Abstract.
A retrospective study was performed of 250 patients with cholelithiasis treated at the Royal Children's Hospital, (RCH) Melbourne, over 25 years by open operation; 32 (12.8%) had proven choledocholithiasis on either preoperative imaging, operative cholangiography (OpCG), or postoperative investigation. A further 3 had underlying congenital biliary abnormalities and were excluded from further study. Thirty-one of the 32 were explored at open operation, 27 after OpCG and 4 on clinical grounds. One retained common-bile-duct (CBD) stone was undetected until the postoperative period (1/250, 0.25%). Seven ducts were not cleared, giving a duct exploration failure rate of 22.6% (7/31). All 8 retained CBD stones were identified in the early postoperative period and managed with a variety of techniques, including endoscopic retrograde cholangio-pancreatography (ERCP). The incidence of retained stones after open CBD exploration was high (22.6%), and can be attributed to difficulties in operative technique dealing with the smaller paediatric CBD. In addition, haemolytic disease seems to induce a propensity for choledocholithiasis. Given the small numbers presenting with cholelithiasis to RCH (10 per year), it is suggested that a selective approach to CBD exploration is appropriate in children. With the increasing use of laparoscopic cholecystectomy in children and the inherent technical difficulties of laparoscopic operative cholangiography, ERCP may offer an alternative solution in dealing with CBD stones rather than open or laparoscopic CBD exploration.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Choledocholithiasis occurs infrequently in childhood, the first recorded incidence being in a 12-year-old boy from Leeth, Scotland, in 1722 [1]. The incidence in children with cholelithiasis ranges from 6% to 10% and is often associated with congenital anomalies of the common bile duct (CBD) [2–6]. Our series contained 3 anatomical anomalies with CBD stones, including 1 incidental post-mortem finding in a spina bifida patient.
Cholelithiasis in children is also frequently associated with haemolytic disease and is seen increasingly after the use of total parenteral nutrition, with gallbladder stasis, and after ileal resection [7]. Increased fat in the Western diet is also postulated to have recently increased the incidence. It is likely that increasing numbers of children will require surgery for cholelithiasis in the future if current trends continue [8].
The aim of this study was to document the incidence of CBD stones in children with cholelithiasis, to document the methods of detection and extraction used, and to develop a strategy to deal with this problem in the laparoscopic era.
Materials and methods
A retrospective study was undertaken of all admissions for cholelithiasis undergoing open cholecystectomy between January 1952 and April 1997. Eleven surgeons participated in the collection of data. Presenting symptoms, physical signs, and investigation results were recorded on a database for analysis (Microsoft Access, Version 2, 1989–1994, Microsoft, USA). The presence of choledocholithiasis was confirmed by radiology both preoperatively and at operative cholangiogram (OpCG). The CBD was explored using 5 Fr Foley balloon catheters, and T-tube cholangiograms were performed in all explored patients postoperatively to confirm clearance of stones. OpCGs were reviewed postoperatively by both a surgeon and a radiologist. Pathology and operation reports were also reviewed.
Results
Thirty-two of 250 (12.8%) cholelithiasis patients had documented choledocholithiasis, and a further 3 had anatomical anomalies of the biliary tree and were excluded from further study. Patients ranged in age from 1 month to 19 years (mean 7 years); most of them were Anglo-Saxon in origin (21, 66%). Haemolytic disease was present in only 6 (18%) choledocholithiasis patients, but was found in 2 of the 8 retained-stone cases (8/32, 25%). Clinical presentations varied, with vomiting, right-upper-quadrant pain, jaundice, and acholuric stools being most common, as expected (Table 1). Laboratory data confirmed an elevated serum bilirubin level in 26 of the 32 cases, while amylase was not routinely recorded.
A variety of investigations were used to detect CBD stones. Oral cholecystography was performed in 7 (prior to 1982), revealing only 1 CBD stone (14%). IV cholangiography (also prior to 1982) performed in 9 revealed CBD stones or obstruction in 7 (78%). Ultrasound (US) performed in 24 patients revealed CBD stones in 14, CBD dilation in 6, gallbladder stones in 2, and was non-contributory in 2 (Table 2).
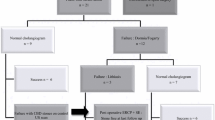
Of the 32 patients with CBD stones, 27 had OpCG and exploration, while 4 had CBD exploration on clinical grounds alone. One stone was unsuspected (1/250, 0.25%). Eight patients had retained stones postoperatively, 6 of whom had OpCGs; 1 had a preoperative "normal" IV cholangiogram but was explored for clinical reasons, and was unsuspected (Table 2). The latter case presented with recurrent pain post-cholecystectomy and was successfully treated by ERCP and sphincterotomy. The other 7 had T-tubes inserted routinely at operation, and T-tube cholangiograms revealed the retained stones, which were removed by a variety of techniques, including ERCP (Table 3).
Discussion
Choledocholithiasis is known to be present in 6%–10% of paediatric patients with cholelithiasis (2–6), while in adults this incidence may be as high as 17% [9]. In this study the incidence of choledocholithiasis with cholelithiasis was 12.8% (32/250). Haemolytic disease was present in 17% of the choledocholithiasis group, but only 2.4% of the total cholelithiasis group, suggesting a propensity for CBD stones with this condition.
OpCG was not performed in 5 patients, 4 of whom had known CBD stones preoperatively. One of these subsequently had a retained stone, even though the duct was explored. Another 6 retained stones followed both cholangiography and CBD exploration, yet the duct was still not fully cleared. Only 1 retained stone was completely unsuspected. The incidence of retained stones post-CBD exploration has been reported as 14% in adults [9], but was much higher in our study (22.6%).
OpCGs were performed via the cystic duct with two injections of 10–20 ml contrast. The films were reviewed postoperatively by the surgeon and a radiologist. Technique is important in performing cholangiography, in particular by rotating the patient to expose the biliary tree separate from the underlying lumbar spine, demonstrating free flow of contrast into the duodenum, showing normal tapering of the distal CBD, and outlining the major intrahepatic ducts [9].
Whitcombe and Cremin showed the normal CBD to range in diameter from 2 mm in infants to 4.9 mm in later childhood [10]. Therefore, standard biliary instruments such as Bakes dilators and De Jardins forceps are not readily applicable in the younger patient. In this series a 5 Fr feeding tube was used to flush the duct and a 5 Fr Fogarty balloon catheter was used to retrieve stones low in the CBD, as has been used routinely in adults during open exploration for many years [11, 12].
Assuming these guidelines were followed, it is of concern that CBD stones were either not detected or subsequently not cleared at open exploration of the CBD. In all 6 cases of retained CBD stones where OpCG was performed, stones were seen at radiologically, but the CBD was not completely cleared at exploration. This indicates possible difficulties in operative technique due to the smaller calibre of the paediatric CBD. In addition, the smaller bile stones of haemolytic disease seem to have a propensity to "float" into the intrahepatic duct system, possibly making clearance more difficult.
The incidence of retained CBD stones postoperatively in adults has been reported as 14% after open operation [9] and 8% after laparoscopic surgery [13]. It was 22.6% in children after open operation in this study, but is currently unknown after laparoscopic surgery in children [14]. The techniques used to retrieve the retained stones are listed in Table 3. All but 1 were detected by T-tube cholangiogram, and presented as recurrent abdominal pain. This last patient, along with 2 others, was successfully managed by ERCP.
The use of ERCP in children has become commonplace and has a number of indications, including pancreatic trauma [15], pancreas divisum, choledochal cyst, and cholelithiasis and choledocholithiasis [16, 17] and can even be performed in infants less than 1 year of age safely [18]. Increasingly, laparoscopic cholecystectomy is recommended as the treatment of choice for symptomatic cholelithiasis, with the advantages of shorter hospital stay and better cosmesis. The disadvantages of learning a new procedure have slowed it's acceptance in some centres [8, 19].
The use of ERCP in the setting of retained CBD stones postoperatively or known CBD stones preoperatively can therefore be expected to increase, and has been shown to be safe and effective in this setting in both the adult and paediatric populations [20, 21]. Post-ERCP pancreatitis remains a problem, and can prolong hospital stay [22]. No studies have been conducted comparing open CBD exploration with ERCP clearance of the CBD in the paediatric age group. Tagge et al., however reported 100% success in clearing the CBD of stones with ERCP in their study [6].
Given the relatively small numbers of patients presenting with this problem, is a laparoscopic cholangiogram necessary in all cases? Taylor et al. reported missed CBD stones in 0.7% of cases, using a selective policy that required performing a cholangiogram in the presence of pre-operative jaundice, pancreatitis, altered liver function tests, or a dilated CBD on US [23]. In children the rate of retained stones is thought to be similar to adults, but laparoscopic cholangiography is far more difficult due to the smaller calibre of the extra-hepatic bile ducts [14].
Our own experience suggests that open CBD exploration is less likely to be successful in the paediatric age group than in adults. Laparoscopic exploration is also more difficult, and less likely to be successful [14]. Further, laparoscopic cholecystectomy can be performed safely without routine cholangiography, if accepted preoperative parameters are met, with a very low incidence of retained CBD stones [23]. The literature suggests that ERCP is a safe and reliable way of dealing with retained CBD stones in both adults and children [7].
In conclusion, exploration of the paediatric CBD is made difficult by its small calibre and the relatively small numbers of children presenting with choledocholithiasis. The high rate of retained stones after open CBD exploration and the learning curve associated with laparoscopic cholecystectomy and OpCG suggest that routine cholangiography may not be indicated in most children with cholelithiasis. A selective approach for OpCG in children and the use of ERCP when CBD stones are detected either pre- or postoperatively is one possible solution to this problem.
References
Gibson J (1925) Medical essays and observations. Quoted by Synder CC In: Cholecystitis and cholelithiasis in young children. JAMA 85: 31
Schwei GP (1958) Cholecystitis with cholelithiasis in childhood. Wis Med J 57: 295–298
Pieretti R, Auldist AW, Stephens CA (1975) Acute cholecystitis in children. Surg Gynecol Obstet 140: 16–18
Porkorny WJ, Saleem M, O'Gorman RB, McGill CW, Harberg FJ (1984) Cholelithiasis and cholecystitis in childhood. Am J Surg 148: 742–744
Harned RK, Babbitt DP (1975) Cholelithiasis in childhood. Radiology 117: 391–393
Man DWK, Spitz L (1985) Choldocholithiasis in infancy. J Pediatr Surg 20: 65–68
Holcomb GW (1993) Laparoscopic cholecystectomy. Semin Pediatr Surg 2: 159–167
Lugo-Vicente HL (1997) Trends in management of gallbladder disorders in children. Pediatr Surg Int 12: 348–352
Hall RC, Sakiyalak P, Seuk KK, Rogers LS, Webb WR (1973) Failure of operative cholangiography to prevent retained common duct stones. Am J Surg 125: 51–63
Witcombe JB, Cremin BJ (1978) The width of the common bile duct in childhood. Pediatr Radiol 7: 147–149
Henzel JH, DeWeese MS (1971) Common duct exploration with and without balloon-tipped biliary catheters. Arch Surg 103: 199–203
Knight CD (1967) Use of balloon-tipped catheter in exploration of the common duct. Am J Surg 113: 717–718
Rhodes M, Nathanson L, O'Rourke N, Fielding G (1995) Laparoscopic exploration of the common bile duct: lessons learned from 125 cases. Br J Surg 82: 666–668
Newman KD, Powell DM, Holcomb GW (1997) The management of choledocholithiasis in children in the era of laparoscopic cholecystectomy. J Pediatr Surgery 32: 1116–1119
Rescorla FJ, Plumley DA, Sherman S, Sherer LR, West KW, Grosfeld JL (1995) The efficacy of early ERCP in pediatric pancreatic trauma. J Pediatr Surg 30: 336–340
Tagge EP, Tarnasky PR, Chandler J, Tagge DU, Smith C, Hebra A, Hawes RH, Cotton PB, Othersen HB (1997) Multidisciplinary approach to the treatment of pediatric pancreaticobiliary disorders. J Pediatr Surg 32: 158–164
Guelrud M (1996) Endoscopic retrograde cholangiopancreatography in children. Gastroenterologist 4: 81–97
Ohnuma N, Takhishi H, Tanabe M, Yoshida H, Iwai J (1997) Endoscopic retrograde cholangiopancreatography in biliary tract disease in infants less than one year old. Tohoku J Exp Med 181: 67–74
Kim PC, Wesson D, Superina R, Filler R (1995) Laparoscopic cholecystectomy versus open cholecystectomy in children: which is better? J Pediatr Surg 30: 971–973
Pencev D, Brady PG, Pinkas H, Boulas J (1994) The role of ERCP in patients after laparoscopic cholecystectomy. Am J Gastroenterol 89: 1523–1527
Rescorla FJ (1997) Cholelithiasis, cholecystitis, and common bile duct stones. Curr Opin Pediatr 9: 276–282
Sees DW, Martin RR (1997) Comparison of preoperative ERCP and laparoscopic cholecystectomy with operative management of gallstone pancreatitis. Am J Surg 174: 719–722
Taylor OM, Sedman PC, Jones BM, Royston, CM, Arulampalam T, Wellwood J (1997) Laparoscopic cholecystectomy without operative cholangiogram: 2038 cases over a five year period in two district general hospitals. Ann R Coll Surg Engl 79: 376–380
Acknowledgements.
The authors wish to thank all 11 surgeons, past and present, from the Royal Children's Hospital, Melbourne, for the use of their patient data in this study and particularly thank current surgeons A.W Auldist, K.B. Stokes, and R.G. Taylor.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Farrow, G.B., Dewan, P.A., Taylor, R.G. et al. Retained common-duct stones after open cholecystectomy and duct exploration in children. Ped Surgery Int 19, 525–528 (2003). https://doi.org/10.1007/s00383-002-0766-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-002-0766-7