Abstract
We have analyzed development of mechanical hyperalgesia after repeated systemic lipopolysaccharide (LPS) injections and correlated these findings with stimulation of astrocytes and microglia in spinal cord. Male Lewis rats received a single or seven intraperitoneal injections of LPS. Mechanical hyperalgesia was measured as rat hindpaw withdrawal thresholds (PWTs). We observed that a single LPS injection elicited a specific change of PWTs while stimulated spinal glial activation was identified by immunoreactivities of specific markers, ED1, P2X4 receptor, endothelial monocyte activating polypeptide II (EMAP II) and glial fibrillary acidic protein (GFAP), respectively; multiple LPS treatments induced tolerance to mechanical hyperalgesia, whereas expression of ED1 and GFAP were further increased. In conclusion, we have demonstrated that the number of activated spinal glial cells was increased as an acute effect of LPS correlating with increased sensitivity to mechanical stimulation. However chronic exposure to LPS can develop a tolerance to mechanical hyperalgesia despite ongoing signs of CNS glial activation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Glial cells contribute to the innate immune system of the central nervous system (CNS), and are active participants in neuroinflammation responding to a variety of stressors to the CNS [18, 23, 39]. Evidence has recently accumulated that pathological pain, including neuropathic pain and inflammatory pain, is amplified as the consequence of spinal cord glial activation, which is elicited by CNS injury or neuroinflammation [8, 49–51]. Upon activation, glial cells change their morphology from a resting, ramified shape into a hypertrophic and less ramified appearance, and up-regulate expression of a variety of cell-surface molecules, including ED1 [7], P2X4 receptor (P2X4R) [16, 17], endothelial monocyte activating polypeptide II (EMAP II) (for activated microglia) [42], and glial fibrillary acidic protein (GFAP) (for activated astrocyte). Also, activated glia release proinflammatory cytokines, which are important in mediating hyperalgesia and allodynia [9, 30, 51].
Noxious-stimuli-induced peripheral nerve damages can elicit pathological pain characterized by hyperalgesia [60], which can be produced by an intraperitoneal (i.p.) injection of proinflammatory cytokines, or a lipopolysaccharide (LPS) [26]. LPS, a major component of the outer membrane of gram-negative bacteria, is an important ligand of toll-like receptor 4 (TLR4). Systemic administration of LPS mimics many clinical effects of the bacterial infections including inflammation, changes in immune functions, and pain [31, 48, 52]. Several studies have shown that an i.p. injection of LPS enhances pain responsiveness to various somatic stimuli. Moreover, LPS-induced alterations in nociception depend on proinflammatory cytokines released from CNS immune cells [52, 58]. While several studies have established that a single injection of LPS can produce behavioral hyperalgesia in rodents [52, 58], little is known about the chronic effect of intermittent exposure to endotoxin on rat behaviors, as well as on spinal glia fate. In this study, we have compared the effects of acute and chronic LPS administrations on rat mechanical sensitivity and spinal glia activation.
Materials and methods
Animals
Six-weeks-old male Lewis rats (160–170 g at the first injection) (Charles River, Sulzfeld, Germany) were used. The animals were housed at a constant temperature of 22°C on a 12/12 h light/dark cycle with food and water ad libitum, and allowed to habituate to the housing facilities for more than 1 week before the tests. All experiments were done in accordance with the published International Health Guidelines under a protocol approved by the Local Animal Care and Use Committee and the Administration District Official Committee.
Drugs
LPS (E. coli serotype 026:B6, Cat. L-8274) was purchased from Sigma Chemicals (Heidelberg, Germany). It was dissolved in sterile phosphate-buffered saline (PBS) at 1 mg/ml concentration and stored at −20°C in volumes of 1 ml. Sterile PBS was used to establish the control cohort. In all the experiments, freshly thawed LPS was administered intraperitoneally at 5 mg/kg body weight [5, 15, 40, 41].
Behavioral assessment
Mechanical hyperalgesia was measured as rat hindpaw withdrawl thresholds (PWTs), which were recorded by aesthesiometry (dynamic plantar aesthesiometer 37400; Ugo Basile, Milan, Italy). Each rat was placed in a clear plastic compartment of a two-compartment box with a wire mesh floor, and acclimatized to the new environment for 10–20 min per day, 3 days before testing. Before each test session, the rats were allowed to explore the surroundings for 3–5 min until they adopted a resting position. With the help of an adjustable angled mirror, the paw-flick response was elicited by applying an increased ascending force (measured in grams) using a steel filament (0.5 mm diameter) on the middle plantar of both hind paws. The force was applied randomly to the left or right hind paw, increasing from 1 to 50 g (5 g/s increasing rate, max. 20 s/test). When the rat withdrew its hind paw, the mechanical stimulus automatically stopped, and the force was recorded as PWT. The results were calculated as mean values of four consecutive measurements, which were separated by 1 min.
The baselines of PWTs were obtained 1 day before drug injection. According to the baseline, the rats were stratified into groups so that there were no significant differences of PWT mean values among groups. Three groups (six rats each) received either a single or multiple LPS injections, and three other control groups received PBS injections, respectively.
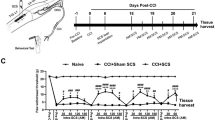
On the first day of the experiment, all the rats received either LPS or PBS i.p. injections. PWTs were measured by the researcher being blind to the treatment from 30 min to 48 h post injection. Then, two groups of rats were killed 2 days post the single injection to study the acute effect of the single LPS or the PBS injection; the two groups were spared to analyze the chronic effects of a single LPS injection; two other groups received six more LPS or PBS injections every second day (multiple treatment groups). The PWT measurements were done at 24 h post each treatment and at intervals of 48 h following the last treatment. All rats were killed 48 h post the seventh injection, i.e. 14 days post the first injection.
Immunohistochemical staining of the spinal cord sections
After the last behavioral test, three rats per group were perfused with 50–100 ml of 0.1 M PBS pH 7.4 containing 4% paraformaldehyde (PFA) under fatal ethyl ether (Sigma, Seelze, Germany) anesthesia. Spinal cords were removed and fixed overnight in PBS containing 4% PFA, equilibrated in PBS for more than 8 h and embedded in paraffin. Immunostaining was done on 3 μm sections.
Spinal cord sections were boiled (in a 600 W microwave oven) for optimized 15 min in citrate buffer (2.1 g sodium citrate/l, pH6, boiling point about 100°) in order to retrieve antigens of which epitopes may be preserved/masked during tissue fixation [44]. Endogenous peroxidase was inhibited by 1% H2O2 in methanol for 15 min. Sections were incubated with 10% normal pig serum (Biochrom, Berlin, Germany) to block non-specific binding of immunoglobulins, then with monoclonal antibodies against ED1 (specific marker for activated microglia/macrophages) (1:100; Serotec, Paisley, Great Britain), endothelial monocyte activating polypeptide II (EMAP-II) (1:100, BMA, Augst, Switzerland), rabbit polyclonal P2X4R antibodies (1:200, Alomone Labs, Jerusalem, Israel) raised against the P2X4R peptide (KKYKYVEDYEQGLSGEMNQ), and monoclonal antibody against glial fibrillary acid protein (GFAP) (1:500; Chemicon International, California, US). Antibodies binding to spinal cord tissues were detected with a biotinylated swine anti-rabbit IgG F(ab)2 antibody fragment (DAKO, Hamburg, Germany) for P2X4R or biotinylated rabbit anti-mouse IgG F(ab)2 antibodies fragment (DAKO, Hamburg, Germany) for ED1, EMAP-II, and GFAP, followed by incubation with a Streptavidin-Avidin-Biotin complex (DAKO, Hamburg, Germany) and development with diaminobenzidine (DAB) substrate (Fluka, Neu-Ulm, Germany). Finally, sections were counterstained by hematoxylin. Sections of rat C6 glioma were used as controls [11] for P2X4R and GFAP, and rat spleen for ED1, and EMAP-II. For negative controls, the primary antibodies were omitted.
Statistical analysis and evaluation of tissue staining
All statistical comparisons were computed using GraphPad Prism 4 for Windows. Data are given as mean values and standard errors of means (mean ± SEM). Behavioral data were analyzed using a two-way ANOVA followed by Bonferroni’s post hoc evaluation; p < 0.05 was considered significant.
Spinal cord sections were studied by light microscopy. Observers were blind to the experimental groups. The numbers of immunolabeled astrocytes and microglia of each spinal cord section were counted to represent the entire spinal cord by using an ocular morphometric grid (Olympus, Hamburg, Germany) in 10 high-power fields (HPF × 200 magnification with an eyepiece grid representing 0.25 mm2). Only positively stained cells with the nucleus at the focal plane were counted. Results are given as mean values of immunoreactive cells per HPF and standard errors of means (mean ± SEM). Statistical analysis was performed by a one-way ANOVA with post-hoc Tukey-HSD test. Significance levels were set at p < 0.05.
Results
A single i.p. injection of LPS-induced mechanical hyperalgesia
Baseline of behavioral data was obtained 1 day before the LPS injection. Then the rats received an i.p. injection of either 5 mg/kg LPS (n = 18) or 1 ml of PBS as a control (n = 18). The animals displayed an apparent sickness behavior (reduced activity, increased defecation, and piloerection) following the LPS treatments. There were no mortalities throughout the experiment. We observed a time-dependent pattern of mechanical hyperalgesia, which was recorded as a reduction in rat hindpaw withdrawal thresholds measured from 30 min to 48 h after the first injection (Fig. 1a). Compared to the PBS-injected control rats, a single injection of LPS produced a significant reduction of PWT. The first significant decrease was measured at 60 min post-injection (vs. baseline, p < 0.05; vs. vehicle group, p > 0.05), and was maximal by 24 h (vs. baseline, p < 0.001; vs. vehicle group, p < 0.001). Therefore, the following PWTs induced by repeated injection were measured 24 h post each treatment. 48 h post injection, PWT values decreased close to baseline levels (vs. baseline, p < 0.05; vs. vehicle group, p > 0.05). Thus, mechanical hyperalgesia induced by LPS injection is an acute effect. As shown in Fig. 1b, PWT data from rats sampled every 48 h for even a longer period clearly demonstrated a maximal reduction of PWTs within the first 24 h only (PBS vs. LPS, p < 0.05; n = 6 for each group). Thereafter, PWT mean values of the LPS group gradually returned to those of the control (Fig. 1b).
Time-dependent reduction of rat hindpaw withdrawal thresholds. Rats received i.p. injections of either 5 mg/kg LPS or PBS. Values represent changes of PWTs (mean ± SEM) obtained at various times after injection. Acute mechanical hyperalgesia was seen within 48 h following single LPS injection (a) (n = 18 for each group). No chronic hyperalgesic effect was seen when PWTs were measured every second day during a 2 weeks period (b) (n = 6 for each group). Statistical analysis was performed by two-way ANOVA with Bonferroni post-tests. *p < 0.05, **p < 0.01, or ***p < 0.001 denote the significance levels of data from the LPS treated group compared to control group
Tolerance developed to induction of mechanical hyperalgesia by repeated LPS treatments
To examine the effects of repeated LPS injections, PBS or LPS was injected every second day for a total of seven injections. As shown in Fig. 2a, the first LPS administration produced a significant reduction in rat hindpaw withdrawal thresholds as compared to the control group (see also Fig. 1a). In contrast, the reduction in PWTs post the seventh injection of LPS was substantially less than that induced by the first one (p < 0.05 at each time point) (Fig. 2a). In detail, we compared PWT mean values at 100 min, 24 h, 48 h post every injection (Fig. 2b, c, and d respectively). During the 2 weeks period of this experiment, no significant changes were measured in PWTs of control rats thus excluding the habituation effect during the present aesthesiometer testing. We observed that hyposensitivity rapidly developed after repeated LPS injections. At 100 min post injection, the reduction of PWTs was maximal after the second LPS treatment (Fig. 2b). At 24 h post every LPS injection, the maximal mean values of PWT reduction were obtained after the first injection. Then the PWTs values slowly returned to baseline levels (Fig. 2c). In addition, at each 48 h post injection recording, no significant hyperalgesia could be detected (Fig. 2d).
Effects of repeated injection of LPS on rat hindpaw withdrawal thresholds. Data show PWTs (mean ± SEM, six rats per group) at various times after the first and the last injection of either LPS of PBS (a). Significant differences can be seen between PWTs of the first and the seventh LPS injection. In details, PWTs values (mean ± SEM) at every 100 min (b), 24 h (c), and 48 h (d) are shown, showing a reduction of the hyperalgesic effect of LPS after repeated injections, thus demonstrating the development of LPS tolerance. Statistical analysis was performed by two-way ANOVA with Bonferroni post-tests. *p < 0.05 denotes the significance level of data from the first compared to the seventh injection
Immunoreactivities of specific markers of spinal cord glia activation following LPS administration
The activation of astrocytes was evaluated as the immunoreactivity of GFAP (GFAP-IR) in both gray matter and white matter. In the white matter, differences of GFAP-IR were not observed (data not shown). In the gray matter as shown in Figs. 3 and 4a, the GFAP-IR was significantly elevated in the spinal cord sections following the LPS administration as compared to the control rats. In these spinal cords mild GFAP-IR (Fig. 3, left column) was observed. In the rat spinal cords sampled at 48 h post a single LPS injection, the GFAP-IR was increased, and an activation of astrocytes was further evident by a hypertrophic morphology (Fig. 3, left column). The number of immunostained cells was significantly higher than that of the control group (1.4-fold increase vs. vehicle group; p < 0.01, n = 3) (Fig. 4a). This activation appears to be transient, and 14 days post injection, no increased numbers of GFAP+ astrocytes could be demonstrated (vs. PBS, p > 0.05, n = 3) (Fig. 4a), although the GFAP staining revealed still an activated astrocytic morphology (Fig. 3, left column). After multiple LPS injections, i.e. seven times, the spinal GFAP-IR was further increased (1.9-fold increase vs. the PBS group; p < 0.001, n = 3) (Fig. 4a) (see also Fig. 3, left column). Interestingly, no changes of GFAP+ cell numbers were recorded between groups which were sampled at 48 h or 14 days after a single LPS injection (p > 0.05), or between 48 h after a single LPS or multiple LPS treated groups (p > 0.05); whereas, significant differences between repeatedly treated group and 14 days post single LPS treated group can be seen (p < 0.001) (Fig. 4a).
Immunoreactivities of GFAP and ED1 in the spinal cord gray matter of LPS treated rat. Representative micrographs of spinal cord sections were taken from different LPS treated rats and controls (injection of PBS). Astrocytes were stained with GFAP antibody (left column), and microglia were stained with ED1 antibody (right column). As indicated, two LPS-treated groups (single injection) were sampled either at 48 h or 14 days after injection, and one group received multiple LPS injections (seven times, every second day). Arrows indicate ED1+ cells, and arrowheads indicate peri-neuronal position of ED1+ cells. Scale bar, 50 μm (n = 3 per group)
Increased glial activation in rat spinal cord gray matter after a single or repeated LPS injections. Spinal cord sections of three rats per group were used for immunostaining. Two LPS treated groups (single injection) were sampled at 48 h or 14 days after injection. One group received multiple LPS injections (seven times, every second day). Statistical analysis was performed by evaluating the changes in numbers of GFAP+ (a), or ED1+ cells (b). Results are given as mean values of numbers of positive cells per HPF (mean ± SEM). Statistical analysis was performed by one-way ANOVA with post-hoc Tukey-HSD test. **p < 0.01, ***p < 0.001 denote significance levels of comparison of data of each LPS treated group to its respective control group; +++ p < 0.001 denotes the significance level of data from of LPS groups
Activated microglia/macrophages were indicated by the immunoreactivity of ED1 (ED1-IR) in both gray matter and white matter. Few ED1+ cells were homogeneously distributed throughout the spinal gray or white matter in all controls spinal cords (Fig. 3, right column). Sections of PBS-treated control rats did not show any ED1-IR changes throughout the experiment (n = 3 for each group). After the first LPS injection, the ED1+ cells exhibited a hypertrophic morphology but not a rounded, amoeboid shape, and numbers of parenchymal ED1+ cells increased significantly (2.4-fold increase vs. vehicle group; p < 0.001, n = 3) (Fig. 4b). However no changes of ED1-IR on perivascular cells were observed and no perivascular accumulation was seen (data not shown), indicating that recruitment of macrophages was not prominent. Peri-neuronal staining can be seen (Fig. 3, right column, arrowhead); 14 days after a single LPS treatment, numbers of spinal ED1+ microglia were still higher than that of the control group (2.6-fold increase versus vehicle group; p < 0.001, n = 3). Repeated LPS injections induced a considerable increase in numbers of ED1+ cells. The numbers of ED1+ microglia in spinal cords of repeatedly LPS treated rats were significantly higher than that after a single LPS treatment (1.6-fold increase vs. single LPS group sampled at 48 h, p < 0.001; 1.8-fold increase vs. single LPS group sampled in 14 days, p < 0.001), as well as higher than control groups (3.6-fold increase vs. PBS group; p < 0.001) (see also Fig. 3, right column).
We further investigated two other markers, P2X4R and EMAP-II, for activated microglia/macrophages. In PBS-treated rats spinal cords, both P2X4R (P2X4R-IR) and EMAPII immunoreactivity (EMAPII-IR) were occasionally seen on single perivascular cells (Fig.5, arrows), but rarely in spinal parenchyma. As there were no differences among the control groups, we grouped all data together. Following the LPS injection, activated microglia cells were indicated by an increase in the number of P2X4R-IR and EMAPII-IR and by morphological criteria—the development of a hypertrophic morphology with thick processes but not in the rounded, amoeboid macrophage-like shape (Fig. 5, higher magnifications). After a single LPS or PBS injection, P2X4R+ cells were still rarely seen in the white matter. The numbers of P2X4R+ cells in gray matter were considerably higher than that in the vehicle spinal cord sections (each single LPS group vs. PBS group: p < 0.05, n = 3) (Fig. 6a) (see also Fig. 5, left column), irrespective of single or repeated LPS injections (p > 0.05). The repeated LPS treatment up regulated the P2X4R expression significantly (multiple LPS treated group vs. vehicle group: p < 0.001, n = 3), and the differences between any single LPS injected group and multiple LPS injected group were significant (multiple LPS treated group vs. each single LPS group: p < 0.001, n = 3) (Fig. 6a). EMAPII-IR produced a similar expression pattern as P2X4R-IR (Fig. 5, right column). Briefly, in the control rats, few EMAPII+ cells were seen in the gray and white matter. An increase of EMAP-II+ microglia was detected after single and repeated LPS injections (Fig. 6b). In addition, there were no changes of P2X4R-IR or EMAP-II on perivascular staining and no perivascular accumulation was seen.
Activated microglia were identified by P2X4R-IR and EMAPII-IR. Spinal cord sections of three rats per group were used for immunostaining. Representative photographs of spinal cord sections showed immunoreactivities for two activated microglia markers, P2X4R (left column), EMAP-II (right column) (a). Control group (PBS injection); the other three groups received injections of LPS. Two LPS treated groups (single injection) were sampled either at 48 h or 14 days later. One group received multiple LPS injections (seven times, every second day). Arrows indicate single positive cells in spinal cords of control rats. Higher magnifications indicate that both P2X4R+ and EMAP-II+ cells showed typical hypertrophic microglial morphology. Scale bar, 25 μm for lower magnification, and 10 μm for higher magnification
P2X4R+ and EMAP-II+ microglia in spinal cord gray matter of LPS treated rats. Three rats per group were used for immunostaining. Control group (PBS injection); the other three groups received injections of LPS. Two LPS treated groups (single injection) were sampled either at 48 h or 14 days later. One group received multiple LPS injections (seven times, every second day). Statistical analysis was performed by evaluating the changes in numbers of P2X4R+ (a), or EMAP-II+ cells (b). Results are given as mean values of numbers of positive cells per HPF (mean ± SEM) as determined by one-way ANOVA with post-hoc Tukey-HSD test. *p < 0.05, ***p < 0.001 denote the significance levels when each LPS treated group was compared to its respective control group; +++ p < 0.001 denotes the significance level of data from LPS groups
Discussion
Here we show that a single LPS injection elicited a mechanical hyperalgesia accompanied by spinal glia activation. The repeated LPS injections induced tolerance to the development of hyperalgesia, but astrocytes and microglia were further stimulated.
Hyperalgesia is an important feature of pathological pain. So far, the exact mechanism of pain facilitation remains unresolved. However most recently, spinal cord glia, including microglia and astrocytes, has been recognized as an active participant in the creation and maintenance of pain facilitation induced by inflammation and damage to peripheral tissues, peripheral nerve, spinal nerves and spinal cord [29, 49, 54, 55]. In the present work, we observed that spinal cord glial cells, both astrocytes and microglia, were stimulated by a single LPS injection, which elicited a behavioral hyperalgesia. After peripheral nerve injury, both neural noxiously or non-noxiously, it is demonstrated that glial activation booms at late phases, generally 24 or 48 h post injury [17, 43]. In the present manuscript, rat spinal cords were sampled 48 h post each treatment [20]. The spinal cord astrocytes up regulated the GFAP expression, and became hypertrophic and less ramified in response to the systemic LPS. This is in line with the well-recognized importance of astrocytes in response to immune and inflammatory cascades in the CNS [2]. However, 48 h post injection, a single LPS did not induce a prolonged increase of GFAP-IR. Similar results have been reported from other inflammation models, which are produced by formalin or zymosan administration [46].
LPS activates microglia in a concentration-dependent manner [22]. LPS can also attract circulating monocytes into the brain but it is not clear as to what extent circulating monocytes entered the spinal cord in our experiments, as there are no reliable cell markers that distinguish macrophages from microglia. In the present work, we observed that LPS-activated microglial cells exhibited hypertrophic morphology but not a round, amoeboid shape, also a perivascular accumulation typical of recruited macrophages was not seen. This suggests, therefore, that microglia, but not recruited macrophages, play a role in the LPS-induced hyperalgesia tolerance. Microglial activation occurs in response to CNS trauma, ischemia, tumors, neurodegeneration and immunogenic components of viruses and bacteria [23]. LPS is a widely used stimulator of microglial activation in vivo and in vitro. We have observed a significant up regulation of ED1-IR in acute and chronic phases of LPS-stimulation that represented spinal microglia activation [7]. A single LPS injection elicited increased ED1-IR and development of mechanical hyperalgesia. This could indicate that activation of microglia might at least correlate with inflammation-induced changes in sensitivity to mechanical stimuli. At the same time, ED1+ cells were observed in perineuronal/axonal positions, implicating that neuron-glial signaling might be associated with hyperalgesia [5, 34]. However, at later stages, ED1+ cells were seen even 14 days after a single LPS injection, when behavioral sensitivity was reduced to control level. This persistence, which was not observed in GFAP-IR, is in line with previous observations in other pathological pain models, that the number of activated microglial cells keeps at submaximal levels 2 weeks after peripheral neural damages [13, 17, 43]. These observations implicate that activated microglia might have distinct roles in acute and chronic stages of inflammatory pathologies. In the chronic stage, microglial activation may reflect an increased response to tissue damages that is not associated with hyperalgesia [13]. Interestingly, according to our data, LPS tolerance was clearly seen in behavioral analysis but not in the expression of glial activation markers. Particularly, ED1-IR was even significantly higher than the response to a single LPS injection. In this case, the stimulation of microglia was independent of behavioral hyperalgesia. It could be presumed that microglia might have a putative role in response to the chronic noxious CNS stimuli that strategically differ from that of the acute phase. The time and distribution patterns of ED+ cells held also true for P2X4R-IR and EMAPII-IR, two specific markers of activated microglia [16, 42]. P2X4R is an ATP-gated ion channel and involved in initiating certain primary afferent signals [38]. Recently, P2X4R has been defined a sensor role in pathological pain [47]. Our previous studies demonstrated that the expression of this receptor paralleled ED1+ cells in either spinal cord injury or formalin-induced inflammatory pain [17, 43]. EMAP-II has emerged as a potential proinflammatory mediator with the ability to stimulate chemotaxis of mononuclear phagocytes and polymorphonuclear leukocytes [21]. EMAPII-IR is a tool to stage activation and differentiation of rat microglial cells [32, 42]. We confirmed in the present study the expression of EMAP-II by activated microglial cells in different stages of LPS-induced inflammation. Moreover, a pronounced increase of numbers in P2X4R+ and EMAP-II+ microglia following single and multiple LPS treatments suggests both P2X4R and EMAP-II might have a role in LPS tolerance in the CNS.
LPS is recognized by toll-like receptor 4 (TLR4), which is involved in controlling the innate immune response to initiate an intracellular signaling pathway [28, 37, 57]. In the CNS, LPS is capable of stimulating in vitro and in vivo expression of a large number of cytokines [12, 26, 52], which can initiate a persistent activity in small primary afferents that in turn evoke a cascade leading to a decreased response threshold, and results into a behaviorally defined hyperalgesia [14, 26, 52]. In the present work, a mechanical hyperalgesia developed as soon as 60 min post systemic LPS injection correlating with other known effects of a single LPS like fever and anorexia, which likewise occur rapidly and coincide with release of immune mediators [34, 35]. We also found that a single LPS administration produced a unique time-dependent mechanical hyperalgesia, which persisted longer (> 24 h) than the documented increases in production of cytokines [22]. It suggests that LPS-stimulated immune responses might attend the initiation rather than maintenance of hyperalgesia. On the other hand, we have demonstrated a tolerance to the hyperalgesic effect of repeated LPS treatments. To date, the molecular mechanisms of endotoxin tolerance of pain related behaviors remain unclear. Generally, LPS tolerance has been termed as a reduced in vivo or in vitro capacity of the host to respond to LPS activation [1, 11]. We observed that LPS tolerance resulted in a reduction of behavioral hyperalgesia and similar observations have been reported in the development of fever, anorexia, and lethality as well [3, 4, 36]. The possible interpretation of our results may be manifold and might include enhanced LPS binding protein synthesis and increase clearance of circulating LPS that lead to dramatic reduction of proinflammatory cytokines synthesis [27, 54, 59, 61]. However, although our data suggest that spinal glia may attend the inflammatory pain induced by a single noxious stimulus, multiple LPS induced immunoreactivities of glial activation markers did not correlate with hyperalgesia.
Many factors influence pain sensitivity. The genetic background influences pain sensitivity, which is widely variable among species and strains. Genetic origin of pain has been investigated and the underlying genes have been tentatively characterized as quantitative trait loci (QTL) only [10, 14, 56]. Strain differences of QTL influences involved in nociceptive process have been mostly discussed in mice, which are rather more sensitive to LPS than rats. The Lewis rat strain is frequently use for study of immune regulation, particularly autoimmune diseases [25, 53], in which the role of glial cells are widely investigated. This is mainly due to peculiarities of MHC-associated antigen recognition but it has been reported that this and other rat strains are over-reactive to immune stimuli [24]. The role of genetic traits in LPS responsiveness in ongoing and cannot be addressed in this study. Over the last few years, the role of spinal glia as a significant contributor to the initiation and maintenance of pain states is becoming more and more evident and thus, they are considered drugs target in the development of new pain therapeutics [29, 51]. Repeated exposure to bacterial infection well mimics clinical chronic inflammation [37]. In the present study, therefore, we have achieved this condition and investigated glial activation during it in Lewis rats. Generally, the neuroprotective or neurotoxic functions of activated microglia and astrocytes should be discussed under different stimuli and pathological conditions [33]. Taken together, the present data suggest that under chronic stimulation, expression of glial activation marker might correlate with inflammation rather than chronic pain state. The fate of microglia and astrocytes in the relationship between inflammatory pain and chronic inflammation needs to be carefully addressed.
References
Ajmone-Cat MA, Nicolini A, Minghetti L (2003) Prolonged exposure of microglia to lipopolysaccharide modifies the intracellular signaling pathways and selectively promotes prostaglandin E2 synthesis. J Neurochem 87:1193–1203
Aschner M (1998) Immune and inflammatory responses in the CNS: modulation by astrocytes. Toxicol Lett 102–103:283–287
Cavaillon JM (1995) The nonspecific nature of endotoxin tolerance. Trends Microbiol 3:320–324
Cavaillon JM, Adrie C, Fitting C, Adib-Conquy M (2003) Endotoxin tolerance: is there a clinical relevance? J Endotoxin Res 9:101–107
Chu SJ, Perng WC, Hung CM, Chang DM, Lin SH, Huang KL (2005) Effects of various body temperatures after lipopolysaccharide-induced lung injury in rats. Chest 128:327–336
Coull JA, Beggs S, Boudreau D, Boivin D, Tsuda M, Inoue K, Gravel C, Salter MW, De Koninck Y (2005) BDNF from microglia causes the shift in neuronal anion gradient underlying neuropathic pain. Nature 438:1017–1021
Damoiseaux JG, Dopp EA, Calame W, Chao D, MacPherson GG, Dijkstra CD (1994) Rat macrophage lysosomal membrane antigen recognized by monoclonal antibody ED1. Immunology 83:140–147
DeLeo JA, Tanga FY, Tawfik V (2004) Neuroimmune activation and neuroinflammation in chronic pain and opioid tolerance/hyperalgesia. The Neuroscientist 10:40–52
DeLeo JA, Yezierski RPB (2001) The role of neuroinflammation and neuroimmune activation in persistent pain. Pain 90:1–6
Devor M, Gilad A, Arbilly M, Yakir B, Raber P, Pisante A, Darvasi A (2005) pain1: a neuropathic pain QTL on mouse chromosome 15 in a C3HxC58 backcross. Pain 116:289–293
Fan H, Cook JA (2004) Molecular mechanisms of endotoxin tolerance. J Endotoxin Res 10:71–84
Ferreira SH, Lorenzetti BB, Bristow AF, Pooles S (1988) Interleukin-1 beta as a potent hyperalgesic agent antagonized by a tripeptide analogue. Nature 334:698–700
Fu KY, Light AR, Maixner W (2000) Relationship between nociceptor activity, peripheral edema, spinal microglial activation and long-term hyperalgesia induced by formalin. Neuroscience 101:1127–1135
Furuse T, Miura Y, Yagasaki K, Shiroishi T, Koide T (2003) Identification of QTLs for differential capsaicin sensitivity between mouse strains KJR and C57BL/6. Pain 105:169–175
Gong JP, Dai LL, Liu CA, Wu CX, Shi YJ, Li SW, Li XH (2002) Expression of CD14 protein and its gene in liver sinusoidal endothelial cells during endotoxemia. World J Gastroenterol 8:551–554
Guo LH, Trautmann K, Schluesener HJ (2004) Expression of P2X4 receptor in rat C6 glioma by tumor-associated macrophages and activated microglia. J Neuroimmunol 152(1–2):67–72
Guo LH, Trautmann K, Schluesener HJ (2005) Expression of P2X4 receptor by lesional activated microglia during formalin-induced inflammatory pain. J Neuroimmunol 163:120–127
Hanisch UK (2002) Microglia as a source and target of cytokines. Glia 40:140–55
Ignatowski TA, Covey WC, Knight PR, Severin CM, Nickola TJ, Spengler RN (1999) Brain-derived TNFalpha mediates neuropathic pain. Brain Res 841:70–77
Jiang-Shieh YF, Wu CH, Chien HF, Wei IH, Chang ML, Shieh JY, Wen CY (2005) Reactive changes of interstitial glia and pinealocytes in the rat pineal gland challenged with cell wall components from gram-positive and -negative bacteria. J Pineal Res 38:17–26
Kao J, Houck K, Fan Y, Haehnel I, Libutti SK, Kayton ML, Grikscheit T, Chabot J, Nowygrod R, Greenberg S, Kuang WJ, Leung DW, Hayward JR, Kisielll W, Heath M, Brett J, Stern DM (1994) Characterization of a novel tumor-derived cytokine. Endothelial-monocyte activating polypeptide II. J Biol Chem 269:25106–25119
Kehl LJ, Kovacs KJ, Larson AA (2004) Tolerance develops to the effect of lipopolysaccharides on movement-evoked hyperalgesia when administered chronically by a systemic but not an intrathecal route. Pain 111:104–115
Kreutzberg GW (1996) Microglia: a sensor for pathological events in the CNS. Trends Neurosci 19:312–318
Lariviere WR, Sattar MA, Melzack R (2006) Inflammation-susceptible Lewis rats show less sensitivity than resistant Fischer rats in the formalin inflammatory pain test and with repeated thermal testing. J Neurophysiol 95:2889–2897
Liebert UG, Linington C, ter Meulen V (1988) Induction of autoimmune reactions to myelin basic protein in measles virus encephalitis in Lewis rats. J Neuroimmunol 17:103–118
Maier SF, Wiertelak EP, Martin D, Watkins LR (1993) Interleukin-1 mediates the behavioral hyperalgesia produced by lithium chloride and endotoxin. Brain Res 623:321–324
Mathison JC, Virca GD, Wolfson E, Tobias PS, Glaser K, Ulevitch RJ (1990) Adaptation to bacterial lipopolysaccharide controls lipopolysaccharide-induced tumor necrosis factor production in rabbit macrophages. J Clin Invest 85:1108–1118
Medzhitov R, Preston-Hurlburt P, Kopp E, Stadlen A, Chen C, Ghosh S, Janeway CA Jr (1998) MyD88 is an adaptor protein in the hToll/IL-1 receptor family signaling pathways. Mol Cell 2:253–258
Miller G (2005) Neuroscience. The dark side of glia. Science 308:778–781
Milligan ED, O’Connor KA, Nguyen KT, Armstrong CB, Twining C, Gaykema RP, Holguin A, Martin D, Maier SF, Watkins LR (2001) Intrathecal HIV-1 envelope glycoprotein gp120 induces enhanced pain states mediated by spinal cord proinflammatory cytokines. J Neurosci 21:2808–2819
Morrison DC (1987) Endotoxin and disease mechanisms. Annu Rev Med 38:417–432
Mueller CA, Schluesener HJ, Conrad S, Meyermann R, Schwab JM (2003) Spinal cord injury induces lesional expression of the proinflammatory and antiangiogenic cytokine EMAP II. J Neurotrauma 20:1007–1015
Nakajima K, Kohsaka S (2004) Microglia: neuroprotective and neurotrophic cells in the central nervous system. Curr. Drug Targets Cardiovasc. Haematol. Disord. 4:65–84
Nava F, Calapai G, Facciola G, Cuzzocrea S, Giuliani G, DeSarro A, Caputi AP (1997) Melatonin effects on inhibition of thirst and fever induced by lipopolysaccharide in rat. Eur J Pharmacol 331:267–274
Nava F, Calapai G, Facciola G, Cuzzocrea S, Marciano MC, DeSarro A, Caputi AP (1997) Effects of interleukin-10 on water intake, locomotory activity, and rectal temperature in rat treated with endotoxin. Int J Immunopharmacol 19:31–38
Nava F, Carta G (2000) Repeated lipopolysaccharide administration produces tolerance to anorexia and fever but not to inhibition of thirst in rat. Int J Immunopharmacol 22:943–953
Nguyen MD, D’Aigle T, Gowing G, Julien JP, Rivest S (2004) Exacerbation of motor neuron disease by chronic stimulation of innate immunity in a mouse model of amyotrophic lateral sclerosis. J Neurosci 24:1340–1349
North RA (2002) Molecular physiology of P2X receptors. Physiol Rev 82:1013–1067
Prat A, Biernacki K, Wosik K, Antel JP (2001) Glial cell influence on the human blood-brain barrier. Glia 36:145–55
Reddy MM, Mahipal SV, Subhashini J, Reddy MC, Roy KR, Reddy GV, Reddy PR, Reddanna P (2006) Bacterial lipopolysaccharide-induced oxidative stress in the impairment of steroidogenesis and spermatogenesis in rats. Reprod Toxicol (in press)
Ribeiro ML, Cella M, Farina M, Franchi A (2003) Crosstalk between nitric oxide synthase and cyclooxygenase metabolites in the estrogenized rat uterus. Prostaglandins Leukot Essent Fatty Acids 68:285–290
Schluesener HJ, Seid K, Zhao Y, Meyermann R (1997) Localization of endothelial-monocyte-activating polypeptide II (EMAP II), a novel proinflammatory cytokine, to lesions of experimental autoimmune encephalomyelitis, neuritis and uveitis: expression by monocytes and activated microglial cells. Glia 20:365–372
Schwab JM, Guo L, Schluesener HJ (2005) Spinal cord injury induces early and persistent lesional P2X(4) receptor expression. J Neuroimmunol 163:185–189
Shi SR, Chaiwun B, Young L, Cote RJ, Taylor CR (1993) Antigen retrieval technique utilizing citrate buffer or urea solution for immunohistochemical demonstration of androgen receptor in formalin-fixed paraffin sections. J Histochem Cytochem 41:1599–1604
Streit WJ, Walter SA, Pennell NA (1999) Reactive microgliosis. Prog Neurobiol 57:563–581
Sweitzer SM, Colburn RW, Rutkowski M, DeLeo JA (1999) Acute peripheral inflammation induces moderate glial activation and spinal IL-1beta expression that correlates with pain behavior in the rat. Brain Res 829:209–221
Tsuda M, Shigemoto-Mogami Y, Koizumi S, Mizokoshi A, Kohsaka S, Salter MW, Inoue K (2003) P2X4 receptors induced in spinal microglia gate tactile allodynia after nerve injury. Nature 424:778–783
Vincent D, Lefort J, Bureau M, Dry J, Vazgaftig BB (1991) Dissociation between LPS-induced bronchial hyperreactivity and airway edema in the guinea-pig. Agents Actions 34:203–204
Watkins LR, Maier SF (2003) Glia: a novel drug discovery target for clinical pain. Nature Reviews Drug Discovery 2:973–985
Watkins LR, Maier SF (2004) Targeting glia to control clinical pain: an idea whose time has come. Drug discovery today Therapeutic Strategies 1:83–88
Watkins LR, Milligan ED, Maier SF (2001) Glial activation: a driving force for pathological pain. Trends Neurosci 24:450–455
Watkins LR, Wiertelak EP, Goehler LE, Smith KP, Martin D, Maier SF (1994) Characterization of cytokine-induced hyperalgesia. Brain Res 654:15–26
Wekerle H, Bradl M, Linington C, Kaab G, Kojima K (1996) The shaping of the brain-specific T lymphocyte repertoire in the thymus. Immunol Rev 149:231–243
West MA, Heagy W (2002) Endotoxin tolerance: a review. Crit Care Med 30:S64–73
Wieseler-Frank J, Maier SF, Watkins LR (2004) Glial activation and pathological pain. Neurochem Int 45:389–395
Wilson SG, Chesler EJ, Hain H, Rankin AJ, Schwarz JZ, Call SB, Murray MR, West EE, Teuscher C, Rodriguez-Zas S, Belknap JK, Mogil JS (2002) Identification of quantitative trait loci for chemical/inflammatory nociception in mice. Pain 96:385–391
Wright SD (1999) Toll, a new piece in the puzzle of innate immunity. J Exp Med 189:605–609
Yirmiya R, Rosen H, Donchin O, Ovadia H (1994) Behavioral effects of lipopolysaccharide in rats: involvement of endogenous opioids. Brain Res 648:80–86
Ziegler-Heitbrock HW (1994) Molecular mechanism in tolerance to lipopolysaccharide. J Inflamm 45:13–26
Zimmermann M (2001) Pathobiology of neuropathic pain. Eur J Pharmacol 429:23–37
Zweigner J, Gramm HJ, Singer OC, Wegscheider K, Schumann RR (2001) High concentrations of lipopolysaccharide-binding protein in serum of patients with severe sepsis or septic shock inhibit the lipopolysaccharide response in human monocytes. Blood 98:3800–3808
Acknowledgment
We wish to thank Mrs. Trautmann for expert technical support. Mrs. Guo is a member of the Graduate College “Cellular mechanisms of immune-associated process” (DFG: GK 794).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Guo, LH., Schluesener, H.J. Acute but not chronic stimulation of glial cells in rat spinal cord by systemic injection of lipopolysaccharide is associated with hyperalgesia. Acta Neuropathol 112, 703–713 (2006). https://doi.org/10.1007/s00401-006-0135-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00401-006-0135-z