Abstract
Dual-specificity phosphatase 14 (Dusp14), an important negative modulator of mitogen-activated protein kinase (MAPK) signaling pathways, has been implicated in inflammatory immune response, cancers, cell differentiation and proliferation. The role of Dusp14 in chronic pressure overload-induced cardiac hypertrophy has not been explored. Here we have shown that Dusp14−/− knockout mice and cardiac-specific Dusp14 transgenic mice were generated and subjected to aortic banding (AB) for 4 weeks. Our results demonstrated that genetic loss of Dusp14 significantly aggravated cardiac hypertrophy, fibrosis, ventricular dilation and dysfunction, whereas transgenic cardiac-specific Dusp14 overexpression significantly attenuated AB-induced cardiac dysfunction and remodeling. In vitro, adenoviral overexpression of constitutive Dusp14 blocked angiotensin II-induced hypertrophic growth of cardiomyocytes, while Dusp14 knockdown led to opposite effects. Mechanistically, excessive phosphorylation of TAK1, P38MAPK and JNK1/2 was evidenced in Dusp14−/− knockout mice post-AB and inactivation of TAK1-P38MAPK and -JNK1/2 signaling using TAK1 inhibitor 5Z-7-ox shares similar antihypertrophic effect as Dusp14 overexpression. Moreover, we show that Dusp14 directly interacted with TAK1. Results from present experiments indicate that Dusp14 protects the heart from AB-induced cardiac hypertrophy and dysfunction possibly through inactivation of TAK1-P38MAPK/-JNK1/2 signaling pathway. Future studies are warranted to test the feasibility of overexpressing Dusp14 as a therapeutic strategy to attenuate cardiac hypertrophy and failure.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cardiac hypertrophy usually occurs in response to mechanical and neurohormonal stimuli such as hypertension, valvular insufficiency, genetic and ischemic heart disease, which is a key risk factor for heart failure, malignant arrhythmia and sudden death [5, 7, 21]. Characteristic features of cardiac hypertrophy include enlarged cardiomyocytes, interstitial fibrosis and reactivation of fetal cardiac gene programs [13]. Although these changes may initially represent a compensatory response of the myocardium, and temporarily normalize or even improve cardiac pump function, prolonged hypertrophy may often become maladaptive pathogenic process and relate to adverse prognosis [6, 8].
Signaling pathways controlling cardiac hypertrophy are intricate but coordinated networks [12]. Mitogen-activated protein kinase (MAPK) signaling cascades which consist of a well-conserved three-tiered kinase cascade (MAP3K–MAP2K–MAPK) are considered as important regulators of cardiac hypertrophic response [9, 29, 33]. Most importantly, once activated, the magnitude, duration as well as the subcellular compartment of MAPK cascades are critical determinants to achieve the desired outcome [29, 33]. Two subgroups of the dual-specificity phosphatases (Dusps), typical Dusps [also known as MAPK phosphatases (MKPs)] and atypical Dusps are able to dephosphorylate both serine/threonine and/or tyrosine residues within one substrate, providing a natural and necessary brake for MAPK signaling pathways [14, 26]. Although growing evidence has indicated the causative contribution of MAPK signaling pathways in the pathogenesis of cardiac hypertrophy, relatively little is known about the role of their negative regulators: Dusps. Therefore, exploration of Dusps-linked mechanisms in the heart may help to understand cardiovascular physio/patho-mechanisms of various cardiovascular diseases and provide potential Dusps-targeting-related therapeutic options for management of cardiac hypertrophy and failure.
Dusp14, a member of the atypical Dusps subgroup, initially was cloned as a novel CD28 cytoplasmic tail interacting protein, expressed ubiquitously with relatively high levels in heart, placenta and liver [23]. Dusp14 dephosphorylates extracellular signal-regulated kinases (ERKs), c-Jun N-terminal kinases (JNKs), and P38 kinases in vitro, while ERK and JNK but not P38 become hyperphosphorylated in dominant-negative Dusp14 (C111S)-transduced primary T cells [23]. β-cells expressing dominant-negative Dusp14 showed an increased rate of proliferation accompanied by increased ERK activation [17]. In both overexpression and endogenous systems, Dusp14 dephosphorylates TGFβ-activated kinase 1 (TAK1), a member of the MAPKKK family, at Thr-187 [39]. Thus, substrate specificity of Dusp14 remained enigmatic in vivo, although Dusp14 plays a part role in the regulation of MAPK signal transduction, and to the best of our knowledge, the role of Dusp14 in cardiac hypertrophy remained largely unaddressed. The aim of this study was, therefore, to elucidate the potential role and mechanism of Dusp14 in the pathogenesis of cardiac hypertrophy.
Herein, we provide the first evidence that Dusp14 serves as a novel negative regulator of pressure overload-induced cardiac hypertrophy and failure. After chronic aortic banding (AB), Dusp14-deficient mice exhibited aggravated prohypertrophic response, while less cardiac hypertrophy and dysfunction were observed in transgenic mice overexpressing Dusp14. At the molecular level, this antihypertrophic activity of Dusp14 involves inactivation of prohypertrophic signaling of TAK1-P38MAPK and -JNK1/2 following cardiac pressure overload. Taken together, aforementioned results indicate that Dusp14 might serve as a promising therapeutic target for targeting cardiac hypertrophy and failure.
Materials and methods
Reagents
Antibodies against phosphor-TAK1 (9339) at Ser412, TAK1 (4505), phospho-MEK1/2 (9154) at Ser217/221, MEK1/2 (9122), phospho-ERK1/2 (4370) at Thr202/Tyr204, ERK1/2 (4695), phospho-P38 (4511) at Thr180/Tyr182, P38 (9212), phospho-JNK1/2 (4668) at Thr183/Tyr185 and JNK1/2 (9258), phospho-NFκB(p65) at Ser536(3033) and NFκB(p65) (4764) were purchased from Cell Signaling Technology. The anti-ANP (sc20158), anti-β-MHC (sc53090) antibodies were from Santa Cruz Biotechnology. The Dusp14 antibody (PAB4143) was from Abnova. TAK1-specific inhibitor 5Z-7-oxozeaenol (5Z-7-ox; O9890-1 MG) was from Sigma. The GAPDH antibody (MB001) was from Bioworld Technology. The BCA protein assay kit was from Pierce. Fetal calf serum (FCS) was obtained from HyClone. All other reagents were purchased from Sigma.
Experimental animals
All animal experiments were performed in accordance with the guidelines of the Animal Care and Use Committee of Xinhua Hospital, Shanghai Jiao Tong University School of Medicine.
Generation of Dusp14 gene-deleted mice
Guide sequences of the target site for Dusp14 gene were obtained in the mouse genome by the online CRISPR design tool (http://crispr.mit.edu). A pair of oligomers (oligo1: TAGGGATGACGCAGGTGATGCCGC and oligo2: AAACGCGGCATCACCTGCGTCAT) for the generation of sgRNA expression plasmids were annealed and cloned into the BsaI restriction site of pUC57-sgRNA (Add gene 51132). DNA was amplified using PCR primers allowed for the detection of T7 promoter and sgRNA regions (forward primer: GATCCCTAATACGACTCACTATAG; reverse primer: AAAAAAAGCACCGACTCGGT). The PCR products were purified before being transcribed using the MEGAshortscript Kit (Ambion, AM1354) and purified using miRNeasy Micro Kit (QiaGen, 217084). Cas9 expression vector (Addgene 44758) was linearized with PmeI and in vitro as the template, transcribed using the T7 Ultra Kit (Ambion, AM1345). mRNA was purified using the RNeasy Mini Kit (QiaGen, 74104) according to the manufacturer’s instructions. Co-injections of one-cell embryos with Cas9 and sgRNA mRNA were performed using the FemtoJet 5247 microinjection system following standard conditions. Tail biopsies of the founder mice were collected to extract genomic DNA. Products from PCR amplification of the target region were subjected to the T7 endonuclease 1 (T7EN) cleavage assay. In brief, a 347-bp DNA fragment containing sgRNA target site was PCR amplified with the following primers: Dusp14-F (5′-GACTCCACTGCTCTCTGGTC-3′) and Dusp14-R (5′-CTTGTCGGCCACAGTGTCAA-3′). The PCR product was purified, then denatured and reannealed in NEB Buffer 2 (NEB). Hybridized PCR products were digested with T7EN (NEB, M0302L) for 45 min and analyzed by 2.0 % agarose gel. The mutant Dusp14 alleles’ presence in the tail samples was confirmed by sequencing PCR products. Primers used to screening F1 and F2 offspring were Dusp14-347-F (5′-GACTCCACTGCTCTCTGGTC-3′) and Dusp14-347-R (5′-CTTGTCGGCCACAGTGTCAA-3′). PCR products were analyzed by 3.0 % agarose gel electrophoresis. The wild-type allele yielded an amplicon of 347 bp, while the mutant allele yielded an amplicon of 291 bp.
Production of transgenic mice
We constructed the transgene vector pCAG-CAT-mDusp14 containing a CAG gene promoter (the modified chicken β-actin promoter with the CMV-IE enhancer)-loxP-CAT gene-loxP-mDusp14 region through replacing the lacZ gene of pCAG-loxP-CAT-loxp-lacZ with mouse Dusp14 cDNA. The construct was linearized and purified using the QIAquick Gel Extraction Kit (Qiagen, 28704) under manufacturer’s instructions followed by pronuclear microinjection. After identification by tail DNA amplification, founder transgenic mice were bred with C57BL/6J mice. Transgene detection with PCR primers [cag-For (5′-CCCCCTGAACCTGAAACATA-3′) and Dusp14-Rev (5′-AATGTCAGCCAGAGGCACTT-3′)] yielded a 582-bp product. CAG-CAT-Dusp14 mice (strain C57BL/6J) were crossed with alpha-MHC-MerCreMer mice to generate CAG-CAT-Dusp14/alpha-MHC-MerCreMer double transgenic mice. The double transgenic mice at 6 weeks age were treated with tamoxifen (80 mg/day) for consecutive 5 days to generate cardiac-specific conditional Dusp14 transgenic mice.
Aortic banding and drug treatment
Aortic banding (AB) in the mouse was established in our laboratory since 2010. This model provided solid evidence of myocardial hypertrophy and was related with low mortality [28]; we, therefore, used this model in the study. AB was performed on mice aged 8–10 weeks (with body weights of 24–27 g) to induce cardiac hypertrophy models. After being anesthetized with pentobarbital sodium (50 mg/kg, i.p., Sigma) and connected to a rodent ventilator, the transverse aorta was isolated by blunt dissection at the second intercostal space. AB was performed by tying the thoracic aorta against a 26G needle (for body weights of 26–27 g)/27G needle (for body weights of 24–25 g) with a 7-0 silk suture. Before closing the thoracic cavity, the needle was promptly removed to induce pressure overload cardiac hypertrophy, and adequate constriction of the aorta was determined by Doppler analysis. A similar procedure was performed in sham-operated animals except for aortic constriction. 5Z-7-oxozeaenol (a highly selective inhibitor of TAK1) suspension was freshly prepared and administered by intraperitoneal injection (5 mg/kg/72 h) for 4 weeks. The control group was given the same volume of dimethyl sulfoxide (DMSO) solution.
Echocardiography measurements
At 4 weeks post-AB, left ventricular function was determined in the mice with the Mylab30CV (ESAOTE) ultrasound system equipped with a 15-MHz probe. Mice were anesthetized by 1.5–2 % isoflurane, parasternal short-axis views at the mid-papillary muscle level were obtained to measure left ventricular end-diastolic and systolic diameter (LVEDd and LVESd), left ventricular fractional shortening \(\left( {{\text{FS,\%}}} \right) { = }\left[ {\left( {{\text{LVEDd}}\text{ - }{\text{LVESd}}} \right) / {\text{LVEDd}}} \right]\, \times\, 100\, \%\) and left ventricular ejection fraction \(\left( {{\text{EF}},\% } \right) = \left[ {\left( {{\text{LVEDV - LVESV}}} \right)/{\text{LVEDV}}} \right] \times100\,\%\), in which LVEDV is the left ventricular end-diastolic volume and LVESV is the left ventricular end-systolic volume. The left ventricle dimensions were obtained from at least three beats and then averaged.
Histological analysis
The mice were deep anesthetized with pentobarbital sodium (50 mg/kg, i.p.) at 4 weeks after AB or sham surgery and then hearts were harvested. All experimental procedures were conducted according the guidelines of the Animal Care and Use Committee of Xinhua Hospital. The tissues were fixed in 10 % formalin, embedded in paraffin and sectioned at 5 microns. Left ventricular sections were stained with hematoxylin and eosin (H&E) for histopathology or with picrosirius red (PSR) to quantify cardiac fibrosis. Myocyte cross-sectional areas were assessed on FITC-conjugated wheat germ agglutinin (WGA; Invitrogen) stained sections using a quantitative digital image analysis system (Image-Pro Plus 6.0). Approximately 100 myocytes in transversely sectioned left ventricular tissue from at least 5 different mouse samples were outlined in each group. More than 40 PSR-stained sections (magnification 20×) from the left ventricle were randomly selected to quantify LV collagen volume.
Culture of NRCMs and adenovirus generation
The direct prohypertrophic effect of Ang II has been extensively characterized in cardiomyocytes [15, 19]. So we exposed cultured neonatal rat cardiomyocytes to 1 μM Ang II for 48 h to induced hypertrophic responses in cardiomyocytes in the present study. Neonatal rat cardiomyocytes (NRVMs) were isolated from 1- to 2-day-old Sprague–Dawley rats as previously described [35]. After isolation, NRVMs were plated onto gelatin-coated culture dishes containing DMEM/F12 medium with 20 % fetal calf serum and penicillin/streptomycin. After 24 h, NRVMs were maintained in serum-free DMEM/F12 for 12 h, followed by stimulation with angiotensin II (Ang II, 1 μmol/L) or PBS for another 24 or 48 h. Replication-defective adenoviral vectors harboring region of the rat Dusp14 gene were generated to overexpress Dusp14. The rat shDusp14 construct was obtained from SABiosciences (KR48023G) to knockdown Dusp14 expression. AdGFP and AdshRNA were used as respective controls. NCRMs were infected with adenovirus at a multiplicity of infection (MOI) of 10 viral particles per cell for 24 h.
Immunostaining assay
After abovementioned treatments, NRCMs were fixed with 3.7 % formaldehyde for 15 min, permeabilized with 0.1 % Triton X-100 in PBS for 40 min, blocked with 3 % BSA for 30 min at room temperature. Cells were incubated with a primary antibody against α-actinin, subsequently by a fluorescent secondary antibody (Sigma). Stained cells were analyzed by fluorescence microscope, and surface areas were measured using Image-Pro Plus 6.0 software.
Immunoprecipitation
For co-immunoprecipitation experiments, cultured HEK293T cells were transfected with the appropriate plasmids, harvested using IP buffer [20 mM Tris–HCl (pH 7.5), 150 mM NaCl, 1 mM EDTA, 0.5 % NP-40 and protease inhibitor cocktail (Roche)]. Cell suspension was centrifuged at 13,000g for 15 min. After centrifugation, the lysates were incubated with Anti-HA or Anti-Flag antibody and 20 μl protein G-agarose beads at 4 °C overnight. Then the beads were washed twice with a washing buffer containing 20 mM Tris pH7.5, 500 mM NaCl, 1 mM EDTA, 0.5 % NP40, followed by two washes with a washing buffer containing 20 mM Tris pH7.5, 150 mM NaCl, 1 mM EDTA, 0.5 % NP40. Finally the immune complex was eluted from agarose beads and were analyzed by Western blot.
Plasmid constructs
Flag-tagged Dusp14 plasmid was constructed by subcloning mouse Dusp14 cDNA into the vector psi-Flag. Mammalian expression plasmids for HA-tagged TAK1, HA-tagged TAB1 were subcloned into the vector pcDNA5-HA by standard molecular biology techniques.
Quantitative real-time PCR and Western blotting
Total RNA from left ventricular tissue and cultured cardiac myocytes was extracted using TRIZol reagent (Invitrogen), as described by the manufacturer, and cDNA was synthesized from the RNA using the Transcriptor First-Strand cDNA Synthesis Kit (Roche). Quantitative real-time PCR was performed using SYBR Green (Roche). Total proteins from ventricular tissue and cultured cardiac myocytes were isolated, respectively. The protein concentration was confirmed using the Pierce BCA Protein Assay kit (Pierce). The proteins were subjected to SDS–polyacrylamide gel electrophoresis and transferred onto a polyvinylidene fluoride membrane (Millipore). After blocking, membranes were incubated with following primary antibodies including antibodies against phosphor-TAK1, TAK1, phospho-MEK1/2, MEK1/2, phospho-ERK1/2, ERK1/2, phospho-P38, P38, phospho-JNK1/2 and JNK1/2, ANP, β-MHC, Dusp14, GAPDH, overnight at 4 °C followed by incubation with secondary antibodies, protein signals were revealed by the Bio-Rad ChemiDoc™ XRS+ (Bio-Rad).
Human heart samples
Samples of failing human hearts were obtained from patients with dilated cardiomyopathy (DCM) undergoing cardiac transplantation for end-stage cardiac heart failure (n = 5). Control samples were collected from prospective multiorgan donors who died in accidents and whose hearts were unsuitable for transplantation for noncardiac reasons (n = 5). All studies are conformed to the principles of the Declaration of Helsinki and the ethical regulations of Xinhua Hospital, Shanghai Jiao Tong University School of Medicine Review Board, Shanghai, China.
Statistical analysis
Data in the text and figures are presented as mean ± SD. Statistical analysis was performed with the SPSS software (Statistical Package for the Social Sciences) 13.0. Comparisons between groups were analyzed by unpaired, two-tailed Student t test (2 groups) or by one-way ANOVA followed by post hoc Tukey test for multi-group comparisons. P values <0.05 were considered as statistically significant.
Results
Myocardial Dusp14 expression under physiological and pathological conditions
To assess the potential role of Dusp14 in response to hypertrophic stress, we analyzed Dusp14 expression in failing human hearts and in AB mouse hearts. Dusp14 protein levels were significantly decreased in failing human hearts compared with normal donor hearts (Fig. 1a, b). Myocardial Dusp14 expression was progressively downregulated in AB mice at 4 weeks and at 8 weeks compared with the sham controls (Fig. 1c). In addition, the expression levels of cardiac hypertrophy markers including ANP, and β-MHC were significantly upregulated post-AB (Fig. 1c, d). In vitro studies, Dusp14 expression was significantly downregulated in angiotensin II (Ang II, 1 μmol/L)-treated NRCMs at 24 and 48 h in a time-dependent manner (Fig. 1e). Similarly, the expression levels of hypertrophic markers were upregulated in NRCMs following Ang II stimulation in a time-dependent manner (Fig. 1e, f).
Myocardial Dusp14 expression is decreased under pathological conditions. a Western blots and b quantification for myocardial Dusp14, ANP and β-MHC expression in normal donor hearts (n = 5) and dilated cardiomyopathy hearts (n = 5, *P < 0.05 vs donor hearts). c Western blots and d quantification for Dusp14, ANP and β-MHC expression in mouse myocardium from AB or sham-operated controls for the indicated time (n = 5 per group, *P < 0.05 vs sham). e Western blots and f quantification for Dusp14, ANP and β-MHC expression in cultured neonatal rat cardiomyocytes following Ang II(1 μmol/L) stimulation for 24 and 48 h (n = 4 samples per group, *P < 0.05 vs PBS). Data are mean ± SD
Aggravated myocardial hypertrophy in Dusp14−/− kockout mice post-AB
Dusp14−/− knockout mice were generated to explore the in vivo effects of Dusp14 in AB model (Fig. 2a). This mouse line was viable, fertile, and did not display apparent phenotypic abnormalities under basal conditions. Dusp14−/− knockout mice exhibited more pronounced cardiac hypertrophy at 4 weeks post-AB, as shown by increased heart weight/bodyweight (HW/BW) ratio, heart weight/tibia length (HW/TL) ratio, larger gross heart size, cross-sectional area of cardiomyocytes compared to their WT littermates. Lung weight/bodyweight (LW/BW) ratio was also increased in Dusp14−/− knockout mice (Fig. 2b–d). Consistently, real-time PCR analysis revealed that AB-induced upregulation of molecular cardiac hypertrophy markers was further enhanced in Dusp14−/− knockout mice (Fig. 2e). In addition, the extent of AB-induced cardiac fibrosis was significantly augmented in Dusp14−/− knockout mice, in that the collagen accumulation both in the interstitial and perivascular spaces measured in picrosirius red-stained sections were more pronounced in Dusp14−/− knockout hearts than in WT hearts at 4 weeks post-AB (Fig. 2f). Figure 2g, h shows that collagen volume and the expression of the fibrotic markers including collagen I, collagen III and connective tissue growth factor (CTGF) were significantly higher in Dusp14−/− knockout mice than in WT mice at 4 weeks post-AB. Echocardiography examination demonstrated significant larger left ventricular (LV) chamber dimension, lower LV fractional shortening (FS) and LV ejection fraction (EF) in Dusp14−/− knockout mice than in WT mice at 4 weeks post-AB (Fig. 2i).
Dusp14 deficiency accelerates pressure overload-induced cardiac hypertrophy. a Generation of Dusp14 knockout mice. A1 Schematic of the Dusp14 genetic locus and target site of single guide RNA (sgRNA), A2 Representative results of the T7E1 assay from pups following microinjection, A3 Representative results of the DNA sequencing from animals (A2) with cleavage products, A4 Agarose gel photograph illustrating genotyping results of PCR products [wild-type mice (+/+), heterozygous mice (+/−) and homozygous mice (−/−)], A5 Representative Western blots of Dusp14 expression in heart tissues from Dusp14−/− mice and WT mice. b Quantification results for the ratios of HW/BW, HW/TL and LW/BW in Dusp14+/+ or Dusp14−/− mice subjected or not to AB (n = 12–13 per group). c Representative images of the HE staining and WGA staining of Dusp14+/+ or Dusp14−/− mice at 4 weeks after sham and AB operation (n = 5 per group, scale bar 20 μm for lower HE staining and WGA staining). d Quantification results of the myocyte cross-sectional area (n ≥ 100 cells per group). e Transcript levels of fetal cardiac gene (ANP, BNP, β-MHC) were analyzed by real-time PCR (n = 4 per group). f Histological sections from hearts subjected or not to AB taken 4 weeks were stained with PSR to detect fibrosis (n = 5 per group scale bar 50 μm). g Quantification results of LV collagen volume (n ≥ 40 fields per group). h Levels of cardiac fibrosis markers (Collagen I, Collagen III, CTGF) were quantified by real-time PCR (n = 4 per group). i Echocardiographic assessment of left ventricular end-diastolic and systolic diameter (LVEDd and LVESd), fractional shortening (FS) and ejection fraction (EF) in Dusp14+/+ or Dusp14−/− mice at 4 weeks after sham and AB operation (n = 7–8 per group). (*P < 0.05 vs Dusp14+/+/sham, # P < 0.05 vs Dusp14 +/+/AB). Data are mean ± SD
Transgenic cardiac Dusp14 overexpression attenuates cardiac hypertrophy post-AB
To determine whether overexpression of Dusp14 would reverse AB-induced cardiac hypertrophic responses, we generated a transgenic (TG) mouse model with specific cardiac Dusp14 overexpression using the α-MHC promoter (Fig. 3a). Four independent lines of transgenic mice were established and verified by Western blot analysis (Fig. 3b, c). At baseline, all Dusp14 TG mice developed normally with no obvious phenotype. TG4 line mice which expressed the highest levels of Dusp14 and their CAG-CAT-Dusp14/MHC-MerCreMer littermates without tamoxifen administration (CDMC) were used in the main study. As expected, in comparison with CDMC mice, the TG mice exhibited less cardiac hypertrophic responses at 4 weeks post-AB as shown by lower heart HW/BW, HW/TL and LW/BW, smaller heart and cardiomyocytes size (Fig. 3d–f). Concordantly, reactivations of myocardial fetal genes associated with cardiac hypertrophy and failure such as ANP, BNP and β-MHC were significantly reduced in TG mice compared to CDMC mice (Fig. 3g). Picrosirius red staining on heart sections also revealed less fibrosis in both interstitial and perivascular spaces in TG mice compared with CDMC mice at 4 weeks post-AB (Fig. 3h–j). Echocardiographic measurements showed LV chamber dimension increase at diastole and systole phases in TG mice was less significant as in the case in CDMC mice at 4 weeks post-AB (Fig. 3k). Likewise, reduction of FS and EF were also less in TG mice compared to CDMC mice (Fig. 3k).
Cardiac-specific overexpression of DUSP14 attenuates cardiac hypertrophy post-AB. a Schematic representation of the construct used to generate Dusp14-transgenic (TG) mouse lines. b Representative Western blots and c quantitative results of Dusp14 in the hearts of 4 Dusp14 TG lines and their CAG-CAT-Dusp14/MHC-MerCreMer littermates without tamoxifen administration (CDMC) (n = 3 independent experiments). d HW/BW, HW/TL and LW/BW ratios of CDMC or Dusp14 TG mice after AB or sham operation (n = 12–13 per group). e Representative images of the HE staining and WGA staining of the indicated groups (n = 5 per group, scale bar 20 μm for lower HE staining and WGA staining). f Quantification of cell surface area (n ≥ 100 cells per group). g The expression levels of hypertrophic markers (ANP, BNP, β-MHC) in hearts of CDMC or Dusp14TG mice were quantified by real-time PCR (n = 4 per group). h Heart sections of CDMC or Dusp14TG mice 4 weeks after AB or sham operation were stained with PSR to detect fibrosis (n = 5 per group, scale bar 50 μm). i Relative fibrosis areas in sections of LV tissue (n ≥ 40 fields per group). j Collagen I, Collagen III and CTGF mRNA expressions at 4 weeks, assessed by real-time PCR (n = 4 per group). k Echocardiographic assessment of left ventricular end-diastolic and systolic diameter (LVEDd and LVESd), fractional shortening (FS) and ejection fraction (EF) in CDMC or Dusp14TG mice from 4 weeks after AB surgery (n = 7–8 per group). (*P < 0.05 vs CDMC/sham, # P < 0.05 vs CDMC/AB). Data are mean ± SD
Dusp14 overexpression inhibits Ang II-induced cardiomyocyte hypertrophy in vitro
Next, to further investigate the functional contribution of Dusp14 to cardiac hypertrophy, we performed gain- and loss-of-function studies in NRCMs. NRCMs were transfected with either AdshDusp14 to knockdown Dusp14 or AdDusp14 to overexpress Dusp14. AdshRNA or AdGFP was used as a control (Fig. 4a, b). Under basal conditions (PBS), NRCMs size or morphology transfected with AdshDusp14 or AdDusp14 were macroscopically indistinguishable from their respective controls (Fig. 4c–e). After stimulation with Ang II for 48 h, cell surface area was significantly larger in NRCMs transfected with AdshDusp14 compared to NRCMs treated with AdshRNA (Fig. 4c, d). In line with this finding, we also observed significantly upregulated mRNA expression of hypertrophy markers (ANP, BNP and β-MHC) in AdshDusp14-transfected NRCMs (Fig. 4d). In contrast, AdDusp14-infected NRCMs were refractory to Ang II-induced hypertrophic responses, the latter was also accompanied by lower expression of hypertrophy markers in comparison with control NRCMs (Fig. 4e). These in vitro results suggested that Dusp14 overexpression could attenuate Ang II-induced hypertrophic responses in cardiomyocytes.
Dusp14 blocks the Ang II-induced hypertrophy of neonatal rat cardiomyocytes (NRCMs). a Western blot analysis of Dusp14 expression in cardiomyocytes after infection with AdshDusp14, Ad Dusp14, as well their respective controls (AdshRNA and AdGFP). b Quantitative results of Dusp14 expression in the indicated groups. c Representative images of cardiomyocytes infected with adenoviral vectors (AdGFP) or Dusp14 (AdDusp14) and AdshRNA or AdshDusp14, and treated with Ang II or control (PBS) for 48 h (green a-actinin, blue nuclear, scale bar 20 μm). d Quantification of the cell surface area of cardiomyocytes infected with AdshDusp14 or AdshRNA in response to Ang II (n ≥ 50 cells per group), and real-time PCR analysis of ANP, BNP and β-MHC as markers of hypertrophy in Dusp14 knockdown cells subjected to PBS or Ang II for 48 h. e Quantification of the cell surface area of cardiomyocytes infected with AdDusp14 or AdGFP in response to Ang II (n ≥ 50 cells per group), and real-time PCR analysis of ANP, BNP and β-MHC as markers of hypertrophy in Dusp14 overexpressed cells subjected to PBS or Ang II for 48 h. (n = 4 samples per group, *P < 0.05 vs AdshRNA or AdGFP/PBS, # P < 0.05 vs AdshRNA or AdGFP/Ang II). Data are mean ± SD
Dusp14 blocks TAK1-P38MAPK/-JNK1/2 signaling pathway
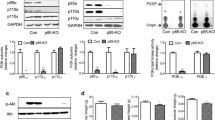
Above experiments suggested protective role of Dusp14 against AB or Ang II-induced myocardial or cardiomyocytes hypertrophy. We next sought to determine candidate signaling molecules related to the antihypertrophic effects of Dusp14. Since Dusp14 mainly regulates MAPK signaling pathways, we analyzed the expression and activity of MAPK cascade components (i.e., ERK1/2, P38 and JNK1/2), which are implicated in pathological hypertrophy [29]. Whereas total ERK1/2, P38 and JNK1/2 protein levels were not altered after AB, phosphorylated P38 and JNK1/2 levels, but not ERK1/2, were significantly upregulated in Dusp14−/− knockout mice as compared with WT controls at 4 weeks post-AB (Fig. 5a). Inversely, AB induced less upregulation of phosphor-P38MAPK and phosphor-JNK1/2 in hearts from TG mice overexpressing Dusp14 compared with hearts from CDMCs at 4 weeks post-AB (Fig. 5b). Considering the activation of P38MAPK and JNK1/2 is inhibited by Dusp14, thus, Dusp14 may affect upstream of both P38MAPK and JNK1/2. In fact, TAK1, an upstream regulator of P38 and JNK1/2, was significantly activated in the AB-induced hypertrophic hearts of Dusp14−/− knockout mice, while phosphorylated TAK1 was remarkably reduced in hearts of TG mice overexpressing Dusp14 post-AB (Fig. 6a, b). Next, we sought to determine that whether Dusp14 could directly interact with TAK1. Although, Dusp14 could indirectly affect TAK1 activity via dephosphorylation of TAB1 at S438 in T cells [37], we did not observe a significant difference in phosphorylated TAB1 expression between Dusp14−/− knockout mice and WT controls or between Dusp14 TG mice and CDMC mice under pressure overload conditions. We transfected Flag-tagged Dusp14 and HA-tagged TAK1/HA-tagged TAB1 into HEK293T cells and then performed co-immunoprecipitation (IP) experiments. Our results showed that Dusp14 precipitated with TAK1 and vice versa (Fig. 6e). Since NFκB is downstream of the TAK1 [39], we also investigated the phosphorylated and total NFκB levels between Dusp14−/− knockout mice and WT controls or between Dusp14 TG mice and CDMC mice after AB or sham operations. The expression levels of phosphorylated NFκB was not different between Dusp14−/− knockout mice and WT controls or between Dusp14 TG mice and CDMC mice after AB. Similarly, Dusp14 knockdown resulted in hyper-phosphorylation of P38MAPK, JNK1/2 and TAK1 in Ang II-stimulated NRCMs (Figs. 5c, 6c). In accordance, P38MAPK, JNK1/2 and TAK1 were remarkably hypophosphorylated in Ang II-stimulated NRCMs overexpressing Dusp14 (Figs. 5d, 6d). Taken together, these data indicate that Dusp14 may physically interact with TAK1 and negatively regulate TAK1-dependent P38MAPK and JNK1/2 signaling in the maladaptive hypertrophic responses.
Dusp14 inhibits P38MAPK and JNK1/2 signaling pathway in vivo and in vitro. a, b Representative Western blots and quantitative results depicting the phosphorylation and total protein levels of ERK1/2, JNK1/2, P38, MEK1/2 in the indicated groups 4 weeks after AB or sham surgery. Top representative blots. Bottom Quantification of data. (n = 5 per group, *P < 0.05 vs Dusp14+/+ or CDMC/sham, # P < 0.05 vs Dusp14+/+ or CDMC/AB). c, d NRVMs were transfected with the indicated plasmids and treated with Ang II for 60 min. Phosphorylated ERK1/2 (p-ERK1/2), p-JNK1/2, p-P38, p-MEK1/2 and total-ERK (t-ERK), t-JNK1/2, t-P38, t-MEK1/2 were analyzed by Western blot. Top representative blots. Bottom Quantification of data. (n = 4 samples per group, *P < 0.05 vs AdshRNA or AdGFP/PBS, # P < 0.05 vs AdshRNA or AdGFP/Ang II). Data are mean ± SD
Dusp14 directly interacts with and inhibits TAK1 signaling involved in hypertrophy. a, b Representative Western blots and quantitative results of the TAK1 protein and its phosphorylation levels in the hearts of Dusp14+/+ or Dusp14−/− and CDMC or Dusp14TG mice subjected to AB or sham surgery for the indicated period of time. Top representative blots. Bottom Quantification of data. (n = 5 per group, *P < 0.05 vs Dusp14+/+ or CDMC/sham, # P < 0.05 vs Dusp14+/+ or CDMC/AB). c, d Western blot detecting phosphorylation and total protein levels of TAK1 in NRVMs infection with the indicated plasmids followed by treatment with PBS or Ang II for 60 min, and quantitative analysis of the results. Top representative blots. Bottom quantification of data. e Left immunoblot analysis was performed with a Flag or HA antibody after co-IP of Dusp14 from HEK293T whole cell lysates using a Flag antibody. Right immunoblot analysis were performed with a Flag or HA antibody after co-IP of TAK1 or TAB1 from HEK293T whole cell lysates using an HA antibody. (n = 4 samples per group,*P < 0.05 vs AdshRNA or AdGFP/PBS, # P < 0.05 vs AdshRNA or AdGFP/Ang II). Data are mean ± SD
Inhibition of TAK1-P38MAPK/-JNK1/2 signaling attenuates cardiac hypertrophic responses in Dusp14−/− knockout mice post-pressure-overload stress
To further determine whether TAK1-P38MAPK/-JNK1/2 signaling pathways is required for Dusp14-mediated antihypertrophic effects post-AB, we treated Dusp14−/− knockout mice and WT mice with TAK1 inhibitor 5Z-7-ox or DMSO solution following AB. As expected, Western blot analysis revealed significantly lower TAK1 phosphorylation levels in animals receiving 5Z-7-ox (5 mg/kg/72, this dose was selected based on our pilot experiments) compared with those received DMSO (Fig. 7a, b). Consistent with this, AB-induced P38MAPK and JNK1/2 activation was also markedly suppressed by TAK1 inhibition (Fig. 7a, b). As shown in Fig. 7c–g, 5Z-7ox treatment protects against AB-induced cardiac hypertrophy and fibrosis to a similar degree as the cardiac-specific Dusp14 overexpression compared with DMSO solution treatment in Dusp14−/− knockout mice. 5Z-7-ox treatment also ameliorated AB-induced cardiac dysfunction in Dusp14−/− knockout mice as shown by less decrease in FS, EF and less LV chamber dimension enlargement (Fig. 7h). These findings indicate that enhanced activation of TAK1-P38MAPK/-JNK1/2 signaling caused by absence of Dusp14 expression significantly contributes to maladaptive response to pressure overload (Fig. 8) and pharmacological inhibition of these pathways may effectively blunt AB-induced pathological hypertrophy and dysfunction.
Ablation of TAK1-P38MAPK and -JNK1/2 signaling prevents pathological cardiac remodeling and dysfunction. a Representative Western blots and b quantitative results of total and phospho-TAK1-dependent signaling pathway protein levels in the hearts from 5Z-7-oxozeaenol-treated or DMSO-treated Dusp14−/− mice 4 weeks after AB surgery (n = 5 per group). c HW/BW, HW/TL and LW/BW ratios of the indicated groups (n = 11 per group). d, e Heart tissue sections in the indicated groups stained with HE or stained with PSR to assess cardiac hypertrophy or fibrosis, respectively (n = 5 per group, scale bar 20 μm for HE staining; scale bar 50 μm for PSR staining). f, g Quantitative analysis of cell-sectional area (n ≥ 100 cells per group) and LV collagen volume (n ≥ 40 fields per group). h Assessment of left ventricular end-diastolic and systolic diameter (LVEDd and LVESd), fractional shortening (FS) and ejection fraction (EF) as measured by echocardiography in mice of the indicated genotypes after AB treatment for 4 weeks (n = 7–8 per group). (*P < 0.05 vs WT/AB/DMSO; # P < 0.05 vs KO/AB/DMSO; n.s. indicates no significant difference). Data are mean ± SD
Dusp14-mediated activation of TAK1-P38MAPK/-JNK1/2 signaling underlies the pathological remodeling induced by pressure overload. Based on the present study, we propose that hypertrophic stimulus results in reduced Dusp14 expression in the heart, thereby triggering the hyperactivation of TAK1. The activated TAK1 induces the activation of the MKK3/6-P38 and MKK4/7-JNK1/2 signaling cascades which then likely induce cardiac pathology
Discussion
Dusps are large and heterogeneous group of phosphatases, comprising typical Dusps and atypical Dusps which could dephosphorylate both serine/threonine and tyrosine residues within the activation loop known as major regulators of MAPK signalling [26]. Typically, MAPK cascades are triple kinase pathways in which a MAPK kinase activates a MAPK kinase which in turn activates a terminal MAPK (ERK1/2, P38, JNK1/2) via serial phosphorylation to allow for signal amplification, modulation, and specificity [29]. Therefore, once the negative regulatory mechanisms derived from Dusps were lost, this canonical activation cascade would be unrestrained and detrimental thereby resulting in cardiac dysfunction and hypertrophy as long as a pathological stimulus is present. In the present study, we identified Dusp14, a member of atypical Dusps, as a novel and negative regulator of pathological cardiac hypertrophy using both gain- and loss-of-function genetic strategies. From a mechanistic perspective, we found Dusp14 might have interacted directly with and dephosphorylated TAK1 and prevented TAK1-dependent P38MAPK and JNK1/2 signaling (Fig. 8). To our best knowledge, the present study is the first experimental report focusing on the antihypertrophic role of Dusp14 based on the genetic mouse models.
Our results showed that Dusp14 is normally expressed in the adult myocardium; however, it is prominently decreased under pathological conditions. More specifically, Dusp14 expression was downregulated in human failing heart and in AB-induced hypertrophic heart. Over time, more severe diminution was observed in AB mice hearts or in Ang II-treated NRCMs, respectively. Data presented here suggest that Dusp14 might be implicated in the development of cardiac hypertrophy and the progression of heart failure which is reminiscent of other endogenous repressors of pathological hypertrophy previously reported [1, 3, 15]. Their expressions are often decreased upon hypertrophic signaling, which then induce maladaptive cardiac hypertrophy. Conversely, compensation for their loss could repress the maladaptive remodeling. Indeed, Dusp14−/− knockout mice displayed not only greater hypertrophic responses but also severer cardiac dysfunction post-AB, whereas, Dusp14 overexpression significantly attenuated AB-induced cardiac hypertrophy and dysfunction. Consistent with the in vivo data, we also observed further aggravated increase in cell size and fetal gene activation in Dusp14 knowdown NRVMs post-Ang II stimulation while Dusp14 transfection in NRVMs significantly attenuated Ang II-stimulated responses. Altogether, these results indicate that Dusp14 may function as a negative regulator for pathological cardiac remodeling under stress condition. Importantly, Dusp14 may not be necessary for normal cardiac development but gain functional importance during cardiac remodeling induced by pathological hypertrophic stimulation, which is supported by the absence of heart phenotypic abnormalities in Dusp14−/− knockout mice and in TG mice overexpressing Dusp14. With the evolution of increasingly efficient gene transfer technology, cardiac gene therapy has emerged as a promising treatment option for treating heart failure in addition to mechanical and pharmacological therapies [11], although safety and efficacy remains to be evaluated in the coming years. Based on our results showing that restoration of Dusp14 expression by genetic strategy improved cardiac function in mice with heart failure, Dusp14 may be a potential target that are amenable to genetic manipulations for the treatment of heart failure in the future. However, it is clear there is a long way to go before gene therapy for heart failure becomes a clinical reality, in fact, the CUPID-2b trial, the first clinically tested gene therapy and a placebo-controlled phase 2b trial enrolled several hundred participants, in that AAV1/SERCA2a was intracoronary delivered to heart failure patients failed to make a significant difference in the primary end point reflecting recurrent HF events between placebo and gene therapy group [10], despite earlier promise in a small dose-finding study. It is to note that present study did not supply evidence elucidating the exact mechanisms responsible for regulating Dusp14 expression following hypertrophic stimuli. Normally, as a negative-feedback mechanism, MAPKs could enhance expression of most Dusps [26]. Marie-Claire and collaborators have shown that the activation of ERK promotes expression of Dusp14 in mice striatum [22]. It is thus possible that undefined activated signaling cascades in response to hypertrophic stimulation might cause degradation of Dusp14 to counteract this negative regulation. However, further experiments are required to explore the underlying cause on Dusp14 expression alteration under cardiac hypertrophy conditions.
TAK1 was initially identified as a member of the MAPKKK family in response to transforming growth factor-β (TGFβ) [36], which is prominently expressed in cardiomyocytes [24]. Upon stimulation, TAK1 could phosphorylate and activate the MAPKKs (MKK3/6, MKK4/7), to transduce the signal to P38MAPK and JNK1/2 [31]. Growing evidences have shown a crucial role of the TAK1 signaling in promoting maladaptive cardiac hypertrophy [18, 38]. Subsequent studies further revealed TAK1-P38MAPK pathway [2, 16] and TAK1-JNK1/2 signaling [27, 34] are strongly implicated in cardiac pathological response to pathological stress. Till now, the exact role of JNK and p38 activation on hypertrophy remains an issue of debate. Some authors demonstrated that JNK and p38 activation does not promote hypertrophy or even play antihypertrophic roles [4, 20]; while there are also reports which imply a positive role for JNK and p38 in the hypertrophic process [25, 30]. In this study, we showed that loss of Dusp14 caused a prolonged activation of P38MAPK and JNK1/2 in hearts post-AB or Ang II-stimulated NRCMs whereas activation of ERK1/2 was not affected; while dephospho-P38MAPK and dephospho-JNK1/2 were dramatically increased in the situation of Dusp14 overexpression. Of interest, we found the phosphorylation of TAK1, a signaling molecule upstream of both P38MAPK and JNK1/2, was regulated by Dusp14. Moreover, we further provided evidence that Dusp14 physically interacts with TAK1. Therefore, it seems that unlike typical Dusps [26], Dusp14 may not directly dephosphorylate P38MAPK and JNK1/2 but directly regulate their upstream kinase in cardiomyocytes. Additionally, our results demonstrated that P38 but not ERK1/2 activation was modulated by Dusp14 in heart, which is in disagreement with the previous reports demonstrating that Dusp14 increased propensity towards ERK1/2 in nonmyocytes [23]. This phenomenon might be partly explained by the fact that Dusp14 might target its substrate(s) in a divergent way up specific cell types and/or up specific stimuli. Taken together, we speculate that activation of TAK1-dependent P38MAPK and JNK1/2 signaling pathway attributable to Dusp14 loss might play a key role on the cardiac pathology following hypertrophic stimulation. Importantly, proof for this hypothesis came from the use of 5Z-7-ox in Dusp14−/− knockout mice, which prevented the pathological development. 5Z-7-oxozeaenol is an inhibitor of TAK1, ERK2, MKK7, MEK1, and also has anti-inflammatory effects, which might affect cardiac hypertrophy. Although, we cannot completely rule out that 5Z-7-oxozeaenol treatment in Dusp14−/− knockout mice at the selected dosing regimen also inhibited ERK2, MKK7, and MEK1, thereby contributing to antihypertrophic response, several recent studies have shown that 5Z-7-oxozeaenol mainly and effectively reduced the phosphorylation of TAK1 in cardiomyocytes or in colon cancer cells [18, 32], thus, the antihypertrophic effects of 5Z-7-oxozeaenol treatment in Dusp14−/− knockout mice might mainly depend on inhibition of TAK1. Therefore, these results indicated that the antihypertrophic effects of Dusp14 are mainly mediated by inhibiting TAK1-P38MAPK/-JNK1/2 signaling.
In summary, present results provide insights into Dusp14-related hypertrophic mechanisms in that enhanced activation of the TAK1-dependent P38MAPK and JNK1/2 signaling pathways caused by downregulated Dusp14 expression in the setting of hypertrophic stimuli might be involved in the pathogenesis of cardiac hypertrophy. Dusp14 restoration could attenuate hypertrophic remodeling and cardiac dysfunction post-chronic stress via inactivation of TAK1-P38MAPK/-JNK1/2 signaling pathway. Dusp14 might thus be a promising therapeutic target for preventing and treating the maladaptive cardiac hypertrophy.
References
Antos CL, McKinsey TA, Frey N, Kutschke W, McAnally J, Shelton JM, Richardson JA, Hill JA, Olson EN (2002) Activated glycogen synthase-3β suppresses cardiac hypertrophy in vivo. Proc Natl Acad Sci 99:907–912. doi:10.1073/pnas.231619298
Biesemann N, Mendler L, Kostin S, Wietelmann A, Borchardt T, Braun T (2015) Myostatin induces interstitial fibrosis in the heart via TAK1 and p38. Cell Tissue Res. doi:10.1007/s00441-015-2139-2
Bisserier M, Berthouze-Duquesnes M, Breckler M, Tortosa F, Fazal L, de Regibus A, Laurent AC, Varin A, Lucas A, Branchereau M, Marck P, Schickel JN, Delomenie C, Cazorla O, Soulas-Sprauel P, Crozatier B, Morel E, Heymes C, Lezoualc’h F (2015) Carabin protects against cardiac hypertrophy by blocking calcineurin, Ras, and Ca2+/calmodulin-dependent protein kinase II signaling. Circulation 131:390–400. doi:10.1161/CIRCULATIONAHA.114.010686 (discussion 400)
Braz JC, Bueno OF, Liang Q, Wilkins BJ, Dai YS, Parsons S, Braunwart J, Glascock BJ, Klevitsky R, Kimball TF, Hewett TE, Molkentin JD (2003) Targeted inhibition of p38 MAPK promotes hypertrophic cardiomyopathy through upregulation of calcineurin-NFAT signaling. J Clin Invest 111:1475–1486. doi:10.1172/JCI17295
Bui AL, Horwich TB, Fonarow GC (2011) Epidemiology and risk profile of heart failure. Nat Rev Cardiol 8:30–41. doi:10.1038/nrcardio.2010.165
de Simone G, Gottdiener JS, Chinali M, Maurer MS (2008) Left ventricular mass predicts heart failure not related to previous myocardial infarction: the Cardiovascular Health Study. Eur Heart J 29:741–747. doi:10.1093/eurheartj/ehm605
Drazner MH (2011) The progression of hypertensive heart disease. Circulation 123:327–334. doi:10.1161/CIRCULATIONAHA.108.845792
Drazner MH, Rame JE, Marino EK, Gottdiener JS, Kitzman DW, Gardin JM, Manolio TA, Dries DL, Siscovick DS (2004) Increased left ventricular mass is a risk factor for the development of a depressed left ventricular ejection fraction within five years: the Cardiovascular Health Study. J Am Coll Cardiol 43:2207–2215. doi:10.1016/j.jacc.2003.11.064
Garrington TP, Johnson GL (1999) Organization and regulation of mitogen-activated protein kinase signaling pathways. Curr Opin Cell Biol 11:211–218. doi:10.1016/S0955-0674(99)80028-3
Greenberg B (2015) CUPID 2: a phase 2b trial investigating the efficacy and safety of the intracoronary administration of AAV1/SERCA2a in patients with advanced heart failure. 917—Hot Line V—Heart Failure, London
Hajjar RJ (2013) Potential of gene therapy as a treatment for heart failure. J Clin Invest 123:53–61. doi:10.1172/JCI62837
Heineke J, Molkentin JD (2006) Regulation of cardiac hypertrophy by intracellular signalling pathways. Nat Rev Mol Cell Biol 7:589–600. doi:10.1038/nrm1983
Hill JA, Olson EN (2008) Cardiac plasticity. N Engl J Med 358:1370–1380. doi:10.1056/NEJMra072139
Jeffrey KL, Camps M, Rommel C, Mackay CR (2007) Targeting dual-specificity phosphatases: manipulating MAP kinase signalling and immune responses. Nat Rev Drug Discov 6:391–403. doi:10.1038/nrd2289
Jiang DS, Wei X, Zhang XF, Liu Y, Zhang Y, Chen K, Gao L, Zhou H, Zhu XH, Liu PP, Bond Lau W, Ma X, Zou Y, Zhang XD, Fan GC, Li H (2014) IRF8 suppresses pathological cardiac remodelling by inhibiting calcineurin signalling. Nat Commun 5:3303. doi:10.1038/ncomms4303
Kinugawa K, Jeong MY, Bristow MR, Long CS (2005) Thyroid hormone induces cardiac myocyte hypertrophy in a thyroid hormone receptor α1-specific manner that requires TAK1 and p38 mitogen-activated protein kinase. Mol Endocrinol 19:1618–1628. doi:10.1210/me.2004-0503
Klinger S, Poussin C, Debril MB, Dolci W, Halban PA, Thorens B (2008) Increasing GLP-1-induced β-cell proliferation by silencing the negative regulators of signaling cAMP response element modulator-α and DUSP14. Diabetes 57:584–593. doi:10.2337/db07-1414
Koitabashi N, Danner T, Zaiman AL, Pinto YM, Rowell J, Mankowski J, Zhang D, Nakamura T, Takimoto E, Kass DA (2011) Pivotal role of cardiomyocyte TGF-β signaling in the murine pathological response to sustained pressure overload. J Clin Invest 121:2301–2312. doi:10.1172/JCI44824
Li H, He C, Feng J, Zhang Y, Tang Q, Bian Z, Bai X, Zhou H, Jiang H, Heximer SP, Qin M, Huang H, Liu PP, Huang C (2010) Regulator of G protein signaling 5 protects against cardiac hypertrophy and fibrosis during biomechanical stress of pressure overload. Proc Natl Acad Sci 107:13818–13823. doi:10.1073/pnas.1008397107
Liang Q, Bueno OF, Wilkins BJ, Kuan CY, Xia Y, Molkentin JD (2003) c-Jun N-terminal kinases (JNK) antagonize cardiac growth through cross-talk with calcineurin–NFAT signaling. EMBO J 22:5079–5089. doi:10.1093/emboj/cdg474
Lorell BH, Carabello BA (2000) Left ventricular hypertrophy: pathogenesis, detection, and prognosis. Circulation 102:470–479
Marie-Claire C, Benturquia N, Lundqvist A, Courtin C, Noble F (2008) Characteristics of dual specificity phosphatases mRNA regulation by 3,4-methylenedioxymethamphetamine acute treatment in mice striatum. Brain Res 1239:42–48. doi:10.1016/j.brainres.2008.08.050
Marti F, Krause A, Post NH, Lyddane C, Dupont B, Sadelain M, King PD (2001) Negative-feedback regulation of CD28 costimulation by a novel mitogen-activated protein kinase phosphatase, MKP6. J Immunol 166:197–206
Matsumoto-Ida M, Takimoto Y, Aoyama T, Akao M, Takeda T, Kita T (2006) Activation of TGF-beta1-TAK1-p38 MAPK pathway in spared cardiomyocytes is involved in left ventricular remodeling after myocardial infarction in rats. Am J Physiol Heart Circ Physiol 290:H709–H715. doi:10.1152/ajpheart.00186.2005
Minamino T, Yujiri T, Terada N, Taffet GE, Michael LH, Johnson GL, Schneider MD (2002) MEKK1 is essential for cardiac hypertrophy and dysfunction induced by Gq. Proc Natl Acad Sci 99:3866–3871. doi:10.1073/pnas.062453699
Patterson KI, Brummer T, O’Brien PM, Daly RJ (2009) Dual-specificity phosphatases: critical regulators with diverse cellular targets. Biochem J 418:475–489
Qin W, Du N, Zhang L, Wu X, Hu Y, Li X, Shen N, Li Y, Yang B, Xu C, Fang Z, Lu Y, Zhang Y, Du Z (2014) Genistein alleviates pressure overload-induced cardiac dysfunction and interstitial fibrosis in mice. Br J Pharmacol. doi:10.1111/bph.13002
Rockman HA, Ross RS, Harris AN, Knowlton KU, Steinhelper ME, Field LJ, Ross J Jr, Chien KR (1991) Segregation of atrial-specific and inducible expression of an atrial natriuretic factor transgene in an in vivo murine model of cardiac hypertrophy. Proc Natl Acad Sci 88:8277–8281
Rose BA, Force T, Wang Y (2010) Mitogen-activated protein kinase signaling in the heart: angels versus demons in a heart-breaking tale. Physiol Rev 90:1507–1546. doi:10.1152/physrev.00054.2009
Satoh M, Matter CM, Ogita H, Takeshita K, Wang CY, Dorn GW 2nd, Liao JK (2007) Inhibition of apoptosis-regulated signaling kinase-1 and prevention of congestive heart failure by estrogen. Circulation 115:3197–3204. doi:10.1161/CIRCULATIONAHA.106.657981
Shim JH, Xiao C, Paschal AE, Bailey ST, Rao P, Hayden MS, Lee KY, Bussey C, Steckel M, Tanaka N, Yamada G, Akira S, Matsumoto K, Ghosh S (2005) TAK1, but not TAB1 or TAB2, plays an essential role in multiple signaling pathways in vivo. Genes Dev 19:2668–2681. doi:10.1101/gad.1360605
Singh A, Sweeney MF, Yu M, Burger A, Greninger P, Benes C, Haber DA, Settleman J (2012) TAK1 inhibition promotes apoptosis in KRAS-dependent colon cancers. Cell 148:639–650. doi:10.1016/j.cell.2011.12.033
Tanaka K, Honda M, Takabatake T (2001) Redox regulation of MAPK pathways and cardiac hypertrophy in adult rat cardiac myocyte. J Am Coll Cardiol 37:676–685. doi:10.1016/S0735-1097(00)01123-2
Villar AV, Garcia R, Llano M, Cobo M, Merino D, Lantero A, Tramullas M, Hurle JM, Hurle MA, Nistal JF (2013) BAMBI (BMP and activin membrane-bound inhibitor) protects the murine heart from pressure-overload biomechanical stress by restraining TGF-β signaling. Biochim Biophys Acta 1832:323–335. doi:10.1016/j.bbadis.2012.11.007
Wollert KC, Taga T, Saito M, Narazaki M, Kishimoto T, Glembotski CC, Vernallis AB, Heath JK, Pennica D, Wood WI, Chien KR (1996) Cardiotrophin-1 activates a distinct form of cardiac muscle cell hypertrophy. Assembly of sarcomeric units in series VIA gp130/leukemia inhibitory factor receptor-dependent pathways. J Biol Chem 271:9535–9545
Yamaguchi K, Shirakabe K, Shibuya H, Irie K, Oishi I, Ueno N, Taniguchi T, Nishida E, Matsumoto K (1995) Identification of a member of the MAPKKK family as a potential mediator of TGF-β signal transduction. Science 270:2008–2011
Yang CY, Li JP, Chiu LL, Lan JL, Chen DY, Chuang HC, Huang CY, Tan TH (2014) Dual-specificity phosphatase 14 (DUSP14/MKP6) negatively regulates TCR signaling by inhibiting TAB1 activation. J Immunol 192:1547–1557. doi:10.4049/jimmunol.1300989
Zhang D, Gaussin V, Taffet GE, Belaguli NS, Yamada M, Schwartz RJ, Michael LH, Overbeek PA, Schneider MD (2000) TAK1 is activated in the myocardium after pressure overload and is sufficient to provoke heart failure in transgenic mice. Nat Med 6:556–563. doi:10.1038/75037
Zheng H, Li Q, Chen R, Zhang J, Ran Y, He X, Li S, Shu HB (2013) The dual-specificity phosphatase DUSP14 negatively regulates tumor necrosis factor- and interleukin-1-induced nuclear factor-κB activation by dephosphorylating the protein kinase TAK1. J Biol Chem 288:819–825. doi:10.1074/jbc.M112.412643
Acknowledgments
We thank Dr. Hong-Liang Li for providing experimental technological assistance (Wuhan University, Wuhan, China).This study was supported by Grants from the National Natural Science Foundation of China (Nos. 81070154, 81270258, 81530015); and the Shanghai Committee of Science and Technology, China (Nos. 11JC1408200, 12411951900, 13140903801).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Additional information
C.-Y. Li and Q. Zhou contributed equally to this work.
Rights and permissions
About this article
Cite this article
Li, CY., Zhou, Q., Yang, LC. et al. Dual-specificity phosphatase 14 protects the heart from aortic banding-induced cardiac hypertrophy and dysfunction through inactivation of TAK1-P38MAPK/-JNK1/2 signaling pathway. Basic Res Cardiol 111, 19 (2016). https://doi.org/10.1007/s00395-016-0536-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00395-016-0536-7