Abstract
The different histochemical ATPase properties of myosins separating the muscle fiber types have been utilized in diagnostic muscle biopsy routine for more than four decades. The ATPase staining method is rather laborious and has several disadvantages, such as weakening of staining over time and non-specific staining of capillaries, making the distinction of extremely atrophic muscle fibers difficult. We have developed a reliable and advanced immunohistochemical myosin double staining method for the identification of fiber types, including highly atrophic fibers in routine diagnostics. With this double staining method, we are able to distinguish among type I (ATPase type 1), IIA (ATPase type 2A), IIX (ATPase type 2B) and remodeled ATPase type 2C fibers expressing both fast and slow myosins using a one slide technique. Immunohistochemical double staining of myosin heavy chain isoforms can be used as an alternative for the conventional ATPase staining method in routine histopathology. The method provides even more detailed information of fast fiber subtypes and highly atrophic fibers on one single slide.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Actomyosin filaments represent the principal structural contractile components of muscle cell sarcomeres [13]. Myosin is a molecular motor that converts chemical energy into movement. This is established by sliding of actin and myosin filaments over each other while hydrolysis of adenosine triphosphate (ATP) provides energy for this process [14]. The thick myosin filament consists of hexameric myosin molecules formed by two heavy chains (MyHC) and four associated light chains. Each myosin heavy chain contains two heads that are the site of myosin adenosine triphosphatase (ATPase), an enzyme that hydrolyzes ATP required for the actin and myosin cross bridge formation. These heads interact with a binding site on actin [14]. Myosin heavy chains are encoded by a multigene family and exist in several isoforms, which are expressed in a tissue-specific and developmentally regulated manner. More than one MyHC gene is expressed in each muscle and developmental stage, but in the single mature and healthy muscle cell only one isoform is expressed [4].
In adult human skeletal muscle fibers, the major MyHC isoform in slow type I (ATPase type 1) fibers is encoded by the MYH7 gene on chromosome 14, which is also the main isoform of the cardiac muscle. In the fast type 2A fibers, the corresponding MyHC isoform IIA is encoded by the MYH2 gene on chromosome 17 [21]. Mutations in MYH7 gene have been reported to cause both skeletal and cardiac or combined myopathies [2, 9, 11, 15, 16, 18], whereas mutations in MYH2 were reported in rare families with skeletal myopathy [8, 10]. In the ultrafast glycolytic type 2B fibers, the corresponding MyHC IIX is expressed by the MYH1 gene on chromosome 17 [21], but so far no human condition has been associated with mutations in this gene.
Hybrid fibers expressing both fast and slow myosin heavy chains are usually regenerated or remodeled fibers that often occur in an excess number in pathological stages as a result of reprogramming in altered muscle fibers. Such secondary changes in the expression of MyHC genes are also useful for the diagnostic assessment of muscle biopsies and reflect compensatory plasticity of muscle tissue [5, 7]. Although the exclusive expression of one MyHC gene per fiber is preprogrammed, various exogenic influences can modulate the expression, such as thyroid hormone, and innervation can also influence and induce isoform transitions [7, 12].
The myosin ATPase properties of different MyHC isoforms is widely used as the main diagnostic method for fiber-type separation. The histochemical method is based on the release of phosphate, the capture of phosphate by calcium resulting in calcium phosphate and substitution of calcium by cobalt. Phosphate is replaced by sulfide and the end product is a black precipitate of cobalt sulfide. The reaction is carried out at non-physiological pH of 9.4 and preincubation at different pHs of 4.3, 4.6 and 10.4 [1]. MyHC isoforms, their corresponding ATPase types, ATPase histochemical stains and immunohistochemical double staining patterns are shown in Table 1. The ATPase histochemical staining method is very laborious and there are disadvantages such as weakening of staining over time and the non-specific staining of capillaries, making a distinction of highly atrophic muscle fibers difficult.
Myotonic dystrophy (dystrophia myotonica, DM) is the most commonly inherited muscular dystrophy in adults. Two different types of myotonic dystrophy have been identified with similarities in their clinical features. Both myotonic dystrophy type 1 [DM1, Steinert’s disease (OMIM #160900)] and type 2 [DM2, PROMM (OMIM #602668)] are dominantly inherited disorders with an estimated DM1 prevalence of 1/8,000 in European populations [3], while in DM2 the prevalence has not been established, but is proposed to be as common as in DM1 [17]. DM2 is caused by a tetranucleotide (CCTG)n expansion in the first intron of zinc finger protein 9 (ZNF9) gene on chromosome 3q21 [6]. The major symptoms of DM2 include proximal muscle weakness, muscle stiffness and/or pain, cataracts, myotonia, tremors, cardiac conduction defects and endocrinological abnormalities [18]. Clinical symptoms are however more inconsistent and diverse in DM2 than in DM1, which makes the clinical diagnosis a real challenge [18, 19]. We have previously reported the identification of a subpopulation of extremely small atrophic type 2 fibers, most of which are very difficult to detect by conventional ATPase staining, as a characteristic finding in DM2 [20]. Since fiber types by ATPase are paralleled by differences in MyHC isoforms, the full assessment of fiber-type distribution can also reliably be achieved by immunohistochemical staining.
Our MyHC immunohistochemical double staining method was primarily developed as an advanced screening method to identify the highly atrophic type 2 muscle fibers characteristic of DM2. However, this method proved a very informative and powerful tool for general diagnostic purposes and may substitute the ATPase stainings in the diagnostic routine. The MyHC double staining method can be performed on one slide only and our experience shows that this staining method is more reliable for the detection and separation of different fiber types and their subtypes, particularly regarding the highly atrophic fibers and hybrid fibers expressing more than one MyHC isoform.
Materials and methods
Frozen sections from ten normal cases, five DM2, five DM1, five muscle biopsies with neurogenic pathology and single biopsies with polymyositis, a genetically verified FKRP-mutated LGMD2I and a genetically verified MYH7-mutated early-onset Laing myopathy were used for MyHC double staining performed on a BenchMark (Ventana Medical Systems Inc., Tucson, AZ 85755, USA) immunostainer, using slow myosin monoclonal antibody against slow type I (ATPase type 1) fibers (clone WB-MHCs, Leica Microsystems, VisionBbiosystems, Newcastle upon Tyne, NE12 8EW, UK) at a dilution of 1:200 and myosin A4.74, a monoclonal antibody against fast type IIA (ATPase type 2A) fibers, at a dilution of 1:100. The myosin A4.74 antibody developed by Helen M. Blau was obtained from the Developmental Studies Hybridoma Bank developed under the auspices of the NICHD and maintained by The University of Iowa, Department of Biology, Iowa City, IA 52242, USA. The immunohistochemical stainings were performed using the official protocol of the BenchMark immunostainer with incubation of primary antibodies for 30 min at 37°C. Slow myosin was visualized with a peroxidase-based detection kit (Universal DAB detection kit, Ventana Medical Systems Inc., Tucson, AZ 85755, USA) and myosin A4.74 with alkaline phosphatase red detection system (ultraViewTM Universal Alkaline Phosphatase Red Detection kit, Ventana Medical Systems Inc., Tucson, AZ 85755, USA). Histochemical ATPase staining with pH 4.3, 4.6 and 10.4 was performed in parallel as described before [1]. Briefly, each of 10-μm sections were pre-incubated in sodium barbiturate and calcium chloride solution of pH 10.4, and barium acetate and hydrochloric acid solution of pH 4.3 and 4.6. The sections were then incubated in a solution of sodium barbiturate of pH 9.4, containing adenosine triphosphate for 30 min at +37°C. After incubation in 1% calcium chloride and 2% cobalt chloride, respectively, the sections were dipped into a solution of 0.01 M sodium barbiturate. The sections were washed and then dipped into a solution of 0.2% ammonium sulfide to form a black precipitate of cobalt sulfide. Fibers without reaction and connective tissue were stained using Van Gieson solution. The Van Gieson staining also changes the appearance of the black precipitate of cobalt sulfide into shades of brown. Nuclei were stained using Weigert’s hematoxylin. The ATPase staining was done on serial sections of the same samples to compare staining methods and fiber-type distribution of muscle biopsies.
Results
All ATPase-based fiber types were easily separated by the double immunostaining technique (Fig. 1). Slow type 1 fibers stained deep brown with slow myosin MyHC I antibody with the peroxidase detection, and fast type 2A fibers stained deep pink-red with fast myosin MyHC IIA A4.74 antibody using the alkaline phosphatase red detection system. Type 2C fibers being MyHC I and IIA isoform hybrid fibers stained red-brown showing the presence of both slow and fast MyHC isoforms in these fibers. Moreover, this technique was also able to separate the ultrafast myosin MyHC IIX expressing type 2B fibers on the same slide that were immunonegative for the myosin A4.74 antibody. Capillaries or other structures were not labeled (Fig. 1).
Immunohistochemical MyHC double staining with red fibers expressing IIA, blue fibers showing IIX, and brown fibers showing I MyHC isoforms a. Corresponding ATPase histochemistry at pH 4.3 b, pH 4.6 c, pH 10.4 d distinguishing different fiber types. *A pink hybrid fiber expressing both IIA and IIX MyHC
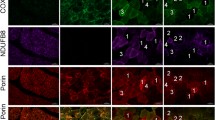
In the disease samples, myosin immunohistochemistry provided additional information not easily obtained by ATPase enzyme histochemistry. In DM 2 samples, all nuclear clump fibers and other highly atrophic fibers were readily detected as fast type IIA (ATPase type 2A) in red (Fig. 2). This finding was re-confirmed by immunoreactivity for neonatal myosin heavy chain isoform, as all these highly atrophic type IIA (ATPase type 2A) fibers also express neonatal MyHC as part of the disease process (data not shown). Fiber-type grouping as a result of chronic neurogenic change was absent in both DM1 and DM2, whereas the number of hybrid fibers was increased in both. In the muscle biopsies of patients with neurogenic disease, fiber-type grouping was comparably identified as with ATPase technique, but highly atrophic fibers in severe neurogenic end-stage samples were more easily identified with the immunohistochemical double staining (Fig. 3). Different fiber types were also easily distinguished in muscle samples of patients with LGMD2I, myositis and a mutation in the MYH7 gene (Fig. 4).
Immunohistochemical MyHC double staining with red fibers expressing IIA, blue fibers IIX and brown fibers I MyHC isoforms a and ATPase stainings at pH 4.3 b, pH 4.6 c and pH 10.4 d. Highly atrophic fibers in severe neurogenic end-stage samples are more easily identified and typed with the MyHC double staining. Arrows in a show highly atrophic fibers. *The same red-brown hybrid fiber co-expressing MyHC isoforms I and IIA (ATPase type 2C)
Immunohistochemical MyHC double stainings of muscle sections with various pathologies. a Patient with genetically verified early-onset Laing myopathy showing fiber-type disproportion with smaller type I fibers. b Genetically verified LGMD2I. c Neurogenic atrophy showing marked fiber-type grouping and d polymyositis asterisks showing red-brown fiber co-expressing MyHC isoforms I and IIA (ATPase type 2C). Red fibers expressing IIA, blue fibers IIX and brown fibers I MyHC isoforms
Discussion
In this study, we have analyzed the utility of immunohistochemistry of MyHC isoforms as an alternative to conventional ATPase histochemistry for fiber-type separation and identification. The immunohistochemical method primarily developed for the screening of fast type IIA (ATPase type 2A), nuclear clump or other highly atrophic fibers characteristic of DM2 disease proved to be a very robust and reliable method for routine diagnostic purposes. The immunohistochemical MyHC double staining was very efficient for the detection and separation of different muscle fiber types and their subtypes. In all DM2 patient biopsies, the subpopulation of highly atrophic fast type IIA (ATPase type 2A) and nuclear clump fibers was clearly identified. In comparison with the conventional ATPase technique, this immunohistochemical method provides a few advantages in the diagnostic routine: (1) The immunohistochemical MyHC double staining is faster and less labor intense. (2) Vanishing of ATPase enzyme histochemistry staining over time is not a problem with immunohistochemical labeling. (3) Frequent minor technical problems with ATPase due to improper reagents is not an issue with immunohistochemistry. (4) Crucial information about fiber-type distribution was not compromised using this novel method. In fact, even more reliable information could be obtained with immunohistochemical double staining, i.e., regarding the occurrence of highly atrophic fibers because capillaries were not stained as with ATPase histochemistry. (5) The identification of 2C fibers as being hybrids of MyHC isoforms I and IIA was easier and very reliable. Type IIX fibers, type 2B with ATPase, were readily separated and showed counterstaining with hematoxylin, but no immunoreactivity. Moreover, the detection of hybrids expressing both IIA (ATPase type 2A) and IIX (ATPase type 2B) MyHC was possible (Fig. 1), which was not the case with ATPase, although the biological or pathological significance of these specific hybrids was not determined. (6) The explicit advantage of this method is that all fiber-type information is available on one and the same slide.
The primary purpose of finding a reliable method for the screening of DM2 disease by the identification of the highly atrophic type IIA (ATPase type 2A) and nuclear clump type IIA(ATPase type 2A) fibers in muscle biopsies was very successful (Fig. 2). However, in our 4 years of experience with this technique, it has proven to be a primary tool of much larger advantage in the routine diagnostic procedure. Since the method provides more reliable and easier access to information of the different fiber types than conventional ATPase histochemistry, we believe that MyHC isoform double staining immunohistochemistry can be used as a very good, if not superior, alternative in routine diagnostics.
References
Bancroft JD, Cook HC (1994) Manual of histological techniques and their diagnostic application. Churchill Livingstone, Edinburgh
Dye DE, Azzarelli B, Goebel HH, Laing NG (2006) Novel slow-skeletal myosin (MYH7) mutation on the original myosin storage myopathy kindred. Neuromuscul Disord 16:357–360
Harper PS (2001) Myotonic dystrophy. WB Sauders, London
Izumo S, Nadal-Ginard B, Mahadavi V (1986) All members of the MHC multigene family respond to thyroid hormone in a highly tissue-specific manner. Science 231:597–600
Laing NG, Laing BA, Meredith C et al (1995) Autosomal dominant distal myopathy: linkage to chromosome 14. Am J Hum Genet 56:422–427
Liquori C, Ricker K, Moseley ML et al (2001) Myotonic dystrophy type 2 caused by a CCTG expansion in intron 1 of ZNF9. Science 293:864–867
Mahadevi V, Strehler EE, Periasamy M, Wieczorek DF, Izumo S, Nadal-Ginard B (1986) Sarcomeric myosin heavy chain gene family: organization and pattern of expression. Med Sci Sports Exerc 18:299–308
Martinsson T, Oldfors A, Darin N et al (2000) Autosomal dominant myopathy: missense mutation (Glu-706 → Lys) in the myosin heavy chain IIa gene. Proc Natl Acad Sci USA 97:14614–14619
Meredith C, Hermann R, Parry C et al (2004) Mutations in the slow muscle fiber myosin heavy chain gene (MYH7) cause Laing early-onset distal myopathy (MPD1). Am J Hum Genet 75:703–708
Oldfors A, Darin N, Martinsson T (2002) Autosomal dominant myosin heavy chain IIa myopathy. In: karpati G (ed) Structural and molecular basis of skeletal muscle diseases. ISN Neuropath Press, Basel, pp 85–87
Oldfors A, Tajsharghi H, Thornell LE (2005) Mutation of the slow myosin heavy chain rod domain underlies hyaline body myopathy. Neurology 64:580–581
Pette D, Vrbová G (1992) Adaptation of mammalian skeletal muscle fibers to chronic electrical stimulation. Rev Physiol Biochem Pharmacol 120:115–202
Rayment I, Holden HM, Whittaker M et al (1993) Structure of the actin complex and its implications for muscle contraction. Science 261:58–65
Ruppel KM, Spundich JA (1996) Structure–function analysis of the motor domain of myosin. Annu Rev Cell Dev Biol 12:543–573
Tajsharghi H, Oldfors A, Macleod DP, Swash M (1997) Homozygous mutation in MYH7 in myosin storage myopathy and cardiomyopathy. Neurology 68:962
Tajsharghi H, Thornell LE, Lindberg C, Lindvall B, Hendriksson KG, Oldfors A (2003) Myosin storage myopathy associated with a heterozygous missense mutation in MYH7. Ann Neurol 54:494–500
Udd B, Meola G, Krahe R et al (2006) 140th ENMC international workshop: myotonic dystrophy DM2/PROMM and other myotonic dystrophies with guidelines on management. Neuromuscul Disord 16:403–413
Udd B, Meola G, Krahe R et al (2003) Report of the 115th ENMC workshop: DM2/PROMM and other myotonic dystrophies. 3rd Workshop, 14–16 February 2003, Naarden, The Netherlands. Neuromuscul Disord 13:589–596
Udd B, Krahe R, Wallgren-Petterson C, Falkc B, Kalimo H (1997) Proximal myotonic dystrophy—a family with autosomal dominant muscular dystrophy, cataracts, hearing loss and hypogonadism: heterogeneity of proximal myotonic syndromes? Neuromuscl Disord 7:217–218
Vihola A, Bassez G, Meola G et al (2003) Histopathological differences of myotonic dystrophy type 1 (DM1) and PROMM/DM2. Neurology 60:1854–1857
Weiss A, McDonough D, Wertman B et al (1999) Organization of human and mouse skeletal myosin heavy chain gene clusters is highly conserved. Proc Natl Acad Sci USA 96:2958–2963
Acknowledgments
We thank Henna-Riikka Koskinen, Jaana Leppikangas and Satu Luhtasela for their expert technical assistance. This research was supported by funding from Tampere University Hospital Medical Research funds, The Folkhälsan Research Foundation and grants from the Liv&Hälsa Foundation.
Conflict of interest statement
None declared.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Raheem, O., Huovinen, S., Suominen, T. et al. Novel myosin heavy chain immunohistochemical double staining developed for the routine diagnostic separation of I, IIA and IIX fibers. Acta Neuropathol 119, 495–500 (2010). https://doi.org/10.1007/s00401-010-0643-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00401-010-0643-8