Abstract
Background
Adult intestinal organoids have been used to study ex vivo intestinal injury in adulthood. However, the neonatal intestinal epithelium has many unique features that are different from adult mature intestine. Establishing a neonatal ex vivo organoid model is essential to study the epithelial physiology in early postnatal development and to investigate derangements associated with disease processes during the neonatal period like necrotizing enterocolitis (NEC).
Methods
Fresh and frozen terminal ileum was harvested from mice pups on postnatal day 9. Crypts were isolated and organoids were cultured. Organoids were exposed to hypoxia and lipopolysaccharide (LPS) for 48 h to induce epithelial injury. Inflammatory cytokines and tight junction proteins were evaluated.
Results
Robust intestinal organoids can be formed from both fresh and frozen intestinal tissue of neonatal mice pups. Hypoxia and LPS administration induced intestinal inflammation and disrupted tight junctions in these neonatal intestinal organoids.
Conclusions
We have established a novel method to grow organoids from neonatal intestine. We demonstrated that these organoids respond to the injury occurring during neonatal intestinal diseases such as NEC by increasing the organoid inflammation and by disrupting the organoid barrier function. Organoids provide an ex vivo platform to study intestinal physiology and pathology during the neonatal period.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The intestine is a particularly complex organ due to its physiological features and structures. The essential function of the intestine is to absorb nutrients from the intestinal lumen. Intestinal epithelium is organized into crypts and villi in order to increase absorptive surface area [1]. The direct contact between the intestinal bacteria and the epithelial cell surface has to be tightly controlled to avoid bacterial invasion triggering an immune response [2]. Due to these complexities, multiple environmental and intrinsic factors are involved and contribute towards the intestine’s postnatal development and intestinal injury during the neonatal period. Consequently, a simple experimental model of intestinal epithelium is essential to study the pathophysiology of neonatal intestinal disorders.
Intestinal epithelium is characterised by high self-renewing capacity to maintain intestinal viability [3]. Intestinal epithelial organoids are derived from intestinal crypts and cultured to represent the tissue-resident intestinal stem cells which retain their ability to regenerate epithelial tissue [4], self-renewal, and multi-lineage differentiation properties even after prolonged culturing [5]. Recent advances in organoid culture technology have provided a greater understanding of stem cell biology, organogenesis, and disease pathology, thus enabling human development and disease modeling in vitro [6,7,8].
However, neonatal intestines are immature at birth and developed postnatally. Therefore, the neonatal intestinal epithelium has many unique features including size, structure, and function that differ from mature adult intestinal epithelium [9,10,11]. Compare to adult intestine, the neonatal intestine has less microvascular folds [12], fewer intestinal epithelium cell types [13], lower intestinal renewal capacity [14], immature barrier function [15], less developed microbiome community [16] and different immune responses [17]. Consequently, the immature neonatal intestine is more susceptible to develop several intestinal injuries such as NEC.
Thus, creating a neonatal ex vivo model is essential to study the epithelium physiology in intestinal pathological processes occurring in neonates. The aim of this study was to report our newly established protocol to form robust neonatal intestinal organoids and to describe the response of these neonatal-derived organoids to epithelium injury.
Methods
Fresh intestinal organoids
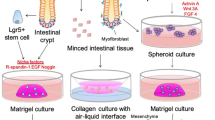
Intestinal organoids were cultured according to the protocol from StemCell Technologies (Cambridge, MA). Terminal ileum was harvested from C57BL/6 mice pups at postnatal day 9. The tissue was cut into small segments. Intestinal crypts were isolated by digestion with Gentle Cell Dissociation Reagent (StemCell Technologies, Cambridge, MA) for 15 min and pelleted by centrifugation. Crypts were then re-suspended in Matrigel (Corning, New York) and transferred into 24-well plates. After polymerization, mouse IntestiCult organoid growth medium (StemCell Technologies, Cambridge, MA) supplemented with penicillin–streptomycin (100 U/mL) was overlaid on the gel in each well. Organoids were maintained in a 37 °C incubator with the culture medium replaced every 2 days.
To induce intestinal epithelial injury, organoids were exposed to hypoxia (5% O2/95%N2) and lipopolysaccharide (LPS; 200 µg/mL, Sigma-Aldrich, St. Louis, MI) for 48 h, which have been reported as stress factors in an in vitro environment to induce intestinal cell injury [18].
Snap frozen tissue organoids
Intestinal tissue (ileum) was harvested from C57BL/6 mice pups at postnatal day 9 and snap-frozen in CryoStor freezing medium. This was then stored at − 80 °C for later use. When used, the frozen tissue was thawed and used to grow organoids as mentioned above.
Forskolin-induced organoid swelling
Forskolin-induced organoid swelling was conducted to study the epithelial integrity and permeability [19]. Forskolin at 50 mM (Sigma-Aldrich, St. Louis, MI) was added into culture medium to induce organoid swelling for 30 min. Samples were imaged every 5 min using a Nikon TE-2000 digital microscope equipped with a Hamamatsu C4742-80-12AG camera.
Gene expression
RNA was isolated with TRIzol (Invitrogen, Carlsbad, CA) after removing culture medium. Total RNA (1 µg) was reverse transcribed using qScript cDNA supermix (Quanta Biosciences, Gaithersburg, MD). SYBR green-based RT-qPCR was performed in a CF384 C1000 Thermal Cycler (Biorad, Hercules, CA) using Evagreen Supermix (Biorad, Hercules, CA), as previously described [20]. Data were analyzed using CFX Manager 3.1 (Biorad, Hercules, CA). Results are from three independent experiments each performed in triplicate. Expression levels were calculated by the ∆∆Ct method and normalized to housekeeping genes Glyceraldehyde 3-phosphate dehydrogenase (GAPDH) and ribosomal protein large, P0 (RPLP0).
Immunostaining
Organoids were fixed using 4% paraformaldehyde for 30 min and were subsequently permeabilized with 0.1% Triton X-100. After blocking of non-specific binding, organoids were incubated overnight at 4 °C with 1 in 500 dilutions of primary antibodies for Zonula occludens-1 (ZO-1) and Claudin-3 (Cl3) (Cell Signaling Technology, Danvers, MA). Organoids were then incubated with 1 in 1000 diluted secondary antibodies and DAPI (Vector Laboratories, Burlington, ON) for nuclei at room temperature for 2 h. Samples were imaged using a Nikon TE-2000 digital microscope equipped with a Hamamatsu C4742-80-12AG camera.
Statistics
Results are presented as means ± SEM for normally distributed data, or median and range for not normally distributed data (Kolmogorov–Smirnov test). Groups were compared using student’s t test. p < 0.05 was considered statistically significant.
Results
Fresh derived neonatal intestinal organoids
Intestinal ileal crypts from neonatal pups were isolated and formed into organoids. After 5 days of culture, the ileal intestinal organoids formed and started budding (Fig. 1a). Ileal intestinal organoids had an increase in number and surface area from day 2 to day 5 of culturing (Fig. 1b).
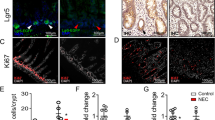
Organoids cultured from fresh neonatal mice terminal ileum. a Corresponding representative micrographs of ileal mouse organoids from fresh tissue after 2 days and 5 days of culturing. b Quantification of ileal organoids per image and surface area (µm2). Experiments were independently repeated three times. Data are presented as means ± SD, compared using student’s t tests
Established an ex vivo model for neonatal intestinal epithelial injury
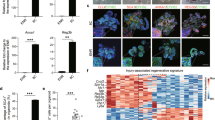
To mimic NEC-like neonatal intestinal injury ex vivo, we incubated the organoids in a hypoxic condition and administered LPS, two stress factors which can induce the development of intestinal cell injury [18]. Hypoxia and LPS exposure induced intestinal inflammation, as indicated by increased gene expression of pro-inflammation cytokines IL-6 and TNFɑ (Fig. 2a). Tight junction marker ZO-1 showed an internal ring immunostaining pattern in the control organoids which was disrupted after exposure to hypoxia and LPS (Fig. 2b). Similarly, tight junction marker Cl-3 relocated from the luminal to the outside membrane of the organoids (Fig. 2c). These data collectively suggest that NEC-like epithelial injury is induced in neonatal intestinal organoids by exposure to hypoxia and LPS.
Ex vivo model of neonatal intestinal epithelial injury in organoids. Neonatal organoids were exposed to hypoxia and LPS to induce NEC-like ex vivo intestinal injury. Comparisons between control organoids and organoids exposed to hypoxia and LPS. a Quantification of gene expression levels of inflammation cytokines IL-6 and TNFɑ for the two groups. b Corresponding representative micrographs of tight junction ZO-1 staining in organoids of the two groups. Control organoids showed a complete ring-like structure and the hypoxia- and LPS-treated organoids showed disrupted ZO-1 as indicated by the white arrows. c Corresponding representative micrographs of tight junction marker Cl-3 staining in organoids of the two groups. Cl-3 marked by the white star relocated from the luminal to basal membrane of the organoids. Experiments were independently repeated three times. Data are presented as means ± SD, compared using student’s t tests
Frozen neonatal intestinal organoids
To enhance the translational applications of these novel techniques, we isolated the organoids not only from fresh intestinal tissue but also from frozen tissue. Intestinal crypts were isolated from frozen neonatal pup ileal tissue and grew into organoids. Similar to fresh tissue organoids, the frozen tissue organoids grew and increased in number and surface area (Fig. 3a, b). To test the viability of these organoids, Forskolin was added to induce organoid swelling. The organoids increased in size as the influx of water increased (Fig. 3c) indicating that the organoids derived from frozen tissue were robust.
Organoids cultured from frozen neonatal mice ileal tissue. a Corresponding representative micrographs of ileal mouse organoids from frozen tissue after 2 days and 5 days of culturing. b Quantification of ileal organoids per image and surface area (µm2). c Corresponding representative micrographs of ileal mouse organoid treated with 50 mM Forskolin to induce swelling at the time prior to treatment (T0) and 30 min after treatment (T30m). Experiments were independently repeated three times. Data are presented as means ± SD, compared using student’s t tests
Discussion
A novel technique is described for the development of intestinal organoids derived from neonatal intestine. We have established that these organoids can be grown from fresh as well as frozen ileum. In addition, the organoids maintain viability and respond to intestinal injury stress factors such as hypoxia or bacterial products (LPS). These organoids have the potential to enhance further research in neonatal intestinal pathophysiology and hold promise for the development of future therapeutic maneuvers.
Developing organoids was based on the knowledge acquired from in vitro studies which investigated the pathogenesis of diseases [6, 7]. Indeed, various studies have been using intestinal organoids from adult mouse to study the progression of intestinal injury [21, 22]. However, the neonatal intestinal epithelium has several characteristics that differ from mature adult intestinal epithelium. In this study, we have established a novel protocol to form robust neonatal intestinal organoids from fresh terminal ileum of newborn mice pups, which is the intestinal area most affected by NEC. This neonatal organoid platform allows us to develop a deeper understanding of the direct effects of injury to intestinal crypts and study the mechanism of action without the complex interference of other organs on the intestine.
Multiple stress factors have been reported for inducing in vitro cell injury; one previous study showed that hypoxia and LPS represent stress factors shown in NEC [18]. Similar to intestinal injury found in mice with NEC [23], the intestinal organoids showed increased inflammation. Disruption of tight junction ZO-1 and translocation of Cl-3 in organoids were also found after hypoxia and LPS administration which were comparable to the experimental NEC model [24, 25]. These findings demonstrate that neonatal mice organoids can be used to study NEC progression. Our findings are in line with a recent study showing that human fetal derived organoids are a relevant human preclinical model for NEC [26]. These findings collectively demonstrate the benefits of using neonatal mice pups or human fetal derived organoids in studying the changes on intestinal epithelium. This likely is applicable to the development of the ex vivo NEC model which can be used to study the pathophysiology of the disease, as well as develop therapeutic agents for NEC in the future.
Similar to a previous publication of successful organoids grown from tumor tissue [27], we have established the snap-frozen technique to preserve the intestinal tissue. We have been able not only to grow intestinal organoids from frozen tissue, but also to demonstrate that these organoids were viable. The Forskolin-induced swelling assay demonstrated integrity of the intestinal organoids [19]. Our observations showed that organoids derived from frozen tissue that have been kept for at least a week are comparable to organoids derived from fresh tissue. This technique is useful as it allows preservation of tissue for later analysis. This may be applicable clinically by allowing the effective preservation of human biopsy samples for later use. This circumvents the need to immediately grow organoids from fresh tissue which often may be difficult, impractical or require multiple biopsies at differing times. Further studies should investigate the growth of these neonatal-derived organoids from frozen tissue over a longer period of time.
In summary, we have established a valid protocol to form robust neonatal intestinal organoids, which will be useful to study the epithelium physiology in postnatal intestinal development and pathology processes in early intestinal disorders.
References
Walton KD, Freddo AM, Wang S, Gumucio DL (2016) Generation of intestinal surface: an absorbing tale. Development 143(13):2261–2272. https://doi.org/10.1242/dev.135400
Ley RE, Peterson DA, Gordon JI (2006) Ecological and evolutionary forces shaping microbial diversity in the human intestine. Cell 124(4):837–848. https://doi.org/10.1016/j.cell.2006.02.017
Cheng H, Leblond CP (1974) Origin, differentiation and renewal of the four main epithelial cell types in the mouse small intestine. V. Unitarian Theory of the origin of the four epithelial cell types. Am J Anat 141(4):537–561. https://doi.org/10.1002/aja.1001410407
Sato T, Clevers H (2013) Growing self-organizing mini-guts from a single intestinal stem cell: mechanism and applications. Science 340(6137):1190–1194. https://doi.org/10.1126/science.1234852
Yui S, Nakamura T, Sato T, Nemoto Y, Mizutani T, Zheng X, Ichinose S, Nagaishi T, Okamoto R, Tsuchiya K, Clevers H, Watanabe M (2012) Functional engraftment of colon epithelium expanded in vitro from a single adult Lgr5(+) stem cell. Nat Med 18(4):618–623. https://doi.org/10.1038/nm.2695
Clevers H (2016) Modeling development and disease with organoids. Cell 165(7):1586–1597. https://doi.org/10.1016/j.cell.2016.05.082
Schweiger PJ, Jensen KB (2016) Modeling human disease using organotypic cultures. Curr Opin Cell Biol 43:22–29. https://doi.org/10.1016/j.ceb.2016.07.003
Dutta D, Heo I, Clevers H (2017) Disease modeling in stem cell-derived 3D organoid systems. Trends Mol Med 23(5):393–410. https://doi.org/10.1016/j.molmed.2017.02.007
Stenson WF (2013) Postnatal growth in the intestine. Curr Opin Gastroenterol 29(2):107–111. https://doi.org/10.1097/MOG.0b013e32835d9ec3
Herbst JJ, Sunshine P (1969) Postnatal development of the small intestine of the rat. Changes in mucosal morphology at weaning. Pediatr Res 3(1):27–33
Paran TS, Rolle U, Puri P (2006) Postnatal development of the mucosal plexus in the porcine small and large intestine. Pediatr Surg Int 22(12):997–1001. https://doi.org/10.1007/s00383-006-1786-5
Unthank JL, Lash JM, Bohlen HG (1990) Maturation of the rat intestinal microvasculature from juvenile to early adult life. Am J Physiol 259(2 Pt 1):G282–G289. https://doi.org/10.1152/ajpgi.1990.259.2.G282
Trahair JF (1989) Remodeling of the rat small intestinal mucosa during the suckling period. J Pediatr Gastroenterol Nutr 9(2):232–237
Dehmer JJ, Garrison AP, Speck KE, Dekaney CM, Van Landeghem L, Sun X, Henning SJ, Helmrath MA (2011) Expansion of intestinal epithelial stem cells during murine development. PLoS One 6(11):e27070. https://doi.org/10.1371/journal.pone.0027070
Rouwet EV, Heineman E, Buurman WA, ter Riet G, Ramsay G, Blanco CE (2002) Intestinal permeability and carrier-mediated monosaccharide absorption in preterm neonates during the early postnatal period. Pediatr Res 51(1):64–70. https://doi.org/10.1203/00006450-200201000-00012
Baumler AJ, Sperandio V (2016) Interactions between the microbiota and pathogenic bacteria in the gut. Nature 535(7610):85–93. https://doi.org/10.1038/nature18849
Cummins AG, Thompson FM (1997) Postnatal changes in mucosal immune response: a physiological perspective of breast feeding and weaning. Immunol Cell Biol 75(5):419–429. https://doi.org/10.1038/icb.1997.67
Lee C, Minich A, Li B, Miyake H, Seo S, Pierro A (2018) Influence of stress factors on intestinal epithelial injury and regeneration. Pediatr Surg Int 34(2):155–160. https://doi.org/10.1007/s00383-017-4183-3
Dekkers JF, Wiegerinck CL, de Jonge HR, Bronsveld I, Janssens HM, de Winter-de Groot KM, Brandsma AM, de Jong NW, Bijvelds MJ, Scholte BJ, Nieuwenhuis EE, van den Brink S, Clevers H, van der Ent CK, Middendorp S, Beekman JM (2013) A functional CFTR assay using primary cystic fibrosis intestinal organoids. Nat Med 19(7):939–945. https://doi.org/10.1038/nm.3201
Li B, Lee C, Filler T, Hock A, Wu RY, Li Q, Chen S, Koike Y, Ip W, Chi L, Zani-Ruttenstock E, Maattanen P, Gonska T, Delgado-Olguin P, Zani A, Sherman PM, Pierro A (2017) Inhibition of corticotropin-releasing hormone receptor 1 and activation of receptor 2 protect against colonic injury and promote epithelium repair. Sci Rep 7:46616. https://doi.org/10.1038/srep46616
Sodhi CP, Neal MD, Siggers R, Sho S, Ma C, Branca MF, Prindle T Jr, Russo AM, Afrazi A, Good M, Brower-Sinning R, Firek B, Morowitz MJ, Ozolek JA, Gittes GK, Billiar TR, Hackam DJ (2012) Intestinal epithelial Toll-like receptor 4 regulates goblet cell development and is required for necrotizing enterocolitis in mice. Gastroenterology 143(3):708–718 e705. https://doi.org/10.1053/j.gastro.2012.05.053
McElroy SJ, Castle SL, Bernard JK, Almohazey D, Hunter CJ, Bell BA, Al Alam D, Wang L, Ford HR, Frey MR (2014) The ErbB4 ligand neuregulin-4 protects against experimental necrotizing enterocolitis. Am J Pathol 184(10):2768–2778. https://doi.org/10.1016/j.ajpath.2014.06.015
Zani A, Cananzi M, Fascetti-Leon F, Lauriti G, Smith VV, Bollini S, Ghionzoli M, D’Arrigo A, Pozzobon M, Piccoli M, Hicks A, Wells J, Siow B, Sebire NJ, Bishop C, Leon A, Atala A, Lythgoe MF, Pierro A, Eaton S, De Coppi P (2014) Amniotic fluid stem cells improve survival and enhance repair of damaged intestine in necrotising enterocolitis via a COX-2 dependent mechanism. Gut 63(2):300–309. https://doi.org/10.1136/gutjnl-2012-303735
Ling X, Linglong P, Weixia D, Hong W (2016) Protective effects of bifidobacterium on intestinal barrier function in LPS-induced enterocyte barrier injury of Caco-2 monolayers and in a rat NEC model. PLoS One 11(8):e0161635. https://doi.org/10.1371/journal.pone.0161635
Khailova L, Dvorak K, Arganbright KM, Halpern MD, Kinouchi T, Yajima M, Dvorak B (2009) Bifidobacterium bifidum improves intestinal integrity in a rat model of necrotizing enterocolitis. Am J Physiol Gastrointest Liver Physiol 297(5):G940–G949. https://doi.org/10.1152/ajpgi.00141.2009
Senger S, Ingano L, Freire R, Anselmo A, Zhu W, Sadreyev R, Walker WA, Fasano A (2018) Human fetal-derived enterospheres provide insights on intestinal development and a novel model to study necrotizing enterocolitis (NEC). Cell Mol Gastroenterol Hepatol 5(4):549–568. https://doi.org/10.1016/j.jcmgh.2018.01.014
Walsh AJ, Cook RS, Sanders ME, Arteaga CL, Skala MC (2016) Drug response in organoids generated from frozen primary tumor tissues. Sci Rep 6:18889. https://doi.org/10.1038/srep18889
Acknowledgements
This work is supported by a Canadian Institutes of Health Research (CIHR) Foundation Grant 353857. AP is the Robert M. Filler Chair of Surgery, The Hospital for Sick Children (HSC). BL is the recipient of HSC Restracomp Fellowship.
Author information
Authors and Affiliations
Contributions
BL, CL, and AP designed experiments; CL, MC, HM, DL, and RW performed experiments; BL, CL, and MC wrote the manuscript; AP provided advice and supervision; all the authors reviewed and revised the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interest.
Rights and permissions
About this article
Cite this article
Li, B., Lee, C., Cadete, M. et al. Neonatal intestinal organoids as an ex vivo approach to study early intestinal epithelial disorders. Pediatr Surg Int 35, 3–7 (2019). https://doi.org/10.1007/s00383-018-4369-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-018-4369-3