Abstract
Purpose
The requisite for a rigorous preoperative understanding of vascular branching continues to grow in parallel with the implementation of laparoscopic surgery. Three-dimensional (3D)-computed tomography (CT) angiography is a less-invasive modality than traditional angiographic examination. Therefore, we aimed to evaluate branching patterns of the superior mesenteric artery (SMA).
Methods
In the present study, 536 consecutive patients who underwent preoperative 3D-CT angiography from April 2012 to March 2014 were prospectively enrolled. The branching pattern of the right colic artery (RCA) and the intersectional patterns of the RCA, ileocolic artery (ICA), and superior mesenteric vein (SMV) were evaluated.
Results
The RCA existed in only 179 cases (33.4 %); the remaining 357 patients (66.6 %) lacked evidence of the RCA. The ICA was detected in all cases. The RCA ran ventral to the SMV in the majority of cases (89.4 %). Conversely, the ICA ran ventral to the SMV in only half of the cases (50.6 %). When the RCA was observed to pass dorsal to the SMV, the ICA also ran dorsal to SMV in all cases.
Conclusions
3D-CT angiography can aid surgeons in identifying and understanding the anatomical vascular variations and intersectional patterns of the RCA, ICA, and SMV. Developing awareness of these variations can aid in the prevention of unexpected vascular injury during laparoscopic right-sided colon surgery.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Indications for laparoscopic colorectal surgery continue to grow as a product of the minimally invasive advantages of laparoscopy, including smaller incisions, less intraoperative blood loss and postoperative pain, and shorter hospitalization time than conventional open surgery [1–3]. However, identifying vascular bifurcation is frequently difficult during laparoscopic surgery owing to the limited field of view [4]; therefore, the requisite for a rigorous preoperative understanding of vascular branching continues to grow in parallel with the implementation of laparoscopic surgery.
The anatomy of the superior mesenteric artery (SMA) is particularly important during right-sided colorectal surgeries. Specifically, it is imperative to understand the branching pattern of the right colic artery (RCA), as substantial variation exists between individuals with respect to the location of the RCA and ileocolic artery (ICA), and whether these vessels are located ventrally or dorsally to the superior mesenteric vein (SMV). Although branching variations of the SMA have been previously investigated with cadaveric and angiographic studies [5–7], these methods are limited by temporality and invasiveness, respectively. Thus, intersectional patterns of the RCA, ICA, and SMV have previously been difficult to study in a rigorous fashion.
Recently, through advances in computed tomography (CT) technologies, three-dimensional (3D)-CT angiography has been adequately well developed to provide an alternative modality for evaluating the branching pattern of the SMA. Importantly, 3D-CT angiography is less invasive than traditional angiographic examination and is useful for preoperatively evaluating the vascular anatomy of patients with gastric cancers, peripheral arterial disease, and middle rectal arteries [8–10].
Previous studies have reported on branching variations of the SMA using CT angiography prior to colorectal surgery [11–13]. However, these studies have typically included small study cohorts, and thus present considerably different results with respect to the frequency of the presence of the RCA and the relationship between the RCA and ICA. Therefore, in the present study, we aimed to evaluate the branching patterns of the SMA in a large number of patients (n = 536) and to demonstrate how 3D-CT angiography can be used in a clinical context to facilitate identification of bifurcation patterns of the SMA.
Materials and methods
Patient selection
In the present study, 536 consecutive patients (328 men and 208 women; median age 66 years [range, 21–91 years]) with colorectal cancers who underwent preoperative 3D-CT angiography at the University of Tokyo Hospital from April 2012 to March 2014 were prospectively enrolled. Patients with left-sided colon cancer or those who underwent palliative surgery were also included. Informed consent was obtained from all patients prior to participation, and study approval was granted by the Ethics Committee of the University of Tokyo.
3D-CT angiography protocol
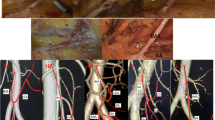
Patients underwent 3D-CT angiography using a 16- or 64-detector CT scanner. The tube potential was 120 kVp, and the tube current was adjusted by automatic exposure control with a noise index of ten and a slice thickness of 0.5–1 mm. Iopamidol (370 mg I/mL, iopamiron 370; Bayer, Osaka, Japan) was used as the contrast agent. Patients were injected with 0.7 g/kg iodine (upper limit, 37 g) for 30 s at a rate of 2.3–3.3 mL/s. The bolus tracking method was used to determine scan timing. The scan was initiated when the contrast in the abdominal aorta (above the renal arteries) reached 150 Hounsfield units. Ninety seconds after the injection of iopamidol, the venous phase image was acquired. Image processing analysis was performed using a 3D volume rendering technique with the ZIO station system (Ziosoft, Tokyo, Japan) (Fig. 1). All CT images were reviewed using a picture archiving and communication system workstation (General Electric Medical Systems, Milwaukee, WI).
Definitions of the middle colic artery, right colic artery, and ileocolic artery
The middle colic artery (MCA) and ICA were defined as the arteries arising from the SMA that approximated the transverse colon and ileocecal valve, respectively, at their distal ends. The right colic artery (RCA) was defined as the artery arising from the SMA that ran ventral to the pancreas toward the ascending colon. In the present study, cases in which the RCA diverge from the MCA or ICA were excluded. These definitions were developed according to 3D-CT images and an axial CT scans.
Intersectional patterns of the RCA, ICA, and SMV
Whilst the RCA and ICA run across the SMV, they exhibit variability in whether they are located dorsal or ventral to the SMV. Therefore, we evaluated the relative frequency of each type of relationship between the RCA, ICA, and SMV. The intersectional patterns of these vessels were assessed using a combination of the results obtained from sequential axial 2D- and reconstructed 3D-CT scans (Fig. 2).
Evidence acquisition
An electronic literature search was performed via PubMed to identify studies that have evaluated the presence of the RCA and intersectional patterns of the RCA, ICA, and SMV. Our search included all English language entries from inception until November 2015, and incorporated ‘right colic artery’ as the only keyword. Case reports, editorials, letters, commentaries, and studies that only validated previously published reports were excluded. The initial search gave 200 publications; after title and abstract screening, 15 studies remained. After full text screening, 11 studies remained, and a further two were added after reviewing the references of the 15 studies; thus, 13 studies were included in the final review.
Results
Frequency of varying SMA bifurcating patterns
The frequencies of the various bifurcation patterns of the SMA are shown in Fig. 1. The RCA existed in only 179 cases (33.4 %); the remaining 357 patients (66.6 %) lacked evidence of the RCA. The ICA was detected in all cases.
Intersectional patterns of the RCA, ICA, and SMV
We evaluated the anteroposterior positional relationship of the RCA, ICA, and SMV (Table 1). The RCA ran ventral to the SMV in the majority of cases (89.4 %). However, in contrast, the ICA ran ventral to the SMV in only half of the cases (50.6 %).
Subsequently, we evaluated the intersectional patterns of the RCA and ICA together (Fig. 3). When the RCA was observed to be ventral to the SMV, the ICA was also ventral in almost half of the cases (14.9 vs. 14.9 % for the ICA dorsal to the SMV). Conversely, when the RCA was observed to pass dorsal to SMV, the ICA also ran dorsal to the SMV, in all cases. In cases without the RCA, the ICA ran ventral to the SMV in almost half of the cases (35.6 vs. 31.0 % for the ICA dorsal to the SMV).
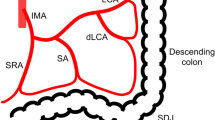
Intersectional patterns of the RCA, ICA, and the SMV. a The RCA and the ICA crossed the SMV ventrally. b The RCA crossed the SMV dorsally and the ICA ventrally. c Defect of the RCA and the ICA crossed the SMV ventrally. d The RCA crossed the SMV ventrally and the ICA dorsally. e The RCA and the ICA crossed the SMV dorsally. f Defect of the RCA and the ICA crossed the SMV dorsally. Bold line indicates artery, and grey line vein
Discussion
Preoperative 3D-CT angiography is associated with a significant reduction in the operative time and incidence of complications related to difficult or erroneous identification of mesenteric vessels [4]. During right-sided hemicolectomy with D3 lymph node dissection, it is necessary to skeletonize the SMV and ligate the root of the ileocolic vessels. Subsequently, it is also necessary to ligate the origin of the right colic vessels and right branches of the middle colic vessels [14, 15]. Therefore, it is important to evaluate whether the RCA branch from the SMA is present or absent. In cases that lack the RCA, it is possible to misidentify the MCA as the RCA. Moreover, when dissecting lymph nodes around the SMV, a lack of information regarding the dorsal or ventral course of the RCA and ICA can result in damage to these arteries. Thus, preoperative identification of SMA branching variations is crucial in obtaining optimal surgical outcomes.
A primary goal of this study was to evaluate the frequency of RCA diversion from the SMA. The RCA was observed in only 179 cases (33.4 %), whilst 357 patients (66.6 %) lacked evidence of the RCA. Although the branching patterns of the RCA have previously been investigated in cadaveric and angiographic studies, the literature remains inconsistent with respect to the relative incidence of the RCA (Table 2) [7, 12, 13, 16–24]. For example, the RCA has been reported to branch from the MCA or ICA at rates of 19–52 % and 8–66.9 %, respectively; this constitutes a substantial range of reported incidences. In some part, this may be due to difficulty in distinguishing the RCA from peripheral arteries branching from the MCA and ICA. Furthermore, as it is important to obtain an overall understanding of the arteries diverting from the SMA for D3 lymph node dissection, we evaluated the frequency of the RCA branching from the SMA. Previously, the frequency of the RCA branching from the SMA has been reported between ranged from 28.3 to 41 % in reports that included more than 200 patients [7, 13, 16, 21]. These results are consistent with the results of 3D-CT angiography observed in the present study.
Subsequently, we evaluated the anteroposterior positional relationship of the RCA, ICA, and SMV, which is important when dissecting lymph nodes around the SMV. The ICA ran ventral to the SMV in almost half of the cases (50.6 %). Conversely, the RCA ran ventral to the SMV in the majority of cases (89.4 %). Intersectional patterns evaluated in cadaveric studies and 3D-CT angiography are shown in Table 3. Previously, the ICA has been shown to lie ventral to the SMV in 20.8–59.1 % of cases (average 46.4 %), whilst the RCA has been reported to lie ventral in 63–92.6 % of cases (average 86.8 %); these findings are consistent with the results of the present study [12, 13, 18–20, 22–24].
Interestingly, when the ICA was observed to run ventral to the SMV, the RCA was also observed to run ventrally, in all cases (Table 4). To date, only three reports exist regarding the correlation between the intersectional patterns of the RCA and ICA. However, the finding of a dorsally located RCA in the context of a ventrally located ICA, with respect to the SMV, has only been noted in one study, with a total pattern rate of 0.6 % [13, 18, 22]. Therefore, when the ICA runs ventrally to the SMV, surgeons should be aware that the RCA is also likely to run ventrally, and should thus be careful to prevent injuring the RCA.
In the current study, we were unable to determine the accuracy of 3D reconstruction with the software used. However, 3D-CT has been reported to have accuracies of 100 and 90.6 % when assessing the hepatic artery and stenoses of the lower extremity arteries, respectively [25, 26]. Therefore, we conclude that 3D-CT angiography is accurate and reliable for evaluating the SMA.
In conclusion, 3D-CT angiography can aid surgeons in identifying and understanding the anatomical vascular variations and intersectional patterns of the RCA, ICA, and SMV. Developing awareness of these variations can aid in the prevention of unexpected vascular injury during laparoscopic right-sided colon surgery.
References
Veldkamp R, Kuhry E, Hop WC, Jeekel J, Kazemier G, Bonjer HJ, et al. (2005) Laparoscopic surgery versus open surgery for colon cancer: short-term outcomes of a randomised trial. Lancet Oncol 6:477–484
Bonjer HJ, Hop WC, Nelson H, Sargent DJ, Lacy AM, Castells A, et al. (2007) Laparoscopically assisted vs open colectomy for colon cancer: a meta-analysis. Arch Surg 142:298–303
van der Pas MH, Haglind E, Cuesta MA, Furst A, Lacy AM, Hop WC, et al. (2013) Laparoscopic versus open surgery for rectal cancer (COLOR II): short-term outcomes of a randomised, phase 3 trial. Lancet Oncol 14:210–218
Mari FS, Nigri G, Pancaldi A, De Cecco CN, Gasparrini M, Dall’Oglio A, et al. (2013) Role of CT angiography with three-dimensional reconstruction of mesenteric vessels in laparoscopic colorectal resections: a randomized controlled trial. Surg Endosc 27:2058–2067
Mayo CW (1955) Blood supply of the colon: surgical considerations. Surg Clin North Am 35:1117–1122
Griffiths JD (1956) Surgical anatomy of the blood supply of the distal colon. Ann R Coll Surg Engl 19:241–256
Michels NA, Siddharth P, Kornblith PL, Parke WW (1965) The variant blood supply to the descending colon, rectosigmoid and rectum based on 400 dissections. Its importance in regional resections: a review of medical literature. Dis Colon Rectum 8:251–278
Lee SW, Shinohara H, Matsuki M, Okuda J, Nomura E, Mabuchi H, et al. (2003) Preoperative simulation of vascular anatomy by three-dimensional computed tomography imaging in laparoscopic gastric cancer surgery. J Am Coll Surg 197:927–936
Kock MC, Adriaensen ME, Pattynama PM, van Sambeek MR, van Urk H, Stijnen T, et al. (2005) DSA versus multi-detector row CT angiography in peripheral arterial disease: randomized controlled trial. Radiology 237:727–737
Bilhim T, Pereira JA, Tinto HR, Fernandes L, Duarte M, O’Neill JE, et al. (2015) Middle rectal artery: myth or reality? Retrospective study with CT angiography and digital subtraction angiography. Surg Radiol Anat 35:517–522
Spasojevic M, Stimec BV, Gronvold LB, Nesgaard JM, Edwin B, Ignjatovic D (2011) The anatomical and surgical consequences of right colectomy for cancer. Dis Colon Rectum 54:1503–1509
Spasojevic M, Stimec BV, Fasel JF, Terraz S (2011) Ignjatovic D (2011) 3D relations between right colon arteries and the superior mesenteric vein: a preliminary study with multidetector computed tomography. Surg Endosc 25:1883–1886
Tajima Y, Ishida H, Ohsawa T, Kumamoto K, Ishibashi K, Haga N, et al. (2011) Three-dimensional vascular anatomy relevant to oncologic resection of right colon cancer. Int Surg 96:300–304
Watanabe T, Itabashi M, Shimada Y, Tanaka S, Ito Y, Ajioka Y, et al. (2015) Japanese Society for Cancer of the Colon and Rectum (JSCCR) guidelines 2014 for treatment of colorectal cancer. Int J Clin Oncol 20:207–239
Liang JT, Lai HS, Huang J, Sun CT (2015) Long-term oncologic results of laparoscopic D3 lymphadenectomy with complete mesocolic excision for right-sided colon cancer with clinically positive lymph nodes. Surg Endosc 29:2394–2401
Sonneland J, Anson BJ, Beaton LE (1958) Surgical anatomy of the arterial supply to the colon from the superior mesenteric artery based upon a study of 600 specimens. Surg Gynecol Obstet 106:385–398
Garcia-Ruiz A, Milsom JW, Ludwig KA, Marchesa P (1996) Right colonic arterial anatomy. Implications for laparoscopic surgery. Dis Colon Rectum 39:906–911
Shatari T, Fujita M, Nozawa K, Haku K, Niimi M, Ikeda Y, et al. (2003) Vascular anatomy for right colon lymphadenectomy. Surg Radiol Anat 25:86–88
Ignjatovic D, Sund S, Stimec B, Bergamaschi R (2007) Vascular relationships in right colectomy for cancer: clinical implications. Tech Coloproctol 11:247–250
Spasojevic M, Stimec BV, Dyrbekk AP, Tepavcevic Z, Edwin B, Bakka A, et al. (2013) Lymph node distribution in the d3 area of the right mesocolon: implications for an anatomically correct cancer resection. A postmortem study. Dis Colon Rectum 56:1381–1387
Yada H, Sawai K, Taniguchi H, Hoshima M, Katoh M, Takahashi T (1997) Analysis of vascular anatomy and lymph node metastases warrants radical segmental bowel resection for colon cancer. World J Surg 21:109–115
Hirai K, Yoshinari D, Ogawa H, Nakazawa S, Takase Y, Tanaka K, et al. (2013) Three-dimensional computed tomography for analyzing the vascular anatomy in laparoscopic surgery for right-sided colon cancer. Surg Laparosc Endosc Percutan Tech 23:536–539
Nesgaard JM, Stimec BV, Bakka AO, Edwin B, Ignjatovic D (2015) Navigating the mesentery: a comparative pre- and per-operative visualization of the vascular anatomy. Color Dis 17:810–818
Kaye TL, West NP, Jayne DG, Tolan DJ (2015) CT assessment of right colonic arterial anatomy pre and post cancer resection—a potential marker for quality and extent of surgery? Acta Radiol 57:394–400
Yang J, Fang CH, Fan YF, Xiang N, Liu J, Zhu W, et al. (2014) To assess the benefits of medical image three-dimensional visualization system assisted pancreaticoduodenctomy for patients with hepatic artery variance. Int J Med Robot 10:410–417
Iezzi R, Santoro M, Dattesi R, la Torre MF, Guerra A, Di Stasi C, et al. (2013) Diagnostic accuracy of CT angiography in the evaluation of stenosis in lower limbs: comparison between visual score and quantitative analysis using a semiautomated 3D software. J Comput Assist Tomogr 37:419–425
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Murono, K., Kawai, K., Ishihara, S. et al. Evaluation of the vascular anatomy of the right-sided colon using three-dimensional computed tomography angiography: a single-center study of 536 patients and a review of the literature. Int J Colorectal Dis 31, 1633–1638 (2016). https://doi.org/10.1007/s00384-016-2627-1
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-016-2627-1