Abstract
The new coronavirus pandemic is affecting the entire world with more than 25 million confirmed cases in August 2020 according to the World Health Organization. It is known that the virus can affect several tissues and can progress to a respiratory failure in severe cases. To prevent the progression to this stage of the disease and minimize all the damage caused by coronavirus (SARS-CoV-2) the immune system must be in its integrity. A healthy nutritional status are fundamental to efficient immunological protection and consequently a good response to SARS-CoV-2. Micronutrients and bioactive compounds perform functions in immune cells that are extremely essential to stop SARS-CoV-2. Their adequate consumption is part of a non-pharmacological intervention to keep the immune system functioning. This review has as main objective to inform how micronutrients and bioactive compounds could act in the essential immunological pathways could stop SARS-CoV-2, focusing on the functions that have already established in the literature and transposing to this scenario.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), the new coronavirus pandemic, named by the World Health Organization (WHO) as coronavirus disease 2019 (COVID-19) has reached almost all countries or territories worldwide, with more than 25 million confirmed cases and more than 800 thousand deaths according to data published on the WHO website at August 31, 2020 [1]. The SARS-CoV-2 is an enveloped virus, nonsegmented, with a simple RNA strand, a phospholipid bilayer covered by “spike” glycoproteins, and its pathogenesis being studied by several researchers [2]. Figure 1 represents a schematic of the main structural components of the virus.

Adapted from Li et al. [2]
Structural scheme of the SARS-CoV-2.
Although the pathophysiological mechanisms associated with COVID 19 are not fully elucidated, Guan WJ and colleagues showed that not all people exposed to the SARS-Cov-2 will be infected and not all those infected will develop the most severe symptoms [3]. Based on that, the infected subject can be classified into three distinct stages, according to the symptoms and presence of the virus [4]. Stage 1 is related to the virus's incubation period, which can be detected or not, and with the absence of COVID-19′s symptoms as well. Stage 2 is the period when the virus can be detected and there are mild symptoms. Lastly, stage 3 represents the period that the subject has a high viral load and severe respiratory symptoms [4]. Besides the respiratory system, SARS-CoV-2 induced functional impairment was observed in the, nervous, cardiovascular and gastrointestinal systems [5, 6]. Once the integrity of the human immune system (IS) has a pivotal role to protect the body against the severity of the symptoms in the different systems the appropriate immune response (IR) is extremely necessary to control or to minimize the effects of the viral infection [2].
A healthy nutritional status are fundamental to efficient immunological protection. To ensure the IS functionality, the ideal contribution of macro and micronutrients should be taken into account [7, 8]. It has already been well established that during infection-induced energy demand increases, the adequate intake of carbohydrates, proteins, and lipids is essential for the activation of IS [7]. On the other hand, the malnutrition status is associated with IR commitment [7]. In addition to the macronutrients, micronutrients also have an important role in the IS. Even so, based on the dietary pattern, almost all subjects probably have a deficient intake of micronutrients, which may impair the performance of IS [7]. It is important to highlight that micronutrients act synergistically, in other words, the human body needs an adequate concentration of all micronutrients involved with the IR to guarantee the immune barrier of cells [8]. Other substances present in healthy nutrition, as some bioactive compounds, especially polyphenols, also play an important role in the IS, because of their antioxidant and anti-inflammatory properties [8]. They act by regulating immune cells, gene expression, and inhibiting certain pro-inflammatory cytokines [9]. Thus, both micronutrients and bioactive compounds might contribute to the adjuvant treatment of patients that have already infected with the SARS-CoV-2, since it targets specific IS cells, such as macrophage, NK cell and T cells [2] that could have responses potentiated by certain nutrients and bioactive compounds. This non-pharmacological intervention could help to decrease the severity of symptoms by modulating the host's IS.
It is important to note that, to the present moment, there is no solid information in the scientific literature showing how adequate nutrition status or specific food consumption could help to decrease SARS-CoV-2 spreads and control the COVID-19 current pandemic scenario progression. However, there are relevant evidences recent published showing the role of some micronutrients reducing risk of COVID-19 and other viral infections (e.g., Influenza), such as vitamin D [10,11,12,13], vitamin A, selenium, zinc [14, 15], copper [16] and vitamin C [17, 18].
A systematic review about potential interventions for COVID-19 suggests the importance of individually evaluation of nutritional status before administration of any treatment proposed [19], highlighting the synergic role of nutrients in IR. Besides, avoid nutritional deficiencies using effective and safe nutrition strategies may help to decrease the number of infected people [20].
Therefore, this review has as main objective to inform how micronutrients and bioactive compounds could act in the essential immunological pathways could stop SARS-CoV-2, focusing on the functions that have already established in the literature and transposing to this scenario.
Search strategy
Search strategy included PubMed using main keywords related to immunological responses, COVID-19, micronutrients and bioactive compounds (e.g., immune system, SARS-CoV-2, vitamins, minerals, polyphenols). Books and a food composition table complemented information about food sources, quantity and bioavailability of micronutrients and bioactive compounds. This review included COVID-19’s evidences published in the years 2019 and 2020. Also included micronutrients, bioactive compounds and immune responses articles published from the 1990s to 2020. In vivo (rodents and human experimental models) and in vitro studies were eligible when published in English or Portuguese. No systematic assessment and statistical analysis were performed.
Immunological responses and Covid-19
After the virus host invasion, the first recognition is made through the innate IS through pattern recognition receptors (PRRs), such as the retinoic acid-inducible gene I-like receptors [rig-I-like receptor (RLR)], which is responsible for recognizing viral genetic material [2, 21]. The inflammation cascade begins through the binding of SARS-CoV-2 to macrophages that consequently presents its antigens for TCD4 cells, generating their activation and also differentiation into T helper type 17 (Th17) cells, for example. Then, cytokines are produced to mobilize the entire adaptive IR. They are interleukins (IL) 1, 6, 8 and 21, tumor necrosis factor β (TNF-β), and monocyte chemoattractant protein-1 (MCP-1). These mediators stimulate T cells to activate natural killer cells (NK) and TCD8 cells [2]. TCD4 cells are responsible for producing specific antibodies to SARS-CoV-2 through the activation of B cells. TCD8 cells are important to viral control, since they are cytotoxic, playing a crucial role in the elimination of SARS-CoV-2 of the infected cells, and are associated with an immunological induction [2, 22].
To reach the cell's cytoplasm, the SARS-CoV-2 binds to a specific receptor, called dipeptidyl peptidase-4 (DPP4), through its spike glycoprotein (S), promoting adhesion between protein and receptor. To the viral genome presentation occurs, protein S needs to bind to the tool-like receptor (TLR)-4. The recognition of protein S triggers pro-inflammatory cytokines production through a primary response protein-dependent signaling pathway to myeloid differentiation factor-88 (MyD88). Then, it is observed the nuclear factor kappa B (NF-kB) activation, IL-1 and IL-6 production, in addition to type 1 interferon (IFN-1) and TNF-β [2].
Another pathway might be stimulated by binding viral RNA to the TLR-3 receptor, which induces the activation of inflammatory pathways through the interferon regulatory factors (IRF). Consequently, it culminates in IFN-1, IL-1, IL- 6, and TNF-β production as well. If the viral RNA binds to TLR-7 and/or TLR-9, it is also observed NF-kB and IRF activation. The presence of these cytokines attracts lymphocytes and leukocytes to the infected cell until the infection can be controlled [2]. It is important to highlight the role of IFN-1 in viral spread control. IFN-1 activate dendritic cells and NK, besides accelerate phagocytosis by macrophages of viral antigens [2, 21]. Figure 2 illustrates the process of immune activation.
Immune response to SARS-CoV-2. The scheme shows the main cells and cytokines involved in the immune defense mechanism against COVID-19 described in this review. SARS-CoV-2 severe acute respiratory syndrome coronavirus 2; NK cell natural killer cell; Th 17 T helper type 17; IL-1 Interleukin 1; IL-6 Interleukin 6; IL-8 Interleukin 8, IL-21 Interleukin 21, TNF-β tumor necrosis factor β, MCP-1 monocyte chemoattractant protein-1, DPP4 dipeptidyl peptidase-4; S protein spike glycoprotein; TLR-3 tool-like receptor—3; TLR-4 tool-like receptor—4; TLR-7 tool-like receptor—7; TLR-9 tool-like receptor—9; MyD88 myeloid differentiation factor-88; NF-kB nuclear factor kappa B; IRF interferon regulatory factors. Red lines refer to inhibitory effects. Green lines refer to activating effects.
If there is an impairment of the immune barrier and the virus spread cannot be contained, SARS-CoV-2 proliferates and affects, principally, tissues that have a high expression of the angiotensin-converting enzyme 2 (ACE 2), like kidneys, intestine, lungs, brain, and cardiovascular system [23, 24]. The virus affinity to ACE 2 may be an explanation for patients who died of multiple organ failure [23]. Recently, Cheng H and colleagues [25] showed that the virus is dependent on the ACE 2 expression in the respiratory epithelium to be able to penetrate and start its replication. Then, the damaged cells generate the inflammatory cascade described above, starting with the presentation of the virus to lymphocytes and ending with pro-inflammatory cytokines liberation. The pro-inflammatory macrophages and granulocytes-mediated IR culminates in respiratory disorders, the main symptom in the most severe stage of the COVID-19 [24, 26]. Pro-inflammatory cytokines such as IL-1, IL-6, and TNF are found in high concentrations in the infected patient's lungs and could be a possible trigger for the formation of pulmonary mucus and fibroblasts induction [23]. Thus, strategies that allow to block or to reduce those pro-inflammatory cytokines' actions can benefit patients in more advanced stages of COVID-19 [24].
Micronutrients
Once the scientific knowledge about the mechanisms and processes involved in cells and cytokines activation and production related to the SARS-CoV-2 immune responses was previously presented, it is important to understand how some micronutrients could be fundamental for the IS homeostasis during SARS-CoV-2 infection. Some micronutrients are related to inhibiting, stimulating, or acting as a cofactor to cells and cytokine altered by that virus. Therefore, this section brings together the main vitamins and minerals that contribute to IS function.
Vitamin A
Some previous scientific reviews highlighted the importance of vitamin A to the proper function of innate IS cells, as NK cells and macrophages [8, 27]. Besides that, vitamin A is fundamental for both T and B cell performance and the mechanism of antibody production in response to the specific antigen [28, 29].
In vivo evidences
Its deficiency is associated with the reduced number and functionality of NK cells and increases of INF γ, and intervenes negatively in phagocytic and macrophages activities as well in experimental study with rodents [30].Also, deficient levels of vitamin A could affect the differentiation and quantity of T cells, reducing the generation of antibodies and consequently decreasing the response to the virus in rodents [31, 32].
In vitro evidences
Deficient status of vitamin A negatively affects the differentiation in growth of B cells [33].
Vitamin B6
Similar to vitamin A, vitamin B6 participates in the production of antibodies and NK cell activity [27, 28, 34]. It is necessary for cytokines and endogenous amino acids the synthesis and metabolism [29].
In vivo evidences
Vitamin B6 also assists in inflammation regulation, maintaining Th 1 responses and the process of lymphocyte proliferation, differentiation, and maturation in experimental studies in rodents [35, 36]. Besides, higher levels of B6 active form decreases inflammation in humans [37]. Its deficiency can lead to lymphocytopenia and consequent immune deficiency, decreasing antibody-mediated responses as well [38].
Vitamin B7
Biotin (vitamin B7 or vitamin H) is an essential co-factor for five carboxylases, known as biotin-dependent carboxylases, involved in metabolism of several pathways such as gluconeogenesis, branched-chain amino acids metabolism and fatty acid synthesis [39, 40]. Metabolic disorders can lead to changes in IS responses and inflammatory process caused by biotin deficiency [39].
In vitro evidences
Previous research shows that biotin deficiency can affect immune responses, enhancing T CD4 lymphocytes in humans’ blood samples [41]. Consequently, leading to an increased level of IFN-γ, TNF and IL-17 and enhance of proinflammatory responses [41]. Besides, dendritic cells leads to Th1 and Th17 responses through increased production of proinflammatory cytokines when biotin levels are insufficient [42].
Vitamin B9
Vitamin B9 or folate is involved in the NK cells cytotoxicity maintenance and the production and metabolism of antibodies, enabling a sufficient antigen response to the antigen [26, 27, 29].
In vivo evidences
Animal and humans studies show folate deficiency association with depressive immune response, impairing, for example, the proliferation of T cells [38]. In rodent model antibody responses can be improper in this situation [29].
Vitamin B12
As vitamin B12 is a cofactor in folate metabolism, it indirectly contributes to the production and metabolism of antibodies [28, 29, 34].
In vivo evidences
An important immunomodulator, vitamin B12 is associated with cytotoxic cells, as NK and TCD8, facilitating its production and helping to regulate the proportion between helper and cytotoxic T cells in humans [43, 44].
Vitamin C
Vitamin C is widely known for its antioxidant and immunomodulatory properties, capable to protect lymphocytes from oxidative stress [29]. It is fundamental to other antioxidant compounds regeneration, as glutathione and vitamin E, enabling conversion to their active form [45].
In vivo evidences
Vitamin C deficiency is related to increases in cell oxidative damage and in the incidence and severity of pneumonia cases in humans [46, 47].
Vitamin C is also involved in maintaining and improving the activity of NK cells and their chemotaxis [27, 28, 48, 49], removal, and macrophages-mediated neutrophils apoptosis in rodents and humans [50]. Besides, it can stimulate the production, function, and movement of leukocytes to the infection site [29, 47].
In vitro evidences
Lastly, vitamin C plays a role in T cells production, differentiation, and proliferation of T cells, resulting in cytotoxic T cell production and in the increase in the antibodies generation [29, 48, 50].
Vitamin D
Vitamin D is one of the most widely studied micronutrient involved with the IS function. Vitamin D receptors can be found in innate IS cells such as macrophages, monocytes, and dendritic cells [29].
In vitro evidences
This vitamin is able to increase the differentiation of monocytes to macrophages [48] and in its active form (i.e. calcitriol), it is associated to promote the macrophages movement and phagocytic capacity, improving their oxidative potential [28, 51,52,53]. Furthermore, vitamin D stimulates the proliferation of the immune cells, increases the synthesis of superoxide, and helps to protect against infection caused by pathogens [29].
About the adaptive IS, vitamin D can induce suppression in the B cells antibodies production and T cell proliferation [29].
In vivo evidences
In addition, vitamin D is related to inhibit T cytotoxic and helper cell functions and to promote T regulatory T cell production [49, 54, 55]. It can reduce the expression of pro-inflammatory cytokines and increase anti-inflammatory cytokines in vitro and in vivo experimental models [29, 51, 56,57,58,59,60].
Its deficiency increases the susceptibility and severity to infections, especially acute respiratory tract infections, decreases the number of lymphocytes, and increases morbidity and mortality in children [46, 61].
Vitamin E
Besides the anti-inflammatory profile, vitamin E is an important antioxidant compound, protecting cells against free radicals [29, 48].
In vivo evidences
Among its anti-inflammatory functions, vitamin E improves NK cell activity, lymphocyte proliferation, and T cell-mediated functions, helping to build immune synapses between T helper cells. Indirectly, vitamin E protects T cell functions by decreasing the production of prostaglandin E2 (PGE2) by macrophages, which has immunosuppressive activity in several studies in animal models and humans [27, 28, 48, 49, 62, 63]. Its deficiency can impair adaptive immunity, affecting the functions of T and B cells [29].
Copper
Copper is a mineral that accumulates at the site of inflammation [29, 34]. As the zinc, copper is directly related to the enzyme superoxide dismutase (SOD), important in the defense against reactive oxygen species (ROS) [28]. Thus, it is considered a free radical scavenger, capable of maintaining an intracellular antioxidant balance [28, 64].
In vivo evidences
To react against the infectious agents, copper acts on macrophages, accumulating in their phagolysosomes and improves the NK activity in rats [65, 66].
In addition, it participates in the differentiation and proliferation of T cells, the production of antibodies, and cellular immunity in animal studies [34, 35]. Its deficiency can cause an abnormal decrease in neutrophils and increase the susceptibility to infections in humans [29, 67, 68].
Iron
Iron is involved in the production and action of inflammatory cytokines such as IFN-γ, TNF-α, IL-2, and IL-10 [48], and it is also important to generate ROS that kills the pathogen that infects IS [29].
In vitro evidences
In relation to the adaptive IS, iron is involved in the differentiation and proliferation of T cells and assists to regulate the proportion between T helper and cytotoxic T cells [29, 49].
In vivo evidences
An adequate plasmatic iron level is able to modulate the IS, reducing the M1 macrophage's pro-inflammatory response in mice [69, 70]. Its deficiency can reduce the immune response in humans [38, 70]
Magnesium
In vivo evidences
In humans, magnesium is associated with DNA protection against oxidative damage [71].
In vitro evidences
In high concentrations, magnesium reduces superoxide anion production [72]. It fundamental to bind the antigens to macrophage RNA, to regulate leukocyte activation, it is a cofactor for antibodies synthesis and is involved in the regulation of apoptosis [65, 66].
Selenium
This mineral is essential for the selenoproteins activity, which is important for the host's antioxidant defense [19].
In vivo evidences
Selenoproteins may affect the NK cells and leukocytes functions and potentially reduce the exaggerated ROS production during the oxidative stress [27, 29, 34, 48, 73].
Selenium also participates in T cell differentiation and proliferation, improves T helper cell counts and antibody levels [34, 64, 74]. Its deficiency can impair cellular and humoral immunity, besides increasing the virulence during viral infections in humans and rats studies [29, 46, 74, 75].
Zinc
Zinc is an important antioxidant agent against both ROS and reactive nitrogen species (RNS) [45, 47].
In vitro evidences
Zinc is essential for the intracellular tyrosine kinase binds to T cells receptors, promoting the T lymphocytes development and activation [45, 47]. Besides that, zinc induces the T cytotoxic cells proliferation and is involved in the development of regulatory T cells (Treg) [49, 76,77,78].
In vivo evidences
This mineral is also an anti-inflammatory agent, able to modulate cytokines release through the regulation of development of pro-inflammatory cells, such as Th17 and Th19, and of the production of cytokines, such as IL-2, IL-6, and TNF-α in several studies with humans and animals, besides in vitro evidences [49, 76,77,78,79,80,81]. It contributes to the maintenance and improvement of the cytotoxic activity of NK cells, in the monocytes phagocytic capacity, it helps in the TCD8 cells proliferation, and it influences the activity of antioxidant proteins [27,28,29, 47,48,49, 78, 82, 83].
Zinc is also involved in the antibodies production, mainly immunoglobulin G (IgG), and in its response in animal models [28, 78, 84, 85].
Finally, adequate levels of zinc are important to maintain the host's immunological defense [49]. Its deficiency is associated with impairment of total IS, affecting the number and function of lymphocytes, particularly T cells, and leads to altered production of cytokines that contribute to oxidative stress and inflammation [29]. It may be associated with an increase in viral (particularly pneumonia) and respiratory infections in humans [38, 46].
In order for all micronutrients to perform their functions, attention must be paid to its intake according to the recommended daily dietary intake (RDA) for healthy individuals, which considers the age range of each individual. Table 1 provides this information for adults, besides to compile the main functions in the IS and food sources of each micronutrient. It is worth mentioning that, the daily values of these micronutrients might be changed, with the necessity for greater amounts of these compounds to provide ideal immune support [8].
In addition, it is common an inadequate daily intake of vitamins and minerals, even when the accessibility to food is easy. For that case, supplementation may be necessary to improve specifics immune responses [8]. However, when this supplementation is in very high doses, it can cause unfavorable consequences for metabolism (e.g., hypervitaminosis) and IS, highlighting a bigger risk for vitamin A, iron and copper [29, 34]. To exemplify, in a small study with humans, high intake of copper for a long period was capable to reduce antibody production to an influenza vaccine [86].
If supplementation is necessary, it is important to respect safety limits previous established by Institute of Medicine (IOM) [8, 87]. Besides, it is essential to consult high quality studies previous published with consistent experimental design [8].
Bioactive compounds
Bioactive compounds are essential and nonessential compounds, widely found in fruits and vegetables [88]. They are responsible for colors, flavors, and they are related to potential pharmacological activities on human health [88, 89]. This compounds have many classifications, such as polyphenols, phytosterols, terpenoids, organosulfur compounds and alkaloids [90]. Many polyphenols have an important impact on IS through the immune cells modulation, the cytokines production, and pro-inflammatory genes expression [91, 92]. This section will present the main immune cells and pathways that are positively related to bioactive compounds.
Inflammation and oxidative stress
Some polyphenols are known for their anti-inflammatory potentials. According to in vivo and in human cells studies, resveratrol can inhibit pro-inflammatory cytokines, such as TNF-α and IL-6, while curcumin contributes to reducing TNF and IL-1. Curcumin also induces a reduction in NF-kB activation and in the TLR 2 and 4 expression [93,94,95,96,97,98,99]. In experimental designs using human cells, Epigallocatechin gallate (EGCG) and gingerol, present in green tea and ginger respectively, are other polyphenols that contribute to the NF-kb function [95, 100,101,102].
Polyphenols intake is directly associated with IS cell count and differentiation. Some studies in vitro, rodents and in humans experimental models observed alterations in the NK cells, macrophages, dendritic cells, Th1, and TCD4 cells count [91, 103,104,105]. Other types of T helper can be modulated, such as Th9 and Th17, by EGCG as well [106].
Several in vivo and in vitro studies show polyphenols’ anti-inflammatories properties that induce free radicals elimination, metal ions chelation, NADPH oxidase inhibition. The polyphenols contribute to the mitochondrial respiratory chain, they also induce a reduction in exaggerated ROS production, by inhibiting some enzymes involved and positively regulating antioxidant enzymes [9].
Regarding metals, curcumin can play a role in chelating transition metals, as Cu2+ and Fe2+, while quercetin and ECGC chelate Fe2+ in cell culture using THP1-monocytes [107]. Resveratrol and curcumin are the polyphenols that can inhibit NADPH oxidase in culture cells studies [108,109,110]. Curcumin, EGCG, phenolic acids, capsaicin, quercetin, anthocyanins, and resveratrol inhibit xanthine oxidase, an enzyme related to the ROS formation in mice and in vitro experiments [111,112,113,114,115,116]. Besides that, in vivo evidences, curcumin can stimulate the production of SOD, catalase, and glutathione peroxidase, antioxidant enzymes that are associated with decreases in ROS formation [117]. EGCG improves the activity of SOD and glutathione peroxidase, in vivo [118].
Cytokines modulation
Inflammatory cytokines modulation is one of the most studied mechanisms of polyphenols immunomodulation [9]. Their properties on macrophages were observed in an animal-model study with Chinese propolis administration in rodent “RAW 264.7” macrophages. The polyphenols present in Chinese propolis induced cyclooxygenase 2 (COX 2) and inducible nitric oxide synthase (iNOS) inhibition and a consequent reduction in the TNF-α, IL-1 β and IL-6 expression [119]. Similarly, this phenomenon was also observed when chamomile extract and quercetin alone were administrated [120]. Besides that, a clinical study highlighted that extra virgin olive oil has been related to reduce IL-6 and C-reactive protein (CRP) expression [121]. Quercetin and catechins have an effect on the balance of pro and anti-inflammatory cytokine production in vitro studies, increasing the IL-10 release and inhibiting TNF-α and IL-1 β [122, 123].
NF-kB signaling pathways
Polyphenols can modulate NF-kB at various points during the activation cascade, which induces an important anti-inflammatory effect through an alteration in the binding of the NF-kB complex to DNA, as an example [9]. In addition, in a previous study was observed a similar phenomenon when quercetin was administered in rodent BV-2 microglia cells [124]. Galangin, a flavonoid present in propolis, can control the NF-kB translocation and consequently decrease TNF-α, IL-6, IL-1β, and IL-8 expression [125]. At least in studies that were developed in cell culture, other polyphenols involved with NF-kB signaling pathways are resveratrol, catechins, and epicatechins [126, 127].
Besides that, it is important to highlight the role of EGCG on Wistar rat's respiratory epithelial cells NF-kb inhibition [128, 129], once it could improve the scientific knowledge between bioactive compounds properties and COVID-19 pandemic control.
Especially in virus infection, it is important to highlight a finding in human culture cell study and curcumin intervention [130]. This polyphenol provided an antiviral effect against enveloped viruses, inhibiting Zika and Chikungunya virus replication. This can be explained because curcumin may interferes with virus-cell binding, reducing its infectivity [130].
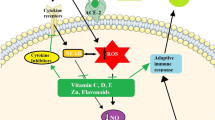
It is worth mentioning that only a healthy, varied, and fruits and vegetables-based diet is able to ensure exposure to all of these bioactive compounds [89]. In this way, an adequate supply of both bioactive compounds and micronutrients is guaranteed, as well as the synergy between vitamins and minerals [7, 8]. Table 2 provides a summary of the main functions of some bioactive compounds and the food sources in which they are found. To a better comprehension of all the mechanisms cited in this article, Fig. 3 shows which point of the SARS-CoV-2 infection pathway the main immunomodulatory polyphenols and micronutrients may act on.
Immune response to SARS-CoV-2 and micronutrients and polyphenols participation in the various cells and cytokines involved in the defense mechanisms. Polyphenols 1 resveratrol, curcumin, EGCG, gingerol, epicatechins, catechins, quercetin, propolis, Polyphenols 2 resveratrol, curcumin, EGCG, quercetin, anthocyanins; Polyphenols 3 resveratrol, curcumin, catechin, quercetin, olive oil, chamomile extract, propolis; Polyphenol 4 curcumin; Polyphenol 5 EGCG; Polyphenol 6 propolis. SARS-CoV-2 severe acute respiratory syndrome coronavirus 2; NK cell natural killer cell; Th 17 T helper type 17; IL-1 Interleukin 1; IL-6 Interleukin 6, IL-8 Interleukin 8; IL-21 Interleukin 21; TNF-β tumor necrosis factor β; MCP-1 monocyte chemoattractant protein-1, DPP4 dipeptidyl peptidase-4; S protein spike glycoprotein; TLR-3 tool-like receptor—3; TLR-4 tool-like receptor—4; TLR-7 tool-like receptor—7; TLR-9 tool-like receptor—s9; MyD88 myeloid differentiation factor-88; NF-kB nuclear factor kappa B; IRF interferon regulatory factors; ROS reactive oxygen species. Red lines refer to inhibitory effects. Green lines refer to activating effects
Immune system and elderly
Aging is a natural and complex process associated with uncountable human body physiological alterations, such as reductions in bone and muscle mass, in the basal metabolism rate (BMR), and total body water. Aging is also related to teeth loos, which can cause damage to the chewing, saliva production decrease, and dysphagia [131]. In this population, these changes also affect the immune system, a process characterized by immunosenescence, which can be defined as a reduced ability to respond to "foreign" antigens and to tolerate self-antigens. Thus, immunosenescence would be associated with a greater susceptibility to infections (including COVID-19), to cancer, to vaccination failure, and to autoimmune diseases [132].
Immunosenescence induces both the innate and adaptive IS modification and is associated with persistent low-grade inflammation. As the men have a more severe age-related immune function alteration than women, they suffer more from its effects [133]. Age-related decrease in phagocytosis, antigens presentation, in immune cells cytotoxic potential, lymphocyte number and function, are observed in this population. Besides that, these changes make the elderly more susceptible to infections, affect the ability to respond to pathogens and cause an exacerbation of the symptoms of these infections [134].
Decreased function of the thymus (an important lymphocyte maturation organ) and the loss of function and differentiation capacity of hematopoietic stem cells are some of them are some hypotheses that attempt to explain the aging-related immune function decline. It is also known that lifestyle during adulthood can directly influence this process: food, nutritional status, physical activity, social isolation, smoking, exposure to alcohol and drugs are factors that affect the degree of decline in the IS in the elderly [27]. The maintenance of an adequate nutritional status, a satisfactory supply of macro and micronutrients, ingestion of bioactive compounds, and the regular practice of physical activity can positively modulate the immune response of these individuals. Besides that, nutritional status can be highlighted as a vital condition for a healthy IS operation. Studies report that elderly people with protein-calorie malnutrition have a lower IR compared to those with adequate nutritional status [134].
In addition to protein-calorie malnutrition, commonly observed in aging, attention should be paid to the micronutrient supply of this a group. Although energy requirements to the elderly are lower, the micronutrients (vitamins and minerals) recommendation remains almost unchanged. Frequently, old people ingest less food than what was recommended, it can induce micronutrients deficiency and consequent impairment of IS and IR. Adequate dietary guidance and possible supplementation could be tools to prevent and/or reverse deficiencies of these nutrients [27].
Vitamin D deficiency, which is quite prevalent in the general population and especially in the elderly, induces impaired immune responses to influenza vaccination [135]. The literature also shows that vitamin D supplementation is associated with improving the immune response of patients with this vitamin deficiency [136]. Konijeti et al. [136] and Hemilä [137] demonstrated that vitamin E supplementation may be able to reduce the incidence of pneumonia in adult and elderly men [137]. Bouamama et al. [138] indicated that vitamins C and E supplementation improved the T lymphocytes response in the elderly and could contribute to the prevention of age-related immune system impairment.
In addition to a higher infection incidence, the elderly are more susceptible to prolonged infections, exacerbated symptoms, and complications. More than half of the elderly with a common cold develop a respiratory disease (e.g. pneumonia) and they have more than tenfold chances of death when compared to young adults. Since the beginning of the COVID-19 pandemic, advanced age has been highlighted as a risk factor for both susceptibilities to symptoms and to the infection outcome. In this way, death a common finding in individuals over 70 years and are associated with age-related physiological changes in IS [27, 139].
In Italy, approximately 87% of the first 2,000 cases of deaths were over 70 years old [140]. Another study compared the mortality rate between American elderly residents [mean 83 (range 51–100) years] and healthy workers and visitors [mean: 43 (range 21–79) years] of a long-term care institution that were positively diagnosed with SARS-CoV-2. The researchers found that 34% of elderly residents and 0% of workers die due to Covid-19. These results show that the disease affects the elderly more severely [140, 141]. Thus, special attention should be given to elderly individuals and to how to improve their immune system, especially those with other risk factors. In this scenario, adequate dietary planning that provides nutritional support within the current recommendations could contribute to a more competent IR, which can result in better chances of SARS-CoV-2 prevention and treatment. During more severe infection episodes, the elderly may have an increased requirement for these nutrients and it might be necessary to evaluate their supplementation.
Final considerations
The literature shows that some infected individuals have their sense of smell and taste affected [142] it is in turn associated with food intake reduction and lack of appetite. Based on that, the elaboration of the specific guidelines is interesting to help with a better understanding between nutrition and current COVID-19 pandemic treatment. For example, it is important to know which foods are better tolerated, respecting the individual's preference. Another example is to stimulate the consumption of harvest fruits and vegetables, once their flavor is more prominent. Besides that, other important nutritional strategies are to add natural spices in the preparation, to do memory exercise regarding the preparation that will be ingested and improving its acceptance, and to make the patient aware of the importance of their food for the correct IS function and the consequent response to COVID-19 [142].
Based on all information present in this review, in conclusion, a healthy, varied, and vegetables and fruits-based diet is important to ensure the IS balance and the consequent IR to SARS-CoV-2. It is worth mentioning the essential role of a qualified nutrition scientist to prescribe individualized guidance that considers a previous disease historic, nutritional status, and age as well.
References
Organization WH (2020) WHO, National Health Commission of the People’s Republic of China https://covid19.who.int/. Accessed 31 Aug 2020
Li G, Fan Y, Lai Y, Han T, Li Z, Zhou P, Pan P, Wang W, Hu D, Liu X, Zhang Q, Wu J (2020) Coronavirus infections and immune responses. J Med Virol 92(4):424–432. https://doi.org/10.1002/jmv.25685
Guan WJ, Ni ZY, Hu Y, Liang WH, Ou CQ, He JX, Liu L, Shan H, Lei CL, Hui DSC, Du B, Li LJ, Zeng G, Yuen KY, Chen RC, Tang CL, Wang T, Chen PY, Xiang J, Li SY, Wang JL, Liang ZJ, Peng YX, Wei L, Liu Y, Hu YH, Peng P, Wang JM, Liu JY, Chen Z, Li G, Zheng ZJ, Qiu SQ, Luo J, Ye CJ, Zhu SY, Zhong NS, China Medical Treatment Expert Group for C (2020) Clinical characteristics of coronavirus disease 2019 in China. N Engl J Med 382(18):1708–1720. https://doi.org/10.1056/NEJMoa2002032
Wang D, Hu B, Hu C, Zhu F, Liu X, Zhang J, Wang B, Xiang H, Cheng Z, Xiong Y, Zhao Y, Li Y, Wang X, Peng Z (2020) Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus-infected pneumonia in Wuhan, China. JAMA. https://doi.org/10.1001/jama.2020.1585
Cui J, Li F, Shi ZL (2019) Origin and evolution of pathogenic coronaviruses. Nat Rev Microbiol 17(3):181–192. https://doi.org/10.1038/s41579-018-0118-9
Madjid M, Safavi-Naeini P, Solomon SD, Vardeny O (2020) Potential effects of coronaviruses on the cardiovascular system: a review. JAMA Cardiol. https://doi.org/10.1001/jamacardio.2020.1286
Childs CE, Calder PC, Miles EA (2019) Diet and immune function. Nutrients. https://doi.org/10.3390/nu11081933
Gombart AF, Pierre A, Maggini S (2020) A review of micronutrients and the immune system-working in harmony to reduce the risk of infection. Nutrients. https://doi.org/10.3390/nu12010236
Yahfoufi N, Alsadi N, Jambi M, Matar C (2018) The immunomodulatory and anti-inflammatory role of polyphenols. Nutrients 10(11):1618. https://doi.org/10.3390/nu10111618
Grant WB, Lahore H, McDonnell SL, Baggerly CA, French CB, Aliano JL, Bhattoa HP (2020) Evidence that vitamin D supplementation could reduce risk of influenza and COVID-19 infections and deaths. Nutrients 12(4):988. https://doi.org/10.3390/nu12040988
Jakovac H (2020) COVID-19 and vitamin D-Is there a link and an opportunity for intervention? Am J Physiol Endocrinol Metab 318(5):E589. https://doi.org/10.1152/ajpendo.00138.2020
Panarese A, Shahini E (2020) Letter: COVID-19, and vitamin D. Aliment Pharmacol Ther 51(10):993–995. https://doi.org/10.1111/apt.15752
Mitchell F (2020) Vitamin-D and COVID-19: do deficient risk a poorer outcome? Lancet Diabetes Endocrinol 8(7):570. https://doi.org/10.1016/S2213-8587(20)30183-2
Jayawardena R, Sooriyaarachchi P, Chourdakis M, Jeewandara C, Ranasinghe P (2020) Enhancing immunity in viral infections, with special emphasis on COVID-19: a review. Diabetes Metab Syndr 14(4):367–382. https://doi.org/10.1016/j.dsx.2020.04.015
Zhang J, Taylor EW, Bennett K, Saad R, Rayman MP (2020) Association between regional selenium status and reported outcome of COVID-19 cases in China. Am J Clin Nutr 111(6):1297–1299. https://doi.org/10.1093/ajcn/nqaa095
Andreou A, Trantza S, Filippou D, Sipsas N, Tsiodras S (2020) COVID-19: The potential role of copper and N-acetylcysteine (NAC) in a combination of candidate antiviral treatments against SARS-CoV-2. Vivo 34(3 Suppl):1567–1588. https://doi.org/10.21873/invivo.11946
Carr AC (2020) A new clinical trial to test high-dose vitamin C in patients with COVID-19. Crit Care 24(1):133. https://doi.org/10.1186/s13054-020-02851-4
Colunga Biancatelli RML, Berrill M, Catravas JD, Marik PE (2020) Quercetin and vitamin C: an experimental, synergistic therapy for the prevention and treatment of SARS-CoV-2 related disease (COVID-19). Front Immunol 11:1451. https://doi.org/10.3389/fimmu.2020.01451
Zhang L, Liu Y (2020) Potential interventions for novel coronavirus in China: a systematic review. J Med Virol 92(5):479–490. https://doi.org/10.1002/jmv.25707
Richardson DP, Lovegrove JA (2020) Nutritional status of micronutrients as a possible and modifiable risk factor for COVID-19: a UK perspective. Br J Nutr. https://doi.org/10.1017/S000711452000330X
Yi Y, Lagniton PNP, Ye S, Li E, Xu RH (2020) COVID-19: what has been learned and to be learned about the novel coronavirus disease. Int J Biol Sci 16(10):1753–1766. https://doi.org/10.7150/ijbs.45134
Cecere TE, Todd SM, Leroith T (2012) Regulatory T cells in arterivirus and coronavirus infections: do they protect against disease or enhance it? Viruses 4(5):833–846. https://doi.org/10.3390/v4050833
Guo W, Li M, Dong Y, Zhou H, Zhang Z, Tian C, Qin R, Wang H, Shen Y, Du K, Zhao L, Fan H, Luo S, Hu D (2020) Diabetes is a risk factor for the progression and prognosis of COVID-19. Diabetes Metab Res Rev. https://doi.org/10.1002/dmrr.3319
Shi Y, Wang Y, Shao C, Huang J, Gan J, Huang X, Bucci E, Piacentini M, Ippolito G, Melino G (2020) COVID-19 infection: the perspectives on immune responses. Cell Death Differ 27(5):1451–1454. https://doi.org/10.1038/s41418-020-0530-3
Cheng H, Wang Y, Wang GQ (2020) Organ-protective effect of angiotensin-converting enzyme 2 and its effect on the prognosis of COVID-19. J Med Virol. https://doi.org/10.1002/jmv.25785
Xu Z, Shi L, Wang Y, Zhang J, Huang L, Zhang C, Liu S, Zhao P, Liu H, Zhu L, Tai Y, Bai C, Gao T, Song J, Xia P, Dong J, Zhao J, Wang FS (2020) Pathological findings of COVID-19 associated with acute respiratory distress syndrome. Lancet Respir Med 8(4):420–422. https://doi.org/10.1016/S2213-2600(20)30076-X
Maggini S, Pierre A, Calder PC (2018) Immune function and micronutrient requirements change over the life course. Nutrients 10(10):1531. https://doi.org/10.3390/nu10101531
Maggini SBS, Sorbara JP, Senatore G (2018) Feeding the immune system: the role of micronutrients in restoring resistance to infections. Cab Rev Perspect Agric Vet Sci Nutr Nat Resour 3:1–21. https://doi.org/10.1079/PAVSNNR20083098
Center MI (2016) Immunity in depth. Linus Pauling Institute. https://lpi.oregonstate.edu/mic/health-disease/immunity. Accessed 3 May 2020
Chang HK, Hou WS (2015) Retinoic acid modulates interferon-gamma production by hepatic natural killer T cells via phosphatase 2A and the extracellular signal-regulated kinase pathway. J Interferon Cytokine Res 35(3):200–212. https://doi.org/10.1089/jir.2014.0098
Tan X, Sande JL, Pufnock JS, Blattman JN, Greenberg PD (2011) Retinoic acid as a vaccine adjuvant enhances CD8+ T cell response and mucosal protection from viral challenge. J Virol 85(16):8316–8327. https://doi.org/10.1128/JVI.00781-11
Hall JA, Cannons JL, Grainger JR, Dos Santos LM, Hand TW, Naik S, Wohlfert EA, Chou DB, Oldenhove G, Robinson M, Grigg ME, Kastenmayer R, Schwartzberg PL, Belkaid Y (2011) Essential role for retinoic acid in the promotion of CD4(+) T cell effector responses via retinoic acid receptor alpha. Immunity 34(3):435–447. https://doi.org/10.1016/j.immuni.2011.03.003
Blomhoff HK, Smeland EB, Erikstein B, Rasmussen AM, Skrede B, Skjonsberg C, Blomhoff R (1992) Vitamin A is a key regulator for cell growth, cytokine production, and differentiation in normal B cells. J Biol Chem 267(33):23988–23992
Saeed FN, Muhammad; Ahmed, Rabia; Nadeem, muhammad kashif; Arshad, Muhammad Sajid; Ullah, Azmat, (2016) Studying the impact of nutritional immunology underlying the modulation of immune responses by nutritional compounds—a review. Food Agric Immunol 27:205–229. https://doi.org/10.1080/09540105.2015.1079600
Maggini S, Wintergerst ES, Beveridge S, Hornig DH (2007) Selected vitamins and trace elements support immune function by strengthening epithelial barriers and cellular and humoral immune responses. Br J Nutr 98(Suppl 1):S29-35. https://doi.org/10.1017/S0007114507832971
Ueland PM, McCann A, Midttun O, Ulvik A (2017) Inflammation, vitamin B6 and related pathways. Mol Asp Med 53:10–27. https://doi.org/10.1016/j.mam.2016.08.001
Huang SC, Wei JC, Wu DJ, Huang YC (2010) Vitamin B(6) supplementation improves pro-inflammatory responses in patients with rheumatoid arthritis. Eur J Clin Nutr 64(9):1007–1013. https://doi.org/10.1038/ejcn.2010.107
Calder P, Prescott S, Caplan M (2007) Scientific review: the role of nutrients in immune function of infants and young children. emerging evidence for long-chain polyunsaturated fatty acids. Mead Johnson Company, pp 1–35. http://eprints.soton.ac.uk/id/eprint/152657
Kuroishi T (2015) Regulation of immunological and inflammatory functions by biotin. Can J Physiol Pharmacol 93(12):1091–1096. https://doi.org/10.1139/cjpp-2014-0460
Leon-Del-Rio A (2019) Biotin in metabolism, gene expression, and human disease. J Inherit Metab Dis 42(4):647–654. https://doi.org/10.1002/jimd.12073
Elahi A, Sabui S, Narasappa NN, Agrawal S, Lambrecht NW, Agrawal A, Said HM (2018) Biotin deficiency Induces Th1- and Th17-mediated proinflammatory responses in human CD4(+) T lymphocytes via activation of the mTOR signaling pathway. J Immunol 200(8):2563–2570. https://doi.org/10.4049/jimmunol.1701200
Agrawal S, Agrawal A, Said HM (2016) Biotin deficiency enhances the inflammatory response of human dendritic cells. Am J Physiol Cell Physiol 311(3):C386-391. https://doi.org/10.1152/ajpcell.00141.2016
Erkurt MA, Aydogdu I, Dikilitas M, Kuku I, Kaya E, Bayraktar N, Ozhan O, Ozkan I, Sonmez A (2008) Effects of cyanocobalamin on immunity in patients with pernicious anemia. Med Princ Pract 17(2):131–135. https://doi.org/10.1159/000112967
Tamura J, Kubota K, Murakami H, Sawamura M, Matsushima T, Tamura T, Saitoh T, Kurabayshi H, Naruse T (1999) Immunomodulation by vitamin B12: augmentation of CD8+ T lymphocytes and natural killer (NK) cell activity in vitamin B12-deficient patients by methyl-B12 treatment. Clin Exp Immunol 116(1):28–32. https://doi.org/10.1046/j.1365-2249.1999.00870.x
Wintergerst ES, Maggini S, Hornig DH (2006) Immune-enhancing role of vitamin C and zinc and effect on clinical conditions. Ann Nutr Metab 50(2):85–94. https://doi.org/10.1159/000090495
Prentice S (2017) They are what you eat: can nutritional factors during gestation and early infancy modulate the neonatal immune response? Front Immunol 8:1641. https://doi.org/10.3389/fimmu.2017.01641
Hemila H (2017) Vitamin C and infections. Nutrients. https://doi.org/10.3390/nu9040339
Budi Haryanto TS, Wintergerst E, Maggini S (2015) Multivitamin supplementation supports immune function and ameliorates conditions triggered by reduced air quality. Vitam Min 4(2):1–15
Wu D, Lewis ED, Pae M, Meydani SN (2018) Nutritional modulation of immune function: analysis of evidence, mechanisms, and clinical relevance. Front Immunol 9:3160. https://doi.org/10.3389/fimmu.2018.03160
Carr AC, Maggini S (2017) Vitamin C and immune function. Nutrients. https://doi.org/10.3390/nu9111211
Wishart K (2017) Increased micronutrient requirements during physiologically demanding situations: review of the current evidence. Vitam Min 6(2):1–16
Sly LM, Lopez M, Nauseef WM, Reiner NE (2001) 1alpha,25-Dihydroxyvitamin D3-induced monocyte antimycobacterial activity is regulated by phosphatidylinositol 3-kinase and mediated by the NADPH-dependent phagocyte oxidase. J Biol Chem 276(38):35482–35493. https://doi.org/10.1074/jbc.M102876200
Tanaka H, Hruska KA, Seino Y, Malone JD, Nishii Y, Teitelbaum SL (1991) Disassociation of the macrophage-maturational effects of vitamin D from respiratory burst priming. J Biol Chem 266(17):10888–10892
Sassi F, Tamone C, D’Amelio P (2018) Vitamin D: nutrient, hormone, and immunomodulator. Nutrients. https://doi.org/10.3390/nu10111656
Cantorna MT, Snyder L, Lin YD, Yang L (2015) Vitamin D and 1,25(OH)2D regulation of T cells. Nutrients 7(4):3011–3021. https://doi.org/10.3390/nu7043011
Lin Z, Li W (2016) The roles of vitamin D and its analogs in inflammatory diseases. Curr Top Med Chem 16(11):1242–1261. https://doi.org/10.2174/1568026615666150915111557
Zhang Y, Leung DY, Richers BN, Liu Y, Remigio LK, Riches DW, Goleva E (2012) Vitamin D inhibits monocyte/macrophage proinflammatory cytokine production by targeting MAPK phosphatase-1. J Immunol 188(5):2127–2135. https://doi.org/10.4049/jimmunol.1102412
Topilski I, Flaishon L, Naveh Y, Harmelin A, Levo Y, Shachar I (2004) The anti-inflammatory effects of 1,25-dihydroxyvitamin D3 on Th2 cells in vivo are due in part to the control of integrin-mediated T lymphocyte homing. Eur J Immunol 34(4):1068–1076. https://doi.org/10.1002/eji.200324532
Cantorna MT, Woodward WD, Hayes CE, DeLuca HF (1998) 1,25-dihydroxyvitamin D3 is a positive regulator for the two anti-encephalitogenic cytokines TGF-beta 1 and IL-4. J Immunol 160(11):5314–5319
Gregori S, Giarratana N, Smiroldo S, Uskokovic M, Adorini L (2002) A 1alpha,25-dihydroxyvitamin D(3) analog enhances regulatory T-cells and arrests autoimmune diabetes in NOD mice. Diabetes 51(5):1367–1374. https://doi.org/10.2337/diabetes.51.5.1367
Wayse V, Yousafzai A, Mogale K, Filteau S (2004) Association of subclinical vitamin D deficiency with severe acute lower respiratory infection in Indian children under 5 y. Eur J Clin Nutr 58(4):563–567. https://doi.org/10.1038/sj.ejcn.1601845
Wu D, Meydani SN (2014) Age-associated changes in immune function: impact of vitamin E intervention and the underlying mechanisms. Endocr Metab Immune Disord Drug Targets 14(4):283–289. https://doi.org/10.2174/1871530314666140922143950
Moriguchi S, Muraga M (2000) Vitamin E and immunity. Vitam Horm 59:305–336. https://doi.org/10.1016/s0083-6729(00)59011-6
Alpert PT (2017) The role of vitamins and minerals on the immune system. Home Health Care Manag Pract 29(3):199–202
Besold AN, Culbertson EM, Culotta VC (2016) The Yin and Yang of copper during infection. J Biol Inorg Chem 21(2):137–144. https://doi.org/10.1007/s00775-016-1335-1
Institute of Medicine (US) Committee on Military Nutrition Research (1999) Military strategies for sustainment of nutrition and immune function in the field. National Academies Press (US), Washington (DC). 16, Trace Minerals, Immune Function, and Viral Evolution. Available from: https://www.ncbi.nlm.nih.gov/books/NBK230971/
Kelley DS, Daudu PA, Taylor PC, Mackey BE, Turnlund JR (1995) Effects of low-copper diets on human immune response. Am J Clin Nutr 62(2):412–416. https://doi.org/10.1093/ajcn/62.2.412
Percival SS (1998) Copper and immunity. Am J Clin Nutr 67(5 Suppl):1064S-1068S. https://doi.org/10.1093/ajcn/67.5.1064S
Agoro R, Taleb M, Quesniaux VFJ, Mura C (2018) Cell iron status influences macrophage polarization. PLoS ONE 13(5):e0196921. https://doi.org/10.1371/journal.pone.0196921
Hassan TH, Badr MA, Karam NA, Zkaria M, El Saadany HF, Abdel Rahman DM, Shahbah DA, Al Morshedy SM, Fathy M, Esh AM, Selim AM (2016) Impact of iron deficiency anemia on the function of the immune system in children. Medicine (Baltim) 95(47):e5395. https://doi.org/10.1097/MD.0000000000005395
Petrovic J, Stanic D, Dmitrasinovic G, Plecas-Solarovic B, Ignjatovic S, Batinic B, Popovic D, Pesic V (2016) Magnesium supplementation diminishes peripheral blood lymphocyte DNA oxidative damage in athletes and sedentary young man. Oxid Med Cell Longev 2016:2019643. https://doi.org/10.1155/2016/2019643
Bussiere FI, Mazur A, Fauquert JL, Labbe A, Rayssiguier Y, Tridon A (2002) High magnesium concentration in vitro decreases human leukocyte activation. Magnes Res 15(1–2):43–48
Baum MK, Shor-Posner G, Lai S, Zhang G, Lai H, Fletcher MA, Sauberlich H, Page JB (1997) High risk of HIV-related mortality is associated with selenium deficiency. J Acquir Immune Defic Syndr Hum Retrovirol 15(5):370–374. https://doi.org/10.1097/00042560-199708150-00007
Hurwitz BE, Klaus JR, Llabre MM, Gonzalez A, Lawrence PJ, Maher KJ, Greeson JM, Baum MK, Shor-Posner G, Skyler JS, Schneiderman N (2007) Suppression of human immunodeficiency virus type 1 viral load with selenium supplementation: a randomized controlled trial. Arch Intern Med 167(2):148–154. https://doi.org/10.1001/archinte.167.2.148
Arthur JR, McKenzie RC, Beckett GJ (2003) Selenium in the immune system. J Nutr 133(5 Suppl 1):1457S-1459S. https://doi.org/10.1093/jn/133.5.1457S
Kitabayashi C, Fukada T, Kanamoto M, Ohashi W, Hojyo S, Atsumi T, Ueda N, Azuma I, Hirota H, Murakami M, Hirano T (2010) Zinc suppresses Th17 development via inhibition of STAT3 activation. Int Immunol 22(5):375–386. https://doi.org/10.1093/intimm/dxq017
Maywald M, Wang F, Rink L (2018) Zinc supplementation plays a crucial role in T helper 9 differentiation in allogeneic immune reactions and non-activated T cells. J Trace Elem Med Biol 50:482–488. https://doi.org/10.1016/j.jtemb.2018.02.004
Fraker PJ, King LE, Laakko T, Vollmer TL (2000) The dynamic link between the integrity of the immune system and zinc status. J Nutr 130(5S Suppl):1399S-1406S. https://doi.org/10.1093/jn/130.5.1399S
Jarosz M, Olbert M, Wyszogrodzka G, Mlyniec K, Librowski T (2017) Antioxidant and anti-inflammatory effects of zinc. Zinc-dependent NF-kappaB signaling. Inflammopharmacology 25(1):11–24. https://doi.org/10.1007/s10787-017-0309-4
Foster M, Samman S (2012) Zinc and regulation of inflammatory cytokines: implications for cardiometabolic disease. Nutrients 4(7):676–694. https://doi.org/10.3390/nu4070676
Wessels I, Rink L (2020) Micronutrients in autoimmune diseases: possible therapeutic benefits of zinc and vitamin D. J Nutr Biochem 77:108240. https://doi.org/10.1016/j.jnutbio.2019.108240
Sheikh A, Shamsuzzaman S, Ahmad SM, Nasrin D, Nahar S, Alam MM, Al Tarique A, Begum YA, Qadri SS, Chowdhury MI, Saha A, Larson CP, Qadri F (2010) Zinc influences innate immune responses in children with enterotoxigenic Escherichia coli-induced diarrhea. J Nutr 140(5):1049–1056. https://doi.org/10.3945/jn.109.111492
Wintergerst ES, Maggini S, Hornig DH (2007) Contribution of selected vitamins and trace elements to immune function. Ann Nutr Metab 51(4):301–323. https://doi.org/10.1159/000107673
Shankar AH, Prasad AS (1998) Zinc and immune function: the biological basis of altered resistance to infection. Am J Clin Nutr 68(2 Suppl):447S-463S. https://doi.org/10.1093/ajcn/68.2.447S
Ibs KH, Rink L (2003) Zinc-altered immune function. J Nutr 133(5 Suppl 1):1452S-1456S. https://doi.org/10.1093/jn/133.5.1452S
Roberfroid MB (2000) Prebiotics and probiotics: are they functional foods? Am J Clin Nutr 71 (6 Suppl):1682S–1687S; discussion 1688S–1690S. https://doi.org/10.1093/ajcn/71.6.1682S
Medicine Io (2011) Dietary reference intakes for calcium and vitamin D. In: Ross AC, Taylor CL, Yaktine AL, Del Valle HB (eds) Dietary reference intakes for calcium and vitamin D. The national academies collection: reports funded by National Institutes of Health, Washington (DC). https://doi.org/10.17226/13050
Biesalski HK, Dragsted LO, Elmadfa I, Grossklaus R, Muller M, Schrenk D, Walter P, Weber P (2009) Bioactive compounds: definition and assessment of activity. Nutrition 25(11–12):1202–1205. https://doi.org/10.1016/j.nut.2009.04.023
Recio MC, Andujar I, Rios JL (2012) Anti-inflammatory agents from plants: progress and potential. Curr Med Chem 19(14):2088–2103. https://doi.org/10.2174/092986712800229069
Somani SJ, Modi KP, Majumdar AS, Sadarani BN (2015) Phytochemicals and their potential usefulness in inflammatory bowel disease. Phytother Res 29(3):339–350. https://doi.org/10.1002/ptr.5271
Karasawa K, Uzuhashi Y, Hirota M, Otani H (2011) A matured fruit extract of date palm tree (Phoenix dactylifera L) stimulates the cellular immune system in mice. J Agric Food Chem 59(20):11287–11293. https://doi.org/10.1021/jf2029225
John CM, Sandrasaigaran P, Tong CK, Adam A, Ramasamy R (2011) Immunomodulatory activity of polyphenols derived from Cassia auriculata flowers in aged rats. Cell Immunol 271(2):474–479. https://doi.org/10.1016/j.cellimm.2011.08.017
Capiralla H, Vingtdeux V, Venkatesh J, Dreses-Werringloer U, Zhao H, Davies P, Marambaud P (2012) Identification of potent small-molecule inhibitors of STAT3 with anti-inflammatory properties in RAW 264.7 macrophages. FEBS J 279(20):3791–3799. https://doi.org/10.1111/j.1742-4658.2012.08739.x
Leiherer A, Mundlein A, Drexel H (2013) Phytochemicals and their impact on adipose tissue inflammation and diabetes. Vascul Pharmacol 58(1–2):3–20. https://doi.org/10.1016/j.vph.2012.09.002
Siddiqui AM, Cui X, Wu R, Dong W, Zhou M, Hu M, Simms HH, Wang P (2006) The anti-inflammatory effect of curcumin in an experimental model of sepsis is mediated by up-regulation of peroxisome proliferator-activated receptor-gamma. Crit Care Med 34(7):1874–1882. https://doi.org/10.1097/01.CCM.0000221921.71300.BF
Marchiani A, Rozzo C, Fadda A, Delogu G, Ruzza P (2014) Curcumin and curcumin-like molecules: from spice to drugs. Curr Med Chem 21(2):204–222. https://doi.org/10.2174/092986732102131206115810
Noorafshan A, Ashkani-Esfahani S (2013) A review of therapeutic effects of curcumin. Curr Pharm Des 19(11):2032–2046
Gupta SC, Prasad S, Kim JH, Patchva S, Webb LJ, Priyadarsini IK, Aggarwal BB (2011) Multitargeting by curcumin as revealed by molecular interaction studies. Nat Prod Rep 28(12):1937–1955. https://doi.org/10.1039/c1np00051a
Bae J-S (2012) Role of high mobility group box 1 in inflammatory disease: focus on sepsis. Arch Pharmacal Res 35:1511–1523
Kanwar J, Taskeen M, Mohammad I, Huo C, Chan TH, Dou QP (2012) Recent advances on tea polyphenols. Front Biosci (Elite Ed) 4:111–131. https://doi.org/10.2741/363
Domitrovic R (2011) The molecular basis for the pharmacological activity of anthocyans. Curr Med Chem 18(29):4454–4469. https://doi.org/10.2174/092986711797287601
Singh BN, Shankar S, Srivastava RK (2011) Green tea catechin, epigallocatechin-3-gallate (EGCG): mechanisms, perspectives and clinical applications. Biochem Pharmacol 82(12):1807–1821. https://doi.org/10.1016/j.bcp.2011.07.093
Sakaguchi S, Miyara M, Costantino CM, Hafler DA (2010) FOXP3+ regulatory T cells in the human immune system. Nat Rev Immunol 10(7):490–500. https://doi.org/10.1038/nri2785
Boissier MC, Assier E, Biton J, Denys A, Falgarone G, Bessis N (2009) Regulatory T cells (Treg) in rheumatoid arthritis. Jt Bone Spine 76(1):10–14. https://doi.org/10.1016/j.jbspin.2008.08.002
Robinson DS, Larche M, Durham SR (2004) Tregs and allergic disease. J Clin Investig 114(10):1389–1397. https://doi.org/10.1172/JCI23595
Wang J, Pae M, Meydani SN, Wu D (2013) Green tea epigallocatechin-3-gallate modulates differentiation of naive CD4(+) T cells into specific lineage effector cells. J Mol Med (Berl) 91(4):485–495. https://doi.org/10.1007/s00109-012-0964-2
Heim KE, Tagliaferro AR, Bobilya DJ (2002) Flavonoid antioxidants: chemistry, metabolism and structure-activity relationships. J Nutr Biochem 13(10):572–584. https://doi.org/10.1016/s0955-2863(02)00208-5
Deby-Dupont G, Mouithys-Mickalad A, Serteyn D, Lamy M, Deby C (2005) Resveratrol and curcumin reduce the respiratory burst of Chlamydia-primed THP-1 cells. Biochem Biophys Res Commun 333(1):21–27. https://doi.org/10.1016/j.bbrc.2005.05.073
Chow SE, Hshu YC, Wang JS (1985) Chen JK (2007) Resveratrol attenuates oxLDL-stimulated NADPH oxidase activity and protects endothelial cells from oxidative functional damages. J Appl Physiol 102(4):1520–1527. https://doi.org/10.1152/japplphysiol.00881.2006
Petronio MS, Zeraik ML, Fonseca LM, Ximenes VF (2013) Apocynin: chemical and biophysical properties of a NADPH oxidase inhibitor. Molecules 18(3):2821–2839. https://doi.org/10.3390/molecules18032821
Shen L, Ji HF (2009) Insights into the inhibition of xanthine oxidase by curcumin. Bioorg Med Chem Lett 19(21):5990–5993. https://doi.org/10.1016/j.bmcl.2009.09.076
Aucamp J, Gaspar A, Hara Y, Apostolides Z (1997) Inhibition of xanthine oxidase by catechins from tea (Camellia sinensis). Anticancer Res 17(6D):4381–4385
Schmidt AP, Bohmer AE, Antunes C, Schallenberger C, Porciuncula LO, Elisabetsky E, Lara DR, Souza DO (2009) Anti-nociceptive properties of the xanthine oxidase inhibitor allopurinol in mice: role of A1 adenosine receptors. Br J Pharmacol 156(1):163–172. https://doi.org/10.1111/j.1476-5381.2008.00025.x
Nguyen MT, Nguyen NT (2012) Xanthine oxidase inhibitors from Vietnamese Blumea balsamifera L. Phytother Res 26(8):1178–1181. https://doi.org/10.1002/ptr.3710
Braunlich M, Slimestad R, Wangensteen H, Brede C, Malterud KE, Barsett H (2013) Extracts, anthocyanins and procyanidins from Aronia melanocarpa as radical scavengers and enzyme inhibitors. Nutrients 5(3):663–678. https://doi.org/10.3390/nu5030663
Huang XF, Li HQ, Shi L, Xue JY, Ruan BF, Zhu HL (2008) Synthesis of resveratrol analogues, and evaluation of their cytotoxic and xanthine oxidase inhibitory activities. Chem Biodivers 5(4):636–642. https://doi.org/10.1002/cbdv.200890059
Sporn MB, Liby KT (2012) NRF2 and cancer: the good, the bad and the importance of context. Nat Rev Cancer 12(8):564–571. https://doi.org/10.1038/nrc3278
Chu AJ (2014) Antagonism by bioactive polyphenols against inflammation: a systematic view. Inflamm Allergy Drug Targets 13(1):34–64. https://doi.org/10.2174/1871528112666131119211002
Gonzalez R, Ballester I, Lopez-Posadas R, Suarez MD, Zarzuelo A, Martinez-Augustin O, Sanchez de Medina F (2011) Effects of flavonoids and other polyphenols on inflammation. Crit Rev Food Sci Nutr 51(4):331–362. https://doi.org/10.1080/10408390903584094
Drummond EM, Harbourne N, Marete E, Martyn D, Jacquier J, O’Riordan D, Gibney ER (2013) Inhibition of proinflammatory biomarkers in THP1 macrophages by polyphenols derived from chamomile, meadowsweet and willow bark. Phytother Res 27(4):588–594. https://doi.org/10.1002/ptr.4753
Fito M, Cladellas M, de la Torre R, Marti J, Munoz D, Schroder H, Alcantara M, Pujadas-Bastardes M, Marrugat J, Lopez-Sabater MC, Bruguera J, Covas MI, Investigators S (2008) Anti-inflammatory effect of virgin olive oil in stable coronary disease patients: a randomized, crossover, controlled trial. Eur J Clin Nutr 62(4):570–574. https://doi.org/10.1038/sj.ejcn.1602724
Comalada M, Ballester I, Bailon E, Sierra S, Xaus J, Galvez J, de Medina FS, Zarzuelo A (2006) Inhibition of pro-inflammatory markers in primary bone marrow-derived mouse macrophages by naturally occurring flavonoids: analysis of the structure-activity relationship. Biochem Pharmacol 72(8):1010–1021. https://doi.org/10.1016/j.bcp.2006.07.016
Crouvezier S, Powell B, Keir D, Yaqoob P (2001) The effects of phenolic components of tea on the production of pro- and anti-inflammatory cytokines by human leukocytes in vitro. Cytokine 13(5):280–286. https://doi.org/10.1006/cyto.2000.0837
Chen JC, Ho FM, Pei-Dawn Lee C, Chen CP, Jeng KC, Hsu HB, Lee ST, Wen Tung W, Lin WW (2005) Inhibition of iNOS gene expression by quercetin is mediated by the inhibition of IkappaB kinase, nuclear factor-kappa B and STAT1, and depends on heme oxygenase-1 induction in mouse BV-2 microglia. Eur J Pharmacol 521(1–3):9–20. https://doi.org/10.1016/j.ejphar.2005.08.005
Kim HH, Bae Y, Kim SH (2013) Galangin attenuates mast cell-mediated allergic inflammation. Food Chem Toxicol 57:209–216. https://doi.org/10.1016/j.fct.2013.03.015
Mackenzie GG, Carrasquedo F, Delfino JM, Keen CL, Fraga CG, Oteiza PI (2004) Epicatechin, catechin, and dimeric procyanidins inhibit PMA-induced NF-kappaB activation at multiple steps in Jurkat T cells. FASEB J 18(1):167–169. https://doi.org/10.1096/fj.03-0402fje
Carluccio MA, Siculella L, Ancora MA, Massaro M, Scoditti E, Storelli C, Visioli F, Distante A, De Caterina R (2003) Olive oil and red wine antioxidant polyphenols inhibit endothelial activation: antiatherogenic properties of Mediterranean diet phytochemicals. Arterioscler Thromb Vasc Biol 23(4):622–629. https://doi.org/10.1161/01.ATV.0000062884.69432.A0
Wheeler DS, Catravas JD, Odoms K, Denenberg A, Malhotra V, Wong HR (2004) Epigallocatechin-3-gallate, a green tea-derived polyphenol, inhibits IL-1 beta-dependent proinflammatory signal transduction in cultured respiratory epithelial cells. J Nutr 134(5):1039–1044. https://doi.org/10.1093/jn/134.5.1039
Aneja R, Hake PW, Burroughs TJ, Denenberg AG, Wong HR, Zingarelli B (2004) Epigallocatechin, a green tea polyphenol, attenuates myocardial ischemia reperfusion injury in rats. Mol Med 10(1–6):55–62. https://doi.org/10.2119/2004-00032.aneja
Richart SM, Li YL, Mizushina Y, Chang YY, Chung TY, Chen GH, Tzen JT, Shia KS, Hsu WL (2018) Synergic effect of curcumin and its structural analogue (Monoacetylcurcumin) on anti-influenza virus infection. J Food Drug Anal 26(3):1015–1023. https://doi.org/10.1016/j.jfda.2017.12.006
Mahan LK, Escott-stump S, Raymond JL (2013) Krause: Alimentos, Nutrição e Dietoterapia, 13th edn. Elsevier, Rio de Janeiro, p 1228
Leroux J, Morrison K, Rosenberg M (2018) Prevalence and Predictors of Food Insecurity among Older People in Canada. Int J Environ Res Public Health. https://doi.org/10.3390/ijerph15112511
Fulop T, Dupuis G, Witkowski JM, Larbi A (2016) The role of immunosenescence in the development of age-related diseases. Rev Invest Clin 68(2):84–91
Maijo M, Clements SJ, Ivory K, Nicoletti C, Carding SR (2014) Nutrition, diet and immunosenescence. Mech Ageing Dev 136–137:116–128. https://doi.org/10.1016/j.mad.2013.12.003
Goncalves-Mendes N, Talvas J, Duale C, Guttmann A, Corbin V, Marceau G, Sapin V, Brachet P, Evrard B, Laurichesse H, Vasson MP (2019) Impact of vitamin D supplementation on influenza vaccine response and immune functions in deficient elderly persons: a randomized placebo-controlled trial. Front Immunol 10:65. https://doi.org/10.3389/fimmu.2019.00065
Konijeti GG, Arora P, Boylan MR, Song Y, Huang S, Harrell F, Newton-Cheh C, O’Neill D, Korzenik J, Wang TJ, Chan AT (2016) Vitamin D supplementation modulates T cell-mediated immunity in humans: results from a randomized control trial. J Clin Endocrinol Metab 101(2):533–538. https://doi.org/10.1210/jc.2015-3599
Hemila H (2016) Vitamin E administration may decrease the incidence of pneumonia in elderly males. Clin Interv Aging 11:1379–1385. https://doi.org/10.2147/CIA.S114515
Bouamama S, Merzouk H, Medjdoub A, Merzouk-Saidi A, Merzouk SA (2017) Effects of exogenous vitamins A, C, and E and NADH supplementation on proliferation, cytokines release, and cell redox status of lymphocytes from healthy aged subjects. Appl Physiol Nutr Metab 42(6):579–587. https://doi.org/10.1139/apnm-2016-0201
Wu Z, McGoogan JM (2020) Characteristics of and important lessons from the coronavirus disease 2019 (COVID-19) outbreak in China: summary of a report of 72314 cases from the Chinese Center for Disease Control and Prevention. JAMA. https://doi.org/10.1001/jama.2020.2648
Livingston E, Bucher K (2020) Coronavirus disease 2019 (COVID-19) in Italy. JAMA. https://doi.org/10.1001/jama.2020.4344
McMichael TM, Currie DW, Clark S, Pogosjans S, Kay M, Schwartz NG, Lewis J, Baer A, Kawakami V, Lukoff MD, Ferro J, Brostrom-Smith C, Rea TD, Sayre MR, Riedo FX, Russell D, Hiatt B, Montgomery P, Rao AK, Chow EJ, Tobolowsky F, Hughes MJ, Bardossy AC, Oakley LP, Jacobs JR, Stone ND, Reddy SC, Jernigan JA, Honein MA, Clark TA, Duchin JS (2020) Epidemiology of Covid-19 in a long-term care facility in King County, Washington. N Engl J Med. https://doi.org/10.1056/NEJMoa2005412
Beltran-Corbellini A, Chico-Garcia JL, Martinez-Poles J, Rodriguez-Jorge F, Natera-Villalba E, Gomez-Corral J, Gomez-Lopez A, Monreal E, Parra-Diaz P, Cortes-Cuevas JL, Galan JC, Fragola-Arnau C, Porta-Etessam J, Masjuan J, Alonso-Canovas A (2020) Acute-onset smell and taste disorders in the context of Covid-19: a pilot multicenter PCR-based case-control study. Eur J Neurol. https://doi.org/10.1111/ene.14273
Tabela brasileira de composição de alimentos (2011) NEPA – UNICAMP, 4th edn. rev. e ampl. NEPA- UNICAMP, Campinas, p 161
Cozzolino SMF (2016) Biodisponibilidade de Nutrientes, 5th edn. Manoele, Barueri, p 1443
Meydani SN, Ribaya-Mercado JD, Russell RM, Sahyoun N, Morrow FD, Gershoff SN (1991) Vitamin B-6 deficiency impairs interleukin 2 production and lymphocyte proliferation in elderly adults. Am J Clin Nutr 53(5):1275–1280. https://doi.org/10.1093/ajcn/53.5.1275
Verbon EH, Trapet PL, Stringlis IA, Kruijs S, Bakker P, Pieterse CMJ (2017) Iron and Immunity. Annu Rev Phytopathol 55:355–375. https://doi.org/10.1146/annurev-phyto-080516-035537
Cassat JE, Skaar EP (2013) Iron in infection and immunity. Cell Host Microbe 13(5):509–519. https://doi.org/10.1016/j.chom.2013.04.010
Grober U, Schmidt J, Kisters K (2015) Magnesium in Prevention and Therapy. Nutrients 7(9):8199–8226. https://doi.org/10.3390/nu7095388
Avery JC, Hoffmann PR (2018) Selenium, Selenoproteins, and Immunity. Nutrients. https://doi.org/10.3390/nu10091203
Guillin OM, Vindry C, Ohlmann T, Chavatte L (2019) Selenium, Selenoproteins and Viral Infection. Nutrients. https://doi.org/10.3390/nu11092101
Tanumihardjo SA, Russell RM, Stephensen CB, Gannon BM, Craft NE, Haskell MJ, Lietz G, Schulze K, Raiten DJ (2016) Biomarkers of nutrition for development (BOND)-vitamin A review. J Nutr 146(9):1816S-1848S. https://doi.org/10.3945/jn.115.229708
Mahalanabis D, Lahiri M, Paul D, Gupta S, Gupta A, Wahed MA, Khaled MA (2004) Randomized, double-blind, placebo-controlled clinical trial of the efficacy of treatment with zinc or vitamin A in infants and young children with severe acute lower respiratory infection. Am J Clin Nutr 79(3):430–436. https://doi.org/10.1093/ajcn/79.3.430
Monacelli F, Acquarone E, Giannotti C, Borghi R, Nencioni A (2017) Vitamin C, aging and Alzheimer’s disease. Nutrients. https://doi.org/10.3390/nu9070670
Mousavi S, Bereswill S, Heimesaat MM (2019) Immunomodulatory and antimicrobial effects of vitamin C. Eur J Microbiol Immunol (Bp) 9(3):73–79. https://doi.org/10.1556/1886.2019.00016
Medrano M, Carrillo-Cruz E, Montero I, Perez-Simon JA (2018) Vitamin D: Effect on Haematopoiesis and Immune System and Clinical Applications. Int J Mol Sci. https://doi.org/10.3390/ijms19092663
Kakodkar P, Kaka N, Baig MN (2020) A comprehensive literature review on the clinical presentation, and management of the pandemic Coronavirus disease 2019 (COVID-19). Cureus 12(4):e7560. https://doi.org/10.7759/cureus.7560
Laaksi I, Ruohola JP, Tuohimaa P, Auvinen A, Haataja R, Pihlajamaki H, Ylikomi T (2007) An association of serum vitamin D concentrations < 40 nmol/L with acute respiratory tract infection in young Finnish men. Am J Clin Nutr 86(3):714–717. https://doi.org/10.1093/ajcn/86.3.714
Lee GY, Han SN (2018) The role of vitamin E in immunity. Nutrients. https://doi.org/10.3390/nu10111614
Maares M, Haase H (2016) Zinc and immunity: an essential interrelation. Arch Biochem Biophys 611:58–65. https://doi.org/10.1016/j.abb.2016.03.022
Bonaventura P, Benedetti G, Albarede F, Miossec P (2015) Zinc and its role in immunity and inflammation. Autoimmun Rev 14(4):277–285. https://doi.org/10.1016/j.autrev.2014.11.008
de Moura RS, Resende AC (2016) Cardiovascular and metabolic effects of acai, an Amazon plant. J Cardiovasc Pharmacol 68(1):19–26. https://doi.org/10.1097/FJC.0000000000000347
Aranha LN, Silva MG, Uehara SK, Luiz RR, Nogueira Neto JF, Rosa G, Moraes de Oliveira GM (2020) Effects of a hypoenergetic diet associated with acai (Euterpe oleracea Mart) pulp consumption on antioxidant status, oxidative stress and inflammatory biomarkers in overweight, dyslipidemic individuals. Clin Nutr 39(5):1464–1469. https://doi.org/10.1016/j.clnu.2019.06.008
Colunga Biancatelli RML, Berrill M, Marik PE (2020) The antiviral properties of vitamin C. Expert Rev Anti Infect Ther 18(2):99–101. https://doi.org/10.1080/14787210.2020.1706483
Kamei M, Nishimura H, Takahashi T, Takahashi N, Inokuchi K, Mato T, Takahashi K (2016) Anti-influenza virus effects of cocoa. J Sci Food Agric 96(4):1150–1158. https://doi.org/10.1002/jsfa.7197
Martins TF, Palomino OM, Alvarez-Cilleros D, Martin MA, Ramos S, Goya L (2020) Cocoa flavanols protect human endothelial cells from oxidative stress. Plant Foods Hum Nutr. https://doi.org/10.1007/s11130-020-00807-1
El-Saber Batiha G, Magdy Beshbishy A, Wasef LG, et al (2020) Chemical constituents and pharmacological activities of garlic (Allium sativum L.): a review. Nutrients 12(3):872. https://doi.org/10.3390/nu12030872
Zhen H, Fang F, Ye DY, Shu SN, Zhou YF, Dong YS, Nie XC, Li G (2006) Experimental study on the action of allitridin against human cytomegalovirus in vitro: Inhibitory effects on immediate-early genes. Antiviral Res 72(1):68–74. https://doi.org/10.1016/j.antiviral.2006.03.017
Majewski M (2014) Allium sativum: facts and myths regarding human health. Rocz Panstw Zakl Hig 65(1):1–8
Anh NH, Kim SJ, Long NP, Min JE, Yoon YC, Lee EG, Kim M, Kim TJ, Yang YY, Son EY, Yoon SJ, Diem NC, Kim HM, Kwon SW (2020) Ginger on human health: a comprehensive systematic review of 109 randomized controlled trials. Nutrients 12(1):57. https://doi.org/10.3390/nu12010157
Kulkarni RA, Deshpande AR (2016) Anti-inflammatory and antioxidant effect of ginger in tuberculosis. J Complement Integr Med 13(2):201–206. https://doi.org/10.1515/jcim-2015-0032
Malaguarnera L (2019) Influence of resveratrol on the immune response. Nutrients. https://doi.org/10.3390/nu11050946
Lin SC, Ho CT, Chuo WH, Li S, Wang TT, Lin CC (2017) Effective inhibition of MERS-CoV infection by resveratrol. BMC Infect Dis 17(1):144. https://doi.org/10.1186/s12879-017-2253-8
Rosa DD, Dias MMS, Grzeskowiak LM, Reis SA, Conceicao LL, Peluzio M (2017) Milk kefir: nutritional, microbiological and health benefits. Nutr Res Rev 30(1):82–96. https://doi.org/10.1017/S0954422416000275
Maciel FR, Punaro GR, Rodrigues AM, Bogsan CS, Rogero MM, Oliveira MN, Mouro MG, Higa EM (2016) Immunomodulation and nitric oxide restoration by a probiotic and its activity in gut and peritoneal macrophages in diabetic rats. Clin Nutr 35(5):1066–1072. https://doi.org/10.1016/j.clnu.2015.07.018
Che L, Zhou Q, Liu Y, Hu L, Peng X, Wu C, Zhang R, Tang J, Wu F, Fang Z, Lin Y, Xu S, Feng B, Li J, Jiang P, Wu CD (2019) Flaxseed oil supplementation improves intestinal function and immunity, associated with altered intestinal microbiome and fatty acid profile in pigs with intrauterine growth retardation. Food Funct 10(12):8149–8160. https://doi.org/10.1039/c9fo01877h
Hosomi K, Kiyono H, Kunisawa J (2019) Fatty acid metabolism in the host and commensal bacteria for the control of intestinal immune responses and diseases. Gut Microbes. https://doi.org/10.1080/19490976.2019.1612662
Caroprese M, Ciliberti MG, Albenzio M, Annicchiarico G, Sevi A (2015) Dietary polyunsaturated fatty acids from flaxseed affect immune responses of dairy sheep around parturition. Vet Immunol Immunopathol 168(1–2):56–60. https://doi.org/10.1016/j.vetimm.2015.08.006
Takeda K, Nagamatsu K, Okumura K (2018) A water-soluble derivative of propolis augments the cytotoxic activity of natural killer cells. J Ethnopharmacol 218:51–58. https://doi.org/10.1016/j.jep.2018.02.035
Al-Hariri M (2019) Immune’s-boosting agent: Immunomodulation potentials of propolis. J Fam Community Med 26(1):57–60. https://doi.org/10.4103/jfcm.JFCM_46_18
Zeitoun R, Najjar F, Wehbi B, Khalil A, Fayyad-Kazan M, Dagher-Hamalian C, Faour WH, El-Makhour Y (2019) Chemical composition, antioxidant and anti-inflammatory activity evaluation of the Lebanese propolis extract. Curr Pharm Biotechnol 20(1):84–96. https://doi.org/10.2174/1389201020666190206201241
Mounce BC, Cesaro T, Carrau L, Vallet T, Vignuzzi M (2017) Curcumin inhibits Zika and chikungunya virus infection by inhibiting cell binding. Antiviral Res 142:148–157. https://doi.org/10.1016/j.antiviral.2017.03.014
Moghadamtousi SZ, Kadir HA, Hassandarvish P, Tajik H, Abubakar S, Zandi K (2014) A review on antibacterial, antiviral, and antifungal activity of curcumin. Biomed Res Int 2014:186864. https://doi.org/10.1155/2014/186864
Acknowledgements
We thank all the health professionals and researchers for all the support and care in the face of this pandemic. We also thank the Coordination of Superior Level Staff Improvement (CAPES—Brazil) for supporting graduate studies and providing us with scholarships to do research.
Funding
This article did not receive any sources of funding.
Author information
Authors and Affiliations
Contributions
JASM and PRS: Conceptualization; investigation process; writing, review and editing; visualization; project administration. LM FC—Investigation process; writing, review and editing; visualization; project administration. JDM—Writing, review and editing; translation. GSR and RFM Conceptualization; investigation process; writing, review and editing; visualization; project administration, supervision.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there are no conflicts of interest.
Rights and permissions
About this article
Cite this article
Arruda de Souza Monnerat, J., Ribeiro de Souza, P., Monteiro da Fonseca Cardoso, L. et al. Micronutrients and bioactive compounds in the immunological pathways related to SARS-CoV-2 (adults and elderly). Eur J Nutr 60, 559–579 (2021). https://doi.org/10.1007/s00394-020-02410-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-020-02410-1