Abstract
Purpose
Given evolving imaging technologies, we noted significant variation in the diagnostic evaluation of pediatric choledochal cysts (CDC). To streamline the diagnostic approach to CDC, and minimize associated expenses, we compared typing accuracy and costs of ultrasound (US), intraoperative cholangiography (IOC), and magnetic resonance cholangiopancreatography (MRCP).
Methods
Records of 30 consecutive pediatric CDC patients were reviewed. Blinded to all clinical data, two pediatric radiologists reviewed all US, MRCPs, and IOCs to type CDCs according to the Todani classification. When compared with pathologic findings, the concordance between and accuracy of each diagnostic test were determined. Inflation-adjusted procedure charges and collections for imaging modalities were analyzed.
Results
Mean typing accuracy overlapped for US, IOC, and MRCP. Inter-rater reliability was 87 % for US (κ = 0.77), 80 % for IOC (κ = 0.62), and 60 % for MRCP (κ = 0.37). MRCP procedure charges ($1204.69) and collections ($420.85) exceeded IOC and US combined ($264.80 charges, p = 0.0002; $93.40 collections, p = 0.0021).
Conclusion
Our data support the use of US alone in the diagnosis of pediatric CDC when no intrahepatic biliary ductal dilatation is visualized. However, when dilated intrahepatic ducts are encountered on US, MRCP should be utilized to distinguish a type I from a type IV CDC, which may alter the operative approach.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Choledochal cysts are congenital dilatations of the extra and/or intrahepatic biliary tree that are postulated to arise secondary to pancreaticobiliary malunion (PBM), predisposing to reflux of pancreatic digestive enzymes into the biliary tree [1]. Over time, chronic exposure of the biliary epithelium to an admixture of digestive enzymes results in variable cystic dilatation of the extra and intrahepatic bile ducts and often leads to obstruction of this ductal network within the duodenum [2]. Given their protean anatomy, to optimize surgical correction, choledochal cysts are typed by the Todani classification, with the most common form being type I, which manifests as fusiform dilation of the common bile duct [3, 4].
The initial diagnosis of choledochal cysts is typically made by ultrasonography (US) [5]. To date, intraoperative cholangiography (IOC) has been the gold standard imaging modality to type choledochal cysts and to devise a strategy for surgical resection [3]. Recent imaging alternatives, including magnetic resonance cholangiopancreatography (MRCP) [6–9], endoscopic retrograde cholangiopancreatography (ERCP) [10], and three-dimensional US [11], have been demonstrated to be safe and effective measures in the diagnosis and mapping of pediatric biliary anomalies. However, few comparative studies have been done using these varied modalities in the pediatric population [12]. Furthermore, cost minimization has not previously been factored into the comparison of these tests in children.
The current economic climate in health-care necessitates physician assessment of resource utilization and identification of redundant costs in the effective care of patients. With the introduction of new imaging technologies, specifically magnetic resonance imaging (MRI), we have noted at our institution significant variation in the diagnostic evaluation of pediatric choledochal cysts (CDC). We aimed to determine whether utilization of all imaging modalities in the diagnostic evaluation of CDCs had increased over the last 12 years at our institution. We then focused on the three imaging modalities most commonly utilized and employed in an overlapping fashion in the diagnosis and assessment of CDCs: IOC, US, and MRCP; we sought to compare their accuracy in the typing of CDC by the Todani classification and to compare their costs using a cost minimization analysis.
Methods
Study cohort
The Institutional Review Board of Vanderbilt University Medical Center approved all studies (IRB# 110122). We conducted a retrospective chart review of medical records for all pediatric patients (age <18 years) who were diagnosed with CDC at our institution between 1 January 1999 and 1 February 2011. Querying billing records ICD-9 codes associated with biliary pathology identified 30 patients with a diagnosis of CDC. Collected information from chart review of these patients included gender, race, age, body weight, ASA class, associated congenital anomalies, whether the CDC was diagnosed prenatally, type of operation, estimated blood loss, operative time, need for transfusion, operative morbidity, and length of stay. Anatomic pathology reports were reviewed in detail to determine the type of choledochal cyst for each patient according to the Todani classification. To calculate the total number of imaging modalities utilized per patient, the medical records of these 30 patients were queried for all radiologic studies utilized in the initial diagnosis and assessment of the patient’s CDC including US, IOC, MRCP, CT scan, ERCP, and nuclear medicine hepatobiliary scan. CT scan, ERCP, and nuclear medicine hepatobiliary scan were used too infrequently at our institution to be included in any of the remaining analyses.
Radiologist review of imaging studies
To assess concordance and typing accuracy of each imaging modality used, the Vanderbilt electronic PACS system (AGFA HealthCare IMPAX 6; Mortsel, Belgium) was queried for all available US, IOC, and MRCPs performed in the initial workup of each patient’s CDC. Images from patients having a biliary cystic malformation with concomitant biliary atresia (n = 3) were excluded from analysis, since these patients are not accounted for in the Todani classification scheme. All studies were de-identified and reviewed independently by two pediatric radiologists, who were blinded to all clinical details and prior radiology reports (n = 23 US; n = 15 IOCs; n = 15 MRCPs). Choledochal cysts were typed after review of each imaging modality using the Todani classification [3]. Concordance between each imaging modality and between each radiologist was then estimated. To determine the typing accuracy of a given imaging modality for CDCs, results were compared for the type of CDC detailed in the patient’s pathology report. For MRCP and IOC, the radiologists also recorded whether the pancreatic duct could be visualized, and, if so, whether PBM was identified [1].
Cost minimization analysis
We queried the records of our billing department to identify all hospital charges associated directly with each US, IOC, and MRCP conducted in the patient cohort. In addition, procedure collections (accounts received) were recorded. Indirect costs and facility charges were not included in this analysis. All charges were adjusted for inflation using the Consumer Price Index for all Urban Consumers estimates specific to medical cost inflation and are indexed to the year 2011 [13].
Statistical analysis
To determine whether the number of all testing modalities (including US, IOC, CT scan, MRCP, hepatobiliary scan, and ERCP) per patient with a diagnosis of CDC has increased at our institution during the study period, we performed a linear regression analysis treating time in years as a continuous variable. Because demographic, clinical, and cost study data were not normally distributed, nonparametric statistical tests were utilized to determine significance: for categorical variables, we used Fisher’s exact test, and for continuous variables, we used Wilcoxon rank sum for hypothesis testing. Statistical significance was set at p < 0.05.
Typing accuracy by the Todani classification was calculated by determining the percentage of correctly typed CDCs when compared with pathology reports. Mean typing accuracy represents the average accuracy of the two reviewers in our study. Cohen’s kappa value was used to assess inter-observer agreement between the two blinded reviewers for the typing of CDC. We considered a value of >0.81 to represent excellent agreement and values of 0.61–0.80 and 0.41–0.60 to represent good and moderate agreement, respectively. Values <0.40 were considered to represent fair agreement. Fisher’s exact test was also used to compare the ability of MRCP and IOC to identify the pancreatic duct and PBM among the available studies. STATA version 11.2 (StataCorp LP; College Station, TX) was used for all statistical analyses.
Results
Description of cohort and utilization of imaging modalities
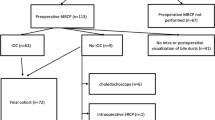
Demographic and outcome variables were collected from 30 patients identified for analysis and are summarized (Table 1). The total number of imaging modalities (including US, IOC, MRCP, CT scan, hepatobiliary scan, ERCP) per CDC patient increased marginally over the study period (Fig. 1a, p = 0.079). Of note, three patients were diagnosed with presumptive CDC prenatally, all by screening ultrasound (Table 1). Notably, the utilization of diagnostic imaging modalities varied during the study period and reflected surgeon preference; however, this could not be reasonably accounted for in the model due to small sample size. We noted significant overlap in the utilization of US, IOC, and MRCP in the initial diagnostic assessment of CDCs; 8 patients (26.7 %) underwent all three diagnostic tests (Fig. 1b).
a Linear regression analysis evaluating the use of diagnostic imaging modalities in the patient cohort during the study period demonstrates variability of resource utilization and a potential trend toward increased resource utilization over time (p = 0.079). Modalities included are US, IOC, CT scan, MRCP, hepatobiliary scan, and ERCP. b Overlapping use of imaging modalities in the diagnostic evaluation of pediatric choledochal cysts. Total n = 30. US ultrasound, IOC intraoperative cholangiography, MRCP magnetic resonance cholangiopancreatography
Concordance of US, IOC, and MRCP in the evaluation of choledochal cysts
Inter-rater agreements and mean typing accuracies for CDCs among the available 23 ultrasounds, 15 IOCs, and 15 MRCPs were calculated (Table 2). Inter-rater reliability (87 %; κ = 0.77) was highest for ultrasound and lowest for MRCP (60 %; κ = 0.37), while mean typing accuracy was highest for MRCP (80 %; SD = 28.3; Table 2). However, the confidence intervals for the three modalities overlap with respect to mean typing accuracy. We noted that nearly all observed discrepancies between the type of CDC diagnosed on imaging and the type by pathology reports arose from difficulty in distinguishing type I from type IV CDCs (89.5 % discrepancies for US, 92.3 % for IOC, and 83.3 % for MRCP).
MRCP visualized the pancreatic duct in 11/15 (73.3 %) cases, and PBM was identified in 6 of these 11 patients (54.5 %). IOC visualized the pancreatic duct in 6/15 (40 %) of cases, with all 6 having PBM. We did not detect a statistically significant difference in the ability of these two modalities to visualize the pancreatic duct (p = 0.139) or to identify PBM (p = 0.102).
Following the above analyses, we sought to evaluate the concordance of MRCP and IOC by reviewing studies from the eight patients who had available images from both modalities. Both radiologists were independently able to match all eight pairs (100 %) of imaging studies (Fig. 2). Blinded concordance (% identical typing of the patient’s CDC by the Todani classification) by a radiologist reading a US and MRCP (n = 8 available pairs) of the same patient was 78.6 % (71.4–85.7 %); 100 % of the discordant results from this analysis came from difficulty in correctly distinguishing type I from type IV CDCs.
Concordance of IOC and MRCP in the evaluation of pediatric choledochal cysts. Case 1 represents a type IVa CDC with cystic dilatation of the left intrahepatic ductal system (arrowheads) in addition to dilation of the common bile duct. Case 2 is a type I CDC with fusiform dilatation of the common bile duct and transmitted, uniform dilatation of the intrahepatic ductal system, presumably due to a distal pancreaticobiliary malunion with associated biliary stricture
Cost minimization analysis
Mean inflation-adjusted MRCP procedure charges ($1204.69) and collections ($420.85) were significantly higher than charges for IOC and ultrasound combined ($264.80 billed, p = 0.0004; $93.40 collected, p = 0.024; Fig. 3b; Table 3). Wide variability was noted for MRCP charges and collections given that a separate general anesthetic was often required for this procedure (Table 3).
Cost-minimization analysis of procedure charges and collections in the diagnostic evaluation of pediatric choledochal cysts. a Mean inflation-adjusted procedure charges for MRCP ($1204.69) were higher than charges for IOC and US combined ($264.80) (*p = 0.0002, Wilcoxon rank sum). b Mean inflation-adjusted procedure collections for MRCP ($420.85) were higher than collections for IOC and US combined ($93.40) (**p = 0.0021, Wilcoxon rank sum)
Discussion
This study demonstrated the wide variability of resource utilization in the diagnostic imaging of pediatric CDC. Reviewing our institutional experience with the diagnostic evaluation of CDCs, we detected a trend toward an increased number of imaging modalities performed per patient during the study period, likely associated with the emergence of MRI capabilities to visualize the pancreaticobiliary tree. In light of recent studies documenting the concordance between the anatomic information garnered from US, IOC, and MRCP [9, 12], we sought to determine the inter-rater reliability and mean typing accuracy (Todani classification) of these modalities for pediatric CDCs. Ultrasound was shown to have the highest inter-rater reliability, while we were unable to show a difference in typing accuracy among the three studied modalities. In comparing the two most heavily utilized preoperative imaging modalities, US and MRCP, we found that they yielded concordant results in 78.6 % of cases. All discordant results from this analysis came from the difficulty in distinguishing type I from type IV CDC.
The operative approach to CDCs is variable and depends on accurate Todani classification. The vast majority of CDCs are type I and are treated by resection and roux-en-Y hepaticoenterostomy. However, CDCs having cystic dilatation of the intrahepatic bile ducts (types IVa) may require hepatic duct dilation if strictures are present, partial hepatectomy if large and isolated to a single lobe, long-term postoperative surveillance, or even liver transplantation [5]. Patients having intrahepatic biliary cystic dilation are more likely to present with recurrent cholangitis and intrahepatic stone formation. For these reasons, proper evaluation of the intrahepatic biliary tree is essential in the management of CDCs. Our data demonstrate that ultrasound alone is adequate for the diagnosis and preoperative planning of type I CDC, consistent with previous reports [14]. In fact, our study found that ultrasound diagnosis of a type I CDC correlated with the pathology report and intraoperative findings 100 % of the time. Although sonography is quite sensitive to establish bile duct dilation, some difficulty may be encountered in distinguishing intrahepatic ductal dilatation due to proximally transmitted pressure related to a distal PBM (type I) from intrahepatic ductal dilatation representing additional cystic malformation (type IVa cysts). This situation obligates a second imaging modality to define the anomalous anatomy and to plan the optimal surgical approach.
MRCP is a non-invasive measure that adequately images the pancreaticobiliary tree and facilitates preoperative planning of CDC resection. Although our data do not show any overt advantages of MRCP over IOC alone, when intrahepatic ductal dilatation is identified on ultrasound and may be cystic in nature and not secondarily transmitted, we recommend MRCP to investigate for a potential type IV cyst. However, when a type I CDC is diagnosed on ultrasound, our data demonstrate that MRCP is a redundant modality that is far more costly than US and IOC combined and may necessitate a separate general anesthetic (which is the case in 6 of the 30 patients included in our study).
MRCP also has obvious utility in highly selected cases where the diagnosis of CDC is initially unclear, such as Forme Fruste type CDC. These patients present with cholestasis due to PBM and typically have marginal and fluctuating dilatation of the common bile duct [15, 16]. In this situation, it is essential to document PBM before taking a child to the operating room. In our study, MRCP was able to image the pancreatic duct with the greatest frequency when compared with IOC. For these patients, MRCP represents an excellent non-invasive alternative to ERCP or percutaneous transhepatic cholangiography (PTC).
The prenatal diagnosis of CDC is becoming more common and has been detected by screening ultrasound as early as 15 weeks of gestation [17]. Three patients in our study (10 %) were diagnosed prenatally by ultrasound. Although all three of these patients were allowed to deliver before confirmatory testing was conducted in our study, prenatal confirmatory diagnosis by MRCP has been described and may represent another situation in which MRCP is of high utility [18].
The use of radionuclide hepatobiliary scan was infrequent in our patient population (n = 4; 13.3 %) and was therefore not included in the imaging analysis; however, this modality may also be a useful adjunct in differentiating CDC from biliary atresia in the jaundiced neonate by identifying whether or not bile is excreted from the liver. The decision to utilize MRCP versus radionuclide hepatobiliary scan to address this diagnostic dilemma is a potential topic for future study.
This retrospective chart and imaging review poses several inherent limitations. First, the mean typing accuracy and inter-rater reliability calculated for US, IOC, and MRCP in this study are specific to the accurate typing of pediatric CDCs. These results should not be used to interpret the efficacy of these imaging modalities in the assessment of the biliary tree overall, which has been extensively documented previously [19]. Second, this study design did not permit calculation of sensitivity, specificity, positive or negative predictive values, or likelihood ratios, which are necessary in describing the true utility of any diagnostic test. Third, our study may underestimate the accuracy of IOC in the typing of CDCs and visualization of the pancreatic duct, because our assessment of IOCs was limited to several static DICOM images captured in our imaging records. Finally, while our cost minimization analysis does demonstrate the relative expense of MRCP compared to US and IOC, the data are not entirely generalizable in specific dollar terms because facility charges were not included and costs were highly variable depending on the need for conscious sedation or general anesthesia.
In summary, our institutional experience supports the use of ultrasound alone in the diagnosis of pediatric CDC when no intrahepatic biliary ductal dilatation is visualized. However, when dilated intrahepatic ducts are encountered on US, MRCP should be utilized to distinguish a type I from a type IV choledochal cyst, which may drastically alter operative planning and approach.
References
Babbitt DP, Starshak RJ, Clemett AR (1973) Choledochal cyst: a concept of etiology. Am J Roentgenol Radium Ther Nucl Med 119(1):57–62
Ito T, Ando H, Nagaya M, Sugito T (1984) Congenital dilatation of the common bile duct in children. The etiologic significance of the narrow segment distal to the dilated common bile duct. Z Kinderchir 39(1):40–45. doi:10.1055/s-2008-1044167
Todani T, Watanabe Y, Narusue M, Tabuchi K, Okajima K (1977) Congenital bile duct cysts: classification, operative procedures, and review of thirty-seven cases including cancer arising from choledochal cyst. Am J Surg 134(2):263–269 (pii:0002-9610(77)90359-2)
Edil BH, Olino K, Cameron JL (2009) The current management of choledochal cysts. Adv Surg 43:221–232
O’Neill JA Jr (2006) Choledochal cyst. In: Grosfeld JL, O’Neill JA Jr, Fonkalsrud EW, Coran AG (eds) Pediatric surgery, vol 2, 6th edn. Mosby/Elsevier, Philadelphia, pp 2 v (xxix, 2146 p)
Schaefer JF, Kirschner HJ, Lichy M, Schlemmer HP, Schick F, Claussen CD, Fuchs J (2006) Highly resolved free-breathing magnetic resonance cholangiopancreatography in the diagnostic workup of pancreaticobiliary diseases in infants and young children—initial experiences. J Pediatr Surg 41(10):1645–1651. doi:10.1016/j.jpedsurg.2006.05.052
Shaffer E (2006) Can MRCP replace ERCP in the diagnosis of congenital bile-duct cysts? Nat Clin Pract Gastroenterol Hepatol 3(2):76–77. doi:10.1038/ncpgasthep0410
Tipnis NA, Werlin SL (2007) The use of magnetic resonance cholangiopancreatography in children. Curr Gastroenterol Rep 9(3):225–229
Suzuki M, Shimizu T, Kudo T, Suzuki R, Ohtsuka Y, Yamashiro Y, Shimotakahara A, Yamataka A (2006) Usefulness of nonbreath-hold 1-shot magnetic resonance cholangiopancreatography for the evaluation of choledochal cyst in children. J Pediatr Gastroenterol Nutr 42(5):539–544. doi:10.1097/01.mpg.0000221894.44124.8e
Vegting IL, Tabbers MM, Taminiau JA, Aronson DC, Benninga MA, Rauws EA (2009) Is endoscopic retrograde cholangiopancreatography valuable and safe in children of all ages? J Pediatr Gastroenterol Nutr 48(1):66–71. doi:10.1097/MPG.0b013e31817a24cf
Haliloglu M, Akata D, Gurel S, Ozmen MN, Akhan O (2003) Choledochal cysts in children: evaluation with three-dimensional sonography. J Clin Ultrasound 31(9):478–480. doi:10.1002/jcu.10206
Saito T, Hishiki T, Terui K, Sato Y, Mitsunaga T, Terui E, Nakata M, Takenouchi A, Matsuura G, Yahata E, Ohno S, Sato H, Yanagawa N, Masuda Y, Yoshida H (2011) Use of preoperative, 3-dimensional magnetic resonance cholangiopancreatography in pediatric choledochal cysts. Surgery 149(4):569–575. doi:10.1016/j.surg.2010.11.004
Halfhill TR (2011) Tom’s inflation calculator v 7.5.2. http://www.halfhill.com/inflation.html
O’Neill JA Jr (1992) Choledochal cyst. Curr Probl Surg 29(6):361–410
Lilly JR, Stellin GP, Karrer FM (1985) Forme fruste choledochal cyst. J Pediatr Surg 20(4):449–451 (pii:S0022346885000975)
Shimotakahara A, Yamataka A, Kobayashi H, Okada Y, Yanai T, Lane GJ, Miyano T (2003) Forme fruste choledochal cyst: long-term follow-up with special reference to surgical technique. J Pediatr Surg 38(12):1833–1836 (pii:S0022346803006249)
Benhidjeb T, Chaoui R, Kalache K, Mau H, Muller JM (1996) Prenatal diagnosis of a choledochal cyst: a case report and review of the literature. Am J Perinatol 13(4):207–210. doi:10.1055/s-2007-994365
Liu YP, Shih SL (2006) Prenatal diagnosis of choledochal cyst by magnetic resonance cholangiography. Pediatr Radiol 36(10):1112. doi:10.1007/s00247-006-0247-6
Rozel C, Garel L, Rypens F, Viremouneix L, Lapierre C, Decarie JC, Dubois J (2011) Imaging of biliary disorders in children. Pediatr Radiol 41(2):208–220. doi:10.1007/s00247-010-1829-x
Acknowledgments
The authors would like to acknowledge Cathey Carney for her assistance in identifying the study cohort and compiling cost data for this project.
Ethical standards statement
This study was considered to pose minimal risk to participants and was therefore considered an exempted study in terms of human subject research and informed consent by the Vanderbilt University Medical Center Institutional Review Board (IRB# 110122). It has therefore been conducted in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki.
Conflict of interest
The authors declare that they have no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Murphy, A.J., Axt, J.R., Crapp, S.J. et al. Concordance of imaging modalities and cost minimization in the diagnosis of pediatric choledochal cysts. Pediatr Surg Int 28, 615–621 (2012). https://doi.org/10.1007/s00383-012-3089-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-012-3089-3