Abstract
Purpose
Local ablative treatment to oligometastatic patients can result in long-term disease-free survival in some cancer patients. The importance of this treatment paradigm in prostate cancer is a rapidly evolving field. Herein, we report on the safety and preliminary clinical outcomes of a modern cohort of oligometastatic prostate cancer (OPC) patients treated with consolidative stereotactic ablative radiation (SABR).
Methods
Records of men with OPC who underwent consolidative SABR at our institution were reviewed. SABR was delivered in 1–5 fractions of 5–18 Gray. Kaplan–Meier estimates of local progression-free survival (LPFS), biochemical progression-free survival (bPFS; PSA nadir + 2), distant progression-free survival (DPFS), and time-to-next intervention (TTNI) were calculated.
Results
In total, 66 OPC patients were identified with consolidative SABR delivered to 134 metastases: 89 bone, 40 nodal, and 5 viscera. The majority of men (49/66) had hormone-sensitive prostate cancer (HSPC). Crude grade 1 and 2 acute toxicities were 36% and 11%, respectively, with no ≥ grade 3 toxicity. At 1 year, LPFS was 92% and bPFS and DPFS were 69%. Of the 18 men with HSPC who had deferred hormone therapy , 11 (56%) remain disease free following SABR (1-year ADT-FS was 78%). In 17 castration-resistant men, 11 had > 50% prostate-specific antigen (PSA) declines with 1-year TTNI of 30%.
Conclusions
Consolidative SABR in OPC is feasible and well tolerated. The heterogeneity and small size of our series limit extrapolation of clinically meaningful outcomes following consolidative SABR in OPC, but our preliminary data suggest that this approach warrants continued prospective study.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Originally proposed by Hellman and Weichselbaum [1], the oligometastatic or low-volume metastatic state is currently defined as having fewer than three-to-five metastatic lesions [2]. As the collective understanding of this state evolves, biological parameters may someday inform or supplant this descriptive clinical definition [3,4,5]. Improvements in imaging and metastasis-directed therapies (MDT) have placed new emphasis on the oligometastatic state [6]. Local ablative treatment for limited metastatic disease has been correlated retrospectively with improvements in long-term disease-free survival in lung, breast, colorectal, and sarcoma patients [6] and mounting prospective evidence suggests improvements in progression-free survival for oligometastatic lung cancers and hormone-sensitive oligorecurrent prostate cancer [7,8,9,10].
Traditionally, metastatic prostate cancer has been, regardless of tumor burden, treated systemically with androgen-deprivation therapy (ADT) and/or chemotherapy [11]. The importance of consolidating all macroscopic tumor deposits in men with oligometastatic prostate cancer is an area of active investigation [9, 12, 13], but the observation that men with lower numbers of metastases have better outcomes [14,15,16] supports a fundamental difference between oligometastatic prostate cancer (OPC) and higher volume disease. By this logic, recent studies have explored MDT of OPC by ablative and surgical treatments [17,18,19,20], as well as stereotactic ablative radiation (SABR) [21], also known as stereotactic body radiation therapy (SBRT) [22]. This highly targeted, high-dose approach provides millimeter-scale precision while minimizing collateral tissue damage and has shown efficacy in the management of OPC [17,18,19, 21, 23, 24].
Studies to date have been conducted predominately in patients with a single metastasis [9, 17,18,19, 23, 24]. Herein, we review our early institutional outcomes with SABR for OPC in 66 consecutively treated patients with the majority having ≥ 2 metastases. We demonstrate that SABR is well tolerated and can significantly delay time to subsequent intervention.
Methods
Criteria
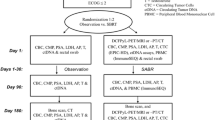
With approval from our institutional review board, we reviewed our retrospectively collected Johns Hopkins prostate cancer (PCa) radiation oncology database for consecutively SABR-treated patients from 02/07/2011 to 1/15/2017. Inclusion criteria were: biopsy-proven PCa, diagnostic imaging consistent with ≤ 5 metastases, and follow-up with post-SABR prostate-specific antigen (PSA) testing. Three patients with ≤ 5 initially observed metastases who were found during treatment planning to have six metastases were included. Of the 84 total men during this period with OPC treated with SABR, we only examined the first 66 men to allow for a minimum of 4.5 months of follow-up.
SABR technique
During CT simulation, patients were immobilized using an Alpha Cradle (Smithers Medical Products, Inc, North Canton, Ohio) or equivalent device. Magnetic resonance imaging (MRI), bone scan, NaF, or DCFPyL positron emission tomography [25]/CT images were used to delineate the gross tumor volume (GTV) and when possible fused with the planning CT. As per our institutional policy, if patients had ≥ 3 mm breathing motion on four-dimensional CT, active breathing control (ABC) was used for motion management. If breathing was < 3 mm, patients were treated free breathing (FB) with an internal target volume based on the 0% and 60% phases of the breathing cycle. GTV was defined as the sum of the abnormalities noted on PET, MRI T1 post-gadolinium sequences, bone scan, and/or CT. In general, the clinical tumor volume (CTV) was equal to the GTV. Most commonly, the planning target volumes (PTV) were the GTV with the addition of 3–5 mm used as the volume to which the prescription was assigned [17]. If men were treated with CyberKnife, then image guidance was as per that device. During non-CyberKnife SABR delivery, a cone-beam CT scan was co-registered (spine) with the FB or ABC simulation scan. To verify tumor positioning before SABR, patients were shifted to align with the GTV for each beam based on fluoroscopy, cone-beam CT, or kV images.
Follow-up
Patients were scheduled for serial follow-up exams every 3–6 months with history and physical, PSA, testosterone, and imaging every 6–12 months unless a shorter interval was clinically indicated. Repeat imaging with NaF or DCFPyL PET/CT, MRI, or bone scans was conducted at 3–6-month intervals after SABR. The majority of patients were treated by a limited number of Johns Hopkins medical oncologists with similar practice patterns. Therefore, broadly, the indication for the next intervention was determined by disease-objective evidence of disease progression by PSA and/or radiographic testing or symptomatic progression.
Statistical analysis
Clinical endpoints reported include biochemical progression-free survival (bPFS), local progression-free survival (LPFS), distant progression-free survival (DPFS), overall survival (OS) [25], ADT-free survival (ADT-FS), and time-to-next intervention (TTNI); all were calculated from the date of SABR. Biochemical failure was defined as: (1) PSA rise ≥ 2 above nadir following SABR or (2) an increase of PSA following SABR with failure to decline initially. LPFS was defined as the lack of tumor progression within the treated planning tumor volume (PTV) margin on follow-up imaging. DPFS was defined as the lack of new metastases on follow-up imaging. For both local and distant progression-free survival, clinically significant events (e.g., bone fractures) in a previously stable lesion were considered as clinical progression. TTNI was defined as the interval to the next local or systemic intervention due to progression. The Kaplan–Meier method was used to estimate the rates of bPFS, LPFS, DPFS, OS, ADT-FS, and TTNI. Analysis of LPFS was performed with each treated lesion considered individually (n = 134), while all the other endpoints were analyzed with each patient considered individually.
Results
Patient and disease characteristics
Sixty-six men with 134 metastatic PCa lesions were identified and analyzed. Prior treatment of metastatic tumors (including radiation and surgery) did not exclude patients from this review. Patients were generally asymptomatic or had minimal pain associated with their metastatic burden. Thirty-eight percent of men presented with synchronous or de novo oligometastases, while 62% developed metachronous oligometastases between the conclusion of definitive treatment for their prostate cancer and consultation for SABR treatment. Prior chemotherapy was allowed with 55% (n = 36) of patients receiving chemotherapy prior to or concurrently with treatment. Forty-nine (or 74%) men had hormone-sensitive prostate cancer (HSPC) at the time of SABR and 17 (or 26%) had castration-resistant prostate cancer (CRPC). Initial Gleason scores (GS) were as follows: GS 6 (n = 7), GS 7 (n = 16), GS 8 (n = 18), GS 9 (n = 22), and GS 10 (n = 3). Additional patient and disease characteristics are shown in Table 1.
The median and mean PSA reported prior to SABR were 1.2 ng/mL and 9.0 ng/mL, respectively. The majority of patients, 68% (n = 45), underwent SABR with a PSA ≤ 5. Fifty-three percent of men (n = 35) had ≥ 2 metastases. Consolidative SABR was delivered to a total of 134 metastases, with 89 osseous (66%), 40 nodal (30%) and 5 visceral (4%) lesions. The mean GTV was 9.1 cm3 (range 0.1–152.3 cm3). Additional patient characteristics at the time of SABR are shown in Table 2. SABR was delivered to all lesions with a total dose in the range of 15–55 Gy. The majority of lesions (72%) were treated with total doses > 15 Gy with varied fractionation, while 28% of lesions were treated with 15 Gy as a single fraction (Supplemental Table 1).
Clinical outcomes
Median and mean follow-up were 61 and 66 weeks, respectively. Acute toxicities were noted in 46% (n = 30) of patients, whereas late toxicities were noted in 27% (n = 18) of patients with the most common toxicities being fatigue and hot flashes (Supplemental Table 2). In total, grade 1 toxicities were noted in 24 patients and grade 2 toxicities were noted in 7. There were no grade 3 or higher toxicities observed.
The average time to any failure was 35 weeks. Overall, LPFS at 1 year was 92% (Fig. 1a) with LPFS of 100% for SABR biologically equivalent doses (BED with α/β = 10) of > 50. The bPFS and DPFS for the entire cohort at 1 year were each 69% (Fig. 1b, c). For all types of failure, men with oligometastatic HSPC had better outcomes than those with CRPC (Fig. 1a–c). Twenty-two men had a new intervention secondary to progression of their disease post-SABR, with median TTNI not reached overall with our current follow-up of 15 months (Fig. 2a). Of the 18 men with HSPC who were not treated with adjuvant hormone therapy, 11 (61%) remain free of disease following SABR corresponding to a 1-year ADT-FS of 78% (Fig. 2b) and a median ADT-FS that was not reached. Of the 17 men with oligometastatic CRPC treated with SABR, 11 had > 50% PSA that declines with a 1-year TTNI of 38% (Fig. 2a) and a median TTNI of 45 weeks. This was congruent with a 1-year bPFS and DPFS of 43% and 33%, respectively (Fig. 1b, c), in men with CRPC. During the study period, two patients died: one of the complications related to their metastatic CRPC and the other from unconfirmed causes not likely related to prostate cancer.
Effect of stereotactic ablative radiotherapy on clinical progression in men with oligometastatic prostate cancer. a Local progression-free survival of the entire cohort (blue), HSPC [34] and CRPC (green). b Biochemical progression-free survival of the entire cohort (blue), HSPC [34] and CRPC (green). c Distant progression-free survival of the entire cohort (blue), HSPC [34] and CRPC (green)
Effect of stereotactic ablative radiotherapy on delaying subsequent therapy in men with oligometastatic prostate cancer. a Time-to-next therapy of the entire cohort (blue), HSPC [34] and CRPC (green). b Time to ADT initiation in men with oligometastatic HSPC
Discussion
This study demonstrates that consolidative SABR in men with OPC is well tolerated and appears to have a clinical signal adding to a growing literature of evidence, validating its use. We report 1-year LPFS of 92% and bPFS and DPFS of 69%, and in those with HSPC not treated with hormone therapy, 61% remain free of disease following SABR. Furthermore, treatment was very well tolerated with 24 patients experiencing grade 1 toxicity, 7 with grade 2 toxicities, and no grade 3 or higher toxicities observed.
Perhaps, the most notable contributor to the subjective well-being of a man with metastatic HSPC is the delaying or deferring of ADT, the side effects of which can significantly hamper a patient’s lifestyle and systemic health [11]. With ADT, in addition to decrease in subjective feelings of wellness associated with androgen loss, there has been reported increased risk of osteoporosis, cardiovascular-related mortality, and diabetes [26]. Consistent with prior retrospective reports [12, 27] and the recently reported randomized phase II STOMP trial [9], our study also suggests that SABR can substantially delay initiation of ADT in men with oligometastatic HSPC for up to a year. In addition, unlike ADT, SABR is associated with mild side effects without an associated decrement in quality of life measured in both acute and long-term follow-ups [9].
STOMP represents the first published prospective randomized trial of MDT in OPC and validated the efficacy of SABR for MDT by demonstrating a superior ADT-FS (21 months vs 13 months) compared to observation [9, 13]. Justification for its advent was supported by an accumulation of retrospective and observational studies reporting durable LPFS, DPFS, and ADT-FS with the use of MDT [17,18,19, 23, 24]. The results of our institutional experience are concordant with these reports and in addition add novel information to the already established body of the literature. Specifically, the majority of men in this report (53%) had ≥ 2 metastases, and thus, our study examines a population of OPC with a heavier disease burden than has been explored in the current literature [9, 17, 19, 28]. Rates of 2-year distant and progression-free survival reported in the literature following SABR range from 30 to 40%, and in a subset of those with oligometastatic progression retreated with SABR, the proportion of individuals remaining progression-free is as high as 50% at last follow-up [28]. Herein, we report a 1-year DPFS rate of 69%, which compares favorably to the aforementioned studies and, therefore, may justify the more aggressive use of MDT in men with several oligometastatic foci.
Thus far, the outcomes of interest and treatment intent of SABR in OPC have, for the most part, been aimed at delaying the start of palliative ADT. With growing support for its efficacy in this realm, the aims and goals of MDT may shift from a palliative nature to a definitive one by offering these men a second (and in the context of salvage radiation, a third) chance for cure. In alignment with the Hellman–Weichselbaum spectrum theory of metastasis, the validation and subsequent adoption of more sensitive imaging modalities such as NaF, Choline C-11, and DCFPyL PET/CT scan can allow for earlier detection of low-volume metastatic disease that subsequently can be treated with local therapy, possibly with definitive intent. Justification for such a paradigm is also supported by retrospective evidence that MDT improves prostate cancer cause specific survival in a propensity-matched cohort [29]. Therefore, treatment intensification aimed at simultaneously eradicating other sites of microscopic metastatic disease through the use of concurrent ADT, which is retrospectively associated with improved DPFS when combined with SABR [17], non-castrating antiandrogens such as enzalutamide, and chemotherapies such as docetaxel and radiopharmaceuticals may be justified.
In addition to prevent the site-specific complications associated with local progression of metastases, SABR is a complimentary local treatment to maximize durability of systemic approaches. SABR has already been shown to improve disease control in lung cancer patients treated with systemic oncogene-directed therapies through ablation of resistant clones [7, 30, 31]. The ability to maintain men with CRPC on second-line hormonal agents that are oligoprogressing and delay chemotherapy adds significantly to the clinical options for these patients. Our data showing that SABR can delay distant progression and time-to-initiation of the next line of therapy (median 42–45 weeks) compares very favorably to any of the approved systemic agents in the CRPC space [32, 35]. Finally, the highly conformal nature of SABR limits radiation-associated immunosuppression [33] and may be well suited for concurrent use with immune therapies.
Our study has all the intrinsic limitations of a small retrospective series, heterogeneity, and inclusion of shorter follow-up timeframes in our series limits definitive conclusions following consolidative SABR in OPC. In addition, a compelling weakness is that attempts to define the oligometastatic state by radiographic enumeration of lesions will always be limited by the sensitivity and specificity of the imaging modality and other patient–disease factors that are not well understood. As molecular imaging modalities such as prostate-specific membrane antigen (PSMA)-targeted imaging mature, the value of MDT in the oligometastatic state may increase further as patients previously defined as oligometastatic based on conventional imaging may have additional detectable tumor deposits and require reclassification as polymetastatic [36]. Regardless, our preliminary data suggest that SABR in OPC men warrants continued prospective study. In addition to the recent reporting of the Belgian STOMP trial, more definitive conclusions await the completion and reporting of other prospective randomized studies such as our Baltimore ORIOLE trial (NCT02680587).
References
Hellman S, Weichselbaum RR (1995) Oligometastases. J Clin Oncol 13(1):8–10
Tosoian JJ, Gorin MA, Ross AE, Pienta KJ, Tran PT, Schaeffer EM (2017) Oligometastatic prostate cancer: definitions, clinical outcomes, and treatment considerations. Nat Rev Urol 14(1):15–25
Uppal A, Wightman SC, Mallon S, Oshima G, Pitroda SP, Zhang Q, Huang X, Darga TE, Huang L, Andrade J, Liu H, Ferguson MK, Greene GL, Posner MC, Hellman S, Khodarev NN, Weichselbaum RR (2015) 14q32-encoded microRNAs mediate an oligometastatic phenotype. Oncotarget 6(6):3540–3552
Wong AC, Watson SP, Pitroda SP, Son CH, Das LC, Stack ME, Uppal A, Oshima G, Khodarev NN, Salama JK, Weichselbaum RR, Chmura SJ (2016) Clinical and molecular markers of long-term survival after oligometastasis-directed stereotactic body radiotherapy (SBRT). Cancer 122(14):2242–2250
Reyes DK, Pienta KJ (2015) The biology and treatment of oligometastatic cancer. Oncotarget 6(11):8491–8524
Palma DA, Salama JK, Lo SS, Senan S, Treasure T, Govindan R, Weichselbaum R (2014) The oligometastatic state—separating truth from wishful thinking. Nat Rev Clin Oncol 11(9):549–557
Gomez DR, Blumenschein GR Jr, Lee JJ, Hernandez M, Ye R, Camidge DR, Doebele RC, Skoulidis F, Gaspar LE, Gibbons DL, Karam JA, Kavanagh BD, Tang C, Komaki R, Louie AV, Palma DA, Tsao AS, Sepesi B, William WN, Zhang J, Shi Q, Wang XS, Swisher SG, Heymach JV (2016) Local consolidative therapy versus maintenance therapy or observation for patients with oligometastatic non-small-cell lung cancer without progression after first-line systemic therapy: a multicentre, randomised, controlled, phase 2 study. Lancet Oncol 17(12):1672–1682
Iyengar P, Wardak Z, Gerber DE, Tumati V, Ahn C, Hughes RS, Dowell JE, Cheedella N, Nedzi L, Westover KD, Pulipparacharuvil S, Choy H, Timmerman RD (2018) Consolidative radiotherapy for limited metastatic non-small-cell lung cancer: a phase 2 randomized clinical trial. JAMA Oncol 4(1):e173501
Ost P, Reynders D, Decaestecker K, Fonteyne V, Lumen N, De Bruycker A, Lambert B, Delrue L, Bultijnck R, Claeys T, Goetghebeur E, Villeirs G, De Man K, Ameye F, Billiet I, Joniau S, Vanhaverbeke F, De Meerleer G (2018) Surveillance or metastasis-directed therapy for oligometastatic prostate cancer recurrence: a prospective, randomized, multicenter phase II trial. J Clin Oncol 36(5):446–453
Collen C, Christian N, Schallier D, Meysman M, Duchateau M, Storme G, De Ridder M (2014) Phase II study of stereotactic body radiotherapy to primary tumor and metastatic locations in oligometastatic nonsmall-cell lung cancer patients. Ann Oncol 25(10):1954–1959
Cornford P, Bellmunt J, Bolla M, Briers E, De Santis M, Gross T, Henry AM, Joniau S, Lam TB, Mason MD, van der Poel HG, van der Kwast TH, Rouviere O, Wiegel T, Mottet N (2016) EAU-ESTRO-SIOG guidelines on prostate cancer. Part II: treatment of relapsing, metastatic, and castration-resistant prostate cancer. Eur Urol 71:630–642
Ost P, Bossi A, Decaestecker K, De Meerleer G, Giannarini G, Karnes RJ, Roach M 3rd, Briganti A (2015) Metastasis-directed therapy of regional and distant recurrences after curative treatment of prostate cancer: a systematic review of the literature. Eur Urol 67(5):852–863
Phillips RM, Hayman J, Tran PT (2018) STOMPing out hormone-sensitive metastases with local therapies in prostate cancer. J Clin Oncol 36(5):435–437
Schweizer MT, Zhou XC, Wang H, Yang T, Shaukat F, Partin AW, Eisenberger MA, Antonarakis ES (2013) Metastasis-free survival is associated with overall survival in men with PSA-recurrent prostate cancer treated with deferred androgen deprivation therapy. Ann Oncol 24(11):2881–2886
Ost P, Decaestecker K, Lambert B, Fonteyne V, Delrue L, Lumen N, Ameye F, De Meerleer G (2014) Prognostic factors influencing prostate cancer-specific survival in non-castrate patients with metastatic prostate cancer. Prostate 74(3):297–305
Sridharan S, Steigler A, Spry NA, Joseph D, Lamb DS, Matthews JH, Atkinson C, Tai KH, Duchesne G, Christie D, Attia J, Holliday EG, Denham JW (2016) Oligometastatic bone disease in prostate cancer patients treated on the TROG 03.04 RADAR trial. Radiother Oncol 121(1):98–102
Ost P, Jereczek-Fossa BA, As NV, Zilli T, Muacevic A, Olivier K, Henderson D, Casamassima F, Orecchia R, Surgo A, Brown L, Tree A, Miralbell R, De Meerleer G (2016) Progression-free survival following stereotactic body radiotherapy for oligometastatic prostate cancer treatment-naive recurrence: a multi-institutional analysis. Eur Urol 69(1):9–12
Muacevic A, Kufeld M, Rist C, Wowra B, Stief C, Staehler M (2013) Safety and feasibility of image-guided robotic radiosurgery for patients with limited bone metastases of prostate cancer. Urol Oncol 31(4):455–460
Muldermans JL, Romak LB, Kwon ED, Park SS, Olivier KR (2016) Stereotactic body radiation therapy for oligometastatic prostate cancer. Int J Radiat Oncol Biol Phys 95(2):696–702
Karnes RJ, Murphy CR, Bergstralh EJ, DiMonte G, Cheville JC, Lowe VJ, Mynderse LA, Kwon ED (2015) Salvage lymph node dissection for prostate cancer nodal recurrence detected by 11C-choline positron emission tomography/computerized tomography. J Urol 193(1):111–116
De Bleser E, Tran PT, Ost P (2017) Radiotherapy as metastasis-directed therapy for oligometastatic prostate cancer. Curr Opin Urol 27(6):587–595
Loo BW Jr, Chang JY, Dawson LA, Kavanagh BD, Koong AC, Senan S, Timmerman RD (2011) Stereotactic ablative radiotherapy: what’s in a name? Pract Radiat Oncol 1(1):38–39
Schick U, Jorcano S, Nouet P, Rouzaud M, Vees H, Zilli T, Ratib O, Weber DC, Miralbell R (2013) Androgen deprivation and high-dose radiotherapy for oligometastatic prostate cancer patients with less than five regional and/or distant metastases. Acta Oncol 52(8):1622–1628
Ingrosso G, Trippa F, Maranzano E, Carosi A, Ponti E, Arcidiacono F, Draghini L, Di Murro L, Lancia A, Santoni R (2017) Stereotactic body radiotherapy in oligometastatic prostate cancer patients with isolated lymph nodes involvement: a two-institution experience. World J Urol 35(1):45–49
Donovan JL, Hamdy FC, Lane JA, Mason M, Metcalfe C, Walsh E, Blazeby JM, Peters TJ, Holding P, Bonnington S, Lennon T, Bradshaw L, Cooper D, Herbert P, Howson J, Jones A, Lyons N, Salter E, Thompson P, Tidball S, Blaikie J, Gray C, Bollina P, Catto J, Doble A, Doherty A, Gillatt D, Kockelbergh R, Kynaston H, Paul A, Powell P, Prescott S, Rosario DJ, Rowe E, Davis M, Turner EL, Martin RM, Neal DE, Protec TSG (2016) Patient-reported outcomes after monitoring, surgery, or radiotherapy for prostate cancer. N Engl J Med 375(15):1425–1437
Crawford ED, Moul JW (2015) ADT risks and side effects in advanced prostate cancer: cardiovascular and acute renal injury. Oncology 29(1):55–58–65–66 (Williston Park)
Berkovic P, De Meerleer G, Delrue L, Lambert B, Fonteyne V, Lumen N, Decaestecker K, Villeirs G, Vuye P, Ost P (2013) Salvage stereotactic body radiotherapy for patients with limited prostate cancer metastases: deferring androgen deprivation therapy. Clin Genitourin Cancer 11(1):27–32
Decaestecker K, De Meerleer G, Lambert B, Delrue L, Fonteyne V, Claeys T, De Vos F, Huysse W, Hautekiet A, Maes G, Ost P (2014) Repeated stereotactic body radiotherapy for oligometastatic prostate cancer recurrence. Radiat Oncol 9:135
Steuber T, Jilg C, Tennstedt P, De Bruycker A, Tilki D, Decaestecker K, Zilli T, Jereczek-Fossa BA, Wetterauer U, Grosu AL, Schultze-Seemann W, Heinzer H, Graefen M, Morlacco A, Karnes RJ, Ost P (2018) Standard of care versus metastases-directed therapy for PET-detected nodal oligorecurrent prostate cancer following multimodality treatment: a multi-institutional case-control study. Eur Urol Focus. https://doi.org/10.1016/j.euf.2018.02.015
Gan GN, Weickhardt AJ, Scheier B, Doebele RC, Gaspar LE, Kavanagh BD, Camidge DR (2014) Stereotactic radiation therapy can safely and durably control sites of extra-central nervous system oligoprogressive disease in anaplastic lymphoma kinase-positive lung cancer patients receiving crizotinib. Int J Radiat Oncol Biol Phys 88(4):892–898
Weickhardt AJ, Scheier B, Burke JM, Gan G, Lu X, Bunn PA Jr, Aisner DL, Gaspar LE, Kavanagh BD, Doebele RC, Camidge DR (2012) Local ablative therapy of oligoprogressive disease prolongs disease control by tyrosine kinase inhibitors in oncogene-addicted non-small-cell lung cancer. J Thorac Oncol 7(12):1807–1814
Handy CE, Antonarakis ES (2016) Sequencing treatment for castration-resistant prostate cancer. Curr Treat Options Oncol 17(12):64
Wild AT, Herman JM, Dholakia AS, Moningi S, Lu Y, Rosati LM, Hacker-Prietz A, Assadi RK, Saeed AM, Pawlik TM, Jaffee EM, Laheru DA, Tran PT, Weiss MJ, Wolfgang CL, Ford E, Grossman SA, Ye X, Ellsworth SG (2016) Lymphocyte-sparing effect of stereotactic body radiation therapy in patients with unresectable pancreatic cancer. Int J Radiat Oncol Biol Phys 94(3):571–579
Kotecha R, Djemil T, Tendulkar RD, Reddy CA, Thousand RA, Vassil A, Stovsky M, Berglund RK, Klein EA, Stephans KL (2016) Dose-escalated stereotactic body radiation therapy for patients with intermediate- and high-risk prostate cancer: initial dosimetry analysis and patient outcomes. Int J Radiat Oncol Biol Phys 95(3):960–964
Beauval JB, Loriot Y, Hennequin C, Rozet F, Barthelemy P, Borchiellini D, Schlurmann Constans F, Gross E, Maillet D, Pasticier G et al (2018) Loco-regional treatment for castration-resistant prostate cancer: is there any rationale? A critical review from the AFU-GETUG. Crit Rev Oncol Hematol 122:144–149
Bouchelouche K, Choyke PL (2016) PSMA PET in prostate cancer—a step towards personalized medicine. Curr Opin Oncol 28(3):216–221. https://doi.org/10.1097/CCO.0000000000000277
Acknowledgements
PT Tran was supported by the Nesbitt-McMaster Foundation, Ronald Rose & Joan Lazar; Movember Foundation, Prostate Cancer Foundation; Commonwealth Foundation; NIH/NCI (R01CA166348 and U01CA2120007).
Author information
Authors and Affiliations
Contributions
CLM data collection or management, data analysis, and manuscript writing/editing. RP data collection or management, data analysis, and manuscript writing/editing. MPD manuscript writing/editing. NR data collection or management, data analysis, and manuscript writing/editing. AER protocol/project development, data collection or management, and manuscript writing/editing. ESA protocol/project development, data collection or management, and manuscript writing/editing. DR protocol/project development, data collection or management, and manuscript writing/editing. JW data collection or management and manuscript writing/editing. SAT data collection or management and manuscript writing/editing. DYS protocol/project development, data collection or management, and manuscript writing/editing. CD protocol/project development, data collection or management, and manuscript writing/editing. PCW protocol/project development and data collection or management. TLD protocol/project development and data collection or management. MC protocol/project development and data collection or management. EMS protocol/project development and data collection or management. KJP protocol/project development, data collection or management, and manuscript writing/editing. ME protocol/project development, data collection or management, data analysis, and manuscript writing/editing. PTT protocol/project development, data collection or management, data analysis, and manuscript writing/editing
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Research involving human participants and/or animals
For this type of study, formal consent is not required.
Informed consent
For this type of study, formal consent is not required.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Moyer, C.L., Phillips, R., Deek, M.P. et al. Stereotactic ablative radiation therapy for oligometastatic prostate cancer delays time-to-next systemic treatment. World J Urol 37, 2623–2629 (2019). https://doi.org/10.1007/s00345-018-2477-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-018-2477-2