N-terminus terminus and in doing so buried the N-terminus of the peptide [44].
Next to pyroglutamate Aβ3–42 Aβ4–42 could be another potential therapeutic target for AD. This peptide aggregates irreversibly and rapidly into soluble toxic oligomers and only slowly reacts further into inert amorphous fibrils [10]. Aβ4–42 is very abundant in AD and was discovered as early as 1985 [40]. However, Aβ4−x has not received much attention as a potential therapeutic target. McLaurin et al. [41] have performed an active immunization approach in TgCRND8 transgenic mice using protofibrillar Aβ1–42 peptides. The mice developed robust titers against Aβ and the sera isolated from these mice stained mature, but not diffuse plaques in TgCRND8 mice. The therapeutically active antibodies were subsequently isolated and characterized. Interestingly, although protofibrillar Aβ1–42 was used as vaccine, beneficial effects in mice arose from antibodies selectively directed against residues 4–10 of Aβ. These antibodies inhibited both Aβ fibrillogenesis and cytotoxicity without eliciting an inflammatory reaction. It seems likely that pre-clinical immunization trials against Aβ4–42 are only a matter of time.
CrenezumabBS and SolanezumabBS were able to detect intraneuronal Aβ in the hippocampus of Tg4-42 mice, expressing Aβ4–42. Again BapineuzumabBS did not recognize the truncated Aβ species in formalin-fixed and paraffin-embedded tissue. As expected, our recently generated the Aβ4−x-specific antibody NT4X showed positive intraneuronal immunoreactivity in Tg4-42 mice expressing only Aβ4–42 and not human APP or any other Aβ variant.
NT4X is able to differentiate between full-length Aβ and the two major N-truncated variants, Aβ4−x and AβpE3−x. NT4X significantly rescued Aβ4–42 toxicity in vitro, while no beneficial effect was observed against Aβ1–42 or AβpE3–42 toxicity [4]. Here, we extended our previous findings and demonstrated that the antibody detects plaques in APP/PS1KI, 5XFAD and 3xTg mice, but barely reacted with plaques in the brain of sporadic AD patients in formalin-fixed, paraffin-embedded tissue or fresh frozen tissue. These data are corroborated by a previous work which analyzed Aβ pathology using chemical and morphological approaches comparing the plaques of APP23 transgenic mice and human AD brain [35]. Chemical analyses revealed that the amyloid plaque cores in APP23 transgenic mice were completely soluble in buffers containing SDS despite an obvious overall structural resemblance to AD pathology. Human AD plaque cores were highly resistant to chemical and physical disruption accounting for the extreme stability of AD plaque cores. An explanation for the differences in solubility between human AD and the APP23 mouse plaques may be due to the lack of post-translational modifications including N-terminal degradation, isomerization, racemization, pyroglutamyl formation and oxidation of transgenic mouse Aβ [35]. NT4X preferably stained Aβ in blood vessels in humans, in which Aβx-40 is a major component.
The weak binding of NT4X to plaques in human tissue could be construed as a potential therapeutic advantage. The strategy of using antibodies that target mainly plaques is increasingly being regarded as a potential risk factor as plaques may serve as reservoirs of toxic Aβ peptides [8, 28]. The failure of Bapineuzumab may at least be partly explained by that hypothesis.
While the insoluble fibrillar aggregates of amyloid-β are the main neuropathological hallmark of AD, the plaque load correlates poorly with brain dysfunction and cognitive impairment in AD patients [39, 54] or in AD transgenic mouse models [45, 62]. In contrast, recent studies indicate that soluble Aβ levels, including soluble oligomers, correlate much better with key features of AD [42, 47, 63]. Furthermore, growing evidence suggests that intraneuronal Aβ accumulation contributes to the pathological events in AD. Intraneuronal Aβ accumulation has also been detected in a variety of AD mouse models including Tg2576, 3xTg, APP/PS1KI and 5XFAD [48, 49, 70]. Early and transient intraneuronal accumulation of Aβ correlated with subsequent neuron loss also in diverse APP/Aβ transgenic mouse models and brain regions [3, 10, 13, 43, 74]. Here, we demonstrated that the three humanized antibodies BapineuzumabBS, CrenezumabBS and SolanezumabBS were able to detect intraneuronal Aβ in young 5XFAD and APP/PS1KI as well as in aged 3xTg mice. Cross-reactivity with APP cannot be ruled out entirely in these models though. NT4X, specific to the N-terminus of Aβ4−x and AβpE3−x, also showing intraneuronal staining in these mouse lines underlines the abundance of Aβ4−x and AβpE3−x in these models of AD. Interestingly, Grundke-Iqbal et al. [27] reported already 25 years ago that intracellular Aβ may precede Aβ plaque formation in AD patients. It should be noted, however, that the existence of intraneuronal Aβ especially in human AD brain sections is disputed in the field [26]. The major information using transgenic mice in the present study came from mice expressing N-truncated Aβ4–42 and pyroglutamate Aβ3–42 as we demonstrated the difference in target engagement among the four antibodies studied.
It has to be noted that the human antibodies used in the current study are ‘bio-similar’ versions based on the available patent literature rather than the original antibodies [14, 44, 71]. Furthermore, it has to be noted that while immunohistochemistry is one of the pillars of diagnostic pathology and an important research tool in pathology and research, the results obtained with immunohistochemistry may not accurately reflect in vivo conditions. Nevertheless, it is an important part of the characterization and comparison of antibodies.
In summary, the present report describes the immunohistochemistry profile of BapineuzumabBS, CrenezumabBS and SolanezumabBS in human and mouse tissue. All three antibodies showed a very similar staining profile in formalin-fixed and paraffin-embedded tissue and fresh frozen tissue and were able to detect plaques and CAA in humans in addition to plaques and intraneuronal Aβ in mice. SolanezumabBS was the only antibody able to detect not only Aβ4–42 but also pyroglutamate Aβ3–42. In contrast, NT4X showed a low binding affinity to plaques in human tissue while recognizing CAA as well as intraneuronal Aβ and plaques in mice.
Change history
25 March 2024
A Correction to this paper has been published: https://doi.org/10.1007/s00401-024-02718-w
References
https://clinicaltrials.gov. Accessed 1 July 2015
Adolfsson O, Pihlgren M, Toni N, Varisco Y, Buccarello AL, Antoniello K, Lohmann S, Piorkowska K, Gafner V, Atwal JK, Maloney J, Chen M, Gogineni A, Weimer RM, Mortensen DL, Friesenhahn M, Ho C, Paul R, Pfeifer A, Muhs A, Watts RJ (2012) An effector-reduced anti-β-amyloid (Aβ) antibody with unique aβ binding properties promotes neuroprotection and glial engulfment of Aβ. J Neurosci 32(28):9677–9689. doi:10.1523/JNEUROSCI.4742-11.2012
Alexandru A, Jagla W, Graubner S, Becker A, Bäuscher C, Kohlmann S, Sedlmeier R, Raber KA, Cynis H, Rönicke R, Reymann KG, Petrasch-Parwez E, Hartlage-Rübsamen M, Waniek A, Rossner S, Schilling S, Osmand AP, Demuth H, von Hörsten S (2011) Selective hippocampal neurodegeneration in transgenic mice expressing small amounts of truncated Aβ is induced by pyroglutamate-Aβ formation. J Neurosci 31(36):12790–12801. doi:10.1523/JNEUROSCI.1794-11.2011
Antonios G, Saiepour N, Bouter Y, Richard BC, Paetau A, Verkkoniemi-Ahola A, Lannfelt L, Ingelsson M, Kovacs GG, Pillot T, Wirths O, Bayer TA (2013) N-truncated Abeta starting with position four: early intraneuronal accumulation and rescue of toxicity using NT4X-167, a novel monoclonal antibody. Acta Neuropathol Commun 1(1):56. doi:10.1186/2051-5960-1-56
Bard F, Cannon C, Barbour R, Burke RL, Games D, Grajeda H, Guido T, Hu K, Huang J, Johnson-Wood K, Khan K, Kholodenko D, Lee M, Lieberburg I, Motter R, Nguyen M, Soriano F, Vasquez N, Weiss K, Welch B, Seubert P, Schenk D, Yednock T (2000) Peripherally administered antibodies against amyloid beta-peptide enter the central nervous system and reduce pathology in a mouse model of Alzheimer disease. Nat Med 6(8):916–919. doi:10.1038/78682
Basi G, Jacobsen JS (2009) Humanized antibodies that recognize beta amyloid peptide. Google Patents. http://www.google.com/patents/US7625560
Bayer TA, Wirths O (2014) Focusing the amyloid cascade hypothesis on N-truncated Abeta peptides as drug targets against Alzheimer’s disease. Acta Neuropathol. doi:10.1007/s00401-014-1287-x
Benilova I, Karran E, DeStrooper B (2012) The toxic Aβ oligomer and Alzheimer’s disease: an emperor in need of clothes. Nat Neurosci 15(3):349–357. doi:10.1038/nn.3028
Blennow K, Zetterberg H, Rinne JO, Salloway S, Wei J, Black R, Grundman M, Liu E (2012) Effect of immunotherapy with bapineuzumab on cerebrospinal fluid biomarker levels in patients with mild to moderate Alzheimer disease. Arch Neurol 69(8):1002–1010. doi:10.1001/archneurol.2012.90
Bouter Y, Dietrich K, Wittnam JL, Rezaei-Ghaleh N, Pillot T, Papot-Couturier S, Lefebvre T, Sprenger F, Wirths O, Zweckstetter M, Bayer TA (2013) N-truncated amyloid β (Aβ) 4–42 forms stable aggregates and induces acute and long-lasting behavioral deficits. Acta Neuropathol 126(2):189–205. doi:10.1007/s00401-013-1129-2
Buttini M, Masliah E, Barbour R, Grajeda H, Motter R, Johnson-Wood K, Khan K, Seubert P, Freedman S, Schenk D, Games D (2005) Beta-amyloid immunotherapy prevents synaptic degeneration in a mouse model of Alzheimer’s disease. J Neurosci 25(40):9096–9101. doi:10.1523/JNEUROSCI.1697-05.2005
Casas C, Sergeant N, Itier J, Blanchard V, Wirths O, van der Kolk N, Vingtdeux V, van de Steeg E, Ret G, Canton T, Drobecq H, Clark A, Bonici B, Delacourte A, Benavides J, Schmitz C, Tremp G, Bayer TA, Benoit P, Pradier L (2004) Massive CA1/2 neuronal loss with intraneuronal and N-terminal truncated Abeta42 accumulation in a novel Alzheimer transgenic model. Am J Pathol 165(4):1289–1300
Christensen DZ, Kraus SL, Flohr A, Cotel M, Wirths O, Bayer TA (2008) Transient intraneuronal A beta rather than extracellular plaque pathology correlates with neuron loss in the frontal cortex of APP/PS1KI mice. Acta Neuropathol 116(6):647–655. doi:10.1007/s00401-008-0451-6
Crespi Gabriela A N, Hermans SJ, Parker MW, Miles LA (2015) Molecular basis for mid-region amyloid-β capture by leading Alzheimer’s disease immunotherapies. Sci Rep 5:9649. doi:10.1038/srep09649
Das P (2001) Reduced effectiveness of AÎ21-42 immunization in APP transgenic mice with significant amyloid deposition. Neurobiol Aging 22(5):721–727. doi:10.1016/S0197-4580(01)00245-7
DeMattos RB, Bales KR, Cummins DJ, Dodart J, Paul SM, Holtzman DM (2001) Peripheral anti-Aβ antibody alters CNS and plasma Aβ clearance and decreases brain Aβ burden in a mouse model of Alzheimer’s disease. Proc Natl Acad Sci USA 98(15):8850–8855. doi:10.1073/pnas.151261398
DeMattos RB, Lu J, Tang Y, Racke MM, Delong CA, Tzaferis JA, Hole JT, Forster BM, McDonnell PC, Liu F, Kinley RD, Jordan WH, Hutton ML (2012) A plaque-specific antibody clears existing β-amyloid plaques in Alzheimer’s disease mice. Neuron 76(5):908–920. doi:10.1016/j.neuron.2012.10.029
Dodart J, Bales KR, Gannon KS, Greene SJ, DeMattos RB, Mathis C, DeLong CA, Wu S, Wu X, Holtzman DM, Paul SM (2002) Immunization reverses memory deficits without reducing brain Abeta burden in Alzheimer’s disease model. Nat Neurosci 5(5):452–457. doi:10.1038/nn842
Doody RS, Thomas RG, Farlow M, Iwatsubo T, Vellas B, Joffe S, Kieburtz K, Raman R, Sun X, Aisen PS, Siemers E, Liu-Seifert H, Mohs R (2014) Phase 3 trials of solanezumab for mild-to-moderate Alzheimer’s disease. N Engl J Med 370(4):311–321. doi:10.1056/NEJMoa1312889
Feinberg H, Saldanha JW, Diep L, Goel A, Widom A, Veldman GM, Weis WI, Schenk D, Basi GS (2014) Crystal structure reveals conservation of amyloid-β conformation recognized by 3D6 following humanization to bapineuzumab. Alzheimers Res Ther 6(3):31. doi:10.1186/alzrt261
Fox NC, Black RS, Gilman S, Rossor MN, Griffith SG, Jenkins L, Koller M (2005) Effects of Abeta immunization (AN1792) on MRI measures of cerebral volume in Alzheimer disease. Neurology 64(9):1563–1572. doi:10.1212/01.WNL.0000159743.08996.99
Frost JL, Le KX, Cynis H, Ekpo E, Kleinschmidt M, Palmour RM, Ervin FR, Snigdha S, Cotman CW, Saido TC, Vassar RJ, St George-Hyslop P, Ikezu T, Schilling S, Demuth H, Lemere CA (2013) Pyroglutamate-3 amyloid-beta deposition in the brains of humans, non-human primates, canines, and Alzheimer disease-like transgenic mouse models. Am J Pathol 183(2):369–381. doi:10.1016/j.ajpath.2013.05.005
Frost JL, Liu B, Kleinschmidt M, Schilling S, Demuth H, Lemere CA (2012) Passive immunization against pyroglutamate-3 amyloid-β reduces plaque burden in Alzheimer-like transgenic mice: a pilot study. Neurodegener Dis 10(1–4):265–270. doi:10.1159/000335913
Garber K (2012) Genentech’s Alzheimer’s antibody trial to study disease prevention. Nat Biotechnol 30(8):731–732. doi:10.1038/nbt0812-731
Gouras GK, Tsai J, Naslund J, Vincent B, Edgar M, Checler F, Greenfield JP, Haroutunian V, Buxbaum JD, Xu H, Greengard P, Relkin NR (2000) Intraneuronal Abeta42 accumulation in human brain. Am J Pathol 156(1):15–20
Gouras GK, Willén K, Tampellini D (2012) Critical role of intraneuronal Aβ in Alzheimer’s disease: technical challenges in studying intracellular Aβ. Life Sci 91(23–24):1153–1158. doi:10.1016/j.lfs.2012.06.004
Grundke-Iqbal I, Iqbal K, George L, Tung YC, Kim KS, Wisniewski HM (1989) Amyloid protein and neurofibrillary tangles coexist in the same neuron in Alzheimer disease. Proc Natl Acad Sci USA 86(8):2853–2857
Haass C, Selkoe DJ (2007) Soluble protein oligomers in neurodegeneration: lessons from the Alzheimer’s amyloid beta-peptide. Nat Rev Mol Cell Biol 8(2):101–112. doi:10.1038/nrm2101
Hardy J, Allsop D (1991) Amyloid deposition as the central event in the aetiology of Alzheimer’s disease. Trends Pharmacol Sci 12(10):383–388
Imbimbo BP, Ottonello S, Frisardi V, Solfrizzi V, Greco A, Seripa D, Pilotto A, Panza F (2012) Solanezumab for the treatment of mild-to-moderate Alzheimer’s disease. Expert Rev Clin Immunol 8(2):135–149. doi:10.1586/eci.11.93
Janus C, Pearson J, McLaurin J, Mathews PM, Jiang Y, Schmidt SD, Chishti MA, Horne P, Heslin D, French J, Mount HT, Nixon RA, Mercken M, Bergeron C, Fraser PE, St George-Hyslop P, Westaway D (2000) A beta peptide immunization reduces behavioural impairment and plaques in a model of Alzheimer’s disease. Nature 408(6815):979–982. doi:10.1038/35050110
Jawhar S, Trawicka A, Jenneckens C, Bayer TA, Wirths O (2010) Motor deficits, neuron loss, and reduced anxiety coinciding with axonal degeneration and intraneuronal Abeta aggregation in the 5XFAD mouse model of Alzheimer’s disease. Neurobiol Aging. doi:10.1016/j.neurobiolaging.2010.05.027
Kotilinek LA, Bacskai B, Westerman M, Kawarabayashi T, Younkin L, Hyman BT, Younkin S, Ashe KH (2002) Reversible memory loss in a mouse transgenic model of Alzheimer’s disease. J Neurosci 22(15):6331–6335
Kummer MP, Heneka MT (2014) Truncated and modified amyloid-beta species. Alzheimers Res Ther 6(3):28. doi:10.1186/alzrt258
Kuo YM, Kokjohn TA, Beach TG, Sue LI, Brune D, Lopez JC, Kalback WM, Abramowski D, Sturchler-Pierrat C, Staufenbiel M, Roher AE (2001) Comparative analysis of amyloid-beta chemical structure and amyloid plaque morphology of transgenic mouse and Alzheimer’s disease brains. J Biol Chem 276(16):12991–12998. doi:10.1074/jbc.M007859200
Lannfelt L, Möller C, Basun H, Osswald G, Sehlin D, Satlin A, Logovinsky V, Gellerfors P (2014) Perspectives on future Alzheimer therapies: amyloid-β protofibrils—a new target for immunotherapy with BAN2401 in Alzheimer’s disease. Alzheimers Res Ther 6(2):16. doi:10.1186/alzrt246
Legleiter J, Czilli DL, Gitter B, DeMattos RB, Holtzman DM, Kowalewski T (2004) Effect of different anti-Abeta antibodies on Abeta fibrillogenesis as assessed by atomic force microscopy. J Mol Biol 335(4):997–1006
Lemere CA (2013) Immunotherapy for Alzheimer’s disease: hoops and hurdles. Mol Neurodegener 8:36. doi:10.1186/1750-1326-8-36
Lesné SE, Sherman MA, Grant M, Kuskowski M, Schneider JA, Bennett DA, Ashe KH (2013) Brain amyloid-β oligomers in ageing and Alzheimer’s disease. Brain 136(Pt 5):1383–1398. doi:10.1093/brain/awt062
Masters CL, Simms G, Weinman NA, Multhaup G, McDonald BL, Beyreuther K (1985) Amyloid plaque core protein in Alzheimer disease and Down syndrome. Proc Natl Acad Sci USA 82(12):4245–4249
McLaurin J, Cecal R, Kierstead ME, Tian X, Phinney AL, Manea M, French JE, Lambermon MHL, Darabie AA, Brown ME, Janus C, Chishti MA, Horne P, Westaway D, Fraser PE, Mount HTJ, Przybylski M, St George-Hyslop P (2002) Therapeutically effective antibodies against amyloid-beta peptide target amyloid-beta residues 4–10 and inhibit cytotoxicity and fibrillogenesis. Nat Med 8(11):1263–1269. doi:10.1038/nm790
McLean CA, Cherny RA, Fraser FW, Fuller SJ, Smith MJ, Beyreuther K, Bush AI, Masters CL (1999) Soluble pool of Abeta amyloid as a determinant of severity of neurodegeneration in Alzheimer’s disease. Ann. Neurol 46(6):860–866
Meissner JN, Bouter Y, Bayer TA (2014) Neuron loss and behavioral deficits in the TBA42 mouse model expressing N-truncated pyroglutamate amyloid-beta3–42. J Alzheimers Dis. doi:10.3233/JAD-142868
Miles LA, Crespi Gabriela A N, Doughty L, Parker MW (2013) Bapineuzumab captures the N-terminus of the Alzheimer’s disease amyloid-beta peptide in a helical conformation. Sci Rep 3:1302. doi:10.1038/srep01302
Moechars D, Dewachter I, Lorent K, Reversé D, Baekelandt V, Naidu A, Tesseur I, Spittaels K, Haute CV, Checler F, Godaux E, Cordell B, van Leuven F (1999) Early phenotypic changes in transgenic mice that overexpress different mutants of amyloid precursor protein in brain. J Biol Chem 274(10):6483–6492
Moreth J, Mavoungou C, Schindowski K (2013) Passive anti-amyloid immunotherapy in Alzheimer’s disease: what are the most promising targets? Immun Ageing 10(1):18. doi:10.1186/1742-4933-10-18
Näslund J, Haroutunian V, Mohs R, Davis KL, Davies P, Greengard P, Buxbaum JD (2000) Correlation between elevated levels of amyloid beta-peptide in the brain and cognitive decline. JAMA 283(12):1571–1577
Oakley H, Cole SL, Logan S, Maus E, Shao P, Craft J, Guillozet-Bongaarts A, Ohno M, Disterhoft J, van Eldik L, Berry R, Vassar R (2006) Intraneuronal beta-amyloid aggregates, neurodegeneration, and neuron loss in transgenic mice with five familial Alzheimer’s disease mutations: potential factors in amyloid plaque formation. J Neurosci 26(40):10129–10140. doi:10.1523/JNEUROSCI.1202-06.2006
Oddo S, Caccamo A, Shepherd JD, Murphy MP, Golde TE, Kayed R, Metherate R, Mattson MP, Akbari Y, LaFerla FM (2003) Triple-transgenic model of Alzheimer’s disease with plaques and tangles: intracellular Abeta and synaptic dysfunction. Neuron 39(3):409–421
Orgogozo J, Gilman S, Dartigues J, Laurent B, Puel M, Kirby LC, Jouanny P, Dubois B, Eisner L, Flitman S, Michel BF, Boada M, Frank A, Hock C (2003) Subacute meningoencephalitis in a subset of patients with AD after Abeta42 immunization. Neurology 61(1):46–54
Panza F, Logroscino G, Imbimbo BP, Solfrizzi V (2014) Is there still any hope for amyloid-based immunotherapy for Alzheimer’s disease? Curr Opin Psychiatry 27(2):128–137. doi:10.1097/YCO.0000000000000041
Pike CJ, Overman MJ, Cotman CW (1995) Amino-terminal deletions enhance aggregation of beta-amyloid peptides in vitro. J Biol Chem 270(41):23895–23898
Pimplikar SW (2009) Reassessing the amyloid cascade hypothesis of Alzheimer’s disease. Int J Biochem Cell Biol 41(6):1261–1268. doi:10.1016/j.biocel.2008.12.015
Price JL, Morris JC (1999) Tangles and plaques in nondemented aging and “preclinical” Alzheimer’s disease. Ann Neurol 45(3):358–368
Prins ND, Scheltens P (2013) Treating Alzheimer’s disease with monoclonal antibodies: current status and outlook for the future. Alzheimers Res Ther 5(6):56. doi:10.1186/alzrt220
Ravid R, Swaab DF (1993) The Netherlands brain bank—a clinico-pathological link in aging and dementia research. J Neural Transm Suppl 39:143–153
Reisberg B, Ferris SH, de Leon MJ, Crook T (1982) The Global Deterioration Scale for assessment of primary degenerative dementia. Am J Psychiatry 139(9):1136–1139
Richard BC, Kurdakova A, Baches S, Bayer TA, Weggen S, Wirths O (2015) Gene dosage dependent aggravation of the neurological phenotype in the 5XFAD Mouse Model of Alzheimer’s disease. J Alzheimers Dis. doi:10.3233/JAD-143120
Rinne JO, Brooks DJ, Rossor MN, Fox NC, Bullock R, Klunk WE, Mathis CA, Blennow K, Barakos J, Okello AA, Rodriguez Martinez de Liano S, Liu E, Koller M, Gregg KM, Schenk D, Black R, Grundman M (2010) 11C-PiB PET assessment of change in fibrillar amyloid-β load in patients with Alzheimer’s disease treated with bapineuzumab: a phase 2, double-blind, placebo-controlled, ascending-dose study. Lancet Neurol 9(4):363–372. doi:10.1016/S1474-4422(10)70043-0
Salloway S, Sperling R, Fox NC, Blennow K, Klunk W, Raskind M, Sabbagh M, Honig LS, Porsteinsson AP, Ferris S, Reichert M, Ketter N, Nejadnik B, Guenzler V, Miloslavsky M, Wang D, Lu Y, Lull J, Tudor IC, Liu E, Grundman M, Yuen E, Black R, Brashear HR (2014) Two phase 3 trials of bapineuzumab in mild-to-moderate Alzheimer’s disease. N Engl J Med 370(4):322–333. doi:10.1056/NEJMoa1304839
Schenk D, Barbour R, Dunn W, Gordon G, Grajeda H, Guido T, Hu K, Huang J, Johnson-Wood K, Khan K, Kholodenko D, Lee M, Liao Z, Lieberburg I, Motter R, Mutter L, Soriano F, Shopp G, Vasquez N, Vandevert C, Walker S, Wogulis M, Yednock T, Games D, Seubert P (1999) Immunization with amyloid-beta attenuates Alzheimer-disease-like pathology in the PDAPP mouse. Nature 400(6740):173–177. doi:10.1038/22124
Schmitz C, Rutten BPF, Pielen A, Schäfer S, Wirths O, Tremp G, Czech C, Blanchard V, Multhaup G, Rezaie P, Korr H, Steinbusch HWM, Pradier L, Bayer TA (2004) Hippocampal neuron loss exceeds amyloid plaque load in a transgenic mouse model of Alzheimer’s disease. Am J Pathol 164(4):1495–1502. doi:10.1016/S0002-9440(10)63235-X
Selkoe DJ (2011) Resolving controversies on the path to Alzheimer’s therapeutics. Nat Med 17(9):1060–1065. doi:10.1038/nm.2460
Sergeant N, Bombois S, Ghestem A, Drobecq H, Kostanjevecki V, Missiaen C, Wattez A, David J, Vanmechelen E, Sergheraert C, Delacourte A (2003) Truncated beta-amyloid peptide species in pre-clinical Alzheimer’s disease as new targets for the vaccination approach. J Neurochem 85(6):1581–1591
Seubert P, Barbour R, Khan K, Motter R, Tang P, Kholodenko D, Kling K, Schenk D, Johnson-Wood K, Schroeter S, Gill D, Jacobsen JS, Pangalos M, Basi G, Games D (2008) Antibody capture of soluble Abeta does not reduce cortical Abeta amyloidosis in the PDAPP mouse. Neurodegener Dis 5(2):65–71. doi:10.1159/000112834
Solomon B, Koppel R, Frankel D, Hanan-Aharon E (1997) Disaggregation of Alzheimer beta-amyloid by site-directed mAb. Proc Natl Acad Sci USA 94(8):4109–4112
Solomon B, Koppel R, Hanan E, Katzav T (1996) Monoclonal antibodies inhibit in vitro fibrillar aggregation of the Alzheimer beta-amyloid peptide. Proc Natl Acad Sci USA 93(1):452–455
Spencer B, Masliah E (2014) Immunotherapy for Alzheimer’s disease: past, present and future. Front Aging Neurosci 6. doi:10.3389/fnagi.2014.00114
Sperling R, Salloway S, Brooks DJ, Tampieri D, Barakos J, Fox NC, Raskind M, Sabbagh M, Honig LS, Porsteinsson AP, Lieberburg I, Arrighi HM, Morris KA, Lu Y, Liu E, Gregg KM, Brashear HR, Kinney GG, Black R, Grundman M (2012) Amyloid-related imaging abnormalities in patients with Alzheimer’s disease treated with bapineuzumab: a retrospective analysis. Lancet Neurol 11(3):241–249. doi:10.1016/S1474-4422(12)70015-7
Takahashi RH, Milner TA, Li F, Nam EE, Edgar MA, Yamaguchi H, Beal MF, Xu H, Greengard P, Gouras GK (2002) Intraneuronal Alzheimer Abeta42 accumulates in multivesicular bodies and is associated with synaptic pathology. Am J Pathol 161(5):1869–1879
Watt AD, Crespi Gabriela A N, Down RA, Ascher DB, Gunn A, Perez KA, McLean CA, Villemagne VL, Parker MW, Barnham KJ, Miles LA (2014) Do current therapeutic anti-Aβ antibodies for Alzheimer’s disease engage the target? Acta Neuropathol. doi:10.1007/s00401-014-1290-2
Wilcock DM, Gordon MN, Ugen KE, Gottschall PE, DiCarlo G, Dickey C, Boyett KW, Jantzen PT, Connor KE, Melachrino J, Hardy J, Morgan D (2001) Number of Abeta inoculations in APP + PS1 transgenic mice influences antibody titers, microglial activation, and congophilic plaque levels. DNA Cell Biol 20(11):731–736. doi:10.1089/10445490152717596
Wirths O, Bethge T, Marcello A, Harmeier A, Jawhar S, Lucassen PJ, Multhaup G, Brody DL, Esparza T, Ingelsson M, Kalimo H, Lannfelt L, Bayer TA (2010) Pyroglutamate Abeta pathology in APP/PS1KI mice, sporadic and familial Alzheimer’s disease cases. J Neural Transm 117(1):85–96. doi:10.1007/s00702-009-0314-x
Wirths O, Breyhan H, Cynis H, Schilling S, Demuth H, Bayer TA (2009) Intraneuronal pyroglutamate-Abeta 3–42 triggers neurodegeneration and lethal neurological deficits in a transgenic mouse model. Acta Neuropathol 118(4):487–496. doi:10.1007/s00401-009-0557-5
Wirths O, Erck C, Martens H, Harmeier A, Geumann C, Jawhar S, Kumar S, Multhaup G, Walter J, Ingelsson M, Degerman-Gunnarsson M, Kalimo H, Huitinga I, Lannfelt L, Bayer TA (2010) Identification of low molecular weight pyroglutamate A{beta} oligomers in Alzheimer disease: a novel tool for therapy and diagnosis. J Biol Chem 285(53):41517–41524. doi:10.1074/jbc.M110.178707
Wisniewski T, Goñi F (2014) Immunotherapy for Alzheimer’s disease. Biochem Pharmacol 88(4):499–507. doi:10.1016/j.bcp.2013.12.020
Wittnam JL, Portelius E, Zetterberg H, Gustavsson MK, Schilling S, Koch B, Demuth H, Blennow K, Wirths O, Bayer TA (2012) Pyroglutamate amyloid β (Aβ) aggravates behavioral deficits in transgenic amyloid mouse model for Alzheimer disease. J Biol Chem 287(11):8154–8162. doi:10.1074/jbc.M111.308601
Zago W, Buttini M, Comery TA, Nishioka C, Gardai SJ, Seubert P, Games D, Bard F, Schenk D, Kinney GG (2012) Neutralization of soluble, synaptotoxic amyloid beta species by antibodies is epitope specific. J Neurosci 32(8):2696–2702. doi:10.1523/JNEUROSCI.1676-11.2012
Acknowledgments
This work was supported by funding from the National Health and Medical Research Council of Australia (NHMRC) to LAM and MWP (APP1021935) and from the Victorian Government Operational Infrastructure Support Scheme to St. Vincent’s Institute. MWP is a NHMRC Research Fellow. JSLN received a Ph.D. stipend from the Mexican Ministry of Education (SEP) for the Improvement of Faculty (PROMEP). We greatly acknowledge the financial support by the Alzheimer Forschungs Initiative to TAB.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
A patent application for the antibody NT4X was filed by the University Medicine of Goettingen and Thomas A. Bayer.
Rights and permissions
About this article
Cite this article
Bouter, Y., Noguerola, J.S.L., Tucholla, P. et al. Abeta targets of the biosimilar antibodies of Bapineuzumab, Crenezumab, Solanezumab in comparison to an antibody against N-truncated Abeta in sporadic Alzheimer disease cases and mouse models. Acta Neuropathol 130, 713–729 (2015). https://doi.org/10.1007/s00401-015-1489-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00401-015-1489-x