Abstract
Neonatal umbilical anomalies usually represent remains of the vitelline duct or the allantois. We describe a case of an umbilical appendix in a neonate. The vermiform appendix was found to be positioned in the umbilical cord. In a brief literature review we found eight other reports concerning umbilical appendices. In this article we describe a possible embryological explanation for the development of an umbilical appendix, and discuss whether or not the appendiceal umbilical fistulae reported are congenital or iatrogenic. The possible association between an umbilical appendix and different forms of malpositioning and rotation of the gut is also discussed. Protrusion of the neonatal appendix into the umbilical cord represents a different entity of congenital anomalies. It is important to realize that, in the case of an unrecognized umbilical appendix, medical procedures (e.g., canulation or clamping of the umbilicus) may produce an iatrogenic appendico-umbilical fistula. Careful inspection and palpation of the umbilical cord prior to these procedures may prevent a fistula being created. Furthermore, because the possible association between umbilical appendices and different kinds of malpositioning of the gut is so far not wholly elucidated, we recommend further (radiological) investigation in each case of an umbilical appendix. Correct positioning of the bowel needs to be confirmed in order to rule out possible future complications.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In this article we describe a case of a neonatal appendix protruding through the umbilical cord. Most umbilical neonatal anomalies described in literature are derived from the vitelline duct (e.g., patent omphalomesenteric duct, POMD), the allantois (e.g., urachus) or originating from primitive vessels. In this article we compare this case with other, previously published case reports. Also, we postulate an embryological explanation of the etiology and discuss the clinical consequences.
Case report
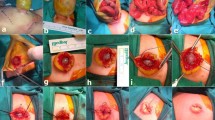
A premature female was delivered per vaginam after an uncomplicated pregnancy on the 34th week of gestation. Premature rupture of membranes occurred approximately 72 h ante partum. The Apgar scores were 6 and 8 at 1 and 5 min, respectively, the birth weight was 2,135 g (25th–50th percentile). Because of the suspicion of a neonatal infection, it was decided to start with intravenous antibiotics immediately post partum. An attempt at peripheral intravenous cannulation was not successful due to poor peripheral circulation. Therefore, we proceeded to umbilical venous cannulation. The umbilical cord was cut off approximately 1 cm above the umbilical ring. The underlying umbilical stump appeared to have a normal anatomy with two clearly identifiable arteries and one larger, open duct, which was assumed to be the umbilical vein. Cannulation with a Charrière 3.5 catheter was straightforward. However, the umbilical catheter returned no blood upon suctioning, therefore a chest/abdominal X-ray film was performed which showed an abdominal position of the catheter, most likely located within the bowel. Also, suctioning of the line with a syringe eventually produced a dark fluid, presumably meconium as was later confirmed by laboratory investigation. Cannulation of a POMD seemed very likely and the catheter was removed. The clinical condition of the neonate remained stable throughout the whole procedure. During the following hours a small discharge of meconium from the duct was observed only once. It was decided to transfer the neonate to the Department of Paediatric Surgery of the nearby University Medical Centre for further evaluation and treatment. Radiological examination by fistulography showed contrast passing into the bowel (Fig. 1). This suggested the existence of a POMD. The operative procedure was performed by a supra-umbilical incision. For exploration of the umbilical ring, it was needed to bring the cecum and terminal ileum outside the abdomen and the umbilical anomaly turned out to be the neonatal appendix, which had protruded through the umbilical ring; also there was a cecum mobile (Fig. 2). An appendectomy was performed and the umbilicus incision was closed. Postoperative recovery was uneventful. Examination of the removed appendix showed that the tip of the peripheral part was partially severed. Pathological examination of the removed fistulous tract showed a normal appendix, the tip of which was closed but partially severed distally to a compressed part of the appendix, presumably by cross clamping during the attempted cannulation of the umbilical vein (Fig. 3a, b).
A barium swallow and follow-through was performed to rule out a malrotation and revealed no abnormal findings.
Discussion
The normal neonatal umbilical cord consists of two arteries and one vein, which are surrounded by the Wharton’s jelly. Occasionally, other embryonic tissues are found in the neonatal umbilicus. These tissues usually are remnants of the vitello-intestinal duct, the allantois or early embryonic vessels. In a large study, Jauniaux et al. examined 1,000 umbilical cords and found in a total of 24 cords remnants of the vitelline duct [1].
In normal embryology, by the fifth week of gestation, the vitello-intestinal duct forms the connection between the apex of the midgut (primary intestinal duct) and the yolk sac. Around the sixth week, the midgut starts to grow rapidly and the increasing intra-abdominal pressure forces the midgut to protrude and enter the umbilical cord. The midgut then differentiates into jejunum and ileum, while at the same time the appendix sprouts from the cecum. By the tenth week, the vitello-intestinal duct detaches from the ileum and becomes obliterated. The herniated loop of the midgut starts to retract and re-enters the abdominal cavity, first the proximal part of the jejunum followed by the cecum and appendix. This process is completed by the 11th week [2]. If the intestinal loops fail to re-enter the abdominal cavity, and therefore remain in the umbilical cord, an omphalocele develops.
In the event that the vitello-intestinal duct does not detach or does not obliterate completely, a few different anomalies may develop, including a POMD. However, these anomalies differ totally from a neonatal appendix protruding in the umbilical cord. This appears to be a different entity of congenital umbilical anomalies.
We searched common literature for case reports concerning umbilical appendices dating from 1922 and found a total of eight cases. These reports are described briefly in Table 1.
Recently a theory has been put forward to explain the development of a neonatal umbilical appendix. Borgna-Pignatti et al. postulated that perhaps some of the intestinal loops fail to re-enter the abdominal cavity during the embryological development [3]. In case of failure of a large part of the gut to re-enter the abdomen, a gross omphalocele results, which is often easily diagnosed post partum. But if the appendix alone fails to re-enter the abdomen, this results only in a small umbilical anomaly, which may not be noticed during neonatal physical examination.
Further, if this umbilical anomaly is not recognized and the umbilical cord is cut off straight above the umbilical ring, for example during the procedure of umbilical vein catherization, this may create a fistula, also known as an appendico-umbilical fistula (AUF). Perhaps even a simple procedure like clamping of the umbilical cord post partum, is enough to iatrogenically create an AUF, in case of a pre-existing umbilical appendix. Careful inspection and palpation of the umbilical cord prior to invasive medical procedures like umbilical catheterization may prevent a fistula being created.
We postulate that the umbilical anomaly reported as AUF in some of the articles in fact are intact neonatal umbilical appendices, which have become a fistula iatrogenically [4–6]. To our opinion, the primary nomenclature for this anomaly therefore should be “umbilical appendix” and not “appendical umbilical fistula” (AUF).
The possible relationship between the existence of an umbilical appendix and different forms of mal-positioning of the gut may in fact support the theory of failure of the appendix to retract. The table shows a total of three cases with a mobile cecum in association with an umbilical appendix. A mobile cecum indicates a freely movable cecum which is unattached to the lateral peritoneum. Clinically a mobile cecum increases the risk of (cecal) volvulus and is known to cause constipation and episodes of abdominal pain [7]. Furthermore, a case of complete non-rotation was reported.
Is there a causal relationship between failure of retraction of the appendix and malpositioning of the bowel? On the one hand, in the case of primal defective fixation of the cecum, the appendix consequently may remain freely movable in the abdomen and is able to protrude in the umbilical cord which results in the neonatal umbilical appendix. On the other hand, primary failure of the appendix to retract completely may hamper correct fixation of the cecum to the lateral peritoneum. Embryologically, as was stated earlier, the midgut re-enters the abdomen by the tenth week of gestation because of decreasing intra-abdominal pressure. It does not appear logical that after this re-entering, the appendix migrates back against the fall of pressure into the umbilical cord and becomes well embedded in Wharton’s jelly in the umbilical cord. We therefore favor the theory that failure of retraction of the appendix is followed by defective fixation of the cecum to the lateral peritoneum resulting in either a mobile cecum or possibly a malrotation.
Because of the at present unclear and possible association between an umbilical appendix and malrotation of the bowel, we recommend that in case of a neonatal umbilical appendix, further (radiological) investigation to the anatomical positioning of the bowel needs to be performed following operative procedure.
References
Jauniaux E, De Munter C, Vanesse M, Wilkin P, Hustin J (1989) Embryonic remnants of the umbilical cord: morphologic and clinical aspects. Hum Pathol 20:458–462
Larsen W (1997) Human embryology, 2nd edn. Churchill Livingstone, New York, pp 240–242
Borgna -Pignatti C, Bergamo Andreis I, Bettili G, Zamboni G (1995) Delayed separation of an appendix-containing umbilical stump. J Pediatr Surg 30:1717–1718
Sandborn W, Shafer A (1967) Appendiceal-umbilical fistula. J Pediatr Surg 2:461–463
Kadzombe E, Currie A (1988) Neonatal fistula from the appendix to the umbilicus. J Pediatr Surg 23:1059–1060
Crankson S, Ahmed G, Palkar V (1998) Patent omphalomesenteric duct of the vermiform appendix: congenital appendicoumbilical fistula. Pediatr Surg Int 14:229–230
Gupta S, Gupta S (1993) Acute caecal volvulus: report of 22 cases and a review of literature. Ital J Gasteroenterol 25:380–384
Crymble P (1922) A case of persistent vitelline duct to vermiform appendix. Br J Surg 19:304–305
Singleton A Jr, King W (1951) Persistent vitelline duct continuous with the appendix. Surgery 29:278–280
Biagtan J, Rosenfeld W, Salazar D, Velcek F (1980) Herniation of the appendix through the umbilical ring following umbilical artery catheterization. J Pediatr Surg 15:672–673
Zaidenstein L, Freud E, Schwartz M, Zer M (1995) Clinical presentation of rare appendico-omphalic anomalies. J. Pediatr Surg 30:1702–1703
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Fuijkschot, J., Wijnen, R.M.H., Gerrits, G.P.J.M. et al. A neonate with an intact congenital umbilical appendix: an alternative theory on the etiology of the appendico-umbilical fistula. Pediatr Surg Int 22, 689–693 (2006). https://doi.org/10.1007/s00383-006-1720-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-006-1720-x