Abstract
Background
Proteoglycans (PGs) are important constituents of the plasma membrane and of the basement membrane supporting the endothelial cell layer. Changes in the amounts or the structures of PGs in the endothelium may affect important functions such as turnover of lipoproteins, filtration properties, and regulation of chemokines during inflammation, which are all relevant in diabetes.
Aim of the study
The purpose of this study was to investigate if hyperglycemic conditions would affect the biosynthesis and secretion of PGs in cultured primary human endothelial cells.
Methods
Primary human umbilical cord vein endothelial cells were established and cultured in vitro. The cells were cultured either in medium with low glucose (LG) (1 g/l) or high glucose (HG) (4.5 g/l). From day 3–4 cells were labeled with 35S-sulfate for 24 h. 35S-Labeled macromolecules (medium) were purified by gel chromatography, and isolated macromolecules were analyzed by gel chromatography after different types of treatment, electrophoresis, and immunoprecipitation.
Results
Lower levels of secreted PGs were found in human endothelial cells exposed to HG. The major part of the PGs released was of the heparan sulfate (HS) type, and immunoprecipitation experiments showed that one such PG was syndecan-1. However, there was no difference in the ratio between HS and chondroitin sulfate (CS) under the different experimental conditions. Further, the PGs expressed neither differ with regard to molecular size of the glycosaminoglycan (GAG) chains, nor were their polyanionic properties affected by the different experimental conditions.
Conclusion:
The results obtained suggest that treatment of primary human endothelial cells with hyperglycemia leads to a decrease in PG secretion in primary cultures of human endothelial cells.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
One of the prime goals of treatment of the diabetic condition is a tight regulation of the blood glucose levels. It has been clearly demonstrated, e.g., through The Diabetes Control and Complications Trail [1] that chronic hyperglycemia is the main contributing factor to the pathological changes observed in persons with diabetes type I. Elevated levels of glucose in the circulation will affect a series of cellular processes [2, 3]. The effects of high glucose (HG) levels can be seen through the modification of several plasma proteins and proteins in the extracellular matrix. Furthermore, HG levels in intracellular compartments will affect signaling pathways, glycosylation processes, and biosynthesis of glycoconjugates [2, 3].
One important class of molecules synthesized by all cells are the PGs. These molecules are found in the extracellular matrix, on cell surfaces, and in intracellular compartments [4, 5]. They have unique properties due to their highly sulfated and negatively charged GAG chains, which are predominantly either of the heparan sulfate (HS) or chondroitin (CS) or dermatan sulfate (DS) type. Depending on cellular location HSPGs will have different functions, which include providing a negative charge in basement membranes, acting as receptors for adhesion molecules and growth factors and providing anticoagulant properties of the vessel wall [6, 7].
In the endothelium HSPGs are found both on the cell surface facing the lumen and the underlying basement membranes [8]. Furthermore, HSPGs are found in the extracellular matrix of the basement membrane in association with other matrix proteins such as collagen type IV, laminin, and fibronectin [9, 10]. Cell surface HSPGs facing the lumen have been shown to be important for extravasation of immune cells during inflammatory reactions [10, 11]. Furthermore, such HSPGs are also important for lipoprotein turnover, as they present lipoprotein lipase to achieve modulation of circulating lipoproteins [6]. The importance of HSPGs in relation to oxidative stress is also evident as these molecules have been shown to present superoxide dismutase on the cell surface of endothelial cells [6].
Modification of vascular basement membrane by hyperglycemic conditions may affect extracellular matrix components structures and thereby their functions. Alterations in such membranes are likely to contribute to the pathological consequences of macro- or microangiopathy seen in diabetes [12–14]. The importance of HSPG has been highlighted in the Steno hypothesis, which states that changes in vascular HSPG expression in diabetes is an important contributor to systemic endothelial dysfunction and increased capillary permeability [15].
Clearly, changes in HSPG biosynthesis and turnover will affect the endothelium to a large extent. In the diabetic state it has been shown that the biosynthesis of HSPGs can be decreased [16], and also the sulfation of the HS chains has been reported to be decreased [17]. A decrease in the amount of HSPGs has been reported to affect the filtration properties in the kidneys [16, 18]. Furthermore, a decrease in the levels of the HSPG perlecan has been observed in a cultured human aortic endothelial cell line exposed to hyperglycemic conditions [14], which has been suggested to affect the binding of monocytes to the sub-endothelial matrix [19].
In this study we have used primary human endothelial to investigate whether exposure to hyperglycemic condition would affect de novo biosynthesis and secretion of PGs. Our data suggest that exposure of human umbilical vein endothelial cells (HUVEC) to HG for only 4 days results in a reduction in amount of PGs secreted, without affecting the type of GAGs being made.
Materials and methods
Endothelial cell culture
Human umbilical vein endothelial cells were isolated enzymatically from infant umbilical cords of normal pregnancies under sterile conditions and established as primary cell cultures. The cells were established at 37°C in 5% CO2 in low glucose medium (LG), DMEM with 1 g/l glucose (Sigma Aldrich, Oslo, Norway). The medium was supplemented with 1% l-glutamine, 1% penicillin/streptomycin, 10% fetal bovine serum, 10 IU/ml heparin, 10 μg/ml Endothelial Cell Growth Supplement (ECGS), (BD Biosciences, Bedford, MA, USA). The cells were passaged 1–4 times and allowed to reach 80% confluence before being used in experiments.
Ethical approval for the use of human endothelial cells was obtained from the Human Research Ethical Committee.
Experimental design
The cells were exposed for 3 days to DMEM, with the above supplements and either containing LG or HG, i.e., 4.5 g/l glucose (Sigma Aldrich, Oslo, Norway). Then from day 3 to 4, the cells were placed in these same media, but without serum and antibiotic added and labeled with 35S-sulfate (0.2 mCi/ml). After incubation for 20–24 h, the conditioned media were collected, centrifuged, and stored at −20°C for further use. The cell fractions were frozen at −20°C and used for protein determination.
Gel filtration and ion exchange chromatography
35S-Labeled macromolecules (medium) were purified by Sephadex G-50 fine gel filtration (Amersham Pharmacia Biotek AB, Uppsala, Sweden). To measure the level of 35S-sulfate incorporated into macromolecules, 1 ml of each fraction was applied to a 4 ml column of Sephadex G-50 Fine in 0.05 M Tris–HCl, pH 8.0, 0.15 M NaCl. The first 1 ml of eluate after application was discarded, the next 1.5 ml was collected, and an aliquot of this fraction was counted for radioactivity using a Wallac 1414 Win Spectral (Wallac Oy, Turku Finland) scintillation counter.
Isolated macromolecules were further analyzed by gel chromatography using a Superose 6 column and a FPLC system (Pharmacia Biosciences). This column was run in 0.05 M Tris–HCl, pH 8.0, with 0.15 M NaCl and 0.2% Triton X-100. Fractions of 1 ml were collected and analyzed for content of radioactivity by scintillation counting. The elution profiles were determined relatively to the elution of the V 0 marker Dextran blue and the V t marker K2CrO4.
Isolated macromolecules were further analyzed by ion exchange chromatography using a MonoQ column and the FPLC system (Pharmacia Biosciences). The column was run in 0.05 M Tris–HCl, pH 8.0, and 0.2 M NaCl. Material binding to the column was eluted with a continuous gradient from 0.2 to 2.0 M NaCl. Eluted fractions were collected and counted in the scintillation counter.
Treatment with chondroitin ABC lyase
Samples from media of ∼5,000 cpm were incubated at 37°C overnight with 0.01 units of chondroitin ABC lyase (C-ABC) (Seikagaku Corporation, Tokyo, Japan) in 0.05 M Tris–HCl pH 8.0, containing 0.025 M sodium acetate and 25 μg/ml BSA. The elution profiles were compared with untreated samples after gel filtration on a Superose 6 column. The degraded material that was eluted in a retarded position represented chondroitin/dermatan sulfate (CS/DS). The amount of CS/DS was calculated on the basis of the elution profiles after enzyme treatment.
Treatment with HNO2
The amount of HSPG was determined by degradation with nitrous acid at pH 1.5, as described by Shively and Conrad [20]. Briefly, equal volumes of 0.5 M Ba(NO2)2 and 0.5 M H2SO4 were mixed and centrifuged for 5 min at 10 000 rpm to remove precipitated BaSO4. Equal volumes of the resulting HNO2 and sample from media of ∼5,000 cpm were mixed and incubated for 10 min at room temperature. The reaction was stopped by the addition of 1 M Tris–HCl (pH 8), and the reaction products analyzed by Superose 6 gel chromatography. The amount of HS was determined from the elution profiles after HNO2 treatment. The elution profiles of the samples were compared with those of untreated samples after gel filtration on Superose 6 column.
Alkali treatment
NaOH treatment leads to the release of intact GAG chains, from their protein cores by β-elimination. NaOH was added to samples from media (∼5,000 cpm) to give a final concentration of 0.5 M, and incubated overnight at room temperature. The incubation was ended by the addition of 5 M HCl to adjust the pH to 7.0–8.0. The molecular size of the free GAG chains was analyzed by Superose 6 column.
SDS-PAGE
35S-labeled macromolecules from cell and medium fractions obtained by Sephadex G-50 Fine gel filtration were subjected to sodium dodecyl polyacrylamide gel electrophoresis (SDS-PAGE) before and after C-ABC or nitrous acid treatment. The samples were boiled in 4X sample buffer containing 1 M Tris–HCl, pH 6.8, 8% (w/v) sodium dodecyl sulfate (SDS), 40% (v/v) glycerol, 10% (v/v) 2-mercaptoethanol, and 0.1% bromophenol blue, and applied to 4–20% polyacrylamide gels (Bio-Rad, Hercules, CA, USA). Standards used were 14C-labeled rainbow standards from Amersham. After electrophoresis the gels were fixed, treated with Amplify (Amersham), dried and subjected to autoradiography using Fuji Medical X-ray film (Fuji, Tokyo, Japan).
Immunoprecipitation
Medium fractions were purified by Sephadex G-50 gel chromatography and incubated over night at 4°C with an antibody against Syndecan-1, obtained from Serotec (Oxford, UK). The samples were subsequently incubated with protein A-Sepharose, prewashed 3 times with washing buffer A (50 mM Tris–HCl pH 7.5, 0.15 M NaCl, 0.05% Triton X-100, 1% BSA, 2 mM EDTA, and 5 mM MgSO4), 3 times with washing buffer B (50 mM Tris–HCl pH 7.5 med 0.5 M NaCl, 0.05% Triton X-100, 1% BSA, 2 mM EDTA and 5 mM MgSO4) and finally 2 times with washing buffer C (0.05 M Tris–HCl pH 7.5). The bound material was finally released from the beads after boiling in sample buffer and thereafter subjected to SDS-PAGE on 4–20% Bio-Rad polyacrylamide gels. Equal amounts of radioactivity from the respective conditioned media were used for each immunoprecipitation. After electrophoresis, the gel was dried and bands were visualized by autoradiography.
Statistical methods
Comparison between groups of data was done by using box-plots and Mann–Whitney U-test. Statistical significance was accepted with P-values fewer than 5%. The incorporation of 35S-sulfate into 35S-macromolecules varied to a large extent between primary endothelial cells from different donors. The incorporation into secreted 35S-macromolecules from LG cells (per μg protein) was set to 1.0 in the separate experiments and compared with the corresponding incorporation in cells incubated in HG.
Results
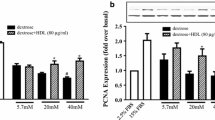
The effect of hyperglycemia on PG synthesis was first explored by incubating HUVEC-cells in media containing LG and HG and thereafter labeling with 35S-sulfate. PG synthesis was measured as 35S-sulfate incorporation into macromolecules isolated from the culture media and cell layer. Pilot studies showed that 35S-sulfate was incorporated almost exclusively into PGs in cultured human endothelial cells (not shown). 35S-sulfate incorporation into total secreted macromolecules was decreased in the presence of HG compared to LG, as can be seen in Fig. 1. The decrease observed after HG treatment was statistically significant (P = 0.002).
Box plot analyses based on secretion of 35S-labeled macromolecules in HUVEC. 35S-labeled macromolecules from cultured primary HUVEC were recovered from medium fractions after Sephadex G-50 Fine gel chromatography. The amount recovered from the media of 6 separate cultures of endothelial cells was used for the box-plot. Significant differences were observed between samples from LG and HG cultures (P = 0.002; Mann–Whitney U-test)
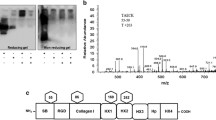
To investigate if the different treatments led to differences in the pattern of PG expression 35S-sulfate labeled macromolecules from the medium fractions were subjected to SDS-PAGE before and after C-ABC or nitrous acid treatment. As shown in Fig. 2A, the pattern of PG expression was the same in medium fractions from endothelial cells, irrespective of being cultured in LG or HG. From the figure it is further evident that the largest PGs, appearing in the top region of the gels, are HSPGs, as they are degraded after HNO2 treatment. The lower molecular weight PG, with an approximate molecular weight of 90–100 kDa is of CS/DS nature, and probably represents decorin. This particular PG has been shown to be expressed by human endothelial cells [21].
SDS-PAGE of 35S-labeled PGs in HUVEC. 35S-labeled macromolecules were recovered from the medium fractions (panel A) and cell fractions (panel B) of HUVEC treated with LG or HG, and subjected to SDS-PAGE prior to and after C-ABC treatment and HNO2 treatment. The migration of high molecular weight markers is shown on the left side of each panel (in kDa)
For comparison we also analyzed the PGs in the cells fractions. After SDS-PAGE, as shown in Fig. 2B, this material was not as well resolved as the medium fractions, but from the migrations pattern we conclude that the PGs expressed had the same approximate molecular weights as the medium PGs. In addition, the high molecular weight PGs were of the HS type, as they were degraded with HNO2. The lower molecular weight component contained CS/DS because of its susceptibility to C-ABC treatment. The PGs in the cell fractions were, accordingly, closely similar to those recovered from the medium fractions. Further analyses were focused on the medium fractions.
Studies on changes in PG expression related to diabetes have to a large extent focused on HSPGs. To try to further identify possible HSPGs expressed by primary human endothelial cells, equal amounts of 35S-macromolecules from the respective medium fractions were subjected to immunoprecipitation using an antibody against syndecan-1. As can be seen in Fig. 3 endothelial cells released syndecan-1 into the medium whether cultured with LG or HG. The lower intensity of the autoradiograph after HG matches the decrease in PG secretion after HG as shown in Fig. 1, and suggests that the decrease is, at least in part, due to lower syndecan-1 release.
SDS-PAGE after immunoprecipitation with anti-syndecan-1 antibodies. 35S-labeled macromolecules from medium fractions of primary cultures of HUVEC incubated with LG or HG were subjected to immunoprecipitations. Equal amounts of radioactivity from the two medium fractions were immunoprecipitated with an antiserum against syndecan-1. Precipitated material from each sample was subjected to SDS-PAGE and autoradiography
Alkali treatment is known to disrupt the serine-xyloside linkage between GAG chains and the protein backbone, leaving the GAG chains intact. This method was employed to investigate whether the different treatments lead to differences in molecular sizes of the GAG chains, as analyzed by possible differences in elution profiles after Superose 6 gel chromatography. From Fig. 4A, B it is evident that there were no major differences in elution profiles in medium material from cells cultured either in LG or HG. Consequently, the decrease in PG secretion after treatment of the cells with HG was not due to the expression of PGs with GAG chains of lower molecular size.
35S-labeled macromolecules in media from HUVEC-cells analyzed by Superose 6 gel chromatography. 35S-labeled macromolecules from HUVEC-cells were recovered from LG medium fractions (A) and HG medium fractions (B) and were subjected to Superose 6 gel chromatography before (♦) and after alkali treatment (■). The column was eluted with 0.05 M Tris–HCl, pH 8.0, containing 0.15 M NaCl and 0.2% Triton X-100. The figure shows representative results from one of six experiments
We also investigated whether the PG decrease observed could be due to differences in polyanionic properties (e.g. decreased sulfation). Liberated 35S-GAG chains were analyzed by ion exchange chromatography and no differences in elution profiles were observed (not shown), suggesting that there were no differences in the polyanionic properties of the respective GAGs.
The decrease in PG biosynthesis and secretion observed could also be due to decreased levels of HSPGs expressed by the endothelial cells when exposed to HG. To investigate this in further detail 35S-macromolecules from the medium fractions of cells cultured with LG or HG were subjected to deaminative cleavage followed by Superose 6 gel chromatography. The amount of HS was calculated on the basis of the 35S-labeled material eluting in retarded positions from the column after deaminative cleavage, which is known to depolymerize HS. From Fig. 5 A and B it is obvious that a major portion of the material released to the medium is of HS nature as the major part of the untreated material (fractions 14–28) is shifted to later eluting fractions (38–44) after deaminative cleavage. In medium from cells treated with LG medium HS was 63% of the labeled GAGs, whereas the corresponding numbers for HG treated cells were 73%. These differences are minor and probably not significant. Identical experiments with material from different HUVEC preparations revealed that HS represented approximately 60–70% of the total PG material labeled under the different conditions.
35S-labeled macromolecules from media of HUVEC analyzed by Superose 6 gel chromatography. 35S-labeled macromolecules were recovered from LG medium fractions (A) and HG medium fractions (B) and subjected to Superose 6 gel chromatography before (♦) and after HNO2 (■) treatment. Running conditions were as described in the legend to Fig. 4. The figure shows representative results from one of six experiments
The rest of the material was degraded with C-ABC (not shown). We can therefore conclude that endothelial cells express approximately the same ratio of HS/CS, even when the PG synthesis and secretion is decreased in the presence of HG.
Discussion
In the present paper we show that exposing primary HUVEC to hyperglycemia led to decreased PG expression. However, the ratio of HS/CS did not change, although the PG expression was lowered. In addition, we could demonstrate that HUVEC expressed the HSPG syndecan-1, both under normal and with hyperglycemia conditions. The data obtained suggest that syndecan-1 levels were decreased under hyperglycemic conditions, as has been shown for perlecan [14, 19]. The data generated therefore suggest that hyperglycemia induces a general decrease in PG expression in cultured primary endothelial cells. As HSPG is a dominant PG in endothelial cells, the decrease we observe would affect HSPGs to a large extent. In arteries of diabetic monkeys it has been observed that cholesterol levels were increased, whereas HS levels were decreased compared to tissues samples taken from control animals. The level of dermatan sulfate, in contrast, was increased with diabetes [22].
A decrease in HSPGs in the endothelium in response to hyperglycemic conditions may have several consequences. It has been shown that fibroblast growth factor is associated with extracellular matrix, in complex with HSPGs [23]. It may be speculated that a decrease in HSPG can influence the local regulation of cell proliferation and matrix deposition mediated by this growth factor [23]. Furthermore, a decrease in HSPG on the basolateral side of the endothelial cells can affect the adhesive properties of the endothelial cells [10]. Also, a decrease in HSPG levels may affect the filtration properties in the endothelium in general, as has been shown for the kidneys [24, 25]. Finally, decreased levels of HSPG on the basolateral side of endothelial cells can affect matrix assembly, where the ratio between the individual components is important for a proper regulation of this process. On the apical side of endothelium, a decrease in cell surface HSPGs, may also lead to changes in the regulation of partner molecules, such as lipoprotein lipase and chemokines. At present there is limited data on the consequences of decreased HSPGs for these important molecules in relation to diabetes.
The molecular bases for a decrease in HSPGs in primary HUVEC have not been studied. However, in pilot studies we have shown that a highly modified advanced glycation end-product (AGE), carboxymethyl lysine bovine serum albumin (CML-BSA) also decreased PG biosynthesis in closely the same way as reported here for HG treatment (Gharagozlian unpublished data). In future experiments it will be on interest to investigate the importance of minimally modified and highly modified AGEs on PG expression in primary human endothelial cells. The fact that exposure to CML-BSA also leads to a decrease in PG expression in cultured endothelial cells, as we have previously observed in cultured kidney epithelial cells [26], indicates that signaling pathways affected by AGEs may be involved. These may include activation of protein kinase C, increased oxidative stress and other changes that evidently will affect endothelial cells [27, 28].
From the data presented it is evident that hyperglycemic conditions lead to decreased levels of HSPG in cultures of primary HUVEC. Such a change may affect the regulation of several types of molecules, normally interacting with HSPGs. Several of these factors are involved in processes related to fibrosis, inflammation, and atherosclerosis [6, 15]. The fact that effects of hyperglycemia can be observed in short-term cultures of primary HUVEC offers new possibilities to study regulatory mechanisms in further detail.
References
The Diabetes Control, Complications Trial Research Group (1993) The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med 329:977–986
Yamagishi S, Imaizumi T (2005) Diabetic vascular complications: pathophysiology, biochemical basis and potential therapeutic strategy. Curr Pharm 11(18):2279–2299
Brownlee M (2001) Biochemistry and molecular cell biology of diabetic complications. Nature 414:813–820
Selleck SB (2000) Proteoglycans and pattern formation: sugar biochemistry meets developmental genetics. Trends Genet 16(5):206–212
Kjellen L, Lindahl U (1991) Proteoglycans: structures and interactions. Annu Rev Biochem 60:443–475
Kolset SO, Salmivirta M (1999) Cell surface heparan sulfate proteoglycans and lipoprotein metabolism. Cell Mol Life Sci 56:857–870
Miner JH (1999) Renal basement membrane components. Kidney Int 56:2016–2024
Saku T, Furthmayr H (1989) Characterization of the major heparan sulfate proteoglycan secreted by bovine aortic endothelial cells in culture. Homology to the large molecular weight molecule of basement membranes. J Biol Chem 264:3514–3523
Iozzo RV (1998) Matrix proteoglycans: from molecular design to cellular function. Annu Rev Biochem 67:609–652
Rops AL, van der Vlag J, Lensen JF, et al. (2004) Heparan sulfate proteoglycans in glomerular inflammation. Kidney Int 65:768–785
Wang L, Fuster M, Sriramarao P, Esko JD (2005) Endothelial heparan sulfate deficiency impairs l-selectin- and chemokine-mediated neutrophil trafficking during inflammatory responses. Nat Immunol 6:902–910
Bollineni JS, Alluru I, Reddi AS (1997) Heparan sulfate proteoglycan synthesis and its expression are decreased in the retina of diabetic rats. Curr Eye Res 16:127–130
Laffont I, Shuvaev VV, Briand O, et al. (2002) Early-glycation of apolipoprotein E: effect on its binding to LDL receptor, scavenger receptor A and heparan sulfates. Biochim Biophys Acta 1583:99–107
Vogl-Willis CA, Edwards IJ (2004) High-glucose-induced structural changes in the heparan sulfate proteoglycan, perlecan, of cultured human aortic endothelial cells. Biochim Biophys Acta 1672:36–45
Deckert T, Feldt-Rasmussen B, Borch-Johnsen K, Jensen T, Kofoed-Enevoldsen A (1989) Albuminuria reflects widespread vascular damage. The Steno hypothesis. Diabetologia 32:219–226
Jensen T (1997) Pathogenesis of diabetic vascular disease: evidence for the role of reduced heparan sulfate proteoglycan. Diabetes 46(Suppl 2):S98–S100
Kjellen L, Bielefeld D, Hook M (1983) Reduced sulfation of liver heparan sulfate in experimentally diabetic rats. Diabetes 32:337–342
Ha TS, Song CJ, Lee JH (2004) Effects of advanced glycosylation endproducts on perlecan core protein of glomerular epithelium. Pediatr Nephrol 19:1219–1224
Vogl-Willis CA, Edwards IJ (2004) High glucose-induced alterations in subendothelial matrix perlecan leads to increased monocyte binding. Arterioscler Thromb Vasc Biol 24:858–863
Shively JE, Conrad HE (1976) Formation of anhydrosugars in the chemical depolymerization of heparin. Biochemistry (Mosc) 15:3932–3942
Jarvelainen HT, Kinsella MG, Wight TN, Sandell LJ (1991) Differential expression of small chondroitin/dermatan sulfate proteoglycans, PG-I/ biglycan and PG-II/decorin, by vascular smooth muscle and endothelial cells in culture. J Biol Chem 266:23274–23281
Edwards IJ, Wagner JD, Vogl-Willis CA, Litwak KN, Cefalu WT (2004) Arterial heparan sulfate is negatively associated with hyperglycemia and atherosclerosis in diabetic monkeys. Cardiovasc Diabetol 3:6
Nugent MA, Iozzo RV (2000) Fibroblast growth factor-2. Int J Biochem Cell Biol 32:115–120
Garin EH, Shirey AJ (1988) Glomerular basement membrane heparan sulfate glycosaminoglycan in aminonucleoside of puromycin nephrosis. Child Nephrol Urol 9:121–126
Sorensson J, Bjornson A, Ohlson M, Ballermann BJ, Haraldsson B (2003) Synthesis of sulfated proteoglycans by bovine glomerular endothelial cells in culture. Am J Physiol Renal Physiol 284:F373–F380
Borrebæk J, Prydz K, Fjeldstad K, et al. (2001) The AGE product N epsilon-(carboxymethyl)lysine serum albumin is a modulator of proteoglycan expression in polarized cultured kidney epithelial cells. Diabetologia 44:488–494
Osawa T, Kato Y (2005) Protective role of antioxidative food factors in oxidative stress caused by hyperglycemia. Ann NY Acad Sci 1043:440–451
Way KJ, Isshiki K, Suzuma K, et al. (2002) Expression of connective tissue growth factor is increased in injured myocardium associated with protein kinase C beta2 activation and diabetes. Diabetes 51:2709–2718
Acknowledgments
This work was supported by grants from Helse og Rehabilitering, Norges Diabetsforbund, and the Throne Holst Foundation.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gharagozlian, S., Borrebæk, J., Henriksen, T. et al. Effect of hyperglycemic condition on proteoglycan secretion in cultured human endothelial cells. Eur J Nutr 45, 369–375 (2006). https://doi.org/10.1007/s00394-006-0608-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-006-0608-9