Abstract
Background
Anastomotic dehiscence is the most severe surgical complication after large bowel resection. This study was designed to assess the incidence, to observe the consequences, and to identify the risk factors associated with anastomotic leakage after colorectal surgery.
Materials and methods
All procedures involving anastomoses of the colon or the rectum, which were performed between November 2002 and February 2006 in a single institution, were prospectively entered into a computerized database.
Results
One thousand eighteen colorectal resections and 811 anastomoses were performed over this 40-month period. The most frequent procedures were sigmoid (276) and right colectomies (217). The overall anastomotic leak rate was 3.8%. The mortality rate associated with anastomotic leak was 12.9%. In univariate analysis, the following parameters were associated with an increased risk for anastomotic dehiscence: (1) ASA score ≥ 3 (p = 0.004), (2) prolonged (>3 h) operative time (p = 0.02), (3) rectal location of the disease (p < 0.001), (4) and a body mass index > 25 (p = 0.04). In multivariate analysis, ASA score ≥ 3 (OR = 2.5; 95% CI 1.5–4.3, p < 0.001), operative time > 3 h [OR = 3.0; 95% CI 1.1–8.0, p = 0.02), and rectal location of the disease (OR = 3.75; 95% CI 1.5–9.0 (vs left colon), p = 0.003; OR = 7.69; 95% CI 2.2–27.3 (vs right colon), p = 0.001] were factors significantly associated with a higher risk of anastomotic dehiscence.
Conclusions
Three risk factors for anastomotic leak have been identified, one is patient-related (ASA score), one is disease-related (rectal location), the third being surgery-related (prolonged operative time). These factors should be considered in perioperative decision-making regarding defunctioning stoma formation.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Anastomotic leakage is the most feared complication specific to colorectal surgery, leading to significant morbidity, increased mortality, prolonged hospital stay, and considerable extra cost. Its reported prevalence varies widely from 1 to 39%, but clinically significant leaks probably occur in 3–6% of cases, depending on the definition and the type of resection undertaken [1]. There is no universally accepted definition of a dehiscent colorectal anastomosis, which may present (a) as a generalized peritonitis requiring abdominal reoperation, (b) as fecal discharge from the wound and/or drain, (c) as a localized abscess, which may be amenable to computed tomography (CT) scan-guided percutaneous drainage, and (d) as an extravasation of radiological contrast in an otherwise asymptomatic patient, which may only require surveillance [2].
Several factors have been shown to have independent prognostic significance for anastomotic leakage, including diverticular disease [3], intraoperative septic conditions [4], male gender [5], smoking/alcohol abuse [6], as well as ASA score and emergency surgery [7]. The most significant risk factor for anastomotic leak remains, however, the site of the anastomosis, with leak rates of 2–4% in intra- vs 8–12% in infraperitoneal anastomoses [8]. In fact, Rullier et al. found that the risk of leakage was six times higher for anastomoses situated less than 5 cm from the anal verge than for those situated above 5 cm [9]. The majority of the large (>700 anastomoses) series, however, report either the experience of highly specialized surgeons over a long period of time (>10 years) [10, 11]; the results of multicenter trials [12, 13]; are limited to anastomoses above the pelvic peritoneal reflection [7]; focus on specific surgical techniques [14, 15]; or are retrospective in nature [16].
Therefore, the aim of this prospective study was (1) to identify the risk factors associated with for anastomotic leakage and (2) to evaluate the outcome of this type of complication in a nonselected series of patients who underwent colorectal resection in a single institution over a relatively short period of time.
Material and methods
From November 2002 until February 2006, all consecutive patients undergoing elective or emergency resection of the colon or rectum in our institution were prospectively included in this study and were entered into a prospective database. The University Hospital in Geneva is the only public medical institution in a mainly urban area with a population of approximately 500,000 inhabitants. The results in a larger series of patients in terms of morbidity and mortality have been previously reported [17]. Perioperative intravenous antibiotic prophylaxis was used in all patients. Most of them received a single dose of ceftriaxone 2G IV and metronidazole 500 MG IV at the time of induction. A majority of patients (>85%) did not receive any oral bowel preparation before surgery, in accordance to the results of a randomized controlled trial previously undertaken in our institution [18]. Our current policy is to restrict the use of mechanical bowel preparation in three different clinical situations: (1) patients scheduled for an APR, (2) patients who may need a perioperative colonoscopy, and (3) patients who are scheduled for a low anterior resection and in whom a diverting ileostomy is anticipated.
The structured sheet for data collection included the following items:
-
1.
Patient characteristics: gender, age, American Society of Anaesthesiology (ASA) score, body mass index (BMI), and comorbidities (cardiopulmonary, neurological, hepatic, renal…).
-
2.
Disease features: cancer, polyp, diverticulosis, diverticulitis, inflammatory bowel disease, other, and location of the pathology.
-
3.
Surgical procedure: urgent or elective, open or laparoscopic, type of anesthesia, type of incision, duration of the procedure, blood loss, blood transfusion, type of resection (right, transverse, left, sigmoid, low anterior, abdomino-perineal), and type and location of anastomosis (manual or stapled, end-to-end, side-to-end, side-to-side, ileocolic, colocolic, colorectal, coloanal, ileorectal, ileoanal).
-
4.
Postoperative events: anastomotic leak, mortality, morbidity, the reoperation, postoperative fever, prolonged ileus…
Anastomotic leakage was defined before the beginning of the study as either:
-
1.
Radiological: demonstration of contrast extravasation on abdominal computed tomography scans with triple contrast or by gastrograffin enema
-
2.
Causing diffuse peritonitis: presence of fecal fluid at relaparotomy
-
3.
Causing local sepsis: presence of a localized abscess in the vicinity of the anastomosis
-
4.
Fecal discharge from the drain/wound
In practice, we did not perform any routine contrast enema in asymptomatic patients, but we had a low threshold for abdomen/pelvic imaging with triple contrast CT scan in patients with suspected anastomotic leak, either clinically (pain, fever, abdominal tenderness, prolonged ileus) or biologically (persistently elevated white blood cell or C-reactive protein).
Statistical analysis
Descriptive statistics were summarized as means, standard deviations, medians, and ranges for the continuous variables and as frequencies and ranges for the categorical variables using the SAS V8.2 statistical software. When inference testing was completed, results with a p value less than or equal to 0.05 were considered statistically significant. Both univariable and multivariable logistic regression modeling techniques were used to identify risk factors for anastomotic leak. Parameter estimates, standard errors, odds ratios, and 95% confidence intervals for the odds ratios were reported along with the p values from the logistic regression modeling.
Results
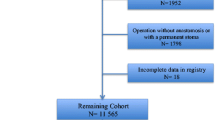
Over a 40-month period, 811 anastomoses were performed in 423 women (52.4%) and 384 men (47.6%) with a median age of 67 (range, 17–98) years. Four patients had two anastomoses (right colectomy + low anterior resection). The median duration of hospital stay was 11 (range, 2–205) days. The characteristics of patients in this series are summarized in Table 1. One half of the operations were performed for tumors and one third for diverticular disease. The median duration of the procedures was 180 (range, 50–640) minutes. Emergency procedures were performed in 128 (16%) patients. A total of 231 patients (29%) presented with an ASA score ≥ 3. We performed 276 sigmoidectomies, 217 right colectomies, 99 low anterior resections, 86 left colectomies, 29 subtotal colectomies, 45 reversal of Hartmann, 40 ileocaecal resections, 11 proctocolectomies, and 8 transverse colectomies. A total of 184 operations (22.8%) were performed by laparoscopy, with a 12.8% conversion rate.
The overall anastomotic leak rate was 3.8% (31 out of 811). The mortality rate associated with anastomotic leak was 12.9%. The overall mortality rate was 2.7% in the group of patients without a dehiscence. Low anterior resections and subtotal colectomies were the two procedures with the higher incidence of anastomotic leakage (11 and 13%, respectively). Eleven (35.4%) patients with an anastomotic leakage needed a reoperation for fecal diversion. The median delay between the first operation and the return to the operating room for anastomotic leak was six (range, 4–28) days. Twenty patients were conservatively treated with CT scan-guided radiological drainage and/or systemic antibiotics.
In univariate analysis (Table 2), the following parameters were associated with an increased risk for anastomotic dehiscence: (1) ASA score ≥ 3 (p = 0.004), (2) a prolonged (>3 h) operative time (p = 0.02), (3) rectal location of disease (p < 0.001), (4) infraperitoneal anastomosis (p = 0.02), (5) and a BMI > 25 (p = 0.04).
In multivariate analysis (Table 3), ASA score ≥ 3 (OR = 2.53; 95% CI 1.5–4.3, p < 0.001), a prolonged operative time (OR = 3.07; 95% CI 1.1–8.0, p = 0.02), and rectal location of the disease [OR = 7.69; 95% CI 2.2–27.3 (p = 0.001) for rectum vs right location, and OR = 3.75; 95% CI 1.5–9.0 (p = 0.003) for rectum vs left location] were factors significantly associated with a higher risk of anastomotic dehiscence.
Discussion
The data presented in this paper indicate that the overall anastomotic leak rate after colorectal surgery in a single teaching institution is inferior to 4% and that two thirds of these cases were managed conservatively. Anastomotic dehiscence, however, remains a life-threatening complication, associated with a significant (13%) mortality and a prolonged (28 days) hospital stay. The risk factors for such a complication included ASA score > 3, prolonged duration of surgery, and an infraperitoneal anastomosis.
The overall anastomotic leak rate of 3.8% reported herein is similar to most other published series (Table 4), and it is interesting to note that the dehiscence rate of low anterior resections (12%) in this study is identical to those reported by the authors of the two most recent randomized trials on adjuvant radiation therapy for rectal cancer [19, 20]. However, the reoperation rate in our study (35%) compares favorably to other series reporting usually reoperation in 50 to 60% of patients with anastomotic dehiscence [21, 22] and up to 95% for leaks occurring after low anterior resections [23]. The mortality rate associated with leakage in this series (13%), although being fivefold higher than in patients without dehiscence (2.7%), is also comparable to those reported in other centers, ranging from 10 to 16% [24, 25, 26]. This relative low reoperation and mortality rates in patients with anastomotic dehiscence may be explained by the routine use of a loop ileostomy in our institution for all patients who underwent either a colo-anal or an ileo-anal anastomosis. It is known that proximal fecal diversion in itself will not reduce the incidence of a leak, but, in association with early recognition of the complication, it represents currently the best strategy to minimize the consequences of severe pelvic sepsis [27].
Three parameters were identified in multivariate analysis as significant risk factors for anastomotic leakage: ASA score ≥ 3, a prolonged (>3 h) operative time, and anastomosis below the peritoneal reflection. In accordance with most authors, the ASA score ≥ 3 was strongly correlated with an increased risk for anastomotic leak [7, 21, 26, 28]: In our series, for every unit increase in ASA score, there is a 2.5 times increased risk of leak. Prolonged operating time has frequently been identified as a risk factor in univariate [4, 14] but more rarely in multivariate [26, 29] analysis: It is likely that long operation time reflects intraoperative difficulties, particularly, when working low in the pelvis or on account of adhesions from previous operations. Finally, anastomosis location within the rectum is over seven times more likely to leak than an ileocolic (right colon) and almost four times more likely to leak than a colocolic anastomosis (left colon).
Recent studies have well documented that anastomotic dehiscence after surgery for colorectal cancer compromises not only the immediate prognosis but, in addition, is associated with worse long-term survival and/or increased rate of local recurrence after a potentially curative resection [30, 31]. Therefore, it is critical to identify pre- or peroperatively high-risk patients to adapt the surgical strategy. We identified three risk factors for anastomotic leak in multivariate analysis: One is patient-related (ASA score), one is disease-related (infraperitoneal location of the anastomosis), the third being directly related to the surgical procedure (prolonged operating time). These factors should be considered in peroperative decision-making regarding defunctioning stoma formation.
References
Chambers WM, Mortensen NJ (2004) Postoperative leakage and abscess formation after colorectal surgery. Best Pract Res Clin Gastroenterol 18:865–880
Bruce J, Krukowski ZH, Al-Khairy G, Russell EM, Park KG (2001) Systematic review of the definition and measurement of anastomotic leak after gastrointestinal surgery. Br J Surg 88:1157–1168
Platell C, Barwood N, Dorfmann G, Makin G (2007) The incidence of anastomotic leaks in patients undergoing colorectal surgery. Colorectal Dis 9:71–79
Alves A, Panis Y, Trancart D, Regimbeau JM, Pocard M, Valleur P (2002) Factors associated with clinically significant anastomotic leakage after large bowel resection: multivariate analysis of 707 patients. World J Surg 26:499–502
Lipska MA, Bissett IP, Parry BR, Merrie AE (2006) Anastomotic leakage after lower gastrointestinal anastomosis: men are at a higher risk. ANZ J Surg 76:579–585
Sorensen LT, Jorgensen T, Kirkeby LT, Skovdal J, Vennits B, Wille-Jorgensen P (1999) Smoking and alcohol abuse are major risk factors for anastomotic leakage in colorectal surgery. Br J Surg 86:927–931
Choi HK, Law WL, Ho JW (2006) Leakage after resection and intraperitoneal anastomosis for colorectal malignancy: analysis of risk factors. Dis Colon Rectum 49:1719–1725
Yeh CY, Changchien CR, Wang JY, Chen JS, Chen HH, Chiang JM, Tang R (2005) Pelvic drainage and other risk factors for leakage after elective anterior resection in rectal cancer patients: a prospective study of 978 patients. Ann Surg 241:9–13
Rullier E, Laurent C, Garrelon JL, Michel P, Saric J, Parneix M (1998) Risk factors for anastomotic leakage after resection of rectal cancer. Br J Surg 85:355–358
Hyman N, Manchester TL, Osler T, Burns B, Cataldo PA (2007) Anastomotic leaks after intestinal anastomosis: it’s later than you think. Ann Surg 245:254–258
Killingback M, Barron P, Dent O (2002) Elective resection and anastomosis for colorectal cancer: a prospective audit of mortality and morbidity 1976–1998. ANZ J Surg 72:689–698
Kockerling F, Rose J, Schneider C, Scheidbach H, Scheuerlein H, Reymond MA, Reck T et al (1999) Laparoscopic colorectal anastomosis: risk of postoperative leakage. Results of a multicenter study. Laparoscopic Colorectal Surgery Study Group (LCSSG). Surg Endosc 13:639–644
Merad F, Hay JM, Fingerhut A, Yahchouchi E, Laborde Y, Pelissier E et al (1999) Is prophylactic pelvic drainage useful after elective rectal or anal anastomosis? A multicenter controlled randomized trial. French Association for Surgical Research. Surgery 125:529–535
Vignali A, Fazio VW, Lavery IC, Milsom JW, Church JM, Hull TL, Strong SA, Oakley JR (1997) Factors associated with the occurrence of leaks in stapled rectal anastomoses: a review of 1,014 patients. J Am Coll Surg 185:105–113
Peeters KC, Tollenaar RA, Marijnen CA, Klein Kranenbarg E, Steup WH, Wiggers T, Rutten HJ, van de Velde CJ (2005) Risk factors for anastomotic failure after total mesorectal excision of rectal cancer. Br J Surg 92:211–216
Golub R, Golub RW, Cantu R Jr., Stein HD (1997) A multivariate analysis of factors contributing to leakage of intestinal anastomoses. J Am Coll Surg 184:364–372
Buchs NC, Gervaz P, Bucher P, Huber O, Mentha G, Morel Ph (2007) Lessons learned from one thousand consecutive colonic resections in a teaching hospital. Swiss Med Wkly 137:259–264
Bucher P, Gervaz P, Soravia C, Mermillod B, Erne M, Morel P (2005) Randomized clinical trial of mechanical bowel preparation versus no preparation before elective left-sided colorectal surgery. Br J Surg 92:409–414
Marijnen CAM, Kapiteijn E, van de Velde CJH, Martijn H, Steup WH, Wiggers T, Klein Kranenbarg E, Leer JWH, Cooperative Investigators of the Dutch Colorectal Cancer Group (2002) Acute side effects and complications after short-term preoperative radiotherapy combined with total mesorectal excision in primary rectal cancer: report of a multicenter randomized trial. J Clin Oncol 20:817–825
Sauer R, Becker H, Hohenberger W, Rödel C, Wittekind C, Fietkau R, Martus P, Tschmelitsch J, Hager E, Hess CF, Karstens JH, Liersch T, Schmidberger H, Raab R, For the German Rectal Cancer Study Group (2004) Preoperative versus postoperative chemoradiotherapy for rectal cancer. New Engl J Med 351:1731–1740
Alves A, Panis Y, Pocard M, Regimbeau JM, Valleur P (1999) Management of anastomotic leakage after nondiverted large bowel resection. J Am Coll Surg 189:554–559
Wong NY, Eu KW (2005) A defunctioning ileostomy does not prevent clinical anastomotic leak after a low anterior resection: a prospective, comparative study. Dis Colon Rectum 48:2076–2079
Law WI, Chu KW, Ho JW, Chan CW (2000) Risk factors for anastomotic leakage after low anterior resection with total mesorectal excision. Am J Surg 179:92–96
McArdle CS, McMillan DC, Hole DJ (2005) Impact of anastomotic leakage on long-term survival of patients undergoing curative resection for colorectal cancer. Br J Surg 92:1150–1154
Branagan G, Finnis D, Wessex Colorectal cancer Audit Working Group (2005) Prognosis after anastomotic leakage in colorectal surgery. Dis Colon Rectum 48:1021–1026
Biondo S, Pares D, Kreisler E, Rague JM, Fraccalvieri D, Ruiz AG, Jaurrieta E (2005) Anastomotic dehiscence after resection and primary anastomosis in left-sided colonic emergencies. Dis Colon Rectum 48:2272–2280
Alberts JC, Parvaiz A, Moran BJ (2003) Predicting risk and diminishing the consequences of anastomotic dehiscence following rectal resection. Colorectal Dis 5:478–482
Makela JT, Kiviniemi H, Laitinen S (2003) Risk factors for anastomotic leakage after left-sided colorectal resection with rectal anastomosis. Dis Colon Rectum 46:653–660
Konishi T, Watanabe T, Kishimoto J, Nagawa H (2006) Risk factors for anastomotic leakage after surgery for colorectal cancer: results of prospective surveillance. J Am Coll Surg 202:439–444
Walker KG, Bell SW, Rickard MJ, Mehanna D, Dent OF, Chapuis PH, Bokey EL (2004) Anastomotic leakage is predictive of diminished survival after potentially curative resection for colorectal cancer. Ann Surg 240:255–259
Law WL, Choi HK, Lee YM, Ho JW, Seto CL (2007) Anastomotic leakage is associated with poor long-term outcome in patients after curative colorectal resection for malignancy. J Gastrointest Surg 11:8–15
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Buchs, N.C., Gervaz, P., Secic, M. et al. Incidence, consequences, and risk factors for anastomotic dehiscence after colorectal surgery: a prospective monocentric study. Int J Colorectal Dis 23, 265–270 (2008). https://doi.org/10.1007/s00384-007-0399-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-007-0399-3