Abstract
Introduction
Ventriculoperitoneal shunt insertion during the neonatal period and early infancy is associated with a high rate of shunt failure when compared to the adult population. Furthermore, the function of flow-regulated valves and differential pressure valves may be different in neonatal hydrocephalus.
Methods
A retrospective case series of all primary shunt procedures carried out during or immediately following the neonatal period, from August 2011 to February 2018 at Sheffield Children’s Hospital. The total sample size was 55. This included 34 patients with adjustable valves (Miethke ProGav) and 21 with flow-regulated valves (Orbis-Sigma); however, only 53 had adequate follow-up.
Results
The overall 1 year shunt survival was 34% (18/53), and there was no significant difference depending on which shunt valve was implanted. The primary shunt infection rate was 11% (6/53) with S. aureus being the most common causative organism. During the first year of life, clinical signs of shunt overdrainage were seen more frequently in patients with adjustable valves than in those with flow-regulated valves (59% [19/32] versus 24% [5/21], p = 0.02). Furthermore, 2 patients in the adjustable valve group developed sagittal craniosynostosis secondary to shunt overdrainage.
Conclusion
Shunt failure is high when inserted during or immediately following the neonatal period. Overdrainage may be less common in patients with flow-regulated valves. However, if overdrainage is observed, adjusting the setting of a differential pressure valve can effectively treat the overdrainage without the need for invasive shunt revision surgery.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Hydrocephalus in early infancy can be secondary to a wide range of pathologies such as intraventricular haemorrhage [1,2,3,4,5,6,7,8,9], myelomeningocele [8, 10,11,12,13,14], aqueductal stenosis [15,16,17], intracranial cysts [18, 19] and meningitis [8]. In patients who require permanent cerebrospinal fluid (CSF) diversion, a ventriculoperitoneal (VP) shunt is usually the first-line procedure. However, shunt failure is high when inserted during the neonatal period and early infancy. Shunt dysfunction may be due to infection, blockage and overdrainage [20,21,22,23,24].
The anterior fontanelle closes at 12–24 months of age [25, 26], and there is variation in age at which an infant learns to crawl and walk [27, 28]. It is likely that non-ambulatory infants with open fontanelles represent CSF shunt physiology which is unique. The effect of different shunt valve systems on this unique neonatal CSF physiology has not been determined.
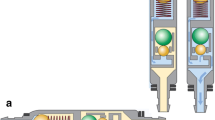
CSF drainage can be restricted by implanting either a differential pressure or flow-regulated valve. A differential pressure valve opens when the positive pressure gradient between the ventricle and peritoneum exceeds the mechanical resistance exerted by the valve. The minimum pressure needed to open the valve can be increased or decreased with the use of adjustable settings, such as in the Miethke ProGav system. Flow-regulated valves do not have an adjustable component; they are designed to maintain a constant rate of CSF drainage throughout physiological pressure changes occurring within the ventricles and peritoneum.
We sought to establish whether there is a difference in the function of a flow-regulated valve such as an Orbis-Sigma (OSV) or a differential pressure valve, such as the Miethke ProGav in neonatal hydrocephalus.
Methodology
A retrospective case series of primary shunt procedures during or immediately following the neonatal period, from August 2011 to February 2018 at Sheffield Children’s Hospital was carried out. The neonatal period was defined as the first 4 weeks of life in full-term babies. In premature babies, the inclusion criteria was extended to 3 months. Fifty-five patients were included in the study. Thirty-four had an adjustable valve (Miethke ProGav), and twenty-one had a flow-regulated valve (Orbis-Sigma) inserted. The distal catheter was placed into the peritoneum in all patients.
Clinical overdrainage was defined as the presence of one or more of the following; sunken fontanelle, overriding sutures and decreasing head circumference. In isolation, irritability and vomiting were not attributed to overdrainage; however, when associated with other signs of overdrainage, they were considered to indicate severe deterioration. Radiological signs of overdrainage included subdural collections, overriding or fused cranial sutures and collapsed ventricles.
The female to male ratio was 1:1.75. The gestational ages at birth were full term (> 37 weeks) in 38%, moderately premature (28–37 weeks) in 46% and extremely premature (< 28 weeks) in 16%. The most common causes of hydrocephalus were intraventricular haemorrhage (44%, 24/55), myelomeningocele (31%, 17/55) and aqueductal stenosis (7%, 4/55) (Table 1).
The corrected gestational age at the time of primary shunt insertion varied, ranging from 35 weeks + 6 days to 47 weeks (Table 2). The median duration from birth to primary shunt insertion was 46 days (range 3–133 days) in patients with adjustable valves and 51 days (range 4–111) in those with flow-regulated valves (Table 2).
The primary outcome was 1 year shunt survival. Overdrainage and shunt infections were assessed as secondary outcomes. Overdrainage was defined clinically, by the presence of sunken fontanelle, decreasing head circumference or overriding skull vault sutures. Shunt infection was defined as clinical shunt infection with a confirmed causative organism grown from the CSF or shunt tip culture. Fifty-three patients had adequate 1 year follow-up. The median duration of follow-up was 4.2 years. Statistical analysis was done using Graphpad Prism 7, and Fisher’s exact test was performed.
Results
For those with adequate follow-up, the overall 30-day and 1-year rates of shunt survival were 77% (41/53) and 34% (18/53), respectively. The 1-year shunt survival was 28% (9/32) for the adjustable valve group and 42% (9/21) for the flow-regulated valve group (p = 0.18) (Fig. 1).
The most common reasons for shunt revision were proximal blockage, distal blockage and shunt infection (Table 3). The total infection rate was 11% (6/53). Organisms grown included S. aureus (3/6, 50%), Coagulase Negative Staphylococcus (1/6, 17%), S. Epidermidis (1/6, 17%) and Pseudomonas (1/6, 16%).
There were two mortalities within the first year of life. One patient with a thoracic myelomeningocele died due to respiratory failure secondary to lung hypoplasia and pulmonary hypertension. Furthermore, this patient had a Chiari II malformation which potentially exacerbated their respiratory dysfunction. A foramen magnum decompression was performed; however, there may still have been brainstem dysfunction contributing to the poor respiratory function. The other patient had hydraencephaly.
Overdrainage
During the first year of the child’s life, clinical signs of overdrainage were seen in 45% (24/53) of the patients (Table 4). These clinical signs were seen in 59% (19/32) of patients primarily treated with ProGav 2 valves and 24% (5/21) of the patients treated with OSV II (p = 0.02).
In the Progav group, the mean initial shunt setting was 5 cmH2O (0–10). 53% (17/32) of the patients had their valve setting increased during the first year of life, and the net increase was 4 cmH2O (1–8). Valve adjustments were well tolerated except in one patient. Two patients with overdrainage had their valves changed to OSV II at ages 2 and 7 months old. One patient with a ProGav valve had a ProSA antigravity device added at 5 years old.
Five patients primarily treated with OSV II developed clinical signs of overdrainage during the first year of life; one of them had a valve change to ProGav 2.
Radiologically small ventricles were seen in 50% (16/32) and 29% (6/21) of the patients treated with ProGav and OSV valves, respectively (p = 0.25).
Two patients with ProGav valves developed scaphocephaly, and CT scans showed sagittal craniosynostosis (Fig. 2). There were no cases of craniosynostosis observed in patients treated with OSVs. The first patient’s primary valve setting was 3 cmH2O; however, by day three post op, she had developed sunken fontanelle, and at 3 months old, she had dropped centiles on her head circumference chart, and her skull vault sutures were overriding. Her valve setting was increased gradually to 10 cmH2O; nevertheless, signs of overdrainage continued to be observed, and by 12 months of age, she had developed a scaphoid head. Attempts were then made to increase the valve setting to 13 cmH2O, but this was not tolerated. The second patient’s primary valve setting was 5 cmH2O. At 3 months post op, she had developed overriding sutures and a left-sided subdural collection; therefore, the valve setting was increased to 9 cmH2O. Despite this, by 7 months old, the patient had developed sagittal craniosynostosis. Both patients have been referred to the craniofacial service and are currently being managed conservatively. However, the patients are being closely followed up in case skull vault reconstructive surgery is required in the future.
Underdrainage
During the first year of life, 24% (5/21) and 28% (9/32) of patients primarily treated with OSVs and ProGavs developed pseudomeningoceles, following either primary or revision shunt surgery (p = 0.7). This was successfully managed conservatively in 11 patients via the use of head bandages and decreasing the valve settings. However, two patients with OSVs and one with a ProGav underwent further surgery due to their pseudomeningocele.
Discussion
VP shunts have a higher failure rate in the paediatric population when compared to adults [29, 30]. Reddy et al. [29] found in their study that 78% of paediatric patients (age < 17 years) required at least one shunt revision, compared to 32% of the adults. In our series, 66% of the patients had required a shunt revision within 1 year of primary insertion. Shunt failure in infants (age < 1 years old) is higher than in older children [14, 31,32,33]. In particular, neonates have been shown to have the highest rate of shunt failure [30]. Gebert et al. [31] found in patients with a mean age of 4 months at the time of shunt insertion, a 1 year shunt survival rate of 69%. Furthermore, the shunt survival was found to be lower in pre-term infants. Thomale et al. [32] found that in infants aged less than 1 year old, the overall shunt survival was 61%. We observed a higher rate of shunt failure. However, the age at primary shunt insertion in our series was young; 18% and 64% of the patients had corrected gestation ages < 37 weeks and between 37 to 42 weeks at the time of primary shunt insertion, respectively. In our series, there was no statistical difference in the 1 year shunt survival between flow-regulated and adjustable valves. Moreover, there were similar rates of confirmed infection and blockage between the two groups. However, there were complications observed only in the adjustable valve group such as catheter disconnection which lead to early revision surgery. It is unlikely that these complications were secondary to the valve technology. Given the small sample size, this may have given a false impression of inferior shunt survival.
In our series, the intraventricular haemorrhage and myelomeningoceles were the most common causes of hydrocephalus. This is in line with the literature where 57–82% of patients with myelomeningoceles repaired postnatally require a shunt [10, 11, 13]. In patients with intraventricular haemorrhage, 39–93% of those who undergo a temporizing neurosurgical procedure will require a permanent VP shunt [1,2,3,4,5,6]. The 1-year shunt survival in intraventricular haemorrhage is approximately 65–71% [2, 7]. In our series, the 1-year shunt survival observed in patients with intraventricular haemorrhage and myelomeningoceles was 30% and 33%, respectively.
Our overall shunt infection rate was 11%. Evidence has shown that the shunt infection rate in patients less than 6 months old can be up to 24% (range 11–24%) [12, 23, 24, 31, 34, 35. Younger age at the time of shunt insertion has been identified as a predictor of CSF infection [23, 36,37,38]. Inserting a VP shunt into a premature neonate was shown to be associated with a fivefold increase in the risk of shunt infection [36]. The most common causative organism in our series was Staphylococcus aureus, whereas Staphylococcus epidermidis is often the most common in other studies [37, 38]. There was no difference in the infection rate between the two valve groups in our series. We have not carried out a secondary analysis of the infections observed, for example, whether or not fontanelle taps prior to primary VP shunt insertion increased the risk of infection.
Overdrainage during infancy can lead to subdural haematoma [22], craniosynostosis [39,40,41,42] and the slit ventricle syndrome later in life [8, 9, 41,42,43,44]. Furthermore, slit ventricles are associated with an increased risk of shunt blockage and requirement for revision surgery [8]. Our clinical criteria for identifying overdrainage included signs which are not specific to overdrainage. For example, sunken fontanelle may also occur secondary to dehydration. This could have potentially lead to false positives for overdrainage. There is evidence to suggest that flow-regulated valves may be associated with fewer complications in relation to overdrainage [21, 45]. Re-adjusting the opening pressure on a valve has shown to be an effective treatment for overdrainage and avoids further operations in the adult population [46]. However, this finding may not be applicable to neonates and infants with hydrocephalus. Weinzierl et al. observed that adjusting the shunt valve settings may not prevent slit ventricles in patients whom are non-ambulatory [8]. Furthermore, an adjustable gravitational antisiphon device, the ProSA, can be implanted in addition to the ProGav valve to reduce overdrainage. Tschan et al. found that the addition of a ProSA device was associated with complete resolution of overdrainage symptoms in approximately 90% of cases in an adolescent population [47].
Babies are often lying flat. At approximately 9–12 months, children may be able to pull themselves upright and stand while holding onto furniture. They may be walking independently by 12–18 months. At this age, their CSF dynamics may be similar to that of an adult, because the gravitational effects of being vertical will commence. However, it is likely that babies with shunts in situ have different CSF flow dynamics. As the Miethke ProGav valve antisiphon device relies on a gravitational unit. This may not be activated in a baby who is predominantly horizontal, leading to overdrainage of CSF. Alternatively, we may have observed high rates of overdrainage because the valve settings we used were too low. Flow-regulated valves are thought to minimize the effects of CSF drainage which occur due to valsalva manoeuvres, such as sneezing. Given that babies can spend several hours per day crying, there may be an added valsalva effect leading to overdrainage of CSF in differential pressure valves which does not apply to flow-regulated valves.
A large proportion of patients with adjustable valves required an increase in their valve setting. The ideal starting opening pressure is unknown. In our study, the mean primary valve setting was 5 cmH2O. However during the first 12 months, 50% of the patients had their valve setting increased.
Given the high frequency of overdrainage, it could be argued that starting with a higher opening pressure would be more ideal. However, we had one case of a premature baby with intraventricular haemorrhage whose initial valve setting was 2 cmH2O. We did not observe any clinical signs of overdrainage in this patient, and his valve setting was not changed. Furthermore, we also observed a high rate of pseudomeningocele. In most cases, this was successfully treated via decreasing the valve setting and applying a tight head bandage or sock. If a neurosurgeon was to insert a primary VP shunt with an adjustable valve set high, they may avoid overdrainage; however, this may be complicated by pseudomeningocele formation. Regardless of the initial valve setting, it is more likely that the important aspect of management is to have a form of monitoring in place to guide your valve adjustments. In our practice, we use the World Health Organization Head Circumference growth charts as a form of monitoring. We have found that this method helps us to identify patients experiencing CSF overdrainage and adjust their valves accordingly. There are other ways to monitor patients post-operatively, such as serial cranial ultrasound imaging to detect a decreasing ventricular size. There was no set protocol for monitoring the head circumference, so measurements were taken opportunistically. Therefore, we do not have robust data to demonstrate whether flow-regulated valves are associated with macrocephaly secondary to underdrainage.
Unfortunately, there was one patient with overdrainage in whom we were unable to adjust their valve setting. This was attributed to the baby having a soft skull vault and therefore difficulty with applying the pressure against the free floating cranial bones needed to change the ProGav valve setting. This is not a common issue for children with adjustable valves.
Despite overdrainage being seen more frequently in patients with ProGav 2 valves, the option to adjust the setting proved invaluable in several patients. Whereas, when overdrainage occurs in a patient with an OSV, there are no further non-operative treatment options available. In our series, we had one patient with an OSV who required surgery due to overdrainage where the valve was changed to a ProGav 2.
The limitations of our study include the small sample size and retrospective data collection. Furthermore, treatment allocation was not randomized, and patients received a shunt valve type depending on the surgeons’ preference. There was no assessment of the patients’ neurological development. Therefore, we have not investigated whether overdrainage leads to any long-term cognitive impairment.
Conclusion
In our series, irrespective of which valve is used, shunt failure rates are high when inserted during or immediately following the neonatal period. Overdrainage may be less common in patients with flow-regulated valves. However, if overdrainage is observed, adjusting the setting of a differential pressure valve can effectively treat the overdrainage without the need for invasive shunt revision surgery.
References
Whitelaw A, Evans D, Carter M, Thoresen M, Wroblewska J, Mandera M, Swietlinski J, Simpson J, Hajivassiliou C, Hunt LP, Pople I (2007) Randomized clinical trial of prevention of hydrocephalus after intraventricular hemorrhage in preterm infants: brain-washing versus tapping fluid. Pediatrics 119:e1071–e1078
Wang JY, Amin AG, Jallo GI, Ahn ES (2014) Ventricular reservoir versus ventriculosubgaleal shunt for posthemorrhagic hydrocephalus in preterm infants: infection risks and ventriculoperitoneal shunt rate. J Neurosurg Pediatr 14:447–454
Badhiwala JH, Hong CJ, Nassiri F, Hong BY, Riva-Cambrin J, Kulkarni AV (2015) Treatment of posthemorrhagic ventricular dilation in preterm infants: a systematic review and meta-analysis of outcomes and complications. J Neurosurg Pediatr 16(5):545–555
Limbrick DD Jr, Mathur A, Johnston JM, Munro R, Sagar J, Inder T, Park TS, Leonard JL, Smyth MD (2010) Neurosurgical treatment of progressive posthemorrhagic ventricular dilation in preterm infants: a 10-year single-institution study. J Neurosurg Pediatr 6:224–230
Lam HP, Heilman CB (2009) Ventricular access device versus ventriculosubgaleal shunt in post hemorrhagic hydrocephalus associated with prematurity. J Matern Fetal Neonatal Med 22:1097–1101
Wellons JC, Shannon CN, Kulkarni AV, Simon TD, Riva-Cambrin J, Whitehead WE, Oakes WJ, Drake JM, Luerssen TG, Walker ML, Kestle JR, Hydrocephalus Clinical Research N (2009) A multicenter retrospective comparison of conversion from temporary to permanent cerebrospinal fluid diversion in very low birth weight infants with posthemorrhagic hydrocephalus. J Neurosurg Pediatr 4:50–55
Alan N, Manjila S, Minich N, Bass N, Cohen AR, Walsh M, Robinson S (2012) Reduced ventricular shunt rate in very preterm infants with severe intraventricular hemorrhage: an institutional experience. J Neurosurg Pediatr 10:357–364
Weinzierl MR, Rohde V, Gilsbach JM, Korinth M (2008) Management of hydrocephalus in infants by using shunts with adjustable valves. J Neurosurg Pediatr 2:14–18
Miranda P, Simal JA, Menor F, Plaza E, Conde R, Botella C (2011) Initial proximal obstruction of ventriculoperitoneal shunt in patients with preterm-related posthaemorrhagic hydrocephalus. Pediatr Neurosurg 47:88–92
Adzick NS, Thom EA, Spong CY, Brock JW 3rd, Burrows PK, Johnson MP, Howell LJ, Farrell JA, Dabrowiak ME, Sutton LN, Gupta N, Tulipan NB, D'Alton ME, Farmer DL, Investigators M (2011) A randomized trial of prenatal versus postnatal repair of myelomeningocele. N Engl J Med 364:993–1004
Melo JR, Pacheco P, Melo EN, Vasconcellos A, Passos RK (2015) Clinical and ultrasonographic criteria for using ventriculoperitoneal shunts in newborns with myelomeningocele. Arq Neuropsiquiatr 73:759–763
Tuli S, Drake J, Lamberti-Pasculli M (2003) Long-term outcome of hydrocephalus management in myelomeningoceles. Childs Nerv Syst 19:286–291
Sankhla S, Khan GM (2009) Reducing CSF shunt placement in patients with spinal myelomeningocele. J Pediatr Neurosci 4:2–9
Liptak GS, Masiulis BS, McDonald JV (1985) Ventricular shunt survival in children with neural tube defects. Acta Neurochir 74:113–117
McMillan JJ, Williams B (1977) Aqueduct stenosis. Case review and discussion. J Neurol Neurosurg Psychiatry 40:521–532
Cinalli G, Spennato P, Nastro A, Aliberti F, Trischitta V, Ruggiero C, Mirone G, Cianciulli E (2011) Hydrocephalus in aqueductal stenosis. Childs Nerv Syst 27:1621–1642
Rodis I, Mahr CV, Fehrenbach MK, Meixensberger J, Merkenschlager A, Bernhard MK, Schob S, Thome U, Wachowiak R, Hirsch FW, Nestler U, Preuss M (2016) Hydrocephalus in aqueductal stenosis--a retrospective outcome analysis and proposal of subtype classification. Childs Nerv Syst 32:617–627
Filardi TZ, Finn L, Gabikian P, Giussani C, Ebenezer S, Avellino AM (2009) Treatment of intermittent obstructive hydrocephalus secondary to a choroid plexus cyst. J Neurosurg Pediatr 4:571–574
van Baalen A, Stephani U (2007) Flexible and floating choroid plexus cyst of the third ventricle: an ultrasonographic video documentation. Childs Nerv Syst 23:259–261
Drake JM, Kestle JR, Milner R, Cinalli G, Boop F, Piatt J Jr, Haines S, Schiff SJ, Cochrane DD, Steinbok P, MacNeil N (1998) Randomized trial of cerebrospinal fluid shunt valve design in pediatric hydrocephalus. Neurosurgery 43:294–303 discussion 303-295
Decq P, Barat JL, Duplessis E, Leguerinel C, Gendrault P, Keravel Y (1995) Shunt failure in adult hydrocephalus: flow-controlled shunt versus differential pressure shunts--a cooperative study in 289 patients. Surg Neurol 43:333–339
Pudenz RH, Foltz EL (1991) Hydrocephalus: overdrainage by ventricular shunts. A review and recommendations. Surg Neurol 35:200–212
Pople IK, Bayston R, Hayward RD (1992) Infection of cerebrospinal fluid shunts in infants: a study of etiological factors. J Neurosurg 77:29–36
Simon TD, Butler J, Whitlock KB, Browd SR, Holubkov R, Kestle JR, Kulkarni AV, Langley M, Limbrick DD Jr, Mayer-Hamblett N, Tamber M, Wellons JC 3rd, Whitehead WE, Riva-Cambrin J, Hydrocephalus Clinical Research N (2014) Risk factors for first cerebrospinal fluid shunt infection: findings from a multi-center prospective cohort study. J Pediatr 164:1462–1468 e1462
Duc G, Largo RH (1986) Anterior fontanel: size and closure in term and preterm infants. Pediatrics 78:904–908
Pindrik J, Ye X, Ji BG, Pendleton C, Ahn ES (2014) Anterior fontanelle closure and size in full-term children based on head computed tomography. Clin Pediatr (Phila) 53:1149–1157
Benjamin Neelon SE, Oken E, Taveras EM, Rifas-Shiman SL, Gillman MW (2012) Age of achievement of gross motor milestones in infancy and adiposity at age 3 years. Matern Child Health J 16:1015–1020
Kimura-Ohba S, Sawada A, Shiotani Y, Matsuzawa S, Awaya T, Ikeda H, Okada M, Tomiwa K (2011) Variations in early gross motor milestones and in the age of walking in Japanese children. Pediatr Int 53:950–955
Reddy GK, Bollam P, Caldito G (2014) Long-term outcomes of ventriculoperitoneal shunt surgery in patients with hydrocephalus. World Neurosurg 81:404–410
Wu Y, Green NL, Wrensch MR, Zhao S, Gupta N (2007) Ventriculoperitoneal shunt complications in California: 1990 to 2000. Neurosurgery 61:557–562 discussion 562-553
Gebert AF, Schulz M, Schwarz K, Thomale UW (2016) Long-term survival rates of gravity-assisted, adjustable differential pressure valves in infants with hydrocephalus. J Neurosurg Pediatr 17:544–551
Thomale UW, Gebert AF, Haberl H, Schulz M (2013) Shunt survival rates by using the adjustable differential pressure valve combined with a gravitational unit (proGAV) in pediatric neurosurgery. Childs Nerv Syst 29:425–431
Stone JJ, Walker CT, Jacobson M, Phillips V, Silberstein HJ (2013) Revision rate of pediatric ventriculoperitoneal shunts after 15 years. J Neurosurg Pediatr 11:15–19
Dallacasa P, Dappozzo A, Galassi E, Sandri F, Cocchi G, Masi M (1995) Cerebrospinal fluid shunt infections in infants. Childs Nerv Syst 11:643–648 discussion 649
Bakhsh A (2011) CSF shunt complications in infants--an experience from Pakistan. Pediatr Neurosurg 47:93–98
McGirt MJ, Zaas A, Fuchs HE, George TM, Kaye K, Sexton DJ (2003) Risk factors for pediatric ventriculoperitoneal shunt infection and predictors of infectious pathogens. Clin Infect Dis 36:858–862
Mancao M, Miller C, Cochrane B, Hoff C, Sauter K, Weber E (1998) Cerebrospinal fluid shunt infections in infants and children in Mobile, Alabama. Acta Paediatr 87:667–670
Renier D, Lacombe J, Pierre-Kahn A, Sainte-Rose C, Hirsch JF (1984) Factors causing acute shunt infection. Computer analysis of 1174 operations. J Neurosurg 61:1072–1078
Golinko MS, Atwood DN, Ocal E (2018) Surgical management of craniosynostosis in the setting of a ventricular shunt: a case series and treatment algorithm. Childs Nerv Syst 34:517–525
Doorenbosch X, Molloy CJ, David DJ, Santoreneos S, Anderson PJ (2009) Management of cranial deformity following ventricular shunting. Childs Nerv Syst 25:871–874
Ryoo HG, Kim SK, Cheon JE, Lee JY, Wang KC, Phi JH (2014) Slit ventricle syndrome and early-onset secondary craniosynostosis in an infant. Am J Case Rep 15:246–253
Weinzweig J, Bartlett SP, Chen JC, Losee J, Sutton L, Duhaime AC, Whitaker LA (2008) Cranial vault expansion in the management of postshunt craniosynostosis and slit ventricle syndrome. Plast Reconstr Surg 122:1171–1180
Petraglia AL, Moravan MJ, Dimopoulos VG, Silberstein HJ (2011) Ventriculosubgaleal shunting--a strategy to reduce the incidence of shunt revisions and slit ventricles: an institutional experience and review of the literature. Pediatr Neurosurg 47:99–107
Gruber RW, Roehrig B (2010) Prevention of ventricular catheter obstruction and slit ventricle syndrome by the prophylactic use of the Integra antisiphon device in shunt therapy for pediatric hypertensive hydrocephalus: a 25-year follow-up study. J Neurosurg Pediatr 5:4–16
Hanlo PW, Cinalli G, Vandertop WP, Faber JA, Bogeskov L, Borgesen SE, Boschert J, Chumas P, Eder H, Pople IK, Serlo W, Vitzthum E (2003) Treatment of hydrocephalus determined by the European Orbis Sigma valve II survey: a multicenter prospective 5-year shunt survival study in children and adults in whom a flow-regulating shunt was used. J Neurosurg 99:52–57
Freimann FB, Sprung C (2012) Shunting with gravitational valves--can adjustments end the era of revisions for overdrainage-related events?: clinical article. J Neurosurg 117:1197–1204
Tschan CA, Antes S, Huthmann A, Vulcu S, Oertel J, Wagner W (2014) Overcoming CSF overdrainage with the adjustable gravitational valve proSA. Acta Neurochir 156:767–776 discussion 776
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Henderson, D., Budu, A., Zaki, H. et al. A comparison between flow-regulated and adjustable valves used in hydrocephalus during infancy. Childs Nerv Syst 36, 2013–2019 (2020). https://doi.org/10.1007/s00381-020-04552-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-020-04552-3