Abstract
Selective stimulation of β3 adrenergic-receptor (β3AR) has been shown to reduce infarct size in a mouse model of myocardial ischemia/reperfusion. However, its functional long-term effect and the cardioprotective mechanisms at the level of cardiomyocytes have not been elucidated, and the impact of β3AR stimulation has not been evaluated in a more translational large animal model. This study aimed at evaluating pre-perfusion administration of BRL37344 both in small and large animal models of myocardial ischemia/reperfusion. Pre-reperfusion administration of the β3AR agonist BRL37344 (5 μg/kg) reduced infarct size at 2-and 24-h reperfusion in wild-type mice. Long-term (12-weeks) left ventricular (LV) function assessed by echocardiography and cardiac magnetic resonance (CMR) was significantly improved in β3AR agonist-treated mice. Incubation with β3AR agonist (BRL37344, 7 μmol/L) significantly reduced cell death in isolated adult mouse cardiomyocytes during hypoxia/reoxygenation and decreased susceptibility to deleterious opening of the mitochondrial permeability transition pore (mPTP), via a mechanism dependent on the Akt-NO signaling pathway. Pre-reperfusion BRL37344 administration had no effect on infarct size in cyclophilin-D KO mice, further implicating mPTP in the mechanism of protection. Large-white pigs underwent percutaneous coronary ischemia/reperfusion and 3-T CMR at 7 and 45 days post-infarction. Pre-perfusion administration of BRL37344 (5 μg/kg) decreased infarct size and improved long-term LV contractile function. A single-dose administration of β3AR agonist before reperfusion decreased infarct size and resulted in a consistent and long-term improvement in cardiac function, both in small and large animal models of myocardial ischemia/reperfusion. This protection appears to be executed through inhibition of mPTP opening in cardiomyocytes.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Acute myocardial infarction (AMI) is a leading cause of mortality and morbidity worldwide. Early coronary reperfusion has been established as the best therapeutic strategy to limit infarct size and improve prognosis; however, reperfusion itself induces additional damage to the myocardium, known as ischemia/reperfusion injury (IRI) [20, 42, 49].
Evidence gathered over the past 40 years indicates that myocardial injury can be attenuated by manipulation of the response to IRI. In 1971 Braunwald et al. [38] demonstrated that the severity of myocardial necrosis due to coronary occlusion could be attenuated by appropriate interventions during ischemia. Since then, multiple strategies and interventions have been proposed as capable of limiting infarct size by reducing IRI in different animal models [5]. Despite these promising preclinical studies, attempts to translate them to the clinic have not been successful [23, 29, 47, 49] partly because of the lack of studies confirming results obtained in small animals in clinically relevant large animal models [10, 26]. The possibility of reducing the extent of cell death during an AMI is of great importance, since infarct size is the main determinant of post-infarction mortality [13]. Consequently, there is a clear need to develop therapies for reducing infarct size that go beyond early reperfusion.
The β3 adrenergic-receptor (β3AR) is a G-protein-coupled receptor preferentially expressed in adipose tissue. The identification of β3AR expression in the myocardium [22] prompted suggestions that it might be a therapeutic target in cardiovascular diseases, and β3AR-selective stimulation has been consistently beneficial in animal models of heart failure [12, 39]. More recently, β3AR agonists have been shown to reduce infarct size in mice undergoing regional myocardial ischemia/reperfusion [3]. However, it remains unknown whether β3AR stimulation during AMI results in long-term benefits on cardiac function and, more importantly, if this strategy is cardioprotective in a more clinically relevant large-animal model [28, 32]. Confirmation of an infarct-limiting effect and long-term benefits from this new therapeutic strategy would have a significant translational impact.
The fate of cardiomyocytes upon IRI is critically dependent on mitochondria [21, 30, 31, 49]. Irreversible and pathological opening of the mitochondrial permeability transition pore (mPTP) at the onset of reperfusion is well established as a major determinant of cardiomyocyte cell death [19, 30, 31]. A key regulator of mPTP opening is mitochondrial cyclophilin-D (CypD) and its pharmacological inhibition with cyclosporin-A (CsA) has been shown to reduce infarct size both in animal models and in clinics [4, 8, 18, 41, 48]. The effect of β3AR modulators on cardiomyocyte mPTP opening remains to be established.
The aims of this study were (1) to analyze the effect of pre-reperfusion β3AR agonist therapy on infarct size and long-term myocardial performance in a mouse model of IRI, (2) to study the cardioprotective mechanisms involved in β3AR stimulation at the cardiomyocyte level, and (3) to confirm the beneficial effect of β3AR agonist therapy in a large preclinical animal model of AMI.
Materials and methods
Study design
Two sets of mice were subjected to temporal left anterior descending (LAD) coronary artery occlusion and randomized to receive a single bolus of the β3AR agonist BRL37344 or vehicle before reperfusion. In the first set, late IRI was evaluated by quantification of infarct size at 24 h reperfusion. In a second set, serial left ventricular (LV) function was assessed by echocardiography and high field (7-T) cardiac magnetic resonance (CMR) at short- (1 and 4 weeks) and long-term (12 weeks) follow-up. To confirm β3AR agonism implication, FVB/N β3AR-knockout (KO) mice were subjected to the same myocardial IRI procedure and infarct size evaluated at 24 h of reperfusion.
To study whether the protective effect of pre-reperfusion β3AR stimulation derives from a direct effect on cardiomyocytes, isolated adult mouse cardiomyocytes were subjected to simulated ischemia/reperfusion (hypoxia/reoxygenation; H/R), and cell viability evaluated in the presence or absence of BRL37344. The role of nitric oxide (NO) production as an intracellular signaling mediator was tested by co-incubation with BRL37344 and the nitric oxide synthase (NOS) inhibitor L-NAME. In addition, the H/R procedure was applied to adult cardiomyocytes from mice lacking endothelial-NOS (eNOS-KO). NO signaling pathway activation was evaluated by western blot in isolated cardiomyocytes subjected to H/R. Susceptibility to mPTP opening during β3AR stimulation was evaluated in isolated cardiomyocytes in the presence of BRL37344, saline, or the CypD inhibitor cyclosporine-A (CsA). The implication of mPTP opening in β3AR-agonist-mediated cardioprotection was tested in vivo in CypD-KO mice subjected to the myocardial IRI procedure and randomized to receive BRL37344 or vehicle before 2 h if reperfusion.
The translational impact of β3AR-agonist-mediated cardioprotection was tested in a pig model of AMI by 60 min of percutaneous angioplasty followed by reperfusion [33, 35] and randomized to receive either BRL37344 or vehicle at the onset reperfusion. Infarct size was evaluated by 3-T CMR at 7 days post-infarction, and LV function was evaluated, also by CMR, at long-term follow-up.
Mouse model of myocardial ischemia/reperfusion injury (IRI)
Male 8- to 12-week-old mice were subjected to 45 min of left anterior descending (LAD) coronary artery occlusion followed by reperfusion. For infarct size evaluation, reperfusion was maintained for 2 or 24 h; for assessment of long-term left ventricular (LV) function, reperfusion was maintained for 12 weeks. For the LAD procedure, mice were intra-peritoneal anesthetized with ketamine (60 mg/kg), xylacine (20 mg/kg), and atropine (9 mg/kg). Once deeply asleep, and under direct visualization of the trachea, animals were orally intubated using a blunted 22G cannula and mechanically ventilated throughout the entire procedure (SAR-830. CWE Inc.). Temperature was controlled (BAT-12, Physitemp Instruments) and kept constant at 37 °C with a heated operating table (V500VStat, Peco Services) to prevent hypothermic cardioprotection [2]. As previously described by Gomez et al. [24], a nylon 8/0 monofilament suture was passed beneath the LAD approximately 2 mm below the tip of the left atrium appendage. After stabilization for 5 min, regional ischemia was induced by tightening a simple snare to stop coronary blood flow. A short segment of PE-10 tubing was placed between the tissue and the suture to minimize damage and allow for complete reperfusion after the ischemic period. Successful LAD occlusion was confirmed by ST-segment elevation on ECG (MP36R, Biopac Systems Inc.) and the appearance of myocardial pallor. During ischemia, the thorax was covered with parafilm to prevent dehydration. Anesthetic mixture was injected intra-peritoneally when needed. Five minutes before the onset of reperfusion, mice were randomized to receive a single bolus injection (50 µL, with an insulin syringe) of the β3AR agonist BRL37344 (5 μg/kg) or saline into the femoral vein. The BRL37344 dose was selected on the basis of dose–response studies performed before the initiation of the IRI procedure (data not shown). The thoraxes of animals designated for infarct-size evaluation at 24 h reperfusion were closed with a 6/0 silk thread, and animals were recovered with 100 % O2 and analgesized with buprenorphine (S.C., 0.1 mg/kg) until the end of the procedure. Animals designated to early IRI evaluation (2 h reperfusion) were maintained completely asleep and under mechanical ventilation until the end of the procedure.
Infarct size quantification
Mice reperfused for 24 h were briefly re-anesthetized at the end of the reperfusion period, and were then intubated and the LAD re-occluded by ligating the suture in the same position as the original infarction. Animals were then killed and 1 mL of 1 % (w/v) Evans Blue dye infused i.v. to delineate the Area at Risk (AAR: myocardium lacking blood flow, i.e. negative to blue dye staining). The heart was then excised, the left ventricle (LV) was isolated and cut into seven 1-mm-thick transverse slices, and pictures were taken from both sides. In order to differentiate infarcted from viable tissue, slices were incubated in triphenyltetrazolium chloride (TTC, 1 % (w/v) diluted in PBS) at 37 °C for 15 min. The slices were then re-photographed and weighed. Regions negative for Evans Blue staining (AAR) and negative for TTC (infarcted myocardium) were calculated by a blinded observer using the computer-assisted planimetry function in ImageJ 6.0 (NIH, Bethesda, MD). Infarct size for each slice was calculated as the average percentage of infarcted myocardium from both sides of each section. Following a previously described method [9], percentile values for AAR and IS were corrected to mg independently for each slice. Finally, absolute infarct size was determined as the ratio ∑mg of IS/∑mg of AAR. This methodology takes into account individual AAR variability [11]. The full set of LV images is shown in supplemental Fig. 2.
Echocardiography functional examination in mice
Echocardiographic evaluations to determine cardiac volume and LV contractility were performed by an experienced observer blinded to the study allocation in mice at 1, 4 and 12 weeks post-infarction. Mice were anesthetized by inhalation of isoflurane/oxygen and examined with a 30-MHz transthoracic echocardiography probe and a Vevo 2100 ultrasound system (VisualSonics, Toronto, Canada). From short-axis and long-axis B-mode views, end-systolic and end-diastolic LV volumes and LV ejection fraction (LVEF) were calculated using the area-length method [16]. LV regional function was evaluated in a 13-segment model (basal, middle and apical segments of the septum, anterior, lateral, postero-inferior walls and the apex) and scored as follows: normal (0), hypo/akinesis (1), dyskinesis/aneurysm (2). A segmental LV wall motion score was defined as the sum of the individual segment scores in each animal.
High field CMR protocol in mice
Myocardial volumes and function were assessed by CMR 12 weeks post-AMI. Mice were anesthetized by inhalation of isoflurane/oxygen (5 %/95 %) and examined with a 7-T field preclinical CMR system (BioSpec 70/20 USR, Bruker BioSpin) with a maximum gradient of 750 mT/m. A volume resonator (72 mm inner diameter) operating in quadrature mode was used for excitation and a four-element phased array surface mouse heart coil (Rapid Biomedical) was used for signal reception. After standard cardiac localizers, cine images were acquired using fast low-angle shot (Intragate-FLASH) sequences in 6–7 short-axis planes to cover the whole LV with a field of view (FOV) of 2.7 × 3 cm, a 1-mm slice thickness without gaps, TE 2.4 ms, TR 8 ms, cardiac phases 10, and matrix of 256 × 256 pixels. Cine images were reconstructed using retrospective ECG-gating performed with IntraGate, which is included in the CMR Paravision Bruker software. ECG and breathing rhythm were monitored with a CMR-compatible system for small animals (Model 1025, S.A. Instruments, Inc., New York, USA).
Isolation of adult mouse cardiomyocytes
The protocol for mouse adult cardiomyocyte isolation was adapted from several studies [36, 44, 50]. Briefly, 10- to 12-week-old C57BL/6J WT or eNOS-KO mice were heparinized (50 USP units) and anesthetized with a mixture of ketamine (140 mg/kg), xylazine (33 mg/kg), and atropine (9 mg/kg). Once pedal pinch reflexes were completely inhibited, animals were placed in a supine position, ventral thoracic regions were wiped with 70 % alcohol, and animals were euthanized. The heart was quickly removed, cannulated through the ascending aorta, and mounted on a modified Langendorff perfusion apparatus. The heart was then retrogradely perfused (3 mL/min) for 5 min at room temperature (RT) with pre-filtered Ca2+-free Perfusion-Buffer [NaCl (113 mmol/L); KCl (4.7 mmol/L); KH2PO4 (0.6 mmol/L); Na2HPO4 (0.6 mmol/L); MgSO4·7H2O (1.2 mmol/L); NaHCO3 (12 mmol/L); KHCO3 (10 mmol/L); Phenol Red (0.032 mmol/L); HEPES-Na salt (0.922 mmol/L); taurine (30 mmol/L); glucose (5.5 mmol/L); 2,3-butanedione-monoxime (10 mmol/L), pH 7.4]. Enzymatic digestion was performed with digestion-buffer [perfusion-buffer with Liberase™ (0.2 mg/mL), Trypsin 2.5 % (5.5 mmol/L); DNase (5 × 10−3 U/mL) and CaCl2 (12.5 µmol/L)] for 20 min at 37 °C. At the end of enzymatic digestion, both ventricles were isolated and gently disaggregated in 5 mL of Digestion Buffer. The resulting cell suspension was filtered through a 100-µm sterile mesh (SEFAR-Nitex) and transferred for enzymatic inactivation to a tube with 10 mL of stopping-buffer-1 [perfusion-buffer supplemented with fetal bovine serum (FBS, 10 % v/v) and CaCl2 (12.5 µmol/L)]. After gravity sedimentation for 20 min, cardiomyocytes were resuspended in stopping-buffer-2 containing lower FBS (5 % v/v) for another 20 min. Cardiomyocyte Ca2+-reintroduction was performed in stopping-buffer-2 with five progressively increased CaCl2 concentrations (62 µmol/L, 112 µmol/L, 212 µmol/L, 500 µmol/L and 1 mmol/L). Cells were resuspended and allowed to decant for 10 min in each step, contributing to the purification of the cardiomyocyte suspension. The homogeneous suspension of rod-shaped cardiomyocytes was then resuspended in M199 supplemented with Earle’s salts and l-glutamine, penicillin–streptomycin (1 %), insulin–transferin–selenium-A (0.1×), bovine serum albumin (BSA, 2 g/L), blebbistatin (25 µmol/L) and FBS (5 %). Cells were plated in single drops onto 22-mm2 glass coverslips precoated with 200 μL of mouse laminin (10 mg/mL) in phosphate-buffered saline (PBS) for 1 h.
Hypoxia/reoxygenation in adult mouse cardiomyocytes
Prior to being subjected to induced hypoxia/reoxygenation, plated isolated adult mouse cardiomyocytes were washed and stabilized for 30 min at 37 °C with normoxic-buffer (NB) [NaCl (113 mmol/L); KCl (4.7 mmol/L); KH2PO4 (0.6 mmol/L); Na2HPO4 (0.6 mmol/L); MgSO4·7H2O (1.2 mmol/L); NaHCO3 (12 mmol/L); KHCO3 (10 mmol/L); HEPES-Na Salt (0.922 mmol/L); Glucose (10 mmol/L); CaCl2 (1 mmol/L) and pH 7.4]. Hoechst 33342 (H42, 1 µg/mL) was added for cell recognition, and propidium iodide (PI, 1 µg/mL) was added to evaluate cell viability. Simulated ischemia was induced at 1 % O2 by placing cells in a H35 Hypoxystation chamber (Don Whitley Scientific Limited, UK) in ischemic-buffer (IB), in which glucose and HEPES were replaced with lactate-Na (10 mmol/L) and PIPES (10 mmol/L), at pH 6.8 for 30 min (IB was pre-equilibrated at 1 % O2 for 2 h prior to use). After the hypoxia incubation, IB was replaced with NB for 1 h to simulate reperfusion. Duplicate wells were randomized to receive (1) control: NaCl (0.9 %), (2) insulin as positive control (2 nmol/L), (3) BRL37344 (7 μmol/L), or (4) NG-nitro-l-arginine methyl ester (L-NAME (10 µmol/L). Fluorescent images were acquired with a Nikon Time-lapse confocal microscope after 15, 30, 45 and 60 min of reoxygenation. An average of 350 rod-shaped cells/well from 6 independent experiments was analyzed by a blinded observer using ImageJ 6.0 (NIH, Bethesda, MD, USA). Cell death, indicated by internalization of red fluorescence (Red, PI positive) was expressed as a percentage of the total number of cardiomyocytes at each point (Blue, H42 positive) and normalized to saline treatment.
Western blot
For protein isolation, cardiomyocytes were maintained in suspension in 1 mL of IB for 30 min at 1 % O2 in a H35 Hypoxystation chamber (Don Whitley Scientific Limited, UK) followed by 15 min of simulated reoxygention in NB in the CO2 incubator. Cardiomyocytes were spun down and proteins isolated in RIPA lysis buffer (150 mmol/L NaCl, 1.0 % IGEPAL, 0.5 % sodium deoxycholate, 0.1 % SDS, 50 mmol/L Tris, pH 8.0) supplemented with protease/phosphatase inhibitors. After quantification (Pierce BCA Protein Assay Kit) 30 µg of protein was loaded on 10 and 7 % SDS polyacrylamide gels. After electrophoresis, proteins were transferred to a polyvinylidene fluoride (PVDF) membrane. Primary antibodies specific for total Akt and phospho-Akt (Ser473) (Cell Signaling Technology, USA) were incubated with the PVDF membranes overnight in Tris Buffered Saline containing 0.1 % Tween and 5 % bovine serum albumin. After HRP-secondary antibody incubation blots were developed by chemiluminescence using Luminata Forte substrate (Millipore, USA). Densitometry of bands was analyzed with ImageJ 6.0 (NIH, Bethesda, MD, USA). The ratio between the phospho-specific and total protein densitometry signals was calculated.
Induction and detection of mPTP opening
To determine the effect of beta-3-adrenoceptor stimulation on the susceptibility to mPTP opening, we used a well-characterized model that simulates the deleterious effect of mitochondrial reactive oxygen species (ROS) production upon reperfusion [6, 15, 17]. Maintained confocal laser-stimulation of the fluorescent mitotraker tetramethyl-rhodamine methyl ester (TMRM) produces ROS within the mitochondria, which results in mPTP opening as indicated by mitochondrial membrane depolarization [51]. Susceptibility to mPTP opening was defined as the time taken to induce mitochondrial membrane depolarization, visualized as dequenching of TMRM fluorescence upon its translocation to the cytoplasm. Isolated adult cardiomyocytes, freshly plated on laminin-precoated (10 mg/mL) coverslips, were loaded with TMRM (3 μmol/L) in Hank’s buffered saline solution (1.2 mmol/L CaCl2, 15 min at 37 °C). Before induction and detection of mPTP opening, cardiomyocytes were randomly assigned to the following treatment groups and loaded for 10 min with (1) vehicle control: DMSO (0.02 %) + NaCl (0.9 %); (2) CsA positive control (0.4 μmol/L); (3) BRL37344 (7 μmol/L); (4) Both treatments in combination (CsA + BRL37344). An average of 200 rod-shaped cells was analyzed per group in 9 different experiments. Cells were monitored with a Leica confocal microscope (SP5), and images were acquired at 2.63-s intervals with simultaneous excitation at 543 nm. The gain was adjusted to achieve maximum signal intensity without saturation. All time values were normalized against the mean time for cardiomyocytes maintained in vehicle.
Pig model of AMI
A re-perfused anterior wall AMI was experimentally induced in 3-month-old castrated male Large-white pigs bred at the CNIC’s farm. The protocol for AMI induction is detailed elsewhere [33, 35]. In brief, anesthesia was induced by intramuscular injection of ketamine (15 mg/kg), xylazine (2 mg/kg), and midazolam (0.5 mg/kg). buprenorphine (0.03 mg/kg) was used as an analgesic during the intervention. All animals were intubated and mechanically ventilated with oxygen (fraction of inspired O2, 28 %) and anesthesia was maintained by intravenous administration of midazolam (0.2 mg/kg/h). A continuous infusion of amiodarone (300 mg, 150 mg/h) was maintained during the procedure in all pigs as prophylaxis for malignant ventricular arrhythmias. The LAD immediately distal to the origin of the first diagonal branch was occluded for 60 min with an angioplasty balloon inserted via the percutaneous femoral route. Animals were allocated 1:1 by a restricted randomization (Efron’s biased coin randomization) to receive the β3AR agonist (BRL37344, 5 µg/kg) or vehicle via marginal vein of the ear 5 min before reperfusion. The treatment (BRL37344 or vehicle) was prepared in non-labeled syringes before the AMI induction and administered by operators blinded to the randomization. After balloon deflation, a coronary angiogram was obtained to confirm appropriate coronary reperfusion. Animals were recovered thereafter and cared by dedicated veterinarians and technicians at the CNIC Comparative Medicine Unit.
CMR protocol in pigs
Cardiac magnetic resonance studies were performed 7 and 45 days after AMI to assess infarct size and LV performance. Pigs were anesthetized by intramuscular injection of ketamine, xylacine and midazolam as described above, and anesthesia was maintained by continuous intravenous infusion of midazolam. All studies were performed using a Philips 3-T Achieva Tx whole body scanner (Philips Medical Systems, Best, The Netherlands) equipped with a 32-element cardiac phased-array surface coil. Images were acquired with the use of ECG gating by operators blinded to the study arm. Segmented cine steady-state free precession (SSFP) was performed to acquire 11–13 contiguous short-axis slices covering the heart from the base to the apex to evaluate global and regional LV motion (FOV of 280 × 280 mm; slice thickness of 8 mm without gap; TR 2.8 ms; TE 1.4 ms, flip angle 45; cardiac phases 25; voxel size 1.8 × 1.8 mm; 3 NEX). Edema imaging (for AAR quantification) was performed with a T2-weighted, triple inversion-recovery fast spin-echo (T2W-STIR) sequence (FOV of 280 × 280; 11–13 short-axis slices with thickness of 8 mm and no gap; TR 2–3 heartbeats; TE 80 ms; voxel size 1.4 × 1.4 mm; STIR delay 210 ms; trigger delay longest; echo-train length 16; 2 NEX). A coil sensitivity correction algorithm for all T2W images was implemented in the scan acquisition. Finally, late gadolinium enhancement imaging was performed 15 min after the administration of 0.2 mmol/kg gadopentate dimeglumine using an inversion-recovery fast gradient-echo sequence to determine MI size (FOV of 280 × 280 mm; 11–13 short-axis slices with a thickness of 8 mm and no gap; TR 5.6 ms; TE 2.8 ms; voxel size 1.6 × 1.6 mm; time interval optimized to null normal myocardium; trigger delay longest; bandwidth, 304 Hz per pixel; 2 NEX).
CMR data analysis
All CMR images were analyzed using dedicated software (QMass MR v.7.6, Medis, Leiden, The Netherlands). Images were analyzed by two experienced observers with vast experience in CMR analysis and blinded to the study allocation. The analysis protocol has been detailed elsewhere [34]. In brief, LV cardiac borders were traced in each cine image to obtain LV end-diastolic volume (LVEDV), end-systolic volume (LVESV) and LVEF. LV volumes normalized to the body surface area were calculated with Brody’s formula [37]. The left ventricle was divided into 16 segments based on the American Heart Association (AHA) segmented model. Fractional wall systolic thickening was quantified from endocardial and epicardial tracings using a centerline analysis and expressed as the mean of the segmental thickenings. A wall systolic thickening index was calculated in each animal as the number of segments of LV with fractional wall systolic thickening higher than 30 % [40]. The area of myocardium AAR was defined as the extent of the LV demonstrating high signal intensity on T2W-STIR images [1]. Infarct size (necrosis) was quantified from the extent of abnormal delayed gadolinium enhancement. AAR and necrosis were identified as hyperintense regions, defined as >50 % of the peak myocardial signal intensity (full width half maximum) with manual adjustment when needed. If present, a central hypointense core within the area of increased signal was included in the T2W-STIR or late gadolinium enhancement analysis. As described above, infarct size was expressed as a percentage of the AAR. In addition, three short-axis slices (basal, mid-cavity and apical) from the SSFP sequence of each animal were selected for deformation analysis using CMR-based feature tracking [45]. Circumferential strain was assessed with ad hoc software (2D Cardiac Performance Analysis MR, TomTec Imaging System, Germany). Endocardial borders were manually drawn in all analyzed slices and then the automatic computation was triggered. Finally, the global circumferential strain (GCS) in each animal was calculated as the median of all segmental circumferential strains.
All animal studies conducted at the CNIC were approved by the local ethics committee, and all animal procedures conformed to EU Directive 2010/63EU and Recommendation 2007/526/EC regarding the protection of animals used for experimental and other scientific purposes, enforced in Spanish law under Real Decreto 1201/2005. Procedures carried out at the Hatter Cardiovascular Institute (UCL) were conducted in accordance with the UK National Institute of Health Guidelines for the Care and Use of Laboratory Animals. Authors had full access to and take full responsibility for the integrity of the data. All authors have read and agree to the manuscript as written.
Drugs
Reagents were purchased from Sigma-Aldrich Co. LLC., Thermo Fisher Scientific Inc., and Tocris Bioscience.
Statistical analysis
The distribution of continuous variables was analyzed with graphical methods. For normally distributed variables, results are expressed as mean (SD) and compared either by Student’s unpaired t test (with Welch’s correction when appropriate) or one-way ANOVA. When repeated measurements were performed, two-way repeated-measures ANOVA were applied followed by Bonferroni correction for post hoc analysis. Non-normal data are reported as median (IQR) and compared by Mann–Whitney U test. Differences were considered statistically significant at p value <0.05 (two-tailed).
Results
Pre-reperfusion administration with β3AR agonist reduces infarct size and improves long-term cardiac function in mice
Administration of the β3AR agonist BRL37344 before reperfusion induced a significant reduction in infarct size (27.1 (13.0) % of area at risk (AAR) in β3AR-treated mice vs. 41.1 (10.7) % with vehicle; p = 0.025) (Fig. 1a). AAR was similar in both groups. Consistent with the reduced infarct size, pre-reperfusion BRL37344 led to a long-term improvement in LV contractile function, as assessed by echocardiography at sequential follow-up evaluations (Fig. 1c; Table 1). Similarly, CMR evaluation revealed that LV ejection fraction (LVEF) was significantly higher in BRL37344-treated mice than controls after 12 weeks (46.5 (6.3) vs. 37.7 (6.0) %; p = 0.004; Fig 1e; Table 1). The cardioprotection afforded by BRL37344 administration was absent in β3AR-KO mice: (31.5 (9.5) % of AAR vs. 24.1 (6.7) %; p = 0.112; Supplemental Fig 1). Echocardiographic and CMR videos are available in the supplemental material online.
Long-term cardioprotective effect in mice subjected to ischemia/reperfusion after pre-reperfusion administration of the β3AR agonist BRL37344. a AAR (%LV) and IS (%AAR) in C57BL/6J WT mice subjected to myocardial IRI and treated with the β3AR agonist BRL37344 (BRL, 5 μg/kg) or vehicle before reperfusion. b Representative histological images of 1-mm-thick transverse ventricular slices of mice treated with BRL37344 or vehicle. Upper images show the AAR (negative for Evans Blue staining). Lower images show the extent of necrosis (paler area) in the same sections after incubation in TTC. c LVEF evaluated by serial echocardiography at 1, 4 and 12 weeks post-infarction in mice treated with BRL37344 or vehicle before reperfusion. d Representative short-axis echocardiography images at mid-ventricular level, illustrating left-ventricular contractility defects (red arrows). e LVEF evaluated by serial CMR at 12 weeks post-infarction in mice treated with BRL37344 or vehicle before reperfusion. f Representative short-axis CMR images at mid-ventricular level, illustrating LV contractility defects (red arrows). LV motion videos obtained by echocardiography and CMR are available in Supplemental material online. Data are presented as mean ± SEM. *p < 0.05
Selective β3AR stimulation with BRL37344 increases survival of isolated adult cardiomyocytes undergoing hypoxia/reoxygenation (H/R)
Isolated adult cardiomyocytes from WT mice were subjected to simulated ischemia/reperfusion in the presence of BRL37344 or saline. Analysis of PI exclusion showed significant reduction of cell death in the presence of BRL37344. Co-incubation with the NOS inhibitor L-NAME abrogated the cardioprotection shown by BRL37344 (Fig. 2a). When we repeated the procedure in eNOS-KO cardiomyocytes no differences were found between BRL37344-treated and non-treated cells. These results confirm the key role of NO in the protection exerted by β3AR-selective stimulation (Fig. 2c). Due to the importance of Akt in cardioprotection [27], we assessed the activation of AKT by western blot. Densitometric analysis showed a significant increase of Akt phosphorylation at serine 473 in BRL37344-treated cells (Fig. 2d).
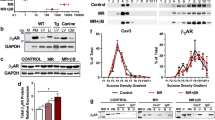
β3 adrenergic receptor stimulation protects isolated cardiomyocytes against hypoxia/reoxygenation through NO-dependent signaling. Isolated adult mouse cardiomyocytes were subjected to 30-min hypoxia followed by reoxygenation in the presence of vehicle (0.9 % NaCl), BRL37344 (BRL, 7 μM), L-NAME (10 μM) or insulin (2 nM; positive control). a Representative fluorescent microscopical images of isolated cardiomyocytes before H/R during (1) normoxia: showing PI-negative rod-shaped fresh cardiomyocytes and (2) reoxygenation: showing a high % of PI-positive hypercontracted rounded cells. b BRL37344 (BRL) treatment significantly reduces cell death while co-incubation with L-NAME abrogates the protective effect, detected as the % of PI-positive cells. Data are mean ± SEM of % PI scores in images taken at 15 min intervals up to 1 h. Groups were compared by two-way repeated measures ANOVA with the Bonferroni correction for post hoc analysis. c Percentage of cell death in adult cardiomyocytes isolated from eNOS-KO mice and subjected to H/R with or without pretreatment with BRL37344. The protective effect of BRL37344 is abrogated in the absence of eNOS. d Phospho-serine 473 AKT [pAKT(473)] levels detected after 15 min of reoxygenation in untreated and BRL37344-treated WT cardiomyocytes. Data are presented as mean ± SEM. *p < 0.05
The cardioprotective effect of β3AR-selective stimulation involves mPTP
To determine whether selective β3AR stimulation has a direct pharmacological effect on mPTP, TMRM-preloaded adult cardiomyocytes were incubated with BRL37344, saline, or CsA, alone or in combination, and subjected to oxidative-stress-induced mPTP opening. BRL37344 treatment delayed the time to mPTP opening by 1.26 (0.67)-fold compared with vehicle values (p < 0.001; Fig. 3c). Interestingly, combined treatment with BRL37344 and CsA did not further delay mPTP opening compared with each treatment independently.
β3 adrenergic receptor stimulation delays mPTP opening in TMRM-preloaded adult cardiomyocytes subjected to laser-mediated oxidative stress. a Time-lapse confocal images showing progressive loss of mitochondrial membrane potential after induction of oxidative stress by sustained confocal laser scanning. Arrows indicate sites of incipient mPTP opening and consequent dequenching of the dye in the cytoplasm. b Detailed view of mitochondrial membrane depolarization: mPTP opening triggers rapid TMRM release from mitochondria, resulting in locally increased fluorescence intensity due to dye dequenching. mPTP opening proceeds in a wave across the cell in a polarized manner and of the phenomenon of cardiomyocyte hyper-contractility, caused by mitochondrial membrane depolarization after sustained exposure to oxidative stress. c Normalized mean values of the time to mPTP opening in cardiomyocytes after addition of vehicle (DMSO, 0.02 %), cyclosporine-A (positive control; CsA, 0.4 μM), BRL37344 (BRL, 7 μM) and BRL + CsA. n independent experiments, with 150–200 cells analyzed per treatment. Data are presented as mean ± SEM. *p < 0.05
To confirm the implication of mPTP in β3AR-mediated cardioprotection in vivo, we tested the effect of pre-reperfusion BRL37344 on early IRI in WT and CypD KO mice. In WT mice, β3AR stimulation significantly reduced infarct size at 2 h reperfusion (28.1 (12.3) % of AAR vs. 45.8 (12.1) % in vehicle-treated mice; p = 0.020; Fig. 4b). Consistent with the in vitro cardiomyocyte experiments, β3AR stimulation did not reduce infarct size in animals lacking mitochondrial CypD (30.9 (14.7) % vs. 30.0 (7.9) % of AAR in BRL37344- and vehicle-treated CypD KO mice, respectively; p = 0.884; Fig. 4b).
Pre-reperfusion administration of BRL37344 does not provide an additional cardioprotective effect in CypD KO mice. a AAR (%LV) in WT and CypD KO mice treated with vehicle or BRL37344 (BRL, 5 μg/kg) (p = ns). b Infarct size (% of AAR) at 2 h reperfusion. Data presented as mean ± SEM. c Representative histological images of heart slices after staining to delineate the AAR (negative for Evans Blue) and infarcted area (paler region on TTC staining) for all groups. *p < 0.05
Pre-reperfusion β3AR agonist administration reduces infarct size and improves long-term cardiac function in a swine model of myocardial I/R
Acute myocardial infarction was induced in Large-white pigs (40.1 (6.2) kg) by percutaneous angioplasty (60 min balloon-mediated LAD coronary occlusion) followed by reperfusion. No pigs died during AMI induction, but seven died within the first week after infarction and, therefore, did not undergo day-7 CMR (3 allocated to BRL37344 and 4 to vehicle). Two pigs (one per treatment group) died suddenly before completing the day 45 CMR. Final numbers of animals are noted in the figures.
Pre-reperfusion administration of BRL37344 provoked a transient increase in heart rate compared with vehicle (10.0 (9.5) vs. −1.2 (2.3) change from baseline bpm; p = 0.013); heart rate returned to baseline after 10 min. Conversely, pre-reperfusion BRL37344 had no significant effect on mean blood pressure (−0.13 (7.4) vs. −0.83 (2.8) mmHg; p = 0.78). Full data in Supplemental Table 1.
On day 7 CMR, infarct size was significantly smaller in the β3AR-agonist-treated group (80.0 (21.4) % of AAR, vs. 93.5 (16.8) % in vehicle-treated pigs; p = 0.044; Fig. 5a). Consistent with this, BRL37344-treated pigs had improved LV contractile performance on day 45 CMR: pigs receiving BRL37344 showed a better regional myocardial contractile function than pigs treated with vehicle, as evidenced by higher fractional systolic thickening (45.4 (5.8) % vs. 36.4 (9.0) %; p = 0.032; Table 2) and systolic thickening index (11.0 (1.0) vs. 9.0 (2.0) segments; p = 0.026; Fig. 5c). BRL37344-treated pigs also showed a trend on day 45 CMR toward a higher LVEF (41.4 (6.3) % vs. 37.0 (4.6) %; p = 0.119; Fig. 5b). Finally, myocardial deformation analyses showed that pigs receiving the β3AR agonist had a better global circumferential strain (−20.1 (1.7) vs. −17.0 (2.8) %; p = 0.018; Fig. 5e). Full CMR is presented in Table 2
Pre-reperfusion treatment of the β3AR agonist BRL37344 reduces infarct size and exerts a long-term beneficial effect in a pig model of AMI. a Infarct size (%AAR) assessed by CMR at 7 days post-infarction in large-white pigs. BRL stands for BRL37344 (5 μg/kg). b Evolution of LVEF in vehicle- and BRL37344-treated pigs, assessed by CMR at 7 and 45 days post-infarction; LVEF tends to improve in BRL37344-treated pigs while it tends to worsen in vehicle-treated pigs. c LV systolic wall thickening index assessed by CMR at long-term follow-up. d Representative short-axis CMR images at the same level of the LV, showing the extent of area at risk (AAR: hyper-intense area in T2-weighted CMR sequence), myocardial necrosis [delayed enhancement (DE) after gadolinium injection], and the merged view of both in one animal receiving pre-reperfusion BRL37344 and in another receiving vehicle. e Global circumferential strain assessed by CMR-based feature tracking. f Representative segmental circumferential strain images evaluated by CMR-based feature tracking in a pig receiving pre-reperfusion β3AR agonist treatment. Data are presented as mean ± SEM. *p < 0.05
.
Discussion
This study presents the first evidence for long-term benefits from pre-reperfusion IV administration of a β3AR-selective agonist in AMI. In a mouse model, these beneficial effects are evident both at very early (2 h reperfusion) and late (24 h reperfusion) stages of IRI and in isolated cardiomyocytes. Analysis with CMR shows that β3AR agonism with BRL37344 limits infarct size and improves cardiac function several weeks post AMI in mice and pigs. This cardioprotective effect is mediated by a delay in mPTP opening dependent on the Akt-NO signaling pathway. To our knowledge, this is the first demonstration of reduced IRI and associated long-term functional benefits after a single i.v. administration of a β3AR agonist in a clinically relevant large animal model of AMI.
β3AR agonist administration before reperfusion reduces infarct size, resulting in a long-term beneficial effect
β3AR-selective stimulation has recently been proposed as a new therapy for several myocardial diseases [3, 12, 39]. Aragon et al. [3] recently demonstrated a reduction in infarct size (evaluated 24 h after IRI) when a β3AR agonist was administered before reperfusion but reported no improvement in cardiac function after β3AR agonist treatment in mice assessed by echocardiography at short-term follow-up (1 week), raising doubts about whether evidence of cardioprotection from histological evaluation translates to functional benefits. Our present data confirm the beneficial pre-reperfusion β3AR agonist administration effect when evaluated at early stages (2 h reperfusion), suggesting that the cardioprotection afforded by this therapy takes place within the first minutes of reperfusion. Similar to Aragon’s results, our data show that LV function 1 week after AMI did not differ significantly between β3AR-agonist- and vehicle-treated animals. However, the longer follow-up period in our study allowed us to demonstrate a clear association of the infarct-limiting effects of pre-reperfusion β3AR-agonist treatment with improved cardiac function shown by both echocardiography and CMR. The most likely reason for the late appearance of improved cardiac function is that at early stages the salvaged myocardium is in a stunned, non-contractile, state and that full contractile recovery is, therefore, seen only after longer follow-up. This interpretation is supported by the gradual recovery of segmental LV wall motion scores after 1-week follow-up in β3AR-agonist-treated mice (Table 1). These results thus highlight the importance of long-term follow-up for evaluation of the functional benefits of a cardioprotective intervention.
It is noteworthy that infarcts in β3AR KO mice appear to be smaller than those in wild-type mice. A similar effect is apparent in previous works by other groups [3]. In this regard, it should be noted that the β3AR KO mice used here were in the FVB/N genetic background, which has been reported to confer innate cardioprotection against IRI [25]. Another potential explanation for this effect could be that the absence of β3AR results in a redistribution of the other two types of βAR. If βAR redistribution would result in an upregulation of β2AR, this might explain the spontaneous protection of these mice, since signaling via β2AR during IRI has been shown to reduce infarct size [7], and its upregulation by gene therapy results in an incremental protective cardiac phenotype [43]. However, this alternative protective scenario in β3AR KO mice is speculative since the actual redistribution of β1AR and β2AR in the absence of β3AR has not been studied in the heart.
Cardiomyocyte β3AR-Akt-eNOS-NO-mPTP signaling pathway is implicated in the cardioprotection afforded by β3AR-selective stimulation
Previous studies into the protective effect of β3AR-selective stimulation in cardiac diseases [3, 14, 39] did not address whether the mechanism involves an action in cardiomyocytes [28]. In our analysis, β3AR-selective stimulation significantly increased the viability of isolated adult cardiomyocytes in response to hypoxia/reoxygenation, indicating that the cardioprotection associated with β3AR-agonist stimulation occurs in the early phases of IRI through an effect at the cardiomyocyte level. We further demonstrate that serine 473 phosphorylation of Akt and NO-dependent signaling are both critical mediators of this protection.
Moreover, BRL37344 significantly delays the opening of the mPTP, which plays a central role in cardiomyocyte death upon IRI [4, 18]. Interestingly, the co-incubation of cardiomyocytes with BRL37344 and a known inhibitor of mPTP opening, CsA, did not significantly increase the delay in mPTP opening, suggesting that the two agents act on the same cardioprotective pathway. Finally, we have documented that β3AR stimulation had no additional infarct-limiting effect in CypD-KO mice [4], which have been shown to be protected against IRI [4, 6], again suggesting action on the same pathway. Although CypD KO mice are strongly protected against IRI, further reductions in infarct size in these animals can be obtained with protective strategies affecting targets other than the mPTP [6]. Altogether, these data indicate that the protection exerted by β3AR selective stimulation involves the mPTP.
Pre-reperfusion β3AR agonist administration provides cardioprotection in a preclinical large animal model of AMI
A key finding of the present study is that pre-reperfusion β3AR-agonist administration reduces infarct size and improves long-term cardiac function in a more translational large animal (pig) model of AMI. Several novel therapies have demonstrated beneficial effects in preclinical studies but subsequently failed in the clinical arena. This poor translation between preclinical findings and clinical studies is in part due to the absence of randomized studies showing robust beneficial outcomes in large-animal models [46]. The pig model was selected because of its anatomical and physiological similarities to humans. To mimic a potential clinical scenario, we administered BRL37344 before coronary reperfusion and quantified infarct size by CMR, assessing the myocardial AAR to better define the protective effect of the intervention.
Taken together, our results show that a single i.v. administration of a β3AR agonist before reperfusion provides a powerful and highly translational cardioprotective therapy for AMI, and this beneficial effect is translated into long-term improvement in cardiac contractile function. In addition, we show that β3AR selective stimulation during IRI is associated with an increase in Akt phosphorylation and bioavailability of NO and ultimately in inhibition of lethal mitochondrial collapse upon restoration of blood flow (see Fig. 6).
Schematic mechanism through β3AR stimulation and the increase of cell viability by the inhibition of the opening of the mPTP. Following ischemia, reperfusion triggers accumulation reactive oxygen species (ROS). Excessive accumulation of ROS induces mitochondrial collapse, subsequent opening of the mPTP and the ultimate cell death. Here we report that a β3 selective agonist BRL37344 (BRL) exerts an Akt-eNOS-NO dependent effect on the cardiomyocytes which is translated into a delay in the opening of the mPTP and thus an increase in cell survival. Inhibition of bioavailability of NO with L-NAME abrogates the effect of BRL. eNOS endothelial nitric oxide synthase, NO nitric oxide, Akt-P Akt phosphorylation at ser473 during reperfusion
References
Aletras AH, Tilak GS, Natanzon A, Hsu LY, Gonzalez FM, Hoyt RF Jr, Arai AE (2006) Retrospective determination of the area at risk for reperfused acute myocardial infarction with t2-weighted cardiac magnetic resonance imaging: histopathological and displacement encoding with stimulated echoes (dense) functional validations. Circulation 113:1865–1870. doi:10.1161/CIRCULATIONAHA.105.576025
Alzaga AG, Cerdan M, Varon J (2006) Therapeutic hypothermia. Resuscitation 70:369–380. doi:10.1016/j.resuscitation.2006.01.017
Aragon JP, Condit ME, Bhushan S, Predmore BL, Patel SS, Grinsfelder DB, Gundewar S, Jha S, Calvert JW, Barouch LA, Lavu M, Wright HM, Lefer DJ (2011) Beta3-adrenoreceptor stimulation ameliorates myocardial ischemia–reperfusion injury via endothelial nitric oxide synthase and neuronal nitric oxide synthase activation. J Am Coll Cardiol 58:2683–2691. doi:10.1016/j.jacc.2011.09.033
Baines CP, Kaiser RA, Purcell NH, Blair NS, Osinska H, Hambleton MA, Brunskill EW, Sayen MR, Gottlieb RA, Dorn GW, Robbins J, Molkentin JD (2005) Loss of cyclophilin d reveals a critical role for mitochondrial permeability transition in cell death. Nature 434:658–662. doi:10.1038/nature03434
Bell R, Beeuwkes R, Botker HE, Davidson S, Downey J, Garcia-Dorado D, Hausenloy DJ, Heusch G, Ibanez B, Kitakaze M, Lecour S, Mentzer R, Miura T, Opie L, Ovize M, Ruiz-Meana M, Schulz R, Shannon R, Walker M, Vinten-Johansen J, Yellon D (2012) Trials, tribulations and speculation! Report from the 7th biennial hatter cardiovascular institute workshop. Basic Res Cardiol 107:300. doi:10.1007/s00395-012-0300-6
Bell RM, Kunuthur SP, Hendry C, Bruce-Hickman D, Davidson S, Yellon DM (2013) Matrix metalloproteinase inhibition protects cypd knockout mice independently of risk/mptp signalling: a parallel pathway to protection. Basic Res Cardiol 108:331. doi:10.1007/s00395-013-0331-7
Bhushan S, Kondo K, Predmore BL, Zlatopolsky M, King AL, Pearce C, Huang H, Tao YX, Condit ME, Lefer DJ (2012) Selective beta2-adrenoreceptor stimulation attenuates myocardial cell death and preserves cardiac function after ischemia–reperfusion injury. Arterioscler Thromb Vasc Biol 32:1865–1874. doi:10.1161/ATVBAHA.112.251769
Boengler K, Hilfiker-Kleiner D, Heusch G, Schulz R (2010) Inhibition of permeability transition pore opening by mitochondrial stat3 and its role in myocardial ischemia/reperfusion. Basic Res Cardiol 105:771–785. doi:10.1007/s00395-010-0124-1
Bohl S, Medway DJ, Schulz-Menger J, Schneider JE, Neubauer S, Lygate CA (2009) Refined approach for quantification of in vivo ischemia–reperfusion injury in the mouse heart. Am J Physiol Heart Circ Physiol 297:H2054–2058. doi:10.1152/ajpheart.00836.2009
Bolli R, Becker L, Gross G, Mentzer R Jr, Balshaw D, Lathrop DA (2004) Myocardial protection at a crossroads: the need for translation into clinical therapy. Circ Res 95:125–134. doi:10.1161/01.RES.0000137171.97172.d7
Botker HE, Kaltoft AK, Pedersen SF, Kim WY (2012) Measuring myocardial salvage. Cardiovasc Res 94:266–275. doi:10.1093/cvr/cvs081
Bundgaard H, Liu CC, Garcia A, Hamilton EJ, Huang Y, Chia KK, Hunyor SN, Figtree GA, Rasmussen HH (2010) Beta(3) adrenergic stimulation of the cardiac na+–k+ pump by reversal of an inhibitory oxidative modification. Circulation 122:2699–2708. doi:10.1161/CIRCULATIONAHA.110.964619
Burns RJ, Gibbons RJ, Yi Q, Roberts RS, Miller TD, Schaer GL, Anderson JL, Yusuf S (2002) The relationships of left ventricular ejection fraction, end-systolic volume index and infarct size to six-month mortality after hospital discharge following myocardial infarction treated by thrombolysis. J Am Coll Cardiol 39:30–36. doi:10.1016/S0735-1097(01)01711-9
Calvert JW, Condit ME, Aragon JP, Nicholson CK, Moody BF, Hood RL, Sindler AL, Gundewar S, Seals DR, Barouch LA, Lefer DJ (2011) Exercise protects against myocardial ischemia–reperfusion injury via stimulation of beta(3)-adrenergic receptors and increased nitric oxide signaling: Role of nitrite and nitrosothiols. Circ Res 108:1448–1458. doi:10.1161/CIRCRESAHA.111.241117
Crompton M (1999) The mitochondrial permeability transition pore and its role in cell death. Biochem J 341(Pt 2):233–249. doi:10.1042/0264-6021:3410233
Cruz-Adalia A, Jimenez-Borreguero LJ, Ramirez-Huesca M, Chico-Calero I, Barreiro O, Lopez-Conesa E, Fresno M, Sanchez-Madrid F, Martin P (2010) Cd69 limits the severity of cardiomyopathy after autoimmune myocarditis. Circulation 122:1396–1404. doi:10.1161/CIRCULATIONAHA.110.952820
Davidson SM, Hausenloy D, Duchen MR, Yellon DM (2006) Signalling via the reperfusion injury signalling kinase (risk) pathway links closure of the mitochondrial permeability transition pore to cardioprotection. Int J Biochem Cell Biol 38:414–419. doi:10.1016/j.biocel.2005.09.017
Davidson SM, Yellon DM, Murphy MP, Duchen MR (2012) Slow calcium waves and redox changes precede mitochondrial permeability transition pore opening in the intact heart during hypoxia and reoxygenation. Cardiovasc Res 93:445–453. doi:10.1093/cvr/cvr349
Duchen MR, McGuinness O, Brown LA, Crompton M (1993) On the involvement of a cyclosporin a sensitive mitochondrial pore in myocardial reperfusion injury. Cardiovasc Res 27:1790–1794. doi:10.1093/cvr/27.10.1790
Eltzschig HK, Eckle T (2011) Ischemia and reperfusion—from mechanism to translation. Nat Med 17:1391–1401. doi:10.1038/nm.2507
Frohlich GM, Meier P, White SK, Yellon DM, Hausenloy DJ (2013) Myocardial reperfusion injury: looking beyond primary pci. Eur Heart J 34:1714–1722. doi:10.1093/eurheartj/eht090
Gauthier C, Tavernier G, Charpentier F, Langin D, Le Marec H (1996) Functional beta3-adrenoceptor in the human heart. J Clin Invest 98:556–562. doi:10.1172/JCI118823
Gerczuk PZ, Kloner RA (2012) An update on cardioprotection: a review of the latest adjunctive therapies to limit myocardial infarction size in clinical trials. J Am Coll Cardiol 59:969–978. doi:10.1016/j.jacc.2011.07.054
Gomez L, Chavanis N, Argaud L, Chalabreysse L, Gateau-Roesch O, Ninet J, Ovize M (2005) Fas-independent mitochondrial damage triggers cardiomyocyte death after ischemia–reperfusion. Am J Physiol Heart Circ Physiol 289:H2153–2158. doi:10.1152/ajpheart.00165.2005
Guo Y, Flaherty MP, Wu WJ, Tan W, Zhu X, Li Q, Bolli R (2012) Genetic background, gender, age, body temperature, and arterial blood ph have a major impact on myocardial infarct size in the mouse and need to be carefully measured and/or taken into account: results of a comprehensive analysis of determinants of infarct size in 1,074 mice. Basic Res Cardiol 107:288. doi:10.1007/s00395-012-0288-y
Hausenloy DJ, Baxter G, Bell R, Botker HE, Davidson SM, Downey J, Heusch G, Kitakaze M, Lecour S, Mentzer R, Mocanu MM, Ovize M, Schulz R, Shannon R, Walker M, Walkinshaw G, Yellon DM (2010) Translating novel strategies for cardioprotection: the hatter workshop recommendations. Basic Res Cardiol 105:677–686. doi:10.1007/s00395-010-0121-4
Hausenloy DJ, Yellon DM (2006) Survival kinases in ischemic preconditioning and postconditioning. Cardiovasc Res 70:240–253. doi:10.1016/j.cardiores.2006.01.017
Heusch G (2011) Beta3-adrenoceptor activation just says no to myocardial reperfusion injury. J Am Coll Cardiol 58:2692–2694. doi:10.1016/j.jacc.2011.09.034
Heusch G (2013) Cardioprotection: chances and challenges of its translation to the clinic. Lancet 381:166–175. doi:10.1016/S0140-6736(12)60916-7
Heusch G, Boengler K, Schulz R (2008) Cardioprotection: nitric oxide, protein kinases, and mitochondria. Circulation 118:1915–1919. doi:10.1161/CIRCULATIONAHA.108.805242
Heusch G, Boengler K, Schulz R (2010) Inhibition of mitochondrial permeability transition pore opening: the holy grail of cardioprotection. Basic Res Cardiol 105:151–154. doi:10.1007/s00395-009-0080-9
Heusch G, Skyschally A, Schulz R (2011) The in situ pig heart with regional ischemia/reperfusion—ready for translation. J Mol Cell Cardiol 50:951–963. doi:10.1016/j.yjmcc.2011.02.016
Ibanez B, Cimmino G, Prat-Gonzalez S, Vilahur G, Hutter R, Garcia MJ, Fuster V, Sanz J, Badimon L, Badimon JJ (2011) The cardioprotection granted by metoprolol is restricted to its administration prior to coronary reperfusion. Int J Cardiol 147:428–432. doi:10.1016/j.ijcard.2009.09.551
Ibanez B, Fuster V, Macaya C, Sanchez-Brunete V, Pizarro G, Lopez-Romero P, Mateos A, Jimenez-Borreguero J, Fernandez-Ortiz A, Sanz G, Fernandez-Friera L, Corral E, Barreiro MV, Ruiz-Mateos B, Goicolea J, Hernandez-Antolin R, Acebal C, Garcia-Rubira JC, Albarran A, Zamorano JL, Casado I, Valenciano J, Fernandez-Vazquez F, de la Torre JM, Perez de Prado A, Iglesias-Vazquez JA, Martinez-Tenorio P, Iniguez A (2012) Study design for the “effect of metoprolol in cardioprotection during an acute myocardial infarction” (metocard-cnic): A randomized, controlled parallel-group, observer-blinded clinical trial of early pre-reperfusion metoprolol administration in st-segment elevation myocardial infarction. Am Heart J 164(473–480):e475. doi:10.1016/j.ahj.2012.07.020
Ibanez B, Prat-Gonzalez S, Speidl WS, Vilahur G, Pinero A, Cimmino G, Garcia MJ, Fuster V, Sanz J, Badimon JJ (2007) Early metoprolol administration before coronary reperfusion results in increased myocardial salvage: Analysis of ischemic myocardium at risk using cardiac magnetic resonance. Circulation 115:2909–2916. doi:10.1161/CIRCULATIONAHA.106.679639
Ibarra C, Vicencio JM, Estrada M, Lin Y, Rocco P, Rebellato P, Munoz JP, Garcia-Prieto J, Quest AF, Chiong M, Davidson SM, Bulatovic I, Grinnemo KH, Larsson O, Szabadkai G, Uhlen P, Jaimovich E, Lavandero S (2013) Local control of nuclear calcium signaling in cardiac myocytes by perinuclear microdomains of sarcolemmal insulin-like growth factor 1 receptors. Circ Res 112:236–245. doi:10.1161/CIRCRESAHA.112.273839
Kelley KW, Curtis SE, Marzan GT, Karara HM, Anderson CR (1973) Body surface area of female swine. J Anim Sci 36:927–930
Maroko PR, Kjekshus JK, Sobel BE, Watanabe T, Covell JW, Ross J Jr, Braunwald E (1971) Factors influencing infarct size following experimental coronary artery occlusions. Circulation 43:67–82. doi:10.1161/01.CIR.43.1.67
Niu X, Watts VL, Cingolani OH, Sivakumaran V, Leyton-Mange JS, Ellis CL, Miller KL, Vandegaer K, Bedja D, Gabrielson KL, Paolocci N, Kass DA, Barouch LA (2012) Cardioprotective effect of beta-3 adrenergic receptor agonism: role of neuronal nitric oxide synthase. J Am Coll Cardiol 59:1979–1987. doi:10.1016/j.jacc.2011.12.046
Nowosielski M, Schocke M, Mayr A, Pedarnig K, Klug G, Kohler A, Bartel T, Muller S, Trieb T, Pachinger O, Metzler B (2009) Comparison of wall thickening and ejection fraction by cardiovascular magnetic resonance and echocardiography in acute myocardial infarction. J Cardiovasc Magn Reson 11:22. doi:10.1186/1532-429X-11-22
Piot C, Croisille P, Staat P, Thibault H, Rioufol G, Mewton N, Elbelghiti R, Cung TT, Bonnefoy E, Angoulvant D, Macia C, Raczka F, Sportouch C, Gahide G, Finet G, Andre-Fouet X, Revel D, Kirkorian G, Monassier JP, Derumeaux G, Ovize M (2008) Effect of cyclosporine on reperfusion injury in acute myocardial infarction. N Engl J Med 359:473–481. doi:10.1056/NEJMoa071142
Piper HM, Garcia-Dorado D, Ovize M (1998) A fresh look at reperfusion injury. Cardiovasc Res 38:291–300. doi:10.1016/S0008-6363(98)00033-9
Rengo G, Zincarelli C, Femminella GD, Liccardo D, Pagano G, de Lucia C, Altobelli GG, Cimini V, Ruggiero D, Perrone-Filardi P, Gao E, Ferrara N, Lymperopoulos A, Koch WJ, Leosco D (2012) Myocardial beta(2)-adrenoceptor gene delivery promotes coordinated cardiac adaptive remodelling and angiogenesis in heart failure. Br J Pharmacol 166:2348–2361. doi:10.1111/j.1476-5381.2012.01954.x
Sambrano GR, Fraser I, Han H, Ni Y, O’Connell T, Yan Z, Stull JT (2002) Navigating the signalling network in mouse cardiac myocytes. Nature 420:712–714. doi:10.1038/nature01306
Schuster A, Kutty S, Padiyath A, Parish V, Gribben P, Danford DA, Makowski MR, Bigalke B, Beerbaum P, Nagel E (2011) Cardiovascular magnetic resonance myocardial feature tracking detects quantitative wall motion during dobutamine stress. J Cardiovasc Magn Reson 13:58. doi:10.1186/1532-429X-13-58
Schwartz Longacre L, Kloner RA, Arai AE, Baines CP, Bolli R, Braunwald E, Downey J, Gibbons RJ, Gottlieb RA, Heusch G, Jennings RB, Lefer DJ, Mentzer RM, Murphy E, Ovize M, Ping P, Przyklenk K, Sack MN, Vander Heide RS, Vinten-Johansen J, Yellon DM (2011) New horizons in cardioprotection: recommendations from the 2010 national heart, lung, and blood institute workshop. Circulation 124:1172–1179. doi:10.1161/CIRCULATIONAHA.111.032698
Sharma V, Bell RM, Yellon DM (2012) Targeting reperfusion injury in acute myocardial infarction: a review of reperfusion injury pharmacotherapy. Expert Opin Pharmacother 13:1153–1175. doi:10.1517/14656566.2012.685163
Skyschally A, Schulz R, Heusch G (2010) Cyclosporine a at reperfusion reduces infarct size in pigs. Cardiovasc Drugs Ther 24:85–87. doi:10.1007/s10557-010-6219-y
Yellon DM, Hausenloy DJ (2007) Myocardial reperfusion injury. N Engl J Med 357:1121–1135. doi:10.1056/NEJMra071667
Zhou YY, Wang SQ, Zhu WZ, Chruscinski A, Kobilka BK, Ziman B, Wang S, Lakatta EG, Cheng H, Xiao RP (2000) Culture and adenoviral infection of adult mouse cardiac myocytes: methods for cellular genetic physiology. Am J Physiol Heart Circ Physiol 279:H429–H436
Zorov DB, Filburn CR, Klotz LO, Zweier JL, Sollott SJ (2000) Reactive oxygen species (ros)-induced ros release: a new phenomenon accompanying induction of the mitochondrial permeability transition in cardiac myocytes. J Exp Med 192:1001–1014. doi:10.1084/jem.192.7.1001
Acknowledgments
We thank Dr. S. Mendez-Ferrer (CNIC) for supplying the β3AR knockout mice. We thank Rachel Dongworth, Rupa Parvin Khaton, and Virginia Zorita for the help and technical support. We also thank Ana V. Alonso for her outstanding technical support in mouse echocardiography and Gonzalo J. López and Angel Macías for theirs in swine CMR evaluations. We are grateful to the animal facilities at the CNIC and the UCL and to CNIC’s farm for their superb support with the animal care. Antonio M. Santos-Beneit provided advice in microscopy and image analysis. Simon Bartlett provided English editing.
CMR images were analyzed using dedicated software (QMass MR v.7) with support through a scientific collaboration with Medis medical imaging systems BV. Regional CMR analysis was conducted with TomTec 2D CPA MR Quantification Software with full support through scientific collaboration with Tomtec.
This work was supported by an award from the Fondo de Investigación Sanitaria to BI a (FIS 10/02268) and by the competitive grant “CNIC translational 01/2009”, also to BI.
D.S-R is supported by a CNIC-Postdoctoral Fellowship; JM.G-R and A.G-A were supported by CNIC-Cardiojoven Fellowships. The “Red de Investigación Cardiovascular (RIC)” of the Spanish Ministry of Health supports B.I (RD 12/0042/0054) and A.G-A. The “Centro Nacional de Investigaciones Cardiovasculares Carlos III (CNIC)” is supported by the Spanish Ministry of Economy and Competitiveness, and the Pro-CNIC Foundation.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Additional information
J. García-Prieto, J. M. García-Ruiz, and D. Sanz-Rosa contributed equally.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
García-Prieto, J., García-Ruiz, J.M., Sanz-Rosa, D. et al. β3 adrenergic receptor selective stimulation during ischemia/reperfusion improves cardiac function in translational models through inhibition of mPTP opening in cardiomyocytes. Basic Res Cardiol 109, 422 (2014). https://doi.org/10.1007/s00395-014-0422-0
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00395-014-0422-0