Abstract
Objective
Spinal dermal sinus tract (DST) is a rare entity which usually comes to clinical attention by cutaneous abnormalities, neurologic deficit, and/or infection. We performed this study to assess presentation patterns, associated anomalies, radiologic, urologic, and surgical findings in children afflicted with spinal DST.
Methods
Medical records of 35 children treated for spinal DST in Children’s Medical Center from January 2001 to December 2008 were reviewed.
Results
Patients’ age ranged from 3 days to 8.44 years. Dermal sinuses were located most frequently in the lumbar and lumbosacral regions. The most common causes for referral were abnormal skin findings (57.1%) and infection (31.4%). Notably eight patients presented with meningitis. The overall rate of neurologic abnormalities was 37.1%, four of whom presented acutely with rapidly progressive paraplegia and meningitis. The most common magnetic resonance imaging finding was tethered cord (63%). At least one urological evaluation was performed in 30 patients, which revealed abnormal results in 77% of them. All patients underwent complete resection of the tract and repair of associated abnormalities. Most tracts terminated within the intradural space. Fifteen patients (42.8%) had inclusion tumor with the dermoid tumor being the most common. None of the patients demonstrated neurological deterioration postoperatively.
Conclusion
Dermal sinus tract is an innocuous-appearing spinal dysraphism that may contribute to devastating morbidities if not timely addressed. In order to prevent complications, timely surgical intervention including complete resection of sinus tract with intradural exploration and correction of associated abnormalities is of utmost importance.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Spinal dermal sinus tract (DST) is a rare congenital dysraphism which occurs in approximately one in every 2,500 live births [1, 9]. Dermal sinuses include a tract lined by epithelia, which traverse for a variable depth into the underlying structures and, in many instances, terminate within the thecal sac [2, 3].
They are seen more frequently at the extremes of neuroaxis with the majority of spinal DSTs occur in the lumbosacral region [9, 11]. Spinal DSTs may have diverse and occasionally serious presentations; in fact, many cases come to clinical attention by neurologic deficit and/or infectious complications including life-threatening conditions such as meningitis [8]. Moreover, DSTs are frequently associated with other anomalies of the central nervous system such as tethered cord, inclusion tumors, and split cord malformations (SCM) [2, 8]. So despite its benign external appearance, it may harbor great risks to the patients’ health if not timely addressed.
There are only a few published series of spinal DST in the literature considering the epidemiologic, clinical, and radiological aspects of this entity which lack detailed urological evaluations [2, 3, 8].
In this study, we present our experience with a group of children afflicted with this relatively rare form of spinal dysraphism including their presentation, radiological findings, surgical observations, and urological evaluations, emphasizing the importance of timely diagnosis and management of DSTs.
Patients and methods
This is a retrospective study conducted in Children’s Medical Center from January 2001 to December 2008. Medical records of all children treated for spinal dermal sinus were reviewed. Information regarding patients’ demographic variables, type of presentation, symptoms, physical examination, radiologic and urological studies, surgical findings, and histopathological evaluation were collected. Our routine approach is, whenever feasible, to perform spinal magnetic resonance imaging (MRI) and thorough urological evaluations including renal and bladder sonography, voiding cystourethrography (VCUG), and urodynamic study. All patients had done MRI except one who admitted with rapidly progressive neurologic deficit needing urgent operation, while MRI facility was not available. Urological evaluations were refused by some families due to economic problems and canceled in a few patients due to their need for emergent surgery.
Those patients who first assumed to have DST but finally this diagnosis was not confirmed by histological evaluations were excluded from the study.
Results
Thirty five patients (19 girls and 16 boys) with spinal dermal sinus were identified from the hospital records. Patients’ age on admission ranged from 3 days to 8.44 years (median 1.13 years). Dermal sinuses were located most frequently in the lumbar and lumbosacral areas (Table 1). Two patients had previously undergone partial surgical procedures before their referral to our center.
Clinical presentations
The most common reasons for referring the patients to neurosurgery service were abnormal skin findings (57.1%) and infectious manifestations (31.4%) (Table 2). Eight patients were admitted with acute meningitis, four of whom had found rapidly progressive paraplegia and were operated on urgently. A 3-day-old girl underwent urgent surgery due to cerebrospinal fluid leakage from a lumbar sinus since birth. A 3-year-old girl was referred due to failure to thrive and recurrent urinary tract infection in association with a lumbosacral DST.
Cutaneous findings
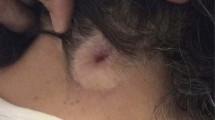
In the majority of the patients (77.1%), sinus ostium was associated with another skin abnormality, the most common of which were inflammation of surrounding skin and abnormal pigmentation (Table 3). Some patients had a combination of these findings. A 7-month-old boy who also had experienced two bouts of meningitis presented with cerebrospinal fluid leakage from the sinus ostium. Dermal sinuses were seen in conjunction with subcutaneous lipoma and myelomeningocele in four and one patients, respectively. Interestingly, three patients had more than one DST. Two patients had two midline dermal sinuses in lumbosacral and sacral regions. The other one had three lumbosacral DSTs located in a triangular order.
Infection
Notably 17 (48.6%) patients had some kind of infection on admission (Table 4). The great majority (88.2%) of them had a combination of these infectious features. Eight patients (23%) had active meningitis on admission. History of recurrent meningitis was positive in four cases. Interestingly, one patient presented initially with brain abscess without any obvious predisposing factor. She presented 1 month after discharge with meningitis and rapidly progressive paraplegia which then found to have an undiagnosed tiny lumbosacral dermal sinus tract with an infected dermoid tumor and intradural abscess.
Those patients presenting with infectious complications were managed with appropriate antibiotics and then after recovery surgery for resection of DST, and correction of associated anomalies was performed.
Neurological findings
Thirteen patients suffered from neurologic abnormalities, four of whom presented acutely (Table 5). Lower limb weakness and atrophy, scoliosis, motor delay, urinary incontinence, and chronic constipation were the other neurologic manifestations in our patients. Five patients also had back pain at the time of presentation, which obviously could be assessed reliably in older children. One patient was admitted for raised intracranial pressure and severe hydrocephalus subsequent to previous episode of meningitis. Orthopedic deformities including scoliosis, club foot, pes cavus, or planus were found in four patients.
To evaluate the effect of age on the type of presentation, we categorized the patients into two age groups: younger and older than 1 year. Seventy one percent of patients, who were older than 1 year at the time of presentation, had infectious manifestations. The rate of infectious complications was significantly higher in patients older than 1 year than those who were younger (p = 0.011). However, younger age did not turn out to be significant when considering neurologic abnormalities (p = 0.06).
Neuroimaging
Magnetic resonance imaging was performed in 34 patients to evaluate the sinus and investigate the probable associated abnormalities (Fig. 1). It was not obtained in one patient considering the lack of emergent MRI facility, since she presented acutely with paraplegia and underwent urgent decompressive surgery. The most common MRI finding was tethered cord seen in 22 (63%) patients (Table 6).
a Magnetic resonance imaging of the patient referring with acute paraplegia and sepsis shows the abscess and the enhancement of inflammatory process with Gadolinium. Due to anatomical distortions, intradural dermoid and thick filum observed intraoperatively are not obvious. b Tethered cord due to the stalk extending from the sinus to the intradural space and attached to the distal part of cord. c Intradural dermoid tumor attached to the thin stalk extending from the sinus to the intradural space producing a tumor far from the sinus location which is apparent in (d) T2-weighted image. e Tethered cord an associated anomaly without any relation to dermal sinus and tract. Cord is tethered with a thick filum
Urological evaluations
At least one urological evaluation was performed in 30 patients. Renal and bladder sonography was obtained in 26 patients before surgery, four of whom were found to have hydronephrosis. Voiding cystoureterography was performed in 29 patients and revealed vesicoureteral reflux in seven (24.1%) patients who were referred to urological service for further management after their surgery (Fig. 2). Urodynamic studies were performed in 25 patients, which disclosed increased bladder pressure in 16 patients (64%) and detrusor sphincter dyssynergia (DSD) in eight (32%) (Table 7).
Operative findings
All children underwent surgical resection of the DST with repair of associated abnormalities found on MRI. Those patients who did not constitute an emergency underwent surgery after obtaining MRI and performing urological evaluations. Patients who were diagnosed in neonatal period were followed up till 3 months of age before carrying out the surgery except for the case referred due to cerebrospinal fluid leakage. Intradural exploration was performed in all cases to observe the normal cord, release any potential adhesions, and exclude any other accompanying anomalies which were supposed to be obscured on MRI (especially in younger patients). Intraoperatively, the most common point where the tracts ended was the intradural space (46.2%) (Table 8).
Fifteen patients (42.8%) had associated tumor with the dermoid tumor being the most common tumor found (Table 9). They were often located in intradural space but could be found in all tissue planes from subcutaneous tissue to intramedullary location. One patient had more than one dermoid tumor along her sinus tracts which were located inside and outside of the dural space. Another child with triple sinuses also had two subcutaneous dermoid tumors at the termination of the upper tracts. Of note, culture of the tumor material revealed the tumor to be infected in eight patients (mostly by Gram-negative bacteria). Forty percent of the patients found to have tight filum terminal intraoperatively. Thirteen (33.3%) patients had arachnoid changes compatible with current or previous arachnoiditis, which all of them except one had a history of infection.
None of the patients demonstrated neurologic deterioration postoperatively. Neurologic function gradually returned to near normal state postoperatively in three of four patients presented with acute paraplegia. Four other cases who had motor weakness for a while before admission found good recovery after releasing their tethered cord and decompressing the neural tissue from tumor or abscess mass effect. Urologic problems remained refractory after the surgery in all children who demonstrated abnormal results on preoperative clinical and paraclinical evaluations. These patients were referred to urology clinic for further evaluation and treatment. Back pain was improved totally after correction of the causative abnormalities.
Discussion
Current literature contains many case reports of patients with spinal dermal sinuses but only limited studies with sufficiently large number of patients have been published [2, 3, 8]. Here, we report the clinical and paraclinical findings of 35 patients afflicted with spinal DST.
Incidence
The incidence of DSTs is usually cited as one in 2,500 live births [9, 13]. However, this figure may not reflect the actual incidence of dermal sinuses, since it is derived from studies which lack sufficient evidence to back up their diagnoses. There is also a possibility that some of the cases were benign sacrococcygeal dimples which were inadvertently included in the study [1]. There are different reports regarding the gender difference in the literature [2, 3, 8]. We found more afflicted girls in our study (54.3%) which is compatible with the Ackerman et al. study [2]. Dermal sinus may involve any level of the neuroaxis with the cervical region affected less than the other segments (<1%). Thoracic area is involved in 10% of cases, lumbar in 40%, lumbosacral in 12%, sacral in 23%, and sacrococcygeal junction in 13% of cases [8]. Most patients in our study had lumbosacral and lumbar dermal sinuses.
Pathology
Congenital dermal sinus tract of the spine is a relatively uncommon developmental defect characterized by a tract lined by the squamous stratified epithelium, extending from the skin surface for a variable distance into the underlying structures [2, 8]. Dermal sinuses are usually seen in the midline but may be found in the paravertebral location [7, 16]. Dermal sinuses may end in any tissue plane; in 6–7% of the cases, the tracts terminate blindly within the underlying soft tissue and dorsal to the vertebral column. Many enter the vertebral canal under or through a bifid lamina. The tracts end in epidural space in 10–20% of the patients [8]. However, in the majority of the cases (58–60%), DSTs pass through the dura to end within the thecal sac and of these, approximately one half will attach to conus medullaris, cauda equine, or filum terminale [1, 16]. They may also extend rostrally a considerable distance to reach several spinal levels above the cutaneous ostium [8, 9]. In our study, most DSTs entered the intradural space (46.2%). Of those DSTs which pass through the dura mater, some may communicate directly with intradural tumors as was the case in seven patients in this series. Notably the extension of tract was the cause of spinal cord cleavage in one patient with SCM type 1.
Dermal sinuses should be distinguished from the more common coccygeal pits. Dermal sinuses are located above the intergluteal cleft, have a cephalically oriented course, and are often associated with other pathologies. On the contrary, coccygeal dimples are usually simple blind sinuses with no associated cutaneous abnormalities which lie within intergluteal cleft a few millimeters cranial to the tip of coccyx. They are oriented caudally or straight and are not associated with other intradural pathologies and thus not warrant further evaluation [2, 3, 8]. Although they rarely have intraspinal extension, it should be remembered that not all coccygeal pits can be dismissed. If a sacral or coccygeal dimple is associated with other cutaneous abnormalities such as hypertrichosis or soft tissue mass, they should be investigated accordingly.
Embryogenesis
Although the embryological origin of the DST is not clearly described, the most widely accepted theory is incomplete disjunction [9]. Between weeks 3 and 5 of embryonic life, two layers of ectoderm, neuroectoderm, and cutaneous ectoderm separate from each other allowing for insertion of mesodermal tissue destined to form vertebral column and musculature [2, 11]. If the cutaneous ectoderm fails to separate from the neural tube at a point, a tract lined by epithelia which is surrounded by dermal elements can develop and constitutes a permanent connection between skin and the spinal cord. Although no level is spared, there is a higher incidence of dermal sinus tracts in regions where the last place of neural tube closure occurs, namely the occipital and lumbosacral regions [9, 11].
Clinical features
Spinal dermal sinuses have been associated with a wide spectrum of clinical manifestations ranging from asymptomatic cutaneous findings to infection, neurological deficit, urinary problems, and orthopedic deformities. Many of the well-described posterior midline cutaneous stigmata may be associated with dermal sinuses including abnormal pigmentation, hemangioma, and hypertrichosis. Other less common accompanying lesions are subcutaneous fatty tissue in the form of spinal lipoma and human tail which is exceedingly rare [14]. In addition, signs of infection such as erythema, induration, and purulent drainage may be seen as a result of local or deep-seated infections. In rare instances, cerebrospinal fluid leakage may occur [5].
Previously, DSTs have generally come to clinical attention after recurrent bouts of meningitis or when the neurologic deficit caused by tethered cord or mass effect of a slowly growing tumor became evident. In 1975, Powell encountered a high rate (75%) of infection among his patients with 59% having meningitis [13]. French had a majority of patients (61%) presented with infection [1]. However, due to increased awareness among the primary care physicians, this entity is now diagnosed earlier than the past. In the study performed by Ackerman et al., cutaneous findings were the predominant (54%) presenting features [2]. Most of our patients (57.1%) were also referred due to cutaneous findings and all except for two had normal neurologic examination. However, 37.1% of our patients had neurological impairment on presentation.
Dermal sinuses provide a portal of entry for bacterial agents into the intraspinal compartments which can cause meningitis or abscess formation. In addition, aseptic meningitis can occur by spillage of inclusion tumor contents or other dermal elements into the cerebrospinal fluid [9, 11, 16]. Therefore, one should have a high level of suspicion for DST and dermoids when encountering any young child presenting with aseptic meningitis. In recent series, relatively lower infection rates have been reported. In the study conducted by Jindal et al. [8], only one patient presented with infection. Ackerman et al. [2] also had a low rate (10%) of infectious complications. Among our patients, 37.1% had meningitis on admission or had experienced it before. This high infection rate suggests that there is still much to be done to raise the knowledge of first line health care providers about the significance of cutaneous stigmata over the neuroaxis.
Infection is the most serious risk associated with spinal dermal sinus. In addition to meningitis, it can also result in extradural, subdural, and intramedullary abscess or infection of an associated tumor. The incidence of abscess formation in our patients was 25.7%, which most of them were located intradurally and were accompanied by meningitis on presentation. Notably a previously healthy 1-year-old girl presented with brain abscess which is an extremely odd presentation for DST [4]. This unusual presentation of DST highlights the need for thorough physical examination in patients presenting with any central nervous system infections, especially in pediatric age group and when no obvious predisposing factors are found. Unfortunately, in many instances, a small opening in the skin, which sometimes only becomes apparent with the aid of magnification or subsequent to purulent discharge, may be overlooked on physical examination.
Hydrocephalus is a well-known complication of post-infectious meningitis. In addition, ventriculitis and/or arachnoiditis caused by spillage of dermoid tumor contents can also result in hydrocephalus. The occurrence of hydrocephalus in patients with dermal sinus has been rarely reported, the incidence of which is assumed to be 3.13% [11]. In this study, we had only one patient who had hydrocephalus in conjunction with two infected intradural dermoid tumor.
It has been said that nearly all children with DSTs have intact neurological function at birth [8]. However, due to the relatively high rates of associated pathologies such as tethered cord, infection, and inclusion tumors, neurological deterioration becomes more common with increasing age.
It has been shown that the chance of neurologic deficit development is higher in patients who present in older ages [2]. Ackerman et al. studied the referral pattern among their patients and noted that patients who were younger than 1 year were more likely to be neurologically intact than older ones, concluding that delay in the diagnosis allows for development of neurologic sequelae [2]. Unfortunately, once a patient develops neurologic deficit, there is a relatively high chance of permanent defect [5, 8]. We did not find a significant association between a certain age at presentation and development of neurologic sequelae. However, our data shows that there is significantly higher chance for development of infectious complications in children older than 1 year. This association shows how important the timely diagnosis and management of DSTs are.
Associated pathologies
Spinal dermal sinuses may be accompanied by other forms of spinal dysraphism such as lipomyelomeningocele and myelomeningocele, reflecting a possible common ontogenic pathway [6]. Gupta et al. showed an association of 11.34% between dermal sinus and other forms of spinal dysraphism [5]. The proposed mechanism for lipomyelomeningocele embryogenesis also includes disorders of disjunction which occurs prematurely in this entity. It is possible that there are some shared molecular pathways responsible for concurrence of these anomalies.
Dermal sinuses are occasionally associated with tethered cord, although they comprise only 1% of patients with this condition [2]. Although there is a considerable variability amongst normal patients with regard to level of the conus, those which terminate below the L2–L3 intervertebral space are considered to be abnormal. In patients with DST, the tract or associated tumor may cause traction on spinal cord resulting in a low-lying conus and tethered cord syndrome [10]. In our study, 22 patients (63%) had tethered cord. Most patients who presented with neurological deficit had tethered cord (70%) but it cannot be applied in reverse.
It is reported that up to 40% of patients with DST can have SCM [3]; conversely, DSTs are seen in 15–40% of split cord malformations [16]. Among our patients, five had SCM, three with type 1 and two with type 2. In one of the patient with type 1 SCM, the sinus tract itself was the cause of cord splitting.
The incidence of filum terminale abnormalities has not been clearly reported yet. Jindal et al. found filum abnormalities in 22% of his patients [8]. The term tight filum terminale refers to a set of conditions in which a low-lying conus medullaris is associated with a short thickened filum without evidence of other tethering pathologies [9, 10]. This entity which arises from failed regression of caudal spinal cord during secondary neurulation causes typical signs and symptoms of tethered cord. Forty percent of patients in our study were found to have thick filum terminale intraoperatively.
Approximately half of all dermal sinuses are associated with dermoid or epidermoid tumor, usually at the termination of these tracts, but they may be located anywhere between the skin and the neural tube [2, 12]. Dermal sinuses and dermoid tumors seem to share a common origin [11]. They are believed to result from focal expansion of these ectoderm-derived tracts. However, only approximately 30% of intraspinal dermoid tumors have an associated sinus tract [9]. While epidermoid tumors are ten times as frequent as dermoid [8, 12], DSTs are associated more frequently with dermoid tumors (83%) than with epidermoid (13%) [5]. We had 13 patients (37.1%) with dermoid tumor and two with epidermoid (5.7%) proved by histology.
Neuroimaging
Although plain film radiographs of the spine may provide some evidence of spinal dysraphism (Fig. 2), it has limited utility in evaluation of DSTs. Magnetic resonance imaging is a crucial part of preoperative evaluations in these patients. Although MRI may miss intraspinal portions of the tract, it is especially useful for determining the level of conus and detecting any other associated anomalies such as inclusion tumors or split cord malformation [3, 8]. It can also help the surgeon predict the extent of the surgery.
Ultrasound is also a well-established imaging modality for evaluating spinal dysraphism in infants. The sinus tract, position of the conus, filum terminale, and presence of any other associated pathology can be reliably assessed with ultrasound and it is also of major help in differentiating dermal sinuses from coccygeal dimples [15, 17]. Moreover, MRI may not yield clear images in neonates due to artifacts caused by rapid pulse and respiration. In these cases, spinal ultrasound may be a more suitable screening modality for diagnosing tethered cord, SCM, or associated tumors. However, the utility of this technique declines in patients older than 4 months when ossifying posterior elements of the spine limits the acoustic window [15]. Despite the invaluable information these imaging modalities provide, the exact site of tract termination and its relationship would not be revealed unless visualized intraoperatively.
Urological aspects
As other forms of spinal dysraphism, these patients are at increased risk of urinary tract dysfunction in addition to other neurologic deficits. Patients may have suffered structural damage of urinary tract at the time of presentation. To the best of our knowledge, none of the previous studies have revealed detailed urological evaluations in these patients. We performed urological evaluations in the majority of our patients, which demonstrated high rate (72%) of abnormal urodynamic findings. Of note, a much lower percentage showed abnormal results on renal sonography and VCUG. Indeed, urodynamic study can detect urinary tract dysfunction before structural damages take place. We would suggest that urodynamic study be the major component of urological evaluations in these patients. Obviously, by performing urological evaluations, at-risk patients could be recognized and preventive measure instituted. Urological interventions may be indicated for patients with urinary tract problems unresponsive to medical treatments.
Surgery
Since none of the imaging modalities can accurately show intraspinal details, all dermal sinuses above the sacrococcygeal region should be explored operatively regardless of neuroimaging findings [3, 9]. The tract should be excised totally to the point of termination; however, resection of the tract without intradural exploration does not seem to be sufficient. There are reports that have demonstrated that patients without primary dural exploration developed neurological deterioration, which required reexploration and treating the unnoticed underlying anomalies [1]. In our study, 40% of the patients were found to have tight filum during the surgery, although it was evident in only 23% of preoperative MRIs. In addition, tissue changes compatible with old or active arachnoiditis such as arachnoid adhesions, which can potentially contribute to tethered cord, were present in 33.3% of the patients. So the dura should always be opened, intradural extension of the lesion evaluated, and any associated pathologies treated accordingly. In cases with intradural infection and anatomical distortion (Fig. 1e), precise exploration is necessary to prevent postoperative neurological damage [18].
Although there has been increased awareness about the importance of dorsal midline cutaneous findings among primary care physicians, there is still much to be done, especially in developing countries. Due to its usually benign and innocuous external appearance, there is always the potential of the lesion being missed or dismissed inadvertently. Early diagnosis and referral allows for timely neurosurgical intervention which can significantly decrease morbidities caused by development of complications secondary to infection, tethered cord, or tumor size increment.
Conclusion
Detection of subtle cutaneous anomalies like dermal sinus in a child can be crucial in preventing serious neurologic, urologic, and orthopedic morbidities. Surgical intervention should be done as soon as possible and in advance of development of neurologic deficit. First line physicians should become more aware of the importance of cutaneous findings over midline neuroaxis.
References
Ackerman LL, Menezes AH, Follett KA (2002) Cervical and thoracic dermal sinus tracts. A case series and review of the literature. Pediatr Neurosurg 37:137–147
Ackerman LL, Menezes AH (2003) Spinal congenital dermal sinuses: a 30-year experience. Pediatrics 112:641–647
Elton S, Oakes WJ (2001) Dermal sinus tracts of the spine. Neurosurg Focus 10(1):1–4
Emami-Naeini P, Mahdavi A, Ahmadi H, Baradaran N, Nejat F (2008) Brain abscess as a manifestation of spinal dermal sinus. Ther Clin Risk Manag 4:1143–1147
Gupta DK, Shastank RR, Mahapatra AK (2005) An unusual presentation of lumbosacral dermal sinus with CSF leak and meningitis. A case report and review of the literature. Pediatr Neurosurg 41:98–101
Hung PC, Wang HS, Wu CT, Lui TN, Wong AM (2007) Spinal intramedullary abscess with an epidermoid secondary to a dermal sinus. Pediatr Neurol 37:144–147
Ikwueke I, Bandara S, Fishman SJ, Vargas SO (2008) Congenital dermal sinus tract in the lateral buttock: unusual presentation of a typically midline lesion. J Pediatr Surg 43:1200–1202
Jindal A, Mahapatra AK (2001) Spinal congenital dermal sinus: an experience of 23 cases over 7 years. Neurol India 49:243–246
Kaufman BA (2004) Neural tube defects. Pediatr Clin North Am 51:389–419
Lew SM, Kothbauer KF (2007) Tethered cord syndrome: an updated review. Pediatr Neurosurg 43:236–248
Martinez-Lage JF, Perez-Espejo MA, Tortosa JG, de San R, Pedro J, Ruiz-Espejo AM (2006) Hydrocephalus in intraspinal dermoids and dermal sinuses: the spectrum of an uncommon association in children. Childs Nerv Syst 22:698–703
Morandi X, Mercier P, Fournier HD, Brassier G (1999) Dermal sinus and intramedullary spinal cord abscess. Report of two cases and review of the literature. Childs Nerv Syst 15:202–206 discussion 207–208
Ramnarayan R, Dominic A, Alapatt J, Buxton N (2006) Congenital spinal dermal sinuses: poor awareness leads to delayed treatment. Childs Nerv Syst 22:1220–1224
Samura K, Morioka T, Hashiguchi K, Yoshida F, Miyagi Y, Yoshiura T, Suzuki SO, Sasaki T (2009) Coexistence of a human tail and congenital dermal sinus associated with lumbosacral lipoma. Childs Nerv Syst 25:137–141
Schenk JP, Herweh C, Gunther P, Rohrschneider W, Zieger B, Troger J (2006) Imaging of congenital anomalies and variations of the caudal spine and back in neonates and small infants. Eur J Radiol 58:3–14
Tubbs RS, Frykman PK, Harmon CM, Oakes WJ, Wellons JC III (2007) An unusual sequelae of an infected persistent dermal sinus tract. Childs Nerv Syst 23:569–571
Unsinn KM, Geley T, Freund MC, Gassner I (2000) US of the spinal cord in newborns: spectrum of normal findings, variants, congenital anomalies, and acquired diseases. Radiographics 20:923–938
van Aalst J, Beuls EA, Cornips EM, Vanormelingen L, Vandersteen M, Weber JW, Vles JS (2006) Anatomy and surgery of the infected dermal sinus of the lower spine. Childs Nerv Syst 22:1307–1315
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Radmanesh, F., Nejat, F. & El Khashab, M. Dermal sinus tract of the spine. Childs Nerv Syst 26, 349–357 (2010). https://doi.org/10.1007/s00381-009-0962-z
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-009-0962-z