Abstract
Pediatric osteomyelitis commonly occurs in the long bones and has rarely been reported in small bones such as the vertebrae and ribs. Rib osteomyelitis occurs in approximately 1% or less of all cases of hematogenous osteomyelitis, and is usually caused by Staphylococcus aureus. We present a case of acute osteomyelitis in the rib of an otherwise healthy and afebrile 1-year-old infant that appeared as a lytic bone lesion on imaging studies and was mistaken for a tumor. Biopsy was needed to rule out malignancy and establish the diagnosis of osteomyelitis caused by group A Streptococcus. This is one of the few reported cases of pediatric rib osteomyelitis caused by this organism.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Osteomyelitis is an inflammatory process of the bone secondary to a bacterial or fungal infection. It can present in an acute, subacute, or chronic manner. Acute osteomyelitis may result from either hematogenous spread of bacteria from a remote source or as a result of direct contact of bone with an infectious source during trauma or surgery [1]. Acute hematogenous osteomyelitis primarily occurs in children, most commonly in the long bones of the femur, tibia, and humerus at the rapidly growing and highly vascular metaphyses. In the United States, the prevalence is 1 in 5,000 children, and as high as 1 in 1,000 newborns. The prevalence is higher in children with sickle cell disease [2]. Although uncommon, acute hematogenous osteomyelitis has been reported in smaller bones such as the vertebrae and ribs. In particular, rib osteomyelitis occurs in 1% or less of all cases of hematogenous osteomyelitis [2]. In the long bones, the onset of acute hematogenous osteomyelitis can be abrupt, manifested by high fevers, chills, joint effusion and local tenderness, edema, and erythema. However, in sites other than the long bones, the disease may have a more insidious onset and slower clinical development and is considered “subacute”. Diagnostic tests such as blood cultures or radiographs, though suggestive, are not specific for osteomyelitis. Thus, in the case of small bone involvement, diagnosis may be difficult and the process may even be misdiagnosed as malignancy [3]. We present an interesting case of rib osteomyelitis that presented as a lytic lesion initially thought to be a tumor.
Case report
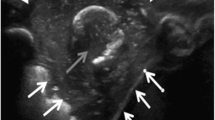
An otherwise healthy 1-year-old male infant presented to the emergency room with complaints of tenderness and edema of his inferior right chest wall. There was no history of previous trauma. He was afebrile, and the rest of his physical examination was unremarkable. Although his total leukocyte count was normal (9.11 × 103/μl), the eosinophil fraction was high at 8% and his serum calcium was slightly elevated (12 mg/dL). The rest of his serum chemistry, serum uric acid, alkaline phosphatase, and lactose dehydrogenase (LDH) levels were normal. Chest radiograph (see Fig. 1) revealed splaying of the right eighth rib. A computerized tomogram (CT scan) of the chest showed an expansive lytic lesion at the tip of the right rib with adjacent soft-tissue swelling (see Fig. 2). At this point, the differential diagnosis included a primary bone tumor such as Ewing’s sarcoma, metastatic disease such as neuroblastoma, Langerhan’s cell histiocytosis, or osteomyelitis. His clinical presentation was not in keeping with acute osteomyelitis so a biopsy was planned. No therapy was started.
An incisional biopsy was performed on an outpatient basis. At surgery, the tissue overlying the right eighth rib was noted to be edematous and a sample of the soft tissue was sent for frozen section. The rib was soft and easily incised. The center of the rib contained a creamy-white fluid that was drained and sent for culture. Gram stain of the milky fluid identified no organisms. Frozen section of the friable tissue within the rib lumen was indeterminate. An incisional biopsy of the outer table of the rib was performed. The child was discharged after surgery, but returned 3 days later with a wound infection. His erythrocyte sedimentation rate (ESR) was high at 33 mm and his C-reactive protein (CRP) level was within normal limits. By this time, cultures from the original biopsy had isolated beta Streptococcus group A. The final pathologic diagnosis from the rib biopsy showed no presence of neoplasia and was consistent with osteomyelitis. The wound infection was debrided and the patient was started on a 28-day course of intravenous cefazolin to treat the osteomyelitis. After a month of outpatient antibiotic therapy, his ESR normalized to 9 mm and his CRP level remained normal. A follow-up chest radiograph at 6 weeks showed a persistent lytic defect in the anterior aspect of the right eighth rib (see Fig. 3), which corresponded with the biopsy site. There did not appear to be any sequestrum or new bone formation. The child recovered very well and is now a healthy, vibrant toddler with no recurrent symptoms at 6 months follow-up.
Discussion
The most common clinical manifestations of rib osteomyelitis are fever, chest pain, and localized chest wall swelling [4]. Laboratory abnormalities often include an elevated leukocyte count with a neutrophil predominance, as well as elevated ESR and CRP, which are typical for a bacterial infection [2]. However, laboratory tests are unreliable as they may be within normal limits [5]. Subacute osteomyelitis is considered one of the great masqueraders of bone disease, and is often reported in children of ages 1–16. Since it presents with vague symptoms such as inconsistent fevers, constant but minimal aching, and minor edema, it is easily mistaken as a malignant bone lesion [3, 6]. The diagnosis of osteomyelitis can be even more insidious when blood cultures exhibit varying levels [3, 6].
Ewing’s sarcoma presents with a very similar clinical profile to osteomyelitis, as these lesions are also found in the metaphysis or diaphysis of the long bones. A radiographic review of 328 cases of Ewing’s sarcoma reported the incidence of primary rib Ewing’s sarcoma as 10% [7]. The affected rib was predominantly lytic in 82% of cases, but mixed lytic-sclerotic (9%), and predominantly sclerotic (9%) patterns were also encountered. The rib also appeared to be “expanded” in 35% of cases [7]. Ewing’s sarcoma typically occurs between the ages of 10 and 25 years [7]. In this age group, rib biopsy would be critical to establish the diagnosis of osteomyelitis versus primary rib’s sarcoma since the radiographic findings are so similar. Imaging techniques such as CT scans, magnetic resonance imaging (MRI), and a bone scan may provide additional information by localizing the site of the lesion and extent of spread, but a definitive diagnosis could only be obtained by biopsy [2].
The most common organism causing osteomyelitis in infants and children is Staphylococcus aureus (80–90%), followed by group B beta-hemolytic Streptococcus [1, 8]. Gram-negatives such as Neisseria, fungi (Candida), viruses or parasites may also occur, and Salmonella is commonly seen in older children with sickle cell disease [1]. In particular, rib osteomyelitis by streptococcal species is extremely rare. Of the approximately 150 cases of rib osteomyelitis that have been reported thus far, less than 60 occurred in children and adolescents less than 20 years of age. Of these, only four cases were reported to be caused by streptococcal species [Streptococcus viridans, Streptococcus pyogenes, and group A Streptococcus (GAS)] [9]. The case reported here is one of the few cases of rib osteomyelitis caused by GAS. GAS may be carried in the throat or on the skin in asymptomatic people. Most GAS infections are relatively mild illnesses such as “strep throat,” or impetigo, but rarely, these bacteria can cause severe diseases such as necrotizing fasciitis and toxic shock syndrome. The association with osteomyelitis is a unique one.
In conclusion, this case highlights an insidious presentation of osteomyelitis that was initially mistaken for a malignant bone lesion and turned out to be a very rare case of streptococcal rib osteomyelitis. Osteomyelitis is not an obvious diagnosis in the face of an afebrile infant without sickle cell disease and with a normal leukocyte count. This report is presented to promote awareness for pediatric osteomyelitis in the rib that presents as a lytic bone lesion. Indeterminate laboratory test and imaging results should always be followed by early surgical biopsy to confirm the diagnosis and rule out malignancy. Biopsy also aids in the identification of the causative organism and enables targeted antibiotic treatment.
References
Blickman JG, van Die CE, de Rooy JW (2004) Current imaging concepts in pediatric osteomyelitis. Eur Radiol Suppl 4:L55–L64
Basa NR, Si M, Ndiforchu F (2004) Staphylococcal rib osteomyelitis in a pediatric patient. J Pediatr Surg 39:1576–1577
Cottias P, Tomeno B, Anract P et al (1997) Subacute osteomyelitis presenting as a bone tumour. a review of 21 cases. Int Orthop 21:243–248
Bishara J, Gartman-Israel D, Weinberger M et al (2000) Osteomyelitis of the ribs in the antibiotic era. Scand J Infect Dis 32:223–227
Dirschl DR, Almekinders LC (1993) Osteomyelitis. Common causes and treatment recommendations. Drugs 45:29–43
Juhn A, Healey JH, Ghelman B et al (1989) Subacute osteomyelitis presenting as bone tumors. Orthopedics 12:245–248
Moser RP Jr, Davis MJ, Gilkey FW et al (1990) Primary ewing sarcoma of rib. Radiographics 10:899–914
Schmit P, Glorion C (2004) Osteomyelitis in infants and children. Eur Radiol Suppl 4:L44–L54
Kalouche I, Ghanem I, Kharrat K et al (2005) Osteomyelitis of the rib due to Streptococcus pneumoniae: a very rare condition in children. J Pediatr Orthop B 14:55–60
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Naik-Mathuria, B., Ng, G. & Olutoye, O.O. Lytic rib lesion in a 1-year-old child: group A beta streptococcal osteomyelitis mimicking tumor. Pediatr Surg Int 22, 837–839 (2006). https://doi.org/10.1007/s00383-006-1725-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-006-1725-5