Abstract
Background
In clinical routine, rapid infarct sizing techniques are warranted, as objective and precise infarct sizing is important for clinical decision-making. Accurate and objective measures of relative infarct size (rIS) using contrast-enhanced cardiac magnetic resonance (ceCMR) have been extensively demonstrated in experimental animals, but less in humans. The aim of this study was therefore to quantify rIS assessed by ceCMR in patients with chronic myocardial infarction using semi-automatic quantitation techniques.
Methods
A total of 62 patients (mean age 66 ± 9 years) with ischemic cardiomyopathy (EF 24 ± 8%) underwent ceCMR for viability testing. rIS was obtained by two time-saving semi-automatic thresholding methods based on: (1) visual definition of a single signal intensity cutoff value (VISUAL) and (2) the full-width-at-half-maximum technique (FWHM). Results were compared to manual tracing (MANUAL) as the reference standard.
Results
VISUAL showed better agreement [r = 0.99; intraclass correlation coefficient (ICC) = 0.98, limits of agreement ±3.2%] to MANUAL than the FWHM technique (r = 0.77, ICC = 0.76, limits of agreement ±12%). Infarct sizing using MANUAL was twice as time-consuming (3.1 ± 0.2 min) compared to VISUAL (1.6 ± 0.1 min) or FWHM (1.6 ± 0.2 min).
Conclusions
Visual estimation of signal intensity cutoff values allows rapid and accurate determination of rIS in patients with chronic myocardial infarction using ceCMR and is superior to the FWHM technique.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Contrast-enhanced cardiovascular magnetic resonance (ceCMR) has emerged as a robust technique for non-invasive quantitation of myocardial scar, owing to its high spatial resolution and high contrast between infarcted and non-infarcted myocardium [1–3].
Estimation of left ventricular (LV) infarct size is of incremental importance in clinical routine, especially in terms of evaluating new therapies that can reduce infarct size, i.e., regenerative therapy with stem cells or new procedures and drugs [4–6]. Several studies have also shown that determination of infarct size using ceCMR conveys important prognostic information [2, 7]. Furthermore, an inverse relationship between the amount of scar and the outcome after revascularization has been demonstrated [8].
Therefore, it is highly important to validate an objective and rapid method that provides exact measurements of the amount of scar in patients with myocardial infarction in clinical routine. Although manual tracing is an accepted method for scar quantitation using ceCMR, it is tedious and time-consuming. Thus, more objective and rapid methods are warranted in clinical routine. Recently, accurate and objective measures of relative infarct size (rIS) using ceCMR have been demonstrated in experimental animals with acute myocardial infarction [9]. In that study, the full-width-at-half-maximum (FWHM) technique was advocated as the optimal method for accurate and reproducible IS quantitation [9]. However, whether this technique is also accurate in humans with chronic infarctions has not been investigated.
Therefore, the aim of this study was to evaluate two different semi-automatic infarct sizing techniques based on: (1) visual estimation of a single signal intensity cutoff value (VISUAL) and (2) the FWHM technique compared to manual tracing (MANUAL) for rapid, objective and time-saving infarct sizing by ceCMR imaging.
Methods
Study design
A total of 62 consecutive patients (mean age 66 ± 9 years) with ischemic cardiomyopathy [ejection fraction (EF) 24 ± 8% as determined by CMR] and clinical indication for viability testing were enrolled. Ischemic cardiomyopathy was defined as reduced EF < 50% and at least one stenosis >50% in one major coronary vessel on invasive coronary angiography.
All patients underwent ceCMR imaging. Patients with contraindications to ceCMR, myocardial infarction within 6 weeks before enrollment in the study and unstable angina pectoris were excluded from the study. Each patient gave informed consent in accordance with the local ethics committee requirements.
Imaging protocol
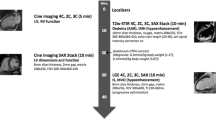
Images were acquired on a 1.5 T clinical scanner (Intera, Philips, Best, The Netherlands) using a five-element phased array cardiac synergy coil. Scout images were acquired in long-axis and short-axis orientation for planning of the final double-oblique long-axis and short-axis views. ECG-gated cine images were acquired using a segmented steady-state free precession sequence (TE/TR 1.8/3.6 ms, spatial resolution 1.8 × 1.5 × 8 mm³, 25 frames per RR interval). Three long-axis views and 10–12 short-axis views (slice thickness 8, 2 mm gap) covering the whole left ventricle were obtained during repeated breath-holds. A gadolinium-based contrast agent (Magnevist, Bayer Vital, Leverkusen, Germany; 0.2 mmol/kg) was then administered intravenously. After 15 min, contrast-enhanced images were acquired in the same orientation as the cine images using a segmented inversion-recovery gradient-echo pulse sequence triggered to end-diastole [10]. The inversion time was set to null the signal of normal myocardium after contrast administration (typically 250–300 ms) and was adjusted in the course of the investigation if necessary. Other parameters of the sequence were: TR/TE 2 heart beats/5.0 ms, FA 25°, matrix 256 × 256, and a typical voxel size of 1.4 × 1.4 × 8.0 mm³.
Data analysis
For data analysis, an observer unaware of the patient’s history performed analysis of all CMR data using the MASS software (release 6.1.5., Medis, Leiden, The Netherlands).
MANUAL analysis
In each patient, the area of delayed enhancement in each short-axis slice was determined by manual contour tracing after visual optimization of window levels for optimal display of the hyperenhanced region (Fig. 1a). The total rIS per patient was calculated after summing all delayed enhancement areas of all short-axis slices divided by the total myocardial area and multiplied by 100. MANUAL analysis served as the reference technique.
Different methods of infarct size quantitation for the comparison of different thresholding techniques. a Delayed enhancement image using ceCMR in a patient with a transmural inferior myocardial infarction. The delayed enhancement area (= infarction area) is manually outlined (yellow line). b The same patient as in (a). The delayed enhancement area is overlaid with a pink color after visual definition of an appropriate signal intensity cutoff value separating non-infarcted from infarcted tissue. For the FWHM technique, see text for details
VISUAL analysis
The MASS software provides a tool for the semi-automatic segmentation of the myocardium within the manually traced endocardial and epicardial borders based on signal intensity thresholds. Pixels demonstrating signal intensities above a set threshold will be overlaid with pink color (Figs. 1b, 2). The range of signal intensities of the myocardium encompassed between the endo- and epicardial boundaries is displayed. The observer sets a signal intensity threshold within the range of signal intensities that optimally covers the hyperenhanced regions with the pink overlay. This threshold is defined for the complete study only once and is not repeated for the different analyzed slices. Based on the overlaid pixels, the infarct area is automatically calculated for all slices. In addition, rIS is calculated relating the infarct area to the total myocardial area.
Contrast-enhanced images (short-axis views) of a patient with chronic anterior myocardial infarction. In all short-axis views, the endocardial and epicardial borders are manually traced. Pixels demonstrating signal intensities above a visually set threshold will be overlaid with a pink color. Based on the overlaid pixels, the infarct area is automatically calculated for all slices
FWHM technique
With this method, the maximum signal intensity within the delayed enhancement area representing infarcted myocardium is determined in a representative slice. The final extent of the scar is defined as the area including all pixels with a signal intensity >50% of the maximum signal intensity, as initially determined.
Assessment of observer variability
In 15 subjects, inter-observer variability was assessed by a second independent observer unaware of the first observer’s results. Intra-observer variability was assessed by the first observer with 2 weeks being allowed to elapse between the two analysis sessions.
Statistical analysis
Data are displayed as mean ± standard deviation. Relative IS measured by the different ceCMR techniques were compared using linear regression analysis. Bland–Altman analysis and intraclass correlation coefficient (ICC) for absolute agreement were performed to assess the level of agreement between the techniques for the determination of rIS. To assess the difference between VISUAL and FWHM, F-statistic was performed. Bland–Altman analysis was performed for the assessment of inter-observer variability. The software SPSS 12.0 (SPSS Inc., Chicago, IL) was used for all statistical analyses. A P value of <0.05 was considered to be statistically significant.
Results
Table 1 displays the clinical characteristics of the patient population. According to invasive angiography, 55% of the patients (n = 34) had three-vessel disease, 23% (n = 14) had two-vessel disease and 23% (n = 14) of the patients had one-vessel disease. Cardiovascular risk factors including smoking, hypertension (use of antihypertensive medication or blood pressure at rest >140/90 mmHg), diabetes mellitus (use of insulin or anti-diabetic agents or fasting serum glucose >130 mg/dl) and hypercholesterolemia (total fasting serum cholesterol >200 mg/dl or use of cholesterol-lowering medication) were assessed from the patient chart. Elevated serum creatinine was defined as a serum creatinine >1.2 mg/dl. All patients received standard pharmacological therapy including beta-blockers, ACE-inhibitors, and statins. Additionally, 71% of the patients received diuretics, 40% nitrates and 29% aldosterone-antagonists. A part of the patient population has been described previously [11].
Thresholding techniques for infarct sizing using ceCMR
The results are summarized in Table 2 and Fig. 3, with MANUAL rIS averaged at 17 ± 9%. Using the semi-automatic thresholding techniques, rIS was 18 ± 9% with VISUAL and 18 ± 9% with the FWHM method. Correlation with MANUAL was higher for VISUAL (r = 0.99; ICC = 0.98; P < 0.001) compared to FWHM (r = 0.77; ICC = 0.76; P < 0.001). In addition, the limits of agreement were narrower for VISUAL compared to FWHM (±3.2 vs. ±12%; P < 0.001).
Comparison of different semi-automatic thresholding techniques. a Bland–Altman analyses for comparison of MANUAL and VISUAL, as well as results of linear regression analysis. b Bland–Altman analyses for comparison of MANUAL and FWHM, as well as results of linear regression analysis. For further details see Table 2
Analysis time
Infarct sizing using MANUAL was twice as time-consuming (3.1 ± 0.2 min) compared to VISUAL (1.6 ± 0.1 min) or FWHM (1.6 ± 0.2 min) (P < 0.001 for both).
Reproducibility
Inter-observer variability
The reproducibility of ceCMR data analysis was within acceptable limits with no significant differences in measurements by two different observers. The inter-observer variability of MANUAL, VISUAL and FWHM achieved a high correlation coefficient and narrow limits of agreement (MANUAL: r = 0.91, limits of agreement ±6%; VISUAL: r = 0.93, limits of agreement ±6%; FWHM: r = 0.95, limits of agreement ±5%).
Intra-observer variability
The intra-observer variability was excellent for all infarct sizing techniques. (MANUAL: r = 0.93, limits of agreement ±5%; VISUAL: r = 0.95, limits of agreement ±5%; FWHM: r = 0.95, limits of agreement ±5%).
Discussion
The results of the study demonstrate that semi-automatic thresholding enables rapid, accurate and reproducible quantitation of rIS in humans with chronic infarctions. In contrast to previous data derived from animal experiments of acute myocardial infarction [9], the FWHM technique proved to be less accurate compared to a method based on visual estimation of a signal intensity threshold for the quantitation of rIS in the routine clinical setting.
Accurate and objective non-invasive infarct sizing gains more and more importance, especially for the evaluation of therapeutic options for infarct size reduction such as stem cell therapy, post-conditioning, etc. [4, 5]. CeCMR offers high resolution with a relatively sharp contrast between infarcted and non-infarcted myocardium which renders this method ideal for the quantitative analysis of rIS. Quantitation of infarct size using ceCMR has been extensively validated in experimental animal studies, but data in humans are sparse [12, 13].
In this study, we compared two different semi-automatic segmentation methods in manual tracing for rapid determination of rIS using ceCMR in patients with chronic myocardial infarction. The first method uses a visually defined signal intensity threshold value, which separates infarcted from non-infarcted myocardium. With this method, the amount of infarcted tissue per slice is displayed as a pink overlay immediately after definition of the threshold value, which allows an easy visual adaptation of the cutoff value. As a disadvantage, the threshold value applies for all short-axis slices of the same patient, which ignores a possible shift in the inversion time between the acquisitions of consecutive short-axis slices when using a 2D acquisition strategy as in the present study. This may be less of a problem with 3D data acquisition strategies. Despite this disadvantage, an excellent accuracy of the technique compared to manual contour tracing was observed.
The FWHM technique is a method where the maximum signal intensity within the infarcted myocardium is determined in a representative slice. The final extent of the scar is defined as the area including all pixels with a signal intensity >50% of the maximum signal intensity, as initially determined. This technique was less accurate for the assessment of rIS as compared to the visually defined threshold value. This is at odds with the results of the study by Amado et al. [9], who recently reported the FWHM technique to be superior to visual assessment of IS. However, that study was performed in an optimal experimental setting, which may not be applicable to the conditions found in clinical routine. Moreover, in the former study, data were acquired 24 h after induction of an acute myocardial infarction, while in the present study we included patients with chronic infarctions. Thus, both studies may not be directly comparable. Although the FWHM method may in theory be more observer-independent and would thus be preferable to a more subjective analysis method such as visual analysis, the results of this study do not support the routine clinical use of the former method for the analysis of rIS in patients with chronic infarctions. An explanation for the inferior results of the FWHM technique may be related to the fact that in clinical routine, nulling of the myocardial signal during acquisition of the delayed enhancement images might be less accurate than in the experimental setting due to patient-related factors. Thus, the transition of signal intensities from non-infarcted to infarcted myocardium may be less sharp, resulting in a broader distribution curve of signal intensities and in inaccuracies when using the FWHM technique. However, both semi-automatic infarct sizing techniques allowed faster data analysis compared to manual tracing with good reproducibility.
Conclusion and clinical implications
When using semi-automatic infarct sizing techniques, VISUAL is superior to the FWHM technique for quantitation of rIS in patients with chronic myocardial infarction. Infarct sizing is clinically important because the amount of scar is an independent predictor for functional recovery of left ventricular function after revascularization [14]. Therefore, a tool that allows accurate and rapid infarct sizing, which is also practicable in clinical routine, is highly important. A ceCMR method based on visual definition of a signal intensity threshold value provides a rapid and accurate tool for infarct sizing in clinical routine.
References
Fieno DS, Kim RJ, Chen EL, Lomasney JW, Klocke FJ, Judd RM (2000) Contrast-enhanced magnetic resonance imaging of myocardium at risk: distinction between reversible and irreversible injury throughout infarct healing. J Am Coll Cardiol 36:1985–1991
Kim RJ, Fieno DS, Parrish TB, Harris K, Chen EL, Simonetti O, Bundy J, Finn JP, Klocke FJ, Judd RM (1999) Relationship of MRI delayed contrast enhancement to irreversible injury, infarct age, and contractile function. Circulation 100:1992–2002
Kuhl HP, Beek AM, van der Weerdt AP, Hofman MB, Visser CA, Lammertsma AA, Heussen N, Visser FC, van Rossum AC (2003) Myocardial viability in chronic ischemic heart disease: comparison of contrast-enhanced magnetic resonance imaging with (18)F-fluorodeoxyglucose positron emission tomography. J Am Coll Cardiol 41:1341–1348
Kin H, Zhao ZQ, Sun HY, Wang NP, Corvera JS, Halkos ME, Kerendi F, Guyton RA, Vinten-Johansen J (2004) Postconditioning attenuates myocardial ischemia-reperfusion injury by inhibiting events in the early minutes of reperfusion. Cardiovasc Res 62:74–85
Mathur A, Martin JF (2004) Stem cells and repair of the heart. Lancet 364:183–192
Piot C, Croisille P, Staat P, Thibault H, Rioufol G, Mewton N, Elbelghiti R, Cung TT, Bonnefoy E, Angoulvant D, Macia C, Raczka F, Sportouch C, Gahide G, Finet G, ndre-Fouet X, Revel D, Kirkorian G, Monassier JP, Derumeaux G, Ovize M (2008) Effect of cyclosporine on reperfusion injury in acute myocardial infarction. N Engl J Med 359:473–481
Kwong RY, Chan AK, Brown KA, Chan CW, Reynolds HG, Tsang S, Davis RB (2006) Impact of unrecognized myocardial scar detected by cardiac magnetic resonance imaging on event-free survival in patients presenting with signs or symptoms of coronary artery disease. Circulation 113:2733–2743
Kim RJ, Wu E, Rafael A, Chen EL, Parker MA, Simonetti O, Klocke FJ, Bonow RO, Judd RM (2000) The use of contrast-enhanced magnetic resonance imaging to identify reversible myocardial dysfunction. N Engl J Med 343:1445–1453
Amado LC, Gerber BL, Gupta SN, Rettmann DW, Szarf G, Schock R, Nasir K, Kraitchman DL, Lima JA (2004) Accurate and objective infarct sizing by contrast-enhanced magnetic resonance imaging in a canine myocardial infarction model. J Am Coll Cardiol 44:2383–2389
Simonetti OP, Kim RJ, Fieno DS, Hillenbrand HB, Wu E, Bundy JM, Finn JP, Judd RM (2001) An improved MR imaging technique for the visualization of myocardial infarction. Radiology 218:215–223
Kuhl HP, Lipke CS, Krombach GA, Katoh M, Battenberg TF, Nowak B, Heussen N, Buecker A, Schaefer WM (2006) Assessment of reversible myocardial dysfunction in chronic ischaemic heart disease: comparison of contrast-enhanced cardiovascular magnetic resonance and a combined positron emission tomography-single photon emission computed tomography imaging protocol. Eur Heart J 27:846–853
Judd RM, Lugo-Olivieri CH, Arai M, Kondo T, Croisille P, Lima JA, Mohan V, Becker LC, Zerhouni EA (1995) Physiological basis of myocardial contrast enhancement in fast magnetic resonance images of 2-day-old reperfused canine infarcts. Circulation 92:1902–1910
Saeed M, Wendland MF, Masui T, Connolly AJ, Derugin N, Brasch RC, Higgins CB (1991) Myocardial infarction: assessment with an intravascular MR contrast medium. Radiology 180:153–160
Beanlands RS, Ruddy TD, de Kemp RA, Iwanochko RM, Coates G, Freeman M, Nahmias C, Hendry P, Burns RJ, Lamy A, Mickleborough L, Kostuk W, Fallen E, Nichol G (2002) Positron emission tomography and recovery following revascularization (PARR-1): the importance of scar and the development of a prediction rule for the degree of recovery of left ventricular function. J Am Coll Cardiol 40:1735–1743
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Neizel, M., Katoh, M., Schade, E. et al. Rapid and accurate determination of relative infarct size in humans using contrast-enhanced magnetic resonance imaging. Clin Res Cardiol 98, 319–324 (2009). https://doi.org/10.1007/s00392-009-0007-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00392-009-0007-3